Digestive system
The Gastrointestinal Tract (GIT) is a continuous tube spanning approximately 7 m in length, featuring two openings: the mouth and the anus. This biological system includes the mouth, pharynx, esophagus, and stomach, followed by the small intestine—which is composed of the duodenum, jejunum, and ileum. It further extends into the large intestine, encompassing the cecum, appendix, colon, rectum, and finally the anus.
Accessory Digestive Organs
Accessory digestive organs are situated outside the GIT but are essential for the digestive process. Most of these organs function as exocrine glands that secrete digestive juices. They include the teeth, tongue, salivary glands, liver, gallbladder, and pancreas.
Structure of the GI Wall
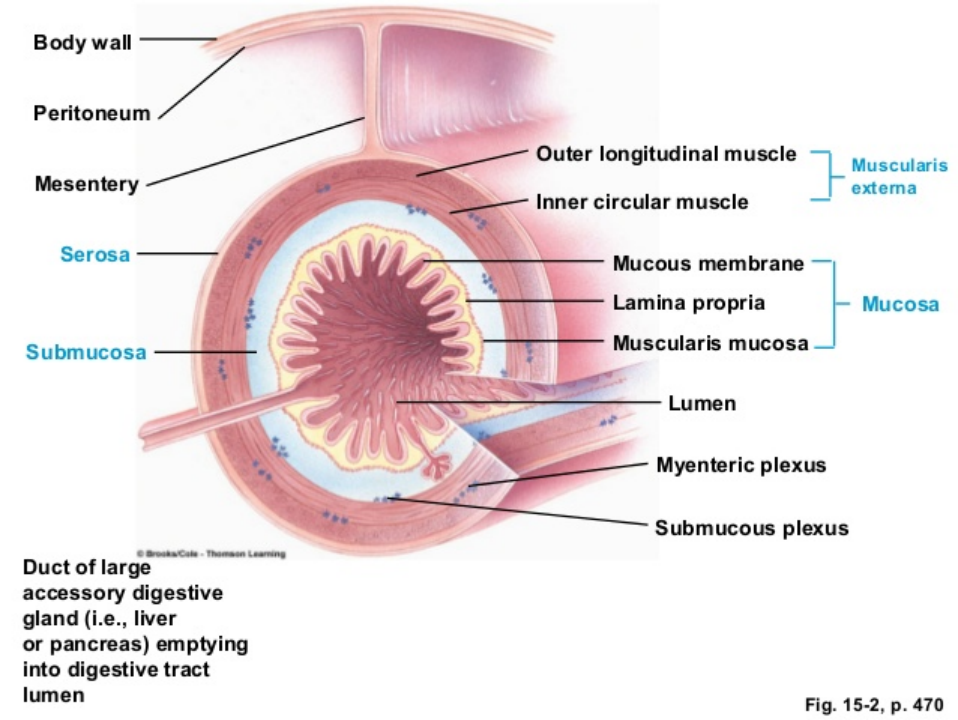
The mucosa is the innermost layer of the digestive tract and is highly folded, although the degree of folding varies regionally. It consists of 3 sublayers: the mucous membrane (epithelium), the lamina propria, and the muscularis mucosa. The mucous membrane is typically composed of columnar cells and is rich in mucus-secreting cells, serving as a protective surface with both exocrine and endocrine glands. The lamina propria is a connective tissue layer containing blood vessels, lymphoid tissue (GALT/MALT), and nerve fibers, which are important for defense against pathogens. The muscularis mucosa is a sparse layer of smooth muscle lying adjacent to the submucosa.
The submucosa is a thick connective tissue layer that provides the digestive tract with distensibility and elasticity. It surrounds the muscularis mucosa and contains large blood and lymph vessels. Additionally, it contains the submucosal plexus, or Meissner’s plexus, which helps regulate local gut activity.
The muscularis externa, or muscularis, surrounds the submucosa and serves as the major smooth muscle layer of the GIT. It is composed of an inner circular layer and an outer longitudinal layer, which are separated by the myenteric plexus, also known as Auerbach’s plexus.
Digestive does job by 5 steps; mechanical processing and motility,secretion,digestion,absorption,elimination
Carbo
Saliva deactibated by acidity in the stomach. starch digestion is completed in the duodenum by pancreatic amylase. further digest of oligosaccharides done by duodenum and jejenum(highest capacity for absorbing sugars).
NB: α-dextrinase which debranches α-limit dextrins
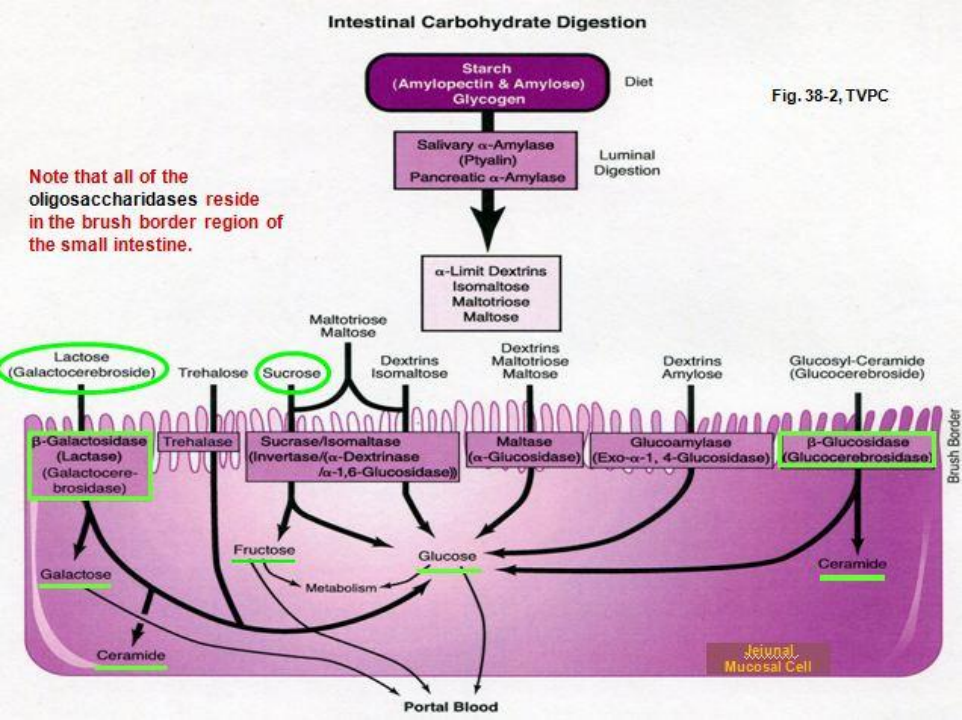
glucose and galactose are actively taken up across the brush border plasma membrane through a Na+-powered secondary active transport protein called SGLT1
fructose is taken up across the brush border membrane by a fructose-specific facilitated transporter called GLUT5
the monosaccharides leave the intestinal epithelial cells at the basolateral membrane via a facilitated diffusion protein called GLUT2 and diffuse into the mucosal capillaries
Protein
pepsins reduce between 10-15% of dietary protein to peptides and amino acids
its digestion in SI done by 3 main proteases;trypsin,chymotrypsin,carboxypeptidase. all made by pancreas. activated by enteropeptidase/enterokinase secreted by mucosa of the duodenum and jejunum. enterokinase converts trypsinogen into trypsin
trypsin activates trypsinogen and also converts chymotrypsinogen and procarboxypeptidases to the active
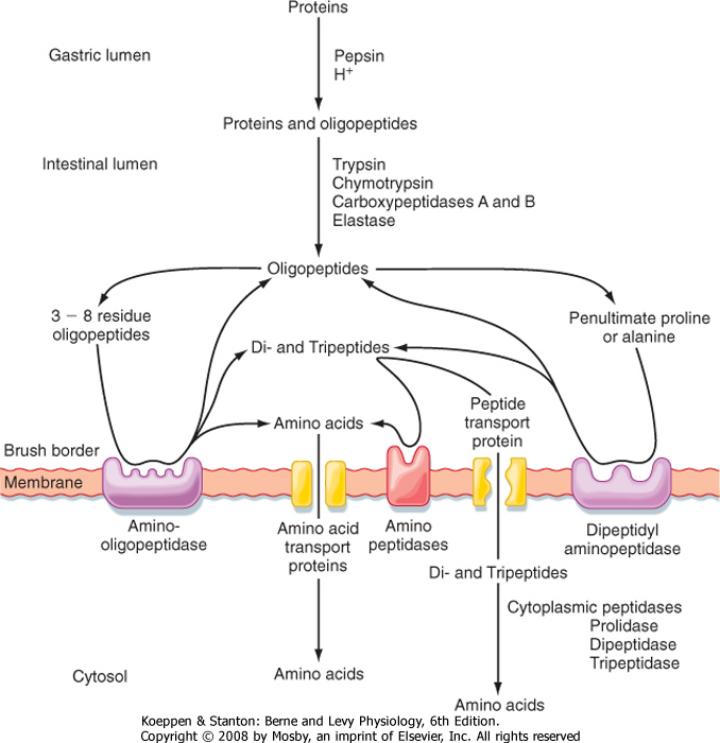
Rate of transport of di and tripeps faster than single amino acids. Membrane responsible for this transport is PepT1 and it brings them in via an H+ conc gradient
amino acids leave the epithelial cells via the basolateral membrane via facilitated diffusion
Lipids
Lipids insolube in water, so they form large fat droplets in the stomach. they only digestd in stomavch and smallm intestine. only the triglycerides on the surface of such fatty masses are accessible to water soluble lipase enzymes
glycerol ester hydroxylase/pancreatic lipase which cleaves off two of the fatty acid chains, yielding free fatty acids and monoglycerides
colipase, a small protein in pancreatic juice is essential for the function of pancreatic lipase
colipase binds the lipase enzyme holding it on the surface of the oil droplet
cholesterol esterase cleaves the ester bond in cholesterol ester to give one fatty acid and free cholesterol
Absorption
Digestion produces micelles which move by the microvilli across the brushborder
when the fat enters, it goes to the SER of the enterocyte, where it is re-esterified before being packaged into chylomicrons(fat with a protein coat) sent to golgi for transport through the lymphatic system through lacteals cause their to big
Water
about 2 l of water is ingested each day
approximately about 7 l/day is contained in GI secretions
about 90% is absorbed across the small intestinal epithelium
only about 50-150 ml of water per day is lost in the feces
its transported by osmosis
NB: Chyme is made isotonic from its hypertonic nature in intestines
water is absorbed from the lumen into capillaries down an osmotic gradient created by the absorption of nutrients in the jejunum and ileum
Na
Na+ movement across the intestinal membrane is greater in the proximal than in the distal intestine
most of the Na+ is transported from the lumen of the SI to the
blood through active mechanisms
these mechanisms depend on a concentration gradient set up by the operation of the Na+, K+-ATPase in the basolateral membrane
these include the:
SGLT1 transporter
Na+-amino acid transporter
Na+/H+ exchanger
the rate of absorption of Na+ is highest in the jejunum because the glucose and neutral amino acid transporters are situated mainly in this region
The Pump (right) basolateral mem uses ATP to create a Sodium "vacuum" inside the cell.
SGLT1 (left) brush border uses that vacuum to suck in Glucose and Sodium.
GLUT2 (right) lets the captured Glucose out into the blood.
Cl- and HCO3-
H+ is transported out of the cell via the Na+/H mechanims. at the same time HCO3- is also transported out via cl/HCO3. the h and HCO3- react to form h2co3 which quicly dissociatesinto H2O and CO2, facilitating the regulation of pH in the intestinal lumen contents below 40-45 mM, .
Ca2+
Can be absorbed either passively throught the whole intestine by sipping through tight junctions or actively
Actively, it enters via CaT1/TRPV6, its then binded as soon as it enters via calbindin or CaBP to carry it through to the other end(basolateral end). Extrusion can occur via CaATPase/PMCA activity
Na+/Ca2+ exchanger
exocytosis
When its inatake is low the active method is more engaged, when high the passive is more engaged, this is because this is due to the short sojourn time of chyme and down regulation of CaT1 and CaBP. CaBP is fully and CaT1 function is approximately 90% vitamin D-dependent
And at high CA2+, vit D is downregulated
Fe
there are two major forms of dietary iron:
heme iron, from haemoglobin and myoglobin from consumption of meat, poultry, and fish
nonheme (ironic) iron obtained from cereals, pulses, legumes, fruits, and vegetables
absorbed by villus enterocytes in the proximal duodenum. efficient in acidic enviro
Fe3+ in nonheme iron is reduced to Fe2+ through the action of a brush border ferrireductase
Iron is transported in by the DMT-1(its not specific for iron only), it maybe stored as ferritin,its ultimately lost when stored like this when the cell is ultimately sloughed at the villus tip
basolateral efflux of iron is iron transport protein ferroportin 1
exported ferrous iron is oxidized by ferroxidase hephaestin to facilitate its binding to plasma transferrin an iron-binding protein of the blood
iron balance controlled by serum-borne, peptide hormone hepcidin (HEPC) of liver
Vitamins
occurs in the intestine
fat soluble vitamins (A, D, E, and K) follow fat path
water soluble are absorbed by diffusion or mediated transport except for b12 due its size and charge
to be absorbed it must first bind to a protein(intinsic factor) made by stomach. when bounded its taken up by lower ileum cells by mediated endocystosis. its also absorbed passively to some extent in SI