chapter 19: the heart
heart anatomy
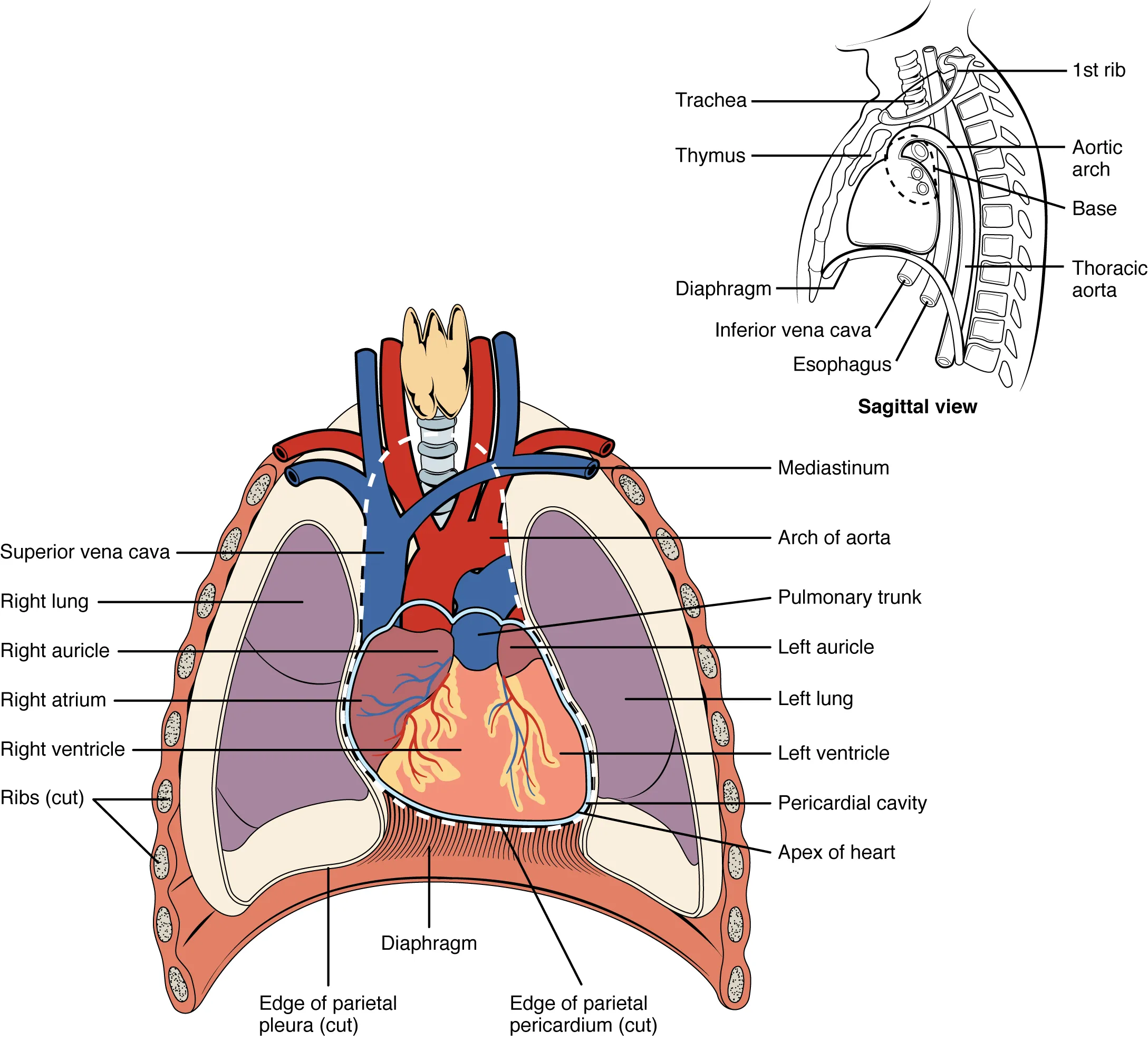
location of the heart
located within the thoracic cavity within the mediastinum
separated from other mediastinal structures by a tough membrane known as the pericardium (pericardial sac) and sits in the pericardial cavity
great veins, vena cavae, great arteries, the aorta and pulmonary trunk are attached to the base of the heart
base located at the level of the third costal cartilage
inferior tip of the heart, the apex, lies just to the left of the sternum between the junction of the fourth and fifth ribs near their articulation with the costal cartilage
slight deviation of the apex to the left reflected on the cardiac notch of the left lung
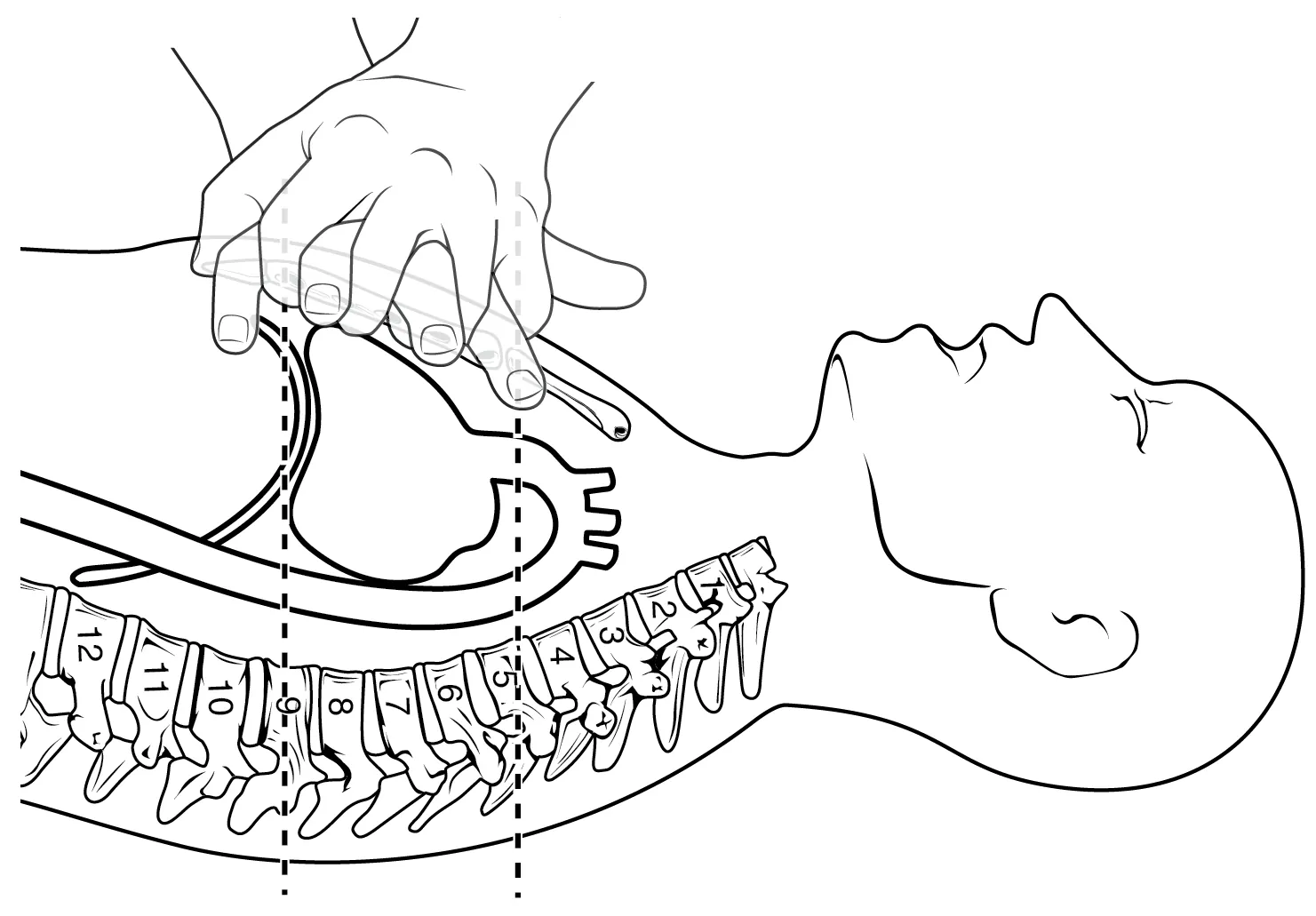
CPR (cardiopulmonary resuscitation)
done by applying pressure with the flat portion of one hand on the sternum between T4 and T9 in order to manually compress the blood within the heart to push the blood to the pulmonary and systemic circuits
compression of chest at least 5 cm deep and at a rate of 100 compressions per minute
shape and size of heart
shaped like a pine-cone and about the size of a fist
12 cm in length
8 cm wide
6 cm thick
weight
female: ~250-300 grams (9-11 ozs)
male: ~300-350 grams (11-12 ozs)
cardiac muscle responds to exercise in a manner similar to skeletal muscle
exercise results in addition of protein myofilaments that inc. the size of the individual cells without increasing their numbers (hypertrophy)
hearts of athletes can pump blood more effectively at lower rates than those of nonathletes
enlarged hearts can also result from pathologies like hypertrophic cardiomyopathy
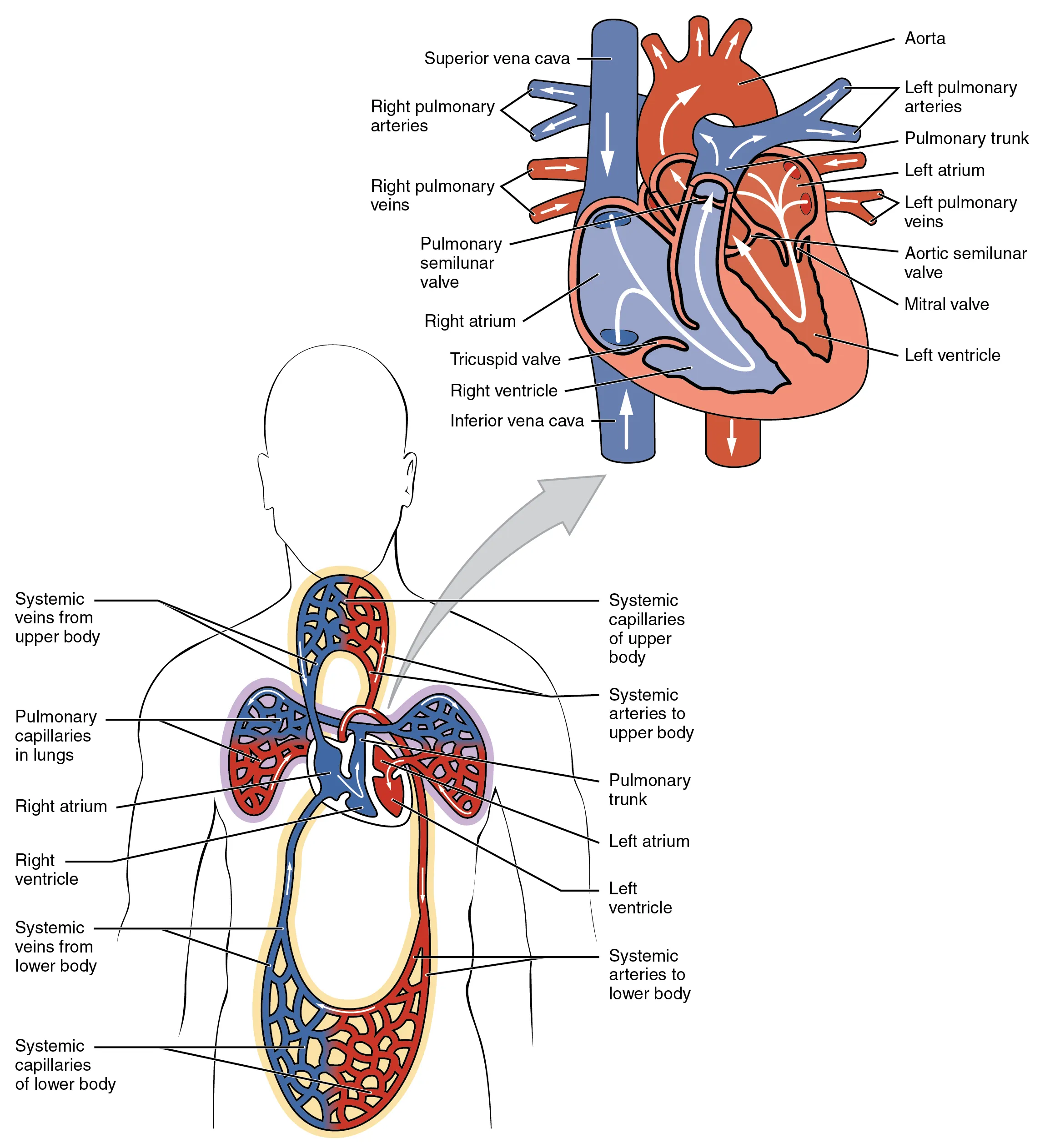
chambers and circulation through the heart
consists of four chambers
atria and ventricles
atria act as receiving chambers and push blood to lower ventricles
ventricles serve as the primary pumping chambers of the and propel blood to the lungs or systemically
pulmonary circuit, transports blood to and from the lungs for oxygenation and exhalation of CO2
systemic circuit, transports oxygenated blood to tissues of the body and returns deoxygenated blood and CO2 to the heart to be sent back to the pulmonary circulation
right ventricle receives deoxygenated blood into the pulmonary trunk which sends blood toward the lungs as it branches to the left and right pulmonary arteries
vessels branch many times before reaching pulmonary capillaries, the site of gas exchange where CO2 exits the blood while oxygen enters
only arteries that carries deoxygenated blood
highly oxygenated blood returning from the pulmonary capillaries in the lungs pass through the pulmonary veins, the only veins that carry highly oxygenated blood
pushes oxygenated blood to the left atrium > left ventricle > aorta > body > systemic capillaries
here, oxygen and nutrients exit capillaries to be used by cells
CO2 and waste products enter the blood
blood exiting systemic capillaries is lower in oxygen concentration than when it entered
capillaries will unit to form venules and then join to form larger veins until the two major systemic veins, the superior and inferior vena cava that will return blood into the right atrium
blood from vena cavae flow
right atrium > right ventricle to be oxygenated again
membranes, surface features, and layers
membranes
membrane that directly surrounds the heart and roots of major vessels and defines the “pericardial cavity” is called the pericardium/pericardial sac
“pericardium” > “around the heart”
two sublayers
sturdy outer fibrous pericardium
tough, dense connective tissue to protect the heart and maintain its position
inner serous pericardium
two layers
parietal pericardium, fused to fibrous pericardium
visceral pericardium/epicardium, fused to the heart and is part of the heart wall
pericardial cavity is filled with lubricating serous fluid and lies between the epicardium and pericardium
epicardium is a macroscopic layer consisting of simple squamous epithelium called mesothelium that is reinforced with loose, irregular, or areolar connective tissue that attaches to pericardium
mesothelium secretes serous fluid that reduces friction during heart contractions
surface features of the heart
four chambers
auricle, ear like structures that can fill will blood and empty into atria
sulcus, fat filled grooves along superior surfaces of the heart that hold coronary blood vessels
coronary sulcus, in btwn atria and ventricles
anterior interventricular sulcus, visible on anterior surface
posterior interventricular sulcus, visible on posterior surface
layers
heart wall composed of three layers
myocardium, thickest middle layer
made up of cardiac muscle cells
framework of collagenous fibers and the blood vessels and nerve fibers that supply it
pumps blood through the heart and major arteries
muscles swirl and spiral around chambers of the heart and form figure 8 patterns around the chambers and around the bases of the great vessels
superficial layers of ventricular muscles wrap around both ventricles
patterns allow for efficient blood pumping
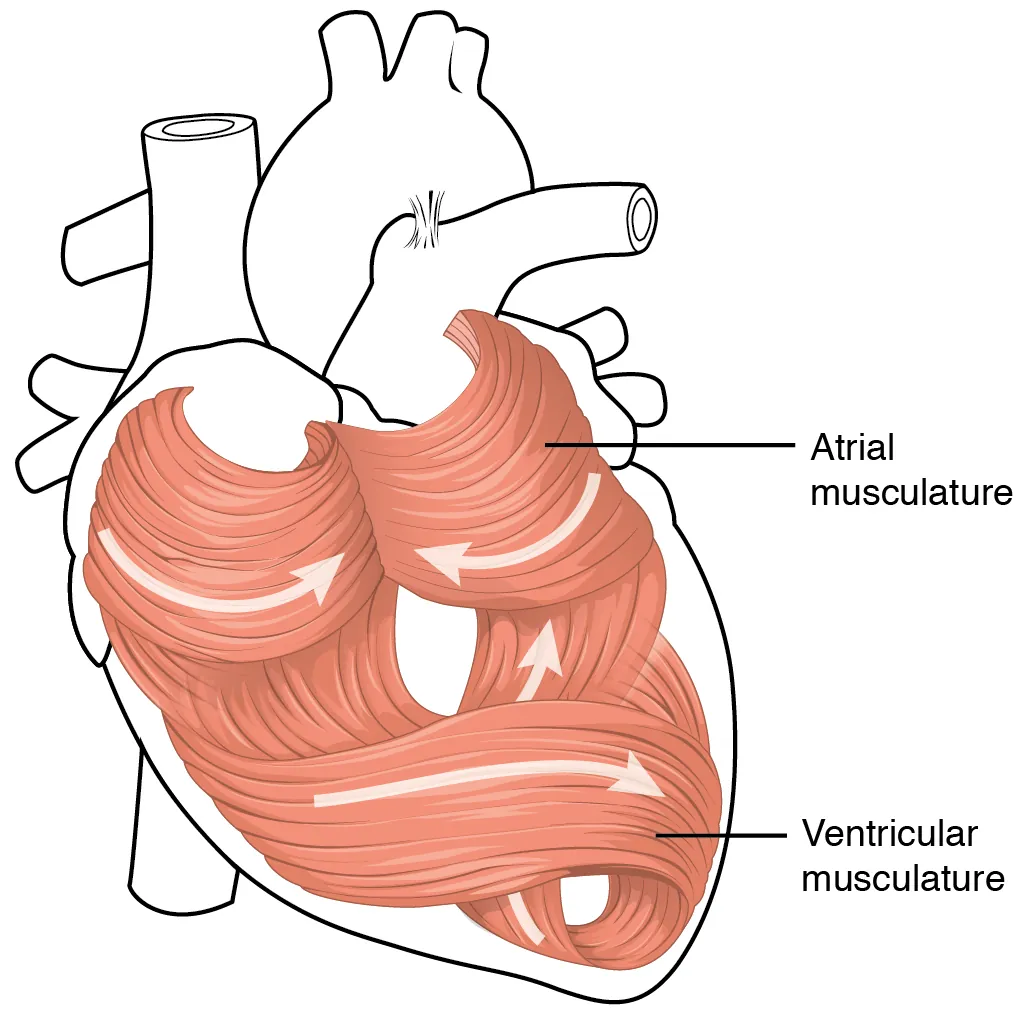
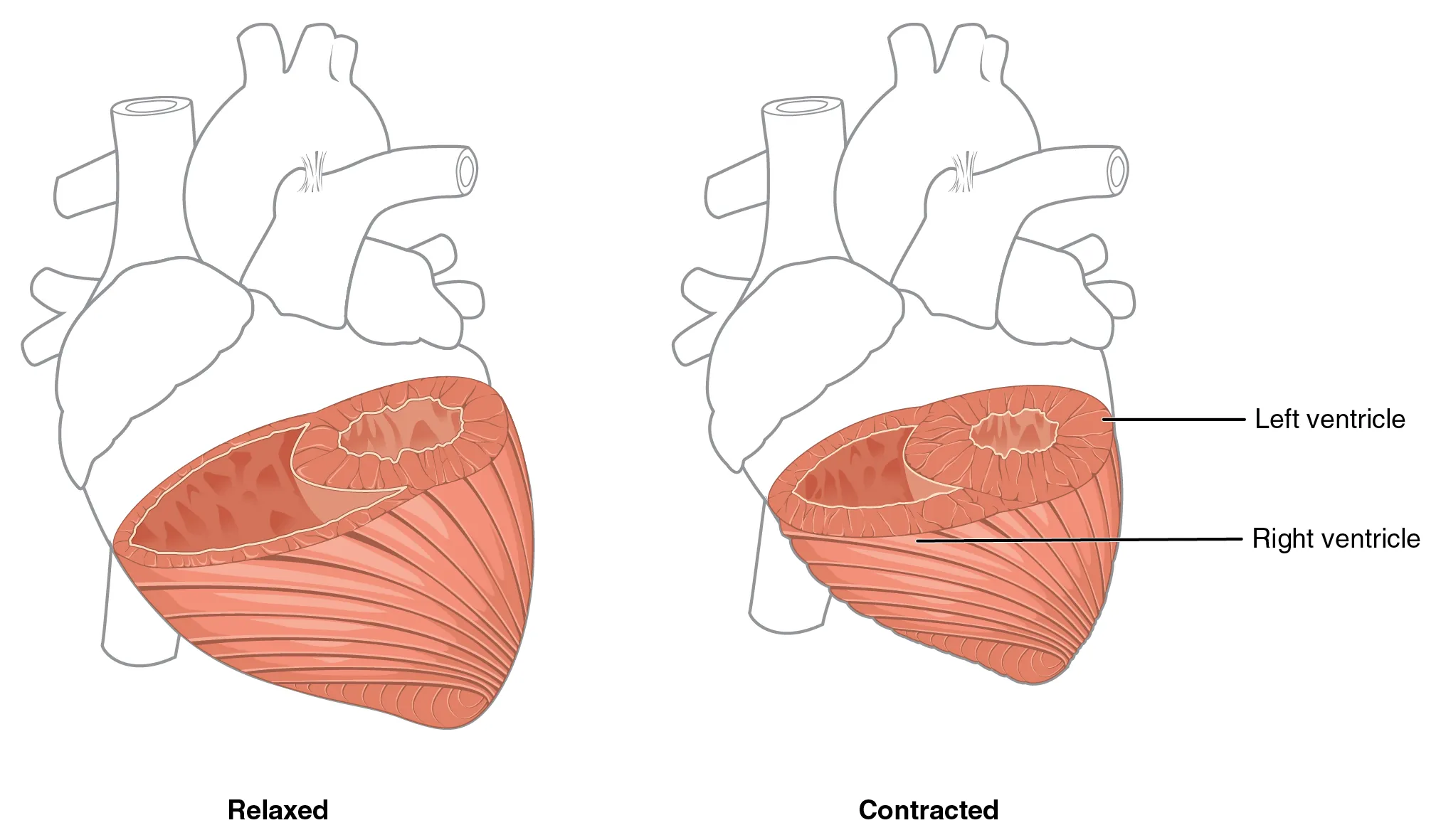
muscles of the left ventricle much thicker and better developed to overcome the high resistance requires to pump blood through the long systemic circuit and must generate a great amount of pressure as compared to right ventricle that only sends it to the pulmonary circuit
endocardium, innermost layer, is joined to the myocardium with a thin layer of connective tissue
lines chambers where blood circulates and covers heart valvues
made up of simple squamous epithelium called endothelium, that is continuous with the endothelial lining of blood vessels
internal structures of the heart
septa of the heart
a septum refers to a wall/partition that divides the heart into chambers
extensions of myocardium lined with endocardium
interatrial septum, in between two atria
in adults, has ana oval shaped depression known as the fossa ovalis, remnant of the opening in the fetal heart known as the foramen ovale, which allowed blood to pass directly from right atrium to left atrium so blood could bypass pulmonary circuit
septum primum
seconds after birth, this flap of tissue that previously acted as a valve will CLOSE the foramen ovale and establish typical cardiac circulation pattern
interventricular septum
intact during fetal development and is substantially thicker than the interatrial septum as the ventricles generate for greater pressure when they contact
atrioventricular septum
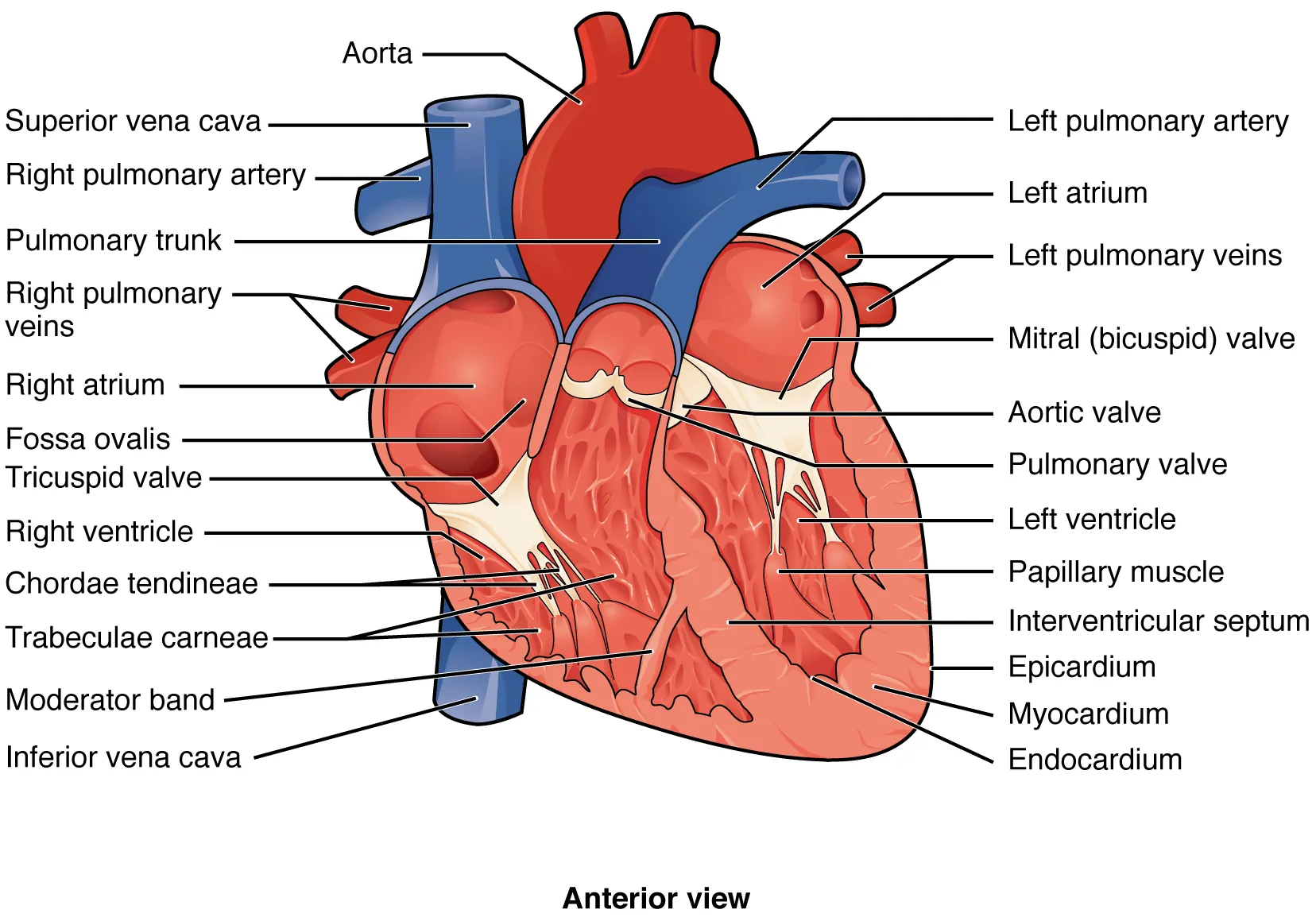
four openings that allow blood to move from atria to ventricles and from the ventricles to great vessels aorta and pulmonary trunk
valve, specialized structure that ensures one way flow of blood
atrioventricular valves, valves btwn atria and ventricles
bicuspid/mitral on the left
tricuspid on the right
semilunar valves, valves btwn ventricles and lead to either the pulmonary trunk or aorta
pulmonary semilunar valve from right ventricle
aortic semilunar valve from left ventricle
remaining tissue is heavily reinforces with dense connective tissue cardiac skeleton, that includes four rings that surround the openings of the atria and ventricles and the openings to the great vessels and a point of attachment for heart valves
important for electrical conduction system
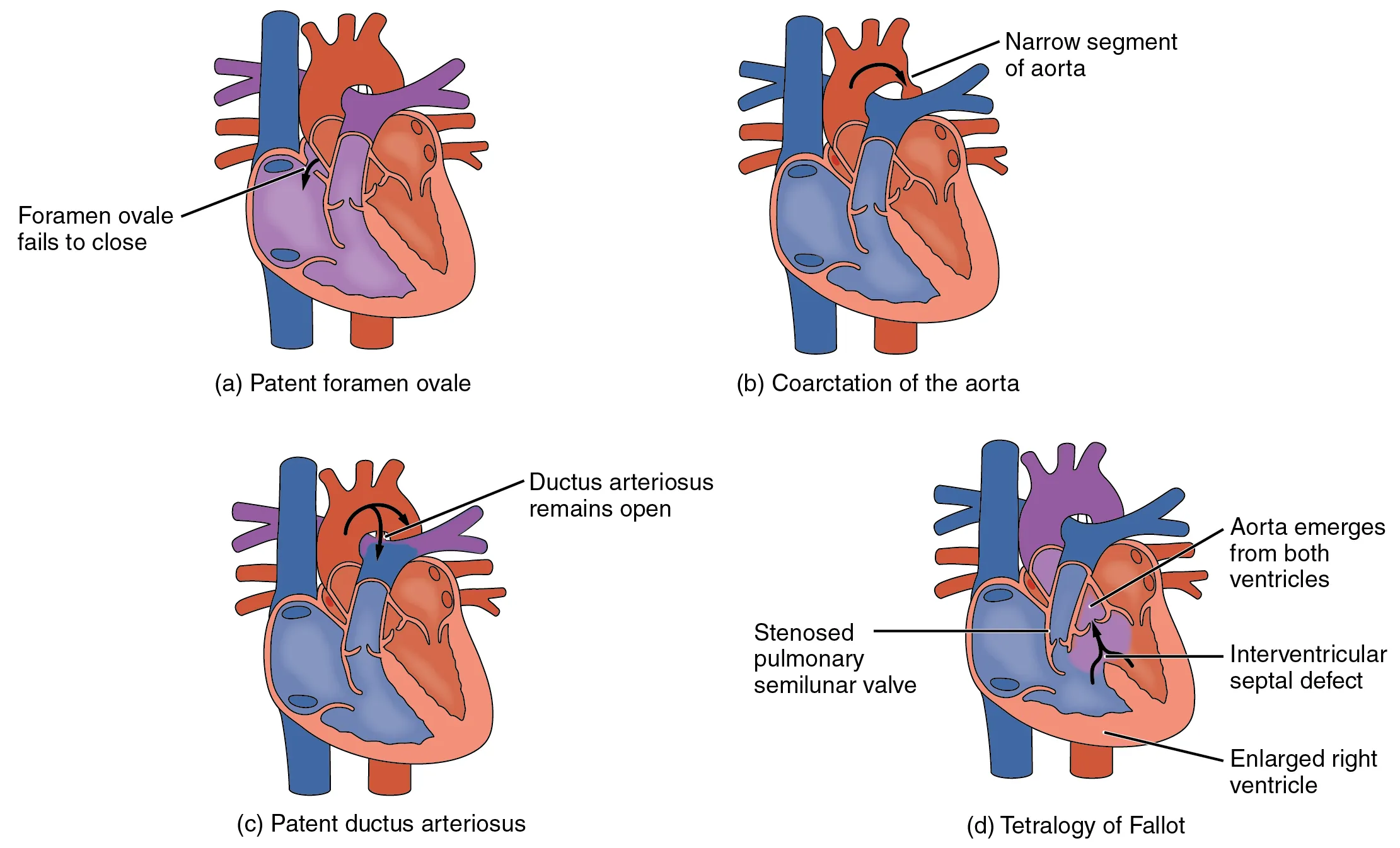
heart defects
patent (open) foramen ovale, septum primum does not close at birth but most people are fortunately asymptomatic. if symptomatic, needs surgery, and is usually noticed with auscultation of a heart murmur and confirmed with imaging with an echocardiogram
coarctation of the aorta, congenital, narrowing of the aorta that is normally located at the insertion of the ligamentum arteriosum (remnants of shunt ductus arteriosus)
if severe, drastically restricts blood flow through primary systemic artery and can be life threatening
symptoms include infants having difficulty breathing, poor appetite and trouble feeding, and failure to thrive
patent ductus arteriosus, ductus arteriosus fails to close
failure to close > blood flowing from higher pressure aorta into lower pressure pulmonary trunk > inc. pulmonary pressure and difficulty respirating
symptoms include shortness of breath, tachycardia, enlarged heart, widened pulse pressure, poor weight gain
treatment includes surgical closure (ligation), manual closure with platinum coils/mesh, or NSAIDs
can lead to congestive heart failure
tetralogy of fallot
occurs from exposure of unknown environmental factors
opening in interventricular septum caused by blockage of pulmonary trunk
low oxygenated blood from RV to the LV and mixes with highly oxygenated blood
distinct heart murmur, low blood oxygen satruation, dyspnea, polycythemia, clubbing of phalanges, difficulty feeding and failure to frow
requires extensive surgical repair
all can lead to “blue baby,” indicating an insufficient supply of oxygenated blood > cyanosis