Ch. 2 - Cornea and Sclera
Cornea and Sclera Overview
The eye's outer connective tissue coat resembles two joined spheres:
Cornea: Anterior transparent sphere, radius of curvature ~8 mm.
Sclera: Posterior opaque sphere, radius of curvature ~12 mm.
Corneal Dimensions
Cornea appears oval from the front; dimensions:
Anterior horizontal diameter: 12 mm
Anterior vertical diameter: 11 mm
View from behind: Circular with diameters of 11.7 mm.
Central curvature is steeper than the periphery:
Radius at anterior surface: 7.8 mm
Radius at posterior surface: 6.5 mm
Thickness:
Central cornea: 0.53 mm
Peripheral cornea: 0.71 mm
Corneal Histo-structural Features
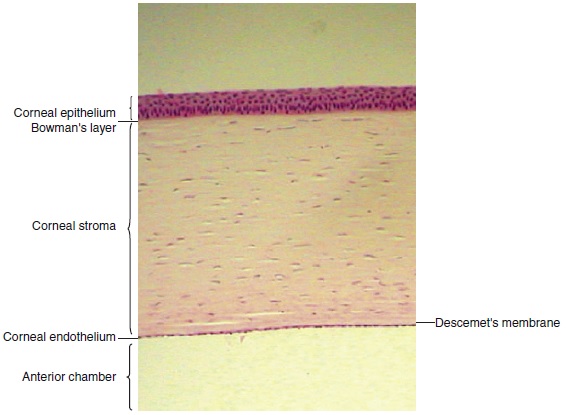
Layers of the Cornea (5 layers from anterior to posterior):
Epithelium: 5-7 cells thick, nonkeratinized squamous cells, contributes to tear film stability.
Bowman's Layer: Dense fibrous sheet, ~8 to 14 µm thick, acellular.
Stroma: Major component of cornea, ~500 µm thick, contains collagen fibrils, keeps the cornea transparent.
Descemet’s Membrane: Basement membrane of endothelium, thickens with age.
Endothelium: Innermost layer, single layer of flattened cells responsible for hydration.
Corneal Function
Refraction: Main refracting surface, contributes 43-48 D to total eye refraction (60-65 D total).
Transparency: Maintains low scattering of light, contributes to vision.
Corneal Cell Types
Epithelial Cells: Superficial layer with tight junctions.
Wing Cells: Transition between surface and basal epithelial cells.
Basal Cells: Stem cells of the corneal epithelium.
Metabolism and Hydration of the Cornea
Oxygen mainly from tears, glucose from aqueous humor; anaerobic metabolism predominates.
Aquaporins: Water channels facilitate hydration, regulate corneal swelling.
Aging and Corneal Pathology
Aging causes thickening of Descemet's membrane, decreased endothelial cell density.
Conditions like keratoconus and recurrent corneal erosion arise from epithelial and stromal irregularities.
Scleral Components
Scleral Structure: Dense connective tissue, varies in thickness (1 mm at posterior pole to 0.3 mm behind rectus muscles).
Episclera: Loose connective tissue, contains blood vessels that supply nutrients to sclera and cornea.
Sclera: Provides shape and support to the eye, rich in collagen fibrils arranged irregularly for strength and flexibility.
Scleral Physiology
Changes occur with myopia and other refractive errors due to altered scleral remodeling.
Conditions leading to scleral thinning include scleral ectasia.
Limbus
Junction between cornea and sclera, contains trabecular meshwork for aqueous drainage.
Clinical relevance in stem cell research, particularly limbal stem cell deficiency.
Key Clinical Comments
Corneal Edema: Caused by loss of barrier functions in the epithelium or endothelium.
Keratoplasty: Surgical replacement of cornea; techniques evolving toward endothelial keratoplasty.
Corneal Neovascularization: Indicative of insufficient oxygen, often seen in contact lens wear.
Stem Cells and Repair: Limbal stem cell deficiency can lead to corneal opacity and loss of clarity, with transplantable epithelium from oral mucosa as a promising treatment.
Conclusion
Understand how corneal structure, function, and pathology interrelate to the overall health of the eye. Aging and surgical interventions noticeably affect the corneal and scleral integrity, impacting visual health and requiring targeted clinical approaches.