Human Physio Blood and Blood Flow
Overview: Cardiovascular system
- Arteries take blood away from the heart.
- Veins return blood to the heart
- Series flow: blood travels through ==systemic== and ==pulmonary== circuits in series
Functional model of the cardiovascular system
- Arteries connect to arterioles, that connect to capillaries, that connect to venules, that connect to veins.
- Systemic arteries maintain pressure during ventricular relacation by changing vessel diameter.
Summary
<<Deoxygenated blood enters the right atrium through superior and inferior vena cava.<<
<<Blood enters right ventricle through triscuspid valve.<<
<<Blood exits right ventricle through pulmonary valve and enters pulmonary artery.<<
<<Left and right pulmonary arteries send blood to lungs, where gas exchange occurs.<<
[[Oxygenated blood returns to heart via pulmonary veins and enters left atrium.[[
[[Blood enters left ventricle through mitral valve.[[
[[Blood exits left ventricle through aortic semilunar valve to enter aorta.[[
[[Aorta distributes blood to the rest of body.[[
Characteristics of blood vessel types
- Endothelium - thin layer, inner lining of all blood vessels
- Surrounded by layers of smooth muscle, elastic and fibrous connective tissue
- Blood vessel types vary in diameter and composition
- Veins have larger diameter and thinner walls as compared to arteries
Pressure gradients in driving blood flow
- Pressure = force exerted by blood through vessel
- Heart creates pressure gradient for bulk flow of blood
- Pressure gradient (△P)
= P at one end of a blood vessel - P at the other end of a blood vessel
- △P in systemic circuit > △P in pulmonary circuit
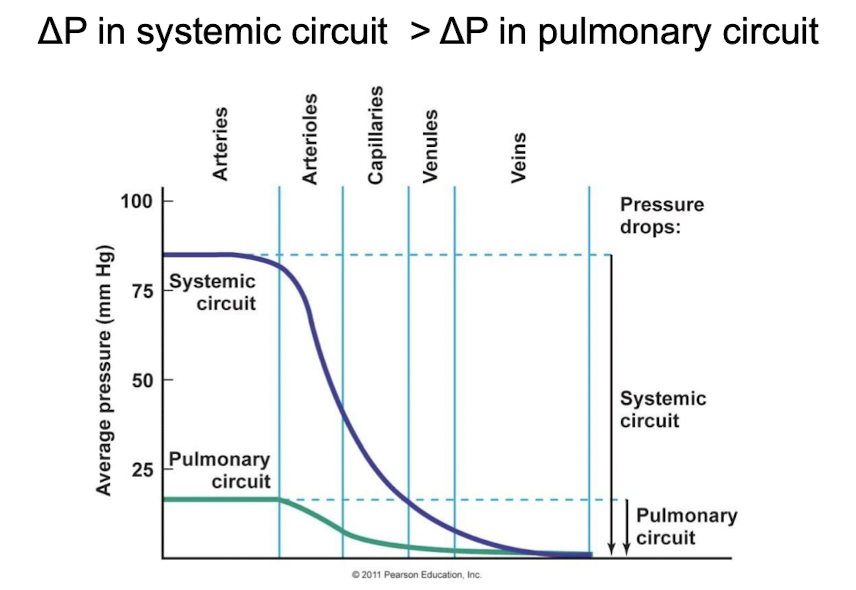
Pressure gradients in blood flow
- Pressure gradient cause a fluid to flow
- Flow α △P
Resistance in blood flow
- Blood Flow = driving force = pressure gradient
- △P drives the blood flow in circulatory system
- Flow direction - high pressure to low pressure
- Factors that affect the blood flow in the cardiovascular system
- Resistance (R) and △P
Flow rate = △P/R
Resistance opposes blood flow
- Resistance to flow - tendency of cardiovascular system to oppose blood flow
- Flow α 1/R
- Factors affecting resistance in blood vessels: equation derived from Poiseuille’s Law
- {{^^Radius (r) of vessel^^{{
- {{In arterioles (and small arteries) - can regulate radius{{
- {{Length of vessel (L){{
- {{Blood viscosity{{
- {{dependent on amount of RBCs and proteins in plasma{{
- Change in ==diameter== → change in resistance and flow
- blood vessels dramatically alter blood flow during ==vasoconstriction== or ^^vasodilation^^
Total peripheral resistance (TPR)
- TPR = combined resistance of all blood vessels within the systemic circuit
- Flow through network varies with resistance
- Vasoconstriction in network → increase resistance → decrease flow
- Vasodilation in network → decrease resistance → increase flow
Pressure throughout systemic circulation
- Blood pressure - highest in arteries and decreases continuously as it flows through circulatory system
- Systolic pressure - exerted on vessel walls when heart contracts
- Diastolic pressure - pressure during relaxation
- Pulse pressure (strength of pressure wave) - systolic pressure - diastolic pressure
- Mean arterial pressure (mean arterial pressure, MAP) is the average arterial pressure throughout one cardiac cycle, systole and diastole
- diastole pressure + 1/3 pulse pressure
Arteries serve as a pressure reservoir
}}Pressure transferred to blood vessels when heart contracts}}
- Ventricular contraction
- Ventricular contracts.
- Semilunar valve opens.
- Aorta and arteries expand and store pressure in elastic walls.
]]Pressure maintained in blood vessels while heart relaxes]]
- Ventricular relaxation
- Isovolumic ventricular relaxation occurs
- Semilunar valve shuts, preventing flow back into ventricle.
- Elastic recoil of arteries sends blood forward into rest of circulatory system.
Arterial Blood Pressure
- Pressure in the aorta
- Varies with cardiac cycle
- Systolic blood pressure = maximum pressure - due to ejection of blood into aorta
- Diastolic blood pressure = minimum pressure - not zero due to elastic recoil
Elastic recoil: the inherent resistance of a tissue (arteries) to changes in shape, and the @@tendency of the tissue to revert to its original shape once deformed.@@
Mean arterial pressure (MAP)
- Mean arterial pressure (MAP) represents the “average” pressure of blood in the arteries, that is, the average force driving blood into vessels that serve the tissues.
Lymphatic system
- Systems of vessels, lymph nodes and organs
- Fluid in the lymphatic system (lymph), carried through the ducts and returned to cardiovascular system
- Allow one-way movement of interstitial fluid from tissues into the circulation
Functions of lymphatic system
- return fluid and proteins filtered out capillaries to circulatory system
- ==pick up fat absorbed== at small intestine and transfer back to circulatory system
- serve as filter to ==help capture and destroy pathogens==
Lymph flow
- valves on lymph vessels
- depend of smooth muscle contractions in larger lymph vessels
Composition of blood
Blood
- Circulation portion of extracellular fluid
- Carry material from one part of body to another
Blood composition
- Plasma
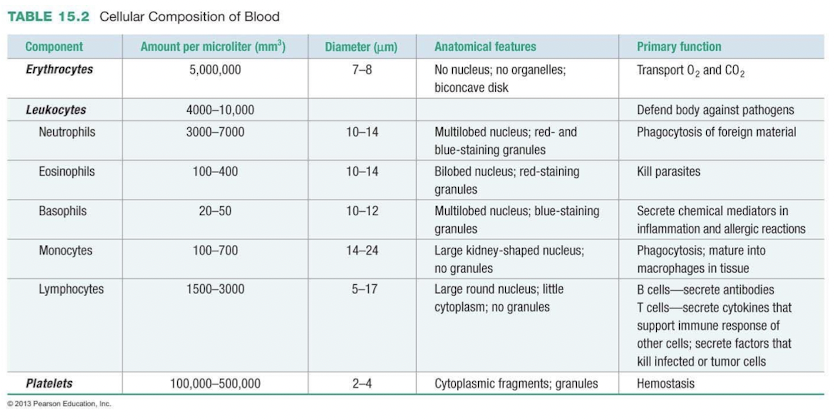
- Erythrocytes (RBC)
- Transport O2 from lung to tissues and CO2 from tissues to lungs
- Leukocytes (WBC)
- Lymphocytes - found in lymphatic system, B- & T-cells
- Monocytes - exit bloodstream and become macrophages
- Neutrophils - phagocyte for bacteria & secretes cytokines
- Eosinophils - phagocyte for parasites & cytokines related to allergies
- Basophils - mediate inflammation & allergies via cytokine release (histamine)
- Platelets
- Coagulation - process by which blood clots prevent blood loss
Hematocrit test
- Measure fraction of RBC to the total blood volume
Hematopoiesis
- controlled by ^^cytokines^^
- Erythropoiesis (RBC production)
- cytokine erythropoietin (EPO)
- EPO made in kidney cells, released in response to low O2 levels in tissues
- White blood cell production
- cytokine colony-stimulating factors (CSFs)
- CSFs made by endothelial cells and white blood cells
- Platelet production
- thrombopoietin (TPO) regulate growth and maturation of megakaryocytes
- TPO produced in liver primarily and kidney
Red blood cells (RBCs)
- Lack nucleus or organelles
- Packed with hemoglobin
- Important characteristics of RBCs:
- concave shape allows for 30% more surface area for carrying O2
- 97% of their content is haemoglobin - binding both O2 and CO2
- Morphology of red blood cells can provide clues to presence of disease
- e.g. sickle cell disease: cells shaped like sickle or crescent moon
genetic defect with abnormal haemoglobin molecules that cause RBCs to change shape
White blood cells (WBCs)
Platelets
- Cytoplasmic fragments derived from megakaryocytes
- Colourless
- Cell fragments
- No nucleus
- Has organelles and granules
- Granules containing secretory products
- Platelets are important in blood clotting
- Hemostasis = stop bleeding
- Three steps to stop bleeding
Vasoconstriction → Platelet plug formation → Coagulation (formation of a blood clot)
Platelet plug formation
- Exposed collagen binds and activates platelets
- Platelet factors are released.
- Factors attract more plateleets.
- Platelets aggregate into platelet plug.
Summary
- [ ] Describe the properties of different blood vessels types
- [ ] Explain the concepts of pressure gradients and resistance in blood flow through blood vessels
- [ ] Describe the major components of blood and their functions