WEEK 1.L.2-Forensic Serology & Bodily Fluids – Comprehensive Exam Notes





Forensic Serology: Scope & Purpose
Detection, identification, classification and study of bodily fluids at or relating to a crime scene.
Extends well beyond blood: any bodily fluid can become evidence.
Evidentiary value:
Link suspect(s), victim(s) and scene(s).
Help establish or reconstruct crime scene(s).
Identify potential weapon(s).
Corroborate / refute circumstantial narratives.
Catalogue of Bodily Fluids Relevant to Forensics
Saliva
Possible components:
Cells → epithelial cells, WBCs, bacterial cells; therefore DNA.
Water , electrolytes, mucus.
Enzymes: (\alpha)-amylase (starch digestion), lingual lipase, kallikrein.
Antimicrobials: lysozyme, lactoferrin.
Opiorphin – endogenous pain-killer.
Forensic merits:
Non-invasive, easy collection (even from stamps, bottles, food, bite marks).
Source of DNA (epithelial cells) & potential ABO antigens (if person is an ABO secretor – of population).
Toxicology: drugs, poisons, alcohol; roadside drug testing common.
Emerging research: highly stable salivary RNA; salivary biomarkers in mass-disaster victim ID.
Sex determination: amelogenin gene, sex-hormone profiling.
Oral microflora as a microbial “fingerprint.”
Semen
Very rich DNA source (spermatozoa).
Contains numerous enzymes & hormones.
Possesses ABH antigens if donor is secretor.
Urine
Composition ≈ water + organic/inorganic chemicals, proteins, hormones.
Can supply cells & chemical signatures (e.g.
drugs, poisons).
Sweat
water; may contain cells, proteins, hormones, chemicals.
Can exhibit ABH antigens in secretors.
Faecal Matter
Dense cellular & chemical matrix; plentiful DNA.
Odour / microbial profile sometimes useful.
Vomit ("Vomitous")
Usually cellular; may contain drug/poison residues.
Scene reconstruction: poisoning, drug abuse, hanging, sexual assault.
Rarely recovered but can corroborate timeline or mechanism.

Blood Fundamentals
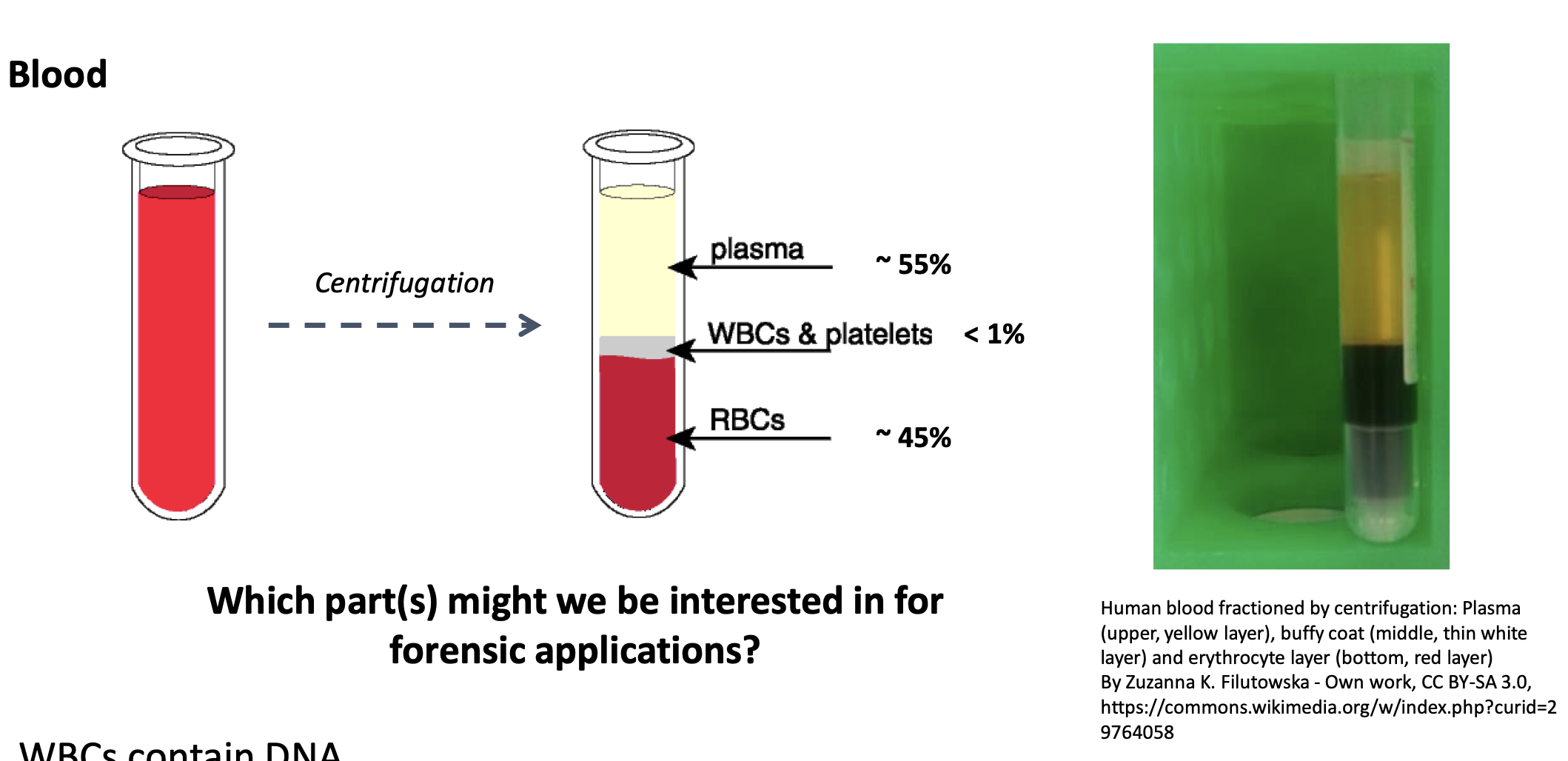
Centrifugation Fractions
Plasma (upper yellow layer; ~):
Contains antibodies & dissolved proteins.
Buffy coat (<): WBCs + platelets.
WBCs = nuclear DNA source.
Erythrocytes (RBCs; ~):
Surface antigens (ABO, Rh, etc.) and haemoglobin.
Whole blood exhibits characteristic blood-spatter patterns essential for Blood Pattern Analysis (BPA).




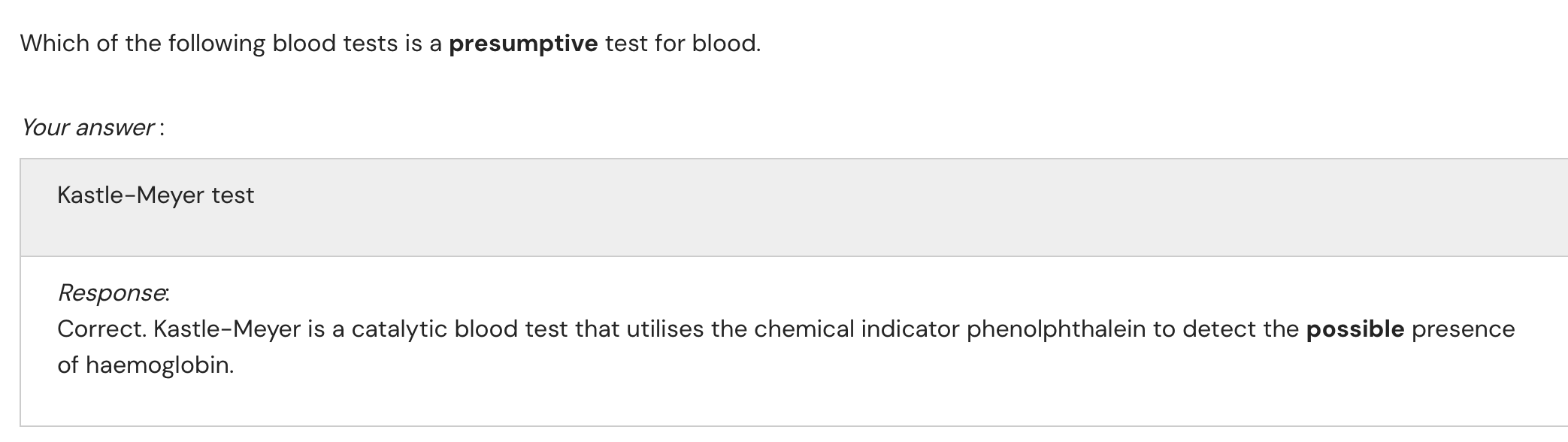
Presumptive Blood Tests
Objective: rapid, inexpensive, colourimetric indication – NOT definitive.
Result language:
“Sample is definitely NOT …” (negative)
“Sample may be / probably is …” (positive)
Common reagents:
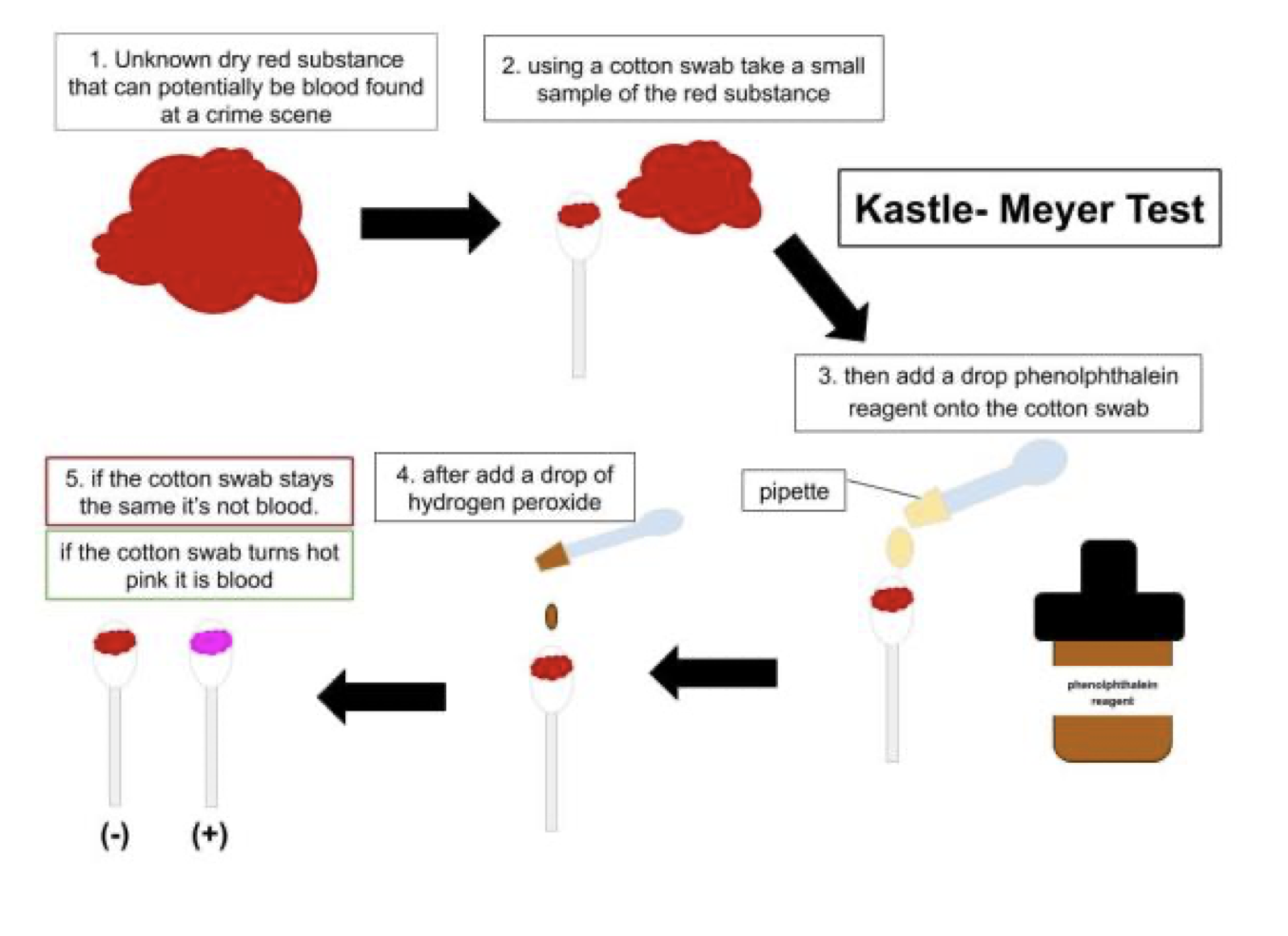
Kastle–Meyer (phenolphthalein).
o-Tolidine, Benzidine (historical, carcinogenic).
Luminol (chemiluminescence).
Principle: haemoglobin’s peroxidase-like activity catalyses → ; coupled oxidation of indicator → colour / light.
Kastle–Meyer Detailed Chemistry
Phenolphthalein is first reduced (colourless) in alkaline solution.
In presence of blood + :
Haeme iron reduces peroxide: .
Phenolphthalein donates the electrons, becoming oxidised → vivid pink.
Caveats:
Wait > ⇒ ambient O(_2) may oxidise reagent → false-positive.
Chemical oxidants (e.g. bleach, Cu(^{2+})) produce colour pre-peroxide.
Works on any vertebrate haemoglobin ⇒ sensitive but not specific.
Luminol
Chemiluminescent spray; reacts with blood traces, glows blue in darkness.
Pros: can reveal latent patterns, even if cleaned.
Cons: dilutes sample; strong oxidiser – may reduce downstream DNA recovery if sample load is low.
Confirmatory Blood Tests
Specific, more costly; designed to prove blood (and sometimes species) presence.
Crystal Assays
Takayama (Haemochromogen)
Sample + pyridine + sugar → pink-red haemochromogen crystals.
Confirms haemoglobin (ferrous) presence.
Teichmann (Haemin)
Dried stain + glacial acetic acid + NaCl/KCl + heat.
RBCs rupture; Fe(^{2+}) → Fe(^{3+}); haemin chloride crystals form.
Crystal morphology can aid species ID.
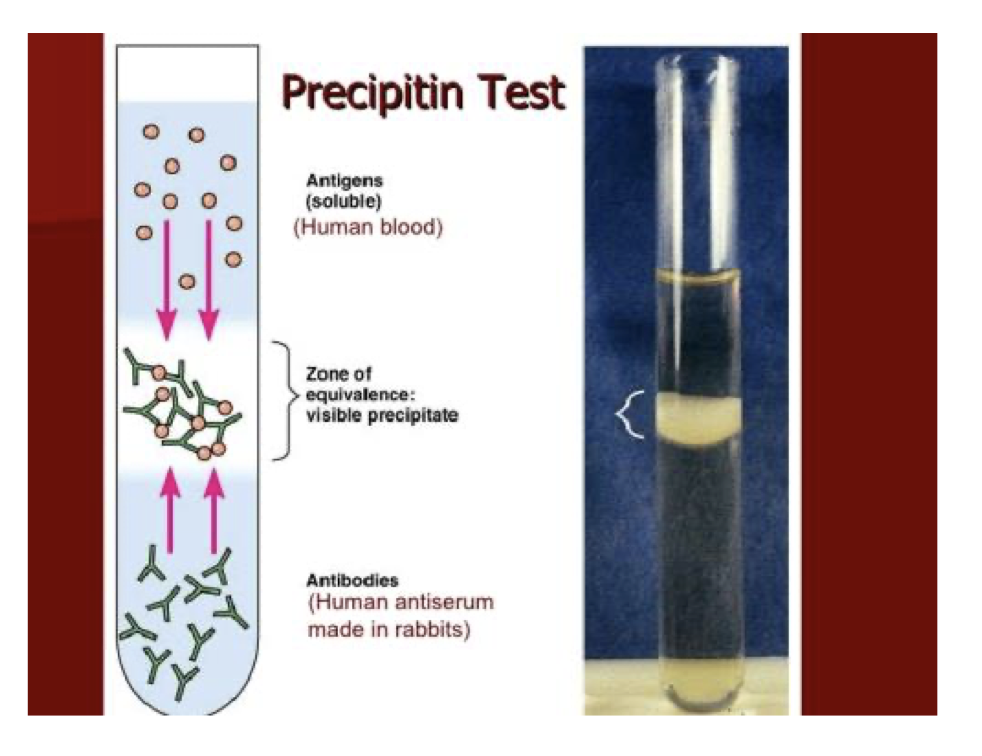
Species Origin — Precipitin Test
Immunological assay: rabbit antiserum raised against known species’ blood.
Antibody + corresponding antigen → visible precipitate.
Distinguishes human vs animal blood.

Blood Typing
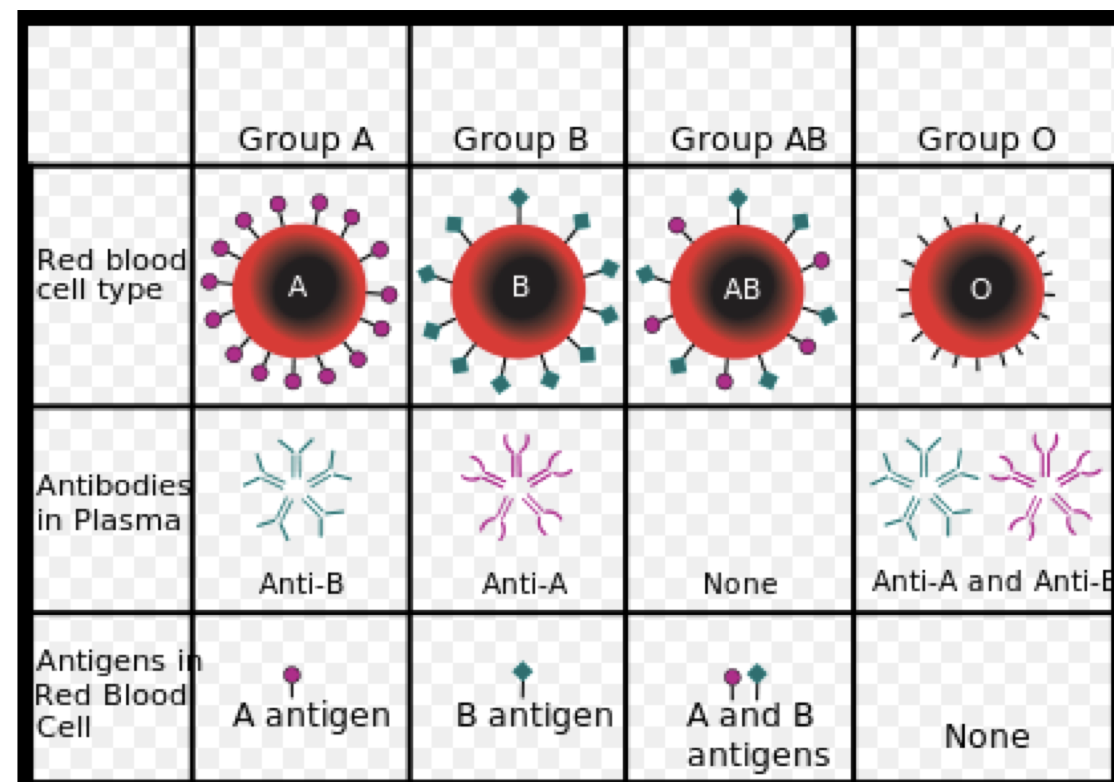
ABO System (1 of 32 Known Systems)
Antigens: A, B carbohydrates on RBC membrane; antibodies reciprocal in plasma.
Type A: A antigen | anti-B antibodies.
Type B: B antigen | anti-A antibodies.
Type AB: both antigens | no anti-A/B antibodies.
Type O: no antigens | anti-A and anti-B antibodies.
Rh(D) antigen designates / (e.g. O(^{+})).
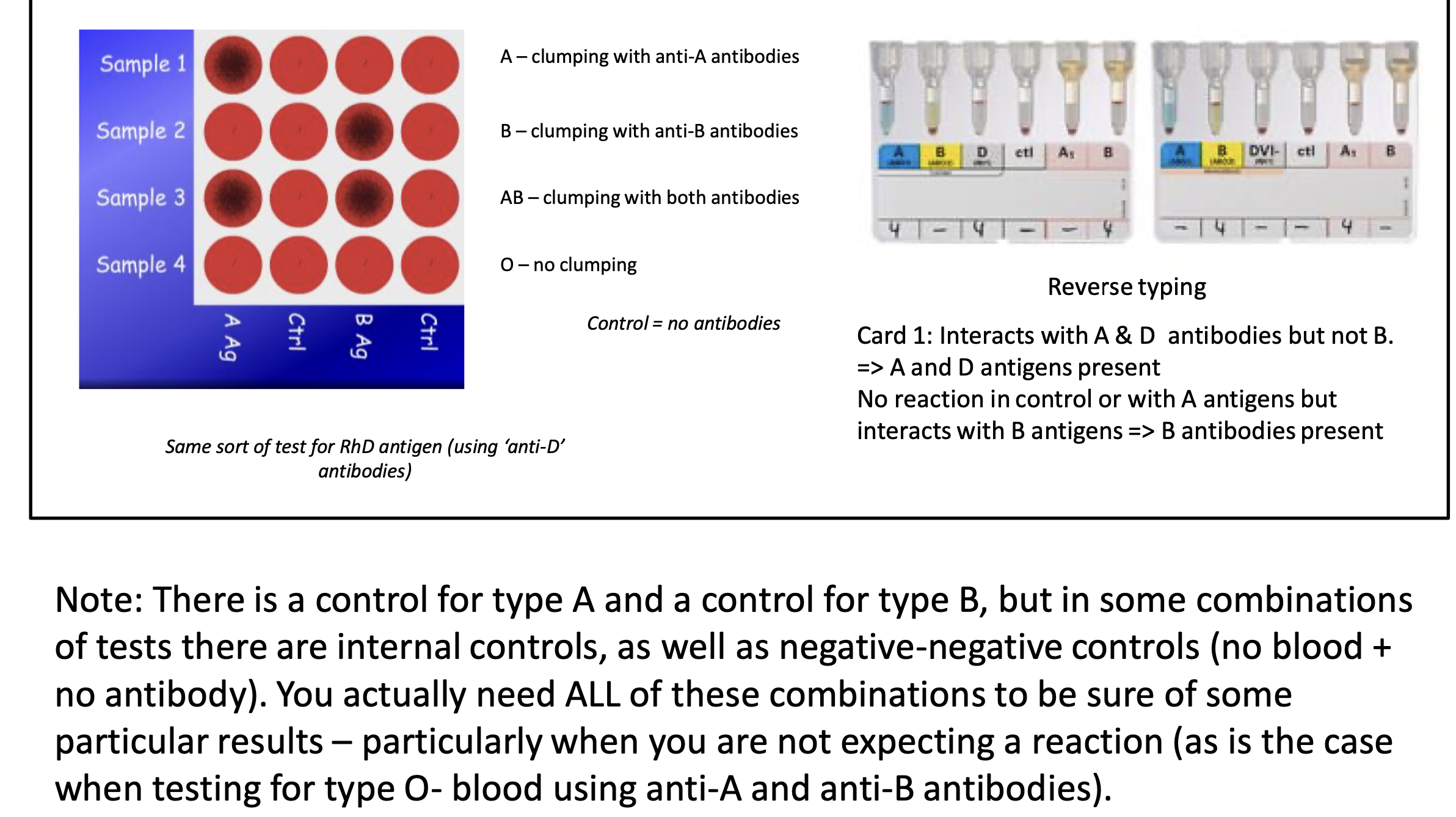
Haemagglutination Test Procedure
Mix unknown blood with anti-A and anti-B antisera (and anti-D for Rh).
Observe clumping (agglutination) pattern:
Clumping in anti-A only ⇒ Type A.
Clumping in both ⇒ AB, etc.
Controls:
Serum/no antibody control to rule out spontaneous agglutination.
Reverse typing: patient serum + known A/B RBCs to confirm reciprocal antibodies.
Population Statistics (Australia as exemplar)
Genetics & Inheritance
Three alleles: A, B (codominant), O (recessive).
Example cross (Parent 1 phenotype A (= AO); Parent 2 phenotype O (= OO)):
Punnett square → AO (Type A) | OO (Type O).
[
\text{Phenotype} \;\longleftrightarrow\; \text{Genotype}\
A: \;AA\;\text{or}\;AO \quad B: \;BB\;\text{or}\;BO \
AB: \;AB \quad O: \;OO
]
answer: You will need to know
1. the antigens and antibodies present in each blood type,
2. possible blood phenotypes inherited given parental phenotype/genotype.
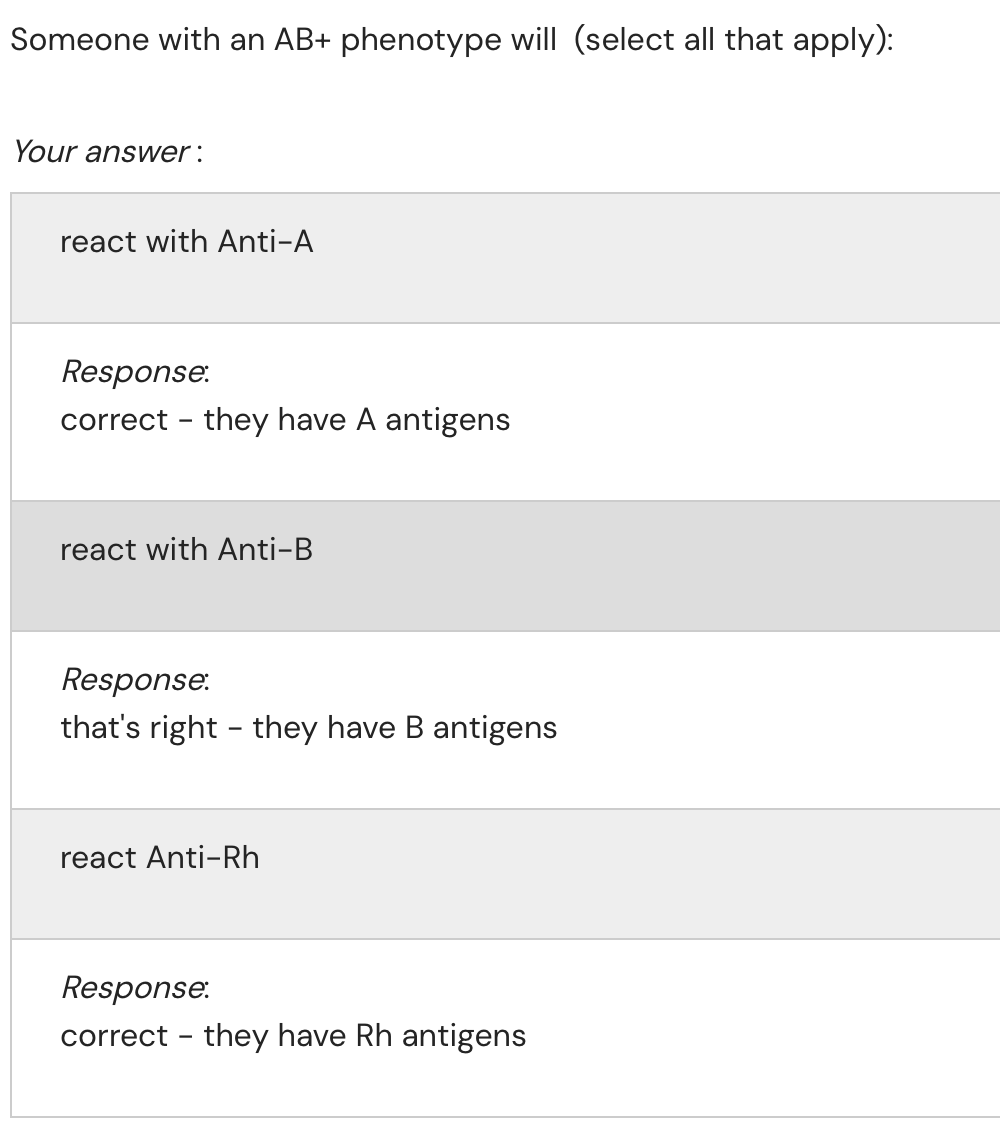
Antigens and Antibodies in Each Blood Type (ABO System)
Type A: Possesses A antigens on RBC membrane and anti-B antibodies in plasma.
Type B: Possesses B antigens on RBC membrane and anti-A antibodies in plasma.
Type AB: Possesses both A and B antigens on RBC membrane and no anti-A or anti-B antibodies in plasma.
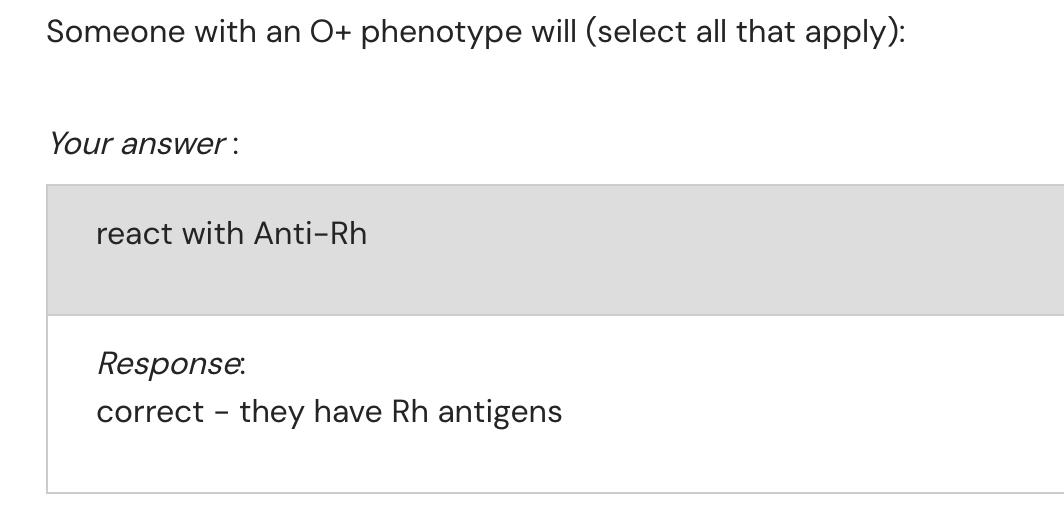
Type O: Possesses no antigens on RBC membrane but has both anti-A and anti-B antibodies in plasma.
The Rh(D) antigen designates blood as positive (+$) or negative ($-), such as O(^{+}$) or O(^{-}$).
Possible Blood Phenotypes Inherited Given Parental Phenotype/Genotype
Blood type inheritance is determined by three alleles: A and B (which are codominant), and O (which is recessive).
Phenotype-Genotype Correspondence:
A: AA or AO
B: BB or BO
AB: AB
O: OO
Example Cross: If Parent 1 has phenotype A (genotype AO) and Parent 2 has phenotype O (genotype OO), a Punnett square cross would show that their offspring could have 50% AO (Type A) and 50% OO (Type O) phenotypes.


Forensic Relevance
Class evidence (cannot individualise, but can exclude).
Quick compatibility check for disputed relationships:
Example table shows which parental combos can/cannot yield an O child.
Bodily-Fluid Test Panels
Fluid | Presumptive Targets | Typical Presumptive Methods | Confirmatory |
|---|---|---|---|
Blood | Haemoglobin | Colour tests (Kastle-Meyer, o-tolidine, Luminol, etc.) | Takayama, Teichmann, ABAcard, precipitin, DNA profiling |
Semen | Acid phosphatase, prostate antigen (p30), ABH antigens | Fast colour tests, ELISA | Microscopy for sperm, DNA extraction |
Saliva | Amylase, ABH antigens | Colour/antibody tests | Commercial kits; DNA on epithelial cells |
Presumptive ≠ definitive; many oxidising agents or metals can mimic blood reactions.

Presumptive tests
How would you select which test to do?
When selecting a presumptive test, you need to balance its sensitivity with the preservation of the sample for downstream DNA analysis. For example, indiscriminate spraying of Luminol may hinder DNA recovery if the stain mass is minimal, indicating a trade-off between revealing latent patterns and preserving the sample's integrity.

Test-Selection Strategy
Balance sensitivity vs preservation for downstream DNA.
Example: indiscriminate Luminol spraying may hinder DNA recovery if stain mass is minimal.
Blood Pattern Analysis (BPA) – Snapshot
Not core serology, but related skillset.
Blood dynamics: drip, ooze, spray, spurt, fling, smear… → unique patterns.
Can infer:
Weapon type & motion.
Injury sequence & locations.
Victim/suspect movement, relocation.
Excluded from current course depth but worth reading.

F
LMS QUESTIONS:
Describe a few presumptive serological tests (at least one per bodily fluid):
Blood: Luminol test – a chemiluminescent reaction that indicates the presence of blood even when it is diluted or washed away.
Saliva: Alpha-amylase test – detects the enzyme alpha-amylase, which is present in saliva and can be used to identify saliva stains.
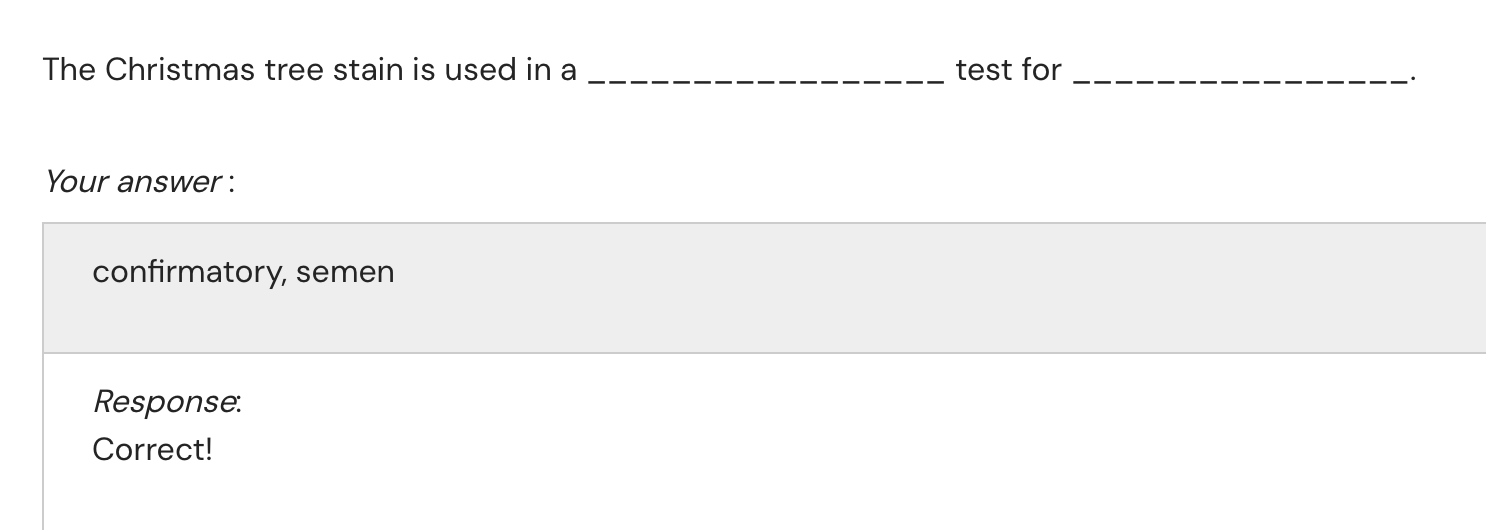
Semen: Acid phosphatase test (AP) Test – identifies the presence of the enzyme acid phosphatase, which is found in high concentrations in seminal fluid.
Describe a few confirmatory tests:
Blood: DNA profiling – utilizes PCR (polymerase chain reaction) to amplify DNA from blood samples for individual identification.
Saliva: Immunological assays – detect specific proteins or antibodies in saliva to confirm its presence and identify its origin.
Semen: Prostate-specific antigen (PSA) test – measures the concentration of PSA, a protein produced by the prostate gland, to confirm the presence of semen.
Describe ABO blood typing and understand how it can be useful in forensic science: ABO blood typing is a method used to classify human blood into four main groups: A, B, AB, and O, based on the presence or absence of specific antigens on the surface of red blood cells. This classification can be particularly useful in forensic science for narrowing down potential suspects in a crime scene by matching blood samples found at the scene with those of the victim or potential suspects. Additionally, ABO typing can aid in paternity cases and provide crucial evidence in legal investigations. Furthermore, the reliability of ABO blood typing increases when combined with other forensic techniques, such as DNA analysis, which can further enhance the accuracy of identifying individuals involved in a case. By understanding the limitations of ABO typing, such as its inability to definitively identify a single individual, forensic experts can utilize this method in conjunction with other markers like Rh factor and genetic profiling to build a more comprehensive picture of the evidence.
•Explain genetic inheritance of ABO blood types: The genetic inheritance of ABO blood types is determined by a single gene located on chromosome 9, which has three primary alleles: A, B, and O. Each individual inherits one allele from each parent, leading to the expression of one of the four possible blood types: A (genotype AA or AO), B (genotype BB or BO), AB (genotype AB), or O (genotype OO). The presence of the A or B allele produces the corresponding antigens on the red blood cells, while the O allele is considered a non-functional variant, resulting in a lack of these antigens. This inheritance pattern follows Mendelian genetics, where the combination of alleles from both parents will dictate the offspring's blood type, thereby providing insight into familial relationships and genetic traits that can be analyzed in forensic contexts.
Case Study: O. J. Simpson Acquittal
At first glance, abundant serological evidence (blood trails, gloves, clothing).
What went wrong?
Mishandling: poor chain-of-custody, contamination, improper storage.
Defence leveraged errors → “reasonable doubt.”
Entire serological dataset (and by extension DNA results) was discounted.
Ethical / practical lesson:
Even strong biochemical assays are only as valuable as the collection & documentation protocols.
Mishandling can nullify otherwise conclusive science, undermining justice.
Ethical, Philosophical & Practical Implications
Chain-of-custody is paramount; errors ripple across all subsequent tests.
Balancing rapid field tests vs preserving evidentiary integrity (e.g. presumptive sprays vs DNA integrity).
Class evidence (blood type) still useful for exclusion, narrowing suspect pool, and triaging expensive DNA tests.
Secretion status (secretor vs non-secretor) adds another discriminant layer.
Always integrate serology with broader forensic toolkit (trace evidence, fingerprints, digital forensics, etc.).
Connections & Further Reading
Immunology basics (antibody-antigen interactions) underpin both precipitin and blood typing.
Enzymology and redox chemistry central to colourimetric presumptive tests.
Molecular genetics (PCR, STR typing) ultimately supersede serology for individualisation but rely on initial serological locating of stains.
Suggested resources:
ABAcard ® user manuals (commercial confirmatory kits).
Science & Justice (2018) 58 : 386-396 – Stewart et al. (Takayama crystal morphology study).
YouTube demonstrations of precipitin & crystal tests (links in slides).
WEEKLY READING
The paper "Analysis of body fluids for forensic purposes: From laboratory testing to non-destructive rapid confirmatory identification at a crime scene" by Virkler and Lednev (2009) provides a comprehensive review of methods used for the detection and identification of body fluids in forensic science. It discusses the progression from traditional laboratory-based techniques, which often require destructive sample collection and extensive processing, to the development of new, non-destructive and rapid confirmatory methods suitable for immediate use at crime scenes.
The authors categorize body fluid analysis into presumptive tests (indicating the possible presence of a fluid) and confirmatory tests (definitively identifying a fluid and sometimes its species origin). The paper highlights the limitations of traditional methods, such as their destructiveness, potential for contamination, and time-consuming nature. It then focuses on emerging spectroscopic techniques, particularly Raman spectroscopy and Fourier transform infrared (FTIR