T cells at Work
T Cells at Work
B Cells vs. T Cells
Cell Type | Recognition Protein | Signaling Proteins | Co-Stimulatory Molecules | CO-Receptor Molecules | Growth factor receptors | Antigen recognized | Function of Cell | Affinity Maturation and continued production |
B cell | BCR (heavy+light) | Igα and Igβ | CD40 (pairs with CD40L on Th cell) | iC3b fragment receptor | Leads to Ab class switching | Any organic molecile | Produce antibody (and memory B cells) | Yes |
T cell | TCR (αβ on traditional T cells) | CD3 (gamma, delta, epsilon, and zeta - 2 proteins | CD28 (pairs with B7 on APC) - upregulated when CD40 on APC binds to CD40L on T cell | CD4 on Th; CD8 on CTL | Helps influince cytokine profile (seen in future lecture) | Peptide in MHC groove | Th = quarterback of the immine system CTL = kilers of infected cells | No |
Effector T cells
Activated T cells are effector T cells, and are ready to go work
Effector CTLs kill infected cells (why they are killer T cells)
Effector Th cells have two main functins
Remain in circulation, traveling among lymph nodes to provide help to B cells and CTLs
Exit the blood at the battle site and provide help for solders of the innate and adaptive immune system
If the immune system is a football team…
Effector Th cells are the quarterbacks
They use cytokines to call the play
DCs are the coaches who collect information on the other team (microbes) and formulate a game plan.
Eg. where the Th cells should go in the body, and what kind of opponent the Th cells need to respond to, to help the CTLs and the B cells to defeat.
How do DCs know the proper instructions to give the Th Cells?
First, what kind of pathogen is invading? PAMPs on invaders, TLRs on and in DCs, will help DCs instruct the Th cells
TLR4: LPS on gram-negative bacteria
TLR2: Gram-positive cell wall “signatures”
TLR3: Double stranded RNA found in many viral infections
TLR9: the unmethylated DNA dinucleotide CpG
Second, where the Th cells needed? (regional identity)
By receiving different cytokine scouting reports, DCs learn the invasion story from local tissue cells (that respond to different pathogens PAMPs) so they can
Th Cell subsets and the immune response
Based on their scouring reports, DCs use different combos of:
a.) Co-stimulatory molecules on their surface (like B7 et al.), and
b.) the profile of the cytokines they secrete
… to stimulate virgin Th0 cells in the lymph nodes to become one of the three main subtypes of the Th cell:
Th Cell Subset | Main cytokines produced by the Th cell (locally at site of infection) | Effect of cytokine packing |
Th1 | TNF activates primed macrophages and natural killer cells IFN-γ activates macrophages, primes B cells to produce IgG3. Th2 antagonist IL-2 - a growth factor for CTLs NK and Th1 cells; recharges NKs GM-CSF - growth and differentiation of granulocytes and monocytes | Fights virus or bacteria attack |
Th2 | IL-3 - Stimulates growth of polymorphonuclear cells IL-4 - a growth factor for Th2, B cells and switch for IgE IL-5 - stimulates B cell switch to IgA IL-10 - B cell proliferation and Th1 antagonist IL-13 - Stimulates mucus production in intestines | Fights parasites or mucosal infections |
Th17 | IL-17 recruits neutrophils IL-21 - a growth factor for Th17 cells IL-23 - stimulates submucisal B cells to produce IgG3 and IgA | Fights fungi and extracellular bacteria |
How DCs influence the induction of Th1 subsets
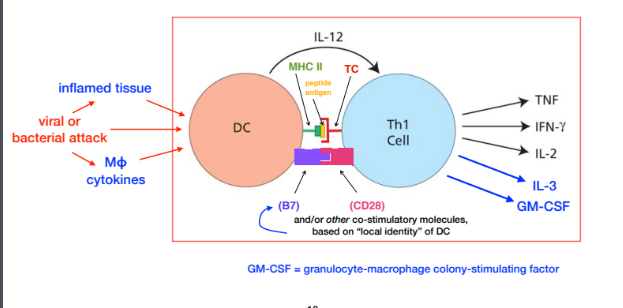
MHC II presents to Th1 cell, and B7 links to Th1 CD28 receptor
TH1 cell receives IL-12 signal from DC, and produces the listed cytokines and factors
How DCs influence the induction of Th2 subsets
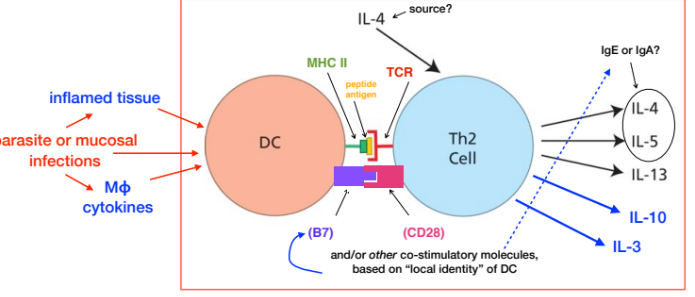
How DCs influence the induction of Th17 subsets
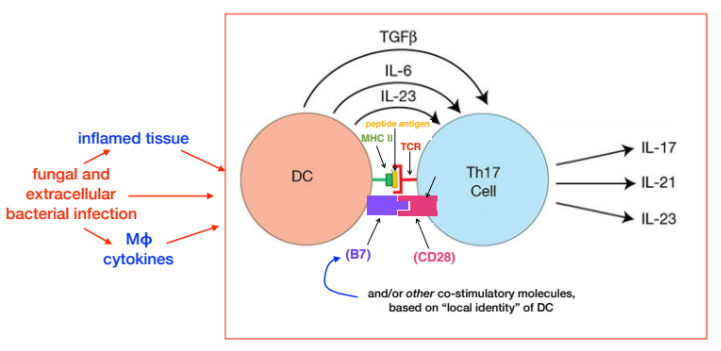
The Th0 subset
Some cells remain unbiased when first activated in the lymph node
Commit to a particular cytokine profile after arriving to battle scene when influenced by local cytokines
Ex. If bacteria are involved:
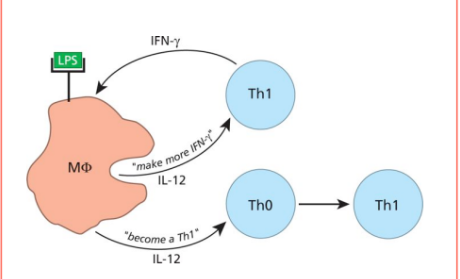
Not always IL-12
Parasitic infection (IL-14) signals Th0 to become Th2
Fingal infection (IL-6 and TGFβ) signals Th0 to become Th17
At the site of the interaction
Committing to a Th Cytokine profile
After committing to a cytokine profile, Th cells reinforce the presence of that profile and suppress the presence of other profiles:
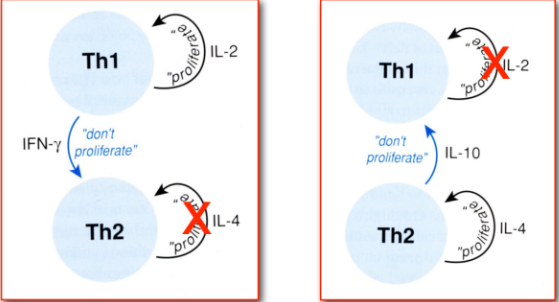
Positive and negative feedback reinforce a particular Th cell cytokine profile
Cytokines only work at a short distance, effects are local
Activated Th cells become effectors - the case of delayed-type hypersensitivity (DTH)
A specific example of Th cells “signal calling”
The tuberculin skin test:
Tuberculin protein (PPD) is injected subcutaneously
Dendritic cells process PPD and present its peptides in MHC II and also provide a B7 co-stimulatory signal to experienced Th1 cells - if you have, or had, TB or BCG vaccine
These experienced Th1 cells secrete TNF and INF-γ
It takes two days (average_ for the Th1 cells to react and proliferate, but then macrophages and neutrophils are recruited to the injection site yielding a raised, red bump
Why is there no stimulation of naive Th cells to induce a positive reaction next time, in someone who’s skin test is negative?
No inflammation with tuberculin peptide = no DC activation
CTL activation and function - how activated CTLs kill (and NK cells)
Once activated, CTLS proliferate and leave the lymph node
Leave the bloodstream at the site of battle and come into physical contact with cells that have foreign peptide displayed in MHCI
Either perforin or FasL (bound Fas on the target cell) trigger apoptosis of the affected cell
Apoptosis is a tidier death than necrosis
Also destroys viral DNA at the same time as it degrades cellular DNA
How CTLs kill thier targets by two mechanisms
FasL on the effector CTL binds to Fas protein on surface of target cell (green)
Caspase-8 is activated and triggers a cascade that leads to apoptosis
Perforin and Granenzyme B are exocytosed from the CTL and endocytosed into the target cell (Purple)
Perforin allows granenzyme B to enter the cytoplasm of target cell and activate a cascade that leads to apoptosis
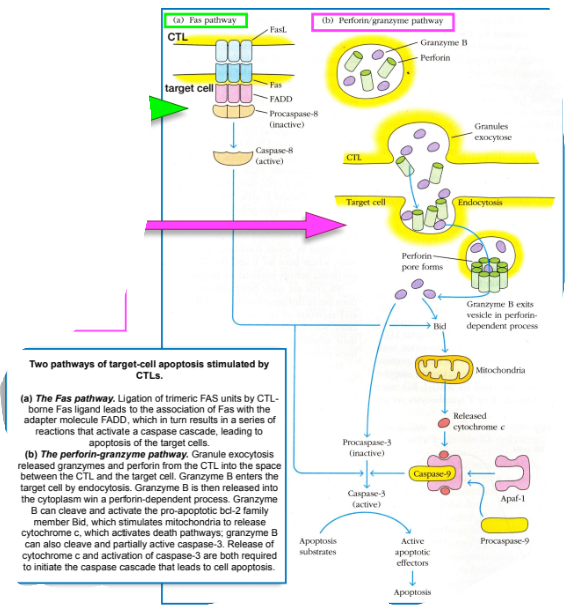
Remember - the effector CTL must use its TCR to recognize its cognate peptide within MHC1 before killing takes place