Exam 2 (1)Erythrocytes
Describe the composition of whole blood:
Plasma:
Proteins (7%) = albumins: help make more soluble (57%); globulins (38%); fibrinogen: important in clotting/hemostasis (4%); prothrombin (1%)
Water (91%)
Other solutes (2%): ions, nutrients, waste products, gases, regulatory substances
Formed Elements:
Platelets: hemostasis (140,000-340,000)
Leukocytes: (5,000-9,000) = neutrophils (60-70%); lymphocytes (20-25%); monocytes (3-8%); eosinophils (3-4%); basophils (0.5-1%)
Erythrocytes (4.2-6.2 million)
Describe the chemical composition of hemoglobin:
Hemoglobin structure, function:
Adult hemoglobin (HbA) is composed of two α globin chains and two B globin chains (α2B2)
Each globin chain is bound to a heme group
Iron in the heme group binds O2 reversibly in a concentration-dependent manner (high O2=bind; low O2=release)
oxyhemoglobin is bright red, while deoxyhemoglobin is dark red
Fetal hemoglobin (HbF) has two y globin chains instead of B globin chains (α2y2)
HbF has higher affinity for O2 than HbA allowing the fetus to acquire O2 from the mother
It is replaced within 6 months of birth by HbA
Describe the structure and function of erythrocytes:
Erythrocyte structure/functions:
specialized to transport O2
97% hemoglobin (dry-weight)
Anaerobic and lack of nuclei and organelles (don’t consume the oxygen they are carrying)
Biconcave shape provides higher surface volume ratio which aids gas exchange
Shape is maintained by spectrin bound indirectly to transmembrane proteins
Flexible: larger than smallest capillaries (bend and flex to go through)
Explain process and regulation of erythropoiesis
Erythrocyte productions:
Erythropoiesis is red blood cell formation and occurs in the red bone marrow
All blood cells arise from hematopoietic stem cells (hemocytoblasts) located in the red bone marrow (most bones - long bones - have yellow bone marrow - fat cells - in adults, red bone marrow is found in irregular shaped bones)
Must balance number of erythrocytes to:
Maintain adequate O2 delivery
Prevent excessive blood viscosity
# = rate of production - rate of destruction
Average production is 2 × 10^6 / second
Erythropoiesis:
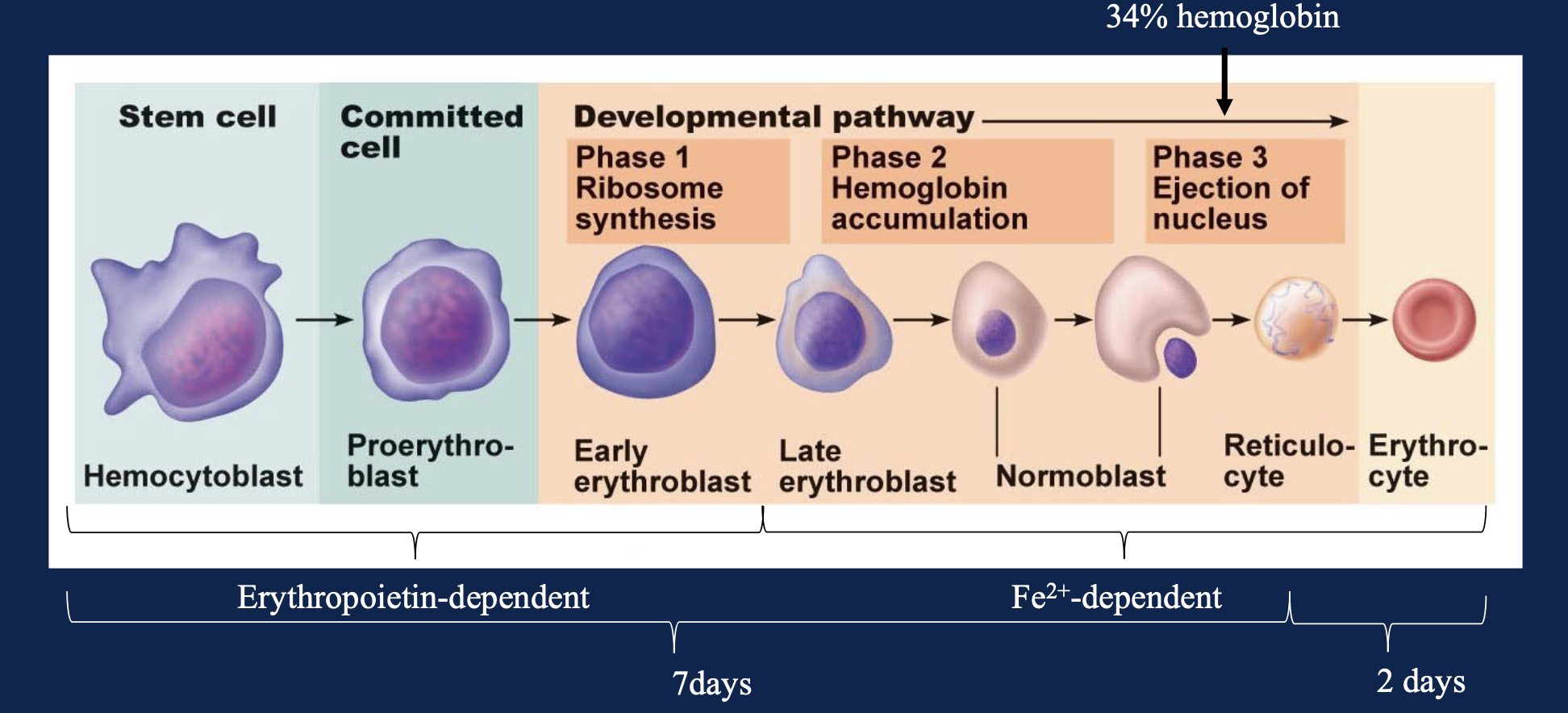
Reticulocytes enter the bloodstream and mature into erythrocytes within two days
Reticulocytes account for ~2% of the total RBC population
Erythropoietin: The rate of erythropoiesis is regulated by the level of erythropoietin (EPO) and the availability of iron
The level of EPO increases in response to hypoxia (decreased O2 delivery to tissue)
EPO is produced by fibroblasts in the kidney cortex > testosterone enhances EPO production by kidneys
Response to Ischemia/Hypoxia:
Hypoxia leads to an increase in the level of transcription factors called hypoxia inducible factors (HIF)
HIF increases transcription of many genes in different cell types to promote metabolism, angiogenesis, and cell survival during hypoxia = hypoxia transcriptional program
Fibroblasts in the kidney cortex respond to hypoxia by increasing the level of HIF which then increases transcription of erythropoietin
HIF is rapidly degraded during normoxia
The enzyme prolyl hydroxylase adds hydroxyl groups to two proline residues
This reaction requires sufficient levels of oxygen
Hydroxylated prolines are recognition sites for ubiquitin ligase leading to rapid proteasonal degradation of HIF
During Hypoxia, prolyl hydroxylase activity is decreased, and HIF is not rapidly degraded
Hypoxia Response Element
HIF binds to the promoter of the EPO gene and increases (erythrocyte production) its transcription
Contains a hypoxia response element
Causes of Hypoxia
Decreased O2 availability
high altitude
lung disease
Increased O2 demand by body
heavy exercise
Decreased O2 carrying capacity
anemia (diminished ability to carry O2 in blood)
Describe the turnover of erythrocytes, the metabolism and excretion of heme, and the scavenging of iron.
Turnover of Erythrocytes:
the normal elimination of erythrocytes occurs via the RES (reticuloendothelial system) composed of sinusoidal capillaries (big gaps and openings) located primarily in the spleen
like all cells, erythrocytes become damaged over time and lose flexibility
Because they have no nuclei or organelles, they cannot repair the damage
Erythrocytes that have lost flexibility become trapped in the sinusoidal capillaries
average lifespan is 120 days
Trapped cells are phagocytosed by tissue-resident macrophages located outside the capillaries
smaller amounts of erythrocytes turnover may also take place in the liver, bone marrow, and lymph nodes
Extravascular Hemolysis: (in stroma of spleen)
tissue-resident macrophages phagocytose the trapped erythrocytes
Globin chains are degraded by proteases
iron is removed from heme and transferred to carrier protein transferrin in the blood
heme groups salvaged and oxidized to bilirubin by cellular enzymes
Excretion of Bilirubin:
it is transported through the blood to the liver bound to a carrier protein called heptoglobin
bilirubin has very poor solubility in the plasma
In the liver the bilirubin is conjugated (linked) to a molecule of glucuronide to make it more soluble and less toxic
the conjugated bilirubin is added to the bile (made in liver) which is secreted into the intestines and excreted with feces
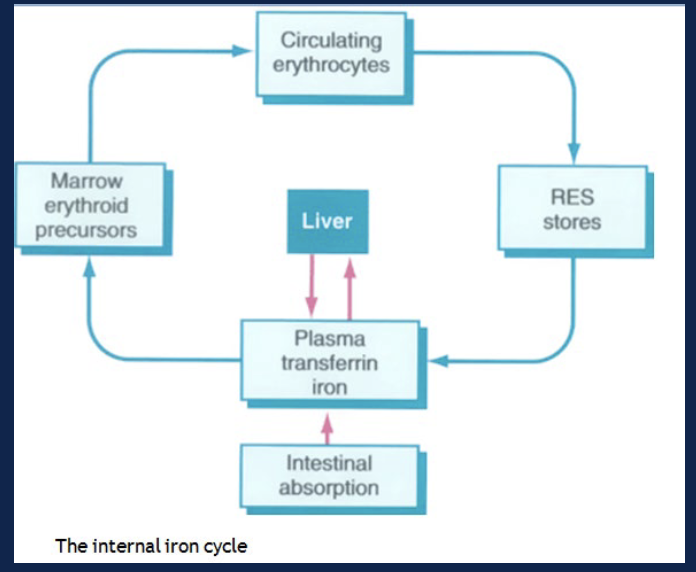
Scavenging and Recycling of Iron
iron can be released into the circulation and returned to the bone marrow for incorporation into new RBC or to the liver
iron binds to the carrier protein transferrin which ferries to other tissues
in the red bone marrow, iron can be removed from transferrin and used to synthesize new hemoglobin in erythropoiesis
in other cells, especially the liver, transferrin is endocytosed, the iron is removed, and it then binds to the cytosolic protein ferritin
> really important part of erythrocyte turnover