CN VII and VIII
Learning Objectives
Describe the anatomical pathways of CN VII and CN VIII
Describe the nerve components of CN VII and CN VIII
Describe the functions associated with each of these nerves
Describe select clinical correlations associated with each nerve
CN VII and CN VIII Pathway (commonality)
Emerge from the brainstem between the pons and medulla
Internal auditory meatus → Petrous portion of temporal
CN VII usually found superficial to CN VIII
Paths diverge from here
CN VIII Vestibulococlear - Hearing and Balance (Special Sensory)
CN VIII Pathway (continuted)
Cochlear and vestibular
Conveys SSA info on sound and equilibrium
Divisions of the Ear
External, middle, inner ear
CN VII innervates inner ear
CN VII innervates external and middle ear
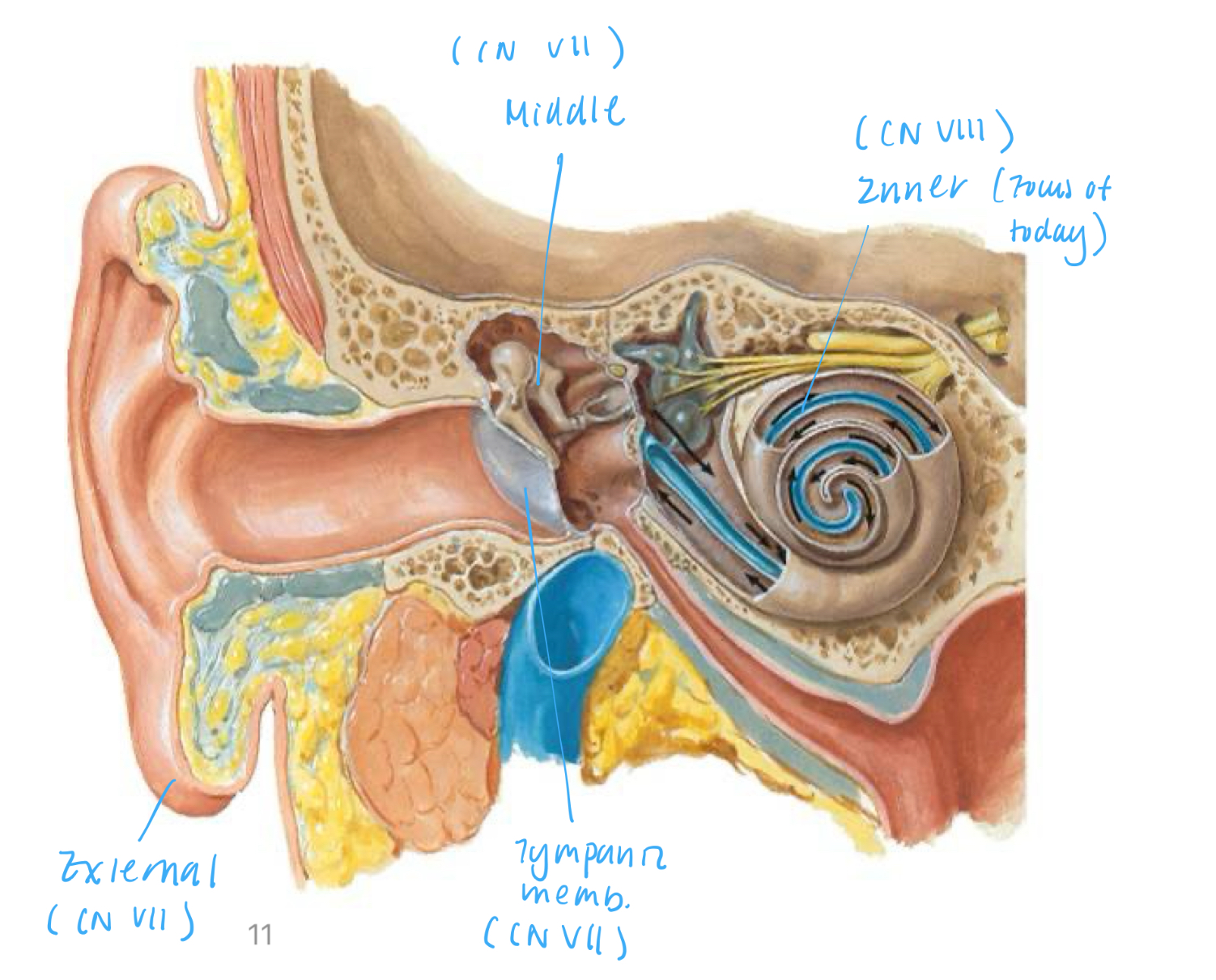
Ear Structure: Inner Ear
Composed of semicircular canals, vestibule, and cochlea
Innervation by vestibulocochlear n.
Has distinct vestibular and cochlear portions
Vestibular portion → Semicircular canals and vestibule
Cochlear portion → Cochlea
Semicircular canals oriented in 3 orthogonal planes
Horizontal canal: turning head left and right
Superior canal: nodding hear
Posterior canal: touching head to shoulder
If damaged → Vertigo
Structure - Tube within a tube
Components from outside → inside
Bony/osseous labyrinth - bone
Perilymph - fluid
Membranous labyrinth
Sensory epithelium - lining
Endolymph - fluid
Cochlea compartments
Scala vestibuli (vestibular duct) - contains perilymph
Tympanic duct (scala tympani) - contains perilymph
Cochlear duct (scala media) - contains endolymph
Organ of Corti sits on top of the basilar membrane in the cochlear duct
Transmits fluid displacement to the brain via hair cells
Path of sound
Sound stimulate stapes to tap the oval window → Pressure waves travel through cochlea → As it passes, displaces basilar membrane and stimulates cochlear portion of n. → Remaining pressure waves shake into the middle ear cavity via the round window (dissipate pressure)
Place theory: Stimulation of hair cells in different parts of the basilar membrane results in differences in sound frequencies
High frequencies: close to middle ear
Low frequencies: close to cochlear apex
Sound processing
Anterior cochlear nucleus: Process low frequency sounds
Posterior cochlear nucleus: Process high frequency and loud sounds
Clinical considerations: Presbycusis
Presbycusis: Very gradual loss of hearing sensitivity related to aging beginning in young adults
Begins with frequencies over 15-16,000
Affects high frequencies more and greater in men
Loss of sensitivity to high frequencies → hard to distinguish between certain consonants especially in noisy environments
Use hearing aids to amplify low frequencies
Clinical considerations: Cochlear implants
Implant takes place of hairs on basilar membrane and directly stimulate cochlear n.
Typically implanted inn younger individuals - speech development
CN VII Facial - SS, SM Para/Pre, Taste
Nerve Components
SS: Skin of the concha of ear and posterior to ear
SM: Muscles of facial expression, stapedius, posterior belly of digastric, and stylohyoid
Para/Pre: For lacrimal (tears), submandibular (salivary), sublingual (salivary), + mucous membranes of nasopharynx and the hard and soft palate
Special sensory: Taste to anterior 2/3 of tongue and hard and soft palate
CN VII Pathway (continued)
Once enters internal auditory meatus → Travels anteriorly within petrous portion of temporal bone → Right angle laterally at geniculate ganglion → exits stylomastoid foramen
Geniculate ganglion: Collection of sensory neurons
Branches of CN VII before exiting stylomastoid foramen: Greater (and lesser) petrosal n., n. to stapedius, chorda tympani
CN VII Somatomotor
SM to muscles of facial expression, stapedius, posterior belly of digastric, and stylohyoid
Branches of CN VII (once exited stylomastoid foramen) - Superior → Inferior + posterior
Temporal: Innervate frontalis + orbicularis oculi (superior portion)
Zygomatic: Innervate orbicularis oculi (inferior portion)
Buccal: Innervate buccinator; orbicularis oris
Marginal mandibular
Cervical: Innervate platysma
Posterior auricular: SS behind ear
Clinical considerations: facial nerve paralysis
Mild weakness to total paralysis → cause significant facial distortion or total loss of muscle tone on affected side
Upper motor neuron lesions (UMNL) vs. Lower motor neuron lesions (LMNL)
UMNL: Forehead will be spared
Caused by stroke, subdural hemorrhage
LMNL: Entire face affected (lesion after exit stylomastoid foramen)
Caused by Bell palsy, Ramsay Hunt syndrome
Forehead vs. Lower face innervation
Forehead innervation: innervated by facial nucleus in the pons from L and R motor cortex
Therefore, UMNL has an unaffected forehead because forehead still connected to one side of motor cortex
Lower face innervation: innervated from lower part of facial nucleus in the pons ONLY contralateral side of motor cortex
Clinical considerations: Bell’s Palsy (LMNL)
Symptoms
Facial asymmetry
Drooping of eyelid; inability to close eye; cornea drying (orbicularis oculi - no SM)
Drooling of mouth and drooling (orbicularis oris - no SM)
Accumulation of food between cheek and teeth when chewing (buccinator - no SM)
Causes
Irritated facial nerve → swollen due to inflammation
Viral infection (BSV1; Lyme disease; Extreme cold)
Peripheral n. problem after stylomastoid foramen
Treatment: minimal; eye-patch → usually spontaneously recover after several days
CN VII Somatosensory
SS to skin of the concha of ear and posterior to the ear
Posterior auricular branch of CN VII innervates occipitalis and most auricular muscles
Most posterior branch of facial runs on top of the mastoid process
Part of tympanic membrane receies SS from CN VII
N. that innervate the tympanic membrane: CN V3, VII, IX, and X
CN VII Para/Pre
Para/pre to lacrimal (tears), submandibular (saliva), and sublingual glands (saliva) + mucous membranes of nasopharynx and hard and soft palate
Greater (and lesser) petrosal n.
First branch off geniculate ganglion → Hiatus for the greater petrosal n. → Travel under CN V ganglion → Cross into foramen lacerum → Pterygopalatine ganglion (in fossa)
Path of para/pre from CN VII that travel on the greater petrosal n.
Para/pre from CN VII travel on greater petrosal n. → Joins with deep petrosal (from the tympanic plexus) → Forms the nerve of the pterygoid canal → Synapse at the pterygopalatine ganglion → Exit to V2
Parasympathetic innervation of lacrimal gland (increase tear production)
Superior salvatory nucleus (in the brain) → Facial n. → Greater petrosal n. → N. of the pterygoid canal VII synapse at pterygopalatine ganglion → Zygomatic branch of V2 → Lacrimal n. of V1 → Lacrimal gland (increase tear production)
Sympathetic innervation of lacrimal gland (decrease tear production)
Lateral horn T1-4 → Ventral root → Spinal n. → Ventral ramus → White communicating ramus → Sympathetic trunk (ascend) → Synapse at superior cervical chain ganglion → ICA plexus → Deep petrosal n. → N. to pterygoid canal → Pass through pterygoid ganglion → CN V2 → Lacrimal n.
Parasympathetic innervation of the nasal mucosa, hard/soft palate (increase mucous secretion)
Superior salivatory nucleus → Facial n. → Greater petrosal n → N. of the pterygoid canal → Synapse at pterygopalatine ganglion → Greater and lesser palatine n. → Nasal & palatine mucosal glands
Sympathetic innervation of the nasal mucosa, hard/soft palate (decrease mucous secretion)
Lateral horn T1-4 → Ventral root → Spinal n. → Ventral ramus → White communicating ramus → Sympathetic trunk (ascend) → Synapse at superior cervical chain ganglion → ICA plexus → Maxillary a.
To nasal cavity: Nasopalatine/sphenopalatine a.
To palate: Descending palatine a.
Can also get to destinations via ICA plexus → Deep petrosal n. → N. of pterygoid canal → Pass through pterygoid ganglion → Nasal and palatine mucosal glands
Parasympathetics to submandibular and sublingual glands (increase saliva secretion)
Superior salivatory nucleus → Facial n. → Chorda tympani → Lingual n. → Synapse at submandibular ganglion → Submandibular gland OR lingual nerve, sublingual gland
Sympathetics to submandibular and sublingual glands (decrease saliva secretion)
Lateral horn T1-4 → Ventral root → Spinal n. → Ventral ramus → White communicating ramus → Sympathetic trunk (ascend) → Synapse at superior cervical chain ganglion → ECA plexus → Facial or lingual artery plexus → Submandibular/sublingual gland
Facial a. plexus → superior side
Lingual a. plexus → inferior side
CN VII Special sensory
Taste to anterior 2.3 of tongue and hard and soft palate
Chorda tympani → Petrotympanic fissure → Hitchhike on lingual n.