Lecture 18: Immune Disorders
Hypersensitivities
Hypersensitivities: immune system overreacts to a something harmless
example: allergies
Type I Hypersensitivity
allergens: harmless antigen that trigger an inflammatory response
Type I Hypersensitivity: Triggered by allergens, mediated by IgE (Immunoglobulin E).
may be localized
example: an exaggerated reaction to pollen (hay fever) or peanuts
may be systematic
example: anaphylaxis effects on a systemic level, inflammation throughout the body, causing blood vessels to get leaky as once, and reducing blood pressure quickly
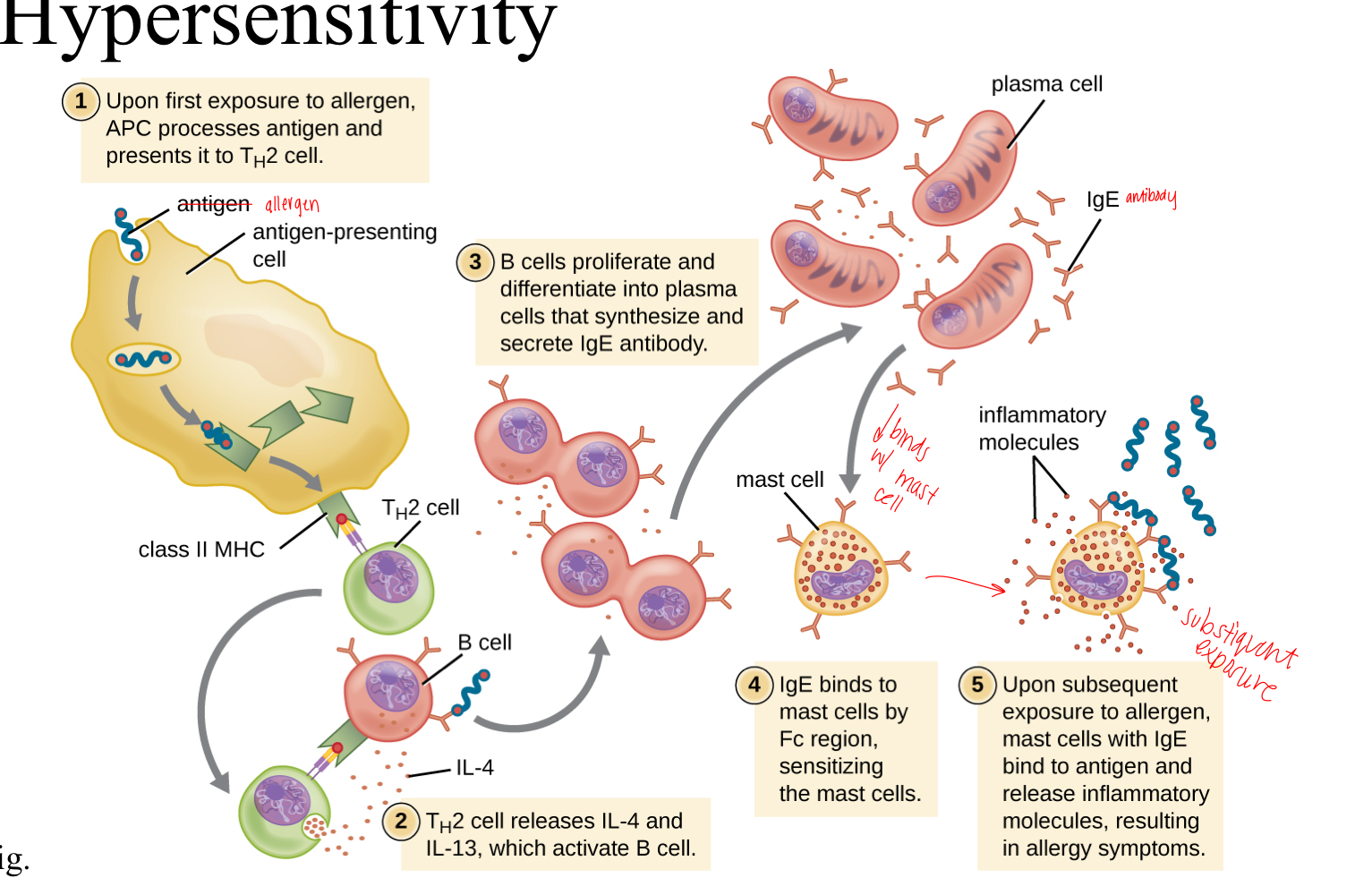
Mechanism of Type 1 Hypersensitivity
Initial exposure to an allergen causes the immune system to produce IgE antibodies.
IgE antibodies bind to mast cells, which contain histamine, but do not trigger histamine release yet.
at secondary exposure to antigen, histamine is released from mast cells
histamine = pro-inflammatory
results in exaggerated response
Sensitization Phase:
Upon initial exposure, Antigen presenting cells (APCs) takes in allergen (harmless, foreign molecule) by mistake, thinking it is dangerous when it is actually harmless
APC presents antigen to CD4 T cell and sends an activation signal to CD4 T cell, turning it in to helper T cell
Helper T cells activate B cells.
B cells transform into plasma cells that produce IgE antibodies.
IgE is inserted on surface of mast cells (which sensitizes them to future exposures to the allergen)
Subsequent Exposure:
Upon re-exposure to the allergen, allergen binds to the IgE on mast cells,
leading to histamine release
causes allergy symptoms
Type II Hypersensitivity (Cytotoxic Reactions)
Type II Hypersensitivity: cytotoxic hypersensitivity, where the immune system attack foreign cells that are harmless.
cytotoxic: attacks antigens present on cells
antibody mediated - involves IgG or IgM
IgG or IgM antibodies bind to antigens on foreign cells, promoting their lysis and inflammation.
Example of Type II Hypersensitivity: Blood Transfusions
during Blood transfusions, mismatched blood types cause the recipient's immune response to attack foreign red blood cells.
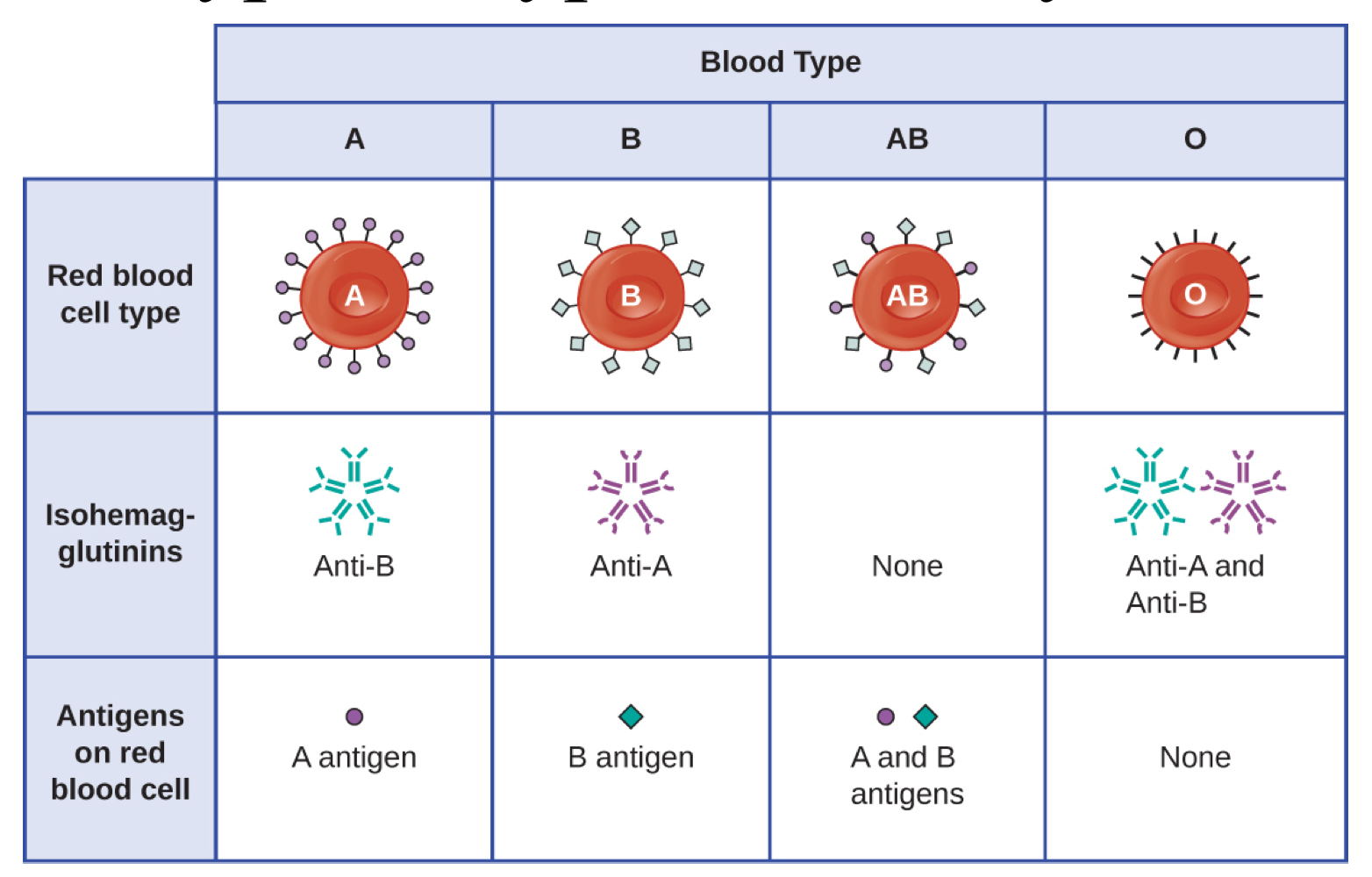
different blood types have red blood cells with different antigens:
If a mismatched blood type is transfused, the recipient’s immune system produces IgG or IgM antibodies against the foreign antigens.
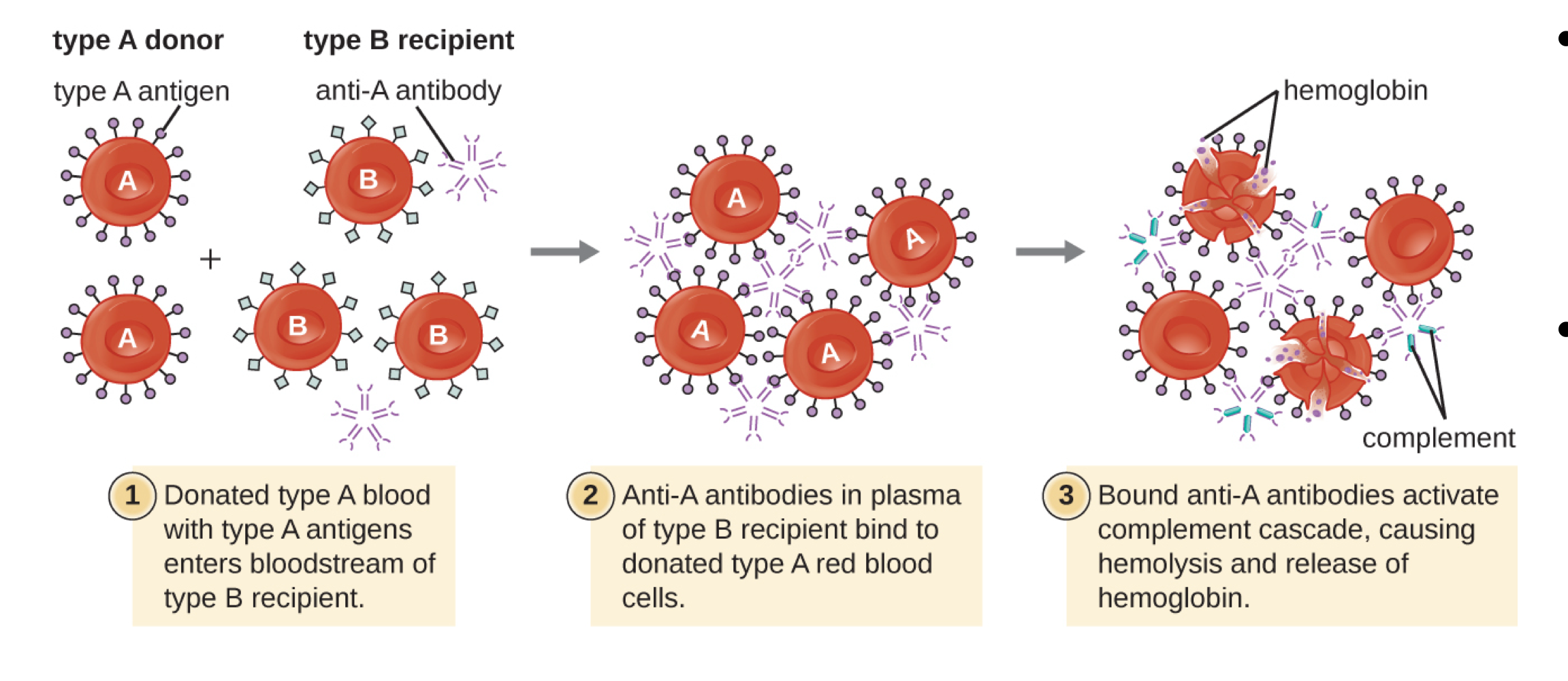
example:
donated type A blood with type A antigen enters bloodstream of type B recipient
IgG or IgM antibodies in plasma of type B recipient binds to donated type A red blood cells
IgG or IgM antibodies activate complement cascade (opsonization, inflammation, and lysis), promoting lysis of cells and inflammation
can lead:
to hemolysis (red blood cells get lysed) and release hemoglobin
antibodies clumped together can cause blockages in bloodstream
inflammation is triggered, shock can occur, reducing blood pressure
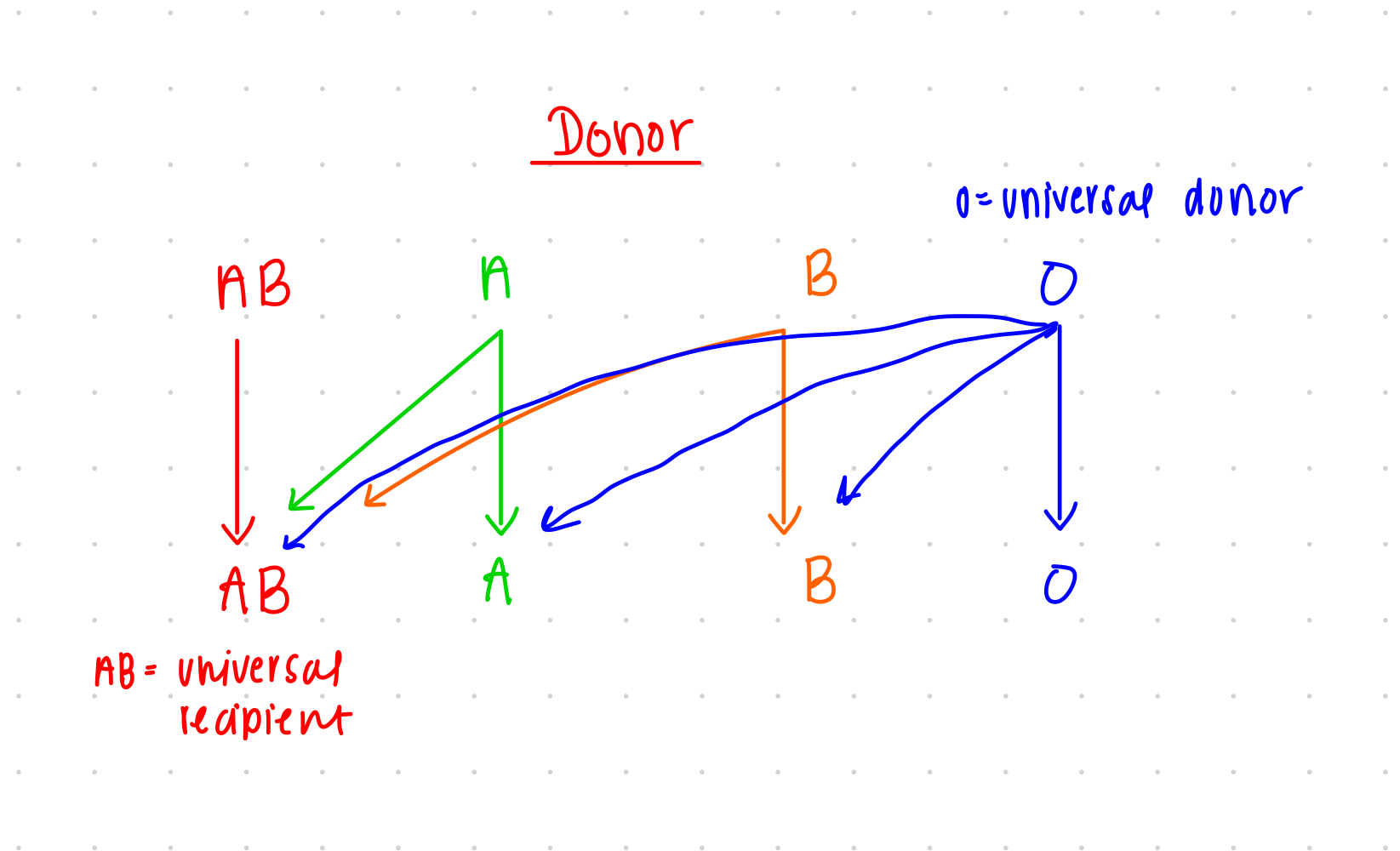
Blood Donation Rules
person with AB blood type can only donate to others with AB
if person with AB blood type attempts to donate to someone with A blood type, body will make antibodies against the B blood type because it perceives the B antigen as foreign
if person with AB blood type attempts to donate to someone with B blood type, body will make antibodies against the A blood type because it perceives the A antigen as foreign
AB blood type can accept blood from anyone because it contains both A and B antigens and therefore does not produce antibodies against either type.
AB blood type: universal recipient
person with A blood type can only donate to others with A OR AB blood type
person with B blood type can only donate to others with B OR AB blood type
person with O blood type can donate to ALL blood types
O blood type cannot accept from any other blood types other than its own because body will raise antibodies to both A and B blood types
O blood type: universal donor
Example of Type II Hypersensitivity: Hemolytic disease of Newborn
Rh Positive and Rh Negative Rules
Rh Factor: Describes the presence (+) or absence (-) of Rh antigens on red blood cells, in addition to blood type antigen
if A positive, means have A antigen and Rh molecule on red blood cells
if A negative, means have A antigen, but do NOT have Rh molecule on red blood cells
Rh positive individuals can donate to ONLY Rh positive
Rh negative individuals can donate to both Rh negative AND Rh positive
O negative blood type: True universal donor but also the most restricted
can donate to everyone
can only receive blood from others who are also O negative
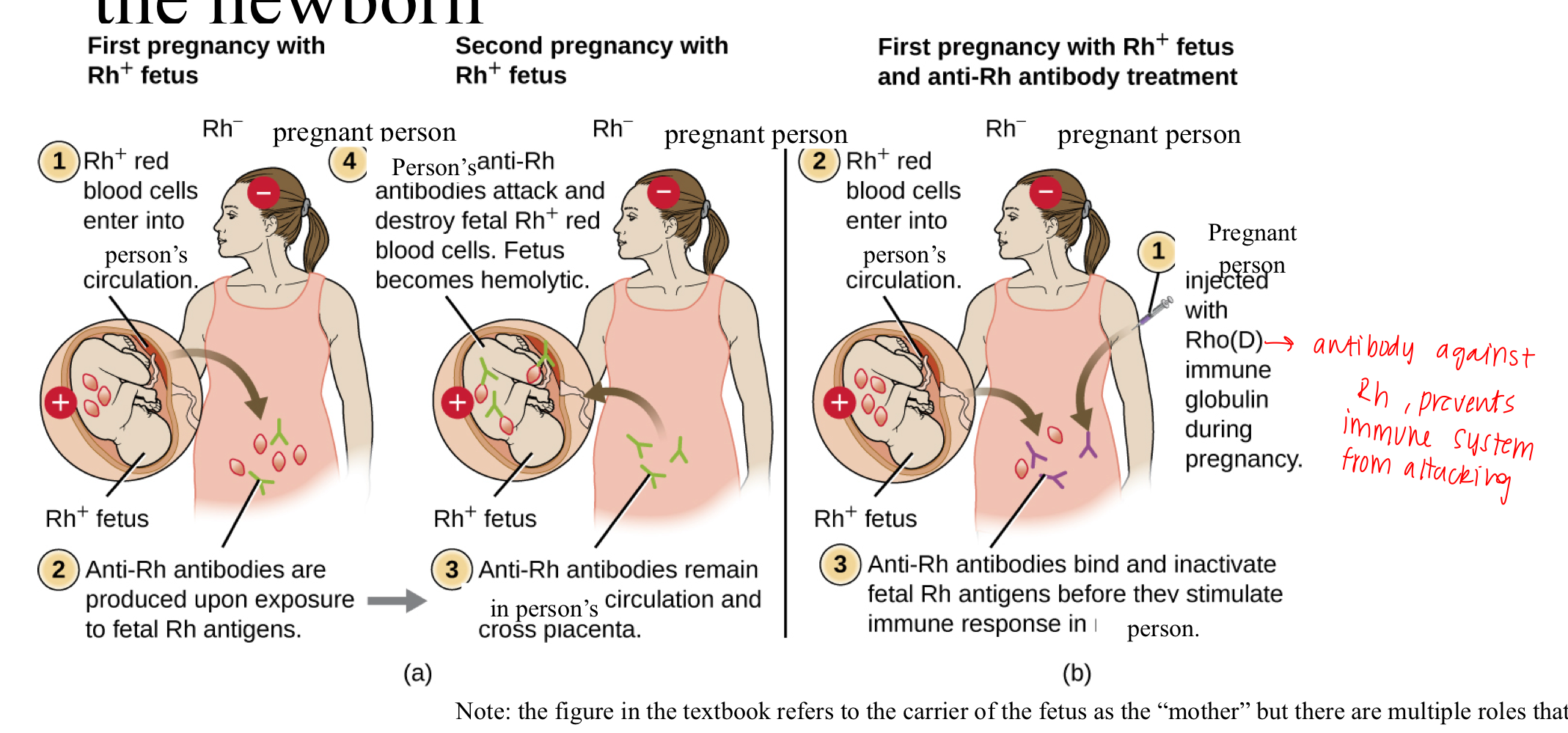
Hemolytic disease of Newborn
If an Rh-negative mother carries an Rh-positive fetus, she can develop antibodies against the Rh factor, affecting future pregnancies.
Treatment: Rh immunoglobulin injections in Rh-negative mothers prevent the formation of anti-Rh antibodies during pregnancy
Example:
During first pregnancy with Rh+ fetus:
Rh+ red blood cells from fetus enter into mother’s bloodstream
anti-Rh antibodies are produced in mother, upon exposure to fetal antigens
During second pregnancy with Rh+ fetus:
anti-Rh antibodies remain in mother bloodstream and cross placenta
Mothers anti-Rh antibodies attack and destroy fetal Rh+ red blood cells
results in fetus becoming hemolytic
Treatment: During first pregnancy with Rh+ fetus and anti-Rh antibody treatment:
Mother is injected with Anti-Rh antibodies during pregnancy
Rh+ red blood cells from fetus enters mothers bloodstream
Anti-Rh antibodies bind and inactivate fetal Rh antigens before they stimulate immune response in fetus
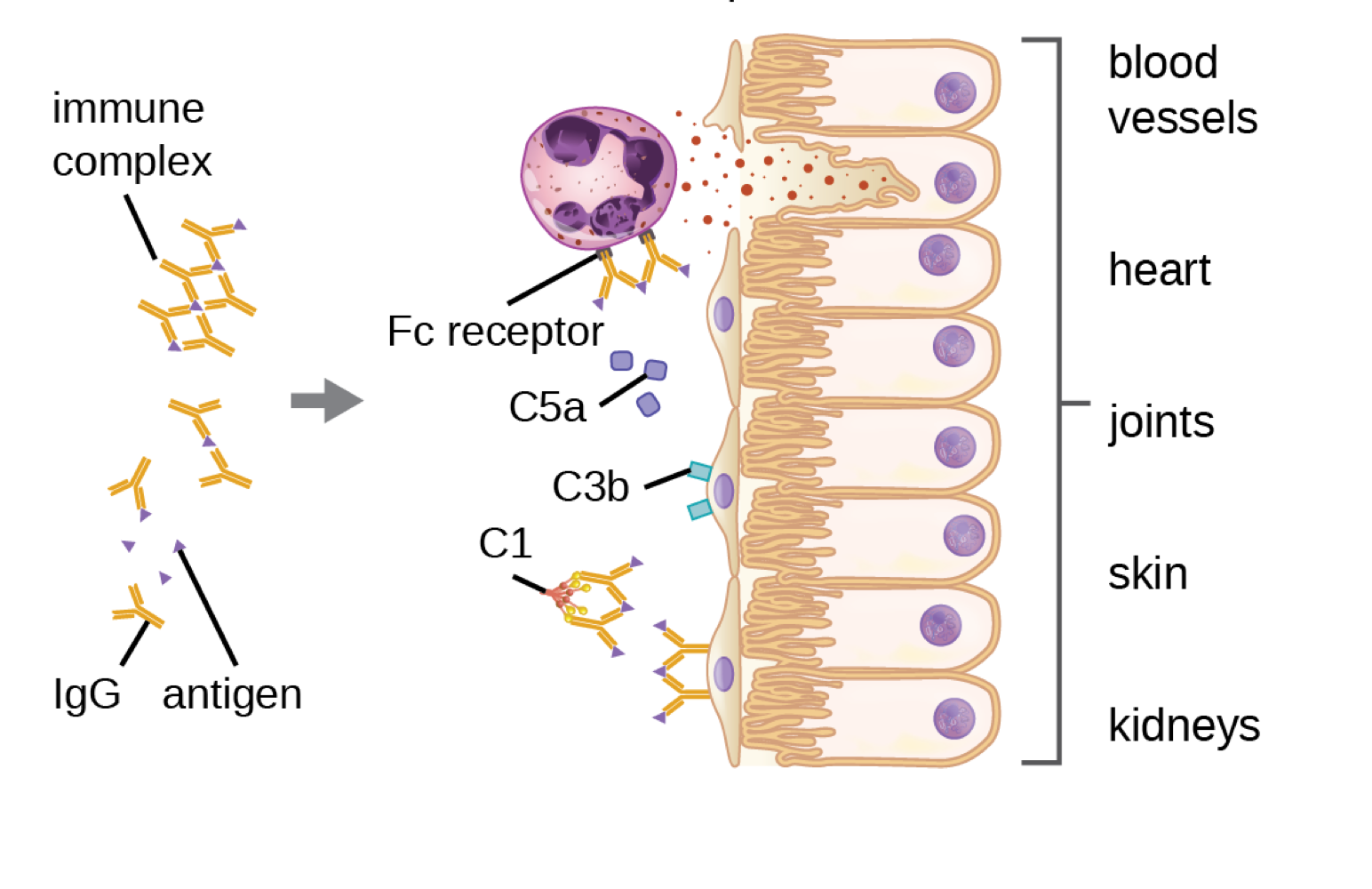
Type 3 Hypersensitivity (Immune Complex-Mediated)
Type III Hypersensitivity: Characterized by the formation of immune complexes
antibody mediated - IgG antibody
immune complexes: more antibodies than antigens
Excessive IgG antibody concentrations can lead to cluster of antibodies accumulating around same antigen
forms immune complex that:
deposit in tissues and prevents phagocytosis
obstruct small blood vessels, leading to tissue damage.
activate complement response (opsonization, inflammation, and lysis)
Opsonization: complement proteins stick to pathogens and make them more recognizable to white blood cells to be engulfed. (phagocytosis)
Inflammation: complement proteins make factors to signal and alert for white blood cells by causing inflammation
Lysis: complement proteins form holes in microbial cells to make cells leak and burst
trigger inflammation
Type 3 Hypersensitivity: Glomerulonephritis
Glomerulonephritis: inflammation of glomerulus
can be caused by accumulation of immune complexes stuck in glomerulus
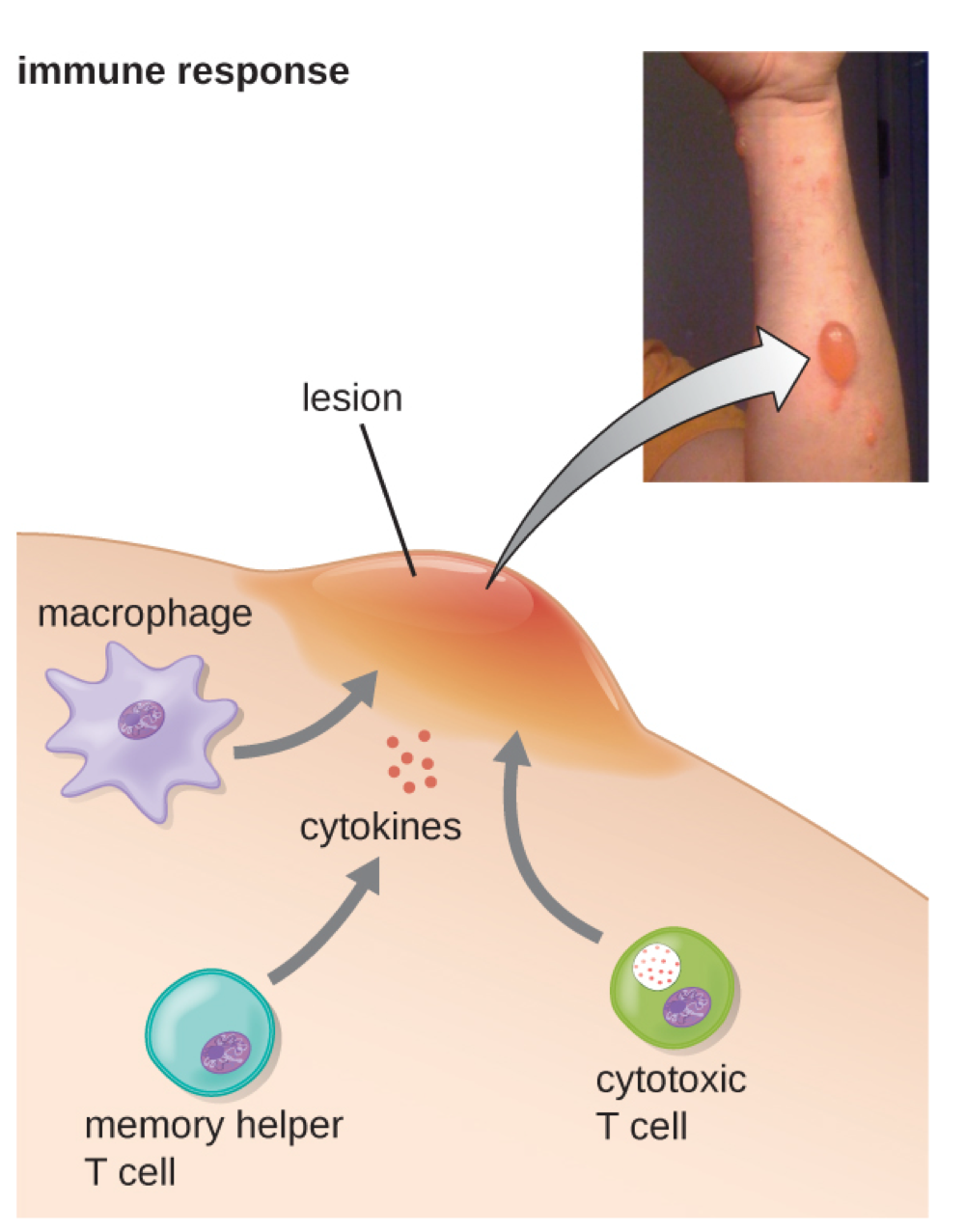
Type IV Hypersensitivity (Delayed-Type)
Type IV hypersensitivity: delayed response, T cells inappropriately attack self cells that are displaying harmless hapten on MHC I
mediated by T cells (rather than antibodies)
Mechanism of Type IV Hypersensitivity:
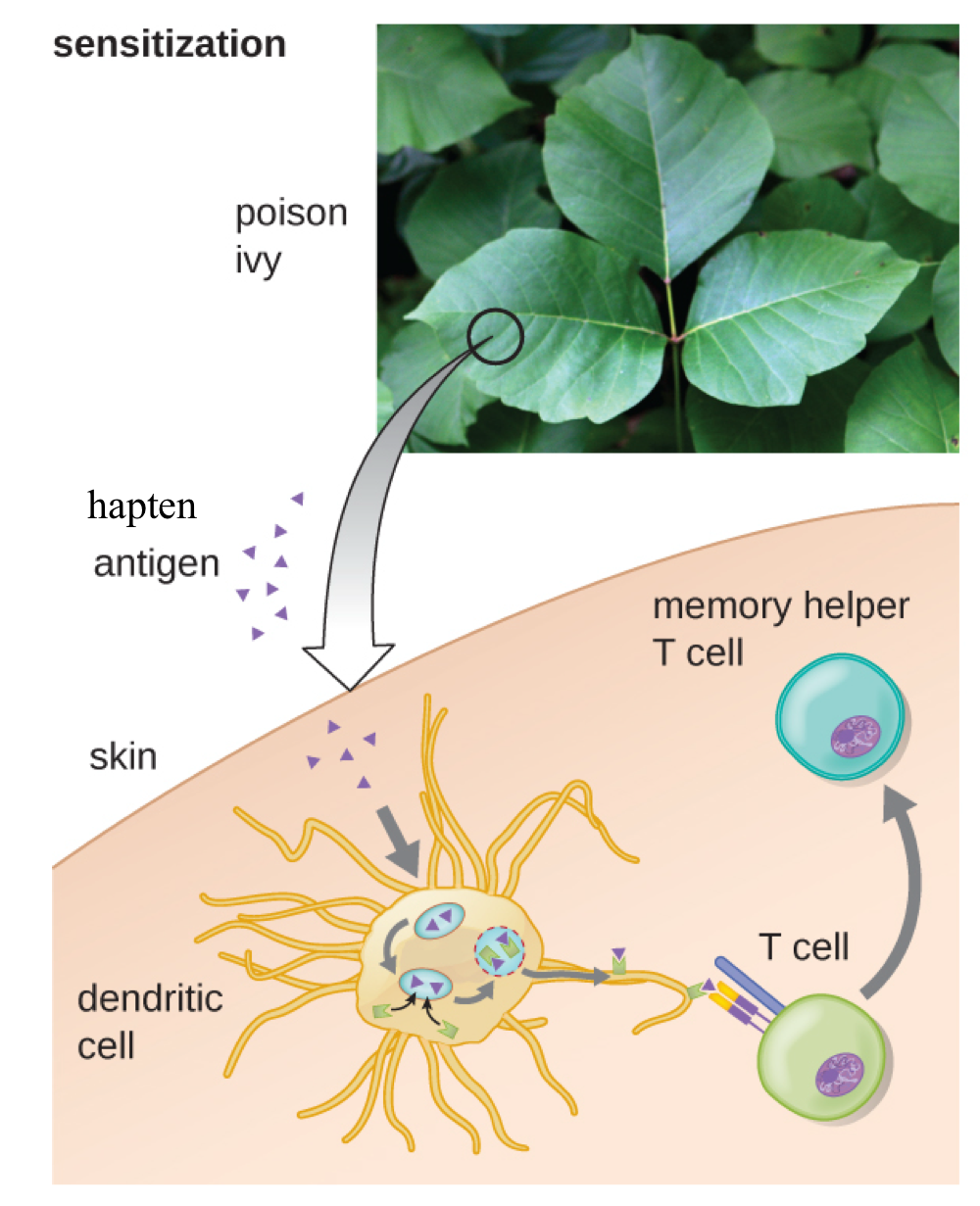
Sensitization:
Antigen Presenting Cell (APC) detects harmless hapten antigen and activate T cells
haptens: small molecules that combine with larger, self-molecules, creating an antigen
memory helper T cells saved
memory cytotoxic T cells saved
Subsequent Exposure:
Helper T cells and macrophages stimulate an inflammatory response when they come in contact with the same hapten again.
Cytotoxic T cells attack body cells presenting the harmless hapten, causing damage.
common in poison ivy, poison oak
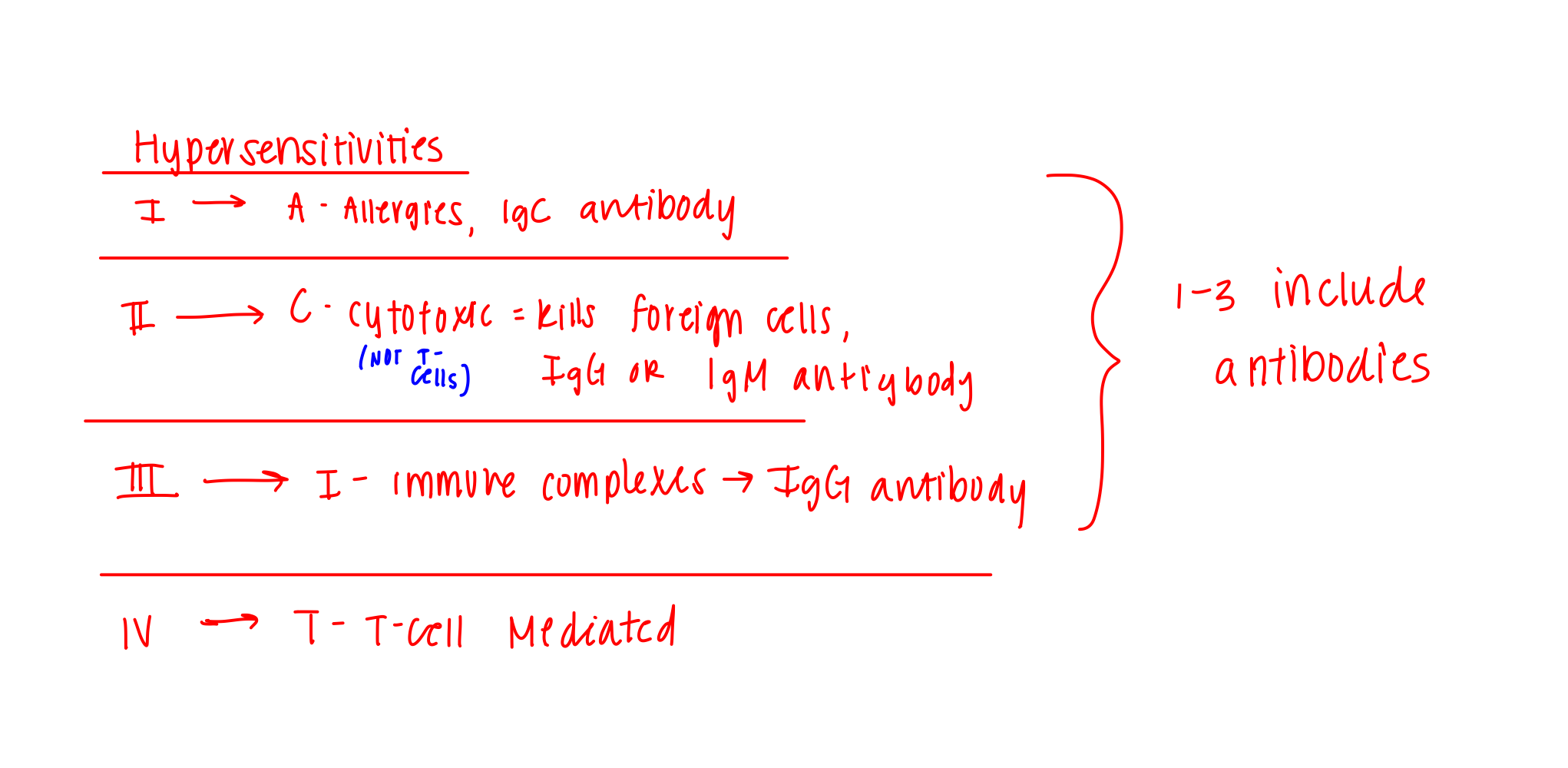
Summary of Hypersensitivities
Type I Hypersensitivity: Allergies
IgE antibodies
Type II Hypersensitivity: Cytotoxic, kills foreign molecules
IgG or IgM antibodies
Type II Hypersensitivity: Immune complexes
IgG antibodies
Type II Hypersensitivity: Delayed
T cell-mediated
Remember by ACID:
allergies (type 1), cytotoxic (type 2) , immune complexes (type 3), delayed/T-cell mediated (type 4)
Hypersensitivity Treatments
Desensitization: Repeated injections of diluted allergens
cause IgG production
if enough IgG is present, it can help neutralize allergens before they bind IgE.
Block immune response:
Antihistamines: Block histamine release from mast cells or bind to histamine and prevent it from being detected from immune cells, preventing action
reduce inflammation
Corticosteroids: hormone body makes naturally when stressed that suppress the immune system
given to patients to suppress the immune response.
longer lasting
Counter anaphylaxis:
Epinephrine: Emergency treatment for anaphylaxis - counteracts inflammatory response, quickly restoring blood pressure and countering severe allergic reactions.
hormone body makes naturally when stressed that suppress the immune system
given to patients to suppress the immune response.
Autoimmune Disorders
Autoimmune Diseases: those in which body is attacked by its own specific adaptive immune response
immune response targets self-antigens, causing tissue damage without external pathogens.
Examples: Hyperthyroidism, rheumatoid arthritis, lupus, etc.
Immunodeficiency Disorders
Immunodeficiencies: inherited (primary) or acquired (secondary) disorders in which elements of host immune defenses are either absent or functionally defective
Types:
primary: inherited, born with it
secondary: acquired, get it you’re older
immune system UNDER reacts
reduced ability of the immune system to respond effectively to pathogens