Anatomy of the Renal System and Urine Formation

Gross anatomy/organs of the renal System
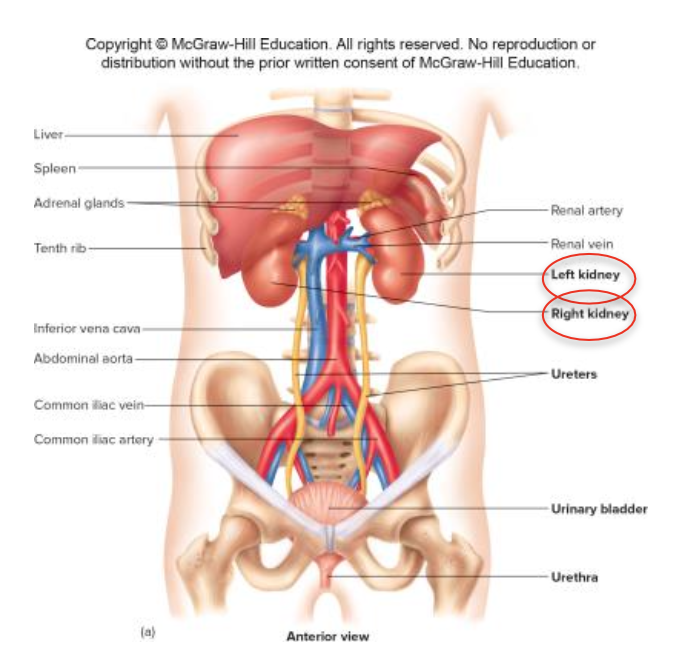
2 kidneys: responsible for urine formation
2 ureters: transport urine from kidneys to bladder
Urinary bladder: stores urine
Urethra: carries urine outside the body
Location and External Anatomy of Kidneys
General Location
posterior to the parietal peritoneum on the posterior abdominal wall.
Lateral to the spine; the right kidney is slightly lower (inferior) than the left due to the liver's position.
Either side of vertebral column; protected by any trauma from bony vertebrae
Average size: ~11 cm long, ~5 cm wide, ~130 grams (around the size of a small fist)
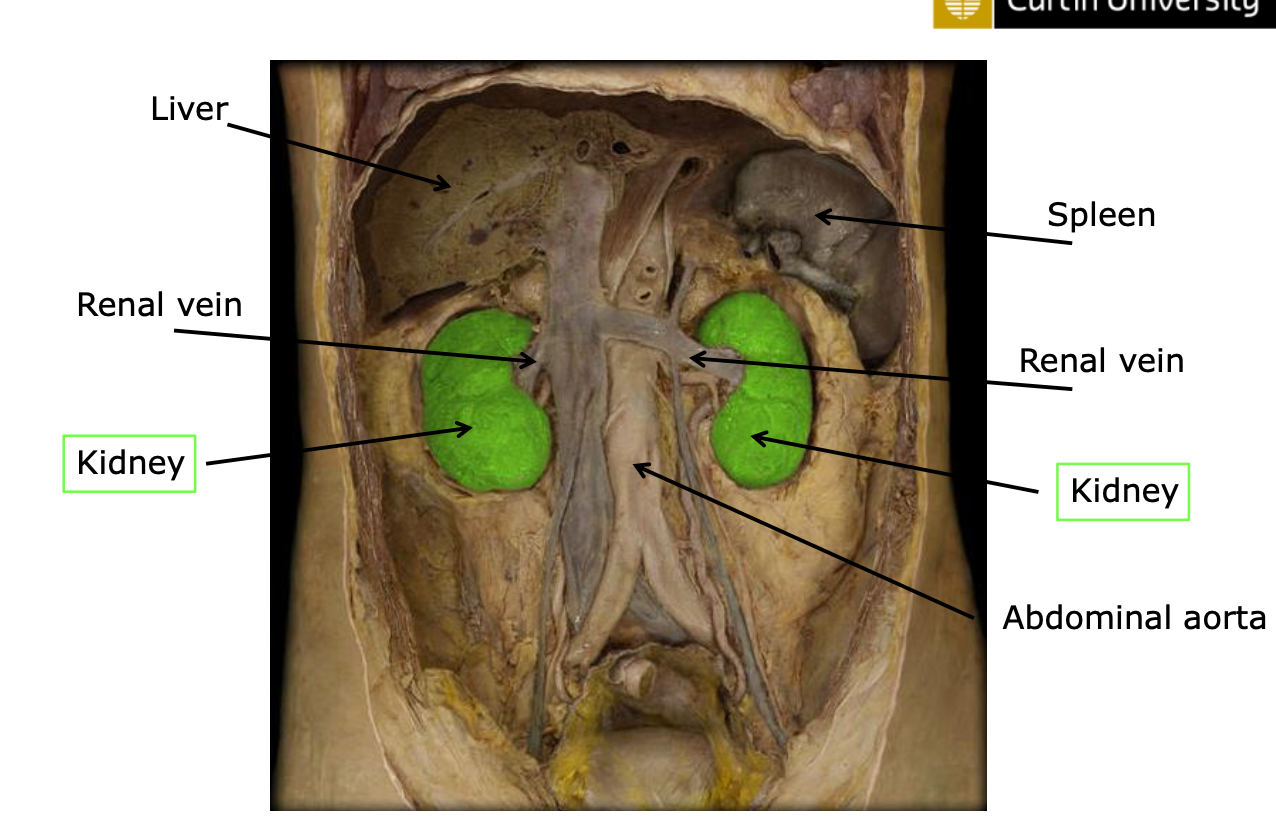
Anatomical Features
#image below shows kidney located OUTSIDE of peritoneal cavity
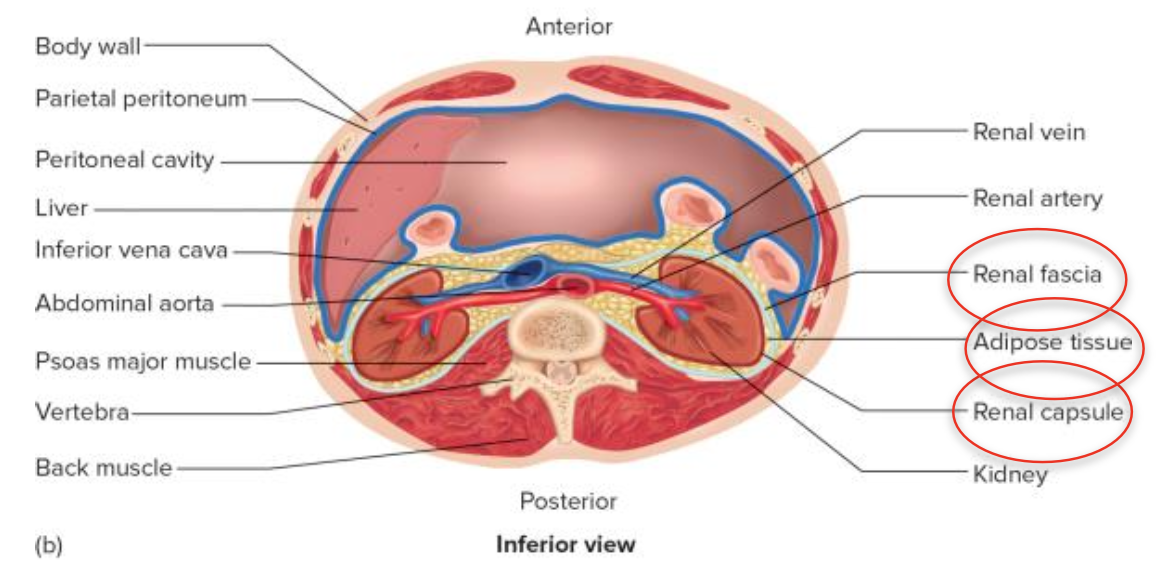
Renal Capsule: fibrous connective tissue that surrounds each kidney.
Adipose Tissue: Provides cushioning outside the capsule for protection.
Renal Fascia: Thin connective tissue layer that anchors kidneys to the abdominal wall.
Kidney external anatomy
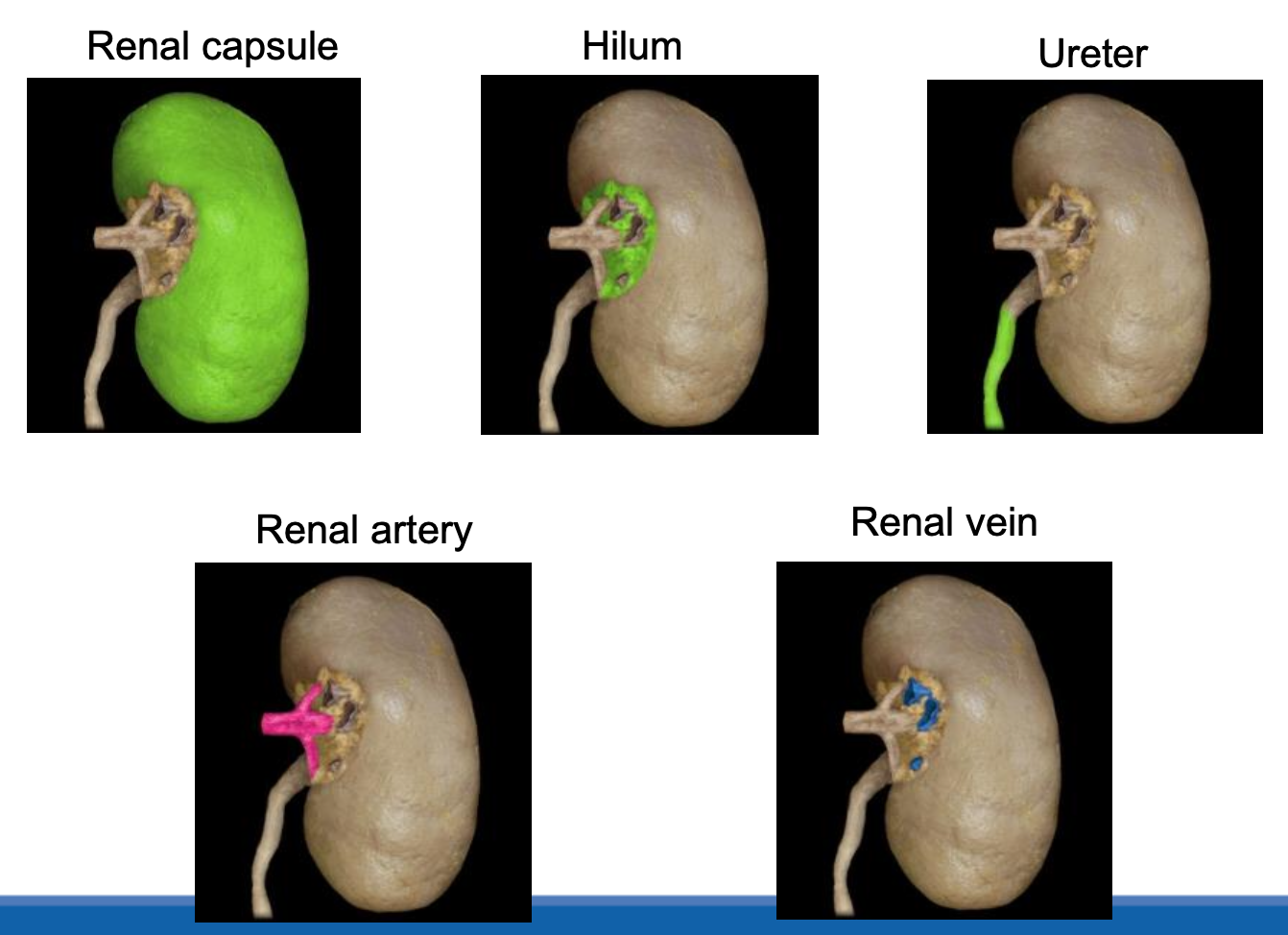
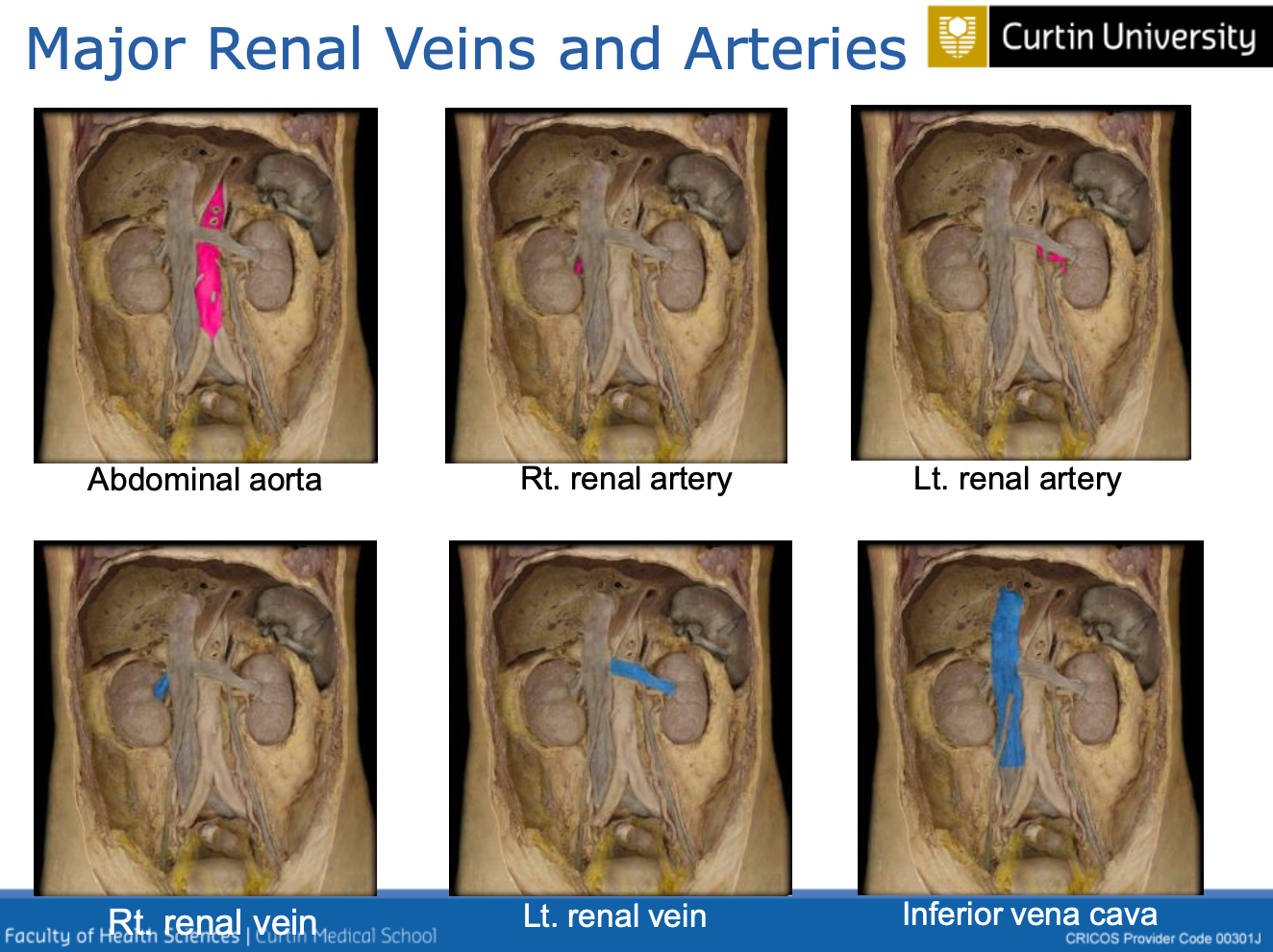
Renal artery: delivers oxygenated blood from heart to kidneys
Renal vein: delivers deoxygenated away from kidneys and to the heart
Internal Anatomy of Kidneys
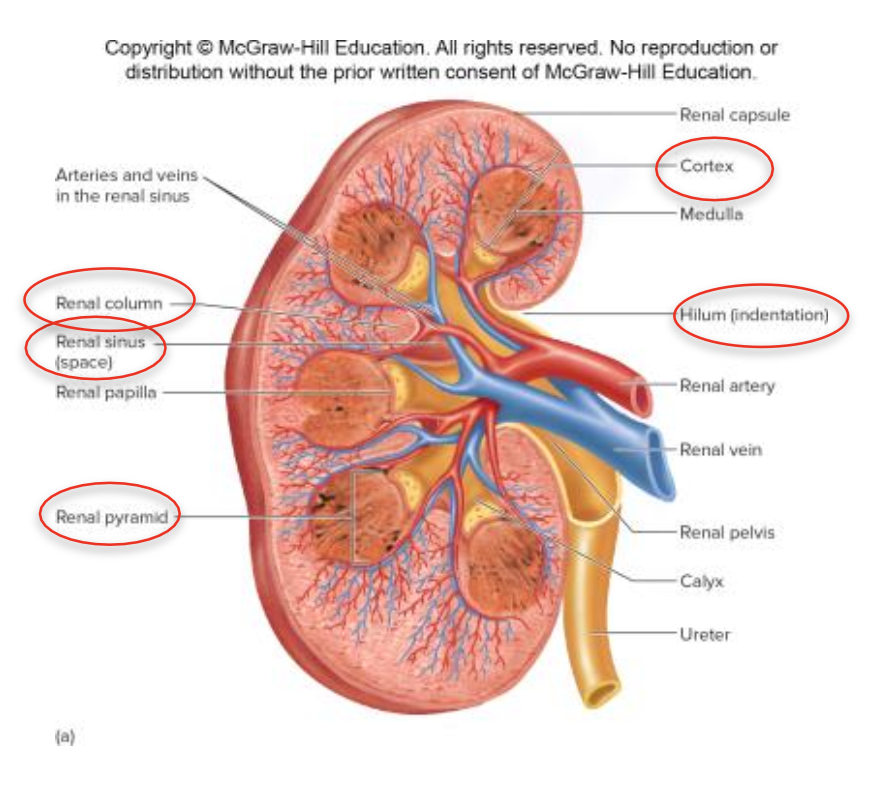
Hilum: Medial concave surface where the renal artery and nerves enter, and the renal vein, ureter, and lymphatics exit.
opens into renus sinus (filled with fat and loose CT)
Regions of the Kidney
Outer Cortex: Contains renal columns (extensions of corticol tissue into medulla) and blood vessels.
Inner Medulla: Contains renal pyramids, which project into the cortex.
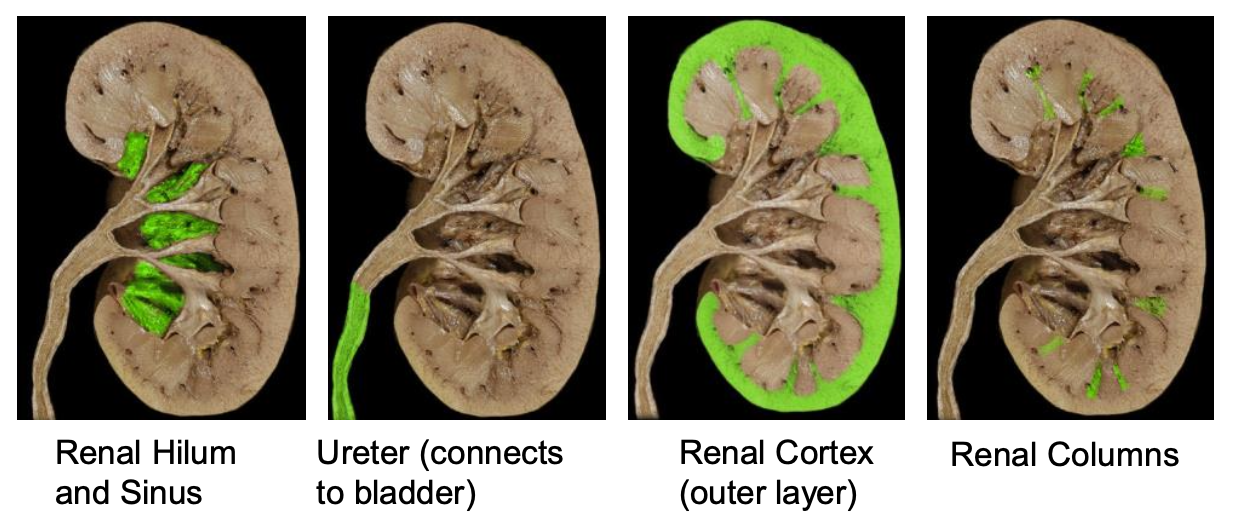
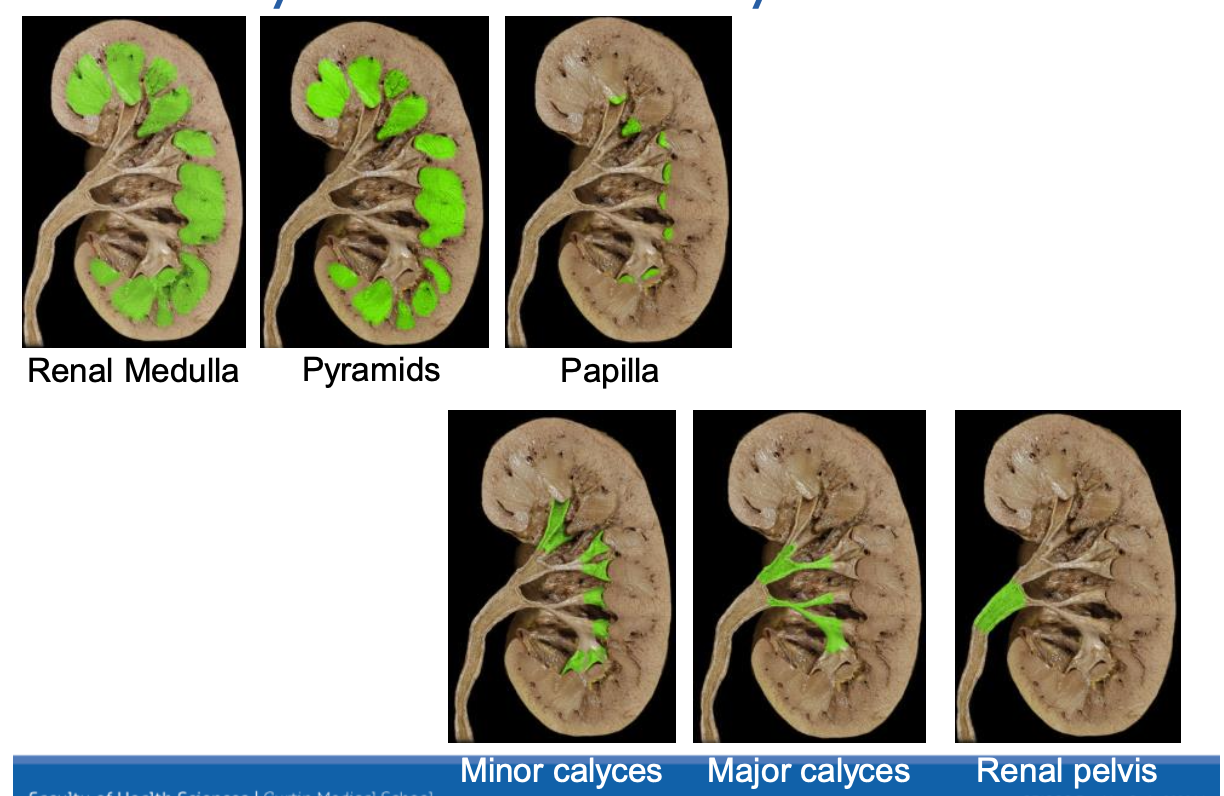
Renal pyramids
forms a boundary between the cortex and medulla
the apex medially points to the renal papilla
pappilae extends into minor calyces (funnel shaped chamber) 8-20 per kidney
minor calyces funnel into major calyces
renal papilla → minor calyces → major calyces → renal pelvis → ureter
renal pelvis: single large funnel-shaped chamber which narrows to form the ureter at the hilum
The Nephron
Functional Unit of the Kidney
Approximately 1.3 million nephrons per kidney, each ~50-55 mm in length.
Blood enters nephron for filtration (filtrate/urine is produced)
Urine flow: nephron → papillary ducts → minor calyces → major calyces → renal pelvis → ureter
Types of Nephrons
Juxtamedullary Nephrons: 15%, deep renal corpuscle, long loop of Henle.
Cortical Nephrons: 85%, located near the cortex, shorter loop of Henle.
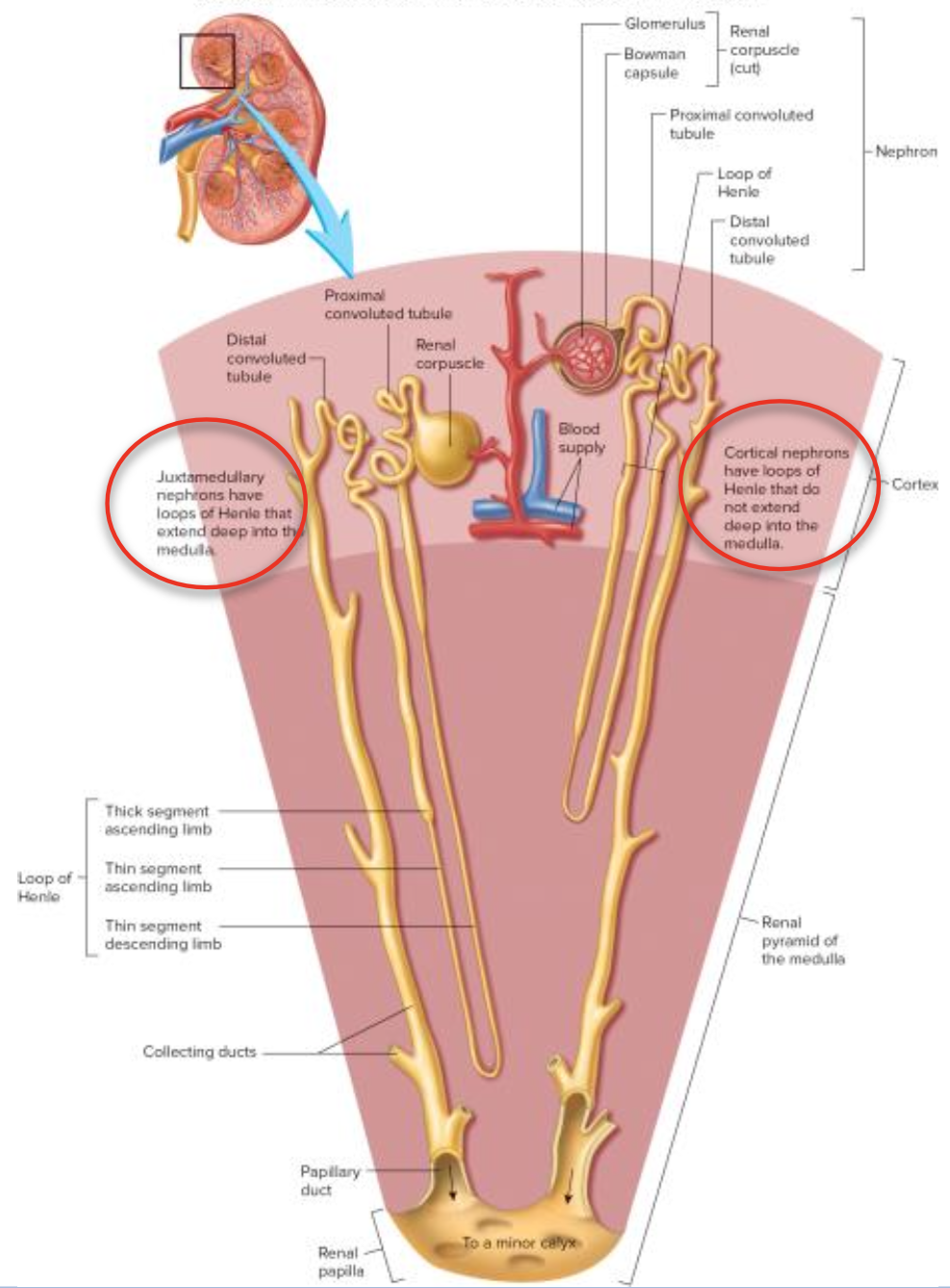
Nephron Structure
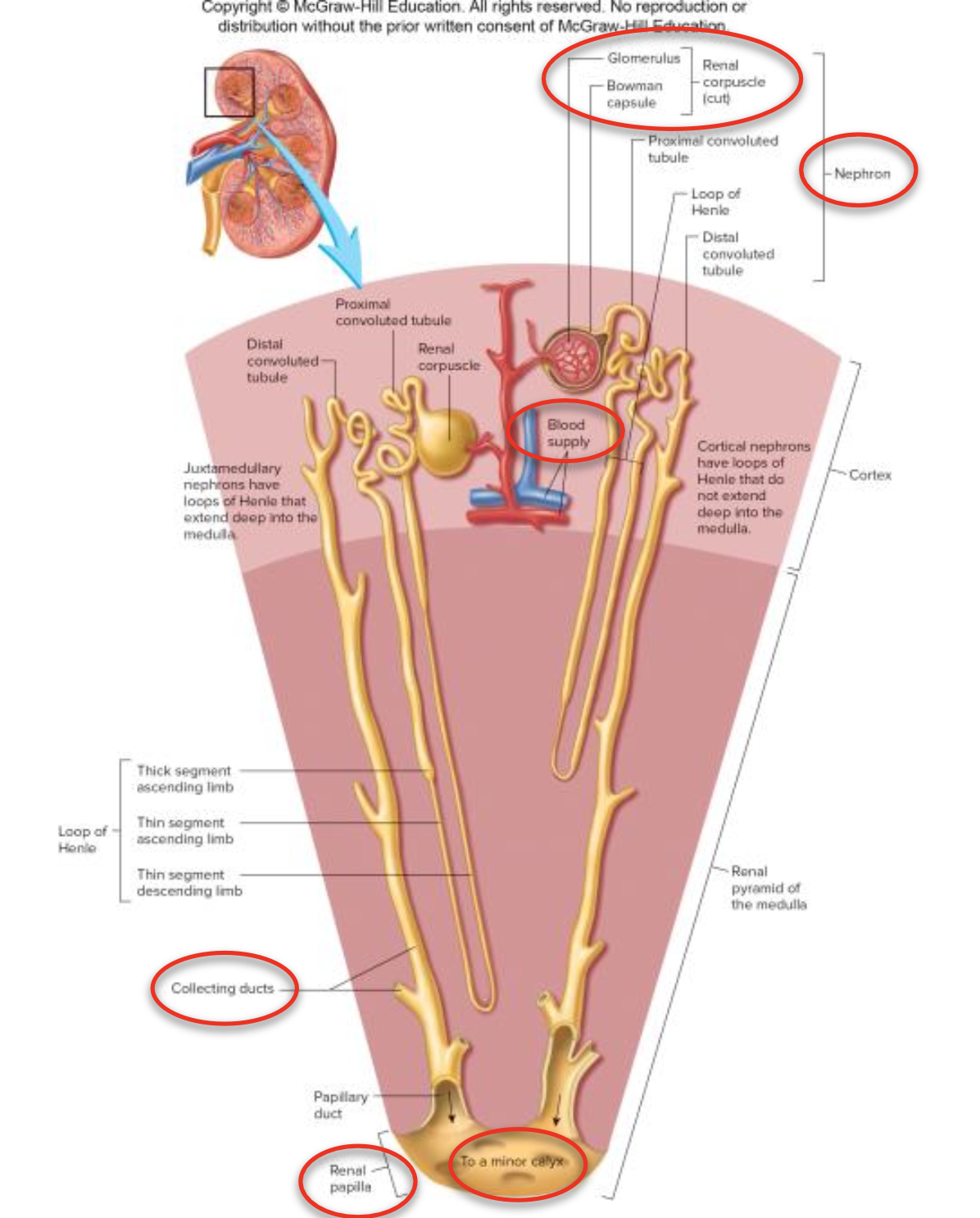
Located in the cortex
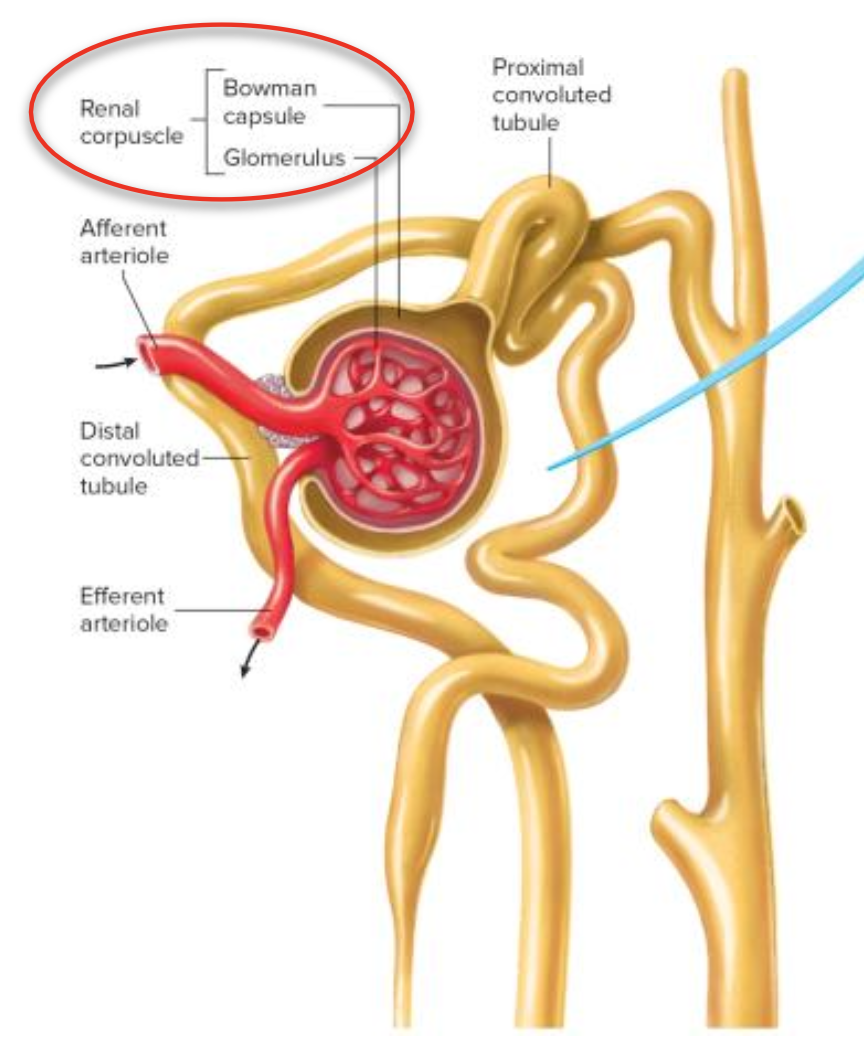
Renal Corpuscle: Glomerulus and Bowman capsule; site of blood filtration.
glomerulus: network of capillaries
bowman capsule: first part of the nephron where blood enters through afferent ateriole, filters in the glomerulus where filtrate sits in bowman capsule
eventually enters PCT and filtered blood exits through efferent arteriole
PARIETAL LAYER - outer, simple squamous epithelium (cuboidal in PCT)
VISCERAL LAYER - podocytes (specialised cells) assists w/ filtration
Proximal Convoluted Tubule (PCT): Major site for reabsorption.
Distal Convoluted Tubule (DCT): Fine-tuning of urine content.
Extended into the medulla
Loop of Henle: Essential for creating a concentration gradient.
Collecting Duct: Drains multiple nephrons into the renal pelvis.
Nephron histology
Proximal convoluted tubule
simple cuboidal epithelium w/ many microvilli and mitochondria
lots of surface area (convoluted, not flat)
active reabsorption: Na+, K+ & Cl-
Loop of Henle
thick areas - simple cuboidal epithelium
thin areas - simple squamous epithelium
osmosis/diffusion
Distal convoluted tubule
simple cuboidal epithelium w/ less microvilli and mitochondria
active reabsorption
Collecting duct
simple cuboidal epithelium
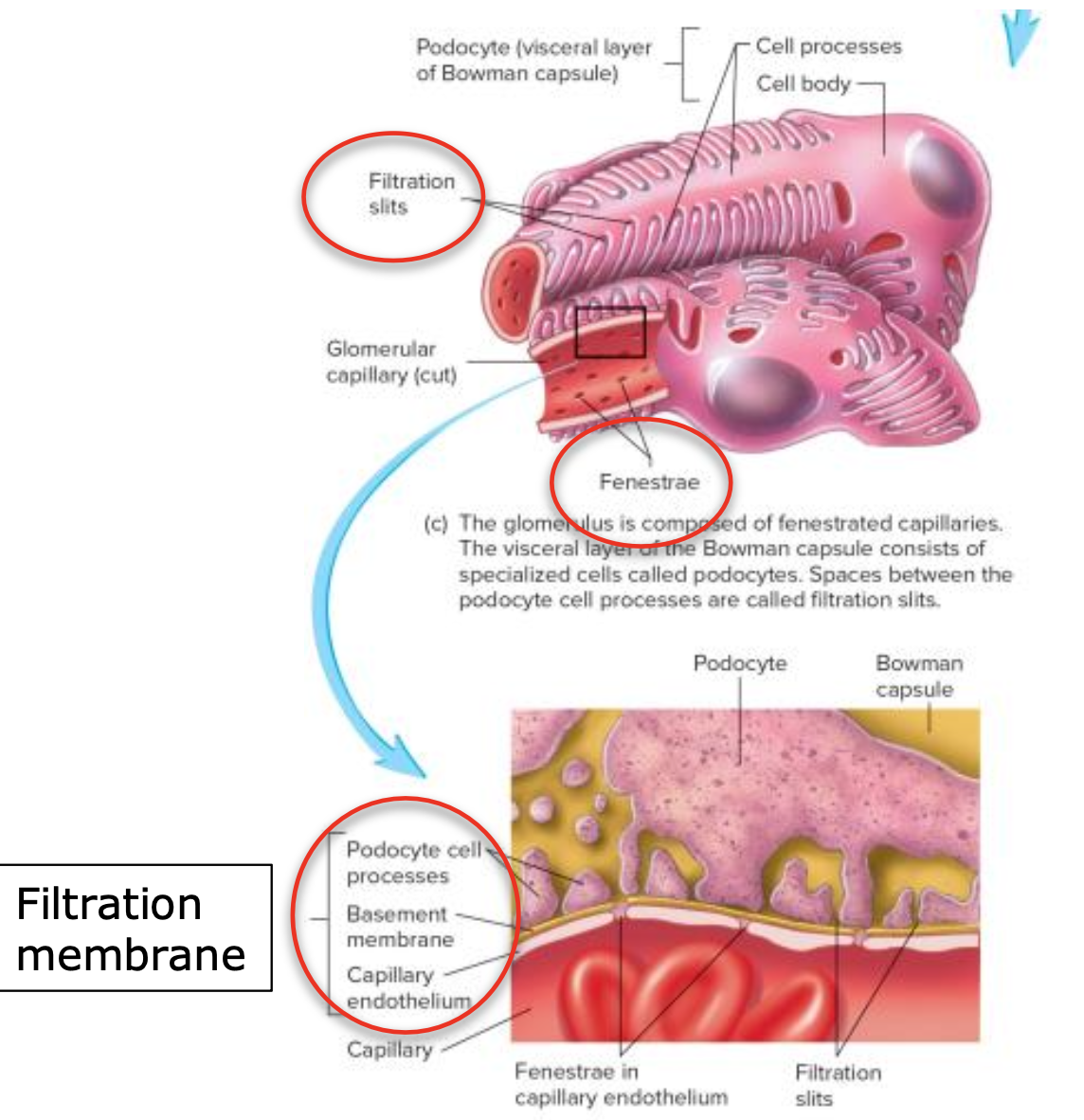
Filtration Membrane
Glomerular has specific characteristics that enable blood to be filtered
Fenestrae: Large pores in the glomerular capillaries increase permeability.
Basement Membrane: Provides additional filtration barrier.
Filtration Slits: Between podocyte cell processes to facilitate filtration.
Bloodflow from heart kidneys and vice versa
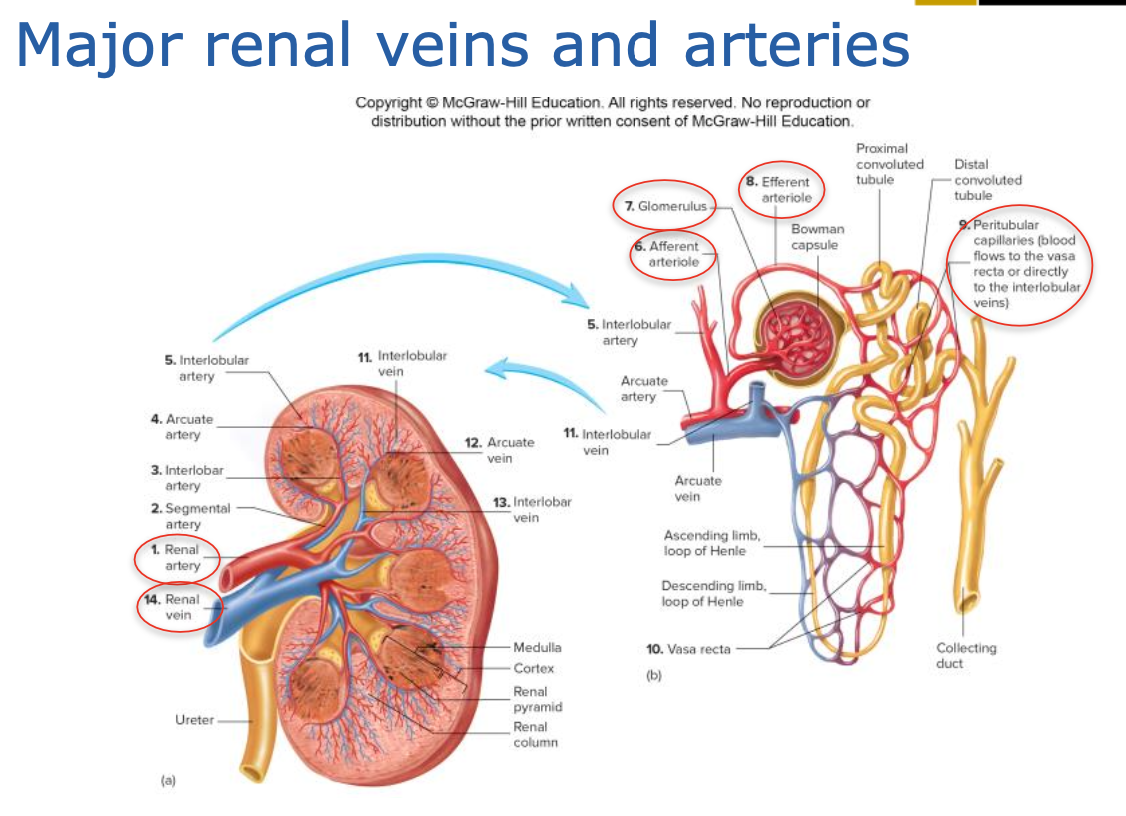
Urine Formation Processes
Glomerular Filtration: Blood enters the nephron, and liquid is filtered through the glomerulus into Bowman capsule.
Tubular Reabsorption: Essential nutrients, water, and ions are reabsorbed in PCT and loop of Henle.
Tubular Secretion: Waste products are secreted into the DCT, adding to the filtrate.
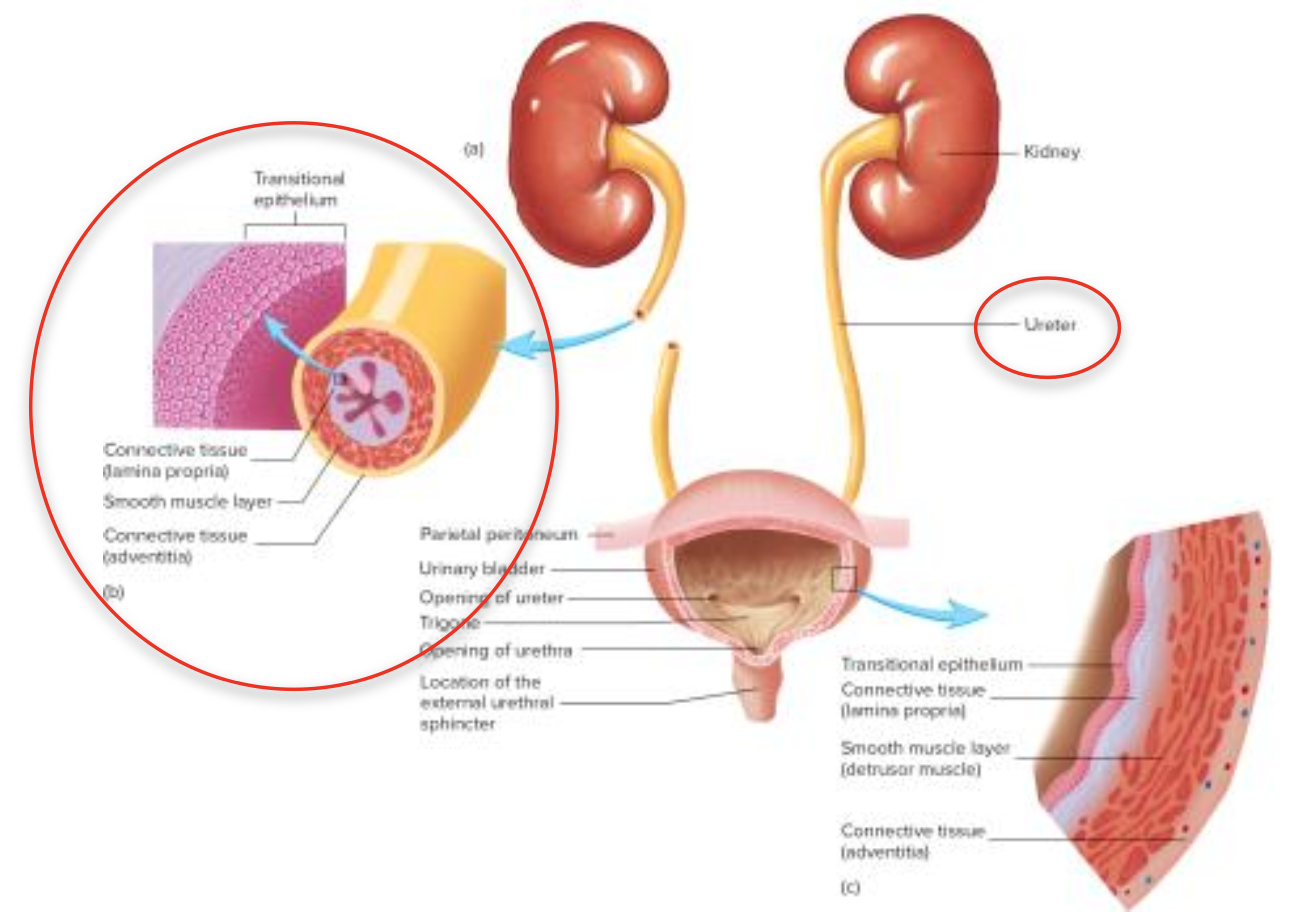
Urine Movement
Pressure Mechanism: Smooth muscle contractions move urine through the ureters via peristalsis from kidneys to bladder.
Ureteral Structure: Lined with transitional epithelium to accommodate urine flow.
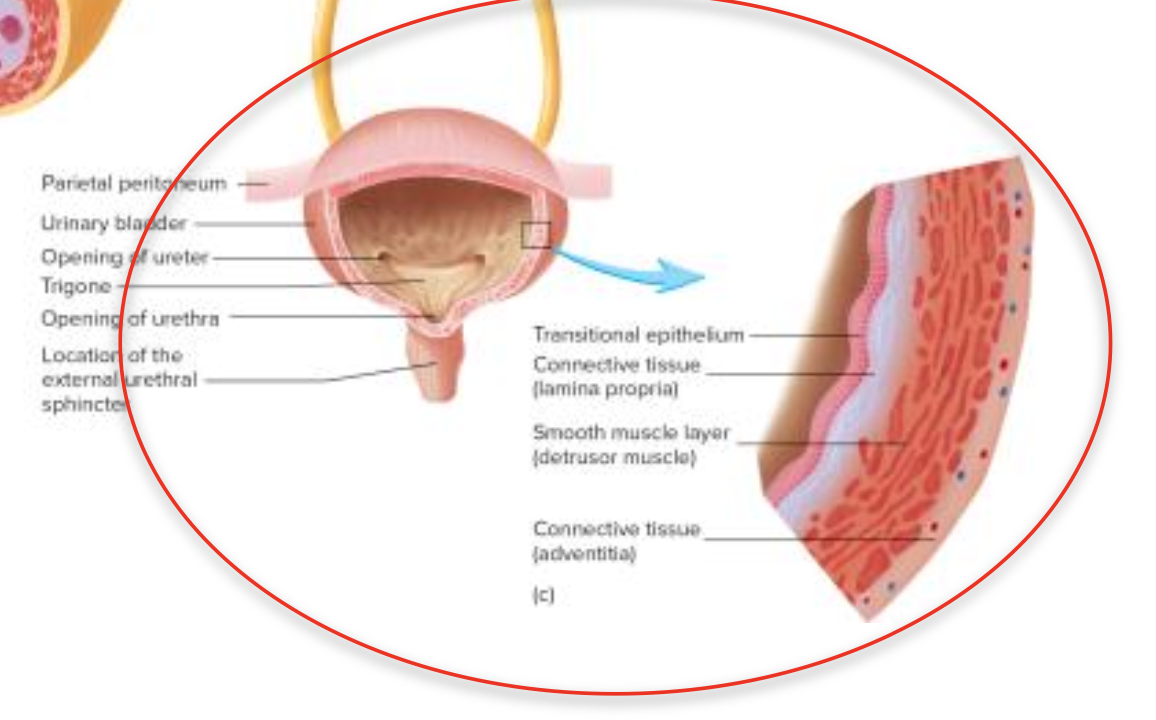
Urinary Bladder and Urethra**
Bladder Anatomy: Hollow muscular organ located in the pelvic cavity, includes the trigone area where the ureters enter.
Urethra Structure: - Different in males (longer, extends to penis) and females (shorter, opens anterior to vagina).
top of urethra - transitional epithelium
rest of urethra - stratified columnar
Sphincters:
Internal (smooth muscle) - prevents urine leakage
External (skeletal muscle) - control of urine flow (starts&stops)
Waste Products in Urine
Common waste products excreted include urea, creatinine, and metabolic waste from protein breakdown.
Review Questions
What main organs comprise the urinary system?
Which organs are involved in urine production vs. transport?
Describe internal kidney structures.
What are the parts of a nephron?
How do nephron parts contribute to urine formation and waste excretion?
What substances are reabsorbed during urine production?
What is secreted into urine during its production?