The Face, Mouth and Pharynx
Neuroanatomy and Neurophysiology Explained:
Identify and explain the neuroanatomy, neurophysiology, and the limbic system as relevant to the control of:
Speech
Language
Hearing
Swallowing
Motivational states
Emotional behavior
Learning and memory
Key Topics to Cover
Bones (Cranial and Facial) Overview:
Relevant to SLT practice through assessment, diagnosis, and treatment of speech and swallowing issues.
Muscle Anatomy:
Muscles of the pharynx.
Muscles of facial expression.
Muscles of mastication.
Muscles of the tongue.
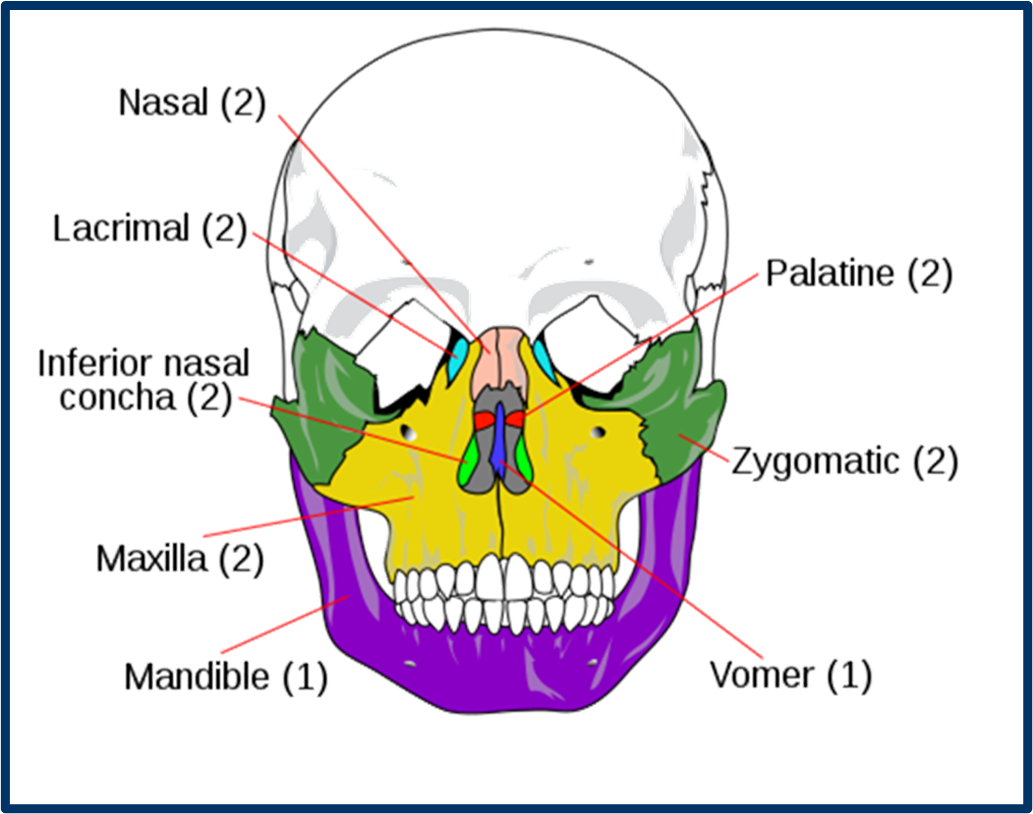
Facial Bones
Facial Bones Overview:
Nasal Bones (2).
Maxillae (2).
Lacrimal Bones (2).
Zygomatic Bones (2).
Palatine Bones (2).
Inferior Nasal Conchae (2).
Vomer (1).
Mandible (1).
Cranial Bones
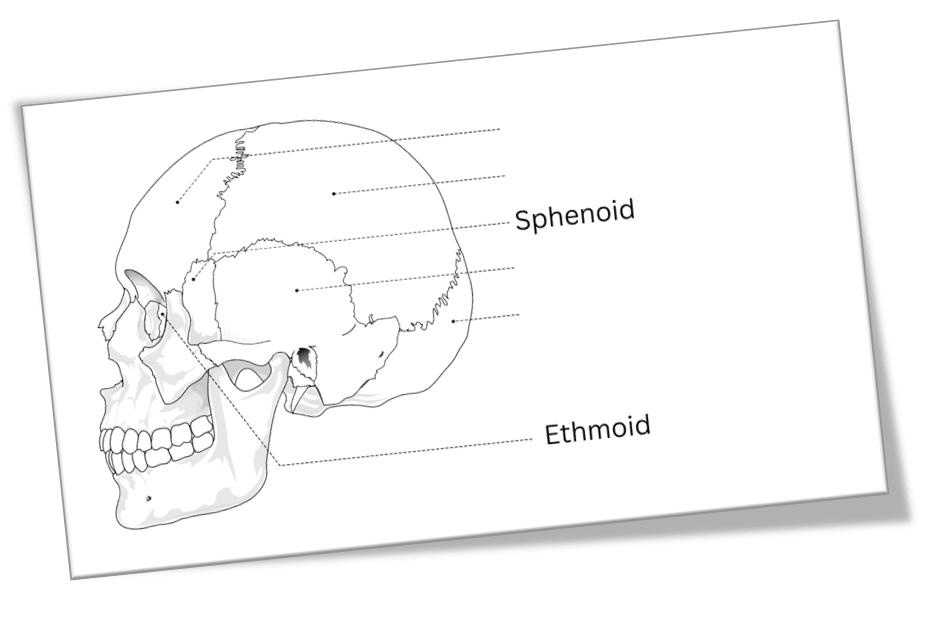
Cranial Bone Overview:
Occipital Bone
Parietal Bones (2)
Frontal Bone
Temporal Bones (2)
Sphenoidal Bone
Ethmoidal Bone
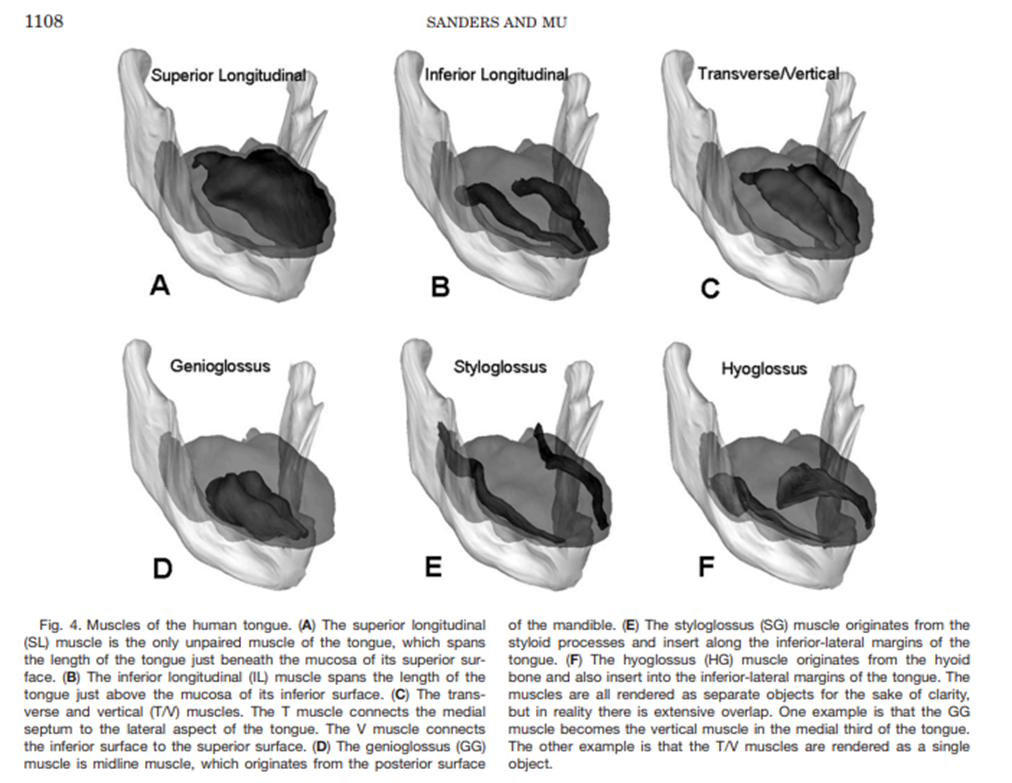
Tongue Muscles
Intrinsic Muscles:
Change the shape of the tongue.
Superior longitudinal muscle.
Inferior longitudinal muscle.
Vertical muscle.
Transverse muscle.
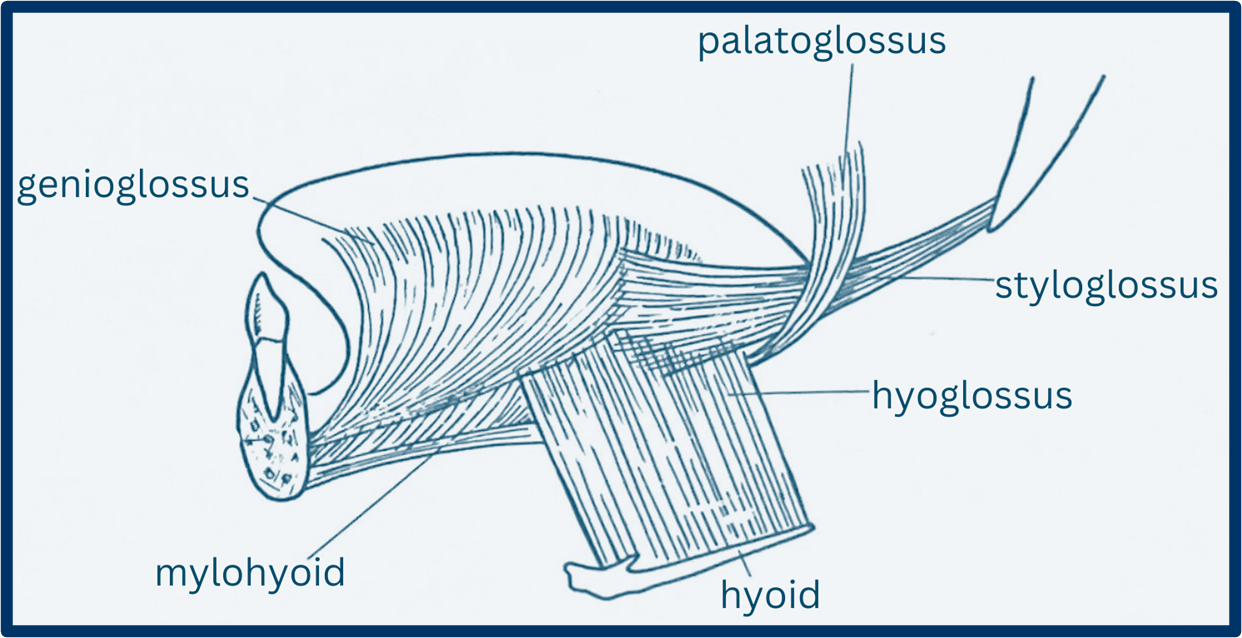
Extrinsic Muscles:
Change the position of the tongue.
Genioglossus muscle.
Hyoglossus muscle.
Styloglossus muscle.
Palatoglossus muscle.
Clinical Relevance of Tongue Function:
Intrinsic muscles allow for fine control:
Extrinsic muscles allow for gross movements, with emphasis on placement for speech clarity.
Styloid- bone

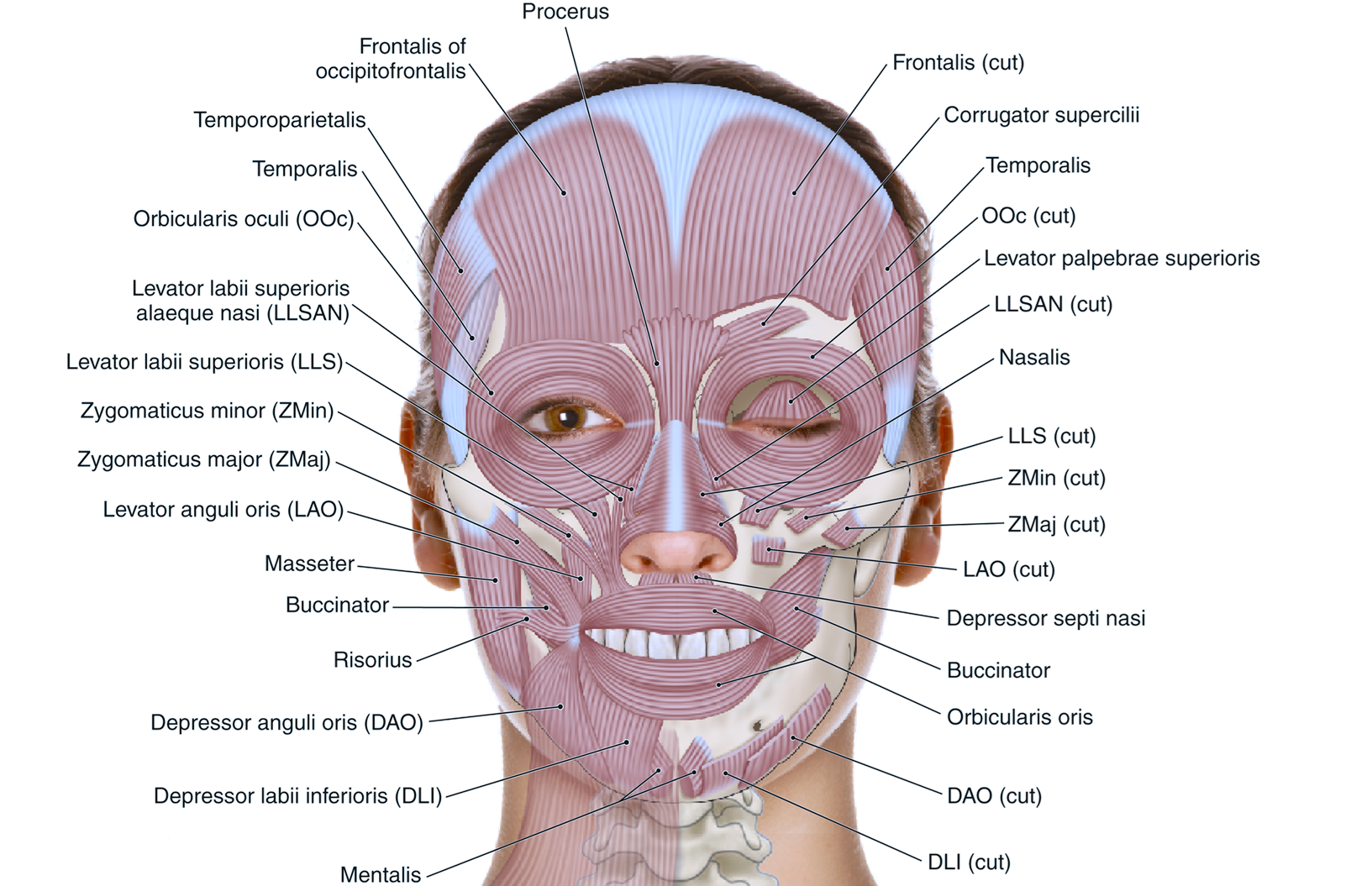
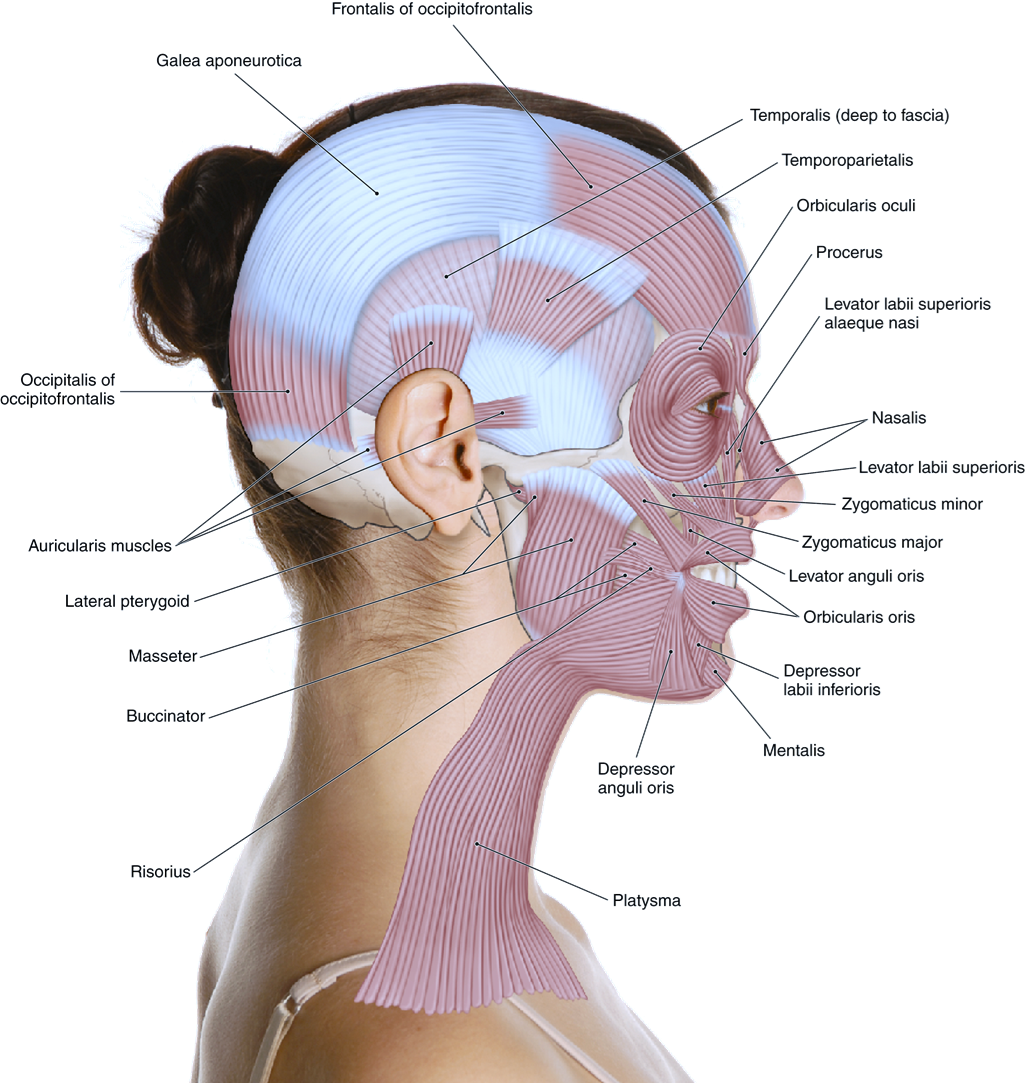
Muscles of Facial Expression
Muscle Overview and Functions:
Example muscles include:
Frontalis
Orbicularis oculi
Zygomaticus (minor and major)
Buccinator
Orbicularis oris
Pharyngeal Muscles
Muscles Overview:
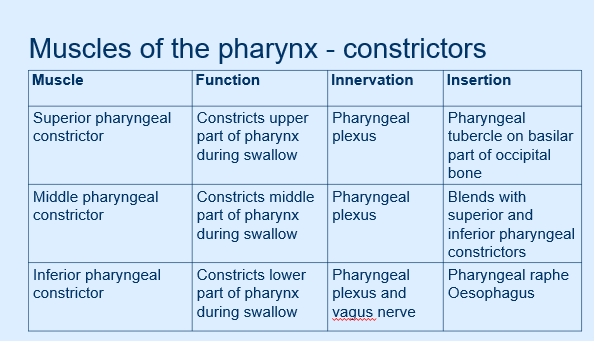
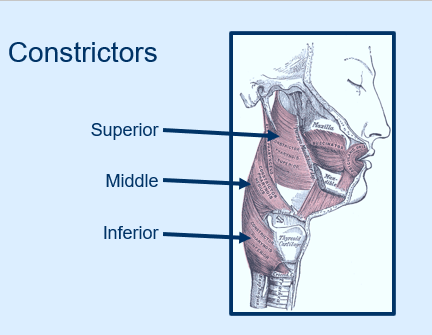
Pharyngeal Constrictors:
Superior, Middle, Inferior
Function: Constricts the pharynx during swallowing.
Innervation: Pharyngeal plexus for the superior and middle constrictors; inferior constrictor also innervated by the vagus nerve.
Insertion Points:
Superior: Pharyngeal tubercle on the basilar part of the occipital bone.
Middle: Blends with superior and inferior constrictors.
Inferior: Pharyngeal raphe and esophagus.
Additional Pharyngeal Muscles and Functions:
Palatopharyngeus: Shortens pharyngeal lumen during swallow
Salpingopharyngeus: Blends with palatopharyngeus and shortens the pharyngeal lumen during swallow
Stylopharyngeus: Innervated by the glossopharyngeal nerve (IX), shortens pharyngeal lumen during swallow.
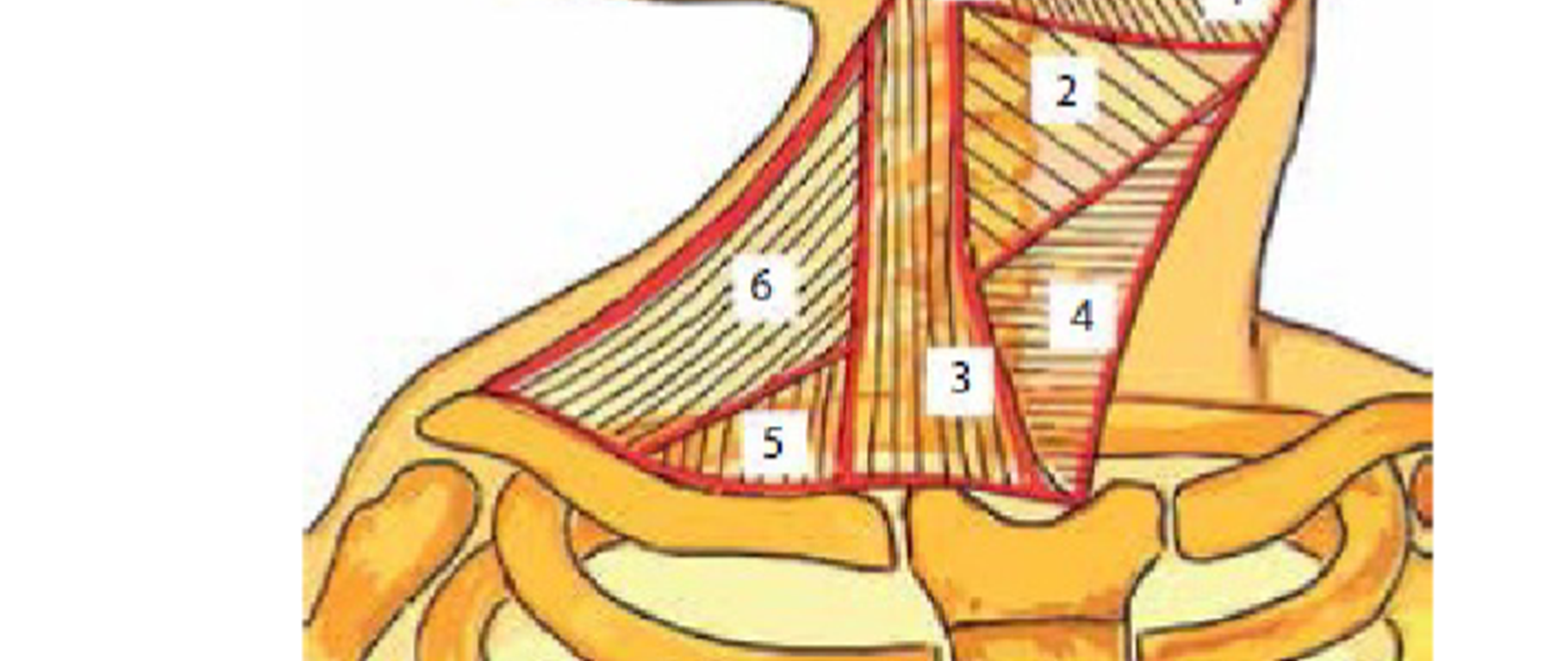
Remember: Anterior, posterior.
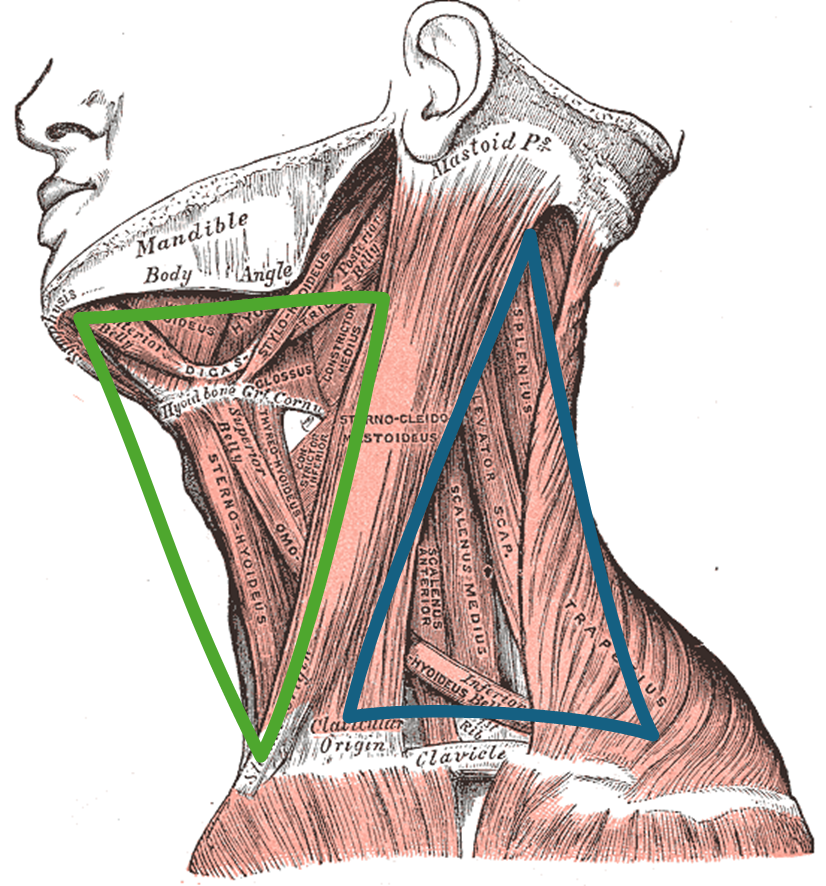
Anatomy and Impact on Speech
Role of Pharyngeal Structures and Muscles in Resonance
Definition of Resonance:
Process of how air and sound vibrations are shaped within the vocal tract.
Key Structures:
Oral, nasal, and pharyngeal cavities act as resonating spaces influencing voice quality.
Role of the Velum:
Affects sound production:
Elevates for oral sounds.
Lowers for nasal sounds.
Factors Influencing Resonance:
Airflow vs. resistance from the nasal cavity.
Structural variations such as palate shape and tongue position.
Soft Palate Anatomy
Components of the Soft Palate:
Palatine aponeurosis and five key muscles involved:
Musculus Uvulae: Shortens and raises the uvula.
Palatopharyngeus & Tensor Veli Palatini: Create tension during swallowing.
Levator Veli Palatini: Elevates soft palate, blocks food from entering the nasal cavity.
Palatoglossus: Depresses the soft palate.
Swallowing Dynamics
Muscle Participation:
Approximately 8-10 muscles involved in the oral stage of swallowing.
Approximately 10-12 muscles involved in the pharyngeal stage of swallowing.

Consequences of Anatomy on Speech and Swallowing
Case Study:
45-year-old woman post partial maxillectomy due to nasopharyngeal carcinoma. Waiting for prosthesis.
Key Questions:
Consequences on articulation, oral cavity function, and resonance.
Impact on speech clarity and nasality.
Potential SLT interventions: compensatory strategies, prosthetic devices, or articulation therapy.
Importance of Knowledge in SLT
Clinical Implications:
Understanding anatomy critical for effective assessment, diagnosis, and treatment of communication and swallowing difficulties, particularly in trauma and cancer recovery patients.
Emphasis on practical application of knowledge rather than mere memorization.
Assessment Preparation:
MCQs and diagram labeling will assess detailed anatomical knowledge, enhancing clinical reasoning and case management skills.
Summary
Core Knowledge Recap:
Understanding the structures and functions of the anatomy directly influences SLT practice, patient assessment, diagnosis, and treatment planning.