Chapter 5: Practitioners and Workplace Settings
Chapter 5: Practitioners and Workplace Settings
Introduction
Health care in Canada is provided by a wide variety of health care providers
Includes conventional (or mainstream) medical practitioners and those practicing complementary and alternative medicine
Informal workers are also integral:
Volunteers of community organizations
Friends and family members caring for loved ones at home
Practice settings include:
Hospitals
Residential care facilities
Rehabilitation centres
Community care facilities
Hospices
A variety of clinics, offices, primary care settings, and home
Who delivers health care, and when, how, and where it is delivered is undergoing continual change
This change aims to provide Canadians with timely, cost-effective access to primary, secondary, and tertiary care to accommodate the health needs of an aging population
Many regions in Canada are experiencing a shortage of primary care practitioners
According to Statistics Canada (2014):
14.9% of Canadians, ages 12 and older—roughly 4.5 million people—reported not having a family physician
To address this issue, the College of Family Physicians of Canada (CFPC) in 2011 proposed the concept called the Patient’s Medical Home (PMH)
The proposal builds on existing models used in delivering primary care such as:
Alberta’s Primary Care Networks
Saskatchewan’s Collaborative Care
Emergency Centres
Ontario’s Family Health Teams
Nova Scotia’s Collaborative Care Teams
The continuing goal is to ensure that all Canadians have a primary care provider, usually a physician, who is the hub of a team of health care professionals
Added objective: Provide a stable medical environment where the patient feels comfortable and can access any required health care
Interprofessional collaboration and expanding roles of health care providers strengthen the team approach to primary health care
Most Canadians still want the security of having a family physician, but there are other options such as nurse practitioners and physician assistants
The amount and type of care rendered within the community continues to expand, with many individuals being cared for at home
Shift to community-based care aims to reduce health care costs by:
Shortening hospital stays
Enhancing patient recovery
Minimizing risk for hospital-based (nosocomial) infections
New procedures, increased community support for home-based recovery, and multidisciplinary teams in primary care settings have facilitated this change
The 2017-2018 Federal Health Accord provided funding to all jurisdictions directly to improve and expand home and community care services
This chapter will look at different health care workers in Canada:
Who they are
What they do
Where they work
It will briefly examine professional organizations that support these individuals, and the regulations, policies, and procedures in place to ensure qualified care
Focuses mainly on evolving team-based models of delivering primary care in Canada
The list of health care professionals represents a cross-section of these providers
The provision of health care involves numerous professionals in both essential and supportive roles:
Clinical practitioners
Those offering IT and administrative support
Categories of health care providers
Health care providers have traditionally been divided into three categories:
Conventional, core, or mainstream
e.g., physicians, nurse practitioners, midwives, nurses, dentists
Allied health professionals
e.g., dental hygienists, dietitians, optometrists, psychologists
Complementary and alternative practitioners
e.g., Indigenous healers, naturopathic doctors, massage therapists
Some sources refer to health professionals as either regulated or nonregulated, dispensing with the previously discussed categories.
See Table 5.1 for a categorization of some of Canada’s many health care providers.
Conventional Health Care Providers
Chiropodists (Podiatrists)
Dental Assistants
Dental Hygienists
Dentists
Registered Dietitians/Nutritionists
Licensed Practical Nurses
Medical Laboratory Technologists
Medical Radiation Technologists
Midwives
Nurse Practitioners
Occupational Therapists
Opticians
Optometrists
Osteopaths
Personal Support Workers (Health Care Aides)
Pharmacists
Physician Assistants
Physicians
Physiotherapists
Psychologists
Registered Nurses
Clinical Nurse Specialists
Registered Psychiatric Nurses
Respiratory Therapists
Social Workers
Speech-Language Pathologists
Audiologists
Complementary and Alternative Health Care Providers
Indigenous Healers
Acupuncture Practitioners
Aromatherapists
Chiropractors
Homeopathic Doctors
Massage Therapists
Naturopathic Doctors
Reflexologists
Reiki Practitioners
Therapeutic Touch Practitioners
Traditional Chinese Medicine Practitioners
Yoga Practitioners
Note:
This list is neither exclusive nor definitive. Titles, roles, and categorization vary by region. For example, chiropractors and acupuncture practitioners may be considered conventional health care providers by some. However, these categories are controversial, as managing the care of patients has taken on a team approach, with numerous health professionals participating in and contributing to the patient’s diagnosis, treatment, and ongoing care. Moreover, interdisciplinary team members are regarded as partners in rendering patient care, contributing differently but equally, relative to their professional expertise and scope of practice.
Conventional Medicine
Conventional medicine is frequently referred to as orthodox, mainstream, traditional, or Western medicine.
It typically encompasses all those modalities not performed by alternative practitioners.
Conventional medicine involves:
Diagnosing health problems
Treating prediagnosed health problems
Rendering technical, therapeutic, or supportive care
Utilizing scientifically proven therapies, medication, and surgery.
Complementary and Alternative Medicine
Complementary and Alternative Medicine (CAM) is practiced by all health care providers not considered mainstream.
There is a difference between alternative and complementary medicine:
Complementary medicine supports or complements conventional medicine.
Alternative medicine provides an alternative often to the exclusion of conventional medicine.
What is considered alternative or complementary is fluid and subjective.
Standards for treatment vary by country or province; e.g., Acupuncture is standard in China but part of CAM in Canada.
Private insurance may cover some CAM therapies, but most provincial and territorial insurance plans do not; therapies are generally not used in hospitals.
Many CAM techniques originate from spiritual, cultural, or religious beliefs and remain unproven by scientific standards.
Critics argue treatments should be scientifically proven (evidence-informed or evidence-based approach).
An example: Therapeutic touch claims to use balance and energy, but lacks scientific evidence to alter disease.
CAM can reduce stress and promote relaxation.
Many Canadians use CAM due to:
Disillusionment with conventional treatment
Difficulty getting appointments
Cultural influences contrasting with mainstream medicine
Information available online
Increased self-participation in health care.
Safe alternative therapies that benefit patients may be welcomed by medical practitioners as a complementary option.
People may seek alternative treatment when conventional medicine has nothing more to offer (e.g., terminal cancer).
Such treatments, if safe, may provide optimism, comfort, possibly prolonging life and easing suffering.
The best outcomes with CAM occur when patients, CAM practitioners, and medical practitioners collaborate to avoid dangerous overlaps in care.
Herbal medicine can interfere with prescribed medications; e.g., St. John’s wort and prescription antidepressants can lead to an overdose.
Some fail to inform doctors about using herbal medications due to beliefs of harmlessness or fear of disapproval.
Integrating both conventional and complementary medicine fosters a trusting alliance with patients, yielding medical and psychological benefits.
Chiropractic: Conventional, Complementary, or Alternative?
Chiropractors (doctors of chiropractic medicine) form the largest group of CAM practitioners.
To obtain a degree to qualify for clinical practice, chiropractors complete 4 to 5 years of postsecondary education.
They work in individual or group practices, diagnosing and treating a wide range of conditions mainly concerning disorders of the spine, pelvis, extremities, and joints, and their effects on the central nervous system.
Chiropractors take a holistic approach to patient care, using various noninvasive therapies such as exercise routines and spinal adjustments.
Chiropractors are not licensed to prescribe medicine like medical doctors or perform surgery.
Chiropractic care is not covered by most provincial or territorial plans, but many private insurance plans will cover a specified number of visits and treatments.
Chiropractic medicine is considered by many to be on the cusp of alternative and complementary medicine.
The relationship between chiropractors and physicians is variable; some share mutual respect while others prefer to keep professional distance.
Regulation of health care professions
The majority of health care professions are self-regulated.
A professional body enters into an agreement with the government to exercise control over and set standards for its members.
Some professions are regulated by the government, meaning that legislation controls the conduct and practice of the profession and its members.
Regulatory authority is granted through legislation (an act or statute) that outlines the framework for behaviour and values for a given profession.
In Canada, provincial and territorial legislation (e.g., British Columbia’s and Alberta’s Health Professions Act, Ontario’s Regulated Health Professions Act) provides the legal framework for regulating most health care professions.
Regulated professions have self-governing bodies called colleges (e.g., College of Registered Nurses of Nova Scotia, College of Massage Therapists of Newfoundland and Labrador), which regulate the conduct and practice of their members.
Each province and territory has 20 to 30 regulated health care professions; professions regulated in some provinces and territories may not be regulated in all.
For example, registered psychiatric nurses in British Columbia are regulated by a college unique to their specialty—the College of Registered Psychiatric Nurses of British Columbia—while in Ontario, psychiatric nurses are under the umbrella of the College of Nurses of Ontario.
The overriding objective of regulated professions is to protect the public, ensuring that safe care is rendered by health professionals working within their scope of practice.
Title Protection
Regulated professionals belong to a professional body and are licensed to practice their profession.
They are legally entitled to use a specific designation, such as registered massage therapist (RMT).
Professions with title protection mean only trained and registered persons can legally use that title.
Example: Untrained individuals cannot call themselves licensed or registered practical nurses.
Degree dropouts (e.g., respiratory therapy) cannot refer to themselves as respiratory therapists.
Health care aides cannot call themselves nurses.
Those trained on the job can call themselves health care aid or equivalent, as there is no regulatory body preventing this title.
Fully trained nurses registered in other countries must meet the local standards set by the college to practice as registered nurses.
Common elements of regulated professions include:
Educational standards
Provincial and territorial examinations
Practitioner’s scope of practice detailing skills and services they can perform competently and safely
Curbing of practice if standards are not met
Formal complaints process for the public
Complaints investigation and follow-up
Title protection
Competence and quality assurance
Any health care profession can apply to the government to become regulated, but it must meet strict criteria.
The minister of health and an advisory body within the province or territory oversee the lengthy and arduous application process.
Regulation proves a person has undergone training and gained a predetermined degree of knowledge, skill, or ability.
Possessing a driver’s license does not guarantee driving excellence; similarly, some regulated professionals may offer substandard services.
All regulated professionals must practice within a framework of skills and services defined by their governing body.
Nurses have specific skills they are trained to do; physicians have a range of trained skills and services; respiratory therapists and other practitioners also have a defined scope of practice.
Different levels of practice may exist within a single profession. For example:
Registered nurses with advanced practice training may perform acts not available to those without training.
Nurses usually need to take specialized courses to acquire skills like initiating an intravenous line or managing wound care.
A family practice medical doctor is not qualified to perform a gallbladder removal or a hip replacement.
A licensed practical nurse is not qualified to perform a complete physical examination, while a nurse practitioner is.
A massage therapist is not qualified to deliver a baby, but a midwife, nurse practitioner, or obstetrician is.
Many skilled procedures specific to certain professions are referred to as controlled acts.
Performing Controlled Acts
Controlled acts (called reserved acts in British Columbia) may cause harm if not performed by a qualified practitioner.
Examples of controlled acts include:
Giving an injection
Setting or casting a fracture
Passing a nasogastric tube
Prescribing a medication
Identified by the Regulated Health Professions Act (RHA) or equivalent in each jurisdiction.
For instance, the RHA in Ontario has identified 14 controlled acts, which are similar across the country.
Acts related to each profession define which controlled act(s) members can perform; for example:
Respiratory therapists and regulated radiation technologists can perform 5 of the 14 acts.
Physicians can perform thirteen.
Some controlled acts can be performed by more than one regulated profession (overlap), but all regulated health professions can perform controlled acts.
Controlled acts may only be performed in response to an order (either direct or indirect) given by a physician or nurse practitioner.
Exceptions
Most provinces and territories allow controlled acts to be performed in certain situations by competent yet nonregulated individuals, including:
A person with appropriate training providing first aid or assistance in an emergency
Students learning to perform an act under the supervision of a qualified person, as long as that act is within the scope of practice of graduates of the student’s professional program
A person, such as a caregiver, trained to perform an act (e.g., giving injections to a person with diabetes)
An appropriate person designated to perform an act in accordance with a religion—for example, a rabbi may perform circumcision on a male child
Exclusions also apply in the case of body piercing for the purpose of jewellery, electrolysis, tattooing, and ear piercing.
Delegated Acts
The health care system is evolving, impacting health care providers' scopes of practice.
Reforms in the health care system, methods of delivery, and provider responsibilities are affecting traditional roles of health care providers.
Patients' needs are also changing, with a demand for more complex care provided more frequently.
To meet patient needs, health care providers may need to perform acts, procedures, and treatments that go beyond standard boundaries.
A delegated act is defined as the means by which a regulated health professional transfers legal authority or permits another person to carry out a controlled act they are otherwise unauthorized to do.
Delegated acts may include specific procedures, treatments, or interventions not within the delegated person's scope of practice.
Example of delegation:
A registered nurse in the community can delegate giving an injection to a nonregulated provider (e.g., personal support worker) or a family member.
Physicians can delegate tasks like obtaining a pap smear to a nurse or giving allergy injections to an administrative assistant.
Not all controlled acts can be delegated; those eligible for delegation are defined by provincial and territorial regulations.
Examples of non-delegable acts:
A nurse practitioner cannot delegate prescribing medication to a registered nurse or occupational therapist.
A licensed practical nurse cannot delegate dispensing medications to a personal support worker.
A respiratory therapist cannot delegate intubation to a physiotherapist, registered nurse, or nurse practitioner.
Acts generally cannot be subdelegated; the delegate cannot assign another person to carry out the act.
Guidelines for delegation vary across Canada; some jurisdictions permit delegation to regulated professionals, while others extend this to nonregulated individuals.
Supervision of delegated acts can be:
Direct: the delegating provider is physically present.
Indirect: the delegating provider is available for consultation by phone.
Health care organizations must have rules and procedures for delegated acts agreed upon by relevant authorities (e.g., board of directors, medical advisory committee).
The delegating health care professional must ensure that the delegate is trained and competent in carrying out the act.
All parties involved (the delegating professional, the delegate, and the facility) share responsibility for the act performed.
The health care professional assessing the delegate’s performance is accountable for ensuring competence.
The delegate is legally responsible if the act is performed ineffectually.
Informed consent from the patient or their power of attorney is usually required for others to perform the procedure.
For acts commonly performed by physicians, delegation occurs only with the patient’s consent after the physician assesses the patient and discusses the procedure.
Regulations for delegated acts can be found on provincial or territorial websites for relevant nursing and medical associations.
Many colleges also offer courses for nonregulated individuals to learn specific interventions like giving injections or administering medications.
Complaint Process
Regulated professions have established a systematic process for the public to launch complaints against a health care provider.
A designated committee is responsible for investigating all complaints.
This system protects the public by ensuring that legitimate complaints are properly assessed and resolved, providing a sense of security.
Health care providers are safeguarded as well, as illegitimate or unfounded complaints are dismissed.
If a health care provider is found to be at fault, they may face several consequences, including:
Suspension of their practice.
Additional training requirements.
Loss of their licence to practise.
Potential for legal proceedings, including criminal investigations.
Educational Standards
A regulator of a profession has the authority to set educational standards for the training of its professional members.
Standards include:
Theoretical components of education.
Practical components of education.
Examinations for entry to practice.
The educational process:
Prepares professional members.
Provides assurance to the public that the health care provider is competent to practice.
Professional bodies often use competency-based assessment programs to ensure the continued maintenance of practice standards, protecting both the health care provider and the public.
Requirements may include:
Use of self-assessment tools.
Participation in continuing education programs.
Keeping a record of professional activities.
Proof that these standards have been met is often a requirement for renewal of a professional’s licence to practice.
Licence to Practise
Regulators of Professions: Each province and territory has its own regulators, which partner with educational facilities to oversee licensing.
Licensing Requirements:
This oversight is in accordance with provincial and territorial requirements.
Regulated professions typically require annual license renewal.
Additional Criteria:
Many professions now require peer reviews or proof of ongoing education to maintain licensure.
Interjurisdictional Challenges:
Professionals moving between provinces or territories may face issues due to lack of agreements and standards for practice in different
Nonregulated Professions and Occupations
Table 5.2 illustrates the current regulated professions in the provinces and territories across Canada.
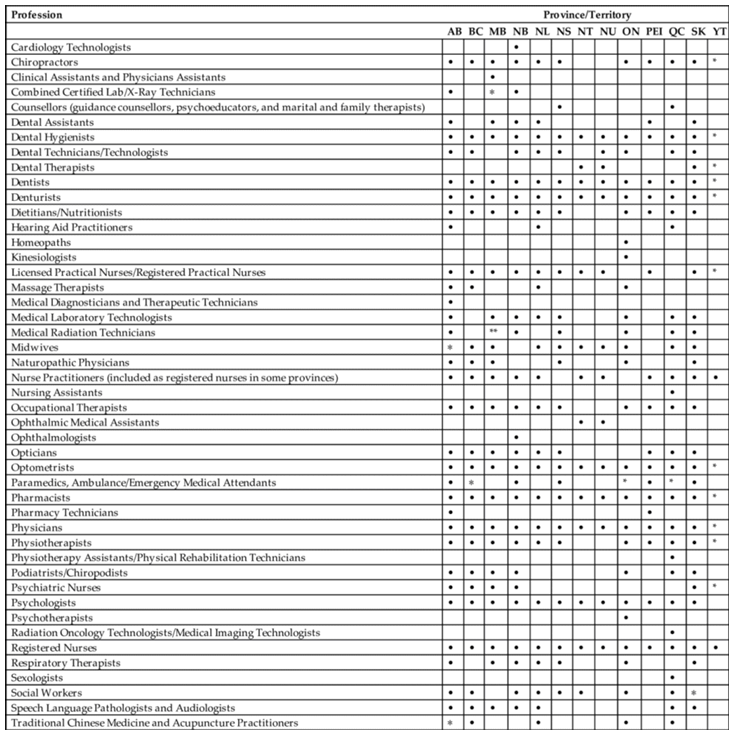
Nonregulated occupations encompass a wide range of jobs, from those requiring university degrees and specialized training to those that necessitate very little education or training.
Individuals in nonregulated occupations do not have federal or provincial legislation governing their work.
Many nonregulated occupations have professional organizations or bodies that offer certification after individuals complete a set of written or practical examinations (e.g., Medical Secretary’s Association in British Columbia).
When a profession is unregulated, job applicants may not have met the educational requirements of their regulatory body; hence, hiring organizations set their own requirements.
For example, to work as a medical secretary or clinical secretary (ward clerk) in a hospital:
A specialized knowledge base is required; however, employers can hire individuals with or without formal certifications.
A doctor can hire someone based on related experience and provide on-the-job training or hire someone graduated from a 1-year certificate or 2-year diploma program in medical office administration.
A hospital might require a clinical secretary to have a grade 12 diploma with some secretarial experience, or a diploma from a 2-year health services administration program.
Many nonregulated disciplines lack specific standards; hence, anyone can claim expertise in practices like ear candling or aromatherapy, inviting the public to seek treatment.
Mainstream health care providers
Health care in Canada has traditionally been dominated by physicians, including family doctors and specialists.
There is a shift occurring toward a team approach to health care.
This evolving model aims to maximize the skills and expertise of various health care providers.
The focus of this shift is particularly evident in the primary care setting.
Physicians
Entrance requirements for medical school in Canada vary but typically include:
Completion of 2 to 4 years of undergraduate work.
Usually obtaining a bachelor’s degree.
Writing an entrance examination, called the Medical College Admission Test (MCAT).
Medical school consists of:
3 to 4 years of study.
Followed by a residency in the individual's area of specialty (e.g., family medicine, internal medicine, general surgery).
A doctor with specialized training in one area is referred to as a specialist, who:
Usually sees patients only upon referral from a family doctor or another specialist.
Most provincial or territorial insurance plans do not cover visits to a specialist without such a referral.
A family doctor refers patients to a specialist or consultant for:
Assessment and treatment that is outside their scope of practice.
Many specialists may work in:
Solo practice.
Private or public organizations.
Or may be employed by hospitals.
Family Physicians
Family Doctors (also called general practitioners or primary care physicians):
Have a wide knowledge base not limited to any specific disease, system, sex, or age group.
Provide ongoing care that includes:
Diagnosis and treatment of conditions and diseases not requiring a specialist.
Counselling
Health promotion and disease prevention
Primary maternity and mental health care
Work Environment:
Most family doctors work in primary care team settings.
Some remain in solo practice.
Others work in various types of clinics or health centres, particularly in remote regions of the country.
Many oversee the medical care of patients in health care facilities such as long-term care residences.
House Calls:
Some family doctors still make house calls (not as prevalent as in the past).
Patients must pay out of pocket for this service.
Hospital Privileges:
Many family doctors choose to give up their hospital privileges.
Care for hospitalized patients may be temporarily passed to a hospitalist or other specialist.
Emergentologists
Emergentologists are physicians who focus on full-time emergency medicine.
This specialty has emerged due to a shift in emergency departments (EDs), commonly known as emergency rooms (ERs).
Many EDs are now opting to hire full-time physicians instead of relying on on-call physicians as they did previously.
Geriatricians
Geriatrics focuses on the care of older people, typically those over 65 years old.
A geriatrician is usually an internist who has additional training in caring for older adults.
Geriatrics does not attract a large number of physicians.
The assessment and treatment of individuals with complex medical conditions is time-consuming.
Geriatricians are typically paid less than other specialists.
Most geriatricians work in:
Private practice
Team-oriented practices
Health care facilities.
Cardiologists
Cardiologists specialize in conditions and diseases of the heart.
They treat a range of issues, including:
Abnormal rhythms
Heart attacks
Related vascular problems
Cardiologists provide treatment from a medical perspective and do not perform surgery.
If surgery is necessary, they refer patients to a cardiac surgeon.
In addition to office visits, cardiologists with special training can:
Carry out diagnostic procedures such as cardiac catheterizations.
These procedures may take place in a hospital or private diagnostic facility.
Gynecologists and Obstetricians
Gynecologists:
Specialize in women's health.
Diagnose and treat disorders of the gynecological and reproductive systems.
Obstetricians:
Focus on the care of pregnant women.
Responsible for the delivery of babies in both normal and high-risk situations.
OB/GYN:
The two specialties are closely related and commonly undertaken together, represented by the abbreviation OB/GYN.
Internists and Hospitalists
Internist:
Typically diagnoses and renders nonsurgical treatment for diseases of a person’s internal organs (e.g., problems of the digestive tract, liver, or kidneys).
Often refers patients to other specialists who deal with specific organs.
Hospitalist:
A physician, usually an internist, who oversees the medical care of patients in the hospital.
Usually cares for patients who do not have a family doctor with admitting privileges to that hospital.
Collaborates with specialists as required for additional care.
Typically employed by the hospital; may or may not have a private practice.
Neurologists
Neurologist: A medical doctor specializing in the nervous system.
Treats various conditions including:
Chronic and potentially fatal conditions:
Parkinson disease
Multiple sclerosis
Sleep disorders
Headaches
Peripheral vascular disease
Brain tumors
Spinal cord injuries
Neurologists do not perform surgery.
Patients requiring surgery are referred to a neurosurgeon.
Ophthalmologists
Ophthalmologists: medical doctors specializing in diseases of the eye
Can perform both medical and surgical procedures, including:
Cataract removal
Ocular emergencies (e.g., glaucoma, eye trauma)
Refractions and prescribing glasses: these functions have largely been taken over by optometrists (who are not medical doctors)
Cataract surgery can be performed in:
Hospitals
Free-standing medical facilities, such as:
Lasik MD clinics
Canadian Centre for Advanced Eye Therapeutics Inc.
Oncologists
Oncology is the branch of medicine focused on all forms and stages of cancerous tumours.
It encompasses the development, diagnosis, treatment, and prevention of cancer.
An oncologist is a medical professional specializing in the care and treatment of individuals with cancer.
Due to the highly specialized nature of cancer treatment, oncologists may focus on specific areas such as:
Radiation therapy
Chemotherapy
Gynecological oncology
Surgery
Oncologists typically practice in large hospitals or medical centres that concentrate on cancer treatment.
They also offer ongoing care to patients in hospices and related facilities
Psychiatrists
Psychiatrists specialize in mental illness and emotional disorders.
Common disorders treated include:
Depression
Bipolar disorder
Schizophrenia
Obsessive Compulsive Disorder (OCD)
Borderline personality disorder
Bulimia
Anorexia nervosa
Personal stress issues
As medical doctors, psychiatrists can:
Order laboratory and diagnostic tests
Prescribe medicine
Unlike psychologists, psychiatrists:
Are not limited to non-medical interventions
Do not perform surgical procedures
Geriatric psychiatry is emerging as a specialized field.
Physiatrists
Physiatrists: Medical doctors specializing in physical and rehabilitative medicine.
Collaborate closely with other health care providers:
Physiotherapists
Occupational therapists
Geriatricians
Common patients include:
Stroke victims
Accident victims
Postsurgical patients
Comprehensive care aims to:
Restore the patient to their maximum level of function.
Family involvement is crucial in the restorative and rehabilitative process due to the long and arduous nature of treatment.
Other professionals who may participate in the health care team include:
Social workers
Psychologists
Psychiatrists.
Radiologists
Radiologist: A physician with additional training in imaging techniques.
Specializes in the use and interpretation of imaging techniques to diagnose and treat disease.
Primarily acts as a consultant to other physicians.
May also participate in the planning of patient care.
Typically found in large diagnostic centres, which can be:
Hospital-based
Respirologists
Respirologists (also known as pulmonologists):
Medical doctors specializing in the diagnosis and treatment of lung diseases.
Common conditions treated include:
Asthma
Emphysema
Pneumonia
Perform tests to evaluate how well a person is breathing.
May utilize procedures such as bronchoscopy to diagnose breathing problems.
Surgeons
Surgeons complete a surgery residency in their field of choice, typically lasting 4 years or more after finishing medical school.
A general surgeon undergoes a series of rotations through various specialties.
General surgeons are qualified to perform a wide range of procedures, primarily concerning the gastrointestinal tract.
Many general surgeons continue to specialize further in areas such as gynecology, neurosurgery, or cardiovascular surgery.
A surgeon’s scope of practice can vary based on:
Experience
Specialty training
Level of comfort with the specific type of surgery requested.
Nurses
Many agree that the nurse, with skills across several disciplines, remains the backbone of the health care system in hospitals, primary care settings, and in the community.
Multiskilled and flexible, with a broad knowledge base, nurses frequently assume responsibilities typically assumed by other members of the health care team.
Example Responsibilities:
When a respiratory therapist is not available, the nurse may do inhalation treatments or set up oxygen for a patient.
When a physiotherapist is unavailable, the nurse ambulats a patient and supervises their related exercises.
When the chaplain is not available, the nurse provides counseling and comfort to the patient and their loved ones.
In the absence of a clinical secretary, the nurse may also take on administrative responsibilities for the patient care unit.
Registered Nurses
Bachelor Degrees: All Canadian jurisdictions except Quebec require bachelor degrees in nursing (BN or BScN) to enter the profession.
Duration of Degrees: Nursing degrees can be completed in 2, 3, or 4 years; accelerated (2-year) programs are available across Canada.
Regulatory Body: The related regulatory body in each province or territory ensures that individuals seeking to practice as nurses meet designated levels of competence.
National Examination: Graduates in all jurisdictions except Quebec must write a national examination, known as the NCLEX-RN, which was introduced in 2015 to replace the Canadian Registered Nurse Examination (CRNE).
Examination Administration: The NCLEX-RN exam is administered by the National Council of State Boards of Nursing (NCSBN).
Additional Examinations: Some jurisdictions may require additional examinations for applicants.
Quebec Requirements: In Quebec, applicants must pass a provincial examination and a Language Proficiency Licensure Examination administered by the Office Québécois de la Langue Française. This is in accordance with Article 35 of the Charter of the French Language.
Ontario Requirements: Applicants in Ontario must also write a jurisprudence examination, testing knowledge of provincial nursing and health care legislation.
Postgraduate Education: Postgraduate and ongoing educational opportunities for RNs vary by province and territory, with specialties such as critical care, emergency nursing, community health nursing, hospice and palliative care, and perinatal and women’s health.
Complex Responsibilities: RNs usually assume the most complex components of nursing care and various leadership roles, both clinical and administrative.
Employment Areas: Many hospitals and other facilities employ RNs only in specific areas like intensive care units, where their skills in assessment and decision making are critical.
Workforce Trends: The number of RNs practicing in Canada dropped by 0.3% between 2014 and 2015, but increased by 2.2% between 2014 and 2016. In 2015, 95.6% of RNs/NPs were working within the profession.
Full-Time Employment: Just over 60% of RNs were employed full-time (Canadian Institute for Health Information, 2016).
Advance Practice Nurses There are two categories of advanced practice nurses recognized in Canada, nurse practitioners, and clinical nurse specialists:
Nurse Practitioners
Nurse Practitioners (NPs):
Registered nurses with advanced training and skills (RN Extended Class).
Authorized to practice in an expanded role with skills and responsibilities once reserved for primary care physicians.
Able to autonomously diagnose and treat health conditions.
Can order and interpret laboratory and diagnostic tests.
Authorized to prescribe a wide range of medications, including controlled substances (e.g., methadone in British Columbia).
Incorporate health education, disease prevention, and health promotion in treatment plans.
Can perform specific controlled acts and activities that other nurses cannot by law.
Educational Requirements:
Approximately 28 postgraduate facilities offer NP programs in Canada, mostly at masters and postmasters levels.
Many NP programs funded by provincial/territorial governments.
To obtain a license, individuals must be registered and in good standing with their regulatory body in the relevant jurisdiction.
Registration Exam:
Requirements vary among provinces and territories.
Three broad streams (or specialties) available for practice: adult, family (or primary health care), and pediatrics.
Some jurisdictions also include neonatology as a specialty.
Specialty candidates must write an examination specific to their chosen area.
Quebec has different specialties, including cardiology and nephrology.
British Columbia and Quebec have a clinical examination, known as objective structured clinical exams.
Other jurisdictions typically require only written exams.
Licensing and Competencies:
NP competencies vary by province and territory in accordance with regional legislation.
NPs must renew their license yearly, usually involving:
Practicing a minimum number of practice hours.
Participation in quality-assurance programs and ongoing education.
Practice Settings:
Include primary care and community settings, hospitals under specialty designations (e.g., pediatrics, cardiology), and emergency departments.
In 2016, NPs had the **highest full-time
Clinical Nurse Specialists
Clinical Nurse Specialists (CNSs) are nurses with:
a master’s or doctoral degree in nursing
wide-ranging nursing knowledge and skills
clinical experience in a specialty area (e.g., cardiology, oncology, mental health, geriatrics, neonatology)
Typically hold leadership positions
Roles include:
Clinicians
Consultants
Educators
Researchers
Contributions to healthcare include:
Promoting evidence-based practices
Ensuring continuity of care
Enhancing patient experiences
Improving treatment and health care outcomes
Note: CNS is not a protected title.
Registered Psychiatric Nurses
Registered Psychiatric Nurses (RPNs) are recognized as a separate regulated health profession in Western Canada (Manitoba, Saskatchewan, Alberta, British Columbia, and Yukon).
They form the largest body of mental health care professionals in Western Canada.
RPNs focus on:
Mental wellness and developmental wellness, using a holistic approach that includes mind, body, and spirit.
Address mental illness, addictions, and substance abuse.
Consider the physical components of health within the overall health context and life situations of individuals.
RPNs apply concepts from biopsychosocial and spiritual models of wellness integrated with cultural norms to provide holistic care.
They collaborate with a variety of other health care providers and work with mental health and community organizations.
Practice settings for RPNs include:
Crisis stabilization units.
Forensic assessment units.
Hospitals.
Community health settings.
Academic facilities.
Education for RPNs is:
Offered at the degree level, unique to Western Canada.
Focused on both medical and surgical nursing skills as well as specific skills related to mental health.
The last intake into the diploma program was in January 2016.
The national organization for RPNs is the Registered Psychiatric Nurse Regulators of Canada (RPNRC), which is an incorporated virtual organization.
The organization consists of nearly 5600 members, including formal regulatory bodies:
College of Registered Psychiatric Nurses of Alberta, British Columbia, Manitoba, and Saskatchewan.
In the Yukon, regulation is overseen by the Ministry of Community Services.
According to the Canadian Institute for Health Information (CIHI), between 2015 and 2016:
94.8% of RPNs
Licensed Practical Nurses
To become a Licensed Practical Nurse (LPN), known as a Registered Practical Nurse (RPN) in Ontario, the following steps are required:
Completion of High School or an equivalent educational credential.
2-Year Diploma Program: Must be completed at a community or private college.
After completing the program, all graduates are required to:
Pass the Canadian Practical Nurse Registration Examination (CPNRE) for provincial or territorial registration.
Use the professional designation after obtaining registration.
The skill set and scope of practice for LPNs have significantly expanded in recent years:
LPNs now perform many skills and responsibilities that were previously limited to registered nurses.
Their skill set includes:
Performing dressings on wounds.
Dispensing medications to patients.
In some facilities, they may take charge of units.
Practical nurses work in collaboration with:
Registered Nurses (RNs).
Other members of the health care team to provide patient care.
LPNs are found in:
Almost all practice settings and the community.
According to the Canadian Institute for Health Information (CIHI) in 2016:
89.4% of LPNs were active in the profession, but less than half were employed full time.
Physician Assistants
Physician Assistants (PAs) are academically prepared health care providers who work directly with or under the direction of a physician.
Their responsibilities are typically outlined in a formal contract between the PA and the physician(s), which may sometimes include the facility where they work.
The scope of practice for PAs includes:
Interviewing patients
Health teaching
Performing physical examinations
Conducting selected diagnostic tests
To become a PA, a candidate must have a Bachelor of Science degree.
Certification is granted upon successful completion of an entry-to-practice examination following a 2-year Canadian Medical Association-accredited program.
Training programs for PAs are available in various locations, including one offered by the Canadian Armed Forces Medical Services School in Borden, Ontario, which trains for the military; civilian programs are limited to selected jurisdictions.
PAs are regulated by the Provincial College of Physicians and Surgeons in Alberta, Manitoba, and New Brunswick.
The practice terms for PAs vary in other jurisdictions; for instance, in Ontario, the profession is currently unregulated.
In Ontario, PAs can work under the Designated Medical Act, only under the direction of a physician.
Importantly, physician assistants cannot practice independently.
Pharmacists
Licensed pharmacists play a crucial role in dispensing medications based on prescriptions.
They serve as experts in their field, providing valuable information regarding medications to health care teams.
Physicians often rely on pharmacists for advice about current prescription drugs and potential interactions.
Patients look to pharmacists for guidance on how to take medications, understanding their risks, and recognizing adverse effects.
In many jurisdictions, provincial or territorial plans financially support pharmacists to review medication profiles periodically, provide advice, and refer patients to their physicians when necessary.
To practice as a pharmacist, one must:
Earn a bachelor’s degree in pharmacy.
Complete an internship.
Pass a national board examination through the Pharmacy Examining Board of Canada.
Pharmacists' roles are expanding to include tasks such as:
Administering flu shots.
Providing funded information sessions and conducting medication reviews with patients.
They are recognized as experts in medication management.
Prescribing responsibilities may vary across regions:
Most can renew or prescribe a limited number of medications.
Alberta allows for the independent prescription of certain controlled drugs (those with a high potential for addiction) under specific conditions.
Other provinces (e.g., Saskatchewan, New Brunswick) do not allow therapeutic substitutions for prescribed medications.
Pharmacists in most jurisdictions, except Quebec and certain territories, are authorized to administer designated vaccines (e.g., travel and flu vaccines).
Many jurisdictions (e.g., British Columbia, Alberta) permit pharmacists to write prescriptions under specific guidelines, including Ontario where they can prescribe certain smoking-cessation drugs.
Since September 2013, Quebec pharmacists have had the authority to:
Write prescriptions
Extend existing prescriptions
Adjust medication doses
Order and interpret laboratory tests.
In some provinces (e.g., Manitoba, Alberta), pharmacists can also order designated lab tests, with pending approvals in other jurisdictions.
They can modify drug dosages or formulations in all areas except the territories.
The overarching goal of expanding pharmacists' responsibilities is to alleviate the workload on doctors and clinics, while providing Canadians with more accessible front-line services.
Midwives
Midwives provide prenatal care (before the baby's birth) and postpartum care (after delivery) for up to 6 weeks post-birth.
Delivery options include:
At the patient’s home
In a birthing centre
In the hospital
Midwives must refer a mother to a physician (usually an obstetrician) if:
Her pregnancy becomes high-risk
There are signs of problems during any phase of the pregnancy, labour, or delivery (e.g., placenta previa, multiple pregnancy).
In some jurisdictions, midwives can provide prenatal care and collaborate with physicians until the time of, and after delivery.
Midwifery is licensed in most jurisdictions in Canada.
In New Brunswick, the first midwife was licensed in early 2017.
To register as a midwife in New Brunswick, the midwife must:
Meet provincial standards
Be hired by the New Brunswick Regional Health Authority.
Once registered, a midwife can work anywhere in New Brunswick.
Provincial regulations for midwifery are determined by the Midwifery Council of New Brunswick.
Licensing for midwives in Prince Edward Island is currently pending.
Midwifery remains an unrecognized profession in the Yukon Territory; however, the Community Midwifery Association of Yukon (CMAY) was founded in January 2015 to support its introduction.
Midwifery regulations in Newfoundland were passed in April 2016 and came into effect on September 30 of the same year.
Optometrists and Opticians
Optometrists:
Typically obtain an undergraduate degree in mathematics or science.
Complete a 4-year university program in optometry at one of Canada’s two schools:
Waterloo, Ontario
Montreal, Quebec
Minimum requirement for entry: 3 years of undergraduate preparation, preferably in science.
Graduates are awarded a Doctor of Optometry degree.
Must be licensed by their province or territory to practice.
Skilled in assessing eye function and conditions.
May prescribe selected medications (topical and oral) for various eye conditions such as:
Bacterial or viral eye infections
Allergic conjunctivitis
Glaucoma
Eye drops for dilation during examination.
Optometrists also prescribe glasses and contact lenses as needed.
Most work in group or solo practices.
Opticians:
Complete a 2- or 3-year college program, often with a practical component.
Can fill prescriptions for eyeglasses or contact lenses.
Responsibilities include:
Fitting glasses
Helping patients select frames
Organizing the grinding and polishing of lenses
Cutting and edging lenses to fit frames.
Conduct health instruction related to contact lenses and glasses, explaining options like lens coating and bifocal lenses.
May work independently or collaborate in a larger centre
Osteopathic Physicians
Osteopathy: A holistic, manual approach to diagnosis and treatment of disease.
Focus on the musculoskeletal system and its relationship with the body's self-healing and self-regulating capabilities.
Practiced Worldwide: While osteopathy is practiced in many countries, it remains a nonregulated profession in Canada.
Training Standards: Set by the World Health Organization (WHO), which describes:
Two types of training:
Individuals without a health background must complete a 4-year university program with clinical training.
Individuals with a health care background follow a modified training program.
Osteopathic Physicians:
Individuals trained in the United States and holding a medical degree from an American Osteopathic Association-approved university.
Their qualifications are equivalent to medical doctors and may practice in Canada if they complete provincial/territorial requirements.
Educational Institutions: Numerous schools of osteopathy in Canada graduate students eligible to work as osteopathic manual practitioners or therapists.
Lack of Regulation: As a nonregulated profession, there is no governing body that:
Provides oversight or sets standards of education and practice.
Protects patients from unqualified practitioners.
Title Protection: Practitioners cannot legally call themselves osteopaths or osteopathic doctors in Canada; these titles are protected in the United States.
Insurance Coverage: Some insurance companies may cover osteopathy services if the practitioner graduated
Podiatrists (Chiropodists)
The term podiatrist is used internationally for foot specialists.
In Canada, only Ontario uses the term chiropodist.
Podiatrists specialize in:
Diagnosis, assessment, and treatment of foot disorders.
Treatment of sports injuries, foot deformities (related to aging and misalignments), infections, and general foot conditions such as calluses, corns, ingrown toenails, and warts.
Scope of practice includes:
Performing specified foot-related surgical procedures.
Administering injections to the feet.
Prescribing medications, including nonsteroidal antiinflammatory drugs and antibiotics, depending on the jurisdiction.
Podiatrists refer patients to surgeons or other doctors when necessary.
The chiropody/podiatry program in Canada is offered only at the Michener Institute in Toronto.
Quebec has a podiatry program, but students must complete 1 year of training in New York.
Training is also available in the United States, the United Kingdom, and Australia.
Practice requirements and scope of practice vary across jurisdictions.
In jurisdictions without a regulatory body, there are no standards of practice, allowing anyone to claim the title of podiatrist.
Practice settings include:
Health care facilities
Clinics
The community
Primary care reform groups
Personal Support Workers
Most jurisdictions recognize a category of health care workers, providing basic care and carrying out auxiliary duties for patients.
Titles for this role vary, including:
Personal Support Worker (PSW)
Health Care Aide
Health Care Assistant
Continuing Care Assistant (used in Nova Scotia)
Health Care Support Worker (common in British Columbia)
Home Care Support Worker
Resident Care Aide
Orderly
Health Care Attendant
Patient Service Associate
This category of caregiver is not regulated and may or may not be categorized as part of allied health.
Educational requirements vary:
Certificate programs (approximately 1 to 1.5 years) are most common, with some components available online.
British Columbia and Ontario offer the largest number of certificate programs, distributed between public and private institutions.
Training includes both classroom and clinical components.
In Nova Scotia, community care assistants must:
Have a certificate from a prescribed program from a community college
Write a provincial examination in order to work in long-term care facilities or in-home care.
Additional training:
Individuals can take a course to administer medications to stable residents under the supervision of a Registered Nurse (RN) or Licensed Practical Nurse (LPN).
Work settings include:
Long-term care facilities
Home care organizations
Adult day care programs
Seniors' residences
Group homes under the direction of other health care team members
Other less common practice settings:
Hospitals
Clinics
Industry
**Interdisciplinary primary care practices
Psychologists
Education: Psychologists graduate from university programs, completing a bachelor's, master's, or doctoral degree.
Licensing: To practice psychology in Canada, psychologists must be licensed by the regulatory body in the province or territory where they work.
Work Settings: Psychologists primarily work as clinicians in various environments, including:
Hospitals
Academic facilities
Clinics
Primary care facilities
Correctional facilities
Private practice
Treatment Focus: They work with individuals and families to treat emotional and mental disorders, primarily through counseling.
Assessment: Psychologists administer noninvasive written and practical tests, including:
Personality tests
Intelligence tests
Assessment tests for Attention Deficit Disorder (ADD)
Diagnostic tests for early stages of Alzheimer's disease or dementia.
Limitations: Psychologists, being non-medical doctors, do not have the authority to:
Prescribe medications
Perform medical procedures
Order lab or diagnostic tests.
Collaboration: Psychologists often work in collaboration with psychiatrists for more effective and ongoing patient treatment.
Insurance Coverage: Private insurance usually covers a specified number of visits to a psychologist; however, most provincial and territorial plans do not offer this coverage.
Speech-Language Pathologists and Audiologists
Speech-Language Pathologists (SLPs):
Experts in disorders of human communication.
Responsible for assessing and managing a diverse range of conditions, including:
Issues with swallowing and feeding.
Stuttering and delays in speech.
Social communication difficulties and literacy issues.
Common practice settings encompass:
Hospitals.
Long-term care and mental health facilities.
Research and academic institutions (such as schools and universities).
Group homes, community settings, and private practice.
Audiologists:
Specialize in addressing issues related to sound, hearing, deafness, and balance.
Provide essential services such as:
Ongoing education and diagnostic services.
Creation and management of detailed treatment plans for individuals of all ages.
In most jurisdictions, audiologists possess the ability to prescribe and fit hearing aids and other auditory devices.
Practice settings are comparable to those of SLPs, with the inclusion of industrial environments.
Educational Requirements:
The minimum qualification for Speech-Language Pathologists and **Audiologists master’s degree in the relevant course of study.
Communications Disorders Assistant
Communications Disorders Assistants (CDAs) work with, or under the direction of:
Speech-Language Pathologists
Audiologists
Responsibilities include:
Assisting clients to communicate effectively
Supporting clients in utilizing alternative forms of communication
Scope of practice encompasses:
Initiating and carrying out diagnostic tests, such as audiology screenings
Assisting with treatments
Providing health teaching
Educational Requirements:
Completion of a graduate certificate
An undergraduate degree or diploma in a related field, with options including:
Linguistics
Early childhood education
Social work
Educational assistants
Respiratory Therapists
Becoming a Respiratory Therapist (RT)
To become a respiratory therapist (RT), one must complete an accredited RT program.
Duration:
College programs: 3 years in length.
University programs: 4 years in length.
The Canadian Society for Respiratory Therapists (CSRT) is the national professional association for respiratory therapists and serves as the certifying body for RTs in nonregulated jurisdictions.
In regulated provinces, provincial regulatory bodies oversee the certification of RTs.
To obtain the RT designation and be licensed to practice in Canada, graduates must:
Write the national certification examination.
Meet designated registration criteria from the CSRT and respective regulatory authorities.
Role and Responsibilities of Respiratory Therapists
Expertise: RTs specialize in caring for individuals with acute and chronic cardiorespiratory disorders.
Settings: RTs perform health-related functions both in and out of hospital settings.
Hospital Tasks
RTs are essential in the hospital setting, providing evaluation, treatment, and support for:
Inpatients.
Outpatients.
Particularly vital in critical care areas such as:
Emergency Departments (ED).
Intensive Care Units (ICUs).
Advanced life support management for patients with cardiopulmonary problems (e.g., patients on respirators).
Emergency Response
Equipped with advanced skills, RTs:
Respond to emergencies, such as cardiac and respiratory arrests.
Are trained to intubate patients, a complex procedure that involves inserting a tube into the airway to facilitate the use of a ventilator.
Initiate the use of ventilators.
Patient Transfer and Delivery Room Support
RTs often participate in the transfer of critically ill patients between facilities or from an accident scene to a hospital.
They are also present in the delivery room when doctors suspect a baby may develop respiratory problems.
Diagnostic Testing and Treatment
Conduct diagnostic testing, including:
Arterial blood gases.
Pulmonary function tests.
In the hospital setting, responsible for:
Setting up oxygen therapy.
Administering inhalation treatments.
Wider Practice Settings
RTs also work in:
Medical centres.
Clinics.
Complex continuing care and rehabilitation facilities.
The community
Physiotherapists
Physiotherapists (PTs): Regulated health care professionals who:
Graduate from university at the master’s level.
Must pass a national exam to enter professional practice.
Essential Role: PTs are a crucial component of the primary care team who:
Work with individual patients to:
Limit and improve physical impairments and disabilities.
Prevent and manage pain associated with:
Acute diseases.
Chronic diseases.
Injuries.
Work Settings: PTs operate in diverse environments, including:
Health care facilities.
Clinics.
Community settings (e.g., home care).
Private practice, often in collaborative groups.
Specializations: Some PTs focus on specific areas such as:
Geriatrics.
Sports medicine.
Pediatrics.
Insurance Coverage: Physiotherapy services are typically:
Covered under specific conditions and limited time frames in most jurisdictions.
Many private insurance plans also offer some coverage.
Occupational Therapists
Occupational Therapists (OTs): Members of a regulated profession providing support, direction, and therapies to individuals in need across various aspects of everyday life.
Assist with recreation, work, and activities of daily living.
Help individuals learn or relearn important activities such as:
Caring for themselves or others.
Maintaining their home.
Participating in paid and unpaid work.
Engaging in leisure activities.
Patient Demographics:
Work with patients facing difficulties due to:
Accidents
Disabilities
Diseases
Emotional or developmental problems
Aging
Access to Services:
In most jurisdictions, individuals can visit OTs without a referral.
The decision to see an OT is often made jointly with a primary care provider.
Work Settings: OTs operate in diverse environments including:
Hospitals
Private homes (typically through provincial or territorial home care programs)
Schools
Long-term care facilities
Mental health facilities
Rehabilitation clinics
Community agencies
Public or private health care offices
Employment evaluation and training centres
Educational Requirements:
The minimum educational requirement to practice as an OT in Canada is a baccalaureate degree in occupational therapy.
All OTs must be registered with their provincial or territorial college.
After passing the national certification exam, OTs can practice anywhere in Canada.
Physiotherapy Assistants and Occupational Therapy Assistants
Programs Offered: Physiotherapy Assistant (PTA) and Occupational Therapy Assistant (OTA) programs are provided at numerous community and private colleges across Canada.
Program Length: Most programs are typically 2 years long and integrate both disciplines.
Single-Discipline Programs: Some private colleges offer individual programs focusing solely on PTAs.
Program Example: For instance, the Southern Alberta Institute of Technology provides a 2-year diploma in Rehabilitation Therapy Assistant, equipping graduates with skills in both OTA and PTA.
Accreditation: All programs are working towards accreditation through the Occupational Therapist Assistant and Physiotherapist Assistant Education Accreditation Program.
Collaboration: OTAs and PTAs work closely with and are directed by Physical Therapists (PTs) or Occupational Therapists (OTs) to perform rehabilitation treatments for individuals facing physical, emotional, or developmental challenges.
Work Settings: Their employment environments encompass rehabilitation centres, long-term care facilities, community settings (such as home care), physiotherapy clinics, and sports and medical clinics.
Professional Associations: In certain regions, like Alberta, there exists a professional therapy assistant association that serves PTAs, OTAs, speech language pathologist therapy assistants, and recreation therapy assistants.
Administrative Roles
Health Information Management
Health Information Management (HIM) professionals hold the designation of CHIM—Certified in Health Information Management.
They provide leadership and expertise in the management of clinical, administrative, and financial health information across various settings such as:
Hospitals
Community care
Long-term care and nursing homes
Physician offices
Clinics
Research facilities
Insurance companies
Pharmaceutical companies
The Canadian College of Health Information Management (CCHIM) administers the National Certification Examination (NCE) on behalf of the Canadian Health Information Management Association (CHIMA), representing approximately 5000 HIM professionals.
To become a CHIM, candidates must:
Graduate from a CHIMA accredited diploma or degree program available at colleges and universities across Canada.
Successfully pass the NCE, assessing entry-level competencies for qualified applicants.
Successful candidates receive:
A certificate of registration from the CCHIM
Eligibility to use the CHIM credential and the title Certified HIM Professional.
Certified CHIMA members must earn continuing professional education (CPE) credits to maintain their certification.
Conestoga College in Ontario offers a Bachelor of Health Information Sciences (BAHIS) degree and considers graduates of accredited HIM diploma programs for advanced standing opportunities.
Detailed contact information for current CHIMA accredited programs, including distance education options, can be found on the CHIMA website.
The HIM profession has four domains of practice:
Data Quality: Involves collection, analysis, coding of health information, and quality assurance.
e-HIM: Focuses on the conversion of health records from physical to digital formats, cloud storage, and management of communication systems.
Privacy: Ensures that health information remains confidential and secure, while enforcing privacy legislation.
HIM Standards: Involves records management, documentation, and terminology standards.
HIM professionals engage in various aspects of health information lifecycles, including:
Data collection
Analysis and retrieval
Destruction of unnecessary information according to facility and legal guidelines.
When managing health records, HIM professionals facilitate:
Proper collection, access, and use of health information.
Accurate and complete health records through quantitative analysis and identification of trends (e.g., births, deaths, diseases, health care costs).
In Canada, HIM professionals are trained in six core competency areas:
Biomedical sciences
Health care systems in Canada
Health information lifecycle
Information systems and technology
Management aspects
Ethics and professional practice
Health Office Administration
Administrative Support in Health Care:
Every aspect of health care requires some level of administrative support.
Role Responsibilities:
Administrative management involves the day-to-day operations of:
Hospital units
Clinics
Physician’s offices
Requires skills such as:
Knowledge
Patience
Commitment
High level of professionalism
Job Titles:
Individuals may work under various titles including:
Medical Secretary
Medical Office Assistant
Unit Clerk
Clinical Secretary
Administrative Coordinator
Knowledge Base Requirements:
Must have sound knowledge in:
Pharmacology
Diagnostic and laboratory testing
Medical terminology
Anatomy and physiology
Disease pathophysiology
Principles of triage
Skills for Doctor’s Offices:
Clinical and administrative skills needed to:
Manage electronic health records
Schedule and triage patients
Perform provincial or territorial billing
Hospital Setting Requirements:
Staff must navigate complex computer software systems (e.g., Meditec) for:
Data-entry responsibilities
Understanding hospital policies and procedures
Personal Attributes:
Essential qualities include:
Ability to multitask
Work efficiently under pressure
Be flexible and friendly
Empathetic and supportive
Comfortable around individuals experiencing health problems
Practice Settings:
Common environments include:
Doctors’ offices
Group practices
Specialists’ offices
All hospital units
Long-term care facilities
Regulation Status:
Health services or health office administrators are not regulated; hence:
No provincial or territorial standards exist.
Professional Organizations:
Outside of British Columbia, there are no professional organizations.
The Medical Office Assistants’ Association of British Columbia serves as an affiliated body for administrative health care providers.
The International Association of Administrative Professionals (IAAP) welcomes members from various administrative disciplines and has chapters across Canada.
Laboratory and Diagnostic Services
The field of medicine heavily relies on laboratory and diagnostic services.
Diagnoses often cannot be confirmed without laboratory or diagnostic tests.
Providers depend on laboratory tests when prescribing the correct antibiotics.
A diverse group of highly qualified individuals includes:
Physician specialists
An increasing number of technicians and technologists specializing in various areas
Numerous specialties exist within laboratory and diagnostic services, including:
Pathology
Hematology
Radiology
Most specialties in this field are regulated in each province and territory.
Alternative Practitioners
Alternative practitioners play a significant role in the health and wellness of Canadians.
Several disciplines have provincial or national organizations that provide differing levels of oversight.
The majority of these practitioners are considered unregulated, indicating that there is no legislative body that governs standards of education and practice, thus not providing adequate protection for both patients and practitioners.
There is considerable variation in educational requirements across disciplines and between provinces and territories.
Practitioners who practice acupuncture often originate from regulated professions such as chiropractic and physiotherapy.
These practitioners must meet specific criteria to be eligible to practice acupuncture.
Chiropractors are required to complete over 200 hours of clinical training.
In addition to clinical training, chiropractors must also take required courses and successfully pass examinations administered by Acupuncture Canada.
Volunteer Caregivers
Friends, family, and volunteer caregivers play a vital role in supporting ill individuals.
They work in partnership with professional caregivers, enhancing the overall care experience.
There is a current shortage of health care providers across various categories.
Many patients depend on volunteer caregivers to help bridge the gaps in their care.
The hours of care offered by these caregivers are immense and difficult to quantify.
The output of care provided by this network is unmatched, showcasing exceptional commitment.
The stress experienced by caregivers is significant, highlighting the demanding nature of their role.
This supportive network is essential, as many individuals would struggle to manage their health without it.