Immune System
Innate/Nonspecific Immunity
The immune system has two lines of nonspecific/innate defense:
- Keep pathogens out: through skin (and skin oils), mucous membranes, and acidic stomach acid
- If pathogens enter, kill them to prevent widespread infection
1. yields inflammatory response (brings blood and fighter cells to the site of infection), phagocytes, white blood cells (nonspecific destruction of pathogens) 2. bacteria can also be destroyed through lysozyme present in blood, tears, saliva (breaks cell walls) 3. extreme acidity in the stomach and also destroy many pathogens that are ingested with food or swallowed after being passed out of the respiratory tract
Phagocytes
Phagocytes: a class of cell that can eat up other things, mostly pathogens
- contains receptors that respond to foreign things. Pathogens binds to receptors and is engulfed by the phagocyte and enters the cell in a vesicle called a phagosome
- other vesicles can merge and destroy phagosomes (i.e lysosome, reactive oxygen species) and break up the pathogen
- Some of the molecules of the consumed pathogen (antigens) are then taken and attached to other proteins * in the phagocyte, its bound to the major histocompatibility complex type II (MHC II) and other membrane surfaces * The antigens are crucial to the immune system because they allow specific immune cells to know what is in the body and to come up with a specific response to the threat
- Phagocytes are also called antigen presenting cells
White blood cells/Leukocyte types
Neutrophils: most common, fast, and abundant- bacteria/fungi phagocytes
- phagocytic cells that are also classified as granulocytes because they contain granules in their cytoplasm.
- Granules are very toxic to bacterial and fungi, phagocyting results in pus formation
- amoeboid motility, chemotaxis
Macrophages: phagocyte debris and microorganisms; amoeboid motility; chemotaxis
Mast Cells: important for wound healing and defense against pathogens via inflammatory response
- found in mucous membranes and connective tissues
- release cytokines and granules when activated to create inflammatory cascade * inflammatory cascade mediated by histamine and causes blood vessel dilation to increase blood flow and cell trafficking to infection area * cytokines act as a messenger service to alert other immune cells
Eosinophils: granulocytes that attack multicellular parasites, can also phagocyte
- use of toxic proteins and free radicals also causes tissue damage during allergic reactions, so activation and release of toxin is heavily regulated
- found in many locations including thymus, lower GI tract, ovaries, uterus, spleen, and lymph nodes
Basophils: granulocytes that attack multicellular parasites.
- can also release histamine like mast cells (key player in allergic response like mast cells)
Natural Killer (NK) Cells: do not directly attack pathogens but destroys infected host cells to stop spread of infection.
- antigen presentation and expression of specific receptors identify compromised cells in need of destruction
Dendritic cells: antigen-presenting cells that are located in tissues and can contact external environments through the skin, inner mucosal lining of the nose, lungs, stomach, and intestines
- located in tissues that are common points for initial infection, they identify threats and act as messengers for the rest of the immune system via antigen presentation
- most effective at eliciting adaptive immune response
\
The Complement System
Also called the complement cascade, this is a mechanism that complements the other aspects of the immune response.
Mostly acts as part of the innate immune system, but it can work with adaptive immune system if needed
Made of a variety of proteins that, when inactive, circulate the blood. When activated, these proteins come together to initiate the complement cascade:
- Opsonization: foreign particles are marked for phagocytosis.
1. all pathways require n antigen to signal that a threat is present. 2. Opsonization tags infected cells and identifies circulating pathogens expressing the same cells
- Chemotaxis: attraction and movement of macrophages to a chemical signal
1. uses cytokines and chemokines to attract macrophages and neutrophils to the site of infection, ensuring that pathogens in the area will be destroyed 2. by bringing immune cells to an area with identified pathogens, it improves likelihood that the threats will be destroyed and the infection will be treated.
- Cell Lysis: destruction of the membrane of a cell
1. proteins of the complement system puncture the membranes of foreign cells, destroying the integrity of the pathogen 2. causes foreign cells or pathogens to weaken their ability to proliferate, which can stop the spread of infection
- Agglutination: uses antibodies to cluster and bind pathogens together
1. allows for the cells of the immune system to mount an attack and weaken the immune system. 2. other innate immune system cells continue to circulate throughout the body in order to track down any other pathogens that have not been clustered and bound for destruction
Adaptive Immune Response: Humoral vs Cell Mediated
Adaptive immunity is activated by exposure to pathogens, and uses immunological memory to learn about the threat and enhance the immune response accordingly
- much slower to respond to threats and infections than the innate immune response, which is primed and ready to fight at all times
Adaptive immune response uses B and T cells
- Lymphocytes (another type of leukocyte) can be divided into B lymphocytes and T lymphocytes * B-cells are produced in the bone marrow and participate in humoral response * T-cells start off in the bone marrow but mature in the thymus and participate in cell-mediated responses
Humoral immunity is a specific type of protection by proteins in the plasma called antibodies (Ab) or immunoglobulins (Ig)
- someone who has never been exposed to a certain disease before can gain humoral immunity through administration of antibodies from someone who has been exposed and survived the same disease
Cell mediated refers to the fact that the response was carried out by cytotoxic cells (T cells)
- someone who has not been exposed to a disease can gain cell-mediated immunity through the administration of T cells from someone that has been exposed and survived the same disease

\
Other Cell Types and Antibodies
B-Cells
B cells have many protein complexes on their surface called membrane bound antibodies (aka immunoglobulins)
- each b-cell has one type of membrane bound antibodies on it. There is a variable portion of antibody structure that is different between b-cells
- during development, potential self-responding combinations, for your own cells are weeded out
Combinations arise even if antibodies come from the same b-cells with the same DNA because recombination occurs during b-cell formation
- this ensures that some b-cell will bind to a foreign pathogen even if its never been seen before.
- epitope: the part of the pathogen/bacteria that attaches to an antibody
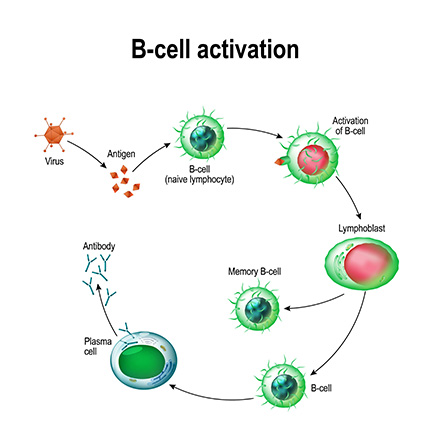
- as soon as the epitope is bound, the b-cell activates (with help of helper t-cells) and starts cloning itself repeatedly
- when a specific b-cell divides over and over again the daughter cells start to differentiate and eventually become memory cells and effector (plasma) cells * Memory cells: stay dormant within the body waiting for the same pathogen to reappear to specifically eliminate it (specific B-cells to a specific antigen and pathogen) * clonal selection: selection of b-cells with specific antigen binding * Plasma/Effector cells: antibody factories that actively produces and secretes variable antibodies that can uniquely bind to the infecting pathogens (can cause opsonization, inhibit pathogen function, or cluster pathogens together)
T-helper cells act to activate other immune cells while T killer cells assist with the elimination of pathogens
\
Helper T Cells
Also called CD4 cells
T cells mature in the thymus and are involved in the cell mediated response
Helper t-cells raises alarm to produce antibodies which disable a specific pathogen that is still floating around
Activation of helper T cells occur when they bond to the MHCII + antigen complex
- different T-cells are specific to a certain MHCII complex and certain parts of the pathogen
- Dendritic cells are the best at activating helper T-cells, especially native helper t-cells (non-effector/non-memory and have not been activated nor had anything bound to it
Once a helper T-cell is activated, it divides into many copies and starts to differentiate into:
- memory T-cells: stay stay around for many years in case the pathogen returns, which will allow for quicker alarm
- effector T-cells: release cytokines (which raise strengthens or multiplies immune response in other immune cells)
1. central role that tells both activated killer t-cells to get in gear and activated b-cells 2. effector t-cells also activate b-cells so they start proliferating and differentiating
1. variable portion of the t-cell connects to the specific virus as the b-cells that engulfed the pathogen; the combination of antigen and MHC II is the same (acts as a fail-safe mechanism)
Cytotoxic T Cells/ Killer T Cells
Also called CD8 cells
Killer T cells directly attack and destroy abnormal host cells which include
- viral-infected host cells
- cancer cells
- foreign cells such as a skin graft given by an incompatible donor
Killer t-cells bind with MHC I complexes (also with a specific variable portion), get activated (if it detects a viral protein displayed on MHC I), and differentiates and divides
- Memory: stick around in case pathogen reappears
- Effector: go on to kill any infected/mutated cells with that specific MHC I complex if they recognize * work by exocytosing perforin proteins that make holes in the membrane of the infected cell or by releasing granzymes that induce apoptosis
Professional Antigen Presenting Cells (APC) and MHC II Complexes
APC’s include macrophages and b-cells and their role is to phagocytize particles or cells and display fragments using major histocompatibility complex 2 (MHC II), which T helpers bind and recognize and activate b-cells (and stimulate proliferation of t-killer cells)
- activated mature b-cells turn into plasma cells and secrete antibodies for the specific antigen.
- explains why the primary immune system takes a week or more
Antibodies
Antibodies/immunoglobulins are specific proteins found within the plasma.
- antibodies specifically recognize and bind to microorganisms (or other foreign particles), leading to their destruction and removal from the body
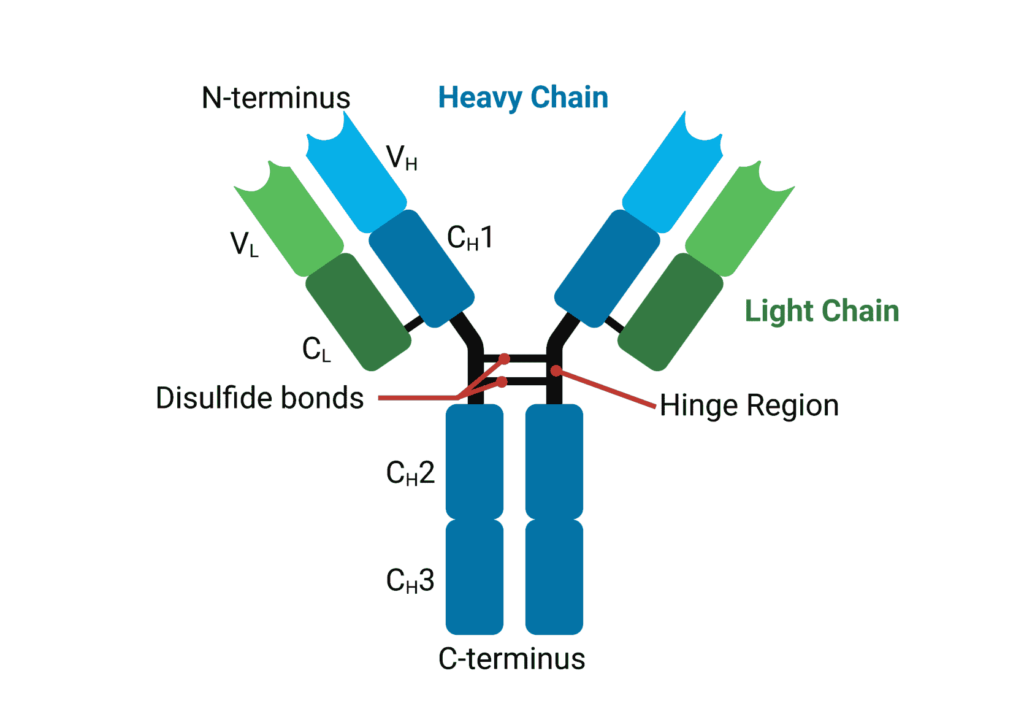
Structure:
- each antibody molecule is composed of two copies of two different polypeptides, the light chains and the heavy chains, joined by disulfide bonds * each antibody molecule has 2 regions; the constant region and the variable (antigen binding) region
There are several different classes of immunoglobulins, differentiated by their constant regions:
- IgM * found in blood and b-cell surface * involved in initial immune response; * pentameric structure in blood, monomeric structure on b-cell as antigen receptor
- IgG * located in blood * involved in ongoing immune response * most common antibody found in blood and can cross placental barrier
- IgD * located on b-cell surface * serves with IgM as antigen receptor
- IgA * located in secretions (saliva, mucus, tears, breast milk, etc.) * secreted in breast milk, helps protect newborns, dimeric structure
- IgE * located in blood * involved in allergic reactions
\
Self vs Non-self Immunity
How does your immune system know not to attack itself?
- There is no way to keep the b-cell from creating antibodies that would react to yourself, so we need to figure out the self-antibodies are and kill them (applicable for both t and b cells) * In the bone marrow, there are various proteins that the body uses that can be used to vet out self harming b-cells * body can respond and kill any b-cell that binds to anything while still in the bone marrow * Similar process occurs with T-cells in the thymus
- In the thymus, t-cells undergo two selection processes to ensure they perform properly: * Positive selection: ensures MHC restriction by testing the ability of MHCI and MHCII to distinguish between self and non-self proteins * T-cells that bind to self-MHC’s move onto the second process * T-cells that bind to non-self-MHC’s are eliminated via apoptosis * Negative selection: tests for self tolerance and tests binding capabilities to CD4 and CD8 to only bind to self-molecules presenting a foreign antigen * Elimination by apoptosis occurs if t-cells binds to self-molecule with no foreign antigens or presents with self-antigens * after selection, we are left with helper, killer, and regulatory (CD25, distinguishes self and non-self molecules- reducing risk of autoimmune disease) t-cells
Autoimmune diseases:
- occurs when the immune system attacks normal body cells or proteins
- treated with immunosuppressants
- examples include: rheumatoid arthritis, type 1 diabetes mellitus, Graves’ disease, myasthenia gravis, and celiac disease
Other Tissues Involved in Immune Response
Bone marrow: site of synthesis of all cells of the blood from a common progenitor
Lymph nodes: filters lymph and contains millions of white blood cells that can initiate an immune response for anything foreign picked up in the lymph
Spleen: filters blood and is a sit of immune cell interactions
Thymus: site of t-cell maturation
appendix and tonsils: masses of lymphatic tissue to catch pathogens, not required for survival so they can be removed if they become infected