7MNT0004 - Gut Microbiota - Week 4
Diet and the Gut Microbiota
Dr. Eirini Dimidi, RD, Reader in Nutritional Sciences, School of Life Course & Population Sciences, Faculty of Life Sciences & Medicine
What is the Microbiota?
Definition of Microbiota:
Power et al., 2014 (British Journal of Nutrition; 111: 387-402)
Walker & Hoyles, 2023 (Nature Microbiology; 8: 1392-96)
Consists of bacteria, fungi, protozoa, and viruses.
Ratio: 1:1 of microbiota cells to human cells.
Total microbiome genes: approximately 200 times the number of human genes.
What Does the Gut Microbiota Do?
Key Functions:
Metabolite Production:
Produces gases and short-chain fatty acids (SCFAs).
Impact on Immune System:
Influences the central nervous system.
Affects enteric nervous system.
Vitamin Production:
Specific Contributions:
B. infantis involved in the metabolism of tryptophan, which is linked to serotonin production (a neurotransmitter) (Backhed et al., Cell Host & Microbe 2012; Parkes et al., Am J Gastroenterol 2018).
Why is the Gut Microbiota Important?
Health Benefits:
Nutritional Supply and Energy Source:
Microbial products and activities such as SCFA production, vitamin synthesis.
Influences energy supply, gut hormones, satiety, and energy expenditure.
Cancer Prevention:
Role of lipopolysaccharides and inflammatory responses.
Importance of butyrate production & phytochemical release.
Effects of toxins and carcinogens, inflammation.

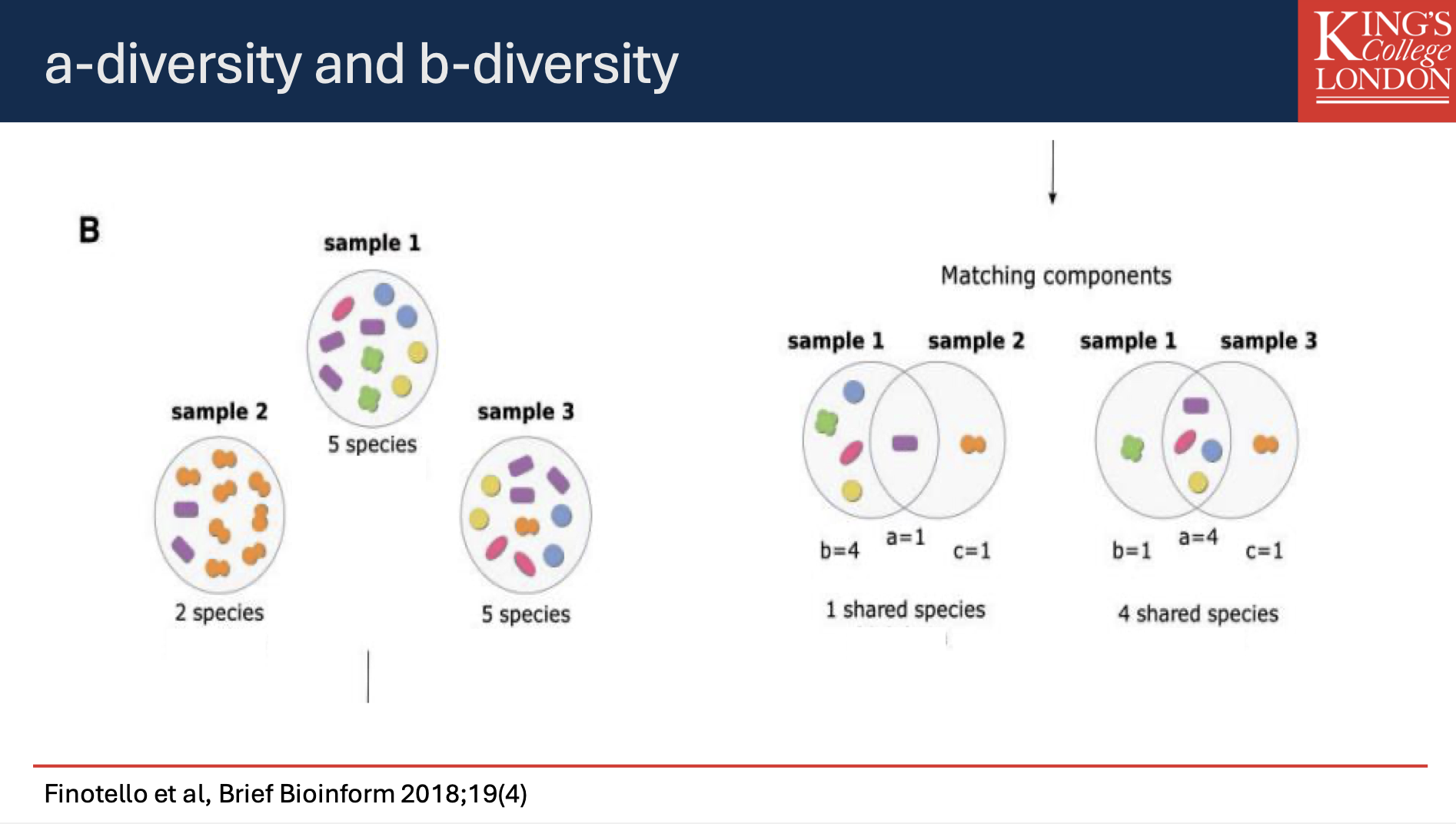
Alpha Diversity: Single sample and bacteria it consists of (Research shows that higher diversity of microbiota is better. Greater alpha diversity is associated with improved gut health and resilience against diseases, highlighting the need for a balanced microbiome.
Beta Diversity: Compares two samples and their gut microbiota composition. This is useful to assess impact of fibre in a disease.
What is a healthy microbiota?
Blackhed et al, Cell Host & Microbe 2012; Joos et al, Nat Rev Microbiol 2024
✓ Stability/resilience to changes
✓ More microbes that convert luminal compounds to beneficial byproducts (e.g. SCFA)
✓ Less microbes that convert luminal compounds to potentially harmful byproducts (e.g. carcinogens)
✓ Sufficient diversity or evenness
Disease Associations:
Obesity and Metabolic Syndrome:
Cancer promotion risk and inhibition of pathogens.
Mechanisms:
SCFA production, intestinal pH alteration, bacteriocin secretion, competition for substrates and/or binding sites.
Potential for toxins, tissue invasion, inflammation.
Impacts on Normal Gastrointestinal Immune Function:
Balance of pro-inflammatory versus anti-inflammatory signals.
Development and inflammation related to immune disorders (IBD).
Gut Motility:
Influence of metabolites (e.g., SCFA, gases) derived from non-digestible carbohydrates.
Cardiovascular Health:
Impacts lipid and cholesterol metabolism.
Specific Disease Associations:
Irritable Bowel Syndrome (IBS):
Symptoms like constipation, diarrhea, and bloating.
Cardiovascular Disease:
Flint et al., 2009 (Nature Reviews Gastroenterology & Hepatology; 9: 577-89).
What is a Healthy Microbiota?
Research Reference:
The Human Microbiome Project Consortium, 2012 (Nature)
Sample Population: 242 healthy adults.
Notable findings indicate a huge variability in bacterial communities (both between individuals and between different sites).
Aspects Evaluated:
Number of microbiota?
Composition?
Diversity?
Definition:
No singular definition of a healthy microbiome.
Diversity Metrics: Alpha-Diversity and Beta-Diversity
Alpha-Diversity (a-diversity):
Reflects the diversity within a specific sample.
Beta-Diversity (b-diversity):
Reflects the diversity between different samples.
Example:
Sample Comparisons:
Sample 1: 5 species (a=1)
Sample 2: 5 species (a=4)
Shared components.
What is a Healthy Microbiota? Additional Characteristics
Desirable Features:
Stability and resilience to environmental changes.
Higher levels of beneficial microbes that convert luminal compounds into beneficial byproducts (e.g., SCFA).
Fewer microbes producing potentially harmful byproducts (like carcinogens).
Sufficient diversity and evenness across microbial communities.
Development of the Gut Microbiota in Early Age
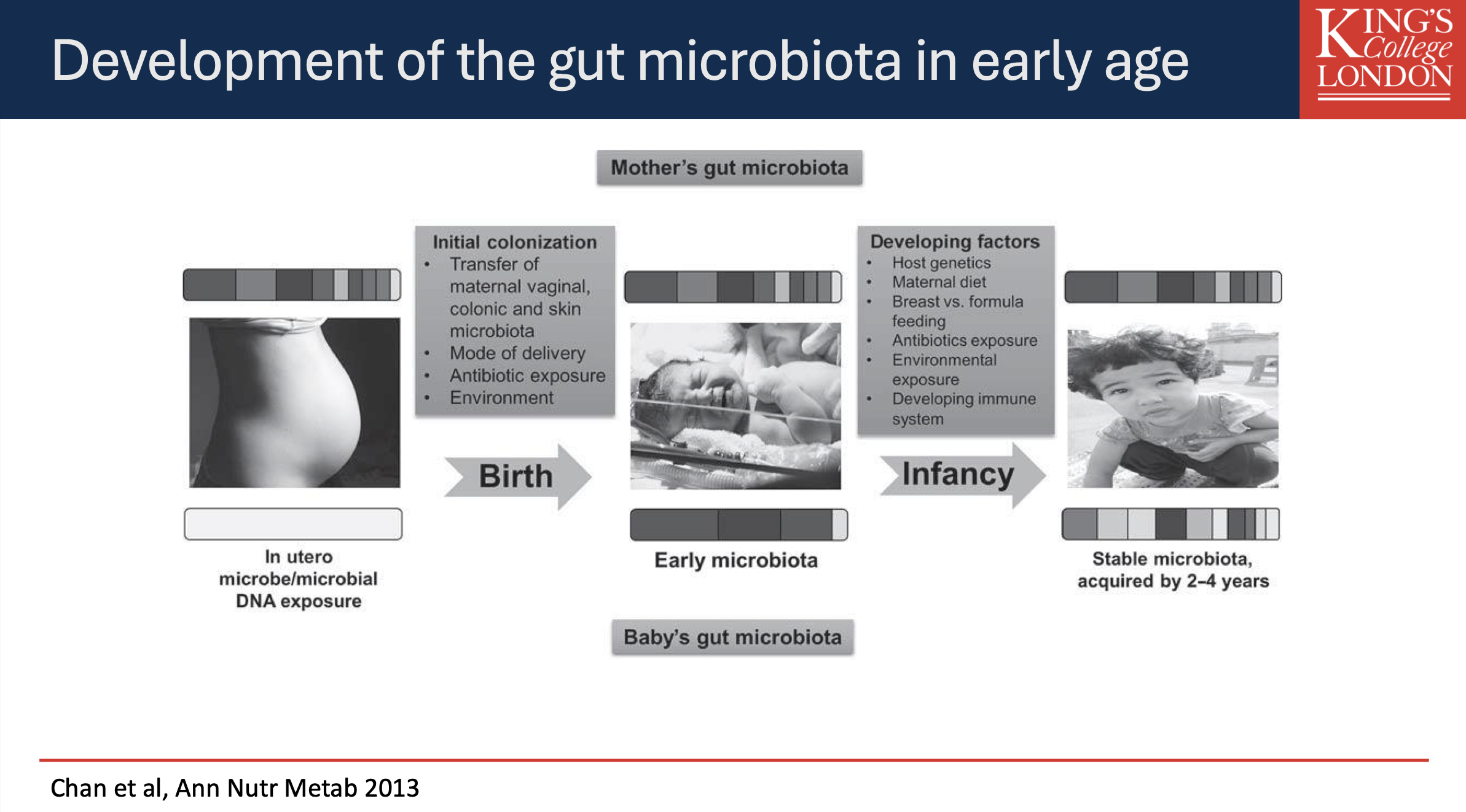
Initial Colonization:
Influences include maternal vaginal, colonic, and skin microbiota transfer during delivery.
Factors influencing early microbiota development:
Mode of delivery (vaginal vs C-section)
Antibiotic exposure
Environmental factors
Maternal gut microbiota
Maternal diet and breastfeeding vs formula feeding.
Host Genetics:
Contributes to gut microbiota establishment.
Stable Microbiota:
Generally established by the age of 2-4 years.
Life Stage | Key Factors | Microbial Impact |
|---|---|---|
Birth | Mode of delivery (Vaginal vs C-section) | Vaginal: beneficial Lactobacillus, Bifidobacterium; C-section: skin/hospital microbes |
Infancy | Breastfeeding vs formula | Breast milk promotes Bifidobacterium; formula = more diverse but less stable microbiota |
Infancy | Antibiotic exposure | Reduced beneficial bacteria, long-term effects |
Infancy/Childhood | Environment (pets, siblings, hygiene) | More exposure = greater microbial diversity |
Childhood | Solid food introduction | Transition to complex, adult-like microbiota |
Adolescence | Hormones, diet, stress | Modulates microbial balance and metabolism |
Adulthood | Diet, exercise, medications, stress | Shapes stability, diversity, and metabolic health |
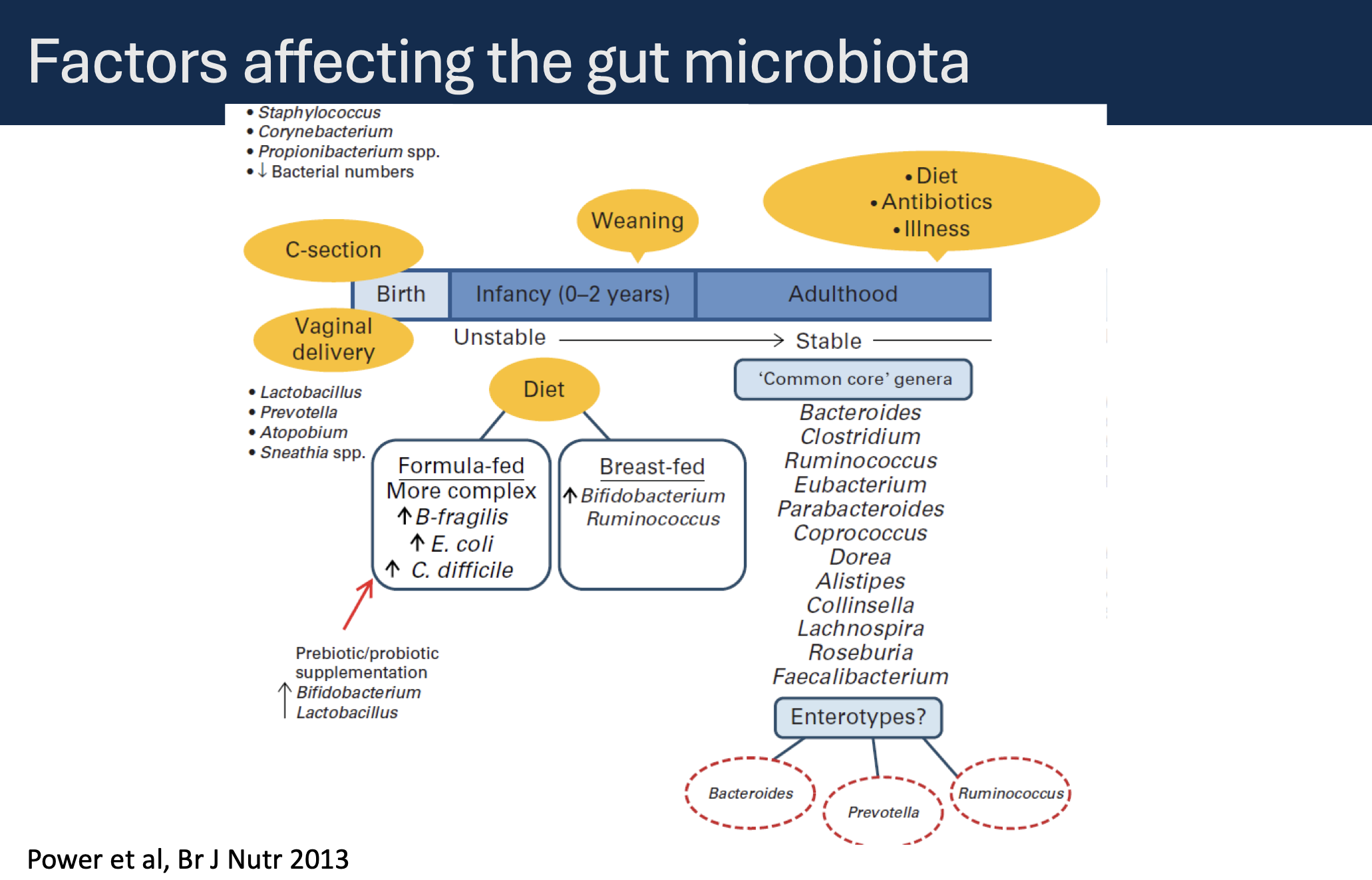
Factors Affecting the Gut Microbiota
Early Life
Birth Mode Effects:
C-section vs Vaginal delivery leads to differences in bacterial acquisition and colonization.
Diet Variations:
Breast-fed infants develop a different microbiota compared to formula-fed infants.
Environmental Exposures:
Influence on microbial communities.
Adulthood
Common Core Genera:
Key species in stable adult microbiota include:
Bacteroides
Clostridium
Eubacterium
Parabacteroides
Ruminococcus.
Changing Factors:
Illness can lead to instability in the gut microbiota.
A complex interplay of dietary habits, antibiotics, and illness further influences microbial composition.
Factors Affecting the Gut Microbiota: Disease Associations
Atherosclerosis:
Shift in microbial populations observed.
Non-Alcoholic Fatty Liver Disease (NAFLD):
Increase in Gammaproteobacteria, decrease in Erysipelotrichia.
Type 2 Diabetes:
Notable decreases in Bifidobacteria and Bacteroides, increase in Ruminococcus.
Chronic Inflammatory Conditions:
Alterations in gut microbiota linked with IBD and CRC.
Non-Digestible Compounds and Diet Impact
Access to Microbiota:
Certain dietary fibers and non-digestible compounds become available to gut microbiota, leading to shifts in microbial populations.
Research Reference:
Scott et al., Pharmacological Research 2013.
How Does Diet Affect the Gut Microbiota?
Dietary Components:
Specific carbs and fibers have different effects on microbiota, for instance:
Wheat, Oats:
Resistant starches and pectin can be fermented by specific microbiota such as Bacteroides and Ruminococcus spp.
Fermentation Byproducts:
Metabolite production leads to SCFA and other beneficial compounds.
Cross-feeding Mechanisms:
Breakdown products shared among different microbes promoting synergistic growth.
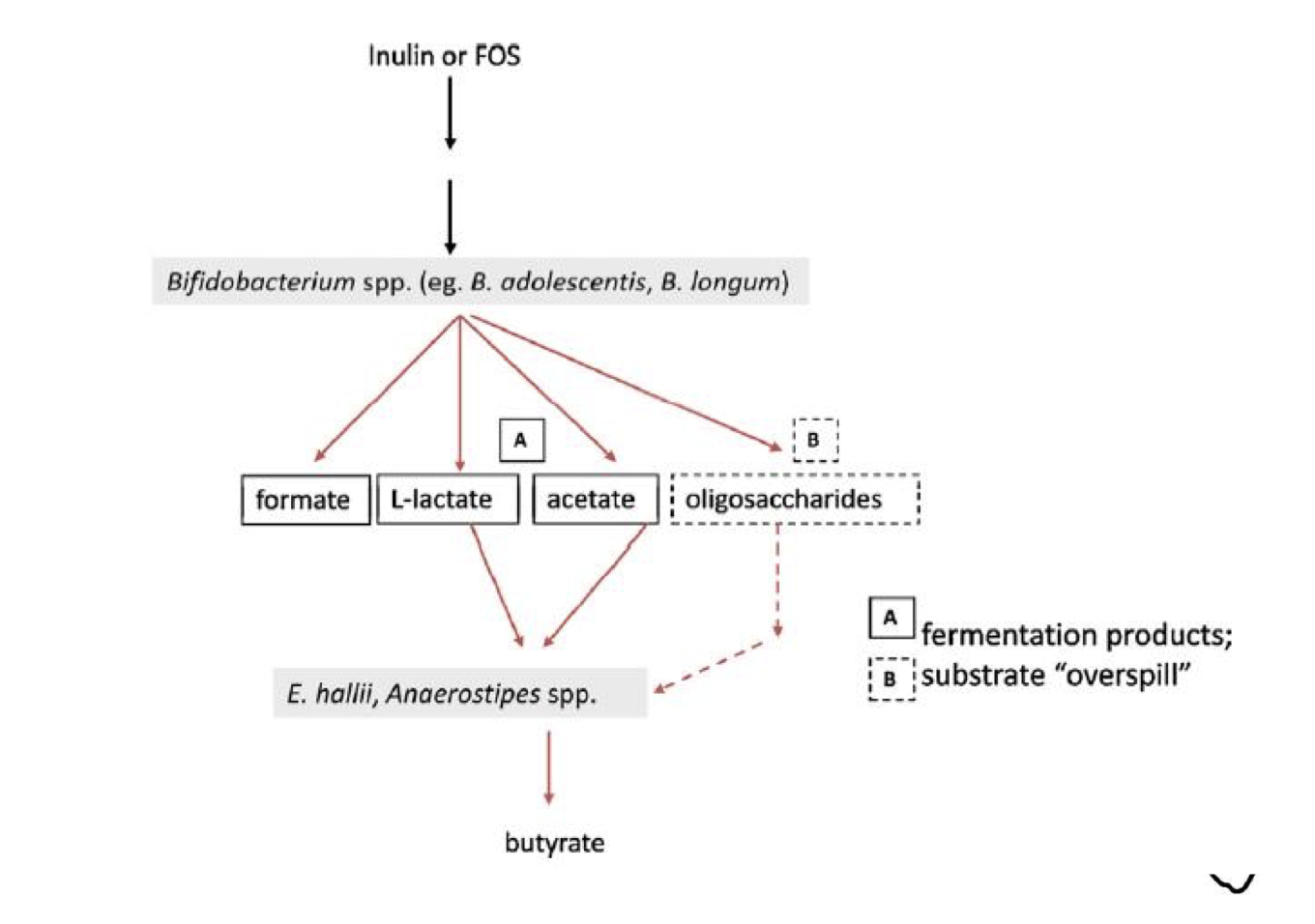
Observational Studies on Diet Impact
Short-term Dietary Composition Change:
David et al., 2013 (Nature; 505: 559-563)
Findings indicated gut microbiota returned to original structure within 2 days after diet cessation in a crossover randomized controlled trial comparing animal and plant-based diets.
Animal-based Diet:
Increased microbial β-diversity, bile-tolerant bacteria, and higher amino acid fermentation products.
Plant-based Diet:
Increased Firmicutes and carbohydrate fermentation products.

Modifying Gut Microbiota Through Diet
Dietary Interventions:
Probiotics:
Fibre:
Prebiotics:
Probiotics
Definition:
Hill et al., 2014 (Nat Rev Gastroenterol Hepatol; 11: 50-14):
“Probiotics are live microorganisms that, when administered in adequate amounts, confer health benefits to the host.”
Example:
Bifidobacterium lactis NCC2818 (genus, species, strain).
Mechanisms of Action:
Probiotics influence immune system engagement and gastrointestinal microbiota dynamics leading to:
Increased SCFA production
Modulations in neurotransmitter release and inflammatory response.
Probiotics: Effect on Gut Microbiota
Healthy Individuals
No significant effects on stool microbiota composition in terms of α-diversity, richness, or evenness compared to placebo.
Disease Context
Evidence shows specific probiotic strains can modify gut microbiota composition, especially in individuals with constipation.
Changes in SCFA levels and composition depend on specific strains and contexts.
Fibre
Mechanisms of Action:
Fibre Effects:
Promotes fermentation, stool bulking, and increases short-chain fatty acids (SCFA) like butyrate, propionate, acetate.
Changes in osmotic load, luminal pH, and gastrointestinal transit time.
Involved in decreasing inflammation and enhancing gut permeability.
Fibre: Effect on Gut Microbiota - Healthy
Various studies show different impacts of fibre on specific microbes:
Bifidobacteria (SMD 0.64, p<0.001)
Lactobacilli (SMD 0.22, p=0.02)
Faecal butyrate (borderline significant higher post-fibre intervention compared to control).
Fibre: Effect on Gut Microbiota - Disease
Systematic reviews indicate fibre supplementation benefits in chronic idiopathic constipation.
Impact varies based on type of fibre used (e.g., inulin, GOS).
Fibre definitely affects gut microbiota composition and metabolism, especially fermented forms of fibre.
Prebiotics
Definition and Effects:
Prebiotics:
As defined by Gibson et al., Nat Rev Gastroenterol Hepatol 2017: “Substrates that are selectively utilized by host microorganisms conferring a health benefit to the host.”
Prebiotics: Effect on Gut Microbiota - Healthy
Evidence supports that various accepted prebiotics positively influence gut microbiota:
Notable increases in Bifidobacteria and Lactobacilli.
Prebiotics: Effect on Gut Microbiota - Disease
Research indicates prebiotic supplementation may provide benefits, but correlation with clinical effectiveness requires further investigation.
Change in microbiota composition does not always lead to clinical effectiveness.
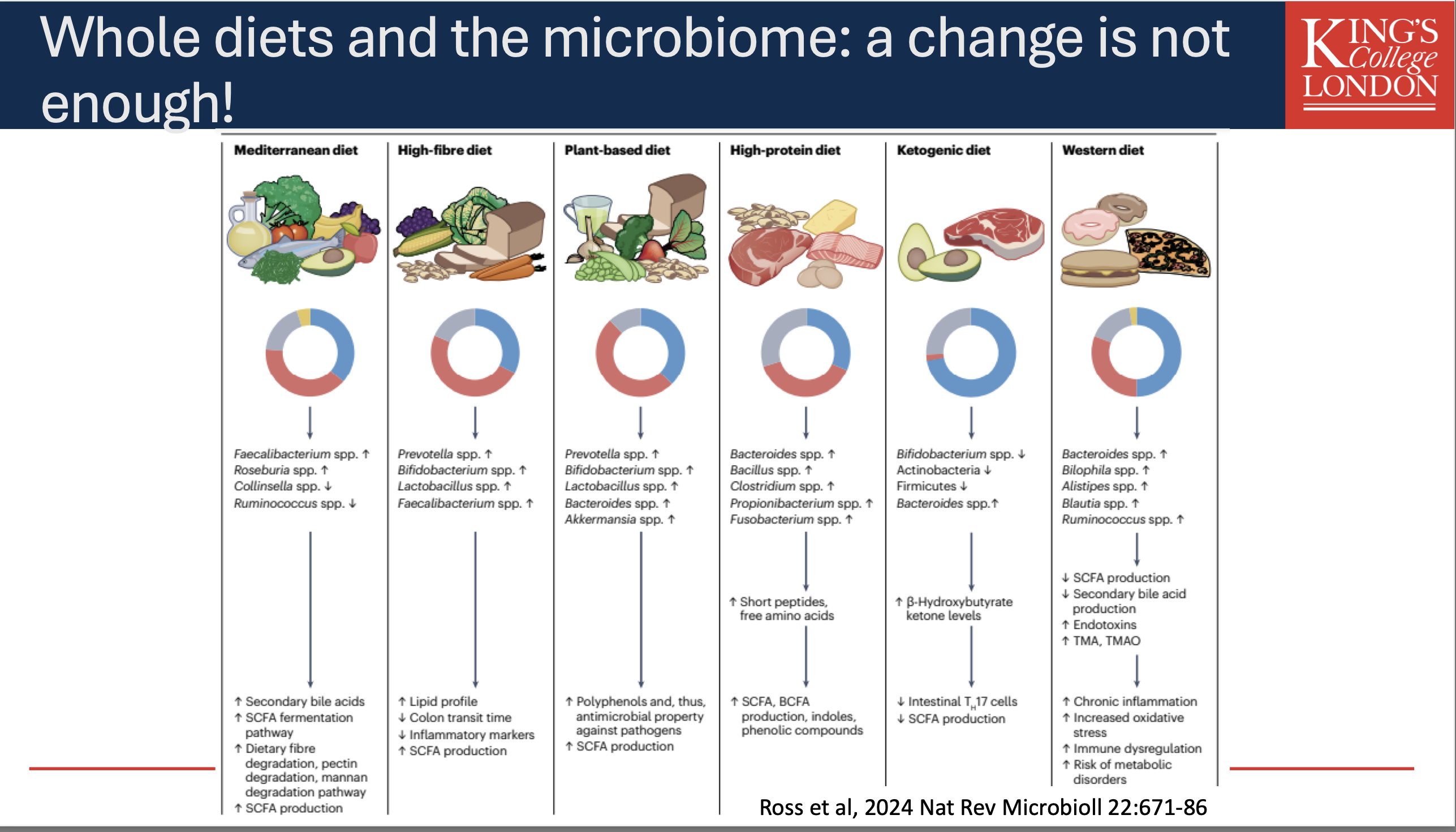
Whole Diets and the Microbiome
Research Overview:
Different dietary patterns such as the Mediterranean diet, high-fiber diet, and Western diet significantly influence gut microbiota composition and functions.
Specific impacts noted in various microbiota genera (e.g., Faecalibacterium, Bacteroides, and Prevotella) and their metabolic pathways.
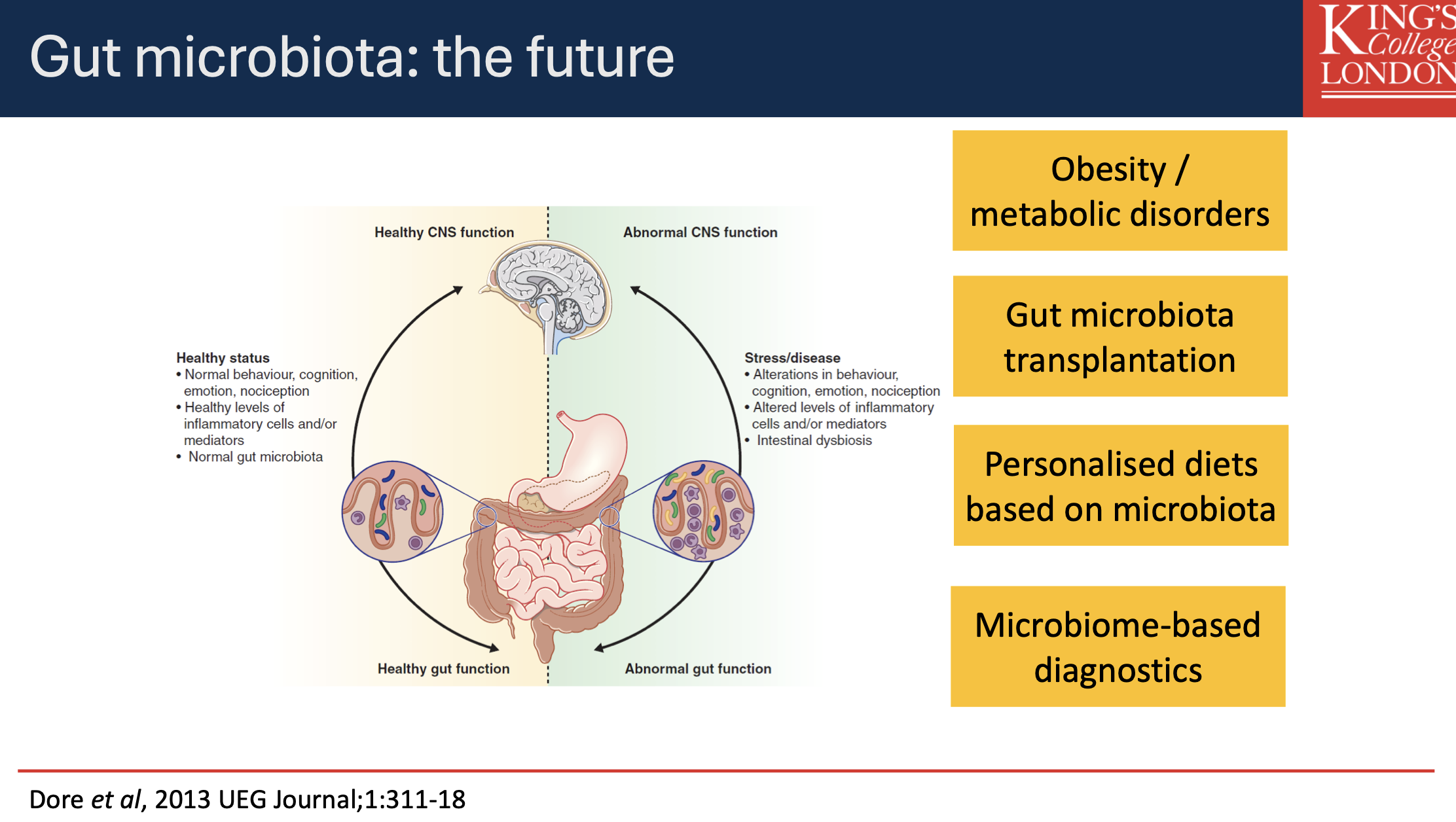
Future Trends in Gut Microbiota Research
Potential explorations include:
Microbiome-based diagnostics
Gut microbiota transplantation
Personalised dietary interventions based on individual microbiota profiles.
Seminar Topics for Further Exploration
The role of probiotics to restore the gut microbiota
The role of Faecalibacterium prausnitzii in health and disease
Gut microbiota metabolism of food
The gut microbiota's role in obesity
The gut-brain axis and its health implications
Dietary influences on gut microbiota
Individual variability in responses to food due to gut microbiota
Contact Information
Dr. Eirini Dimidi
Department of Nutritional Sciences
Email: Eirini.Dimidi@kcl.ac.uk
School of Life Course & Population Sciences
Faculty of Life Sciences & Medicine