Chapter 1 - Intro to Professional Ethics
Professional Code of Ethics
broad guidelines for members of various organizations
mental health professional organizations have their own unique code of ethics, they share common themes:
Being interested in the welfare of clients
Practicing within the scope of one’s competence
Understanding and respecting the cultural values of clients
Distinguishing between personal values and professional values
Avoiding harm and exploitation
Establishing and maintaining appropriate professional boundaries
Protecting client’s confidentiality and privacy
Practicing within an ethical and legal framework
Avoiding discrimination in providing services to clients
Striving for the highest level of ethical practice
Recognizing the importance of self-care as a basis for competent practice
Limitations of Code of Ethics
Some issues cannot be handled solely by relying on ethics codes
Ethics codes do not address the many situations that lie in an ethical gray zone
Some codes lack clarity and precision, which makes assessment of an ethical dilemma unclear.
Simply learning the ethics codes and practice guidelines will not necessarily make for ethical practice
Answers to ethical dilemmas are not contained in the ethics codes
Conflicts sometimes emerge within ethics codes as well as among various organizations’ codes
Ethics codes tend to be reactive rather than proactive
No set of rules or ethical standards can adequately guide practitioners through many of the complex situations they may encounter
New situations arise frequently, and no two cases are exactly the same
A practitioner’s personal values may conflict with a specific professional value or standard within an ethics code
Codes may conflict with institutional policies and practices
Ethics codes need to be understood within a cultural framework; therefore, they need to be adapted to specific cultures
Codes may not align with state laws or regulations regarding reporting requirements
Codes of ethics are often updated and require continuing education and professional development throughout a professional’s lifelong learning journey
Using Ethics Codes as Guides
A rule-based approach to ethics is limited in providing meaningful assistance to clinicians who are concerned with practicing at the highest level of ethical functioning
Herlihy & Corey (2015a) suggest codes of ethics fulfill 3 objectives:
educate professionals about sound ethical conduct
expand awareness & clarify values
ethical standards provide a mechanism for professional accountability
obliged to monitor their own behavior and ethical conducts in colleagues, protection from malpractice suits
serve as catalysts for improving practice
clarify positions on dilemmas that do not have simple or absolute answers
primary purpose - safeguard clients & the public, guide professionals in their owrk to provide the best service possible
community standard - what professionals actually do
ethical standard - what professionals should do
Ethics Codes & the Law
Ethics - standards that govern the conduct of its professional members
Law - body of rules that govern the affairs of people within a community, state, or country
defines the minimum standards society will tolerate, enforced by govt
practitioners obligated to act in accordance with relevant federal & state statutes and govt regulations, the law overrules ethics in court
can be difficult to determine if there is a legal problem
legal proceedings have been initiated
lawyers are involved
the practitioners is in danger of having a complaint filed against them for misconduct
laws and ethics codes tend to emerge from what has occurred rather than from anticipating what may occur
fear-based ethics - obeying statutes and following ethical standards to a t is inadequate
concern-based ethics - striving for the highest level of ethical care for clients
serve as a form of protection for the client, but also help clinicians ensure their own self-care
Conflict between ethics code and the law may arise in areas such as advertising, confidentiality, and clients’ rights of access to their own files
If there is a real conflict between the law and ethics, and if the conflict cannot be avoided, “psychologists should either obey the law in a manner that minimizes harm to their ethical values or adhere to their ethical values in a manner that minimizes the violation of the law”
Apparent conflicts between the law and ethics can often be avoided if clinicians anticipate problems in advance and take proactive measures.
Example: counseling children; there may be conflicts between ethical beliefs about counseling the child versus the the legal responsibilities to the parents/guardians right to know what is going on with their child
Example: mental health providers in the military obligations to clients and obligations to military organization (client-centered vs organization-centered)
With ethical dilemmas, it is better to seek advice from legal counsel and to discuss with colleagues
Evolution of Ethics Codes
established by prof groups for protecting consumers, providing guidelines for practitioners, and clarifying the prof stance of the organizations
undergo periodic revision, living documents responsive to the needs of counselors/clients they serve/society in general
revised code of ethics of the american counseling association (ACA) addressed ethical issues with:
ethical decision making
professional values
managing and maintaining boundaries
technology
nonimposition of counselor personal values
counselor education
legal issues
A new section of the code covers informed consent, privacy, and security of electronic communications, distance counseling, online and research maintenance, and social media
most are revise every 5-10 years
Professional Monitoring of Practice
legal & ethical practice of most mental health professionals is regulated in all 50 states, some through registration & certification - others through licensure
major duties of regulating boards:
determine standards for admission into profession
screen applicants applying for certification or licensure
regulate the practice of psychotherapy for the public good
conduct disciplinary proceedings involving violations of standards of professional conduct as defined by law
Ethical Decision Making
values - beliefs and attitudes that provide direction to everyday living
ethics - beliefs we hold about what constitutes right conduct
moral principles adopted by an individual or groups to provide rules for right conduct
represents aspirational goals, or the maximum or ideal standards set by the profession, practiced through your professional behavior and interactions
morality - concerned with perspectives of right and proper conduct and involves an evaluation of actions on the basis of some broader cultural context or religious standard
codes of ethics are conceptually broad in nature and generally subject to interpretation by practitioners
community standards - vary on interdisciplinary, theoretical, and geographical bases
often become the ultimate legal criteria for determining whether practitioners are liable for damages
define what is considered reasonable behavior when malpractice case is litigated
reasonableness - defined as the care that is ordinarily exercised by others practicing within that specialty in the professional community
professionalism - has some relationship to ethics but you can act unprofessionally yet still not act unethically
Levels of Ethical Practice
mandatory ethics - level of ethical functioning where counselors act in compliance with minimal standards, “musts” vs “must nots”
behavioral rules focus - informed consent in professional relationships
legally safe in courts of law or from professional censure by state licensure boards
aspirational ethics - highest standards of thinking and conduct, requires that counselors do more than simply follow ethics code
understanding the spirit behind the code and principles within the code
go further and reflect on effects of interventions on welfare of clients
positive ethics - how professionals can harm clients and on how therapists can do better at helping clients
looking at “what psychologists cab be, not simply avoiding what they should not do” (Knapp, 2015)
shifts emphasis of mental health providers away from focus on wrongdoing and disciplinary actions and more towards the highest level of practice
being unethical is not just extreme violations, but also inadvertent violations in clinical practice
ethics codes typically require self-monitoring and to take responsibility for misconduct
Moral Principles to Guide Decision Making
autonomy - the promotion of self-determination, freedom of clients to be self-governing
acknowledging right of others to choose and act in accordance with their wishes and values
decrease client dependency & foster client empowerment
client right to privacy & confidentiality
understand diverse cultural backgrounds of clients while exploring own cultural identities & how it affects their values and beliefs about counseling process
nonmaleficence - avoiding doing harm, refraining from actions that risk hurting clients, responsibility to minimize risks for exploitation/practices that harm or potentially harm
some diagnostic practices can be inappropriate for certain cultural groups
certain behaviors may be considered abnormal here that are normal in other cultures (inhibition of emotional expression, hesitation to confront, being cautious about self-disclosing, not making direct eye contact while speaking)
beneficence - doing good for others and promoting well-being of clients, concern for the welfare of society/doing good for society, being proactive and preventing harm when possible
culture can come into play - encouraging a course of action with good intentions but bad outcome
justice - fairness by giving equally to others and treat others justly, responsibility to provide appropriate services to all clients and treat clients fairly (regardless of age, sex, race, ethnicity, disability, socioeconomic status, cultural background, religion, sexual orientation)
fidelity - professionals make realistic commitments and do their best to keep these promises
fulfilling one’s responsibilities of trust in a relationship, loyalty to clients, making their welfare the primary concern
client right to enter & remain in counseling relationship & to be knowledgeable about the process and counselor
informed consent - writing & verbally
veracity - truthfulness, obligation to deal honestly with clients, develop trust, truthful in all interactions
self care - taking adequate care of ourselves so that we can implement the moral principles and virtues that are fundamental ethical concepts
Steps in Making Ethical Decisions
think about personal values and client values
careful consider ethical decision-making process - deliberation, consultation, and action
document process
consider personal feelings or emotions
involve clients when possible
social constructionist model - interactive process rath than individual or intrapsychic process, places decision in social context itself
negotiating, consensualizing, arbitrating if necessary
transcultural integrative model - address need for cultural factors to be involved in resolving ethical dilemmas
step-by-step format
multicultural perspective - based on universalist philosophy; cultural differences recognized - altruism, responsibility, justice, caring
identify problem or dilemma
is conflict ethical, legal, clinical, cultural, professional, moral? multiple?
identify the potential issues involved
list & describe the critical issues and discard irrelevant ones, evaluate rights/responsibilities/welfare of those affect in situation, consider culture
review the relevant ethics codes
consult available guidelines
know the applicable laws and regulations
obtain consultation
consider possible and probable courses of action
identify multiple options for dealing with situation, consider ethical & legal implications
enumerate and consider the possible consequences of various decisions
choose what appears to be the best course of action
recommended to document of ethical decision-making process - options considered and ruled out, outcome, additional actions, consultations
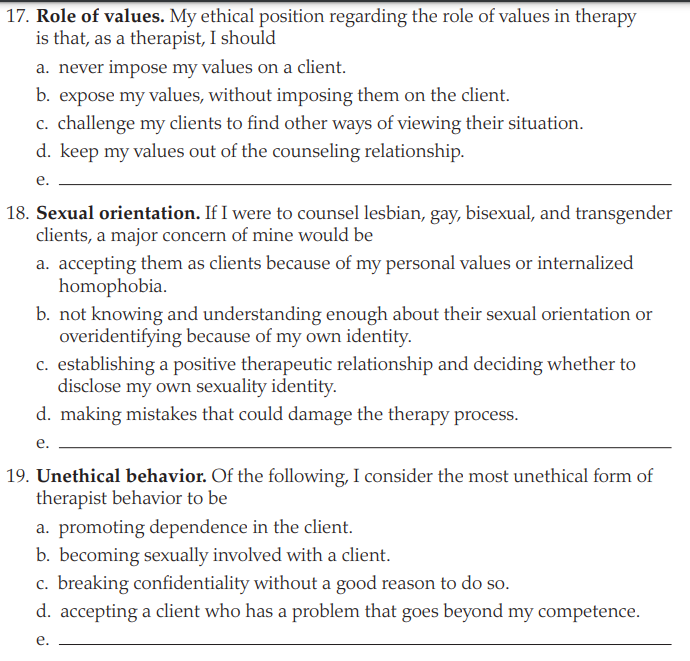
Self-Assessment - attitudes and beliefs about ethical and professional issues