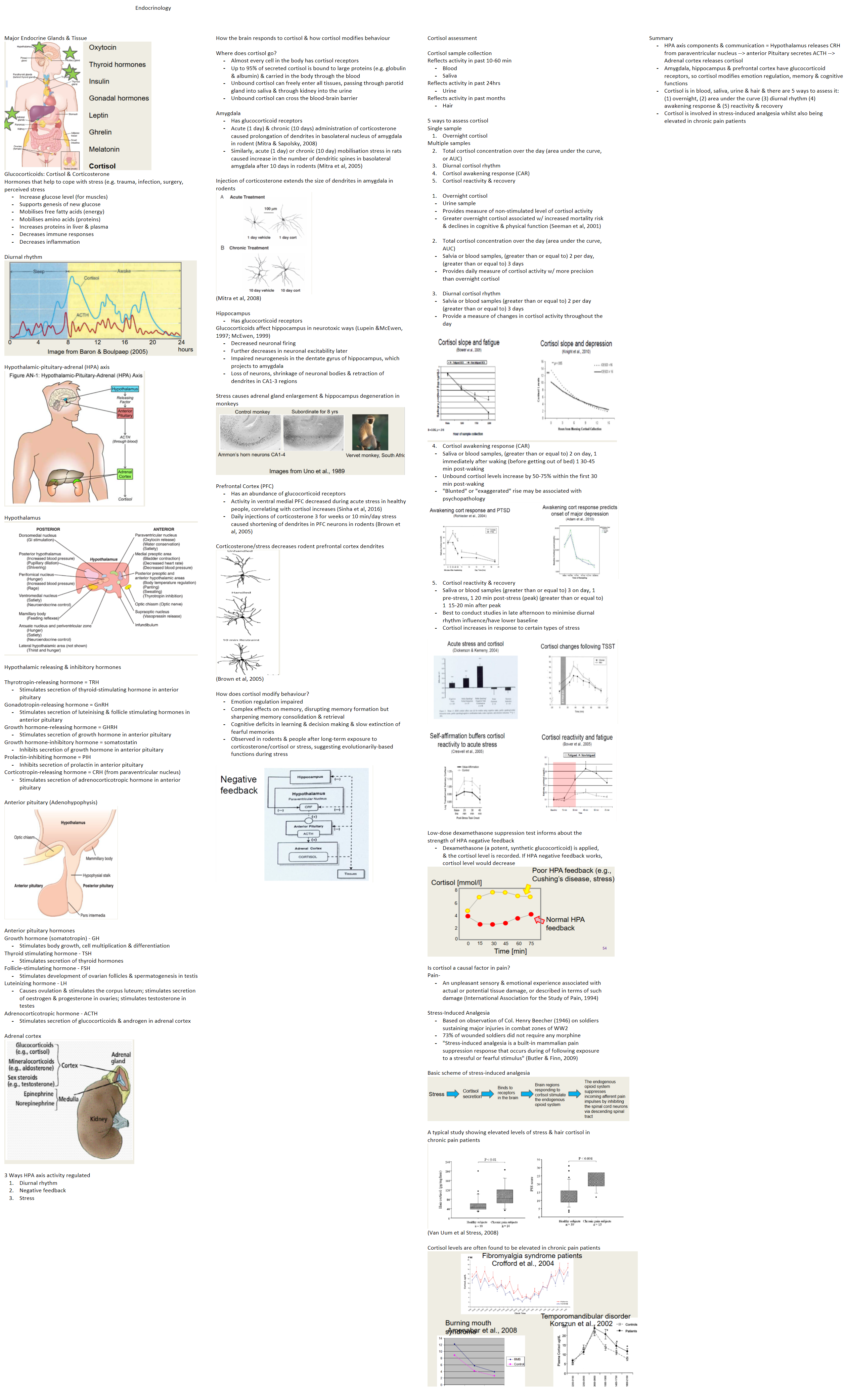
| Major Endocrine Glands & Tissue Glucocorticoids: Cortisol & Corticosterone Hormones that help to cope with stress (e.g. trauma, infection, surgery, perceived stress Increase glucose level (for muscles) Supports genesis of new glucose Mobilises free fatty acids (energy) Mobilises amino acids (proteins) Increases proteins in liver & plasma Decreases immune responses Decreases inflammation
Diurnal rhythm Hypothalamic-pituitary-adrenal (HPA) axis Hypothalamus Hypothalamic releasing & inhibitory hormones Thyrotropin-releasing hormone = TRH Gonadotropin-releasing hormone = GnRH Growth hormone-releasing hormone = GHRH Growth hormone-inhibitory hormone = somatostatin Prolactin-inhibiting hormone = PIH Corticotropin-releasing hormone = CRH (from paraventricular nucleus) Anterior pituitary (Adenohypophysis) Anterior pituitary hormones Growth hormone (somatotropin) - GH Thyroid stimulating hormone - TSH Follicle-stimulating hormone - FSH Luteinizing hormone - LH Adrenocorticotropic hormone - ACTH Adrenal cortex 3 Ways HPA axis activity regulated Diurnal rhythm Negative feedback Stress
| | How the brain responds to cortisol & how cortisol modifies behaviour Where does cortisol go? Almost every cell in the body has cortisol receptors Up to 95% of secreted cortisol is bound to large proteins (e.g. globulin & albumin) & carried in the body through the blood Unbound cortisol can freely enter all tissues, passing through parotid gland into saliva & through kidney into the urine Unbound cortisol can cross the blood-brain barrier
Amygdala Has glucocorticoid receptors Acute (1 day) & chronic (10 days) administration of corticosterone caused prolongation of dendrites in basolateral nucleus of amygdala in rodent (Mitra & Sapolsky, 2008) Similarly, acute (1 day) or chronic (10 day) mobilisation stress in rats caused increase in the number of dendritic spines in basolateral amygdala after 10 days in rodents (Mitra et al, 2005)
Injection of corticosterone extends the size of dendrites in amygdala in rodents (Mitra et al, 2008) Hippocampus Glucocorticoids affect hippocampus in neurotoxic ways (Lupein &McEwen, 1997; McEwen, 1999) Decreased neuronal firing Further decreases in neuronal excitability later Impaired neurogenesis in the dentate gyrus of hippocampus, which projects to amygdala Loss of neurons, shrinkage of neuronal bodies & retraction of dendrites in CA1-3 regions
Stress causes adrenal gland enlargement & hippocampus degeneration in monkeys Prefrontal Cortex (PFC) Has an abundance of glucocorticoid receptors Activity in ventral medial PFC decreased during acute stress in healthy people, correlating with cortisol increases (Sinha et al, 2016) Daily injections of corticosterone 3 for weeks or 10 min/day stress caused shortening of dendrites in PFC neurons in rodents (Brown et al, 2005)
Corticosterone/stress decreases rodent prefrontal cortex dendrites (Brown et al, 2005) How does cortisol modify behaviour? Emotion regulation impaired Complex effects on memory, disrupting memory formation but sharpening memory consolidation & retrieval Cognitive deficits in learning & decision making & slow extinction of fearful memories Observed in rodents & people after long-term exposure to corticosterone/cortisol or stress, suggesting evolutionarily-based functions during stress
| | Cortisol assessment Cortisol sample collection Reflects activity in past 10-60 min Reflects activity in past 24hrs Reflects activity in past months 5 ways to assess cortisol Single sample Overnight cortisol
Multiple samples Total cortisol concentration over the day (area under the curve, or AUC) Diurnal cortisol rhythm Cortisol awakening response (CAR) Cortisol reactivity & recovery
Overnight cortisol
Urine sample Provides measure of non-stimulated level of cortisol activity Greater overnight cortisol associated w/ increased mortality risk & declines in cognitive & physical function (Seeman et al, 2001)
Total cortisol concentration over the day (area under the curve, AUC)
Salvia or blood samples, (greater than or equal to) 2 per day, (greater than or equal to) 3 days Provides daily measure of cortisol activity w/ more precision than overnight cortisol
Diurnal cortisol rhythm
Cortisol awakening response (CAR)
Saliva or blood samples, (greater than or equal to) 2 on day, 1 immediately after waking (before getting out of bed) 1 30-45 min post-waking Unbound cortisol levels increase by 50-75% within the first 30 min post-waking "Blunted" or "exaggerated" rise may be associated with psychopathology
Cortisol reactivity & recovery
Saliva or blood samples (greater than or equal to) 3 on day, 1 pre-stress, 1 20 min post-stress (peak) (greater than or equal to) 1 15-20 min after peak Best to conduct studies in late afternoon to minimise diurnal rhythm influence/have lower baseline Cortisol increases in response to certain types of stress
Low-dose dexamethasone suppression test informs about the strength of HPA negative feedback Dexamethasone (a potent, synthetic glucocorticoid) is applied, & the cortisol level is recorded. If HPA negative feedback works, cortisol level would decrease
Is cortisol a causal factor in pain? Pain- Stress-Induced Analgesia Based on observation of Col. Henry Beecher (1946) on soldiers sustaining major injuries in combat zones of WW2 73% of wounded soldiers did not require any morphine "Stress-induced analgesia is a built-in mammalian pain suppression response that occurs during of following exposure to a stressful or fearful stimulus" (Butler & Finn, 2009)
Basic scheme of stress-induced analgesia A typical study showing elevated levels of stress & hair cortisol in chronic pain patients (Van Uum et al Stress, 2008) Cortisol levels are often found to be elevated in chronic pain patients | | Summary HPA axis components & communication = Hypothalamus releases CRH from paraventricular nucleus --> anterior Pituitary secretes ACTH --> Adrenal cortex releases cortisol Amygdala, hippocampus & prefrontal cortex have glucocorticoid receptors, so cortisol modifies emotion regulation, memory & cognitive functions Cortisol is in blood, saliva, urine & hair & there are 5 ways to assess it: (1) overnight, (2) area under the curve (3) diurnal rhythm (4) awakening response & (5) reactivity & recovery Cortisol is involved in stress-induced analgesia whilst also being elevated in chronic pain patients
|