Week 10: Nutritional Fundamentals for Nursing
Learning Outcomes
Apply the nursing process to nutrition & patient care.
Discuss factors affecting nutrition.
Identify elements of nutritional assessment.
Explain therapeutic diets and their uses.
Recognize nursing interventions for optimal nutrition.
Describe enteral and parenteral nutrition interventions and corresponding nursing actions.
Nutrients
Definition: Biochemical substances for growth, development, activity, reproduction, lactation, health maintenance, and recovery from illness/injury.
Essential Nutrients: Not synthesized or insufficient in the body, must come from diet or supplements.
Macro-nutrients: Provide energy and build tissue (carbohydrates, fats, proteins).
Micro-nutrients: Regulate and control body processes (vitamins, minerals).
Six Classes of Nutrients
Macronutrients (Supply Energy)
Carbohydrates
Proteins
Lipids (fats)
Saturated fats come from animals and unsaturated come from plants.
Micronutrients (Regulate Body Processes- Growth & Metabolism)
Vitamins
Water-soluble: vitamins B & C; whatever the body doesn’t use that is excreted.
Fat-soluble: vitamins A, D, E, and K; overconsumption can affect health and reach toxic levels.
Minerals
Water
Energy Balance
Definition: Difference between energy intake from foods and energy expenditure from bodily processes.
Energy Measurements: Measured in kilocalories; includes total daily energy expenditure (TDEE) and total daily energy intake (TDI).
TDEE: all of the calories used to perform physical activity, maintain metabolism, and digest, absorb, and metabolize food.
TDI: total calories for each food item eaten.
Basal Metabolic Rate (BMR): Energy needed for involuntary activities at rest after 12 hours; is higher in males due to larger muscle mass.
Factors affecting BMR:
Increase: Growth, infections, fever, emotional stress, extreme temperatures, hormones.
Decrease: Aging, prolonged fasting, sleep.
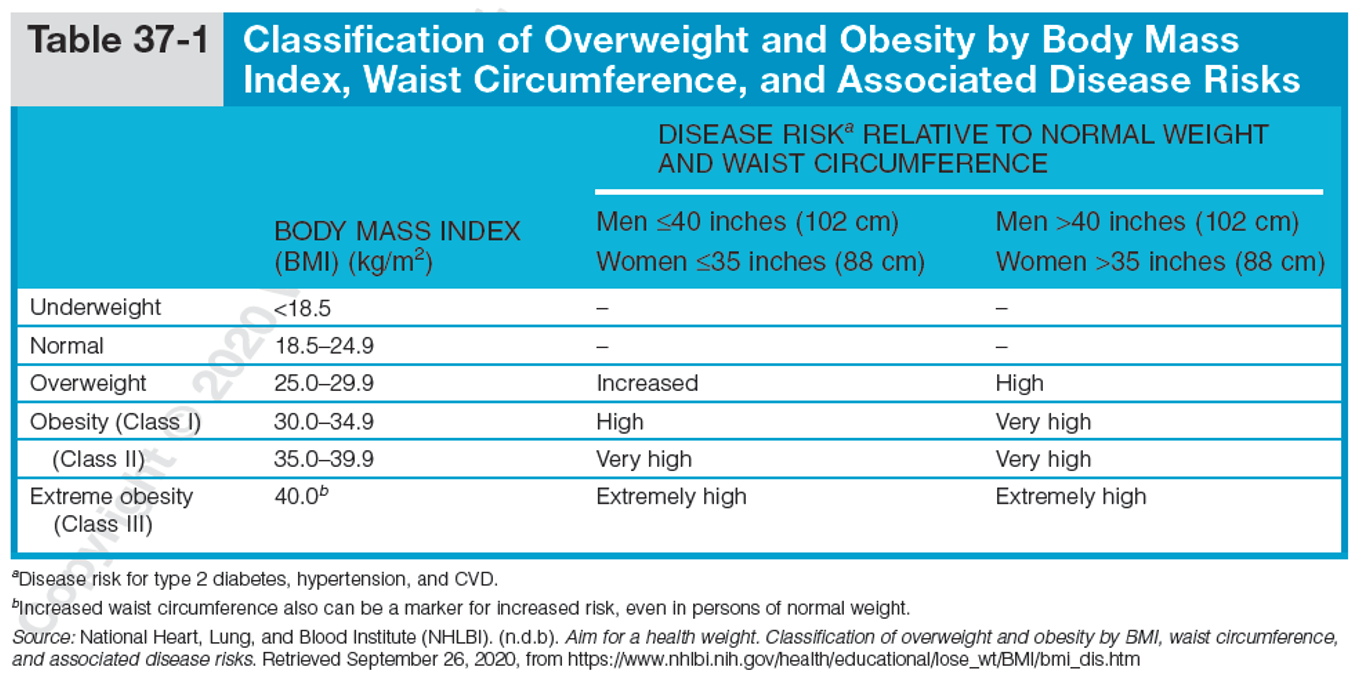
Body Mass Index (BMI)
Definition: Ratio of weight (kg) to height (m^2), estimating body fat and associated disease risks.
Overweight and obesity are defined differently for children and teens.

Limitations: May not accurately reflect risk in all populations.
Ex. Someone with a high amount of muscle mass may be classified as overweight or obese according to BMI, despite having a healthy body fat percentage. In addition to someone who has edema or who is extremely dehydrated.
Waist Circumference: The best indicator of abdominal fat; risk increases with 40 inches for men and 35 inches for women.
Prefer being pear-shaped rather than apple-shaped.
Waist-to-Hip Ratio (WHR): Tool for identifying central obesity.
Macronutrients Overview
Carbohydrates
Most abundant and least expensive source of calories in the world.
Types: Sugars and starches; primary energy source.
Lactose is the only animal source.
Classification: Simple vs. complex sugars.
Intake Recommendation: 45% to 60% of total daily calories.
Digestion: Quick and easy to digest, converted to glucose for energy use.
90% of intake is ingested.
Transported from the GI tract, through the portal vein, to the liver, where it is stored as glucose and regulates entry into the blood.
Proteins
Function: Vital for body structures, formed from amino acids (22 types). Continuously breaks down (catabolizes) and builds up (anabolizes) tissues.
Occurs in the small intestine and transports to the liver for released amino acids.
Types:
Complete: Animal sources (sufficient essential amino acids).
Incomplete: Plant sources (except soy and quinoa).
Vegetarians can combine different plant proteins to supply a complete protein.
RDA: 0.8 g/kg body weight, constitutes 10% to 35% of total calorie intake.
Fats
Composition: Insoluble in water; composed of carbon, hydrogen, and oxygen. It is the most concentrated source of energy in the diet.
Types: Saturated (raised cholesterol, animal-based) and unsaturated (lower cholesterol, plant-based).
Digestion: Occurs in the small intestine, aided by bile from the liver (and stored in the gallbladder). 95% of lipids in diet are triglycerides.
Fats are absorbed into the lymphatic circulation and transported to the liver.
Recommended Intake: Limit saturated fats to <10% of total calories.
Vitamins
Function: Organic compounds needed in small amounts for metabolism, do not provide calories. Fresh foods are higher in vitamins than processed foods.
Digestion: Absorbed through the intestinal wall directly into the bloodstream.
Classification:
Water-soluble: Vitamins C, B-complex (not stored).
Fat-soluble: Vitamins A, D, E, and K (stored).
Minerals
Organic elements are found in all body fluids and tissues.
Function: Involved in body structure and regulating processes.
Types:
Macrominerals: Calcium, phosphorus, sodium, potassium, etc.
Microminerals: Iron, zinc, selenium, etc.
Water
Importance: Accounts for 50-60% of body weight; crucial for chemical reactions and biological processes. It acts as a solvent and aids digestion, absorption, circulation, and excretion.
Fluid Compartments: Intracellular (ICF) and extracellular fluids (ECF).
Key Factors Affecting Nutritional Requirements
Developmental Considerations:
Growth: infancy, adolescence, pregnancy, and lactation increase nutritional needs.
Activity increases nutritional needs.
Age-related changes in metabolism and body composition.
Nutritional needs level off in adulthood.
Fewer calories are required in adulthood because of a decrease in BMR.
Additional Factors: Sex assigned at birth, state of health, alcohol use disorder, medications, and megadoses of nutrient supplements.
Factors that Influence Food Choices: SDOH, religion, meaning of food, and culture.
Nutritional Assessment Components
History Taking: Dietary, medical, socioeconomic.
Physical Assessments: Anthropometric data and clinical evaluations.
Biochemical Data: Assess protein, vitamin, and mineral status.
Methods:
24-hour recall
Food diaries
Food frequency records
Nursing Interventions
Education: Teach nutritional information to patients.
Monitoring: Keep track of nutritional status.
Assistance: Help stimulate appetite and assist with eating.
Visually-impaired patients: use the clock method.
“Your carrots are at 12 o’clock, your rice is at 3 o’clock.”
Support: Provide oral nutritional solutions and long-term support.
Dietary Guidelines and Interventions
Therapeutic Diets: Tailored to specific conditions (e.g., renal, low fiber).
Modified Consistency: Clear or pureed diets for certain medical situations.
Clear Liquid Diet: Typically used for temporary use, avoid red liquids if GI concerns.
Ex. Broth, gelatin, popsicles, carbonated beverages, coffee, and tea.
Full Liquid Diet: “clears”, pourable, liquid supplements.
Ex. Have all clear liquids and milk, pudding, and custard.
Enteral Nutrition: Short-term support via NG tubes; long-term via gastrostomy.
Parenteral Nutrition (PN): Given IV, composed of amino acids, carbohydrates, and lipids, more concentrated than enteral. Monitor for complications like infections and metabolic imbalances.