3.2 Cells and the Immune System
Defences Systems
- Lymphocytes have to be able to recognise between foreign and self cells otherwise body tissues would be accidentally destroyed
- Each cell has a @@specific protein that can be recognised@@ due to its intricate tertiary or quaternary structure
- There are @@very few of many types of lymphocyte cells that are able to recognise different foreign pathogens@@
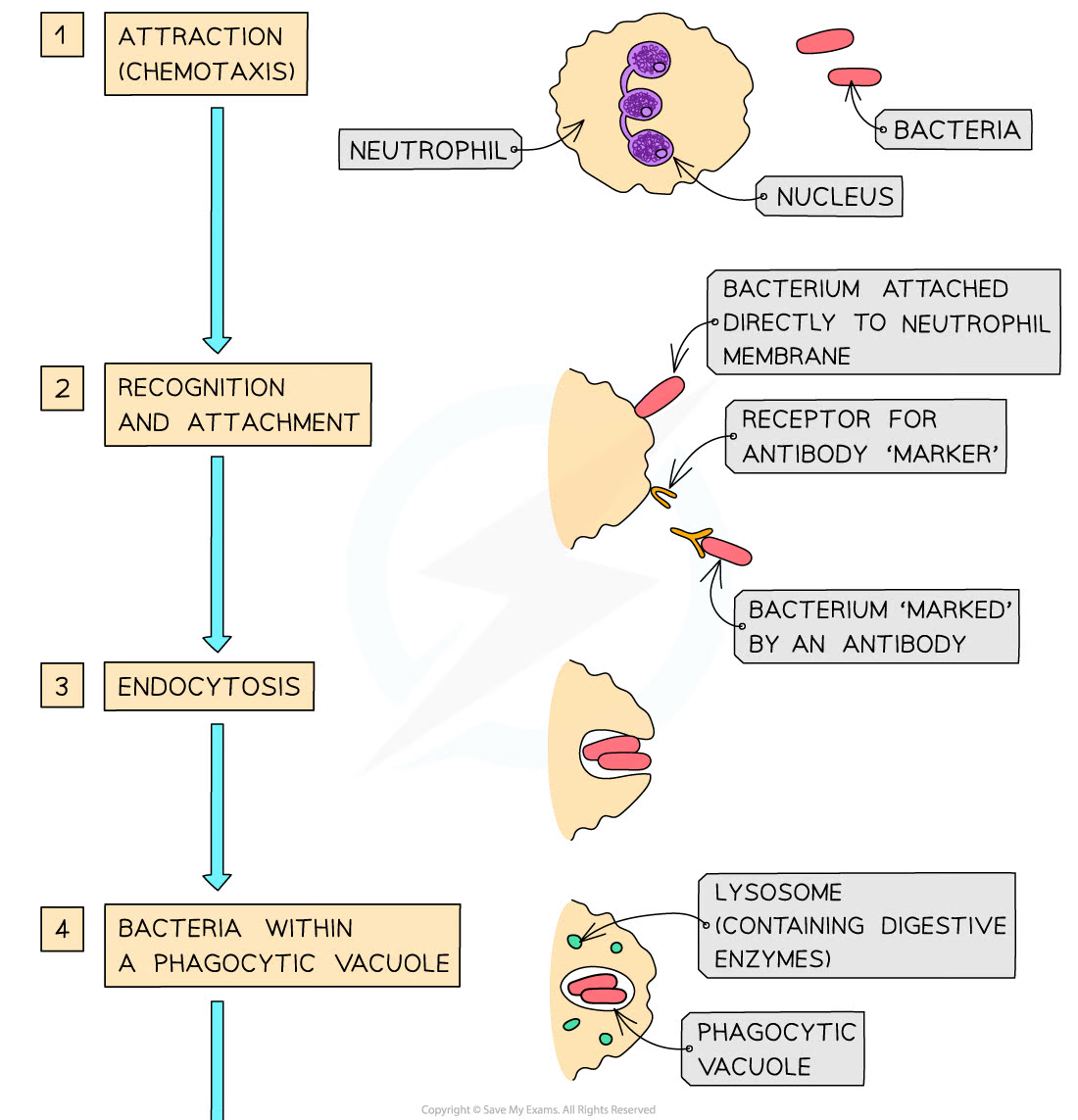
Phagocytosis
- @@Pathogen is detected by a phagocyte@@. Pathogens have unique antigens called Pathogen Associated Molecular Patterns (PAMPs). Phagocytes can recognise these PAMPs through specialised receptors on their cell surface membranes known as Pathogen Recognition Receptors (PRRs)
- @@The phagocyte is activated@@. When the PRRs recognise and bind to a PAMP, it activates the phagocyte. Signalling molecules such as interferons may also help in phagocyte activation
- @@The phagocytes engulfs the pathogen@@. The phagocyte grows cytoplasmic extensions to engulf the pathogen, and @@internalises it into its cytoplasm@@. The pathogen is engulfed in a vesicle known as the @@phagosome@@. The mechanism for phagocytosis is the same as the mechanism for endocytosis discussed in the previous chapter
- @@Lysozymes break down the pathogen@@. Inside the phagocyte, the @@phagosome fuses with a lysosome. Upon fusion, the lysosome releases lysozymes into the phagosome which then hydrolyse the pathogen@@
- @@The phagocyte absorbs the digestive products@@. The hydrolysis products, such as broken-down proteins, are then absorbed by the phagocyte
- Cell becomes @@antigen presenting@@
Lymphocytes
- An antigen is any part of an organism or substance that is @@recognised as non self@@
- The recognition of one @@triggers the production of antibodies@@ as part of the immune response
- T-Lymphocytes are matured in the thymus gland
- B-Lymphocytes are matured in the bone marrow
- Lymphocytes @@respond to self cells that have been infected as well as foreign cells from the same species@@
- Phagocytes have engulfed and hydrolysed the pathogen, becoming an @@antigen presenting cell@@
- Body cells invaded by same pathogen begin to present the pathogens antigens on their surface membrane as well
- Transplanted cells from different individual of same species have different antigens on their surface
- Own bodies cancer cells present antigens on their membrane too
- T-Lymphocytes @@only respond to antigens on the cell surface membrane@@ not in blood plasma etc
The stages of T-Lymphocyte response are as follows…
- @@Pathogens invade body cells or are taken up by pathogens@@
- Phagocyte becomes @@antigen presenting cell@@
- Receptors on @@T-Cells match the antigen shape@@ exactly
- The two attach and this triggers the T-Cell to r@@apidly divide by mitosis to form genetically identical cells@@
- The cloned T-Cells…
- Differentiate into @@memory cells@@ that enable rapid response to future infection of same pathogen
- @@Stimulate phagocytes to engulf pathogens and undergo phagocytosis@@
- Stimulate @@B-Cells to divide and secrete antibody@@
- @@Activate Cytotoxic T-Cells@@
Cytotoxic T-Cells
- @@Kill abnormal cells@@ or those @@infected by the pathogen@@
- They perform @@apoptosis@@
- Produce a protein called @@perforin@@
- This creates @@holes in the cell membrane@@ which makes the @@cell more freely permeable to other substances and the cell dies as a result@@
B-Lymphocytes and Humoral Immunity
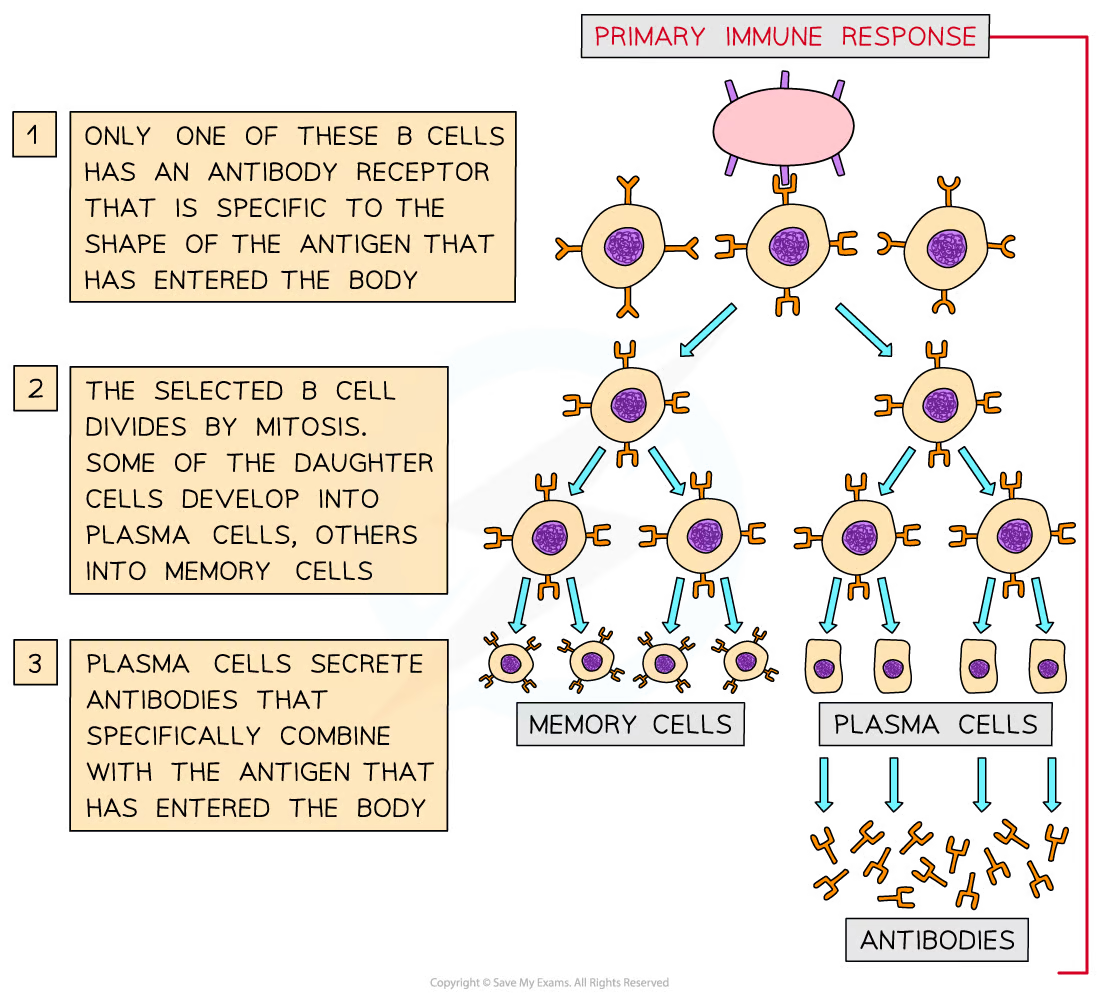
- When an antigen enters the blood stream on the surface of a cell there will be 1 @@B-Cell that fits it perfectly@@
- The antigen then @@attached to the complementary antibody@@
- The @@antigen enters the B-Cel@@l by endocytosis and gets @@presented on the surface@@ of the cell
- Helper T-Cells then bind to them and this @@triggers clonal selection@@
- This allows the B-Cell to @@divide rapidly to form plasma or memory cells@@
- Plasma cells s@@ecrete antibodie@@s into blood plasma. They @@do not survive for very long@@ but make lots of antibodies at a very rapid pace. These antibodies are responsible for killing the pathogen and are therefore the @@primary response@@
- Memory cells live in the blood for many years until a reinfection when they can @@become plasma cells to produce antibodies or become more memory cells. They are the secondary immune response@@
Antibodies
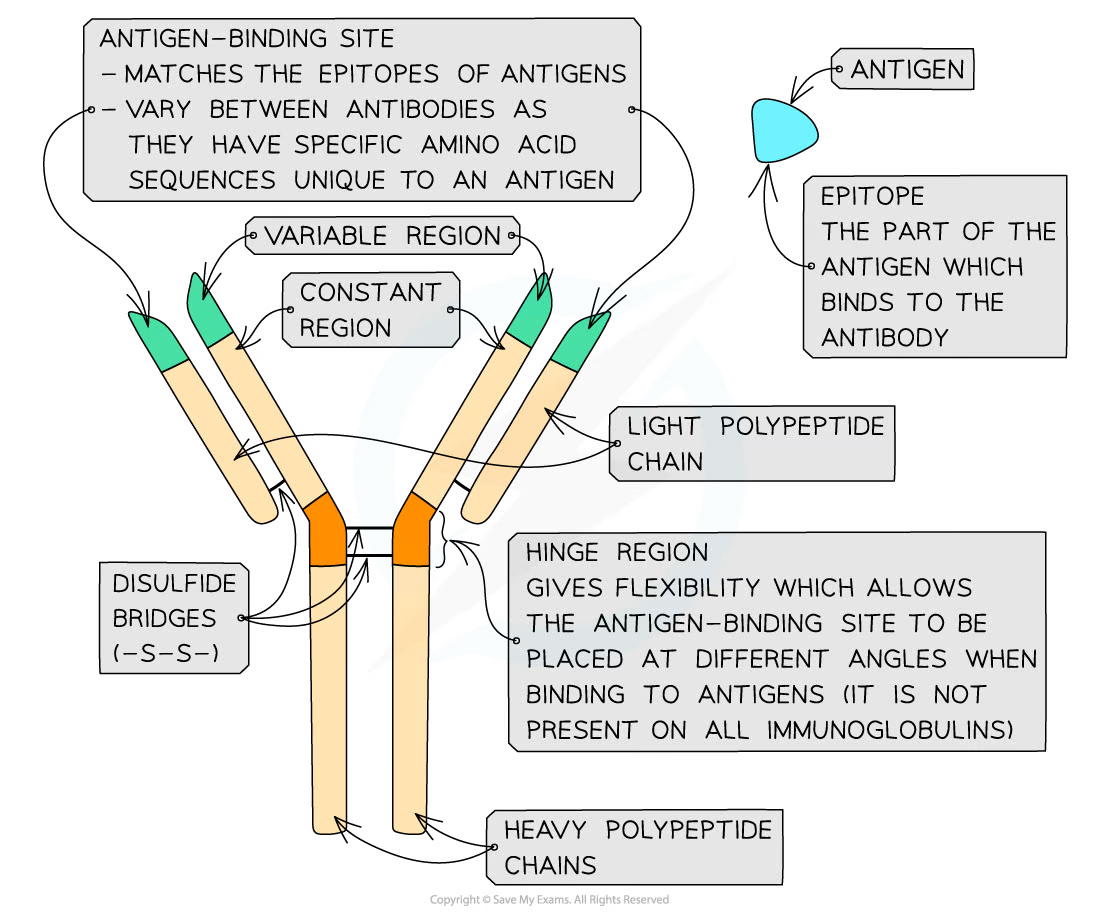
- Made up of 4 polypeptide chains
- The chains of 1 pair and longer and therefore the heavy chains and the other pair are shorter so are the light chains
- Antibodies have a constant region. @@Every antibody has the same constant region. The antibody uses this to bind to phagocytes@@
- Antibodies have a variable region. The variable region has a unique structure that is different for each and every antibody molecule. @@This variable region is the antigen binding site of the antibody by which the antibody molecule can recognise and bind to a particular antigen.@@ It is like the active site of an enzyme
- Antibodies have hinge regions. Antibodies have flexible hinge regions, which make allow the branches of the Y to move away from each other. This @@makes antibodies more flexible, so can bind to multiple antigens@@
Functions
- Neutralising toxins. Many pathogens can produce endotoxins, which harm the host organism. A@@ntibodies can bind to endotoxins and neutralise them@@
- Neutralising antigens. Additionally, antibodies can directly neutralise viruses. Most viruses have attachment proteins that are necessary for binding to and infecting host cells. @@If an antibody binds to these viral attachment proteins, the virus cannot infect cells@@
- Agglutination. Antibodies will clump pathogens together. @@Antibodies can bind to multiple antigens and therefore clump the pathogens into one big group. This big group cannot infect cells, and also makes it easy for phagocytes to engulf multiple pathogens in one go.@@
- Antibodies mark pathogens. @@Antibodies bound to a pathogen are beacons for immunological cells@@, and attract phagocytes and lymphocytes to the area
- Lysis. Enzymes can work with antibodies. Enzymes can bind to antibodies bound to pathogenic antigens. @@These enzymes can then catalyse enzymatic reactions which break down the bacteria which are bound the antibodies@@.
Monoclonal Antibodies
- Monoclonal antibodies have a @@highly specific antigen binding site@@ and can only recognise and @@bind to a very unique and specific antigenic sequence@@
Production
- A mouse (or another mammal) is @@injected with an antigen@@. The antigen may be a vaccine, and it may be injected several times. This @@causes an immune response@@ in the mouse i.e. @@corresponding antibodies are produced by B cells.@@
- @@Spleen cells which are responsible for producing the lymphocytes are removed from the anima@@l. The spleen produces B cells which are responsible for the antibody production.
- These spleen cells are removed from the mouse via a small operation.
- The spleen cells are @@fused with tumour cells to form hybridoma cells@@. The mouse’s spleen cells are fused with myeloma cells (cancerous white blood cells from humans), forming hybridoma cells.
- @@The hybridoma cells continuously produce monoclonal antibodies@@. These hybridoma cells have both the properties of the lymphocytes and tumour cells i.e. @@they are able to divide indefinitely and produce many monoclonal antibodies.@@
- These cells are checked and grown in culture in the lab. The monoclonal antibodies are @@harvested@@.
- The monoclonal antibodies produced by the hybridoma cells can be @@separated and harvested for further use@@
Uses
- Treating poisoning – monoclonal antibodies are used to @@neutralise various poisons@@ in patients.
- Cancer treatment – cancer cells often have antigens called tumour markers. We can design monoclonal antibodies specific to these antigens, so that they @@can neutralise cancer cells, as well as to attract TC cells. We can also attach anti-cancer drugs to the monoclonal antibodies.@@
- Medical diagnosis – monoclonal antibodies can be used to @@detect particular antigens in patient samples of blood or tissue.@@ For example, pregnancy testing uses monoclonal antibodies to detect for human chorionic gonadotrophin (hCG). If a woman is pregnant, @@hCG will be found in urine, so we can do urine tests using monoclonal antibodies@@
Ethics
- @@Mouse is harmed@@ e.g. spleen removed which will kill the mouse
- Requires @@animal testing@@
- @@Some deaths involved in the use of them to treat Multiple Sclerosis@@, patient should know associated risks
- @@Testing of new drugs presents danger for human test subjects@@
Vaccines
- Passive immunity. Immunity gathered by antibodies @@passed from an outside source without individual being exposed to actual pathogen@@ e.g. foetus
- Immunity @@does not last@@ as @@antibodies are not replaced@@ once broken down and no memory cells produced
- Can be used in snake venom treatment for example
- Active Immunity. @@Immunity gathered by direct contact to pathogen@@ either naturally or artificially e.g. vaccinations
Features of a Successful Vaccination Program
- @@Economically sustainabl@@e in sufficient quantities for vulnerable populations
- @@Few side effect@@s that will not severely damage most of the participants
- Means of producing, transporting and storing vaccine must be @@easy and efficient@@
- @@Means of administering vaccine availabl@@e at correct time such as trained nurses available throughout whole population
- Large proportion of population able to be vaccinated for @@herd immunity@@
Herd Immunity
- When sufficiently large proportion of population vaccinated so @@difficult for pathogen to spread throughout population@@
- Make it less probable that a @@vulnerable individual is less likely to come into contact with an individual carrying the pathogen@@
- Vaccinations should take place in one time period to create a circuit breaker for pathogen
- However this @@does not eliminate pathogen entirely@@
- @@Not whole population is vaccinated@@
- Vaccinated individual may develop disease after vaccine but their immunity level is high enough that they are not sick but @@can still harbour pathogen and pass it on@@
- Pathogen may mutate via @@antigenic variation@@ e.g. flu
- @@Varieties of pathogen availabl@@e so impossible to vaccinate against all of them
- Certain @@pathogens ‘hide’ from immune system@@ either in body cells or in out of reach places like intestines
Ethics
- Often involves testing and use of animals
- Can have @@side effect@@s that have life long impact
- Vaccine must be @@tested on humans@@, who is it appropriate to test on and how can you ensure individual understands fully the possible consequences
- @@Should vaccines be compulsory to ensure herd immunity@@
- Should @@expensive vaccination schemes continue even if disease is mostly eradicated@@
- @@Can individual health risk be balanced against overall population protection@@
HIV
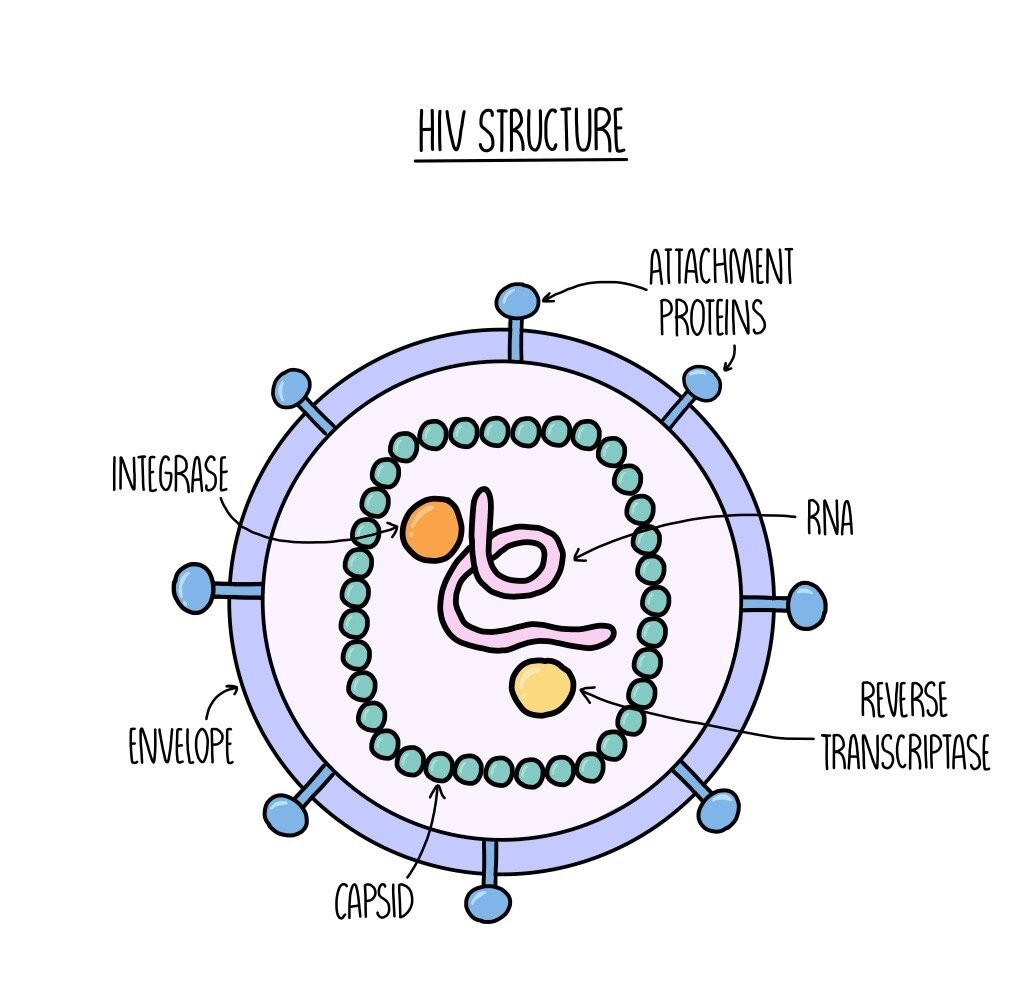
- HIV is a @@retrovirus@@ so contains RNA
- On outside is @@lipid envelope@@ with @@attachment proteins to help virus attach to host cel@@l
- Inside cell is c@@apsid that holds RNA@@ and enzymes r@@everse transcriptase and integrase@@
- @@Reverse transcriptase catalyses tor production of DNA from RNA@@
Replication of HIV
- HIV enters bloodstream and @@circulates around body@@
- @@Protein on HIV readily binds to CD4, which mainly is present on Helper T-Cells@@
- Protein capsid fuses with cell surface membrane @@RNA and enzymes of HIV enter host cell@@
- HIV reverse transcriptase @@converts viral RNA to DNA@@
- New DNA moves into host cell nucleus and @@inserts into host DNA@@
- @@Creates mRNA of viral proteins and RNA@@ to go into new HIV cells
- @@HIV particles are produces then break away from from Helper T-Cel@@l with piece of its membrane to form new lipid envelope
- Replication of HIV often goes dormant and individual is only develops AIDS when the replication recommences
How HIV causes AIDS
- HIV @@interferes with Helper T-Cells@@ which are necessary for the immense system, @@reducing the overall number of them@@
- Without sufficient amount @@B-Cells cannot be stimulated to produce antibodies and cytotoxic T-Cells are not stimulated either@@ so individual becomes very sick from any infection
- @@Patients die of other diseases due to weakened immune system@@ from HIV
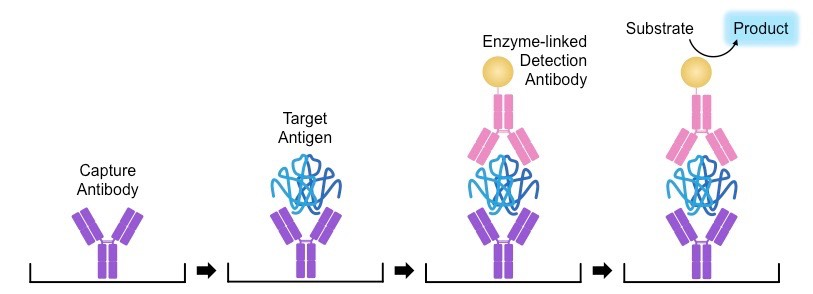
Elisa Test
- @@Known monoclonal antibodies are affixed to wells in a plate@@ (these are the 'capture antibodies')
- @@A sample to be tested is added to the wells and any antigens present will bind to the appropriate capture antibod@@y
- The plates are then @@washed@@ to remove any unbound antigen
- A second set of monoclonal antibodies linked to @@colour-changing enzymes are then added to the wells@@
- These 'detection antibodies’ will bind to any antigens captured, creating a sandwich (antibody - antigen - antibody)
- The wells are then @@washed again to remove any unbound detection antibodies@@
- When an appropriate substrate is added to the wells, the enzyme-linked detection antibodies will @@trigger a colour change@@
- @@Only wells in which a sandwich complex has formed will show a colour change@@, hence identifying the presence of an antigen
Why Antibiotics are Ineffective Against HIV
- One way @@antibiotics work is by preventing bacteria from making normal cell walls@@
- In bacteria, the cell wall prevents water entering via osmosis and killing the cell as the wall is reinforced with murein
- When antibiotics prevent formation of cell wall the cell dies due to inability to withstand pressure and it bursts
- @@Viruses rely on host cells so lack their own cell structures and metabolic structures@@
- @@Therefore no processes to disrupt@@
- @@Viruses also have protein coat not murein cell wall so no site for antibiotics to work@@