Integrative Physiology: Cardiovascular Physiology Study Notes
Cardiovascular System Anatomy Review
Outline
Cardiovascular system – anatomy review
Pressure, volume, flow, and resistance
Cardiac muscle and the heart
The heart as a pump
Cardiac cycle
Cardiac output
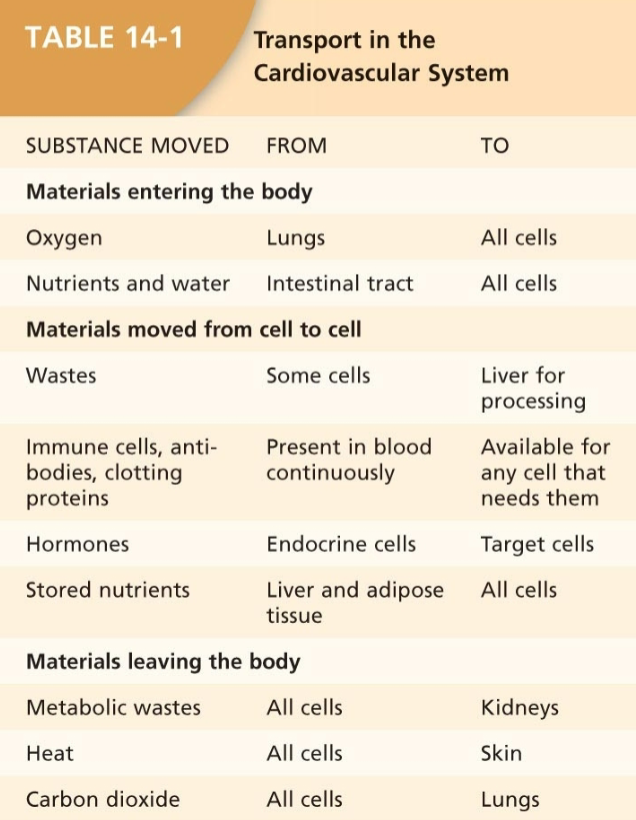
Transport in the Cardiovascular System
Table 14-1: Transport
Cardiovascular Circulation
Pulmonary and Systemic Circulation
Pulmonary Circulation
Pathway:
Right side of heart
Pulmonary arteries
Pulmonary capillaries of alveoli of lungs
Pulmonary veins to left side of heart
Systemic Circulation
Pathway:
Left side of heart
Systemic arteries
Systemic arterioles
Systemic capillaries of all body organs and tissues
Systemic venules to right side of heart
Venae cavae
Heart Anatomy
Size of a fist, located in thoracic cavity, mostly left side
Composed mostly of myocardium with a membranous sack, pericardium
Valves ensure one-way flow:
Right Side:
Tricuspid AV valve
Pulmonary semilunar valve
Left Side:
Bicuspid AV valve
Aortic semilunar valve
Heart Valves
Have a fibrous skeleton to prevent stretching
Open and close to prevent backflow during heart contractions
Pressure Dynamics
Pressure Change in CVS
Blood pressure created by contracting muscles, mainly by the left ventricle
Factors Affecting Blood Pressure:
Blood vessel constriction increases blood pressure
Blood vessel dilation decreases blood pressure
Volume changes greatly affect blood pressure in the cardiovascular system (CVS)
Pressure Gradient
Blood flows from high pressure to low pressure
Flow only occurs with a positive pressure gradient
Pressure gradient formula:
Requires a positive pressure difference for flow
Resistance to Flow
Resistance is affected by radius:
Flow rate is inversely related to resistance:
Example: Tube A and B with differing radii affect flow significantly due to this relationship
Cardiac Muscle vs. Skeletal Muscle
Cardiac Muscle Characteristics:
Smaller, single nucleus per fiber
Contains intercalated disks:
Desmosomes transfer force
Gap junctions provide electrical connections
Larger T-tubules, smaller sarcoplasmic reticulum
Higher mitochondria volume, important for ATP production
Contraction Mechanism:
Action potential initiates calcium influx, inducing contraction through interactions with troponin and actin
Relaxation occurs when calcium unbinds from troponin and returns to the sarcoplasmic reticulum
Cardiac Cycle
Major Phases:
Late Diastole: Both chambers relaxed, ventricles fill passively
Atrial Systole: Atria contract, forcing more blood into ventricles
Isovolumic Ventricular Contraction: Ventricles contract, pressure builds, AV valves close
Ventricular Ejection: Semilunar valves open, blood ejected into circulation
Isovolumic Ventricular Relaxation: Semilunar valves close, ventricles relax, and pressure falls
Cardiac Output
Definitions:
Stroke Volume (SV): Amount of blood pumped by one ventricle per contraction
Formula:
Cardiac Output (CO): Volume of blood pumped by one ventricle over time
Formula:
Average CO = 5 L/min
Factors Influencing Stroke Volume:
Frank-Starling law: Stroke volume increases with end-diastolic volume (EDV)
Affected by venous return, sympathetic innervation, and length-force relationships
Electrical Conduction in the Heart
Components:
SA node (70 bpm, natural pacemaker)
AV node (50 bpm)
Purkinje fibers (25-40 bpm under certain conditions)
Paths of Electrical Activity:
Depolarization spreads from SA node to AV node via internodal pathways
Slower conduction through the AV node allows for atrial contraction before ventricular depolarization
ECG Waves:
P Wave: Represents atrial depolarization
QRS Complex: Represents ventricular depolarization
T Wave: Represents ventricular repolarization
Modulation of Heart Rate by the Autonomic Nervous System
Sympathetic Nervous System: Increases heart rate through norepinephrine, enhancing depolarization rates
Parasympathetic Nervous System: Decreases heart rate through acetylcholine, causing hyperpolarization and slower depolarization
Summary of Action Potentials
Comparison:
Contractile Myocardium vs. Skeletal Muscle
Cardiac muscle has a prolonged action potential due to calcium influx, unlike skeletal muscle which has a short refractory period
Einthoven’s Triangle: Method for recording the electrical activity of the heart using electrode placement on the body