The Female Reproductive System
Vocabulary
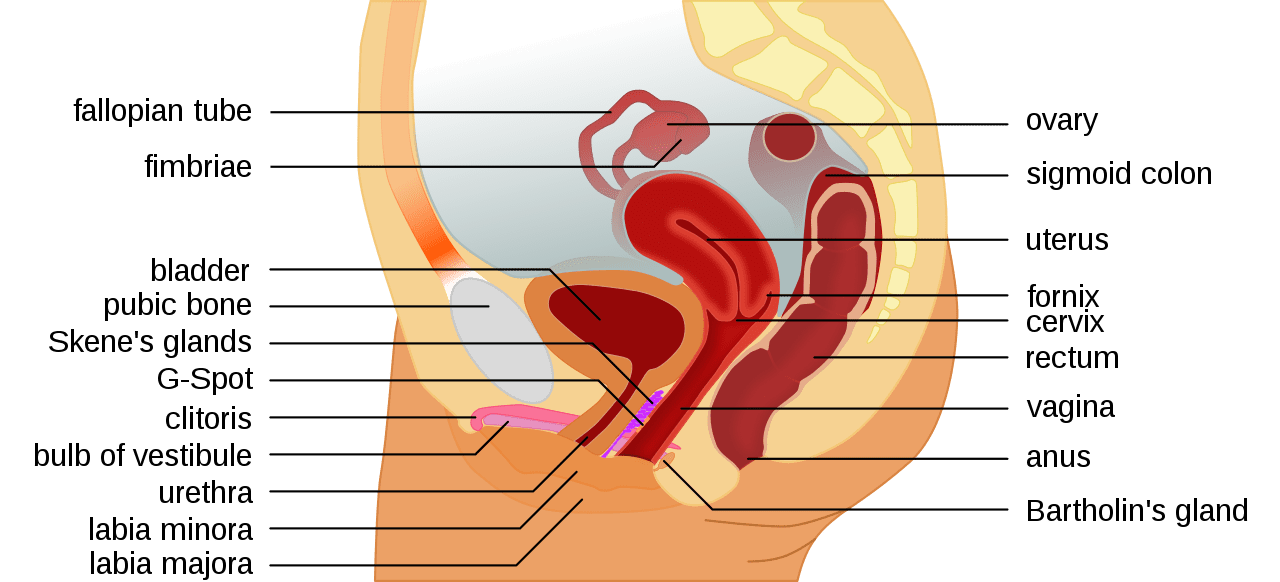
Ovaries- The primary female reproductive organs, or gonads, are the two ovaries.
Fallopian tubes- The female structures that transport the ova from the ovary to the uterus each month. In the presence of sperm and fertilization, the uterine tubes transport the fertilized egg to the uterus for implantation.
Uterus- The uterus, also known as the womb, is a female reproductive organ that is responsible for many functions in the processes of implantation, gestation, menstruation, and labor.
Cervix- The cervix connects the body of the uterus to the vagina. Part of the lining of the cervix contains glands that make and release mucus. For most of the menstrual cycle and during pregnancy, the mucus is thick and stops sperm from entering the uterus
Vagina- The vagina has 3 main functions: provides a passageway for blood and mucosal tissue from the uterus during a woman’s monthly period. receives the penis during sexual intercourse and holds the sperm until they pass into the uterus. provides a passageway for childbirth.
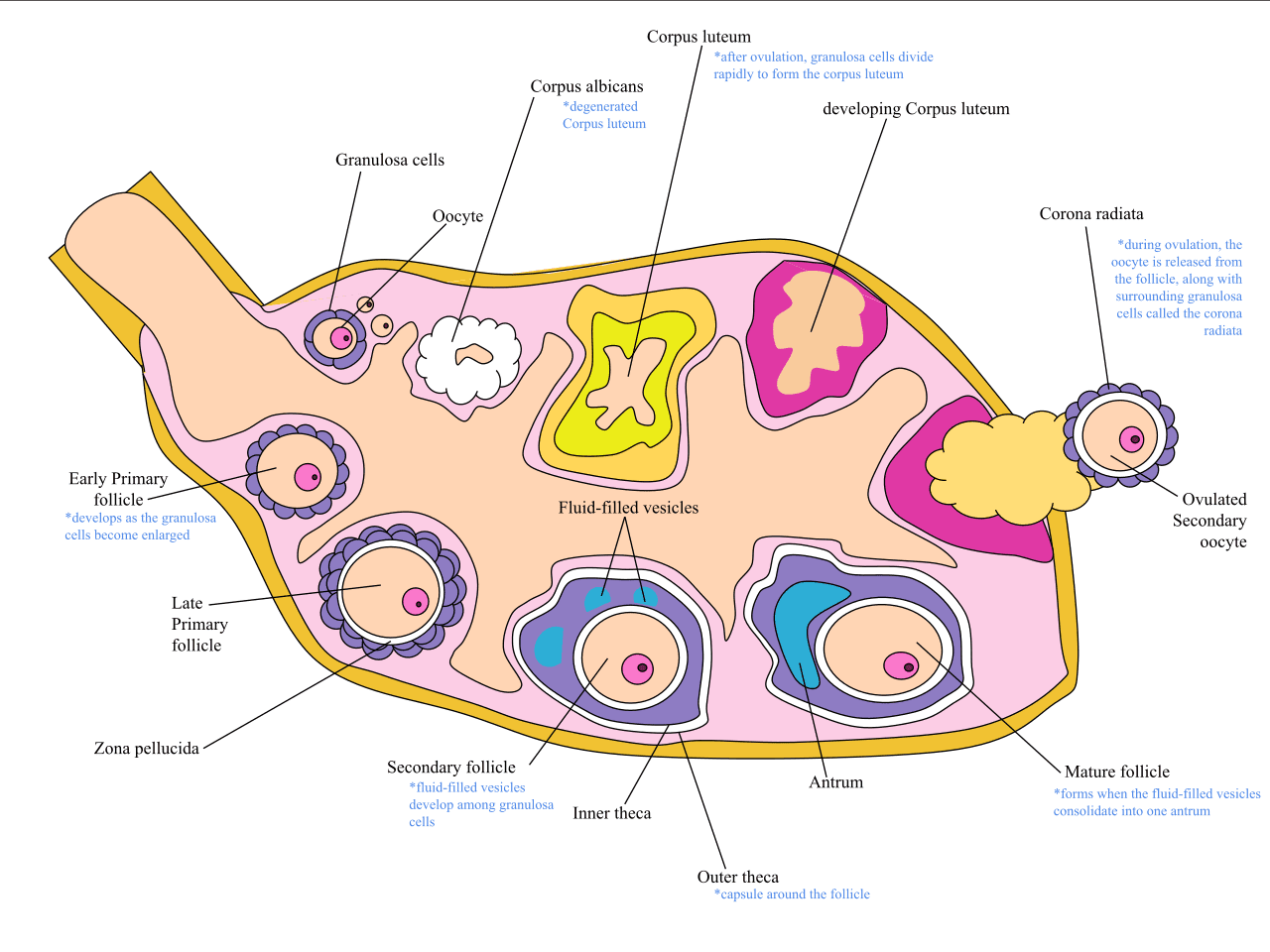
Ovarian follicles (Graafian follicles)- are rounded enclosures for the developing ova in the cortex near the surface of the ovary, providing for the maturation and release of a fertilizable oocyte (ovum),it also forms the corpus luteum, which promotes and maintains implantation of the embryo.
The Female Reproductive System
The primary reproductive system organs in the female are the ovaries. The ovaries contain the oocytes which mature during the ovarian cycle.
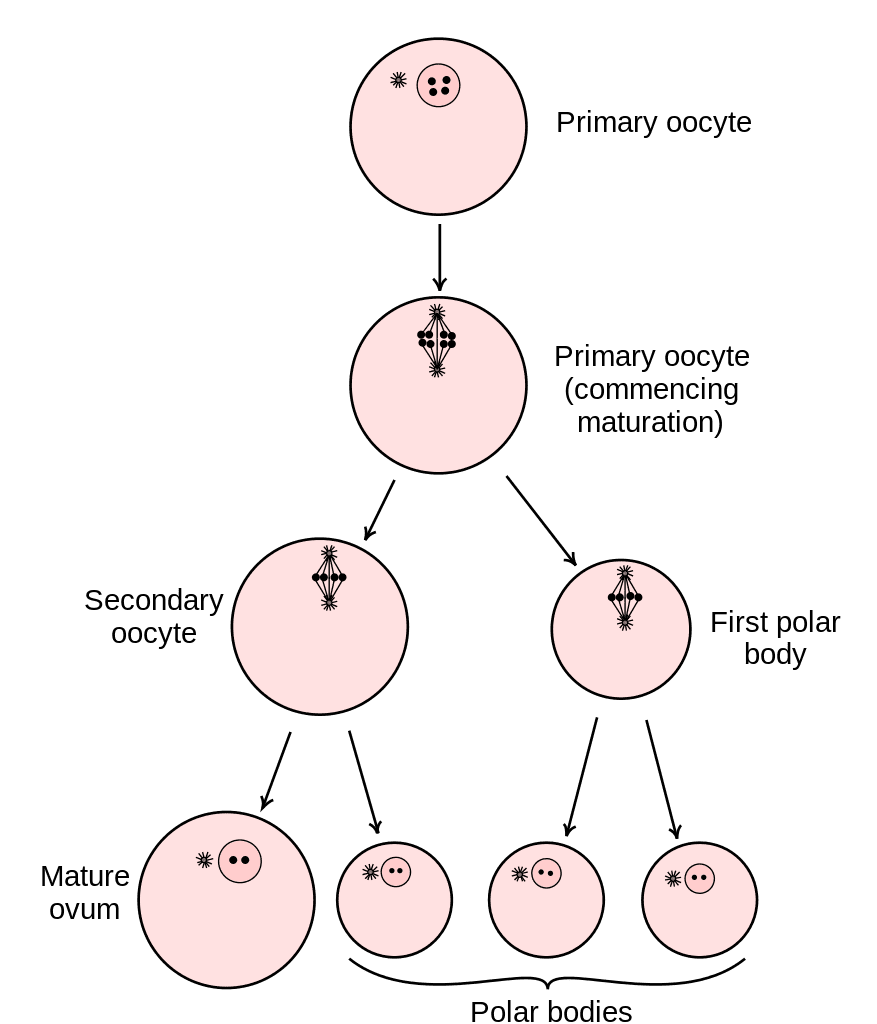
The oocytes develop by way of a process called oogenesis. During oogenesis a primary oocyte develops into a secondary oocyte. The primary oocyte is diploid, so it contains all 46 chromosomes. As it undergoes meiosis it becomes a haploid secondary oocyte which only contains 23 chromosomes. The other 23 chromosomes are eliminated as a polar body. Here maturation ceases unless fertilization occurs which produces a zygote which again has 46 chromosomes—23 from the female and 23 from the male.
The fallopian tube connects to the ovary by way of finger like projections called fimbrae. The fallopian tube connects to the uterus which is a muscular organ containing 3 layers which include the outer perimetrium, middle smooth muscle myometrium layer and inner endometrium which is the layer that is eliminated during menstruation.
The cervix is at the tip of the uterus with the remaining structures including the vagina and outer vulva which contain the labia major and minor and clitoris.
The female menstrual cycle begins at puberty and continues until menopause. During a cycle a follicle begins to mature under the control of follicle stimulating hormone secreted by the anterior pituitary gland.
As the follicle matures, it secretes estrogen and progesterone. Both work to enlarge the endometrium and supply it with blood vessels to make it ready for potential implantation of a fertilized oocyte. A mature follicle is called Graafian Follicle.
About midway through the cycle, a surge of luteinizing hormone causes ovulation whereby the follicle releases the oocyte from the ovary.
The follicle remains as a corpus luteum which continues to secrete estrogen and progesterone. The corpus luteum then degenerates into a corpus albicans and the levels of estrogen and progesterone drop causes menstruation.
Estrogen is the primary female hormone and works to first develop the female reproductive system in utero and then finishes maturation of the female during puberty.
Testosterone is also present in females. The role of testosterone is to promote muscle development, bone growth, the development of secondary sex characteristics, and maintaining libido (sex drive) in both males and females.
A fertilized oocyte or zygote (single cell) will develop into a blastocyst (group of cells) that travels though the fallopian tube to the uterus for implantation. A significant percentage (50–75 percent) of blastocysts fail to implant
When this occurs, the blastocyst is shed with the endometrium during menses.
The high rate of implantation failure is one reason why pregnancy typically requires several ovulation cycles to achieve.
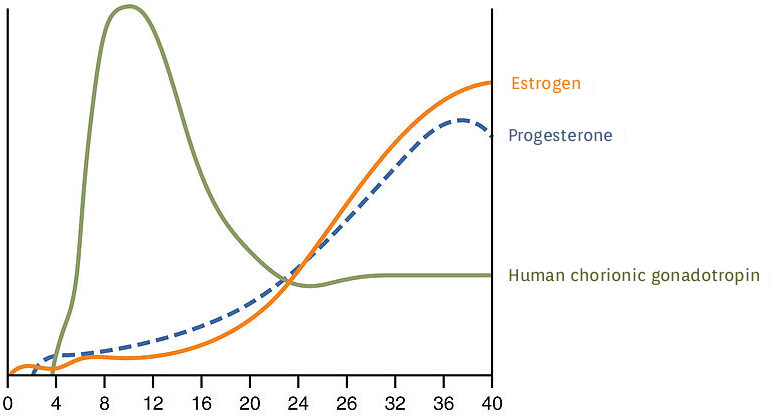
The outer layer of the blastocyst or trophoblast secretes human chorionic gonadotrophin (hCG) hormone which directs the corpus luteum to survive, enlarge, and continue producing progesterone and estrogen to suppress menses.
Study the Female Reproductive System in the following images.

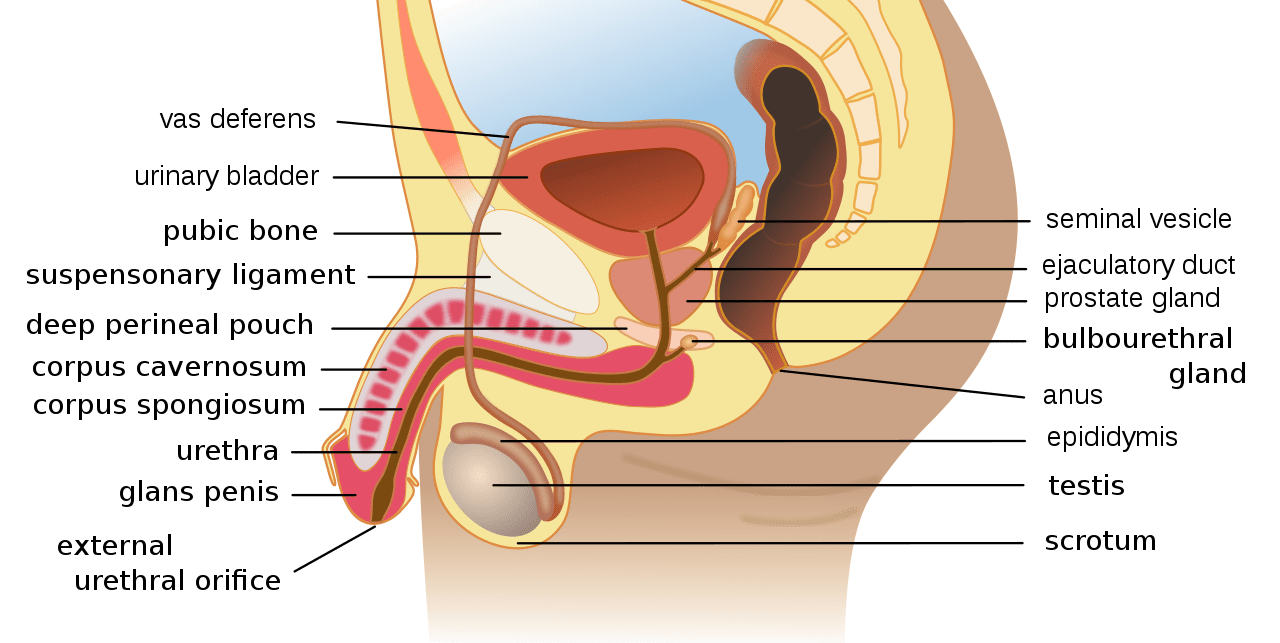
The Male Reproductive System
Vocabulary
Penis- the male genital organ carrying the duct for the transfer of sperm during copulation; consists largely of erectile tissue and serves also for the elimination of urine.
Scrotum- the sac that holds testes away from the body to maintain lower temperature during sperm production
Vas deferens- thick-walled tube in the male reproductive system that transports sperm cells from the epididymis, where the sperm are stored prior to ejaculation.
Testes- primary reproductive organ
Seminiferous tubules- reside in testes and produce sperm
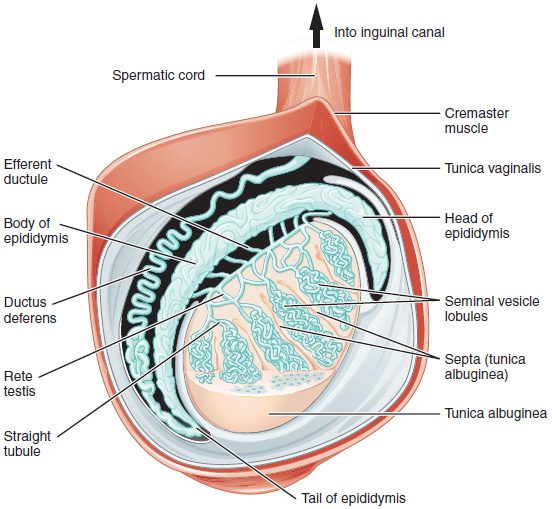
Epidymus- a highly convoluted duct behind the testis, along which sperm passes to the vas deferens
Bulbourethral gland– gland just inferior to the prostate gland that secretes mucous
Introduction
The reproductive system includes complex anatomical components as well as hormones and secretions. The baseline knowledge of this body system will significantly support your success on the TEAS as well as future success in the nursing program. The mastery of the anatomical and physiologic components of the reproductive system now will be pivotal as you learn a variety of disease processes, disorders, and other abnormalities in the nursing program. You will be able to refer to this content as remediation upon entry into the nursing program.
The Male Reproductive System
The testes are the primary reproductive organs of the male system. The testes are tubular glands located in a pouch-like structure called the scrotum which keeps the testes at slightly lower temperature than body temperature which is more conducive to sperm development.
Inside the testes are a series of tubes called seminiferous tubules. Sperm cells reside on the perimeter of the tubules and mature as they enter the hollow portion or lumen.
The seminiferous tubules allow sperm to move into the epididymis, which is another tubular structure that stores sperm prior to ejaculation and helps them to continue to mature. Sperm move through the epididymis in about 10-15 days.
Sperm then travel to the vas deferens which is lined with smooth muscle which can perform rhythmic contractions during ejaculation which help to move the sperm to the prostatic duct.
The prostate gland is located inferior to the bladder and the seminal vesicle is located just posterior to the prostate gland.
The seminal vesicle produces fluids which help to nourish the sperm and the prostate gland produces an alkaline fluid to help move the sperm along.
Sperm pass though the prostatic duct to the urethra. The sections of the urethra include the prostatic, membranous, and penile urethras.
The bulbourethral gland or Cowper’s gland is located just below the prostate gland. This gland secretes mucous in response to sexual stimulation.
The penis contains 2 columns of tissue called corpora cavernosa and 1 column called the corpora spongiosum.
There are deep arteries in each corporal cavernosa that transport blood during an erection which is under parasympathetic control. The corpus spongiosum contains the urethra.
Sperm cells develop by way of spermatogenesis. Here a spermatogonium matures under the influence of hormones and becomes a primary spermatocyte. The primary spermatocyte contains the full 46 chromosomes which is called a diploid cell. As the primary spermatocyte matures into a secondary spermatocyte during a process called meiosis, each secondary spermatocyte contains only 23 chromosomes which is called a haploid cell. The sperm then continue to mature as the move into the lumen of the seminiferous tubules.
The primary male reproductive hormone is testosterone. Testosterone moderates the development of the male reproductive system during fetal development and then again during puberty where it completes maturation of the male.
Testosterone is secreted in response to hormones from the hypothalamus and anterior pituitary. Gonadotropin releasing hormone secreted by the hypothalamus promotes the secretion of follicle stimulating and luteinizing hormones from the anterior pituitary gland. These hormones stimulate production of testosterone by the testes. Testosterone also feeds back to the hypothalamus to inhibit the secretion of gonadotropin releasing hormone. This helps to regulate testosterone levels.
Study the Male Reproductive System in the images below.