Trends and Issues
Chapter 1
LEARNING OBJECTIVES
Discuss current evidence-based nursing care that promotes optimal outcomes in labor and birth.
Examine maternal and infant health outcomes in the United States and analyze how social determinants of health impact outcomes, leading to health disparities.
Identify leading causes of maternal and infant morbidity and mortality in the United States.
Discuss current maternal and infant health issues.
Identify the primary maternal and infant goals of Healthy People 2030.
WELCOMING AND INCLUSIVE CARE
Social Determinants of Health: Factors that impact individual and community health outcomes, including:
Housing and Neighborhood Environment: Quality and stability of housing and neighborhood infrastructure.
Economic Stability: Employment, income level, and financial resources.
Access to Health Care and Quality of Care: Availability and quality of health services.
Community and Social Context: Interconnectedness and support systems, including the impact of racism and discrimination.
CHANGES IN LAST 50 YEARS
Influence of organizations and initiatives in maternal and newborn health:
La Leche League: Advocacy for breastfeeding and maternal support.
Association of Women’s Health, Obstetric and Neonatal Nurses (AWHONN): Promotes optimal healthcare for women and newborns.
Baby-Friendly Hospital Initiatives: Encouraging breastfeeding and proper infant care.
Safe to Sleep: Campaign addressing sudden infant death syndrome (SIDS) through safe sleep practices.
Black Mamas Matter Alliance: Advocacy focused on improving maternal health outcomes for Black women.
INFANT MORTALITY
Definition: Death of an infant before the first birthday.
Global Infant Mortality Rates: Variations observed worldwide, with data accessible at the CIA World Factbook.
U.S. Infant Mortality Rates:
Current rate: 5.1 deaths per 1,000 live births.
U.S. ranking: #173 out of 227 countries.
Five Leading Causes of Infant Deaths:
Congenital malformations and chromosomal abnormalities.
Disorders related to short gestation and low birth weight.
Sudden Infant Death Syndrome (SIDS).
Respiratory Distress in Newborns.
Newborns affected by maternal complications of pregnancy.
MATERNAL MORTALITY
Definition: Death of a woman during pregnancy, childbirth, or within 42 days of termination of pregnancy.
Causes of Maternal Mortality According to WHO: Various health and socio-economic factors contribute to the risk of maternal mortality.
Risk Disparities: Black women have a higher risk of maternal death compared to white or Hispanic women, highlighting systemic health inequalities.
OTHER ISSUES IN MATERNAL NEWBORN NURSING
Teen Pregnancy: Increased health risks for both mother and child.
Tobacco/E-Cig Use in Pregnancy: Adverse effects on fetal development.
Substance Abuse in Pregnancy: Impact on maternal health and infant outcomes, including exposure to addiction-related complications.
Overweight and Obesity: Associated risks for both maternal and infant health.
Violence: Domestic violence affects maternal mental health and safety.
LGBTQIA+ Care: Addressing specific health needs and promoting inclusivity in care.
Racism and Discrimination: Their role in impacting health outcomes for marginalized communities.
Healthy People 2030 Goals
CHAPTER 2: ETHICS AND STANDARDS OF PRACTICE ISSUES - Maternal Newborn Nursing
LEARNING OUTCOMES
Debate ethical issues in maternity nursing, including autonomy, beneficence, and justice.
Explore standards of practice in maternity nursing that guide ethical decision-making.
Describe legal issues pertaining to maternity nursing and potential areas for malpractice.
Analyze concepts related to evidence-based practice in maternity care.
UNIQUE CHALLENGES OF ETHICS IN OBSTETRICS
Ethical considerations include:
Balancing the needs and rights of the mother and fetus.
Addressing dilemmas that arise during pregnancy and childbirth.
AMERICAN NURSES ASSOCIATION (ANA) CODE OF ETHICS
Ethical principles outlined in the code:
Beneficence: Acting in the best interest of the patient.
Nonmaleficence: To do no harm.
Respect for Autonomy: Upholding patients’ rights to make informed decisions.
Justice: Fair treatment in health care.
ETHICAL DILEMMAS
Obligations and duties to mother and fetus
Because maternity nurses must advocate for both maternal and fetal well-being, it may not be possible to “do the right thing” for both.
Dilemmas
Ethical dilemma refers to when there is difficulty in deciding which action takes precedence over the other.
Moral distress
ETHICS IN NEONATAL CARE
Ethical obligations
Counterbalancing–to do no harm
Veracity to parents
Autonomy: respect parental decisions, facilitate communication and collaboration
Categories for neonates in the NICU may include:
Infants for whom aggressive care would probably be futile, where prognosis for a meaningful life is extremely poor or hopeless.
Infants for whom aggressive care would probably result in clear benefit to overall well-being, where prevailing knowledge and evidence indicate excellent chances for beneficial outcomes and meaningful interactions.
Infants for whom the effect of aggressive care is mostly uncertain.
NURSES’ RIGHTS AND RESPONSIBILITIES
AWHONN supports nurses’ rights
Nurses should not abandon a patient nor refuse to provide care based on prejudice or bias.
Nurses have the professional responsibility to provide high-quality, impartial nursing care to all patients in emergency situations, regardless of the nurses’ personal beliefs.
Nurses have a professional obligation to inform their employers of any attitudes and beliefs that may interfere with essential job functions.
AWHONN core values: CARING acronym
Commitment to professional and social responsibility
Accountability for personal and professional contribution
Respect for diversity of and among colleagues and clients
Integrity in exemplifying the highest standards in personal and professional behavior
Nursing excellence for quality outcomes in practice, education, research, advocacy, and management
Generation of knowledge to enhance the science and practice of nursing to improve the health of women and newborns
STANDARDS OF PRACTICE
Standards of Practice serve as guidelines determining the scope of practice for nurses, informed by:
The state nurse practice act, HIPAA regulations, and defined roles of the nurse.
AWHONN standards of research and clinical practice, ensuring quality care.
LEGAL ISSUES IN MATERNITY
Maternity: most litigious practice area
Evidence-based practice (EBP) is the gold standard. Problem areas include clinical judgment, communication, and collaboration.
“Failure to communicate” leads to most malpractice suits against nurses.
Five clinical situations account for most fetal and neonatal injuries and litigation in obstetrics (Simpson, 2014):
Inability to recognize or inability to appropriately respond to intrapartum fetal compromise
Inability to perform a timely cesarean birth (30 minutes from decision to incision) when indicated by fetal or maternal condition
Inability to appropriately initiate resuscitation of a depressed neonate
Inappropriate use of oxytocin or misoprostol, leading to uterine tachysystole, uterine rupture, and fetal intolerance of labor or fetal death
Inappropriate use of forceps/vacuum or preventable shoulder dystocia
FETAL HEART RATE MONITORING
Legally important: failure to assess correctly
Safe and effective fetal heart rate (FHR) assessment
Risk management issues
EVIDENCE-BASED PRACTICE
Professional Organizations involved include:
American College of Obstetricians & Gynecologists (ACOG).
Association of Women's Health, Obstetric & Neonatal Nursing (AWHONN).
Centers for Disease Control (CDC).
Professional Journals
Training, Certifications & Professional Organizations
Certifications can be obtained from American Nurses Credentialling Center (ANCC) and other specialty groups, requires years of practice and an exam.
Neonatal Resuscitation Program (NRP)
S.T.A.B.L.E. Program
Electronic Fetal Monitoring (EFM) certification.
Certification exams required for specialization may include requirements for years of practice.
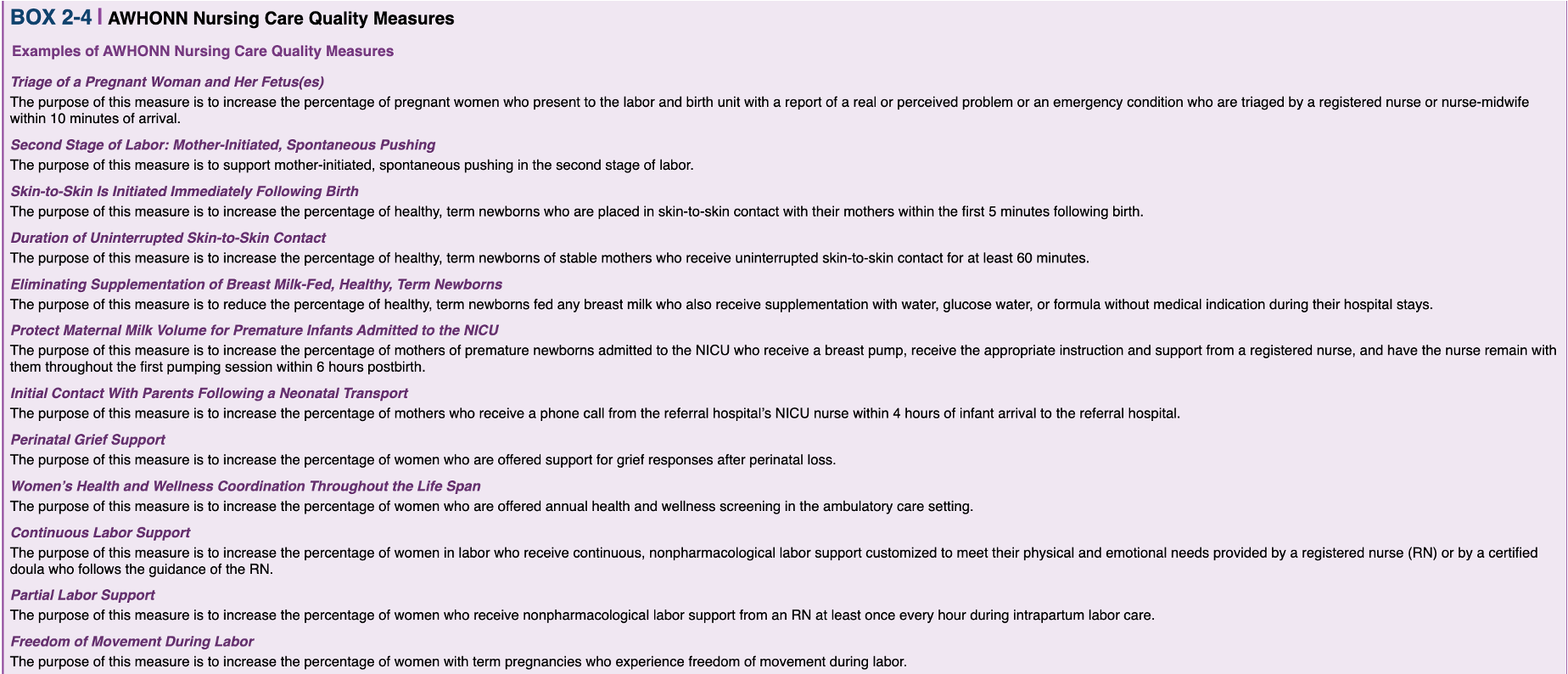
AWHONN Perinatal Quality Measures