Midterm
List facts about:
AAPD (American Academy of Pediatric Dentistry)
Definition: advocates policies, guidelines, and oral health care for children
1st dental visit BEFORE 12 months
early morning/after nap
Recall every 4–6 months or as needed

ADA (American Dental Association)
Recommend soft bristles
recommends a minimum of 2x daily
List of approved products on the website
AAPD / ADA Age Classification
Infant: Under 1 year
Toddler: 1–3 years
Preschooler: 3–5 years
School-age: 6–11 years
Adolescent: 12–17 years

ADA Seal of Approval (1931)
Evaluate OTC products for safety and effectiveness
voluntary
awarded after full review of effectiveness/safety
acceptance is for 5 years
use must have an ADA approval statement
lack of seal does not mean unsafe or ineffective

ADHA (American Dental Hygienist Association)

CDC (Centers for Disease Control and Prevention)

FDA
Cosmetic: Cleans or improves appearance only (whitening, fresh breath).
Therapeutic: Prevents or treats disease (caries prevention, gingivitis reduction).

CAMBRA
What does CAMBRA stand for?
Caries management by risk assessment
What is the purpose of CAMBRA?
assessment data to determine caries risk level for children under 6 or adults (over 6+)
classify child’s risk levels

Early Childhood Caries (ECC)
List factors/microbes that contribute to ECC
high level of S. mutans in biofilm → risk factor
transfer by saliva-sharing behaviors (AVOID)
Lactobacilli and Candida contribute
Predisposing factors: bottle in bed, prolonged breastfeeding
Pattern: maxillary anteriors → primary molars
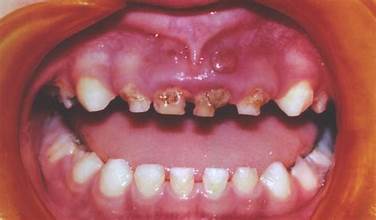
List facts about ECC
Also known as: Nursing bottle caries, baby bottle caries, or rampant caries.
presence of 1 or more decayed, missing, or filled tooth surfaces in any primary tooth in a child under 6
S-ECC → child under 3 with any smooth-surface caries
Adolescence: One of the highest caries-risk periods, particularly for males
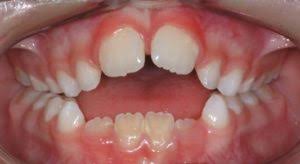
List the consequences of thumb sucking
narrow maxillary arch
anterior open bite
posterior crossbite
increased overjet
decrease overbite
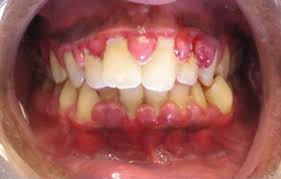
List facts about biofilm-induced gingivitis in adolescents
Severity may increase during puberty
clinical and hormonal changes related to increased biofilm
exaggerated response to biofilm
fluoride supplement chart:
Less than 0.3ppm | 0.3–0.6ppm | More than 0.6ppm | |
|---|---|---|---|
Birth – 6 months | 0 | 0 | 0 |
6 months – 3 years | 0.25ppm | 0 | 0 |
3 years – 6 years | 0.50ppm | 0.25ppm | 0 |
6 years – 16 years | 1.0ppm | 0.50ppm | 0 |

Home Care:
List considerations when choosing oral health aids for patients:
anatomy
ability to perform self-care
product they use
time dedicated to oral health
barriers to self-care

Finance and Usage Factors:
affordability of the product
product upkeep (battery)
current product usage (suggest to the appointment)

Anatomy and Access:
Position of teeth
Embrasure type:
type I: gingiva fills interproximal area
Type II: missing/reduced papilla
Type III: extensive recession; may be lost
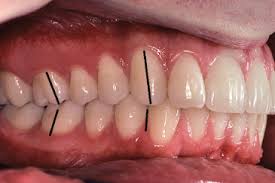
Biofilm and compliance factors:
extent and location of biofilm with BFI
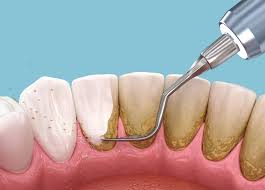
Recommendations for home care
Research shows ____power_____ manual toothbrushes are more effective at biofilm removal by 10-20%

the ADA recommended ____2_____ manual toothbrushes
AM/PM
What toothbrushes are best for patients in orthodontics?
Interdental brushes
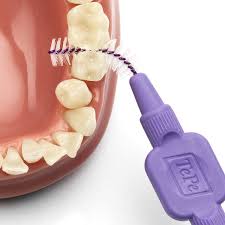
Which teeth are more likely to suffer from toothbrush abrasion?
canine, 1st premolar, bucco/linguoverted teeth
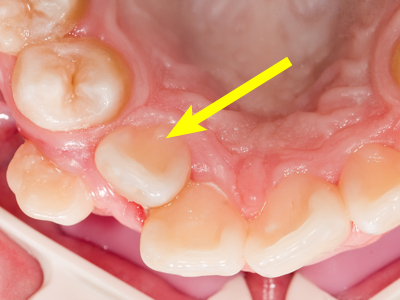
List methods to disinfect toothbrushes and intraoral aids.
3% hydrogen peroxide
CPC/CHX
essential oil rinse
microwave or UV light

When can children start using mouth-rinse?
over 6 years
Under 3 years: Smear (rice-sized amount)
Ages 3–6 years: Pea-sized amount
List defining properties of each toothbrushing method:
Modified Bass | 45° to sulcus, light pressure, vibrate ×10, roll to crown 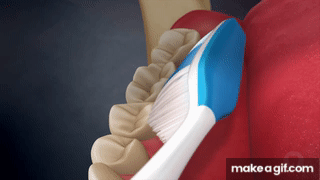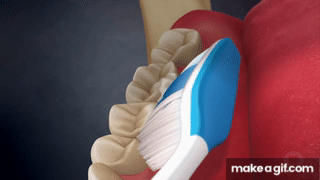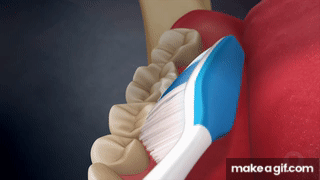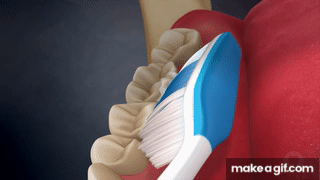 | + Gingival stimulation− Limited subgingival biofilm removal |
Modified Stillman | Filaments partly on gingiva, blanch, vibrate, roll 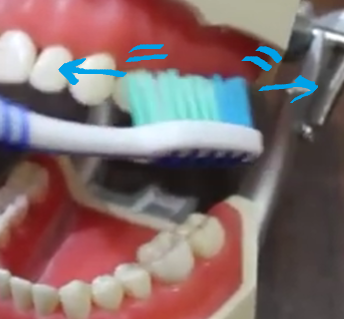 | + Gingival stimulation− Slippage may cause lacerations |
Charters | 45° toward occlusal, rotary strokes 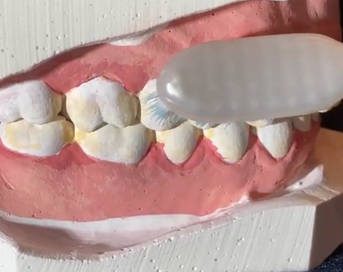 | + Marginal gingiva stimulation− No subgingival removal |
Fones | Teeth edge-to-edge, circular motion 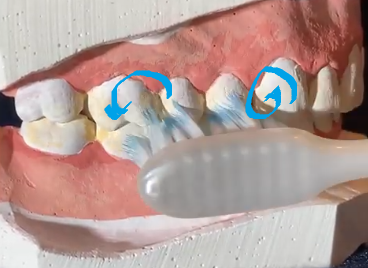 | + Easy for children− Lower biofilm removal |
Leonard | Teeth edge-to-edge, vertical strokes 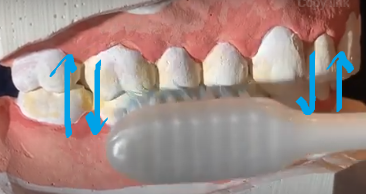 | + Easy for children− Minimal interproximal/sulcular cleaning |
Horizontal Scrub | 90° to tooth, back-and-forth 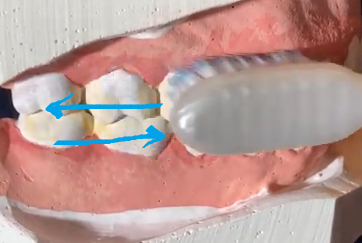 | Only for children <7− Cervical abrasion |
Special Areas: Anterior linguals: Brush vertically, overlapping strokes
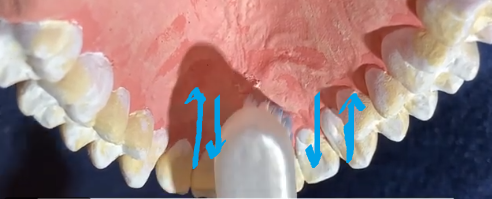
Occlusals: Handle parallel; overlapping strokes and vibration into pits/fissures
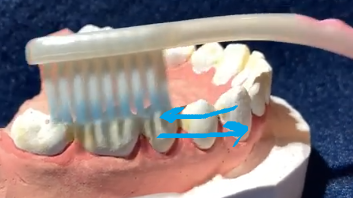
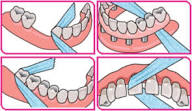
List the best interdental aids for:
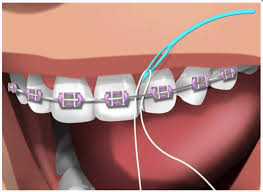
Orthodontics
floss threader
interdental brushes
toothpick holder
water-piks
Bridges
superfloss
interdental brushes
rubber tips
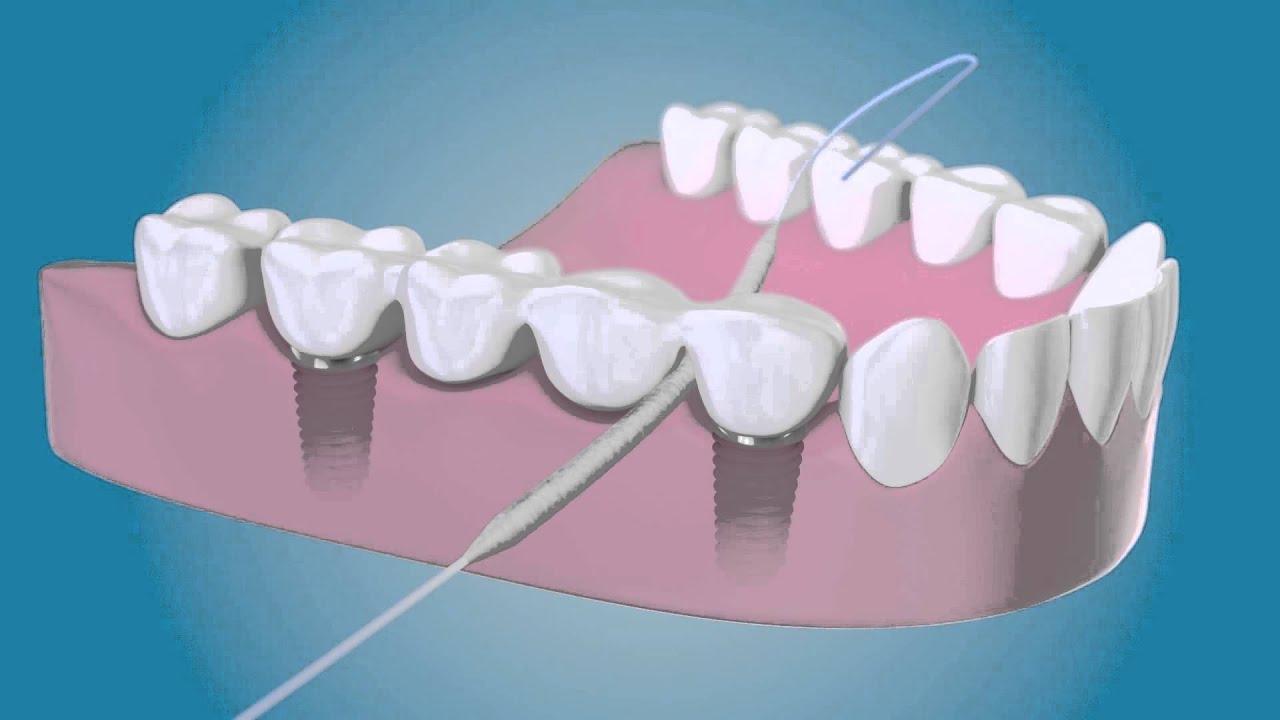
Implants
superfloss
floss threader
interdental brushes
soft-piks
rubber tips
water-piks
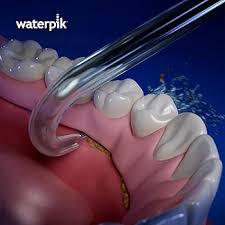
Teeth next to edentulous areas
gauze strips
Type I embrasures
dental floss

Type II embrasures
interdental brushes

Type III embrasures
Stim-U-Dent
For mouthrinses, describe the function of:
Surfactant (detergent)
foam and cleanse
lower surface tension
penetrate/loosen surface deposits
suspension of debris
emulsify/disperse flavor oil
contribute to foaming action

Humectant
moisture stabilizer
retain moisture
prevent hardening when exposed to air
Preservatives
prevent bacterial growth
prolong shelf life

Dyes
adds color

Flavor/sweetener
add pleasantness/freshness
contributes to overall flavor perception

Alcohol
enhances flavor impact
contributes to cleaning
acts as perservative

Water
major vehicle to carry ingredients

Process of Removable Appliances in Clinic
Place wet paper towels in denture cup.
Give patient tissue and instruct them to remove appliance.
If tight, apply even vertical pressure — avoid pulling on clasp.
Inspect appliance for defects.
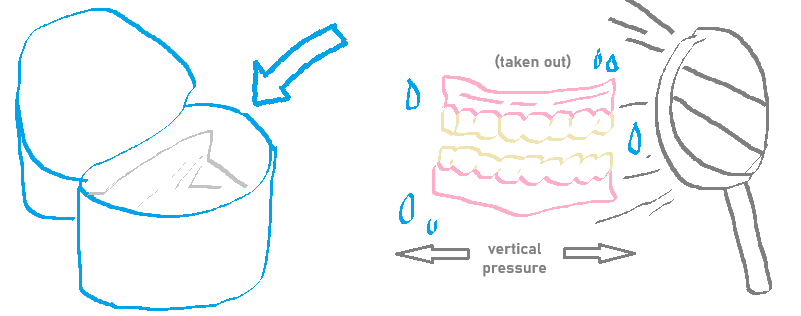
Place appliance in denture cup to transport for sterilization
Double-bag:
Write patient’s name on outer bag.
Put cleaning solution in inner bag with appliance.
Seal bag and place in ultrasonic cleaner for 10 minutes
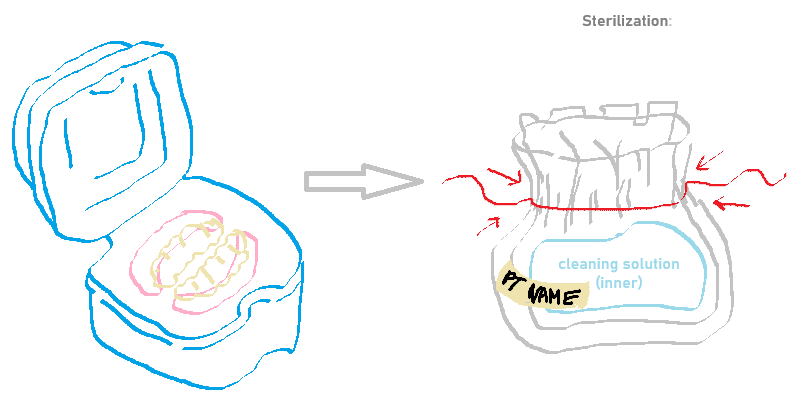
Remove bag and discard.
Rinse appliance under warm water.
Clean with denture brush to remove debris.
Place wet paper towel in denture cup and set appliances on top.
Allow patient to inspect and reinsert appliance.
Return empty denture cup and brush to care bag
After removing ortho brackets, fluoride can remineralize up to:
38-44%
Define: Oral Concerns
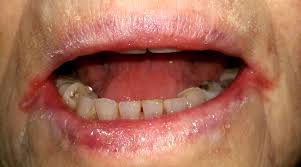
Angular cheilitis
inflammation of the corners of the mouth
nutrient deficiency, fungal or yeast infection, loss of vertical dimension
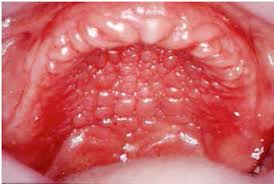
Denture stomatitis
inflammation of the oral mucosa under a prosthesis
Tissue hyperplasia
excessive growth of tissue in response to inflammation or trauma
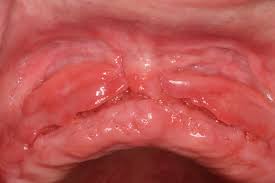
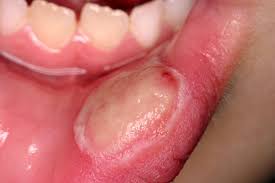
Traumatic ulceration
isolated, red, inflamed area surrounding ulcerated lesions
Fixed/Removable Appliances:
List the purposes for replacing missing teeth
preserves alveolar bone
enhances oral functions
improved psychological impact
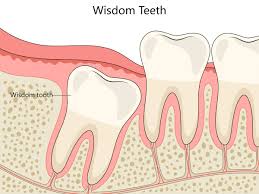
Which teeth are usually not replaced?
third molars
extractions for ortho
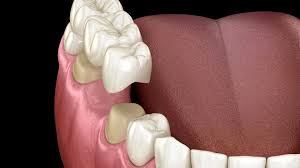
Examples (fixed):
fixed partial prosthesis
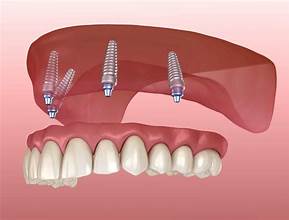
implanted-supported overdentures
fixed ortho appliances
perio splint
space maintainer
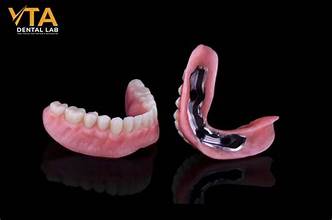
Examples (removable):
removable partial dentures
complete dentures
root-supported overdentures
obturatory
removable ortho appliances
List the best methods to clean around fixed appliances
soft toothbrush
mouth rinse
gum stimulator
superfloss
waterpik
soft pik
non-abrasive dentifrice

Describe:
Abutment
natural tooth or implant supporting pontic
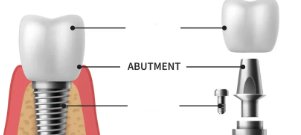
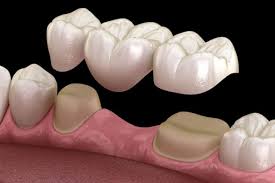
Pontic
false (floating) teeth
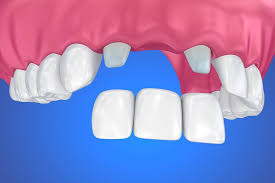
Bridge
fixed partial prosthesis
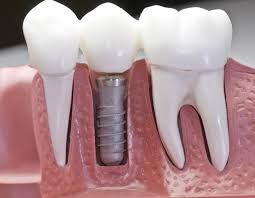
Implant
prosthetic device placed in the jaw to which a tooth or denture may be anchored
Denture Type | Classification | Description and Purpose |
|---|---|---|
Partial Denture | Removable | Replaces only some missing teeth in a dental arch rather than the full set. |
Tissue-supported Denture | Removable | Rests directly on the residual ridges and replaces an entire arch of teeth. |
Interim Denture | Temporary | designed to be replaced by a more definitive restoration at a later time. |
Immediate Denture | Removable | Fabricated for placement immediately following the removal of teeth; it often requires relining or replacement as the bone heals and remodels. |
Implant-supported Denture | Fixed | Anchored to dental implants (prosthetic devices placed in the jaw) |
l