Muscle and Muscle Tissue
Introduction
most distinguishing characteristic of muscle = its ability to turn chemical energy into mechanical energy → contraction
Function of Muscle Tissue: motion, heat production, posture and body support, breathing, speaking, protection of vital organs, regulating elimination of materials
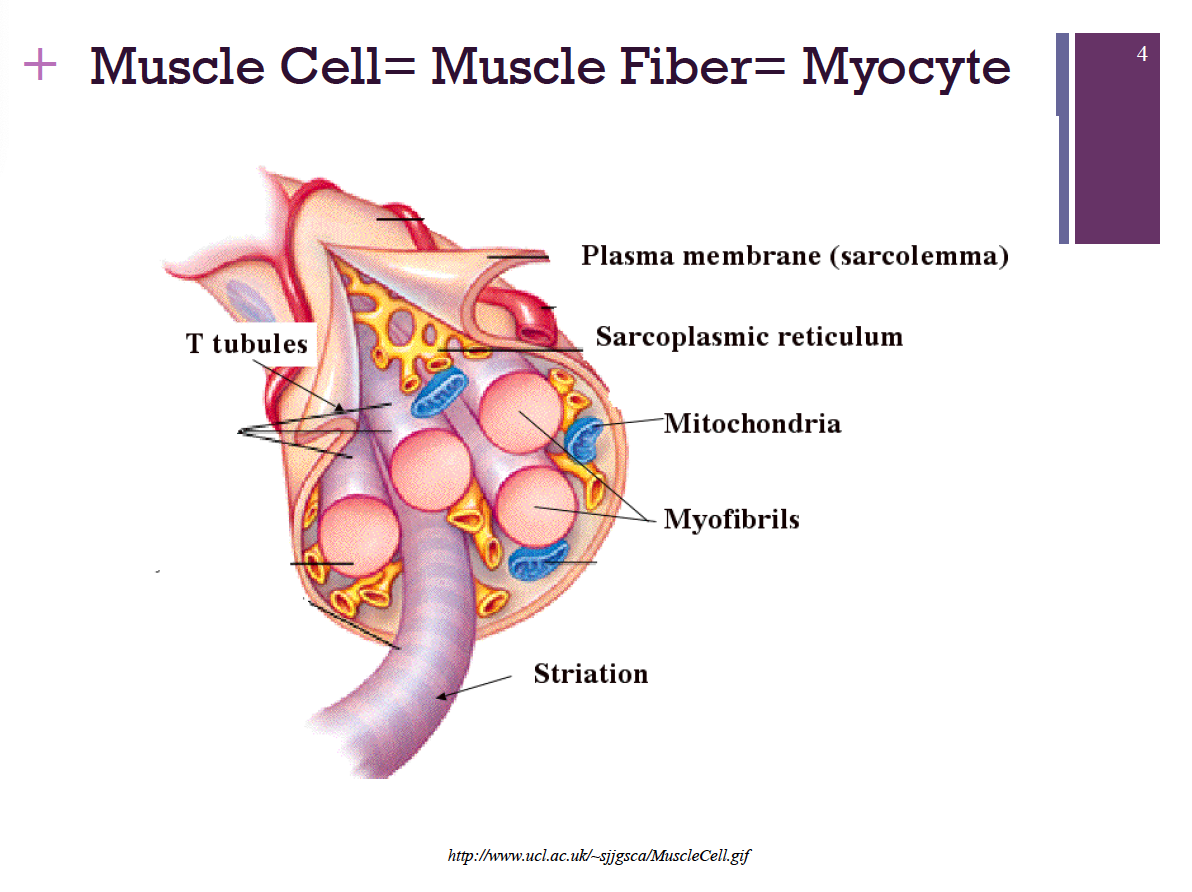
Muscle Terminology/Organelles
sarcolemma: muscle fiber plasma membrane
sarcoplasm: muscle fiber cytoplasm → Contains many glycosomes for glycogen storage, as well as myoglobin for O2 storage
Modified organelles
Myofibrils
Sarcoplasmic reticulum
T tubules
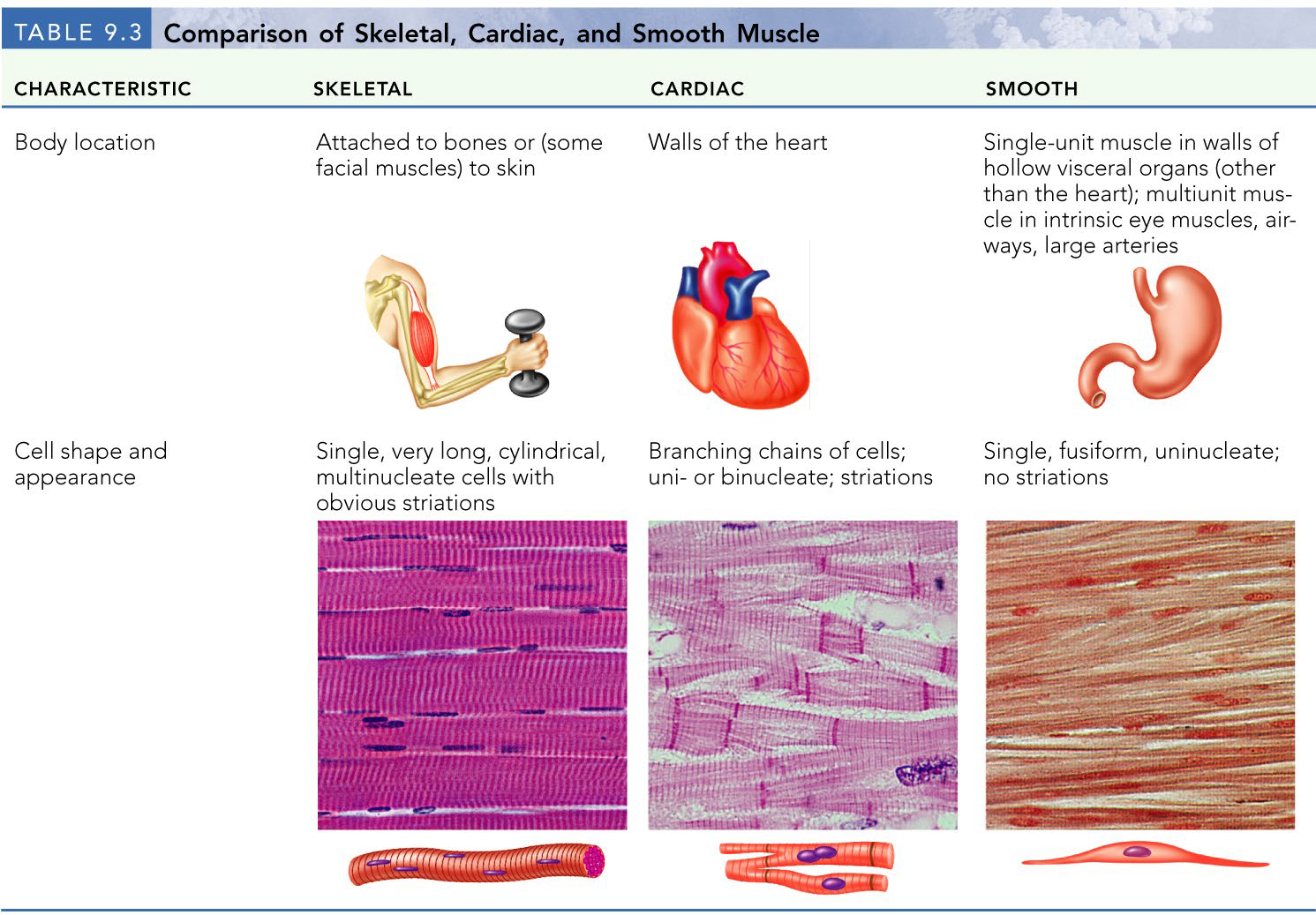
Types of Muscle Tissues
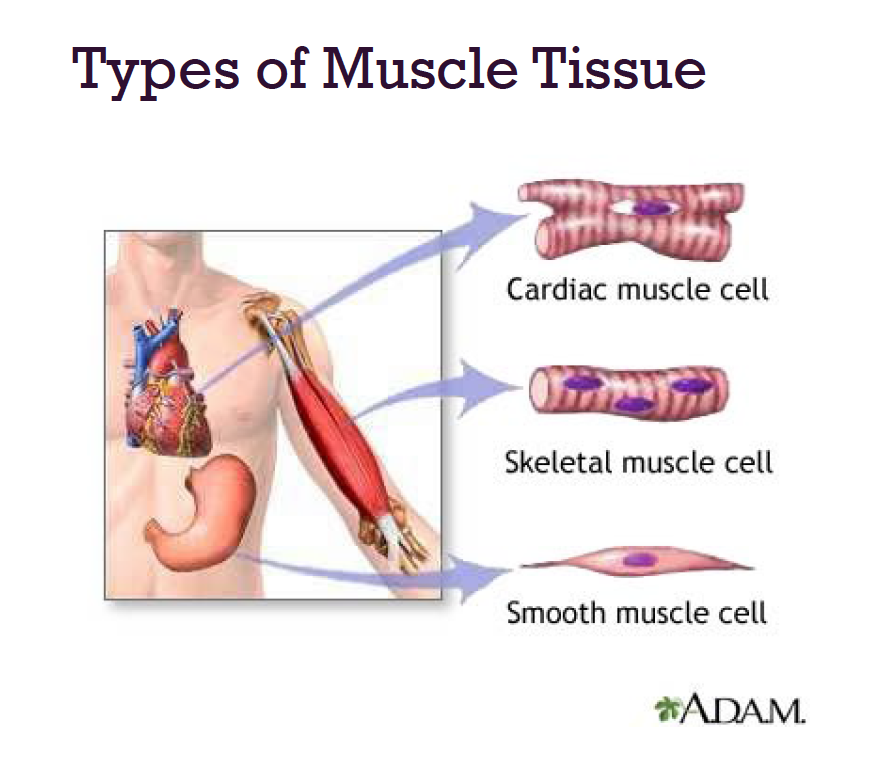
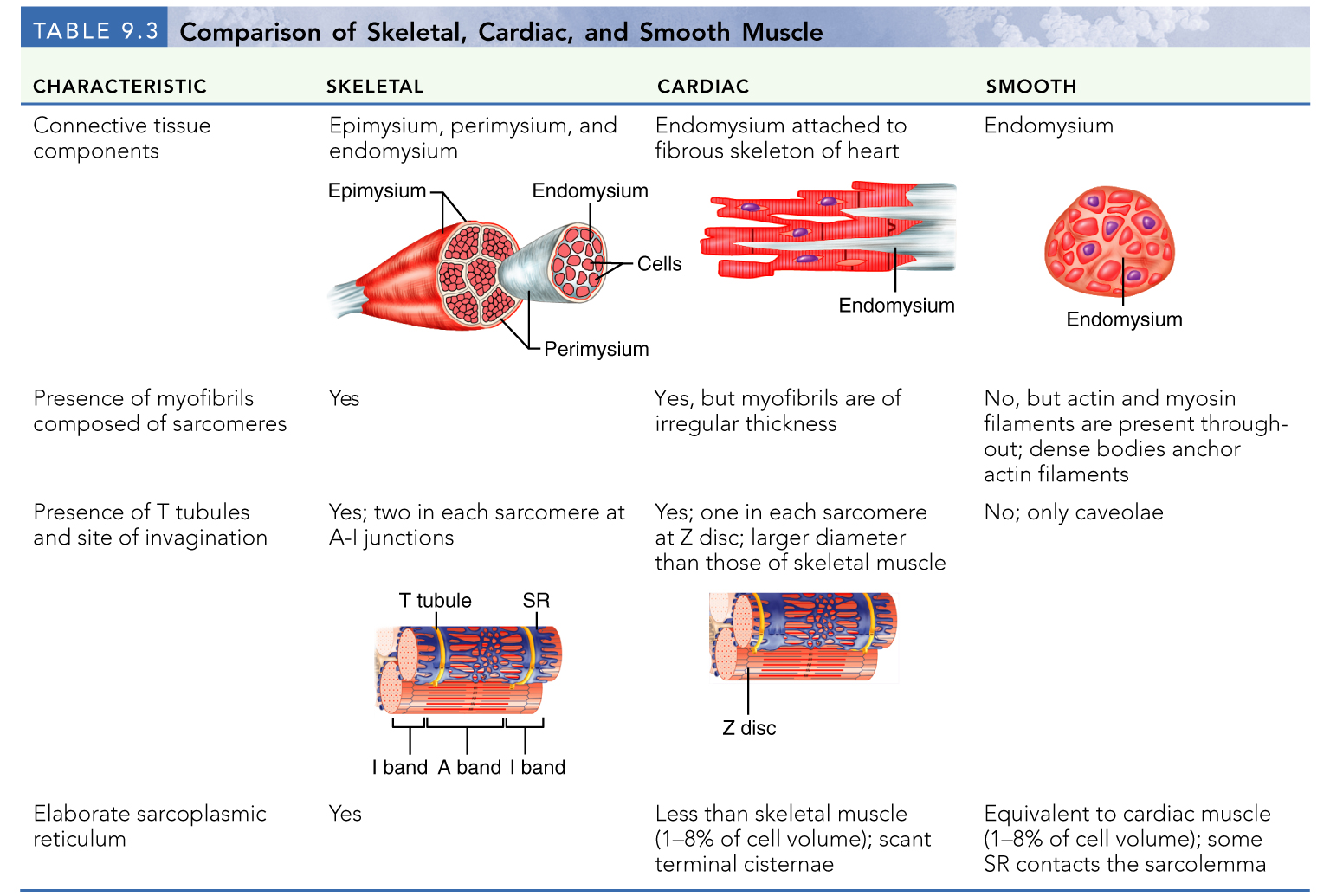
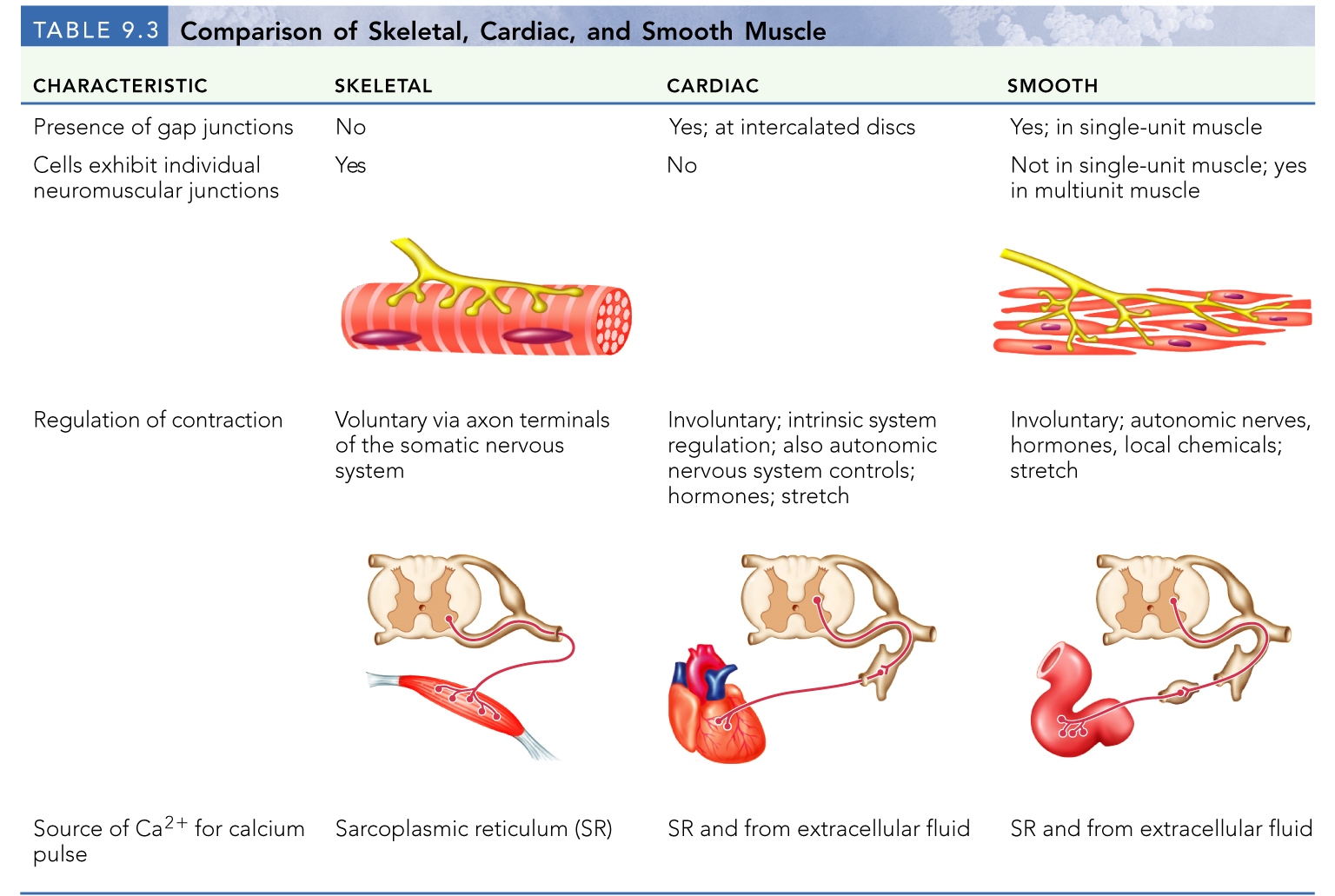
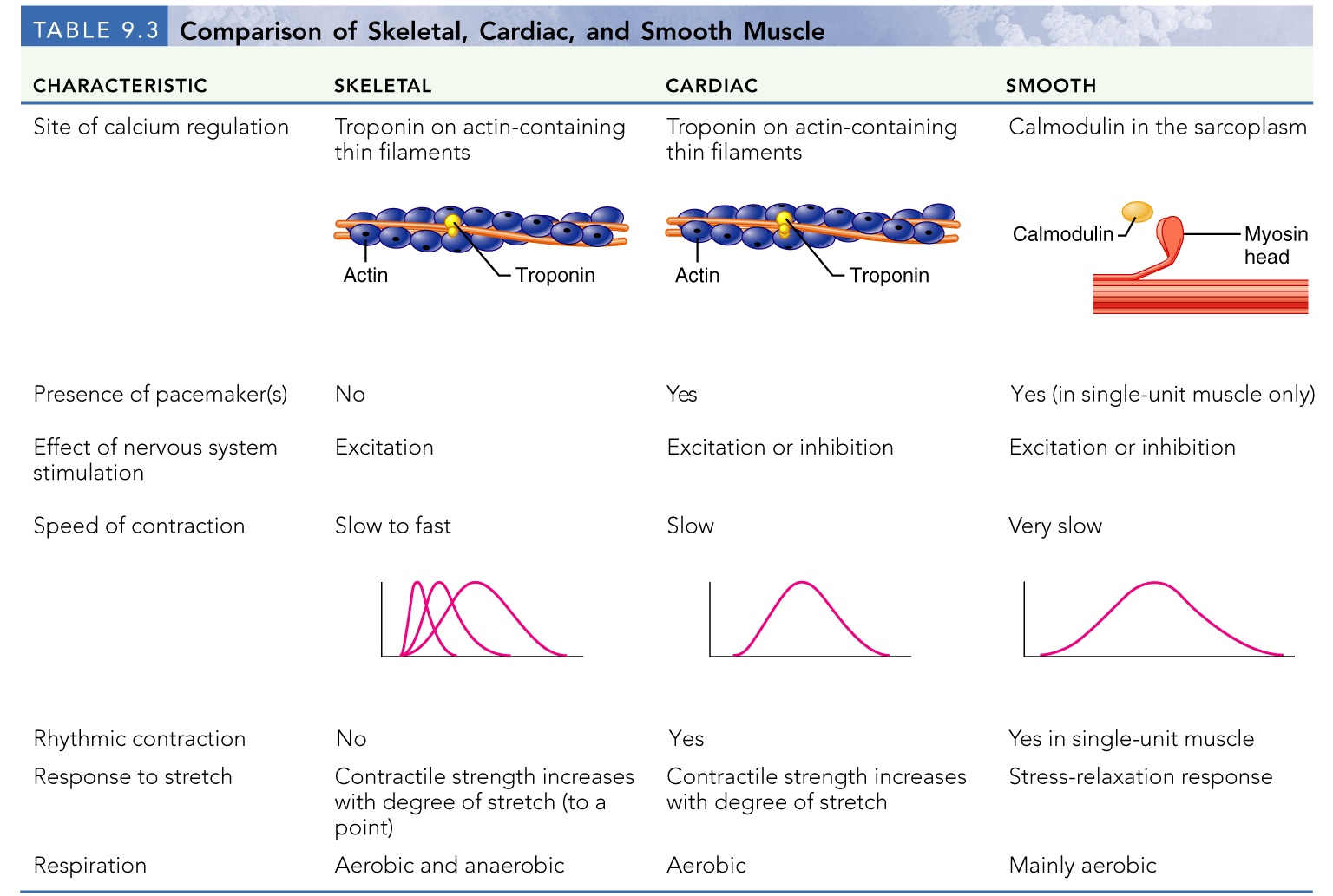
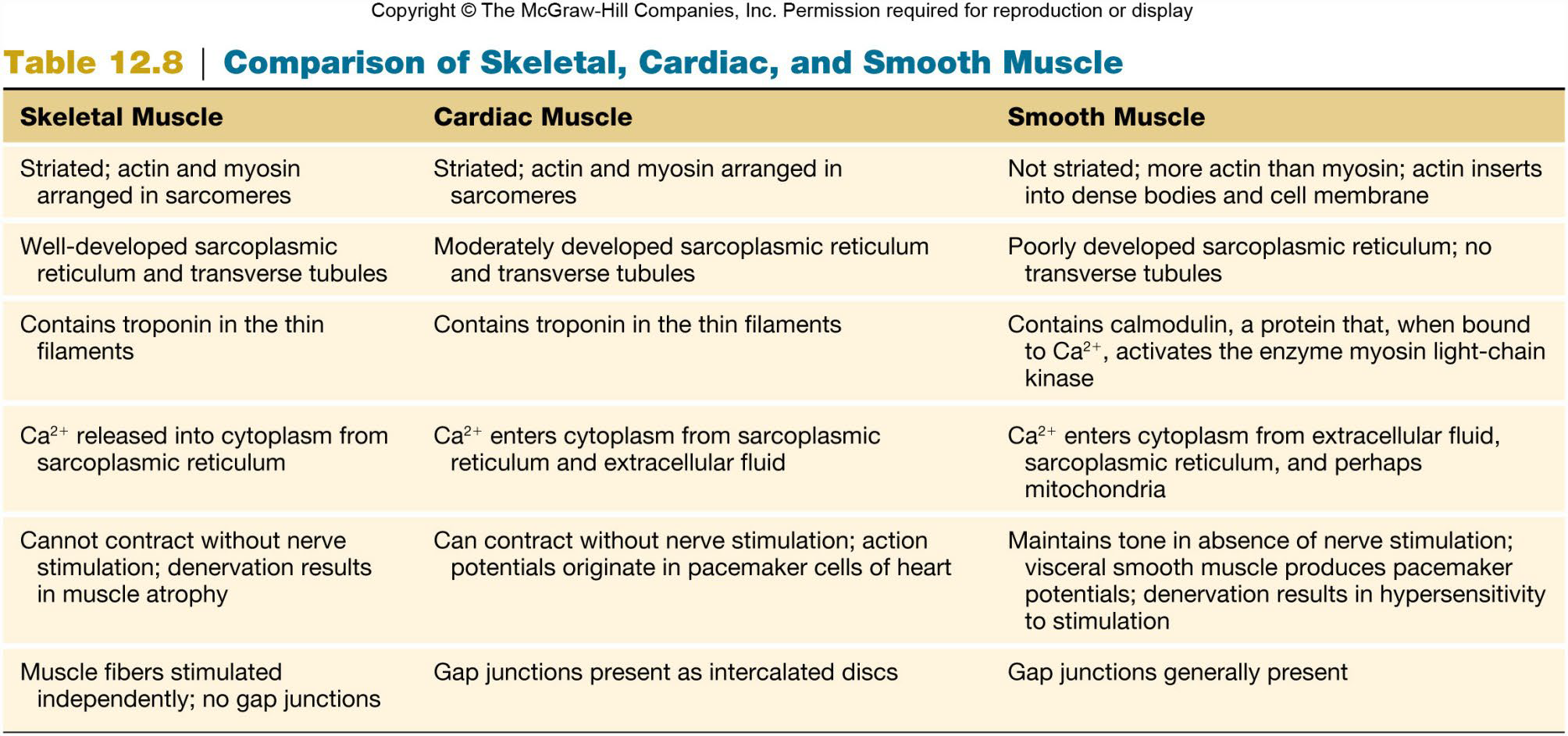
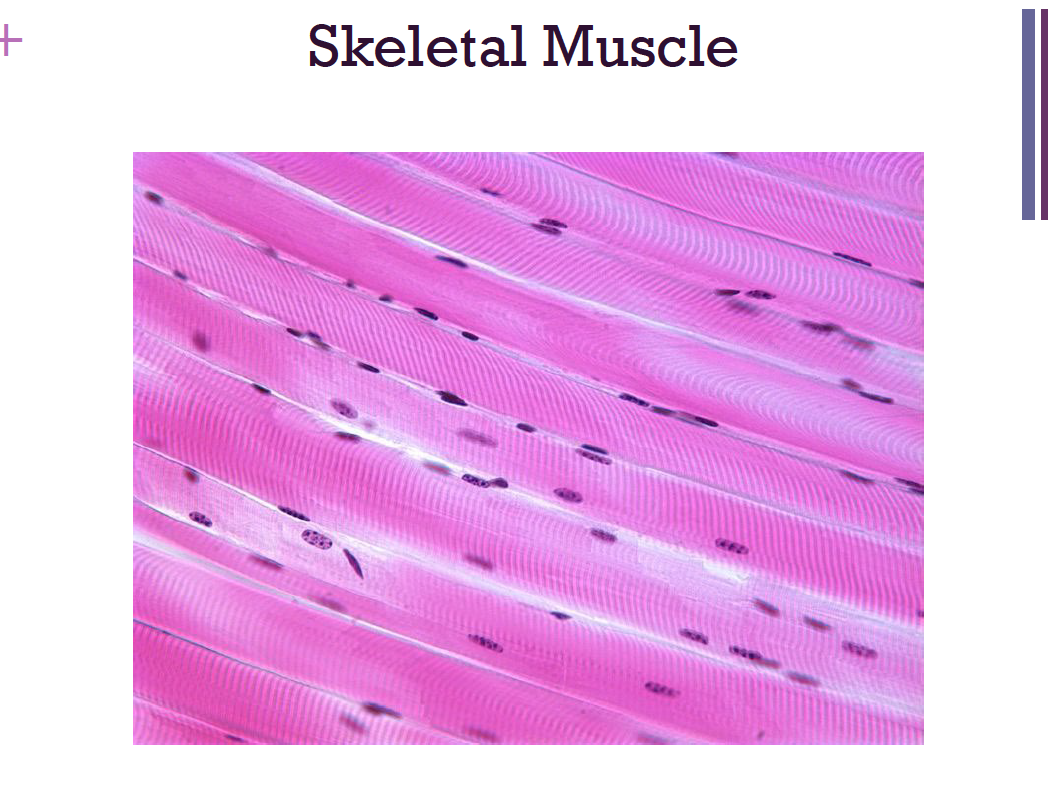
skeletal muscles
attach to and cover the bony skeleton
longest muscle cells
stripes = striations
voluntary
Function: Motility and Heat production
Contracts rapidly but tires easily
Adaptable → forces ranging from a fraction of an ounce to well over 70 lbs
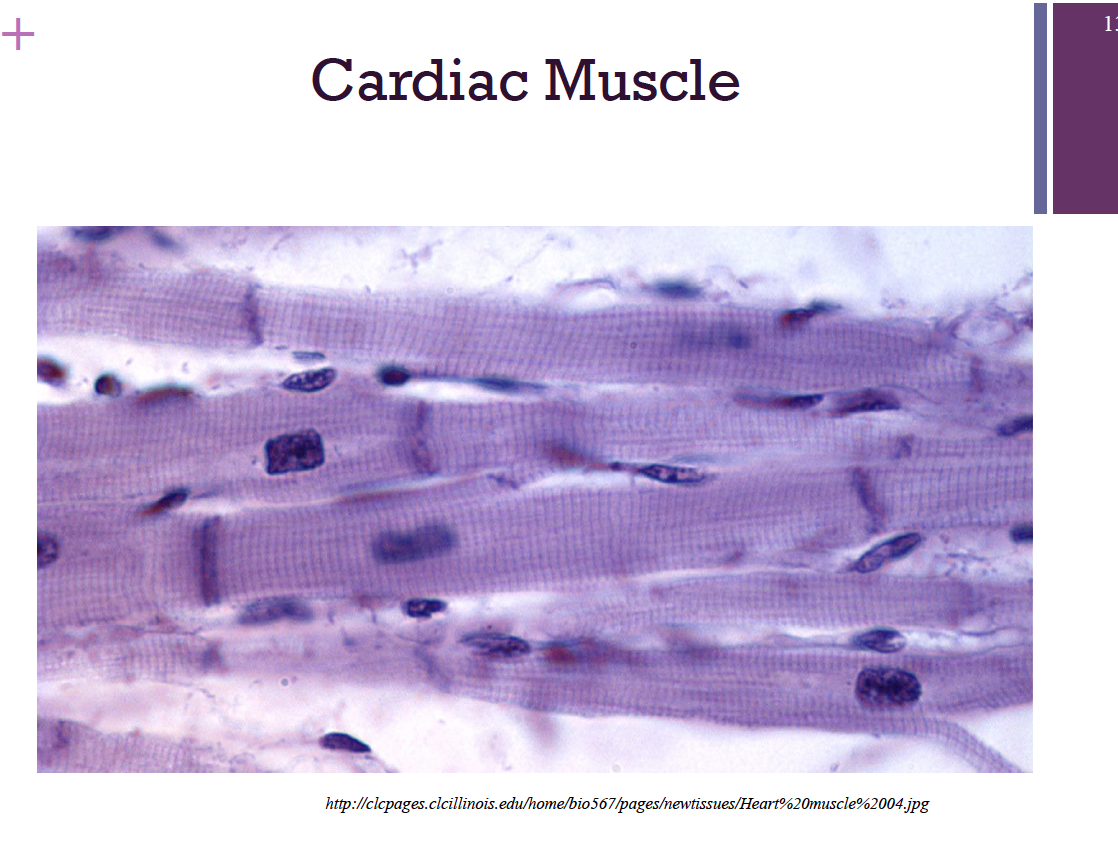
cardiac muscle
Only in the heart
Striated
Not voluntary
Function: To pump blood throughout the body
Under neural and hormonal controls
The heart and smooth muscle both have automaticity → Contains gap junctions
smooth muscle
Found in the walls of hollow visceral organs
Makes up the heart valves
Function: To force food and other substances through internal body channels
Not striated and involuntary
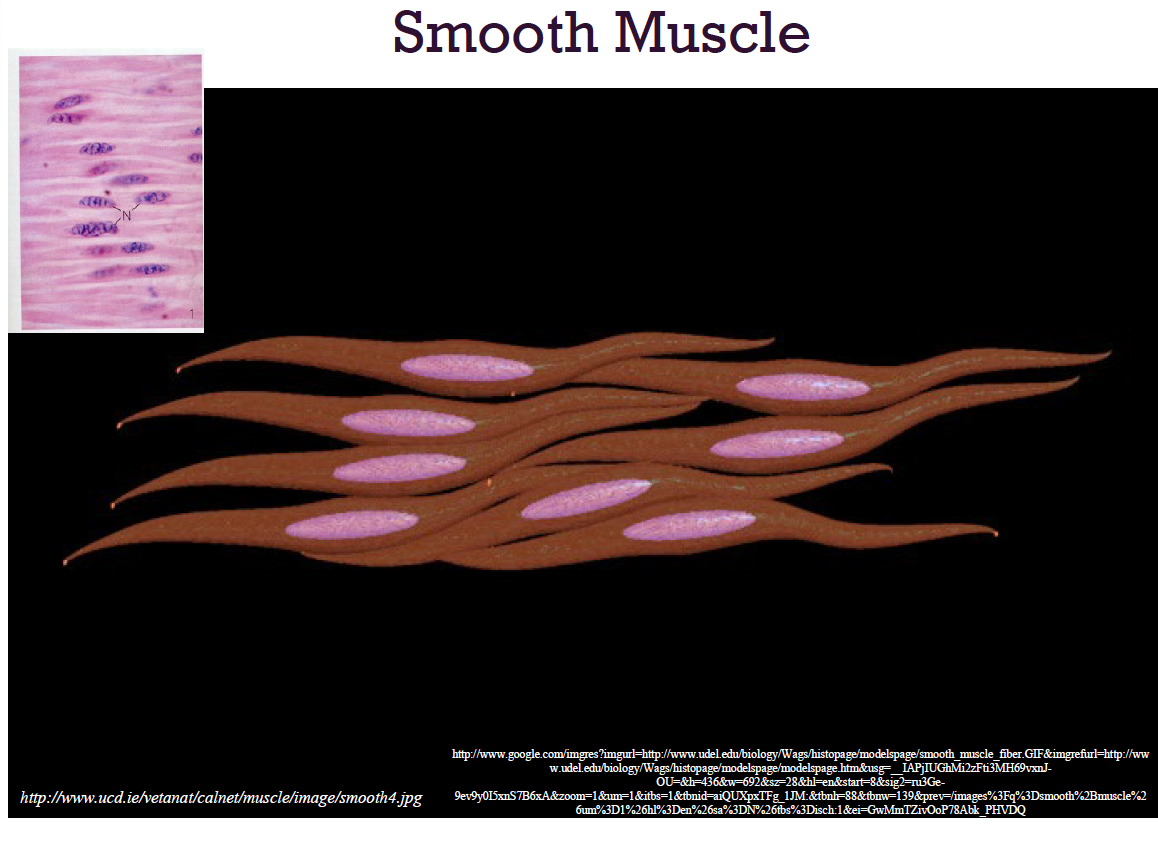
functional characteristics of muscle tissue
Excitability (or irritability) and conductivity
Contractility
Extensibility
Elasticity
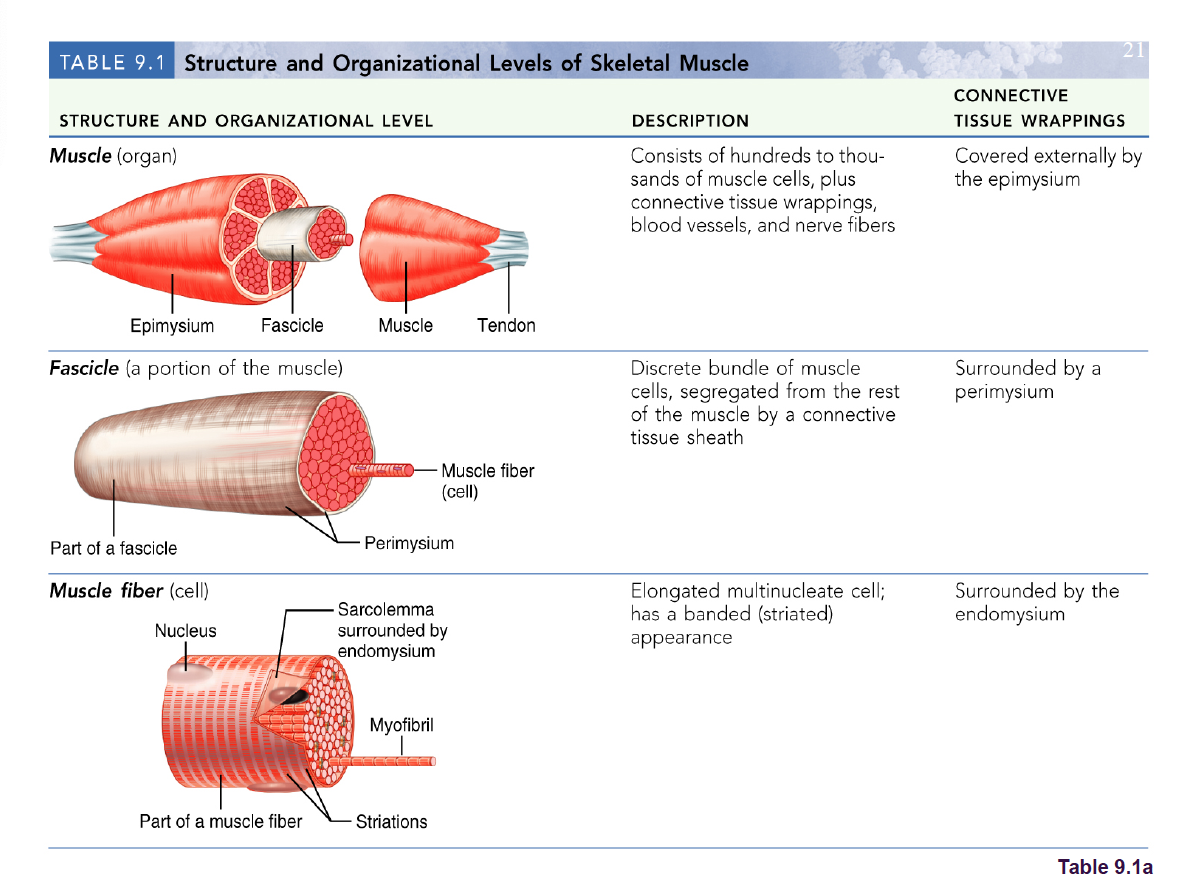
Skeletal muscle
Each muscle is a discrete organ:Muscle tissue
Blood vessels
Nerve fibers
Connective tissue
Requires nerve stimulation
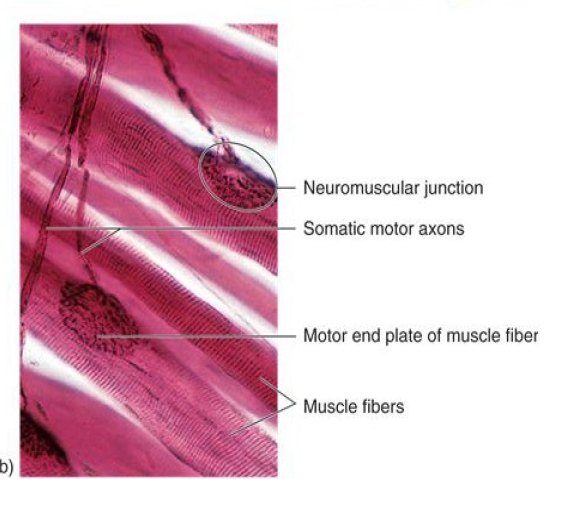
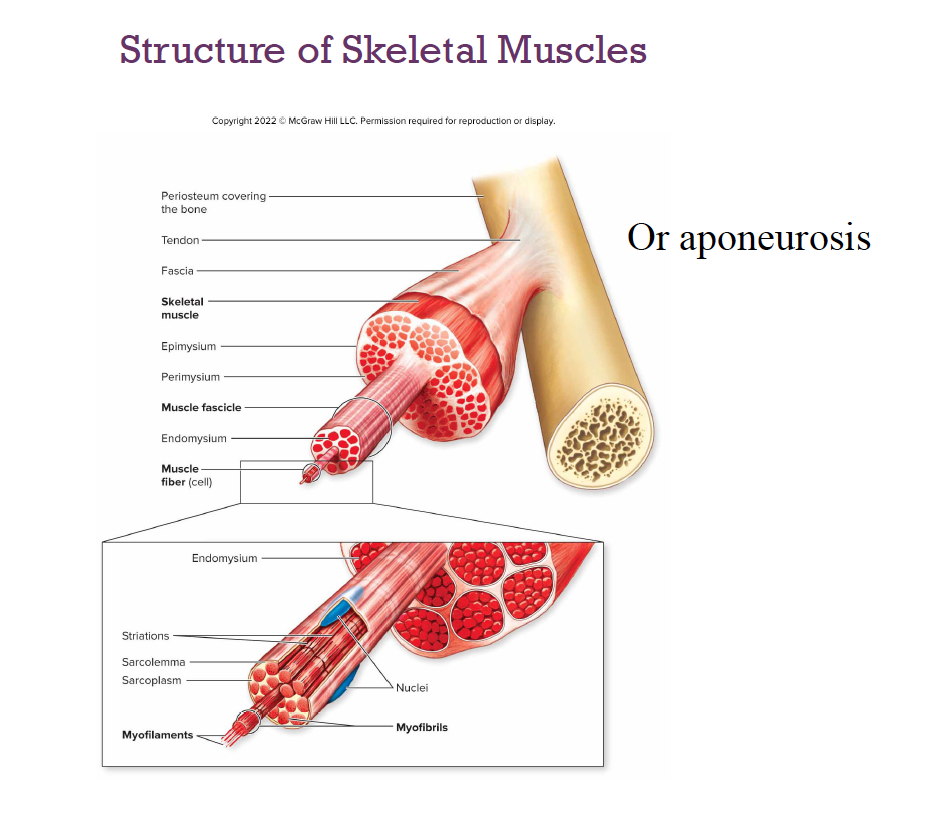
Nerve and Blood Supply
Each muscle is served by one nerve, an artery, and one or more veins
Contracting fibers require continuous delivery of oxygen and nutrients
Wastes must be removed
Skeletal Muscle: Attachments
Attached to bone in at least 2 places
Point of attachment to an immovable bone = the origin
Point of attachment to a movable bone= the insertion
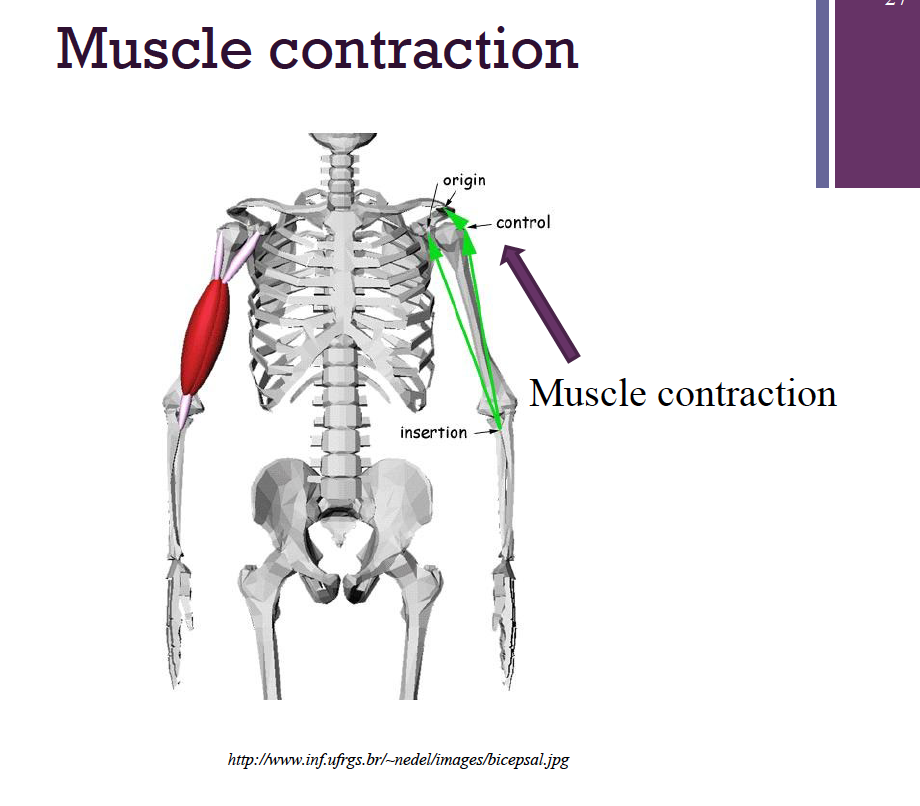
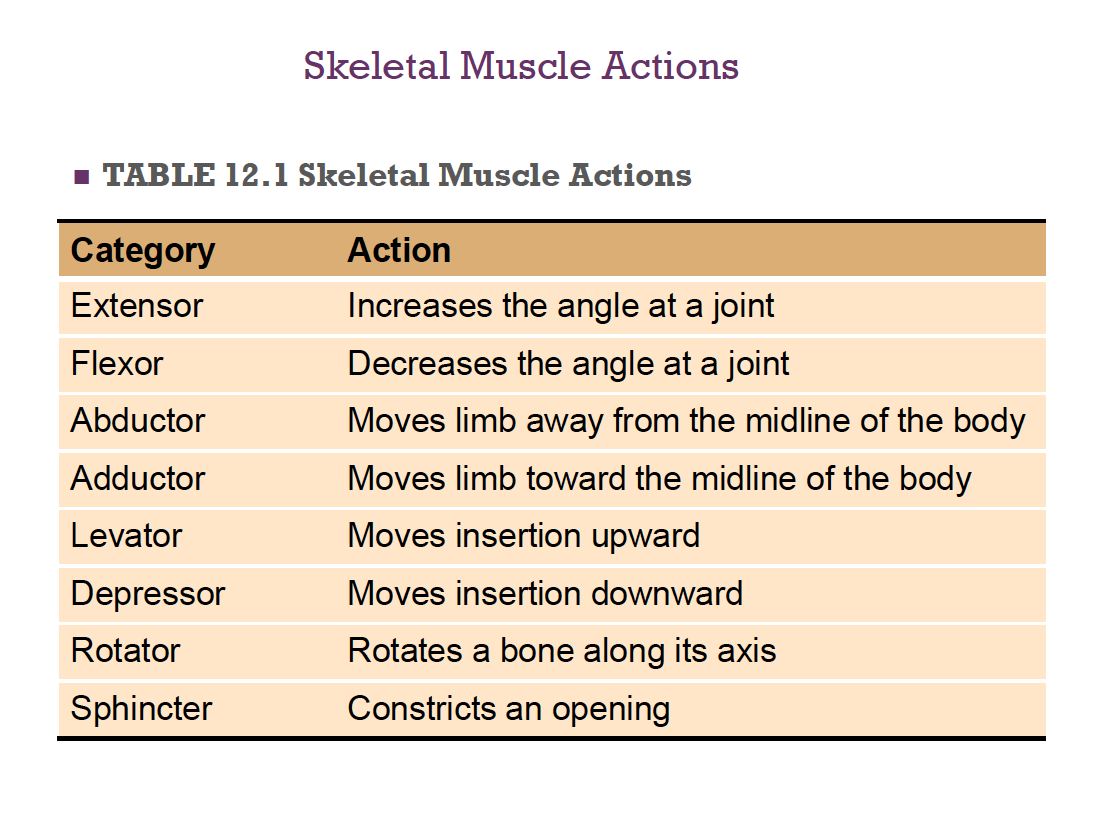
Mechanism of Skeletal Muscle Contraction
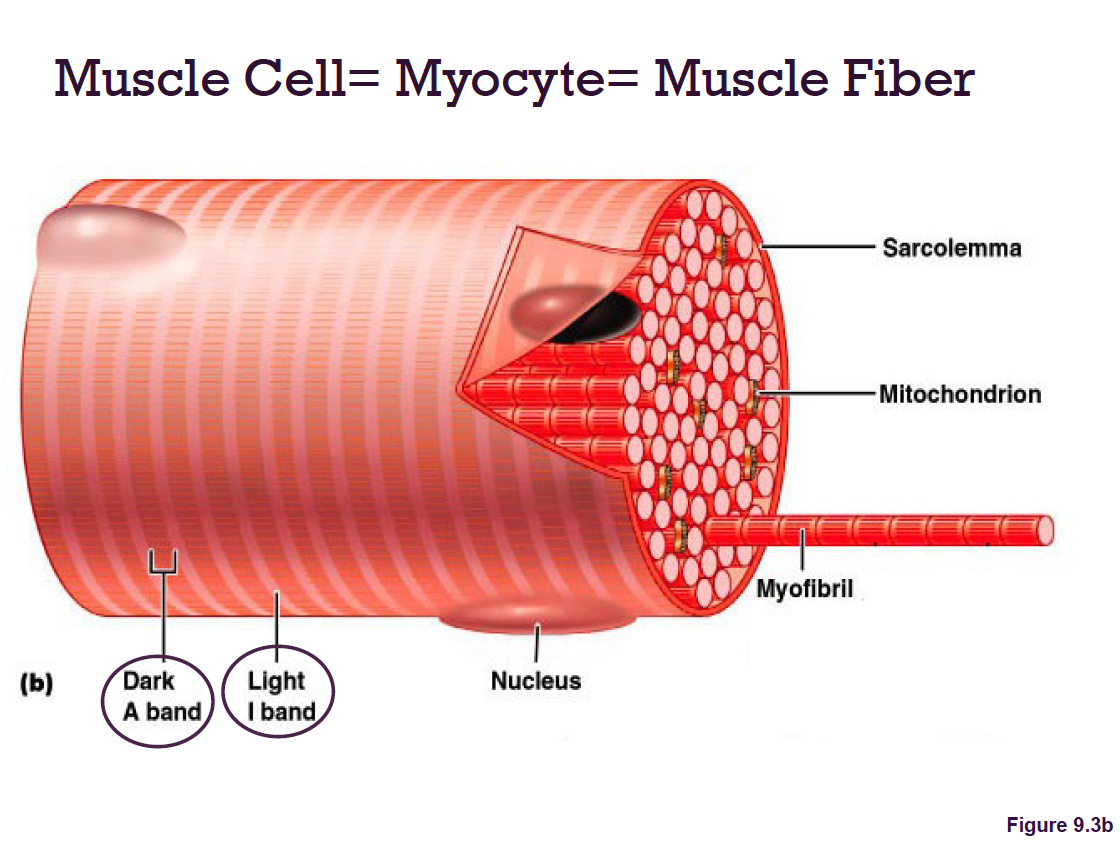
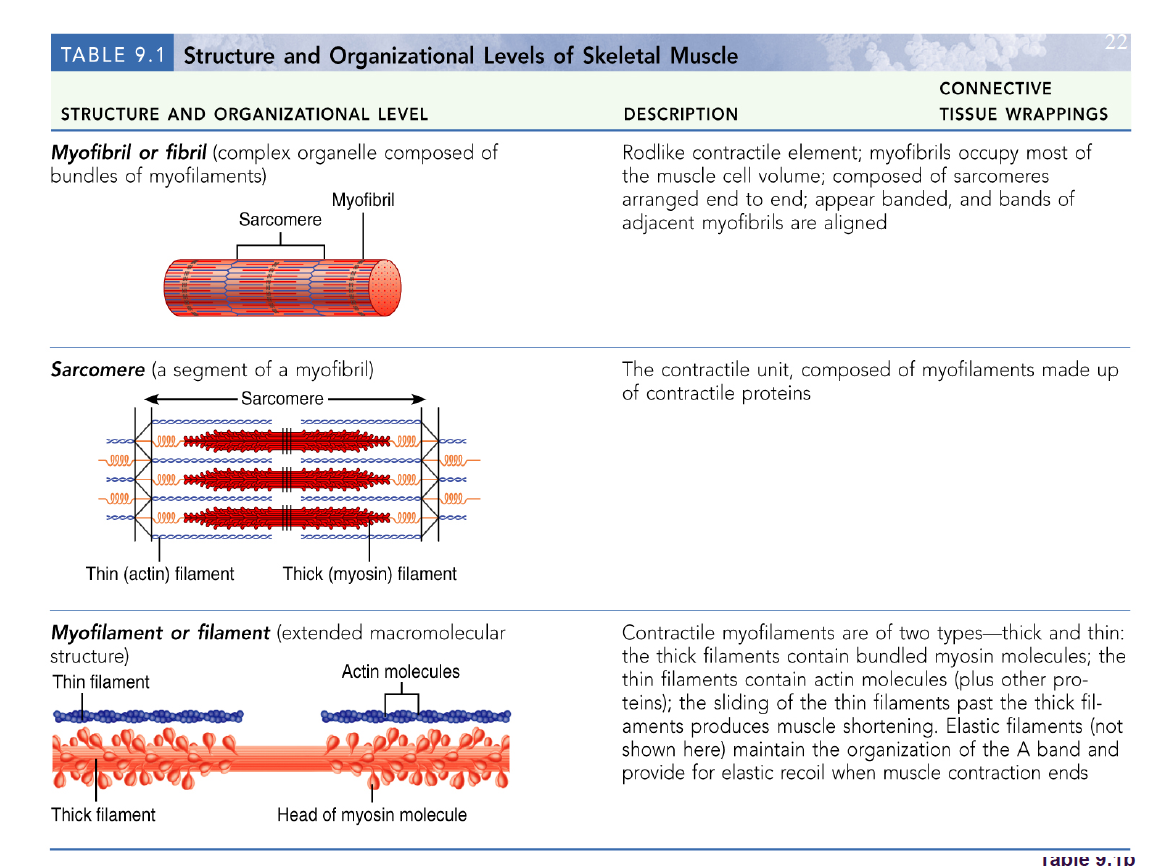
Sarcomeres:
Smallest contractile unit
Myofibril region between 2 Z discs
Composed of myofilaments:
Thick (myosin)
Thin (actin)
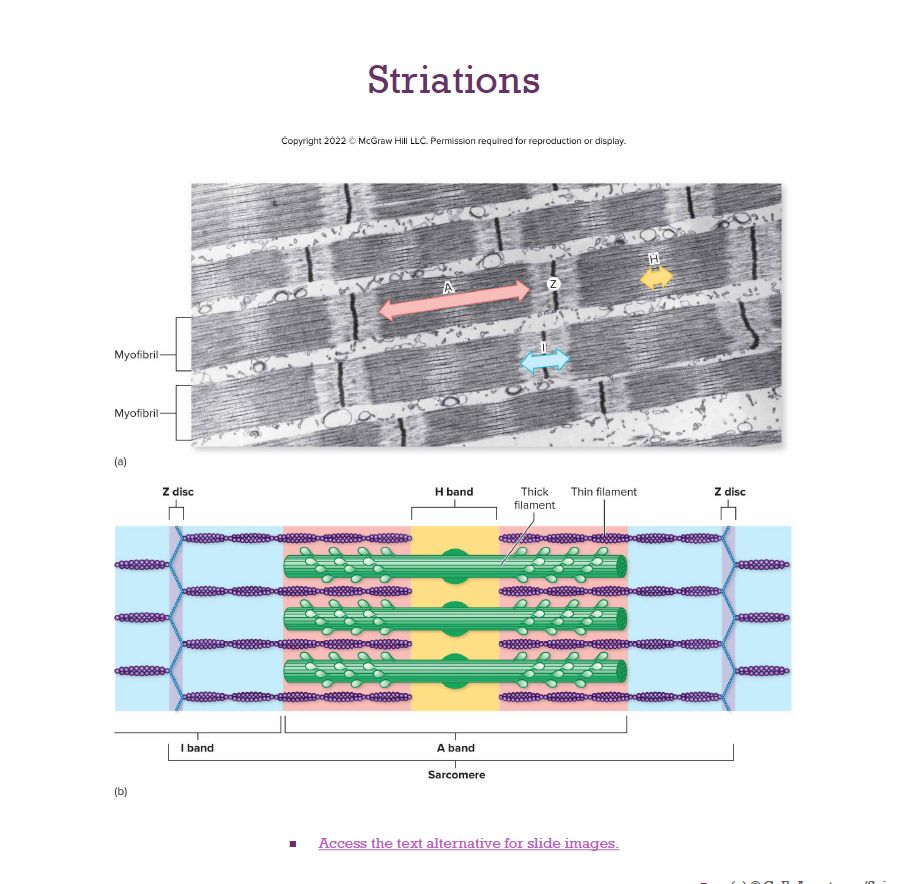
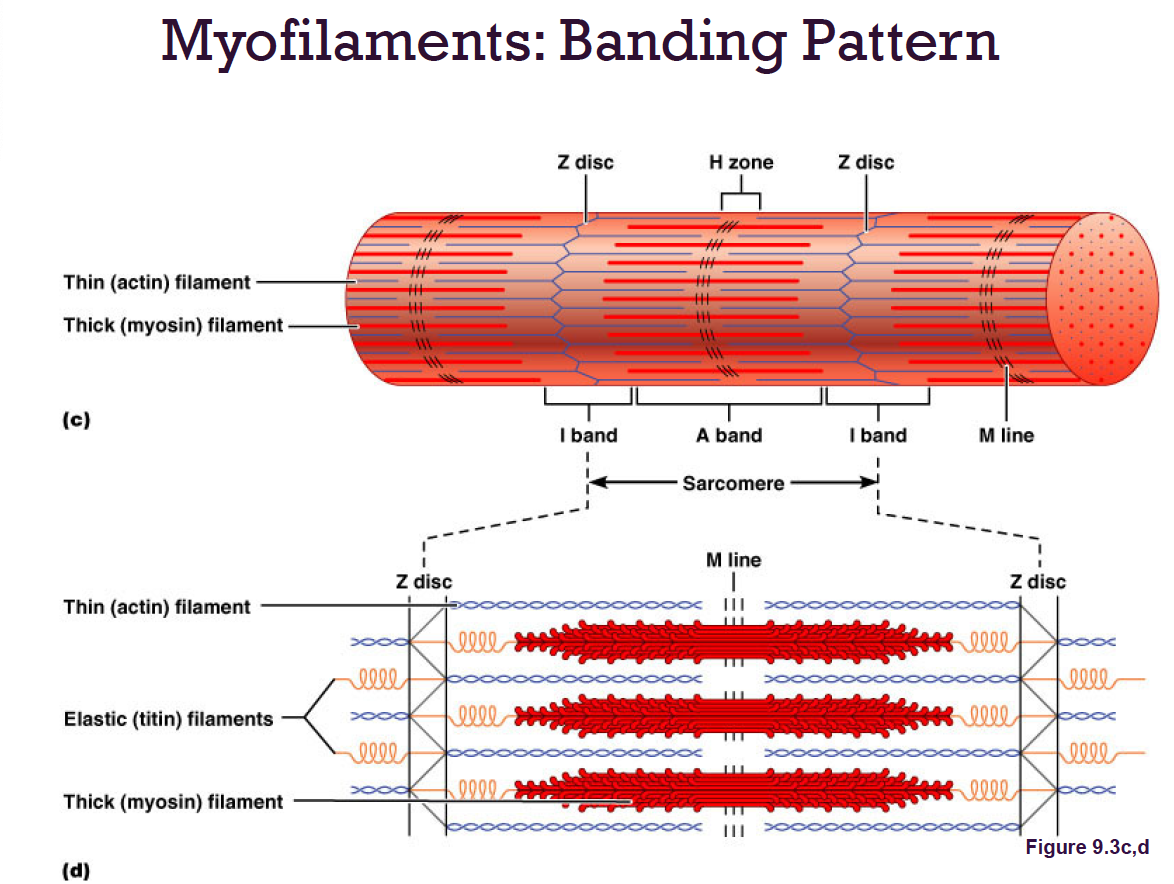
Ultrastructure of Myofilaments: Thick Filaments
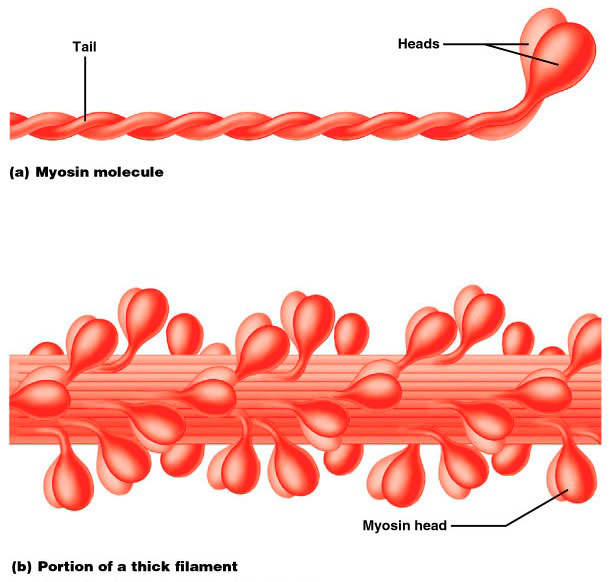
Thick filaments: Composed of protein myosin that contains two heavy and four light polypeptide chains
Heavy chains intertwine to form myosin tail
Light chains form myosin globular head
During contraction, heads link thick and thin filaments together, forming cross bridges
Ultrastructure of Myofilaments: Thin Filaments
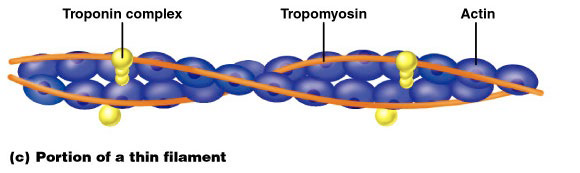
Tropomyosin and troponin (Tn) are regulatory subunits
Troponin (Tn) complex of 3 proteins:
TnI: binds to actin
TnT: binds to tropomyosin
TnC: binds Ca+2
Mostly made up of actin → helial polymer of globular subunits
2 actin strands as an interwoven string
Active sites to which myosin heads attach during contraction
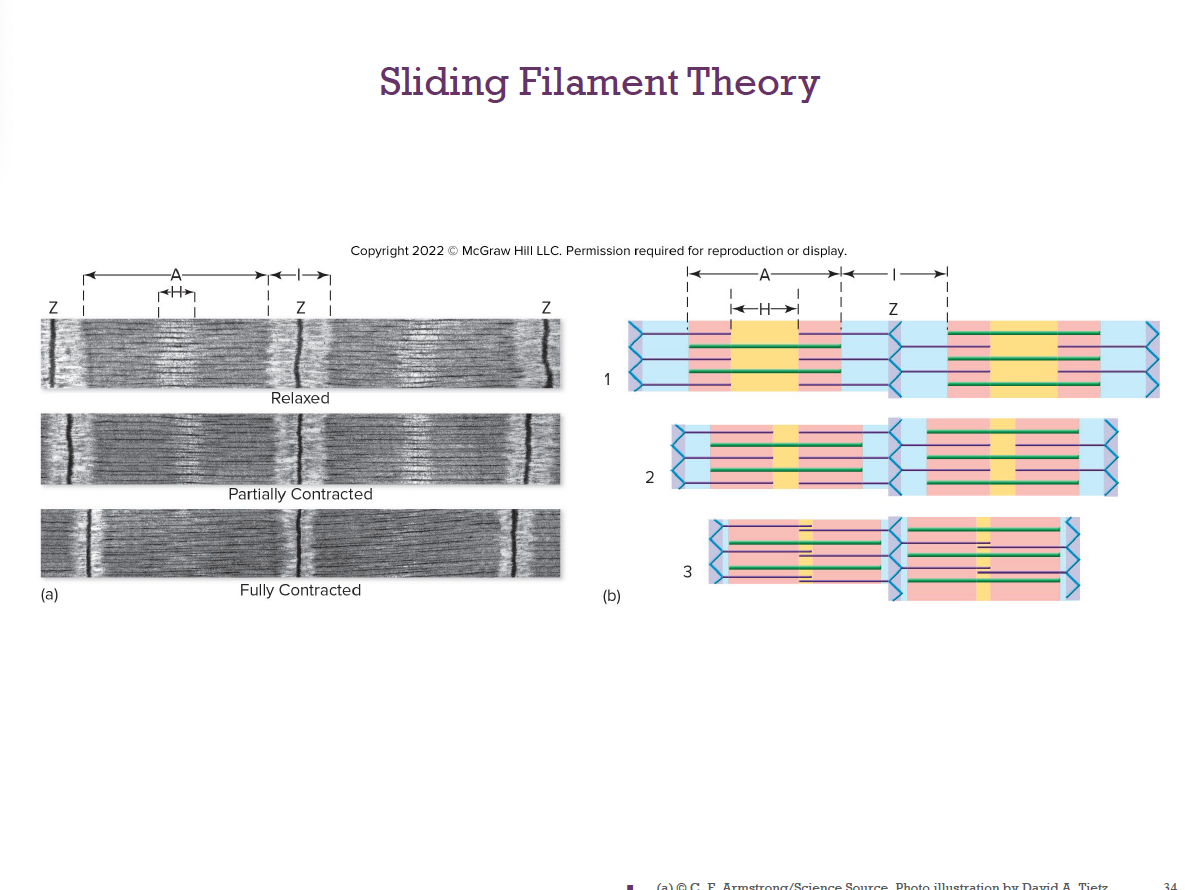
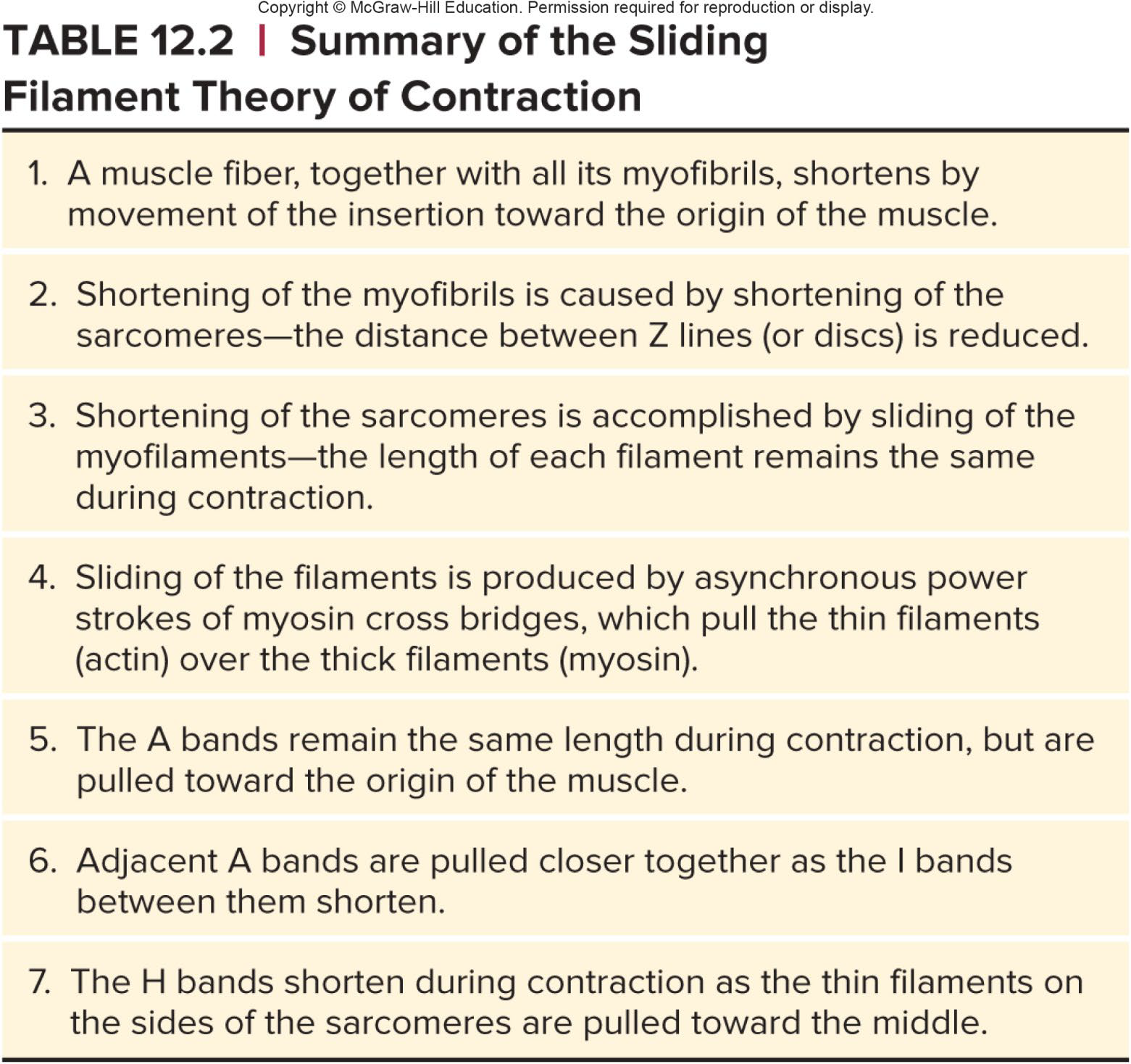
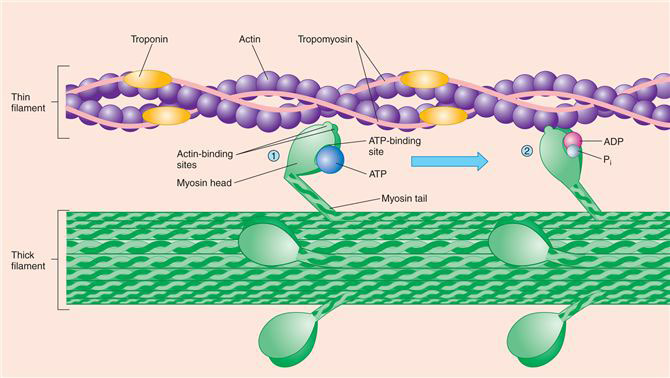
Sliding Filament Theory
2)Release of Pi upon binding cocks the myosin head, producing a power stroke that pulls the thin filament toward the center.
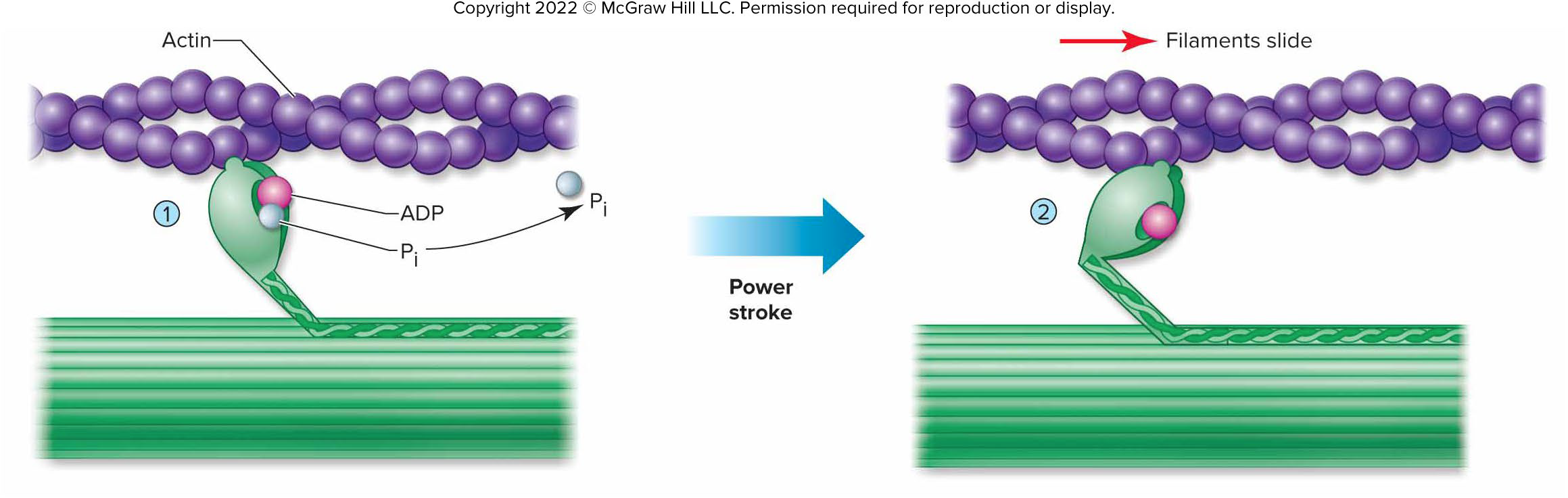
After the power stroke, ADP is released and a new ATP binds.
a) This makes myosin release actin.
b) The new ATP is split.
The myosin head straightens out and rebinds to actin farther back.
Continues until the sarcomere has shortened
Other Components of the Myofibril
Elastic filament: composed of protein titin → Holds thick filaments in place; helps recoil after stretch; resists excessive stretching
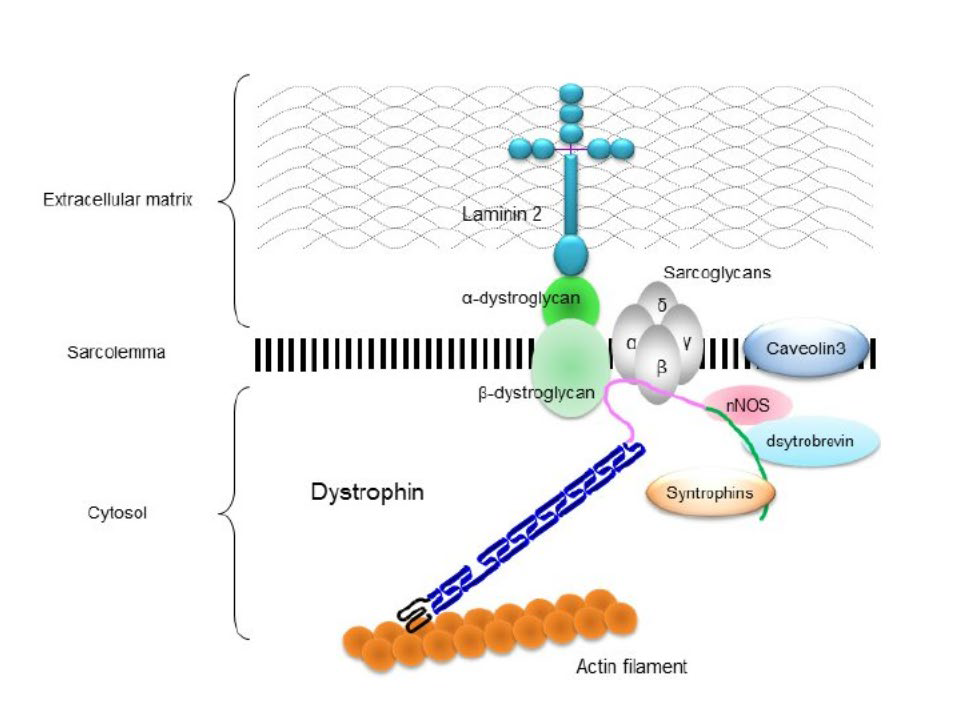
Dystrophin: Links thin filaments to proteins of sarcolemma
Nebulin, myomesin, C proteins bind filaments or sarcomeres together → Maintain alignment of sarcomere
Sarcoplasmic Reticulum
Smooth endoplasmic surrounds each myofibril
Functions in the storage and regulation of intracellular Ca+2
T tubules (transverse) penetrate deep into the cell’s interior→ conduct impulses
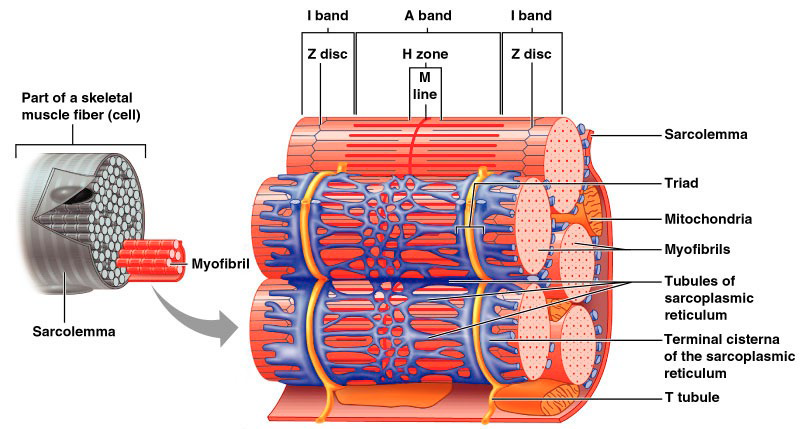
Skeletal Muscle Contraction
Skeletal muscle MUST
Be stimulated by a nerve ending
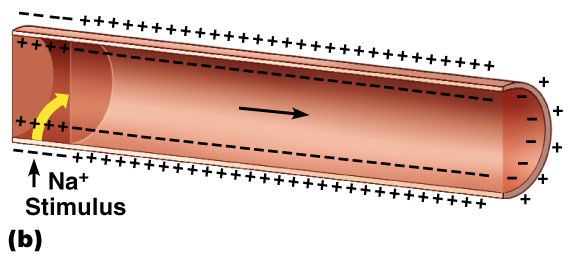
Propagate AP along its sarcolemma
↑intracellular Ca2+
ATP
Linking the electrical signal to the contraction is excitation-contraction coupling
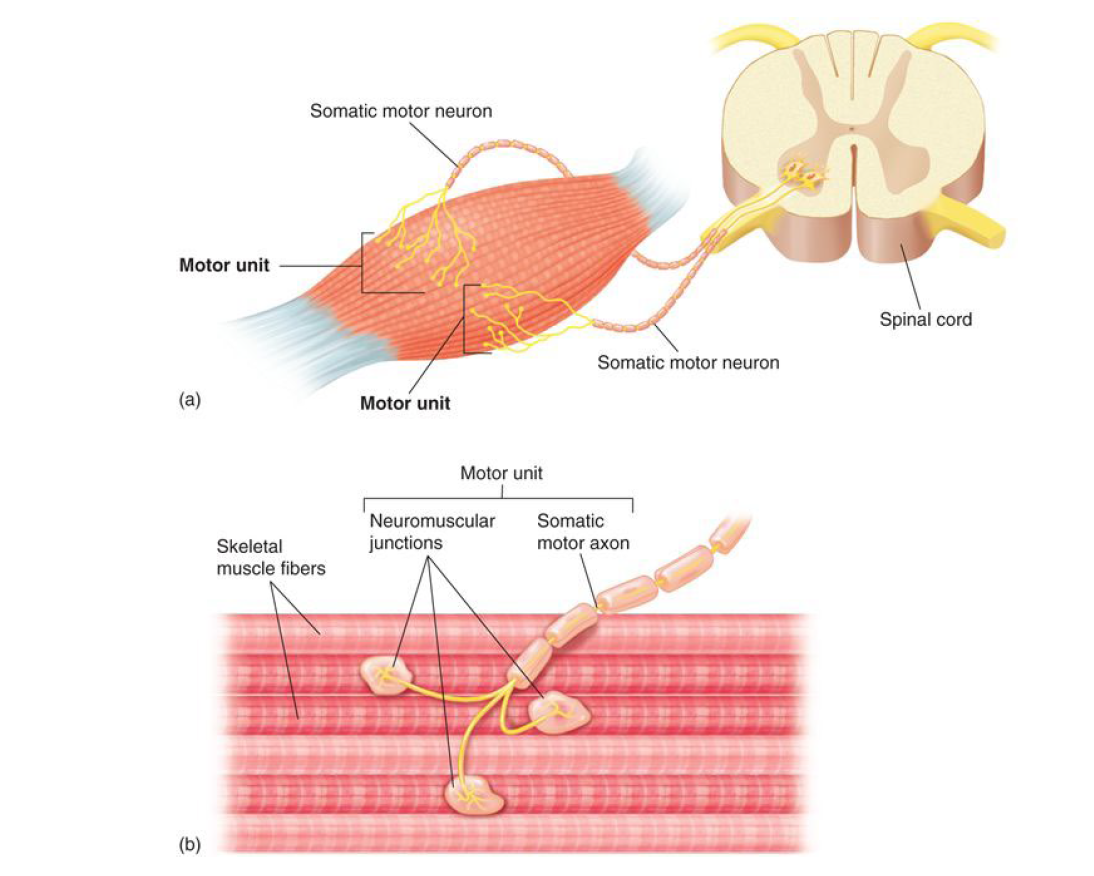
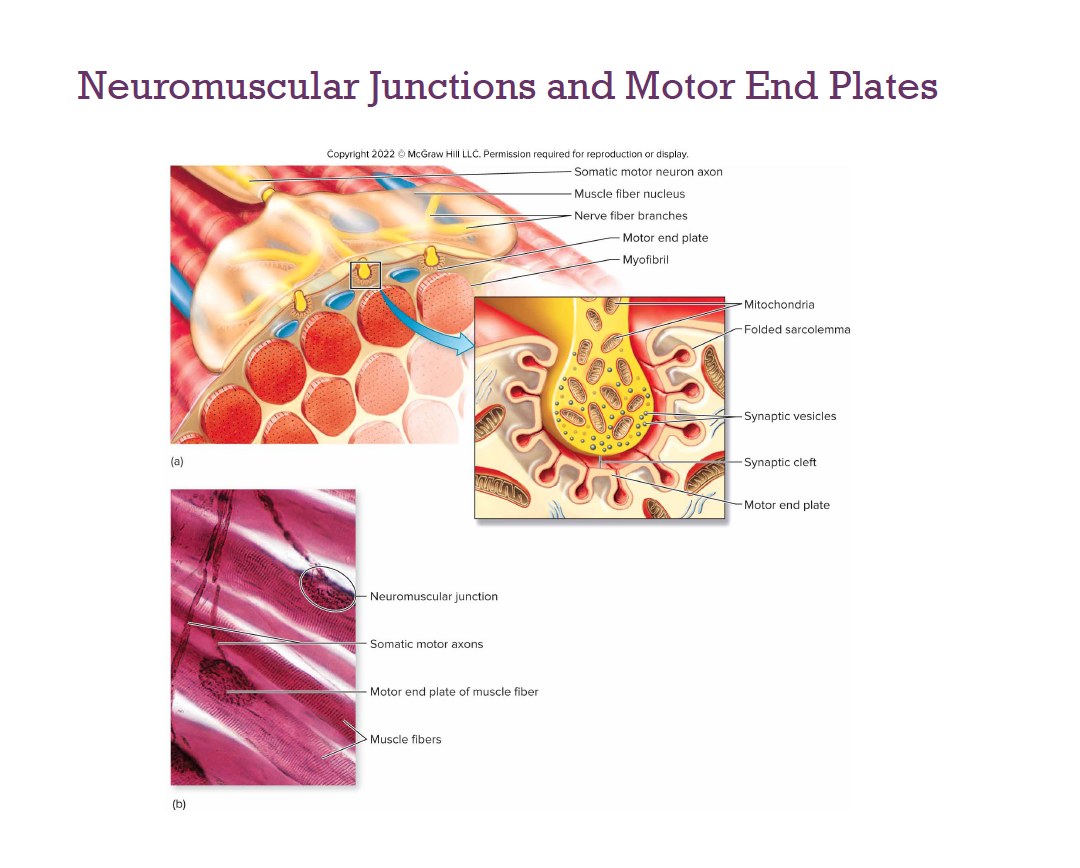
Nerve Stimulus of Skeletal Muscle
Motor neurons of the somatic NS
Axons branch profusely
Each axonal branch forms a neuromuscular junction with a single muscle fiber
Stimulating a Muscle Fiber
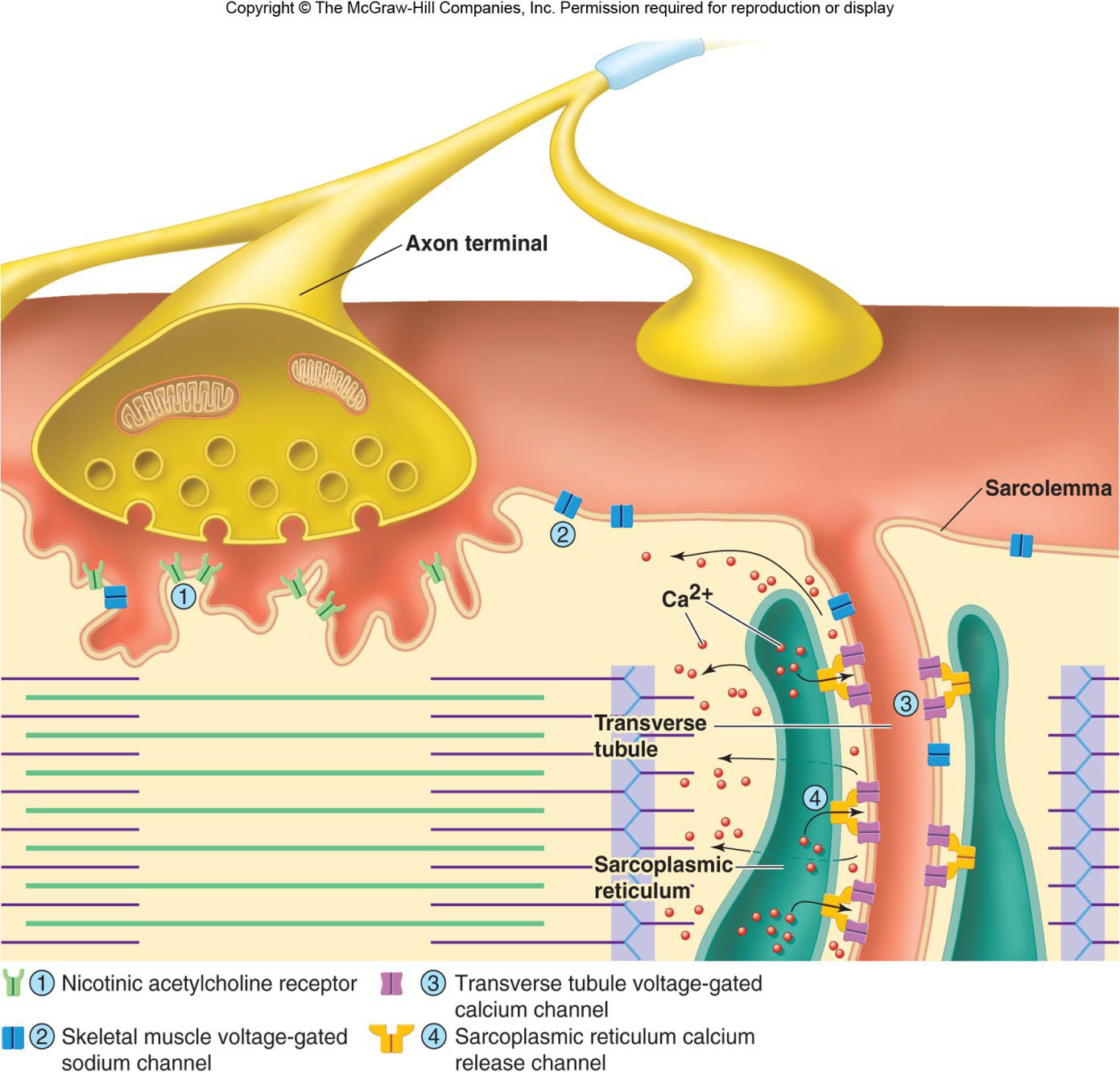
Action Potential in the Muscle
Ligand-gated sodium channels open → Na+ enters the cell
If the stimulus is strong enough, an action potential is initiated
Excitation-Contraction Coupling
Action potential:
Propagated along the sarcolemma
Travels down the T tubules
Triggers Ca2+ release from SR terminal cisternae
Ca2+ binds to troponin: Tropomyosin moves → Actin active binding sites exposed
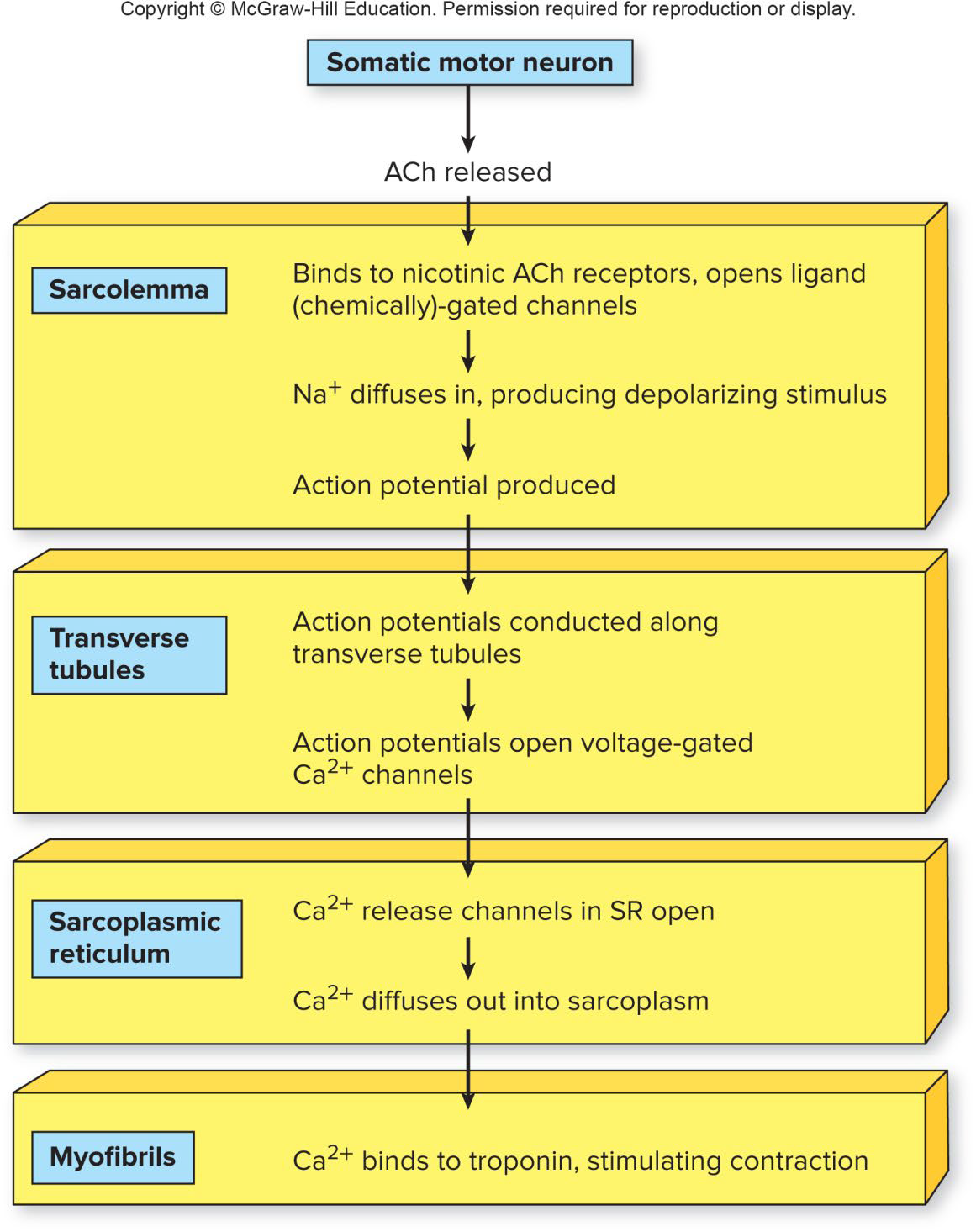
Contraction of Skeletal Muscle
The two types of muscle contractions are:
Isometric contraction – ↑ muscle tension (muscle does NOT shorten during contraction)
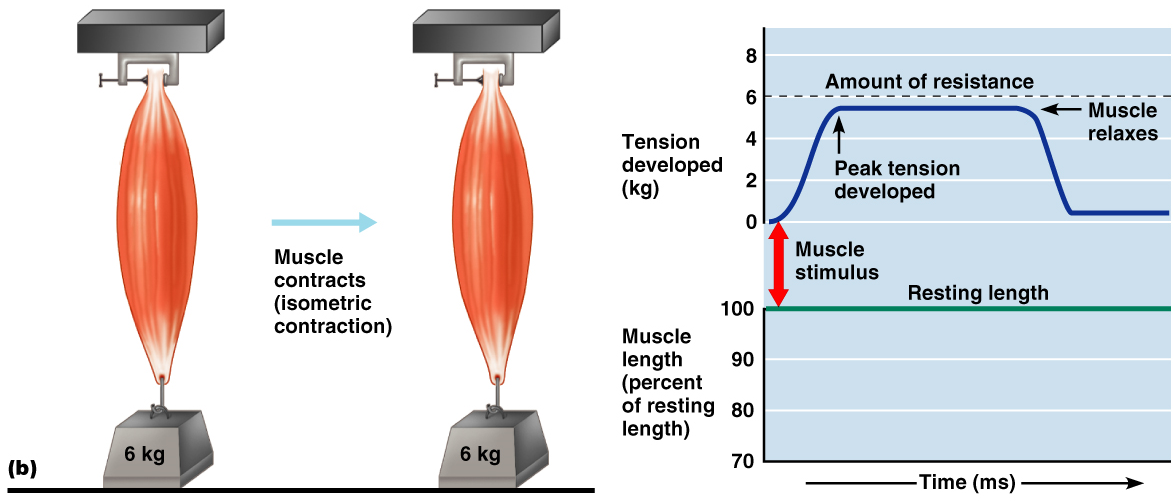
This muscle is attached to a weight that exceeds it’s maximum
tension producing capacity.
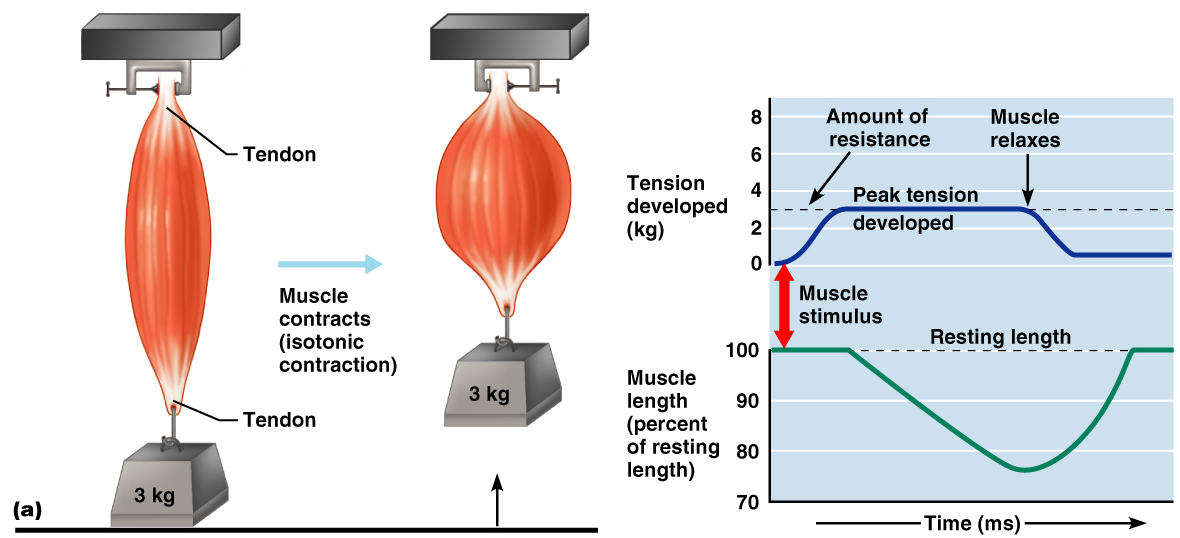
Isotonic contraction – ↓ muscle length (muscle shortens during contraction)
Motor Unit
An α motor neuron and all the muscle fibers it supplies
# of muscle fibers per motor unit can vary from four to several hundred
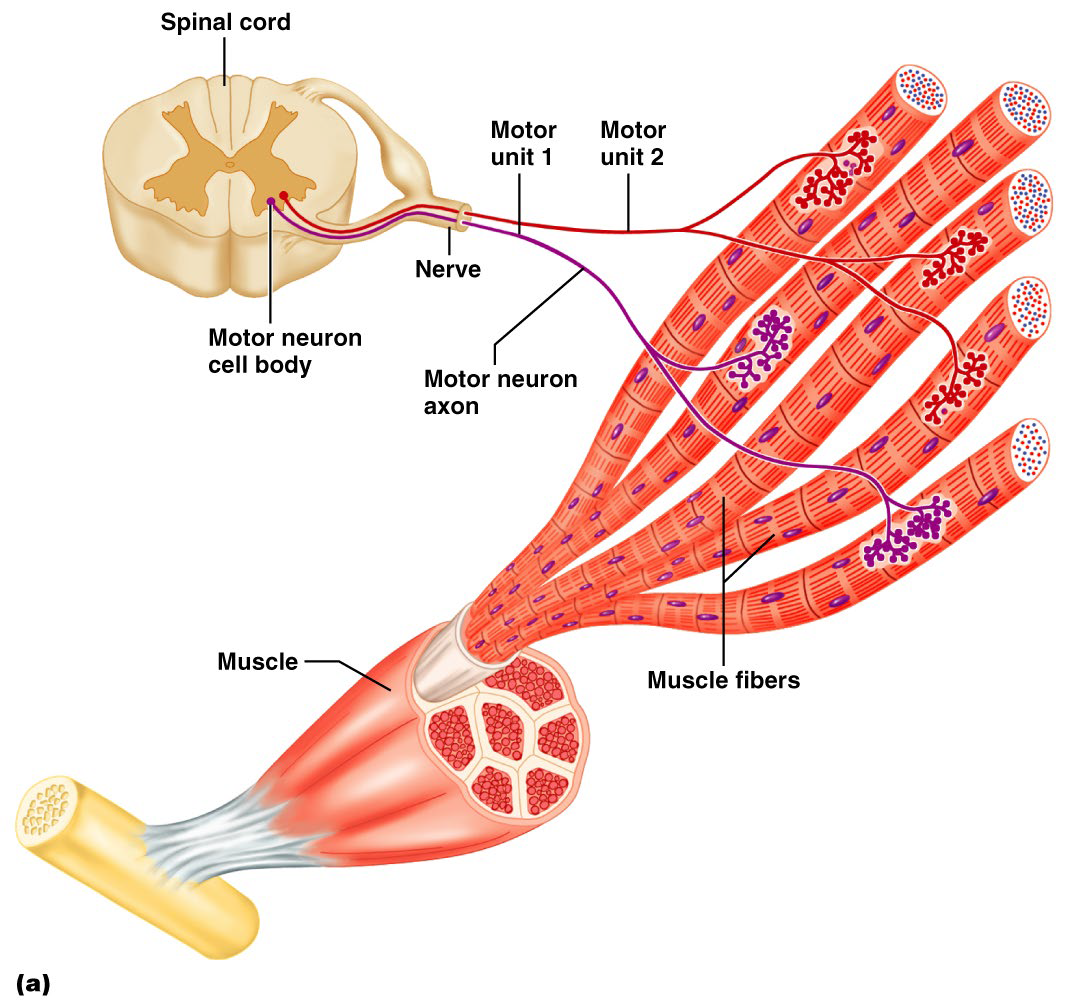
↓#muscle fibers = ↑ control = finer more precise movements
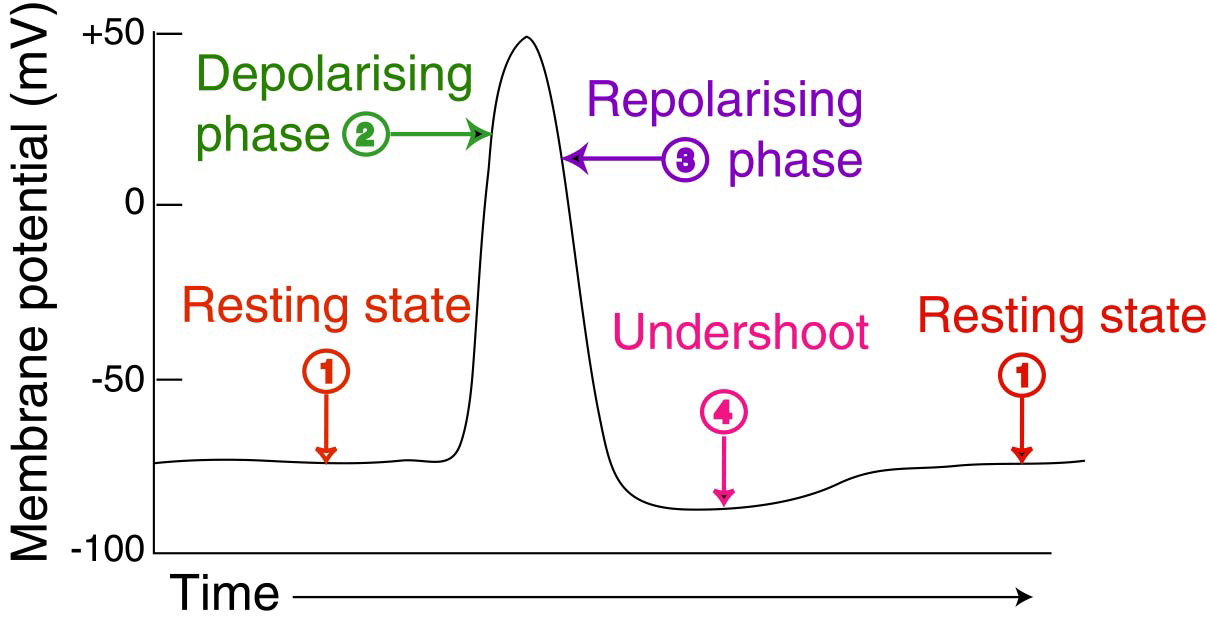
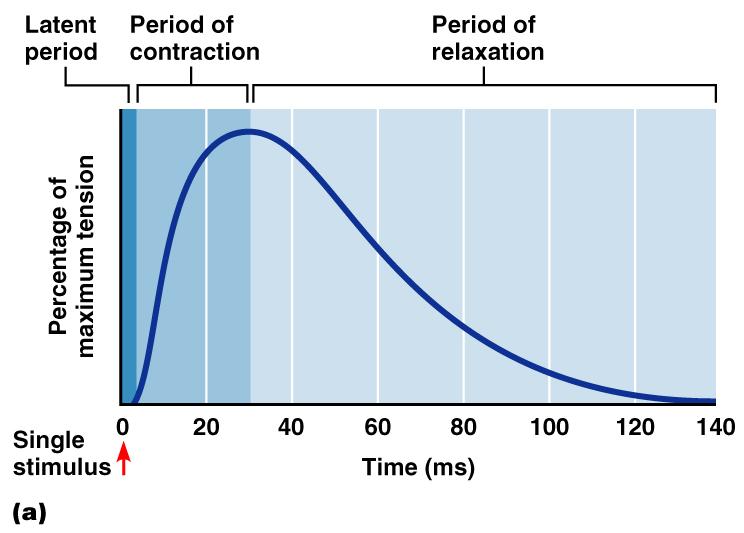
Muscle Twitch, Summation, and Tetanus
A muscle twitch =A single action potential
3 phases=
Graded Muscle Responses
Muscle twitches → NOT how muscles usually contract
Muscle contractions:
Smooth
Vary in strength depending on the demand placed on them (Graded)
Responses are graded by:
Changing the frequency of stimulation
Changing the strength of the stimulus
Muscle Response to Varying Frequency of Stimuli
↑ frequency = ↑contractile force = twitch summation
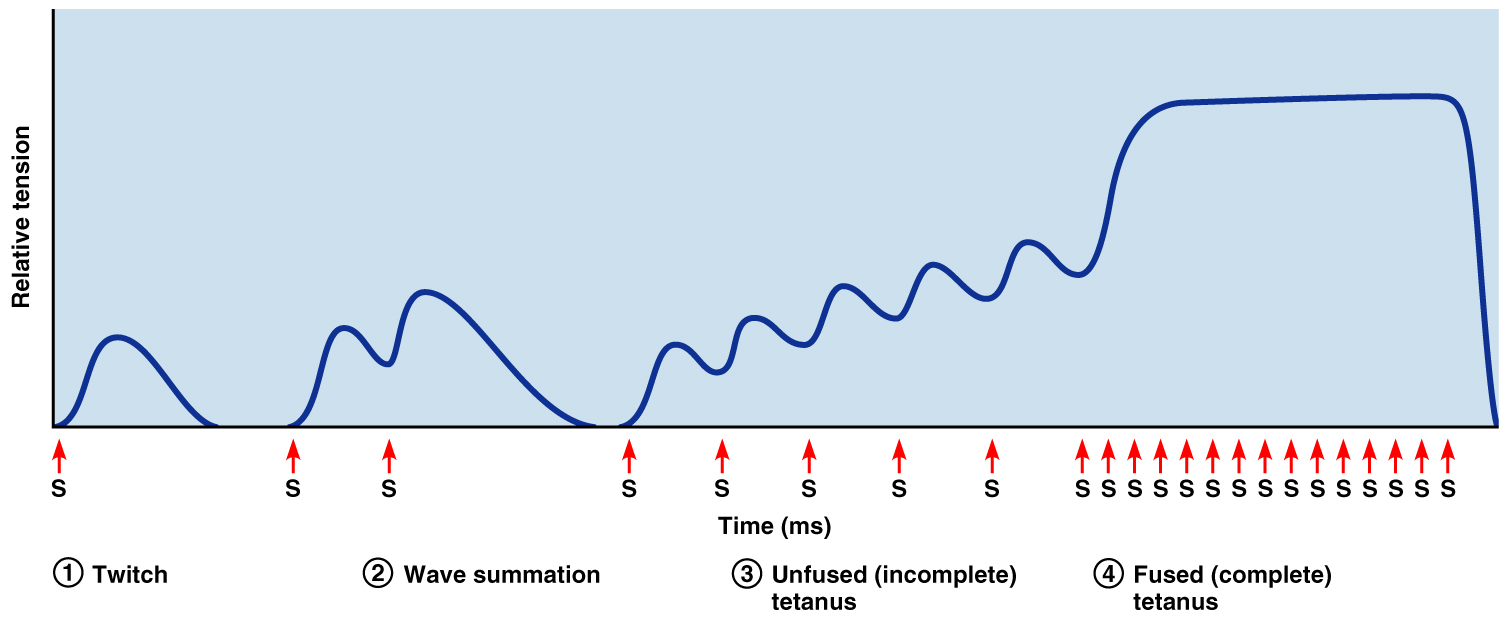
Tetanus results:
Muscle relaxation disappears
Contractions fuse into a smooth, sustained contraction
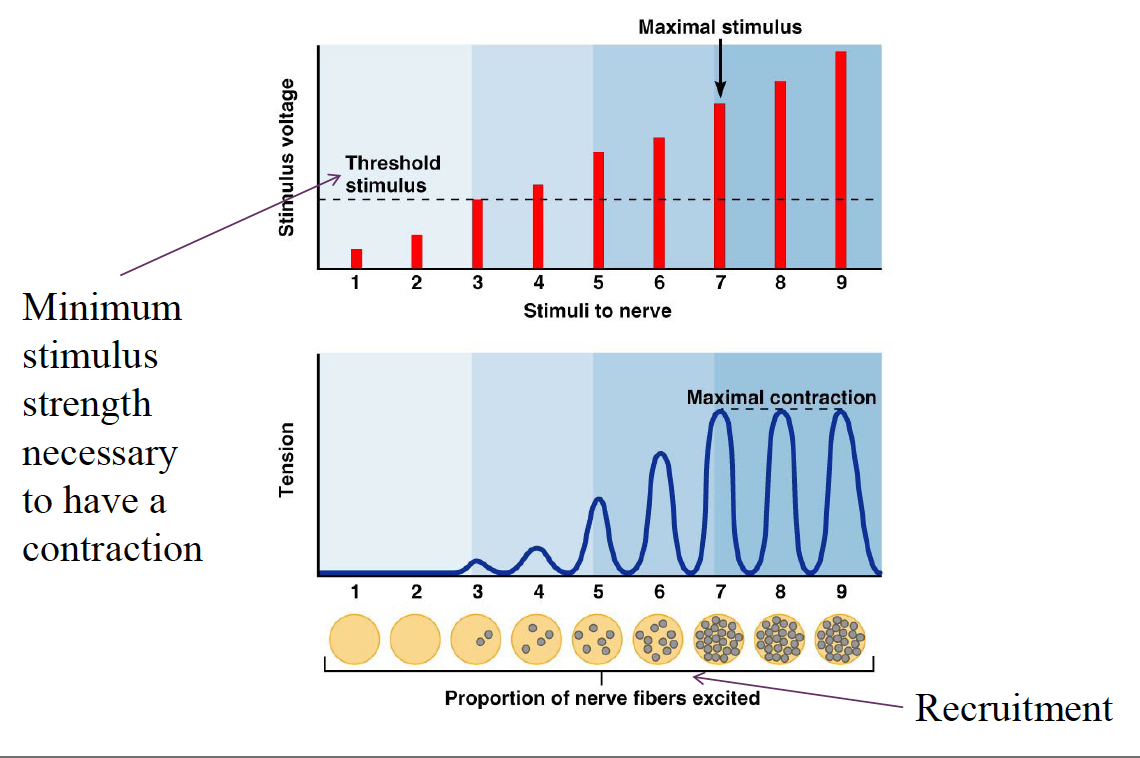
Muscle Response: Stimulation Strength
↑strength of stimulus = ↑ strength of muscle contraction = Multiple Motor Unit Summation
Stimulus Intensity and Muscle Tension
Size Principle
Recruitment is dictated by the size principle →
In any muscle, motor units with the smallest fibers are controlled by small ↑ excitable motor neurons → activated first
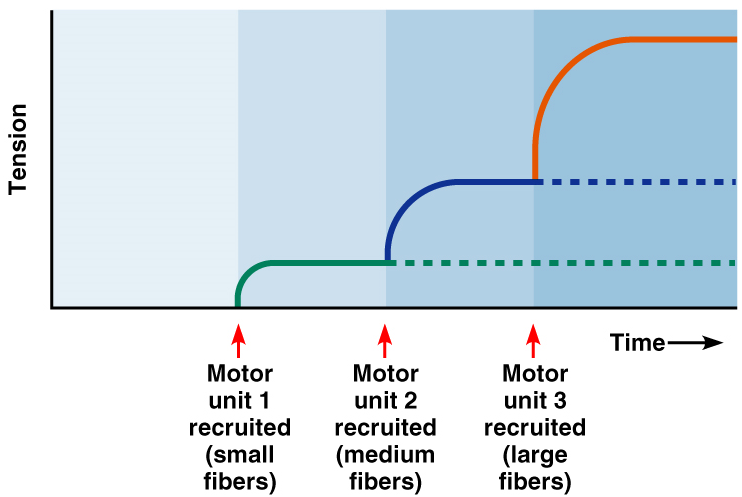
The largest motor units have contractile forces ~50 times > small muscle fibers
→ Innervated least excitable neurons (large)
Treppe: The Staircase Effect
A long period of rest → initial contractions may be only ½ as strong as subsequent contractions
↑ contraction strength in response to multiple stimuli of the same strength
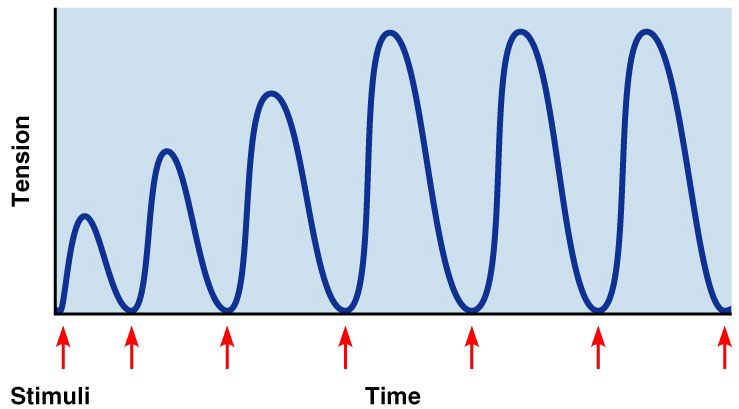
Contractions ↑ because:
↑Ca2+ in the sarcoplasm
↑heat generated = ↑efficiency enzymes
Muscle Metabolism
Energy for Contraction
ATP is the only source used
ATP regenerated by 3 pathways:
ADP with creatine phosphate (CP)
Anaerobic glycolysis
Aerobic respiration
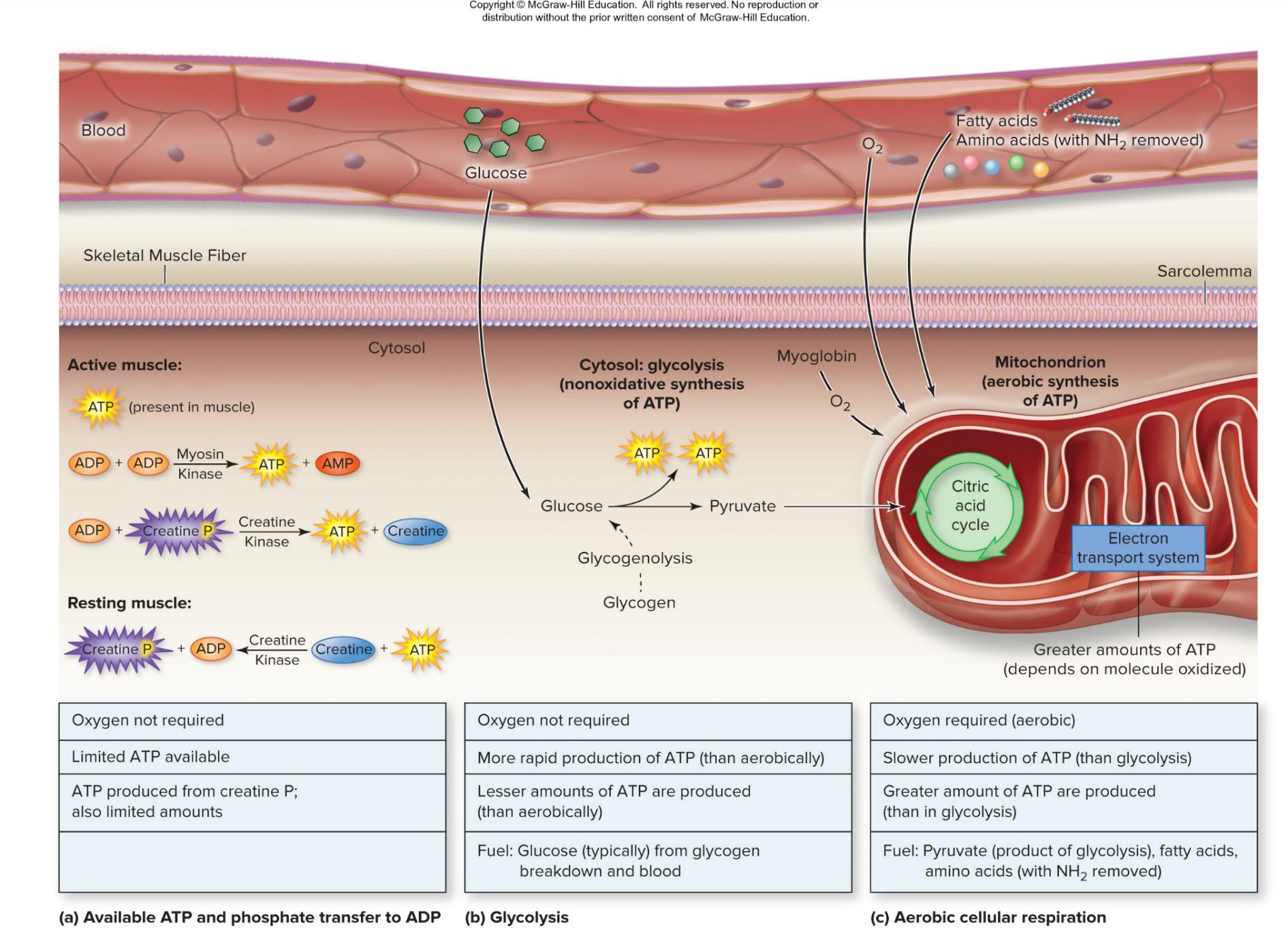
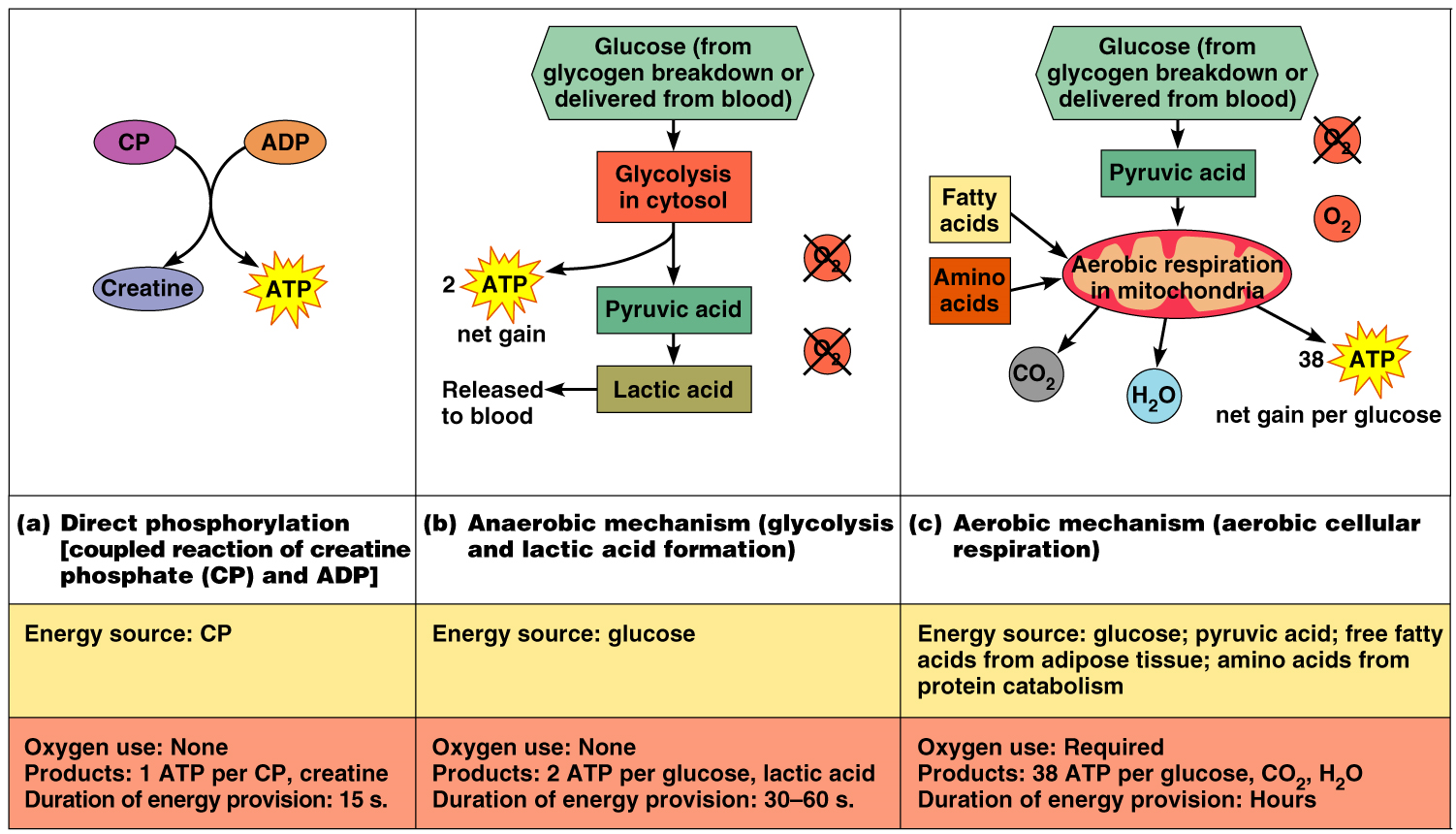
Where Muscles Get Their Energy
At rest and for mild exercise: from the aerobic respiration of fatty acids
For moderate exercise: from glycogen stores
For heavy exercise: from blood glucose
As exercise intensity and duration increase, GLUT4 channels are inserted into the sarcolemma to allow more glucose into cells.
Muscle Fatigue
Reversible reduction in the muscle’s ability to generate a force
Muscle fatigue occurs when ATP production fails to keep pace with ATP use
There is a relative deficit of ATP, causing contractures (states of continuous contractions because cross bridges can’t detach)
Lactic acid accumulates in the muscle (cause?)
Ionic imbalances are present
Intense exercise → rapid muscle fatigue
Na+-K+ pumps cannot restore ionic balances quickly enough
Prolonged ↓intensity exercise → slow-developing fatigue
SR is damaged → impairs Ca2+ regulation
Adaptation to Endurance Exercise Training
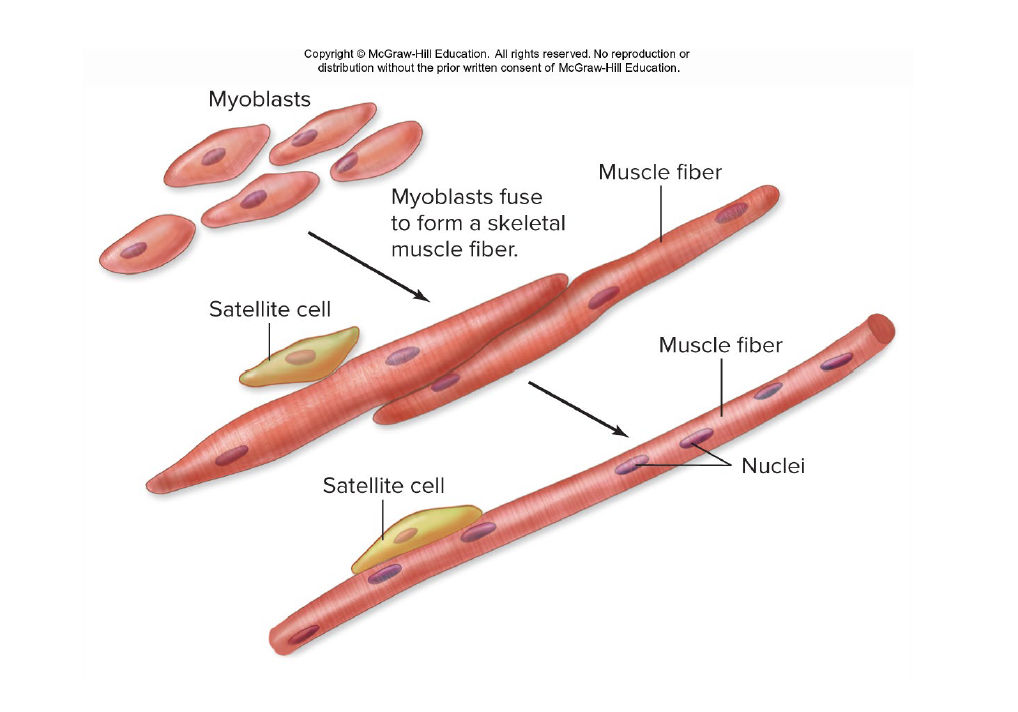
Skeletal Muscle Damage and Repair
Stem cells called satellite cells located near muscle fibers.
These can fuse to damaged muscle cells and repair them or fuse to each other to form new muscle fibers.
Myostatin is a paracrine regulator that inhibits satellite cells.
Force of Muscle Contraction
Affected by:
# of muscle fibers contracting – the ↑ # motor fibers in a muscle, the stronger the contraction
The size of the muscle – the bulkier the muscle, the greater its strength
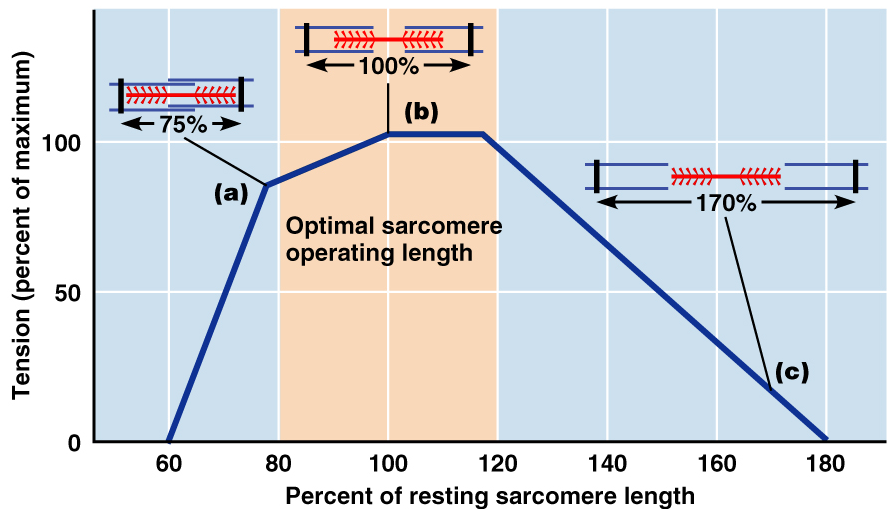
Degree of muscle stretch –strongest when muscle fibers are 80-120% of their normal resting length
Length-tension relationship
Smooth Muscle
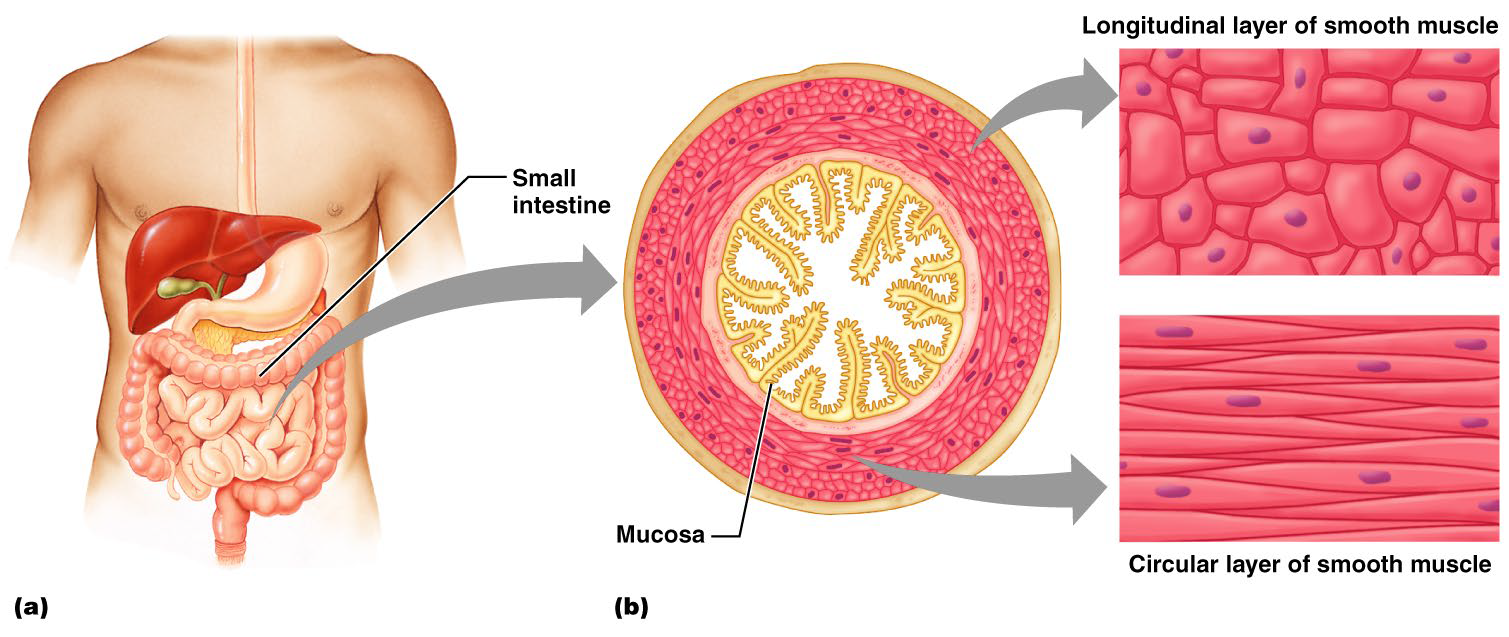
Spindle-shaped fibers
Lack the coarse connective tissue sheaths
Longitudinal layer contracts → organ dilates and contracts
Circular layer contracts → organ elongates+ lumen narrows
Innervation of Smooth Muscle
NO neuromuscular junctions
Innervating nerves have axonal terminal swellings called varicosities
Varicosities release neurotransmitters into wide synaptic clefts called diffuse junctions
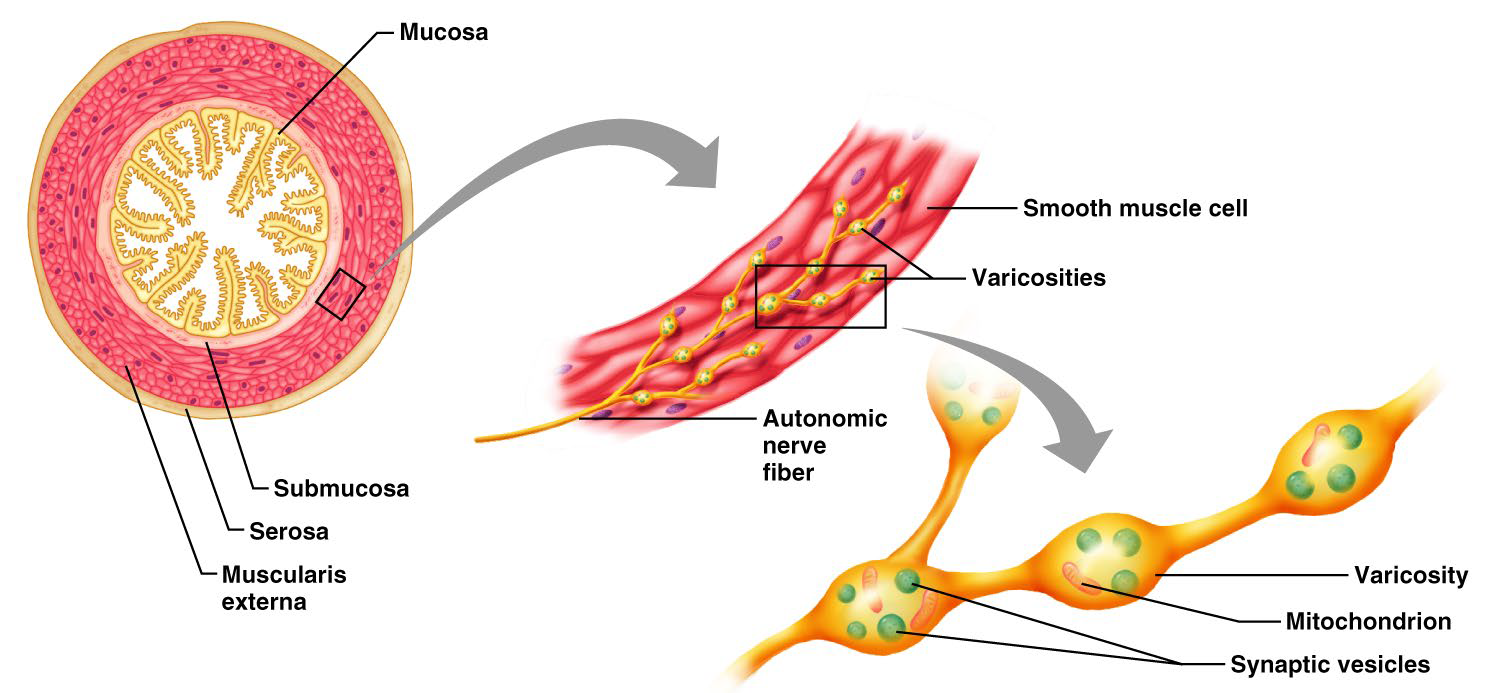
Microscopic Anatomy of Smooth Muscle
SR is less developed and lacks a specific pattern
NO T tubules
Plasma membranes have pouchlike infoldings called caveoli
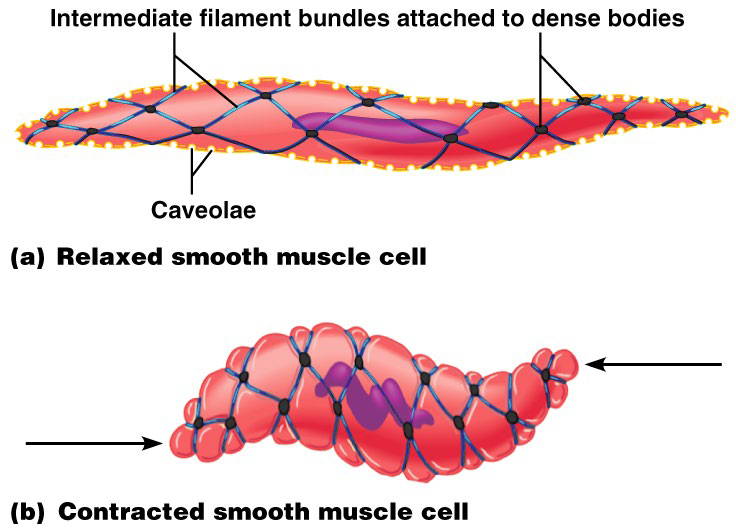
Ca2+ is sequestered by caveoli from outside the cell
NO striations + NO sarcomeres
Thin and thick filaments
NO troponin complex
NO Z discs
Thick and thin filaments arranged diagonally → corkscrew contraction
Smooth Muscle Contraction
They contract in unison
Gap junctions
Some smooth muscle cells: Act as pacemakers → Self-excitatory and depolarize without external stimuli
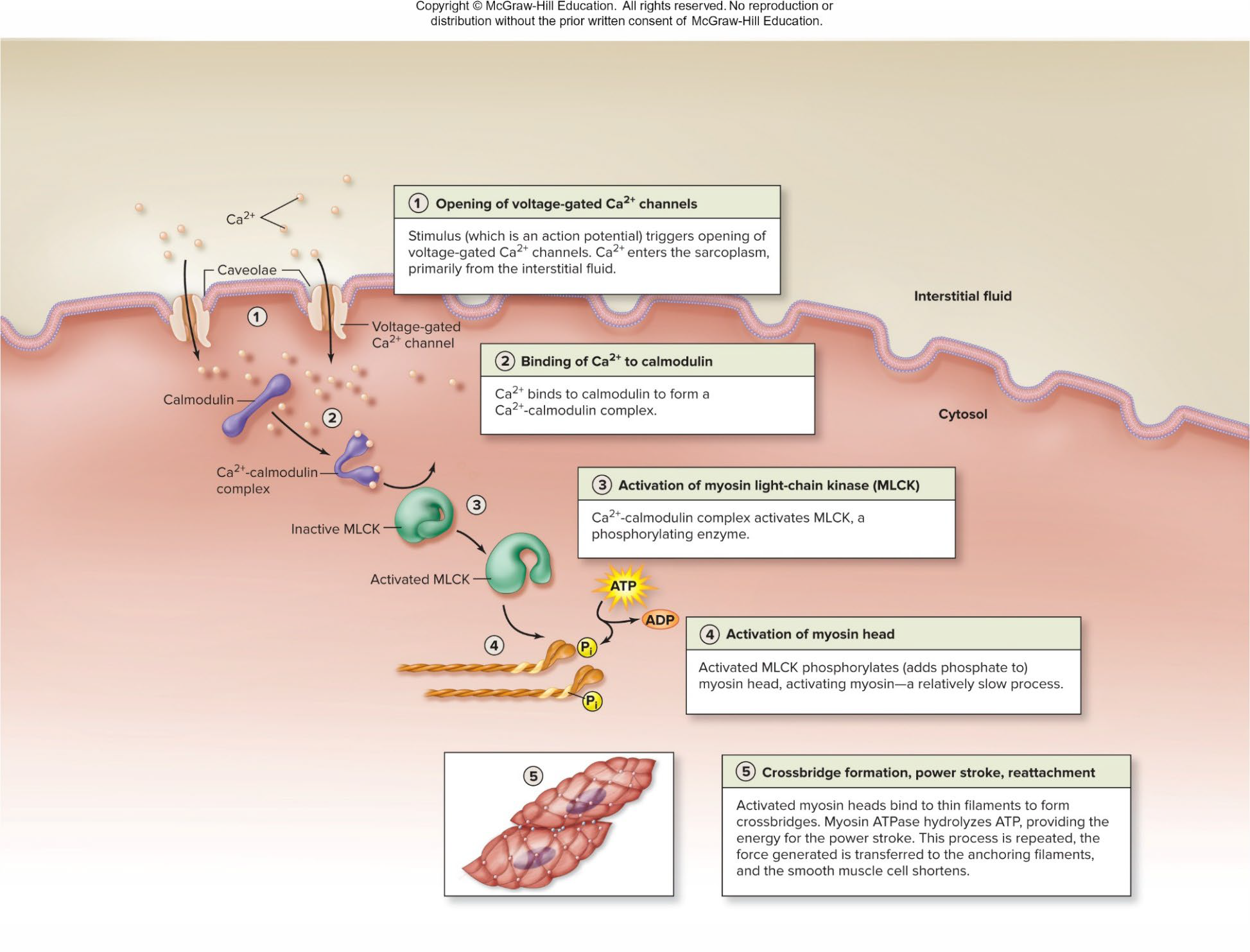
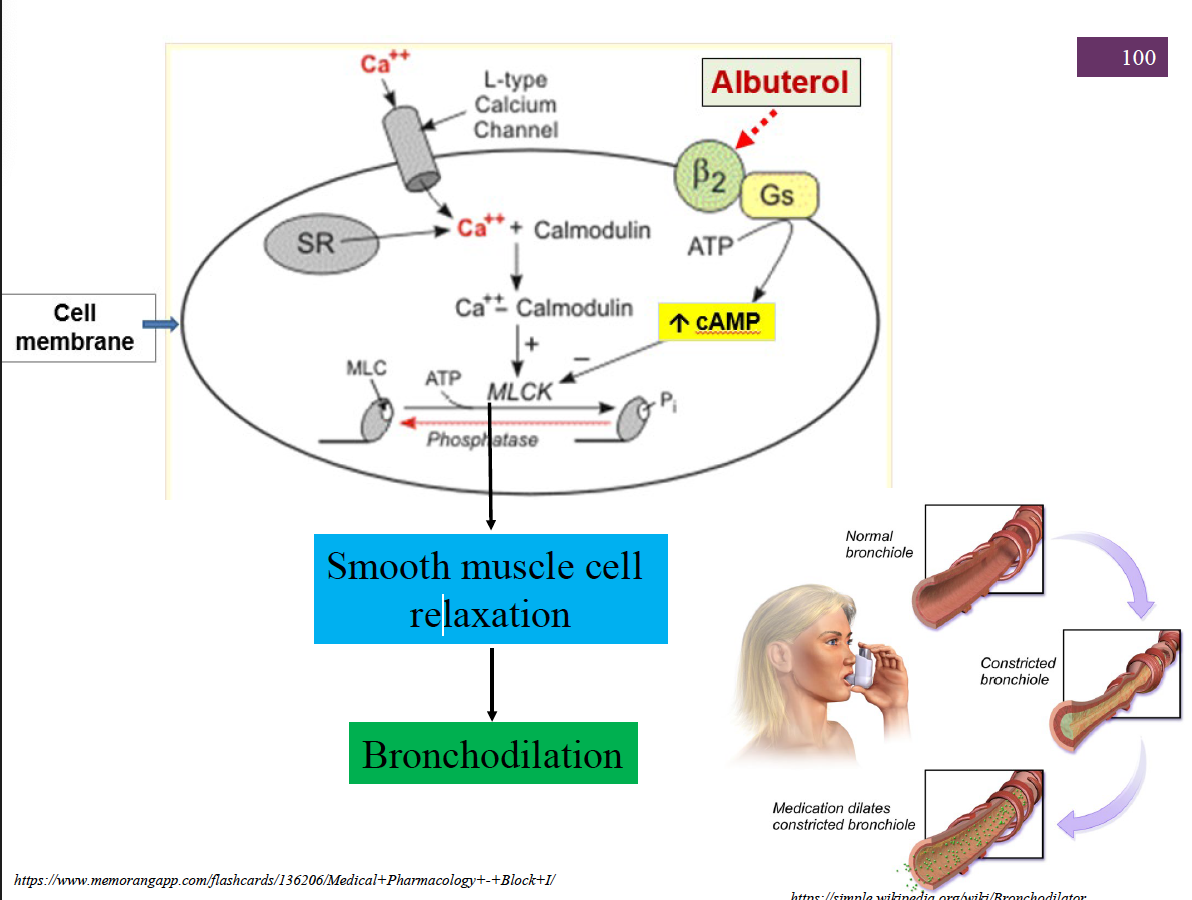
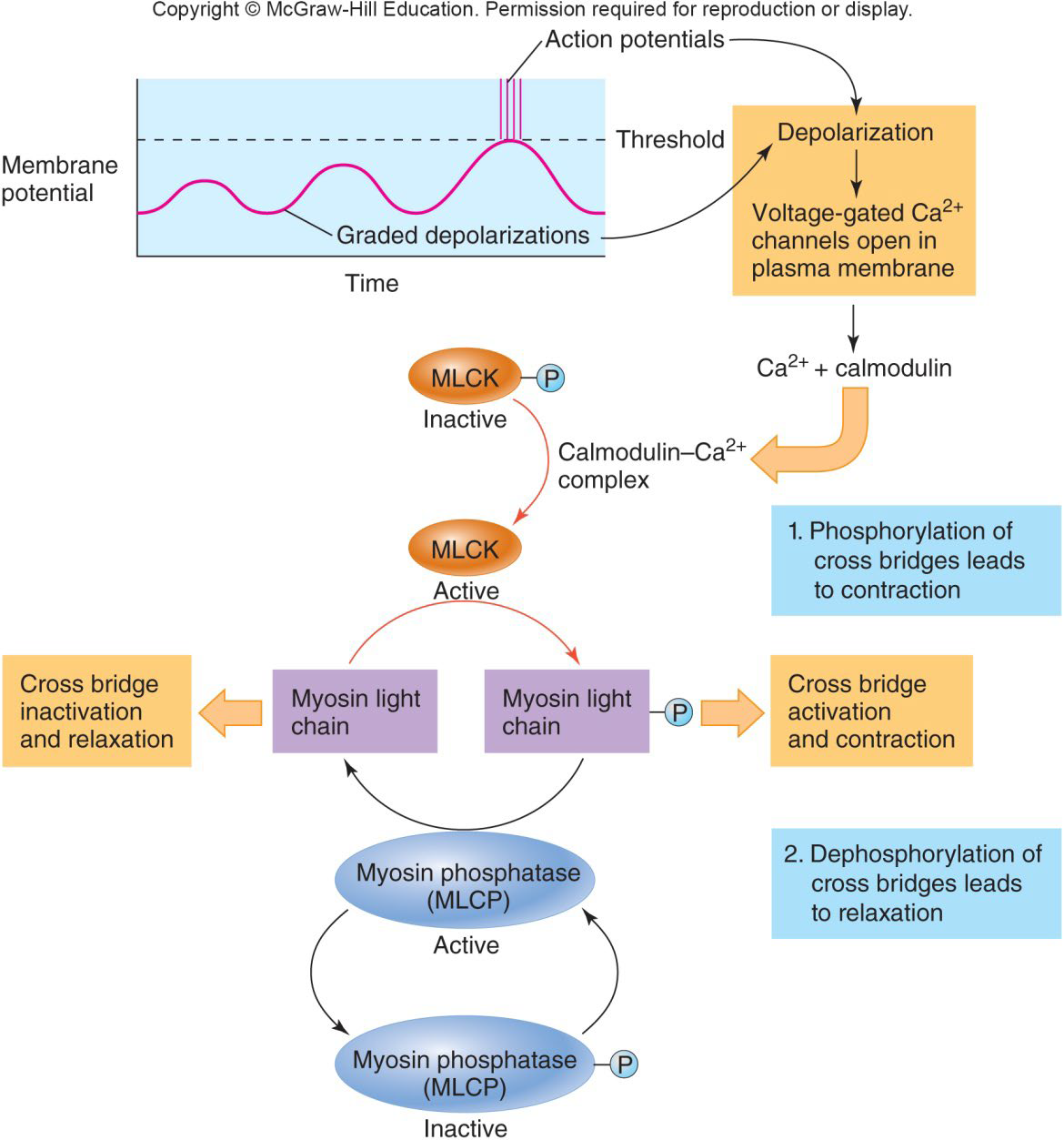
Excitation-Contraction Coupling in Smooth Muscle
Special Features of Smooth Muscle Contraction
Takes 30 X longer to contract and relax
Smooth muscle tone: without fatiguing
Slow, prolonged contractile activity
↓ energy requirements
Response to stretch
Response to Stretch
Stress-relaxation response:
Responds to stretch only briefly, and then adapts to its new length
However, it retains its ability to contract
This enables organs such as the stomach and bladder to temporarily store contents
Types of Smooth Muscle: Single Unit
Contract rhythmically as a unit
Are electrically coupled to one another via gap junctions
Often exhibit spontaneous action potentials
Are arranged in opposing sheets and exhibit stress-relaxation response
Types of Smooth Muscle: Multiunit
Their characteristics include:
Rare gap junctions
Infrequent spontaneous depolarizations
Structurally independent muscle fibers
A rich nerve supply, which, with a number of muscle fibers, forms motor units
Graded contractions in response to neural stimuli