Pharmacology Board Exam Review Video Notes
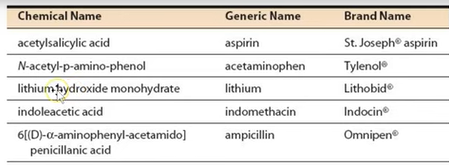
Drug Names:
Chemical name-determined by the chemical structure of the compound; the code name
Trade (Brand) name-Motrin, Advil (uppercase)
Generic name-ibuprofen (lowercase); before marketing (official name)
Characterization of Drug Action:
Potency
function/the amt of the drug requires to produce an effect
less amt=more potent
review proper dose of each drug before it’s prescribed
Efficacy
the maximum intensity of effect or response that can be produced by a drug
giving more drug won’t increase it, but increase the probability of an adverse reaction
NOT related
Pharmacokinetics: the study of how a drug enters the body, circulates within, and changed, and leaves
Four Major Steps: ADME
absorption
distribution
metabolism (biotransformation)-primary organ involved is the LIVER
excretion
Half-life: amt of time that passes for its [ ] to fall to half of its original blood level
4-5 half lives for a drug to be considered eliminated from the body
few drugs show zero-order kinetics (rate of metabolism remains constant over time)
Routes of Administration Dose Forms:
Onset-time it takes for the drug to begin to have its effect
Duration-the length of time of a drug’s effect
Enteral-via GI tract (oral, sublingual, rectal)
Oral
Pros-small intestine presents large absorbing area, produces slower onset of action
Cons-nausea, vomiting, some drug inactivated by acidity or enzymes, drug interactions, pt cooperation
Rectal
Pros-for vomiting or unconscious, local or systemic effect
Cons-poorly and irregularly absorbed, poor pt acceptance
Parental-via outside GI tract (intravenous)
Injection
IV
Pros-most rapid drug response, predictable response, emergencies
Cons-phlebitis, drug irretrievability, allergy, side effects related to high plasma [ ]
Intramuscular
Pros-increased tolerance to irritating drugs, allows injection suspensions (sustained effect)
Subcutaneous (insulin)
Cons-irritating solutions may cause sterile abscesses
Inhalation
Pros-rapid onset of action, no needles
Cons-popular route for abuse of drugs
Topical
Pros-systemic side effects are rare
Cons-increased risk of systemic side effects if surfaces are large and/or abraded, inflamed, or sloughing; intraorally spayed anesthetics may be absorbed into blood stream
Other
Intradermal-epidermis of skin
Intrathecal-spinal subarachnoid space
Intraperitoneal-body cavity
Agonists and Antagonists:
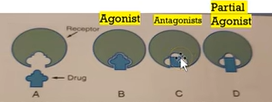
Agonist
affinity for a receptor
combines with the receptor
produces effect
Antagonist
counteracts action of agonist
Ex) competitive, noncompetitive, physiologic
Drug Tolerance:

Therapeutic Index= LD50/ED50

If small=toxicity is more likely
Pharmacologic Effects of Cholinergic Agents and Anticholinergic Agents
Cholinergic (Parasympathetic/cholinergic) ; acetylcholine
increase saliva, decrease HR + BP, pupil constriction
Anticholinergic (Mimic sympathetic/adrenergic) ; epinephrine
decrease saliva, increase HR + BP
Drug used to treat xerostomia
Pilocarpine-Salagren; parasympathetic/cholinergic
Hypertension Drugs: ABCD
Angiotensin Converting Enzyme (ACE) inhibitors
inhibit the enzyme that produces angiotensin II, which narrows blood vessels
dry cough
Drugs: enalaPRIL, lisinopRIL, PRIL
Angiotensin II Receptor Blockers (ARB)
block action of angiotensin II (narrows blood vessels)
Drugs: losarTAN, TAN
Beta blockers
Beta 1=increase heart muscle contraction
Beta 2=relax bronchial smooth muscles
Drugs-atenOLOL, lopresor, OLOL
Calcium channel blockers
Inhibit Ca (muscle contraction) from entering heart and blood vessels
gingival hyperplasia
drugs: nifediPINE (procardia), diltiazem, amlodiPINE, PINE
Diuretics
Drugs: hydrochlorothiazIDE, furosemIDE,
Congestive Heart Failure Drug: Digoxin
Pharmacologic effects
increases force and strength of heart contractions
reduces edema
Uses
treatment of HF
treatment of arrhthmias
Tip: Digoxin=Deep Contraction=Decreases HR
Anti-Anginal Drugs: Nitroglycerin
management of acute anginal episodes
prevent anginal attacks induced by stress or exercise
vasodilator
SL NTG
SL isosorbide dinitrate
Emergency drug

Anticoagulants:
drugs that interfere with coagulation
blood thinner
given in an attempt to prevent clotting
Warfarin (Coumadin) used after a MI or thrombophlebitis
Aspirin-anti platelet
Clopidogrel (Plavix)
Pain Drugs: Non-opioids and Opioids
Non Opioids:
NSAIDS
Ibuprofen (Advil, Motrin)- antipyretic, analgesic, anti-inflammatory
Naproxen (Aleve)-antipyretic, analgesic, anti-inflammatory
Acetaminophen (Tylenol)
Antipyretic, analgesic, NOT anti-inflammatory
Aspirin (salicylic acid)
anti-platelet
antipyretic, analgesic, anti-inflammatory
could be used for arthritis and cardiovascular diseases
not for peeps with acid stomach issues
Opiods:
Codeine
Tylenol #3
Most commonly used in dentistry
Morphine
Oxycodone
Bind to to three opioid receptors (Mu, Kappa, Delta)
Depresses the CNS and stops pain
Pharmacologic actions-analgesia, cough suppression, sedation and euphoria
Mechanism of action of nonopioid analgesics (prostaglandins, cox II)
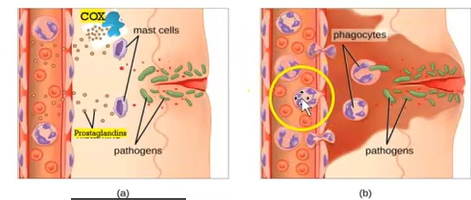
Acetylsalicylic Acid: Mechanism of Action (ASA Aspirin)
inhibit prostaglandin synthesis
enzyme cyclo-oxygenase (COX I and II)
Prostaglandins can
sensitize pain receptors
lower pain threshold to painful stimuli
cause inflammation and fever
affects vascular tone and permeability
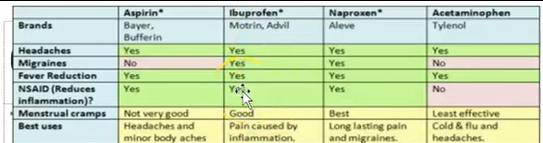
The Drug of Choice for Inflammatory Dental Pain is IBUPROFEN
The medication is contraindicated with aspirin is WARFARIN
Adverse effects of Opioids: Respiratory Depression
cause of death with overdose
elderly-decrease in pulmonary ventilation
reduced ventilation produces vasodilation
vasodilation results in intracranial pressure
mask CNS diagnostic symptoms
hyperthyroidism
hypothyroidism
Treatment Opioid Addiction
substituting oral opioid for injectable form
cold turkey
methadone maintenance
administering Naltroxen (Trexan) ; opioid antagonist
Specific Opioid Analgesics and Antagonists:
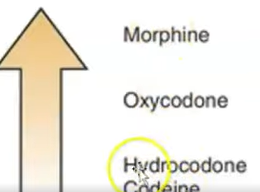
Opioid agonists
Morphine
Oxycodone
Oxymorphone
Hydrocodone
Codeine
meperidine
Hydromorphone
Methadon
Fentanyl family
Superinfection: Suprainfection
infection occurring after or on top of an earlier infection, especially following treatment with broad spectrum antibiotics (candidiasis after antibiotic use)
can be minimized by use of the most specific anti-infective agent, the shortest effective course of therapy, and enough doses

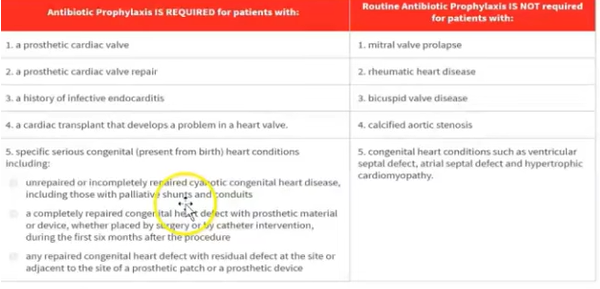
Antibiotic prophylaxis used in dentistry:
prosthetic cardiac valve
previous infective endocarditis
congenital heart disease (CHD)

Preventive antibiotic regimen for adults:
2g amoxicillin 1 hr prior to appointment
If patient is allergic to penicillin use:
600 mg clindamycin 1 hr prior to appointment
500 mg azithromycin 1 hr prior to appointment
500 mg clarithromycin 1hr prior to appointment
Anti-viral agents: Infections lesions: Herpes
self limiting to the patient with normal immunity
HSV 1= oral
HSV 2=genital
Treatment
antiviral agents: acyclovir, valacyclovir, penciclovir (topical only, reduces lesion duration and viral shedding by ½ day), docosanol (no prescription, reduces lesion duration and viral shedding by ½ day)
topical diphenhydramine (Benadryl) or viscous lidocaine
Kaopectate, Maalox Quick Dissolve, Mylanta Gas, Orabase plain or with benzocaine
according to the CDC, pts with active herpetic lesions can be treated provided that they are either emergency dental care or the treatment of the lesions only. All other care should be delayed
Antifungal agents: Nystatin for thrush
used for both treatment and prevention of thrush
cariogenic
sucrose content
lozenges
dentures
mechanism of action-binding to sterols in the fungal cell membrane
not absorbed from mucous membranes or intact skin
poorly absorbed from GI tract
excreted unchanged in the feces
fungicidal and fungistatic
Antifungal agents for thrush: Imidazoles
useful in dentistry (Clotrimazole/Mycelex and ketoconazole/nizoral)
Other-fluconazole (diflucan)
GI Diseases:
Ulcers
Causes- Helicobacter pylori and use of NSAIDs
Treatment-combo of one or more antibiotics and an H2 blocker or a PPI to reduce stomach acid
Histamine2 Blocking agents-block and inhibit gastric acid secretion by competitive inhibition of histamine at the H2 receptors of parietal cells: Cimetidine (Tagamet) is the prototype, Famotidine, Ranitidine, Nizatidine
Proton Pump Inhibitors PPIS Side Effects-headache, diarrhea (C. difficile), nausea, dizziness, mucosal atrophy of tongue, dry mouth, osteoportic fractures, gastroduodenal tumors

GERD
Antiemetics: drugs used to induce vomiting and to prevent vomiting
Phenothiazines (prochlorperazine)
Promethazine
Laxative: constipation
Bulk laxatives-pros (safest, act the most like normal physiology)
Lubricants-cons (interfere with absorption of fat soluble vitamins)
Stimulants-cons (intestinal cramping)
Stool softeners-Pros ( nontoxic)
Osmotic (saline) laxative-caution in peeps with renal implants
Antipsychotic Agents:
Mechanism of Action
1st gen-dopamine antagonists
2nd gen-action at more than one receptor
Slowing of psychomotor activity
calming of emotion
suppression of hallucinations and delusions
antiemetic

Best non-narcotic analgesic for the management of a dental pt with peptic ulcer disease or GERD is ACETAMINOPHEN
Antidepressant Agents:
Electroconvulsive therapy (ECT)
Fastest results seen with depression
Reserved for pts who are refractive to antidepressants
Selective serotonin reuptake inhibitors (SSRIs)

Fluoxetine (Prozac), citalopram (Celexa)
Serotonin norepinephrine reuptale inhibitors (SNRIs)
Tricyclic antidepressants (TCAs)
Amitriptyline (Elavile)
Other agents

Anti-anxiety Agents:
reduce anxiety, treat seizures, induce sleep
side effect-xerostomia
drugs used:
Benzodiazepines-reduced anxiety, anticonvulsants, muscle relaxants
Diazepam (Valium), lorazepam (Ativan), alprazolam (Xanax)
End in ZEPAM, ZOLAM
Anti-convulsants: Phenytoin
gingival enlargement symptoms
often painless enlargement of the gingival margin
interproximal papillae involvement
coalesce to cover occlusal surfaces of the teeth
prevention-oral hygiene, home care
Asthma:
reversible airway obstruction
linked with reductio in expiratory airflow
allergens
exercise
stress
URT infection
environmental pollution
signs-wheezing
COPD:
irreversible airway obstruction
chronic bronchitis is a result of chronic inflammation of the airways and excessive sputum production
emphysema is characterized by alveolar destruction with airspace enlargement and airway collapse
Metered-dose inhalers (MDIS)
Pros
med delivered directly into bronchioles
bronchodilator effect is greater than oral dose
inhaled dose can be accurately measured
rapid and predictable onset of action
compact, portable, and sterile
Sympathomimetic or adrenergic agents for asthma and copd
Inhaled short acting B2 agonists (asthma and copd_
Albuterol (Ventolin, ProAir HFA, Proventil)
Metaproterenol
Levelbuterol
Inhaled short acting B2 agonists/short acting anticholinergic combos (COPD)= Albuterol/Ipratropium
Sympathomimetic or Adrenergic agents for persistent asthma
Inhaled acting B2 agonists
Salmeterol
Budesonide/formoterol
Mometason/formoterol
Used with low does corticosteroids to treat not well controlled (low dose)
Corticosteroids for asthma
hasten recovery and decrease morbidity (reduce hyperreactive airway) despite no immediate benefits in acute asthma attack
Inhaled-most effective long term treatment for persistent asthma
Beclomothasone and Fluticasone
Oral corticosteroids
Prednisone
Adverse effects with chronic use of inhalation
Candidiasis
Local Anesthesia:
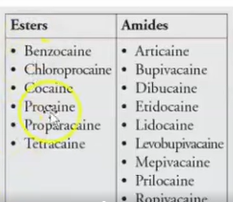
Ester
metabolized in plasma
allergic
Amide
metabolized in liver
no allergic reactions
I before caine
Don’t give too much epinephrine to cardiac patients (0.04 mg max dose)
healthy patients (.20 mg)
not for uncontrolled diabetes
carefully if someone is on tricyclic antidepressants
LA Agents:
Lidocaine
safe in pregnancy
can have epinephrine or be plain
Mepivacaine
can have levonordefrin or plain
used in short in dental procedures if epinephrine is contraindicated
Bupivacaine
teratogenic in rats (category C)
slow onset (takes long to kick in)
used for long dental procedure (7 hours!)
Vasoconstrictor:
vasodilation when LA
epinephrine and levonordefrin (more toxic)
constrcition=longer duration
Nitrous Oxide:
oxygen for 5 min to prevent diffuse hypoxia
relieve anxiety
conscious, can follow instructions
weak anesthetic agent, pain free, can cause memory loss
average peeps needs 35% nitrous oxide in oxygen with a range of 10 to 50%
adverse effects: nausea, vomiting
NO respiratory depression, bronchodilation or low P
Contraindications
COPD
Respiratory obstructions
1st trimester
bowel obstructions
Immunosuppressant drug:
used in organ transplant pts to prevent rejection of organ
azathioprine, cyclosporine (gingival enlargement), tacrolimus
Bisphosphonate drugs
prevent loss of bone density for osteoporosis, slow tumor development
Many cancer pts with pain may take this=can develop osteonecrosis of the jaw
Diabetes:
Type I=can’t make insulin (need injections)
Type II=can’t make enough or use insulin; metformin, fortamet
side effects=hypoglycemia (most common), poor wound healing, weight gain, infections