Oral Mucosa Notes
Oral Mucosa
Learning Objectives
Identify and describe the general structure of mucosal surfaces in the body.
Compare and contrast the structure of mucosa with other lining epithelia like skin.
Compare the microscopic structure of oral cavity mucosa with the GIT (gastrointestinal tract) mucosa regarding their functions.
Demonstrate knowledge of oral cavity anatomy, including features of the vestibule and oral cavity proper regions.
Show knowledge of the structure and function of different types of oral mucosa (classified by function: masticatory, lining, and specialized).
Compare and contrast the types of epithelium from different regions of the oral cavity (keratinized vs. non-keratinized, orthokeratinized vs. parakeratinized).
What is Oral Mucosa?
Oral mucosa is a mucous membrane, which are moist linings of body cavities that communicate with the exterior.
Examples of locations: oral cavity, nasal passages, pharynx, GIT, and urogenital tract (UGT).
Oral Mucosa Details
Oral mucosa is a mucous membrane that's a moist lining of the oral cavity.
Structurally, it resembles skin and other mucous membranes like those in the esophagus, cervix, and vagina.
It is notably different from GIT mucosa.
Mucous Membrane Functions
Mucous membranes are moist linings of body cavities that communicate with the exterior.
They line various cavities/lumens in the body and cover the surface of internal organs.
Functions include:
Protection of underlying tissues.
Prevention of dehydration.
Prevention of pathogen entry.
Prevention of particulate matter entry.
Mucosa Layers
Epithelium
Lamina propria:
Underlying connective tissue.
Loose papillary layer.
Dense reticular layer.
Muscularis mucosa:
Only present in GIT.
Not present in oral tissues.
Comparison of Epithelial Linings
Oral mucosa is structurally similar to skin, esophagus, cervix, and vagina.
It differs significantly from GIT mucosa.
Mucosa Barrier Function
Epithelium:
Protection (physical/mechanical, chemical, and cellular).
Lamina propria:
Protection (cellular/immune defense).
Ground substance (attachment, mechanical).
Muscularis mucosa:
Absent in oral mucosa.
Nomenclature of Layers: Oral Coverings vs. Skin
Oral mucosa:
Epithelium.
Lamina propria (papillary & reticular layers).
Submucosa (not always present).
Skin:
Epidermis.
Dermis (papillary & reticular layers).
Hypodermis.
Functions of Oral Mucosa
Function | Structures Involved |
|---|---|
Protection | Epithelium (stratum corneum) |
Friction/abrasion | Mechanical role |
Compression/shearing | Lamina propria (collagen/elastin) |
Barrier role | Epithelium (superficial barrier), Molecules |
Taste | Epithelium (taste buds) |
Sensory | Epithelium & lamina propria (sensory receptors) |
Synthesis/secretion | Saliva (minor salivary glands in lamina propria/submucosa) |
Esthetics | Vermilion border of lips, Sebaceous glands (lamina propria) |
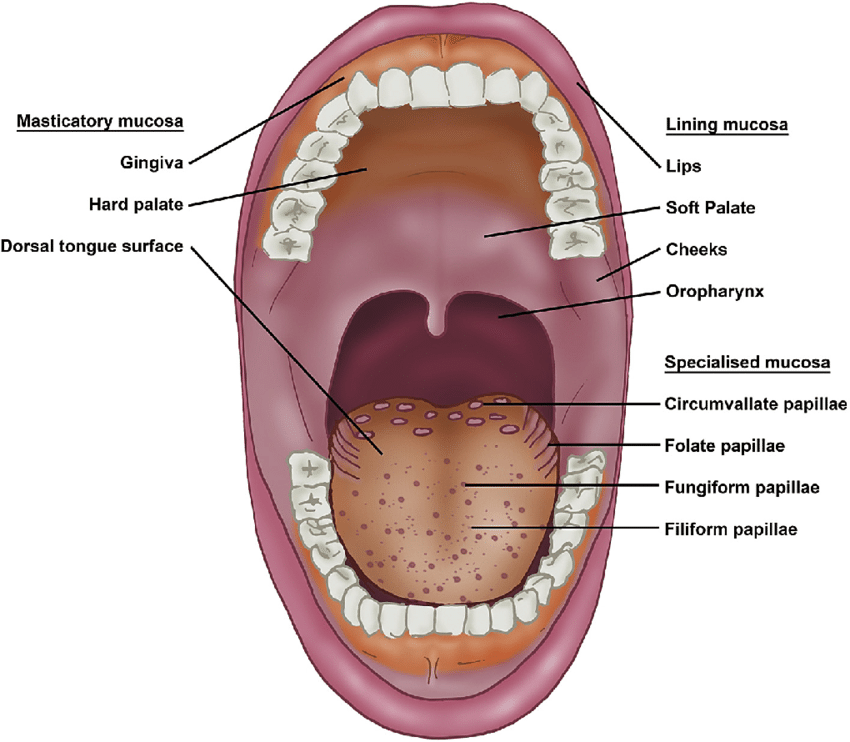
Anatomy of the Oral Cavity
Structures include:
Teeth, gingiva (gum).
Hard palate, soft palate, uvula.
Tongue, tonsil.
Buccal mucosa (lip and cheek lining).
Floor of mouth, lip.
Oral Cavity Definition
The oral cavity extends from the lips to the pharynx and contains the tongue and teeth.
Two parts:
Vestibule:
Space between the lips/cheeks (labial & buccal).
Oral cavity proper:
Enclosed by teeth.
Contains the hard & soft palates and the mouth floor.
Oral Mucosa Lining - Vestibule
Attached gingiva.
Alveolar mucosa.
Lining mucosa.
Vermillion zone.
Adjoining labial mucosa.
Secretions from minor salivary glands.
Types of Oral Mucosa (Classified by Function)
Masticatory mucosa: 25% of total area.
Lining mucosa: 60% of total area.
Masticatory vs. Lining Mucosa
Masticatory mucosa (mucoperiosteum):
Epithelium, lamina propria, and bone.
Lining mucosa:
Epithelium and lamina propria.
Types of Keratinization
A. Keratinization:
* Keratinization Subtypes
* Orthokeratinization
* Parakeratinization
B. Non-keratinization:
* Buccal mucosa
Parakeratinized vs. Orthokeratinized Epithelium
Parakeratinized epithelium:
Similar to keratinized epithelium, except cell nuclei are present in the keratinized layer (stratum corneum).
Present in the oral cavity, specifically the gingiva.
Outside of the oral cavity it's considered a pathology.
Orthokeratinized epithelium:
Normal keratinized epithelium.
Present in skin or the outer part of the lip.
Comparison of Stratified Epithelium
A. Orthokeratinized epithelium:
* Keratinized layer.
* Granular layer.
* Prickle cell layer.
* Basal cell layer.
B. Parakeratinized epithelium:
* Keratinized layer.
* Granular layer.
* Prickle cell layer.
* Basal cell layer.
C. Nonkeratinized epithelium:
* Superficial layer.
* Intermediate layer.
* Prickle cell layer.
* Basal cell layer.
Oral Cavity Mucosa
Lining mucosa:
Present on the lips, buccal mucosa, alveolar mucosa, soft palate, underside of the tongue, and floor of the mouth.
Epithelium is usually nonkeratinized.
Masticatory mucosa:
Hard palate and gingiva regions.
Specialized mucosa on the dorsum of the tongue.
Inflexible, tough, resistant to abrasion, and tightly bound to the lamina propria.
Covered by a layer of keratinized cells (except sulcular and junctional).
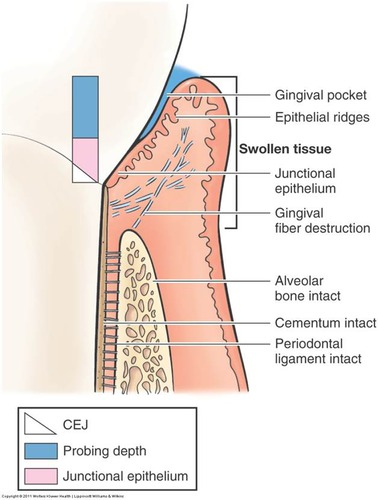
Gingival Mucosa - Dentogingival Junction
Papillary layer of lamina propria.
Enamel space.
Free gingiva.
Junctional epithelium (attaches to enamel).
Attached gingiva (tooth, below to bone).
Oral Mucosa Orientation
Includes structures such as:
Vermillion border, hairy skin.
Gingiva, enamel, dentine, pulp, cementum.
Free gingiva, attached gingiva, alveolar mucosa.
Gingival margin, gingival groove, mucogingival junction.
Gingival crevice/sulcus.
Junctional epithelium.
Periodontal membrane.
Skeletal muscle.
Root canal, apical foramen.
Alveolar bone, body of mandible.
Cementoenamel junction.
What's Below the Mucosa?
Submucosa:
Present in cheeks, lips, and hard palate.
Contains adipose/glandular tissue, nerves, and blood vessels.
Direct attachment to bone in some places (oral mucosa, gingiva, parts of hard palate) directly to periosteum.
Submucosa is absent leading to firm inelastic attachment
Desmosomes.
Hemidesmosomes.
Tonofilaments.
Gap & tight junctions.
Lining Mucosa
Non-keratinized stratified squamous epithelium.
Locations:
Lips.
Buccal mucosa.
Alveolar mucosa.
Soft palate.
Underside of the tongue.
Floor of the mouth.
Masticatory Mucosa (Summary)
Keratinized stratified squamous epithelium.
Locations:
Hard palate.
Attached gingiva.
Dorsum of tongue.
Areas of repeated mechanical exposure/physical damage exhibit distinct resistance to deformation under load, abrasion, thermal, and chemical damage.
Questions to Consider
What is a mucosa?
What are the structural & functional differences between lining mucosa & masticatory mucosa?
How does the mucosa function as a barrier?
What is the difference between orthokeratinised & parakeratinised epithelium?
How is oral mucosa classified by function?
References
Mescher AL Junquiera’s Basic Histology McGraw-Lange 13thEd
Kerr JB Atlas of Functional Histology
Nanci A. Ten Cate’s Oral Histology Development Structure and Function 6th Ed Mosby
Squier C & Brogden K 2011, Human Oral Mucosa Development, Structure & Function Wiley-Blackwell
Turabelidze A, Guo S, Chung AY, Chen L, Dai Y, Marucha PT, et al. (2014) Intrinsic Differences between Oral and Skin Keratinocytes. PLoS ONE 9(9): e101480. doi:10.1371/journal.pone.0101480 http://dx.doi.org/10.1371/journal.pone.0101480