WEEK 15 - Abdominal cavity and GI tract INTRO
Lecture learning objectives- PART 1 AND 2
To identify the boundaries of the abdominal cavity and which organs are within this cavity
To name the intraperitoneal and retroperitoneal organs
To differentiate between parietal and visceral peritoneum and explain what is the peritoneal space
To identify and explain the main functions of the mesenteries and, greater and lesser omentum, greater and lesser sacs and pouches/cul-de-sacs
To Identify the components of the GI tract and the accessory organs of digestion and their main functions
Abdominal Cavity
Body Cavities
= Body compartments that contain the organs
are maintained by = membranes, sheaths and structures
abdominopelvic cavity is the largest in the body
ABD Cavity Boundaries
Superior = Diaphragm
Inferior = Pelvic Inlet
Ant/Post/Lat = Abdominal walls (inferior ribs and costal cartilages, lumbar vertebrae L1-L5, abdominal muscles)
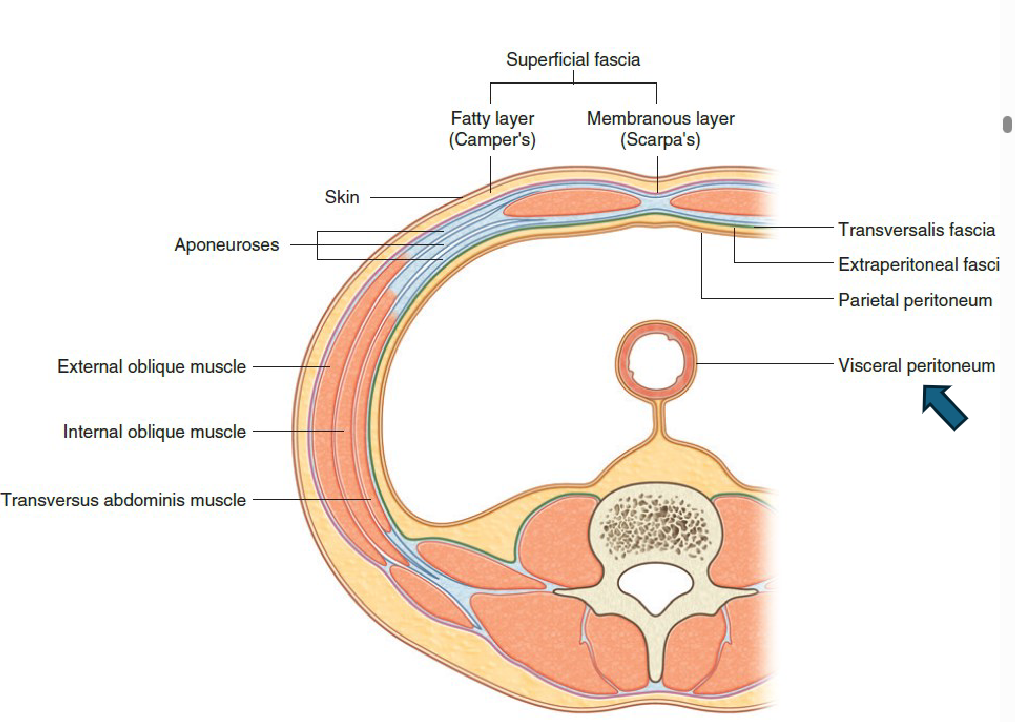
Layers of the ABD Wall
Skin
Superficial fascia
a. Camper’s fascia - Superficial fatty fascia
b. Scarpa’s fascia – Superficial membranous fascia
Muscles
a. External obl
b. Internal obl
c. Transverse abdominis
d. rectus abdominis
Transversalis (connective tissue)
Extraperitoneal fascia (fat)
Parietal Peritoneum
ABD Cavity Organs
GI tract organs: stomach and intestines (digestive system)
Kidneys (adrenal gland) and ureters (urinary system)
Liver, gallbladder, pancreas (endocrine and digestive functions)
Spleen (immune system)
Peritoneum
= Serous membrane lining the abdominal cavity walls and covering many of the abdominal visceral organs
PARIETAL PERITONEUM = lines the walls of the abdominal cavity
VISCERAL PERITONEUM = package visceral organs
INTRAPERITONEAL
= Organs ALMOST entirely enclosed by visceral peritoneum
e.g. stomach
RETROPERITONEAL
= Organs localized outside of the peritoneum cavity
e.g. kidney
MESENTERY
= double layer of peritoneum (continuity of visceral + parietal)
NOTE: Every organ must have an area not covered by visceral peritoneum to
allow the passage of nerves and vessels
Retroperitoneal Space
located between the posterior abdominal wall and the parietal peritoneum
where organs outside the peritoneal cavity reside
Retroperitoneal Organs
S – suprarenal (adrenal gland)
A – aorta/IVC
D – duodenum (2nd and 3rd parts)
P – pancreas (except tail)
U – ureters
C – colon (asc. and desc.)
K – kidneys
E – esophagus
R – rectum
Peritoneal Cavity
= Potential space between parietal and visceral layers of peritoneum
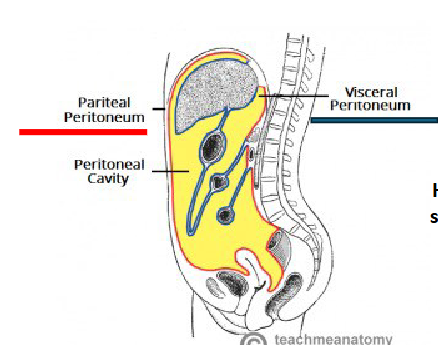
Peritoneal Fluid
produced by = serous peritoneal membrane
found within = the peritoneal cavity (thin layer)
function = to provide essential lubrication and allows sliding of viscera
without friction or irritationcontains = white blood cells and antibodies (immune function)
accumulation of PF = ascites
Mesenteries
= Fold of peritoneal membrane (double layer)
contains = blood vessels, lymphatic vessels and nerves supplying intraperitoneal organs
Functions
Suspend and anchor intraperitoneal organs to the posterior abdominal wall
Provide flexibility of movement in the abdomen for the intraperitoneal organ BUT tethers the organ to the posterior abdominal wall
Prevent blood vessels to get tangled
Mesenteries of the ABD cavity
MESENTERY OF THE SMALL INTESTINE
Suspends the majority of the small intestine from the posterior abdominal wall
TRANSVERSE MESOCOLON
Connects transverse colon to the posterior abdominal wall
SIGMOID MESOCOLON
Connects sigmoid colon to the posterior abdominal wall
Stomach
shape = J- shape
Curvatures
Lesser Curvature (medial)
Greater Curvature (lateral)
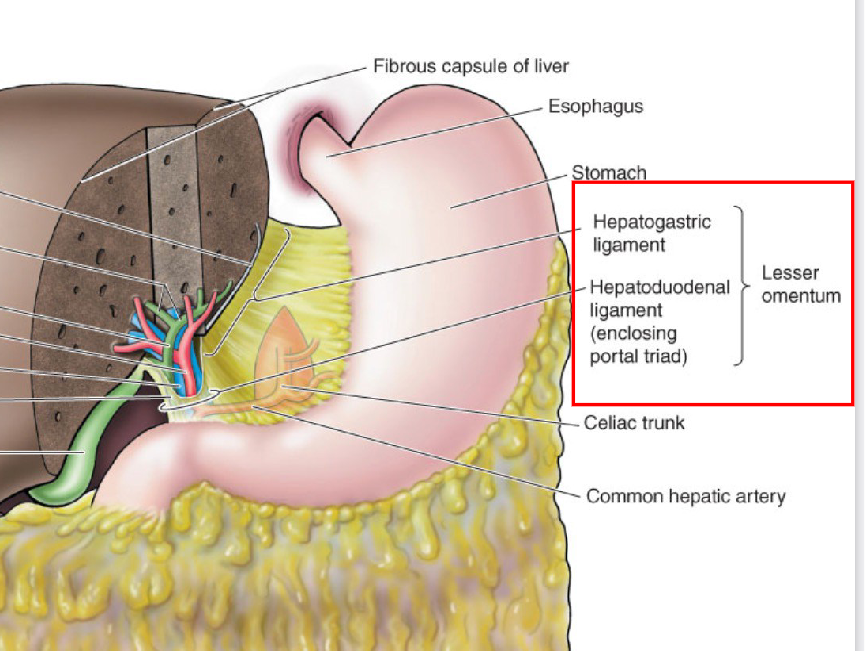
Lesser Omentum
= Mesentery extending between the liver and the lesser curvature of the
stomach and proximal 1st part of duodenum
HEPATOGASTRIC LIGAMENT = anchor liver to stomach
HEPATODUODENAL LIGAMENT = anchors liver to the initial part of intestine; passageway for the portal triad (hepatic portal vein,
hepatic artery proper, common bile duct)
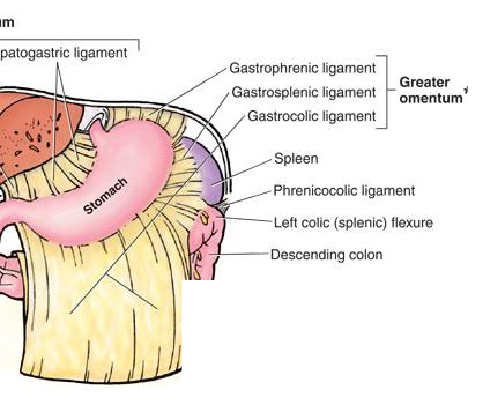
Greater Omentum
= generally, location for at storage, passageway for vessels and, physical and immune protection
= Mesentery that form an “apron” draping off the greater curvature of the
stomach
GASTROPHRENIC LIGAMENT = Anchors stomach to diaphragm
GASTROSPLENIC LIGAMENT = Anchors stomach to spleen
GASTROCOLIC LIGAMENT = Anchors stomach to duodenum and covers the intestine and abdominal viscera
Sacs
= omenta subdivide the peritoneal cavity into the greater sac and the lesser sac
Connection Between Sacs
OMENTAL FORAMEN (of Winslow) – EPIPLOIC FORAMEN = an opening posterior to the hepatoduodenal ligament
Greater Sac
= accounts for most of the space in the peritoneal cavity
= extends from the diaphragm to the pelvic cavity
Compartments
Supracolic Compartment = Superior to the colon and anterior to the greater omentum
SUBPHRENIC SPACE ➔between diaphragm and anterior
surface of liverSUBHEPATIC SPACE ➔between visceral surface of liver and right kidney
Infracolic Compartment = Inferior to the colon, posterior to the greater omentum
Lesser Sac / Omental Bursa
= posterior to the lesser omentum and the stomach but anterior to the pancreas
Anterior wall = lesser omentum and posterior wall of stomach
Left Lateral wall = gastrosplenic ligament and splenorenal ligament
ABD Cavity Floor
= ABD Cav is continuous with pelvic cavity but parietal peritoneum that lines the
abdominal cavity drapes over the organs of the pelvic cavity creating ”pouches” between adjacent pelvic organs
Male Pouches / cul-de-sacs
RECTOVESICAL POUCH = between bladder and rectum
Female Pouches / cul-de-sacs
VESICO-UTERINE POUCH = (anterior cul-de-sac) - between bladder and
uterusRECTO-UTERINE POUCH OF DOUGLAS = (posterior cul-de-sac) – between uterus and rectum
GI Tract
= Continuous muscular tube
Composition:
mouth
pharynx
esophagus
stomach
small intestine
large intestine
anus
Accessory Organs
teeth
tongue
salivary glands
liver
gallbladder
pancreas
Oral Cavity
first step in digestion through the secretion of saliva
types of salivary glands:
Parotid
Sublingual
Submandibular
Pharynx
Oropharynx
laryngopharynx
NOTE: both are shared by respiratory and digestive systems
Esophagus
= collapsible muscular tube extending from laryngopharynx to stomach, posterior to trachea
Anterior to thoracic aorta and posterior to trachea
Pierces diaphragm at the esophageal hiatus (level → T10)
Layers:
adventitia
Fibrous tissue connecting it to neighboring structures
small vessels, lymphatic vessels and nerves
muscularis propria
Transition from skeletal (upper 1/3) to smooth muscle
Inner circularly arranged layer
Outer longitudinally arranged layer
submucosa
Connective tissue
Esophageal mucous glands
mucosa
Nonkeratinized stratified squamous epithelium
Lamina propria
Muscularis mucosae (smooth muscle)
Function:
Propulsion of food bolus to stomach by PERISTALSIS (wave-like)
UPPER ESOPHAGEAL SPHINCTER (skeletal muscle) = pharynx into Esophagus
LOWER ESOPHAGEAL SPHINCTER (smooth muscle) = prevents retrograde movement of stomach contents
Stomach
= stores food and continues the digestion (little) that started in
the mouth
Intestines
small intestine
= where most of digestion occurs (and finishes)
duodenum
jejunum
ileum
large intestine
absorption of water and formation of feces
Rectum
= feces exit through the anus
GI Tract Wall Layers
Mucosa Layers (inner - outer)
Surface Epithelium
Stratified squamous (ex. pharynx, esophagus)
Simple columnar (ex. stomach, small intestine)
Secretory cells (especially for mucus and enzymes will be found in here)
Continuously being replaced (stem cells)
Lamina Propria
loose connective tissue holding epithelium in place
Small blood vessels and lymphatics, lymphoid tissue, innervation, immune cells absorbed nutrients enter the blood/ lymph circulation here
Muscularis mucosae
Thin layer of smooth muscle
Submucosa Layers
= Regulates release of digestive secretions based on the detected
presence of food in the lumen
Loose connective tissue layer with large blood vessels and lymph vessel
Submucosal glands - secrete mucus
Submucosal (Meissner’s) plexus→ enteric nervous system
(ENS) → innervates structures of the mucosa and submucosa
Muscularis Externa Mucosa
Proximal GI Tract = skeletal muscle
Distal GI Tract = smooth muscle
inner sheet of circularly arranged fibers (decreases diameter)
between muscle layers: Myenteric plexus (Auerbach’s plexus) = innervation that controls GI tract motility - peristalsis and segmentation
outer sheet of longitudinally arranged fibers (decreases length)
Serosa Histology
= Serous membrane (visceral peritoneum) covering organs within the abdominal cavity (outer layer)
Mesothelium (simple squamous)
Loose connective tissue (thin layer)
Functions:
Secretes serous fluid
Facilitates movement /reduce friction