Endothelial Cells Lecture Notes
Lecture Overview
Module: PHSI3X10
Lecture Number: 15
Presenter: A/Prof Anna Waterhouse
Focus: Endothelial Cells
Context: Chronic Diseases
Last Lecture Summary
Discussion on collagen layers in heart valves and their roles:
Spongiosa: Contains hyaluronan and proteoglycans
Ventricularis: Composed of elastin, fibrillins, and fibulin
Fibrosa: Contains collagens I, III, V
Basement membrane: Composed of collagen IV, laminin, perlecan, fibronectin
Endomysial collagen: Allows for stress-bearing coaptation, compression, and extension
Today's Lecture Objectives
Features and functions of endothelial cells
Role of the endothelium in homeostasis
Mechanical forces on endothelial cells, their sensory pathways for shear and pressure
Causes and consequences of endothelial dysfunction
Characteristics of Endothelium
Structure:
Inner cellular lining of blood vessels and lymphatic system, 1 cell layer thick
Contact with fluids (blood/lymph), the body’s largest organ (>1 kg, 1-2 trillion cells, ~4000-7000 m² surface area)
Morphology:
1-2 μm thick, 10-20 μm diameter, 'cobblestone' appearance
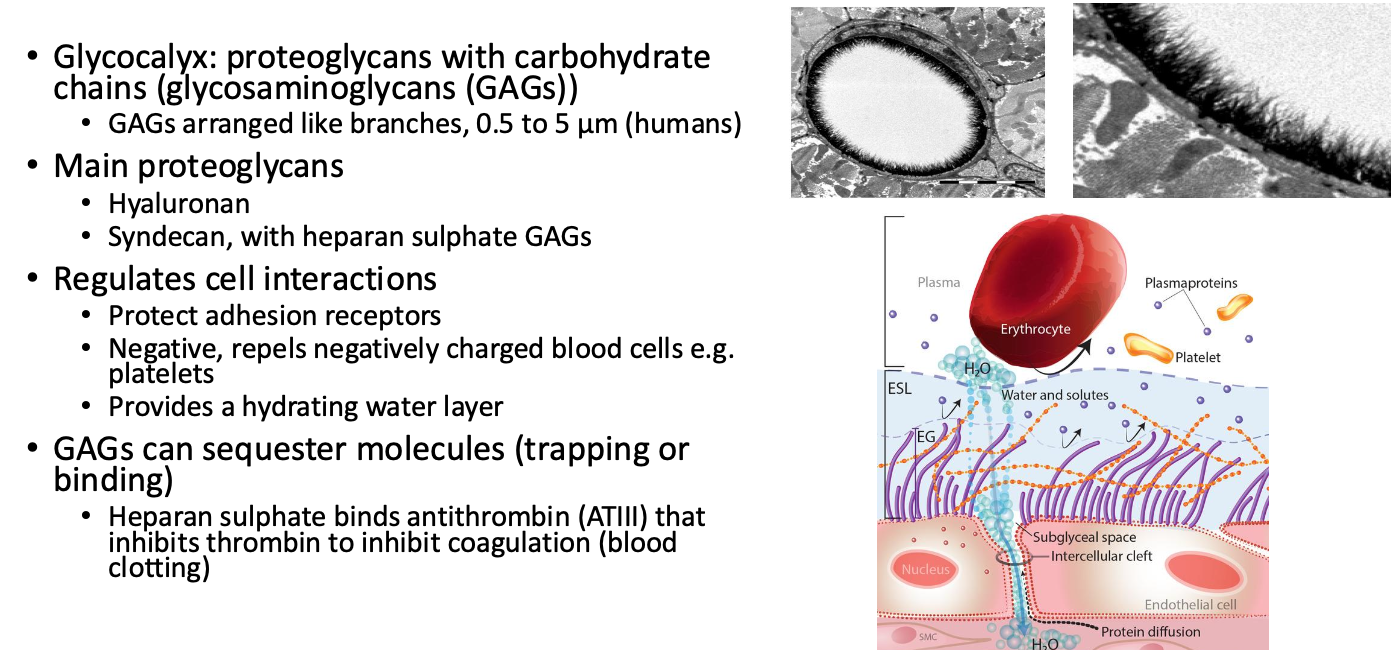
Glycocalyx: made of proteoglycans with carbohydrate chains
Tight junctions: Maintain vessel wall integrity but are disrupted by toxins (e.g., nicotine) leading to disease
Endothelial Cell Functions
Contains vesicles for transport (pinocytosis and macropinocytosis)
Facilitates bulk exchange of gases, nutrients, etc.
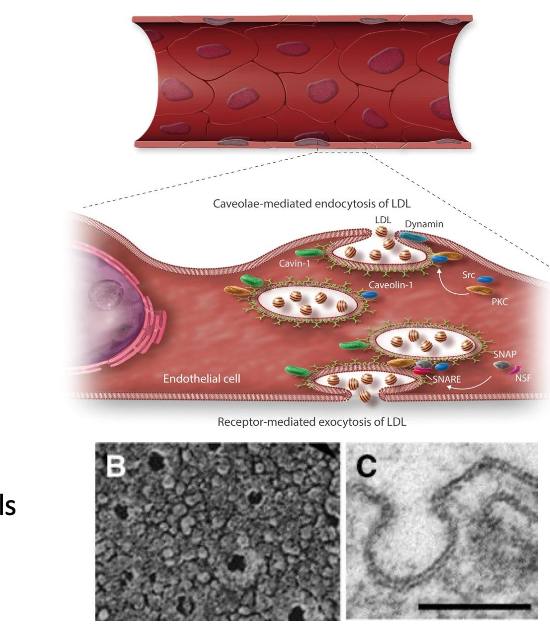
Caveolae: Specialized vesicles that mediate endocytosis and transcytosis, containing caveolin
Weibel-Palade Bodies: Storage granules for von Willebrand Factor; play role in thrombosis and inflammation
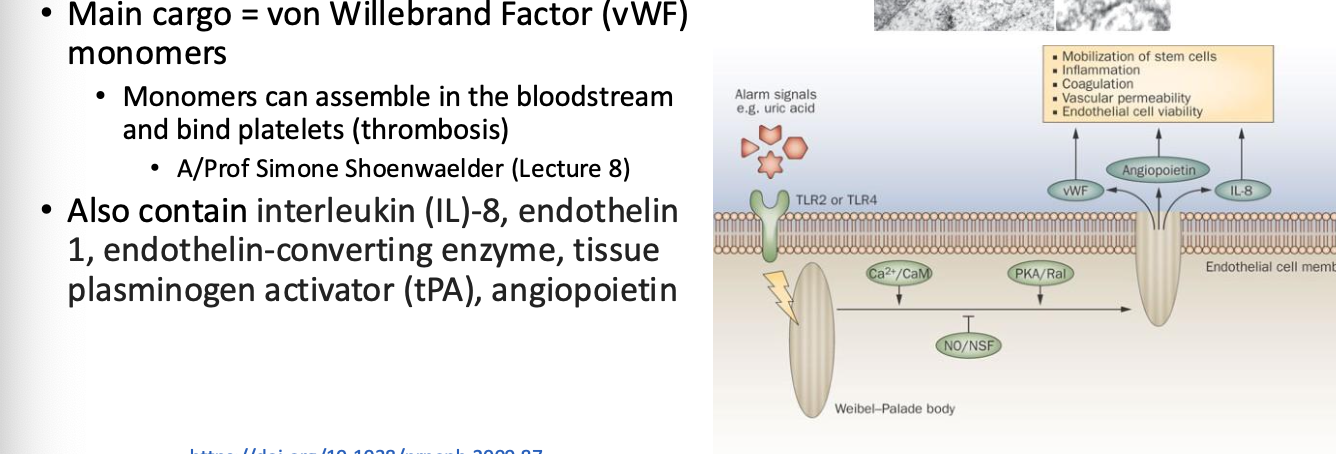
Arrangement of Endothelial and Smooth Muscle Cells (SMCs)
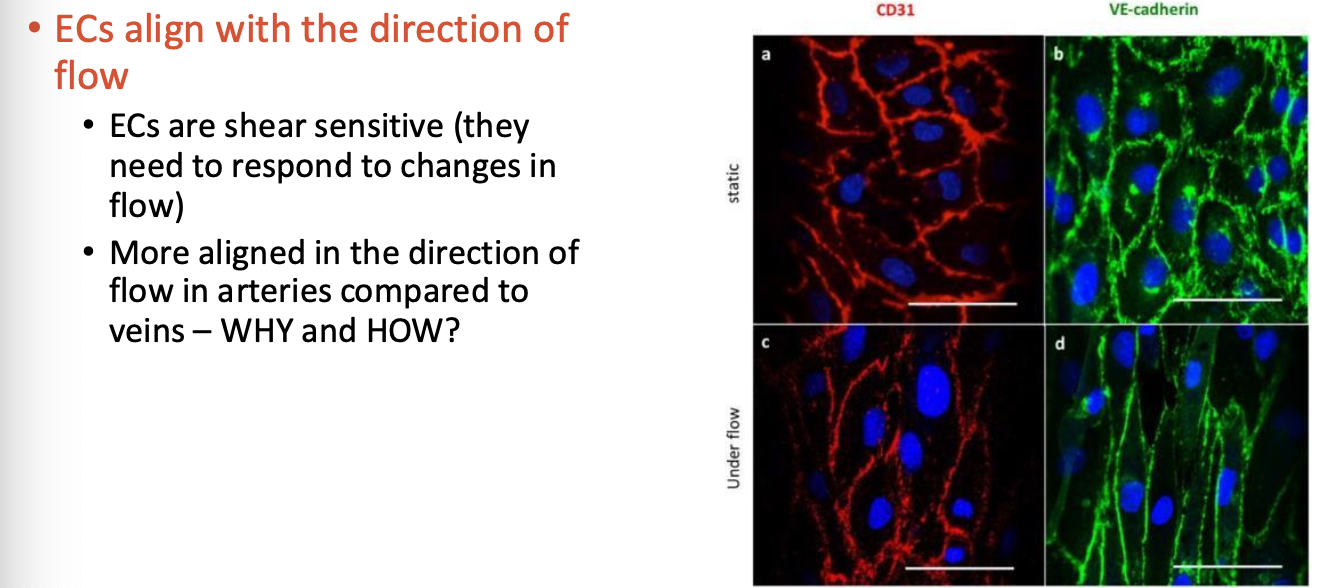
ECs align with blood flow, responding to biochemical and physical changes
SMCs: Organized circumferentially, providing pulsatile force
Barrier Function: ECs act as a semipermeable barrier between blood and SMCs
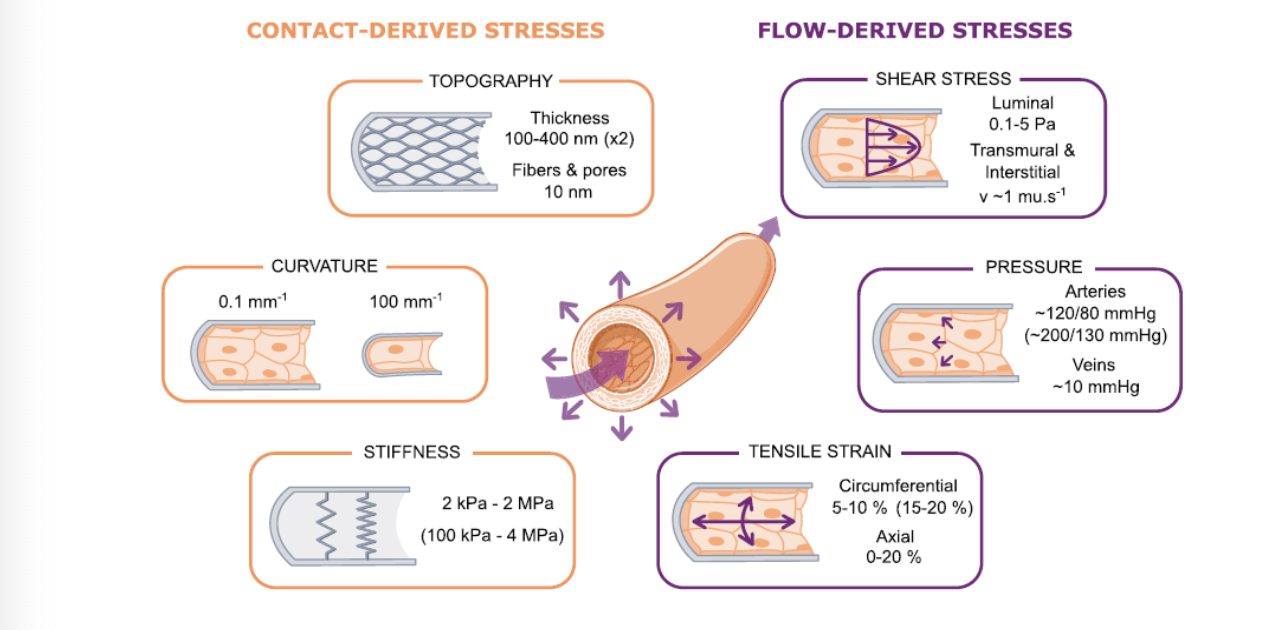
Mechanical Forces on Endothelial Cells
Contact-derived stresses and flow-derived stresses:
Shear Stress: Range of 0.1-5 Pa
Transmural and interstitial pressure: Affects ECs significantly
Tensile strain: 5-20%; arterial pressures ~120/80 mmHg
Roles of Endothelium in Cardiovascular Function
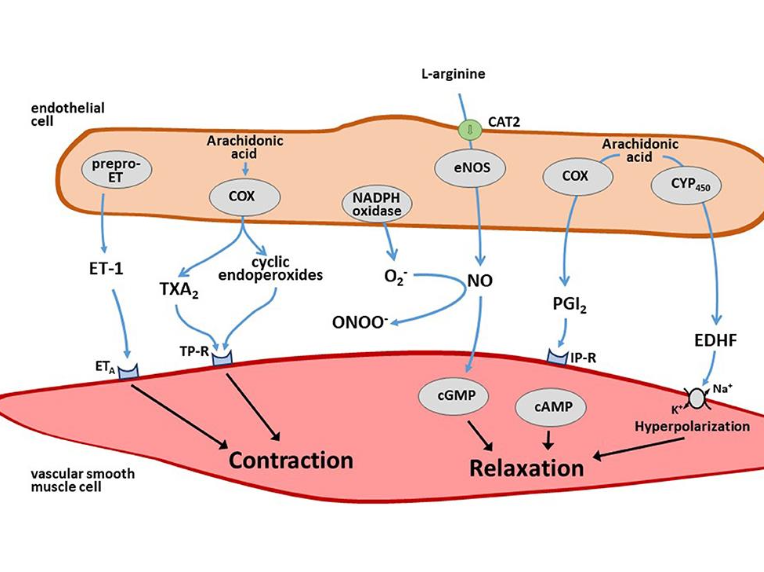
Vascular tone regulation: Responds to hormones and factors (e.g., NO, Prostacyclin, Thromboxane A2)
ECs control vascular tone by responding to various hormones,
neurotransmitters and vasoactive factors
Vasodilatory factors
• Nitric Oxide (NO)
• Prostacyclin (PGI2)
• Endothelium derived hyperpolarizing factor (EDHF)
Vasoconstrictive factors
• Thromboxane A2 (TXA2)
• Endothelin-1 (ET-1)
• Catecholamines and others
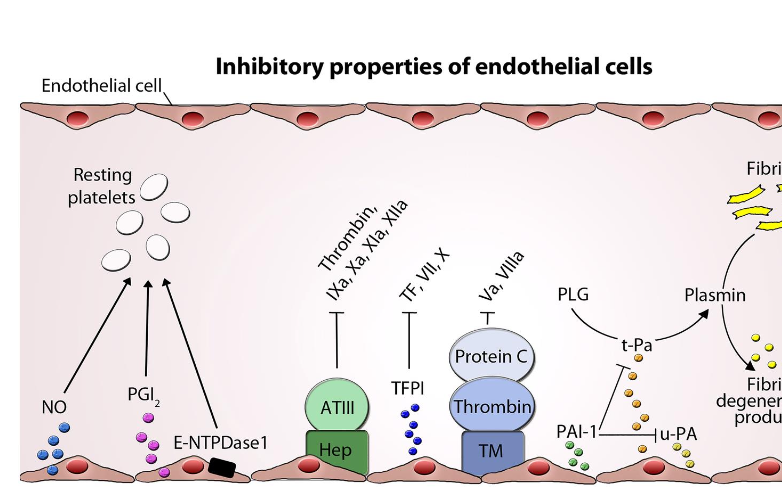
Involved in coagulation processes: produces activators and inhibitors of thrombosis
Anticoagulants (inhibit coagulation)
• Thrombomodulin/Protein C
• Sequesters ATIII on HS
• ATPase/ADPase (CD39)
• TFPI
• PAI-1
Anti-platelets (inhibit platelets)
• Nitric Oxide (NO)
• PGI2
Factors to break down fibrin
• tPA activates plasmin
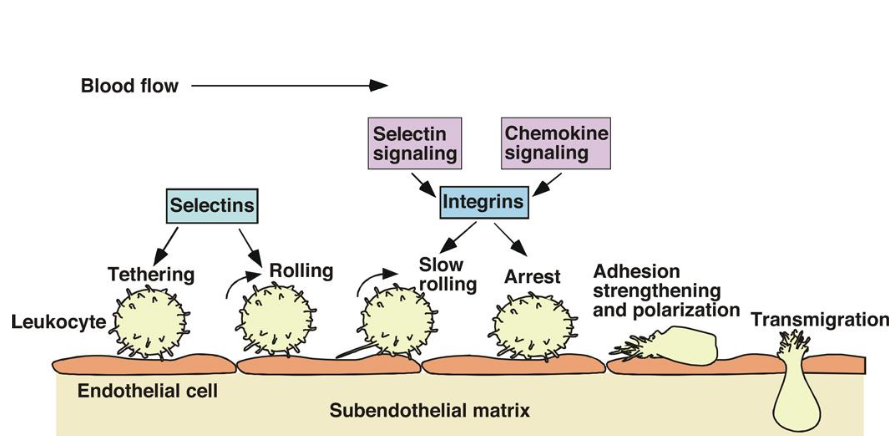
Inflammation regulation: Leukocyte adhesion and migration mediated through endothelial interactions
Leukocytes can attach an roll on the endothelium, particularly when the endothelium is inflamed/injured.
• Tethering and rolling = selectins
• Slow rolling and arrest = integrins
• Leukocytes transmigrate into the surrounding tissue.
Mechanotransduction in Endothelial Cells
Physical forces create biochemical responses through changes in cell membrane and cytoskeleton
1. Physical Force
1. ECM, Glycocalyx
2. Tight junctions, Ion channels
2. Receptor/protein conformational change/activation
3. Protein phosphorylation
4. Cytoskeletal rearrangement
5. Activation of signalling molecules
6. Changes in transcription
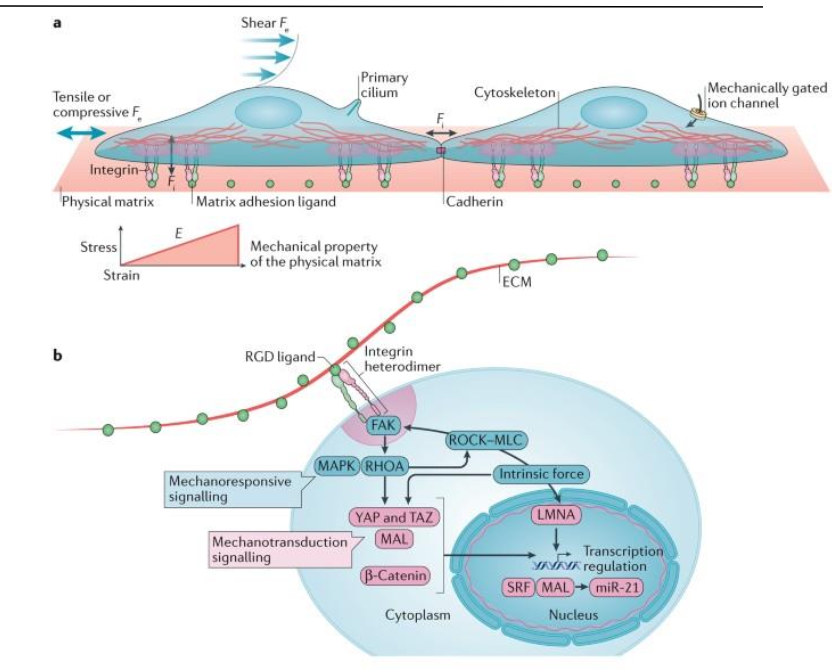
Glycocalyx and transmembrane proteins play roles in sensing mechanical stimuli
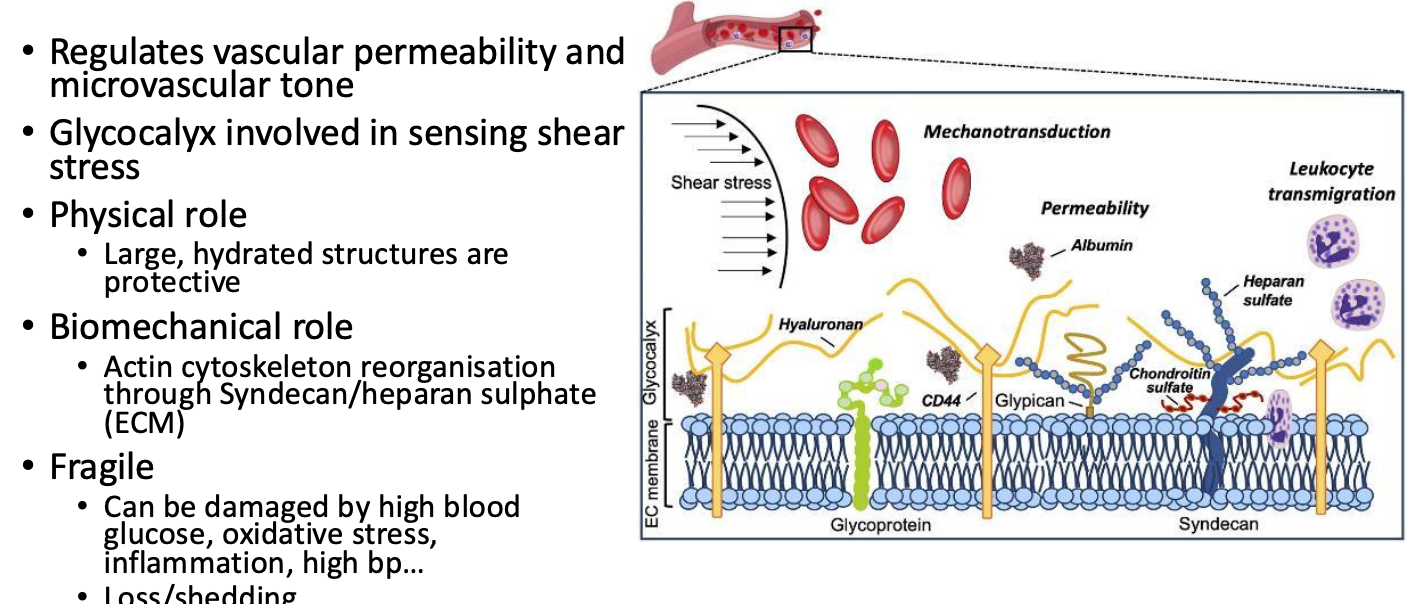
Barrier Function
Maintains barrier function through specific proteins:
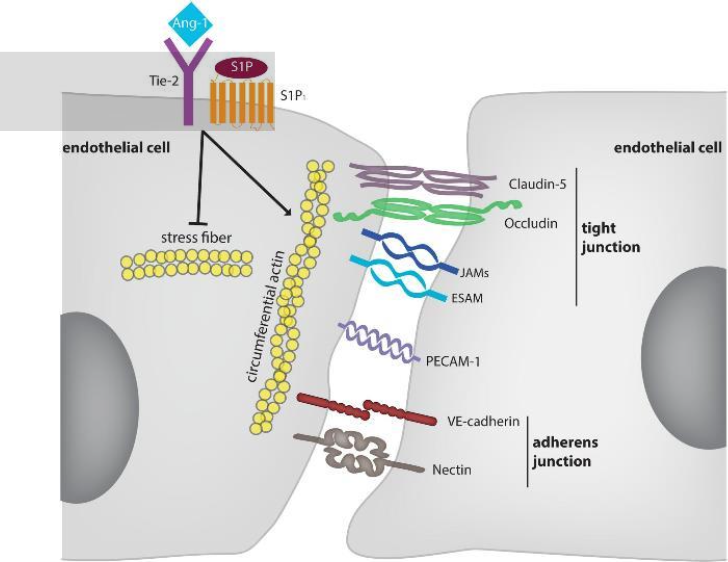
Endothelial specific tight junctions:
Claudin-5
Occludin (linked to cytoskeleton)
JAM
ZO (not on image)
Adherens junctions
VE-Cadherin
Nectin (evidence only in vitro)
Not on image:
Connexins (gap junction proteins)
Other receptors:
Tie-2 and S1P1 indirectly stabilize
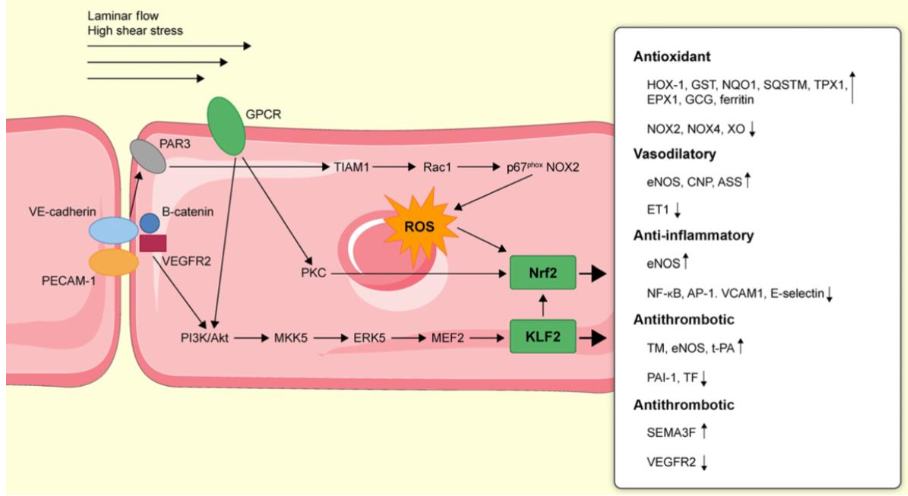
Shear Sensing by the Endothelium
Mechanosensory complex/Mechanosome:
VE-cadherin, VEGFR2 and platelet EC adhesion molecule (PECAM-1 aka CD31)
Shear stress causes conformational changes in PECAM-1
VE-cadherin acts as a mechanoadaptor to transmit signal to VEGFR2
VEGFR2 activates PI3K/Akt
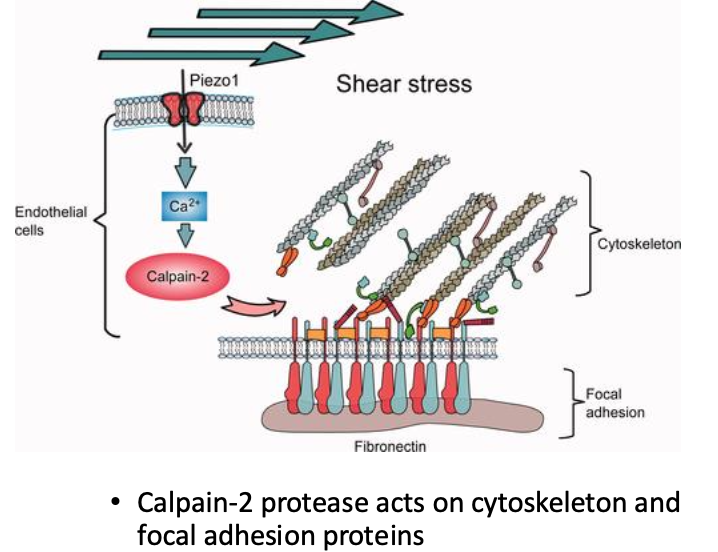
Shear and Pressure Sensing by the Endothelium
Piezo1 is also located on endothelial cell membranes
Ion channel that mediates Ca influx
Multiple roles identified so far:
Required for vascular development
Causes polarisation of ECs in direction of flow
Involved in blood pressure regulation
Regulates endothelial barrier function in the lungs…
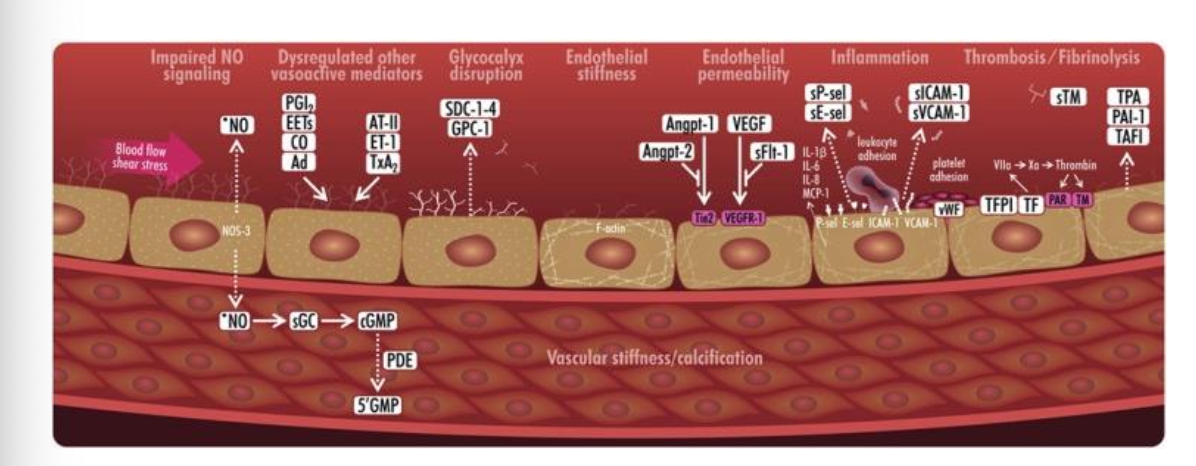
Endothelial Dysfunction
Causes: Oxidative stress, hypertension, inflammation, unhealthy lifestyles
Effects: Impaired NO signaling, increased permeability, thrombosis, linked to atherothrombosis
Can lead to pathologies affecting multiple organ systems
Conclusion
Glycocalyx: Key role in signaling and maintaining barrier function; adaptations can lead to pathology
Upcoming topics: Smooth Muscle Cells
Ends with an invitation for questions.