Module 12 Book Notes
NOTE: not complete read through chapter/pages assigned!
Enterobacteria general characteristics
gramn-egative bacilli and coccobacilli.
they do not produce cytochrome oxidase except for Plesiomonas
they all ferment glucose
they reduce nitrate to nitrite except for Photorhabdus and Xenorhabdus
they are motile at body temperatures except for Klebsiella, Shigella, and Yersinia
except for Klebsiella, Proteus, and some Enterobacter isolates, none has remarkable colony morphology on laboratory media
they appear large, moist, and gray on sheep blood agar (SBA), chocolate (CHOC) agar, and most nonselective media
microscopic and colony morphology
gram-negative, non-spore forming, facultative anaerobes, bacilli
may appear coccobacilli or as straight rods
no value in using SBA or chocolate agar for ID (except Klebsiella)
many E. coli isolates are B-hemolytic
best to use methylene blue, MAC agar, and highly selective media for culturing
Hektoen enteric (HE)
xylose-lysine-desoxycholate (XLD)
positive result indicated by color change in agar due to fermentation of present carbohydrate
can also distinguish species that produce hydrogen sulfide (H2S)
classification
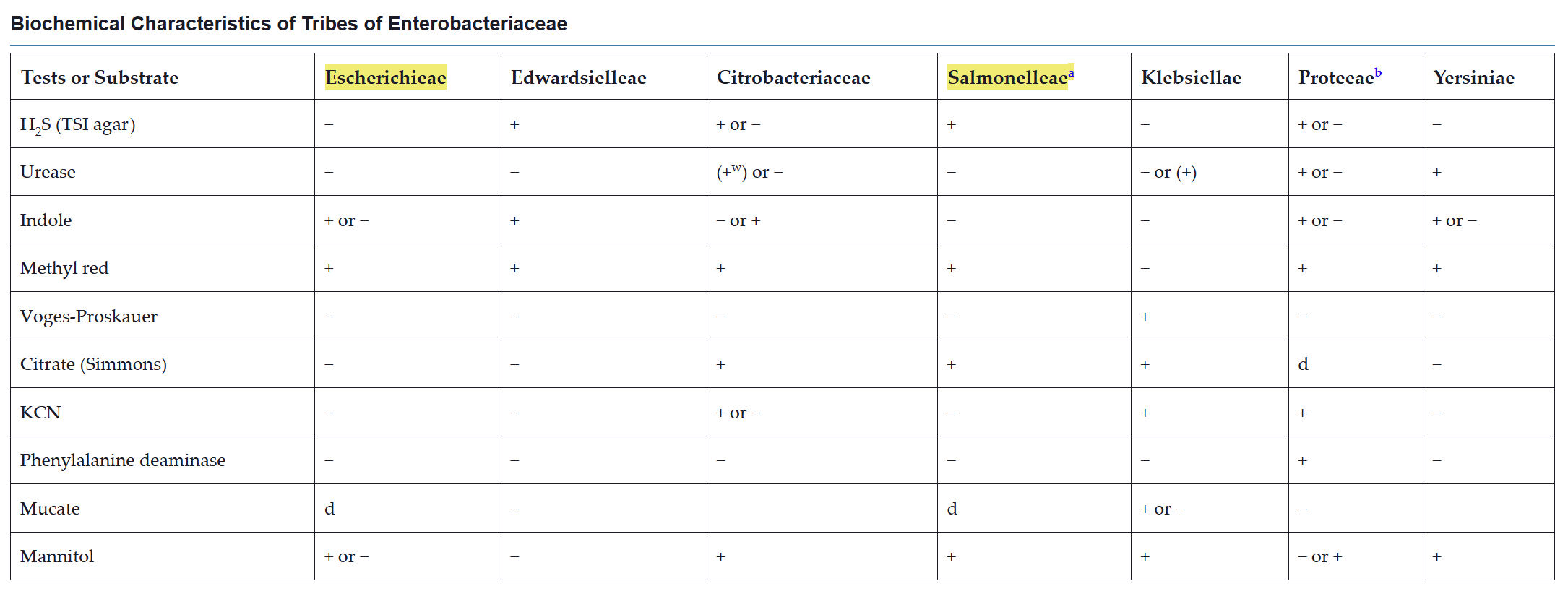
virulence and antigenic factors
O antigen (somatic antigen) — heat-stable antigen located on the cell wall
H antigen (flagellar antigen) — heat-labile antigen on the surface of flagella
K antigen (capsular antigen) — heat-labile polysaccharide found in some encapsulated species
clinical significance
ubiquitous in nature
reservoir: GI tract; some live in water, soil or sewage; plant pathogens
opportunistic pathogens
part of usual intestinal flora in humans and animals
harmful when moved to another body site
primary pathogen
bacteria introduced from environment to host by contaminated soil or water; also devastating in the immunocompromised
antimicrobial resistance
three categories - urgent, serious, concerning
carbapenemresistant Enterobacteriaceae (CRE) prevalent in clinical settings
resistance to imipenem, meropenem, doripenem, or ertapenem, or documentation that the isolate possesses a carbapenemase
plasmid-transmittable colistin marker mcr-1
allows pathogen to exhibit more resistance to a variety of antibiotics
Escherichia coli as an opportunistic pathogen
can cause UTI’s diarrheal diseases, central nervous system infections, bacteriuria, septicemia, neonatal sepsis, and meningitis
most strains are motile and have adhesive fimbriae and sex pili
they may also have O, H, and K antigens
colony morphology on selective and differential media, like MAC or EMB agar
lactose-positive (pink) with surrounding precipitated bile salts on MAC agar
green metallic sheen on EMB agar
general associations of E. coli
Fermentation of glucose, lactose, trehalose, and xylose
Production of indole from tryptophan
Glucose fermentation by the mixed acid pathway: methyl red positive and Voges-Proskauer negative
Does not produce H2S, deoxyribonuclease (DNase), urease, or phenylalanine deaminase
Cannot use citrate as a sole carbon source
uropathogenic E. coli
cause of UTI’s from indigenous biota in the large intestine
virulence factors present that allow them to attach to urinary epithelial mucosa by the use of pili
cytolysins & aerobactins also contribute
cytolysins kill immune effector cells and inhibit phagocytosis & chemotaxis of certain WBC
aerobactin allows the bacterial cell to chelate iron; free iron is generally unavailable within the host for use by bacteria
can also cause acute pyelonephritis
gastrointestinal pathogens
five major categories of diarrheagenic E. coli
enterotoxigenic Escherichia coli (ETEC)
enteroinvasive Escherichia coli (EIEC)
enteropathogenic Escherichia coli (EPEC)
enterohemorrhagic Escherichia coli (EHEC)
enteroadherent
includes: enteroaggregative Escherichia coli (EAEC) and diffusely adherent Escherichia coli (DAEC)
enterotoxigenic Escherichia coli
ETEC strains that cause traveler’s diarrhea which is spread by contaminated food or water
self-limiting; symptoms experienced are watery diarrhea, abdominal cramps, and sometimes nausea, usually with no vomiting or fever
transmission of disease by poor hygiene, reduced availability of potable water sources, and inadequate sanitation
stomach acidity as a protective mechanism to inhibit colonization and initiation of disease
high infective dose — 106-1010 required
ETEC strains can produced one or both of two toxins into the small intestine
a heat-labile toxin (LT) ~ similar in action and amino acid sequence to cholera toxin
AB toxin in which B subunit facilitates entry into cell & A subunit activates cellular adenylate cyclase (increase in cAMP)
this results in hypersecretion of electrolytes and fluids into the intestinal lumen
a heat-stable toxin (ST) ~ stimulates guanylate cyclase and results in cGMP abundance which causes hypersecretion