Gastrointestinal System
Overview of Gastrointestinal Tract
Mouth: chewing and hydrolysis (enzymatic breakdown) =bolus
Esophagus: propels bolus
Stomach: churning + hydrolysis + storage = chyme
Small intestine: hydrolysis + absorption
Large intestine (colon): absorption (of ions, water, vitamin K, not nutrients)
Rectum: storage of processed food until we expel it
Anus: expulsion
Mouth (oral/buccal cavity)
Goal of the mouth is to convert food into bolus, which we do in 2 steps:
Mastication (chewing)- accomplished by teeth and tongue
tongue is made of extrinsic and intrinsic muscles
extrinsic: causes elevation, depression, protrusion, and retraction
intrinsic: (inside the tongue) shorten and widen, and lengthen and narrow
Break down of food particles by hydrolysis. The enzymes in our mouth that do this come from glands
Glands release serous content (for enzyme breakdown/and cut food by hydrolysis) and mucinous content (wet the food so its easier to make bolus)
Parotid glands: serous, release 25% of saliva content, release alpha amylase
Submandibular: mostly serous, release 70% of saliva, releases alpha amylase
Sublingual gland: mainly mucin, release 5% of saliva, releases alpha amylase
Von Ebner gland: tip of tongue, serous, 5% of saliva
also breaks down triglycerides with lingual lipase into free fatty acids, diglycerides, and monoglycerides
Alpha amylase breaks down starches into smaller cards
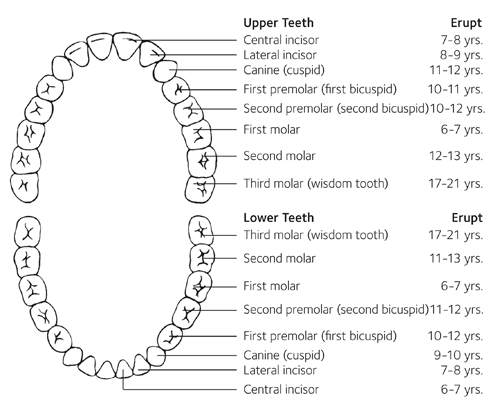
Teeth
Mandible: lower jaw
Maxilla: upper jaw
There is symmetry on both left and right sides as well as between mandible and maxilla
28% of people have:
4 central incisors, 4 lateral incisors, 8 premolars, and 12 molar teeth
72% have the third molars (wisdom teeth) removed due to inadequate space within the mouth which can lead to tearing and inflammation within the gums (becomes impacted)
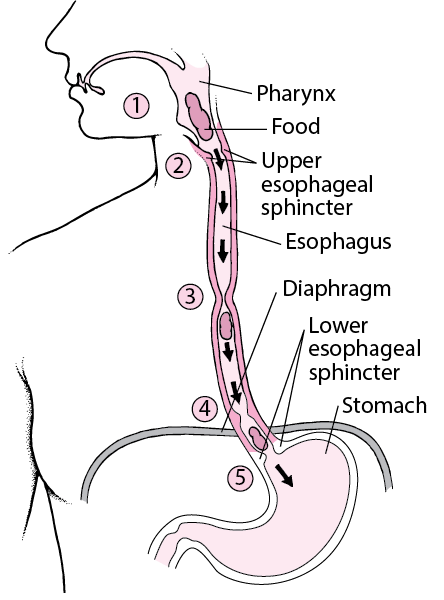
Esophagus
There are sphincters- circular localizations of muscle- at the very top and very bottom of the esophagus. These keep food moving in one direction
Upper esophageal sphincter: voluntary, made of skeletal muscle
Lower esophageal sphincter: its actually the diaphragm, looks like a sheet of muscle between the thoracic cavity and the abdominal cavity and helps lungs expand and breathe
forms a ring around the base of the esophagus and holds it in place
over time, humans can get a hernia where the esophagus moves up through the diaphragm and causes acid reflux
Works as a passageway for food and doesn’t do much except for peristalsis
Muscle-makeup is split into thirds:
top third: all skeletal muscle, voluntary control
middle third: combination of skeletal and smooth
bottom third: all smooth muscle, involuntary control
Stomach
Stomach is responsible for 3 steps:
receives bolus of food
churns bolus/breaks down food even more
hydrolysis (enzyme assisted breakdown) of bolus
The end product is chyme, which sits there for a little bit (stomach stores up to 4L of food at a time) before moving on to the small intestine
Stomach is lined with many infoldings (rugae) of the gastral wall that help increase surface area. The folds are lined with gastric glands and goblet cells:
Gastrin hormone causes the secretion of HCl, pepsinogen and increases stomach motility
Goblet cells: found along the entire GI tract and secretes mucus
Mucus in the stomach protects the stomach wall from pepsin and HCl
Gastric glands
Parietal cells: release HCl (pH of stomach is about 2)
Chief cells: release pepsinogen (turns/activates into pepsin due to HCl presence)
pepsin breaks down proteins by cleaving peptide bonds, thus protein is the only type of molecule to be broken down in the stomach
Pepsinogen is a type of zymogen (inactive forms that are activated by proteolytic cleavage by another enzyme) BUT PEPSINOGEN AUTCLEAVAGES ITSELF BY ACIDIC PROTEOLYSIS
Small intestine
Chyme enters the small intestine by the pyloric sphincter
stomach emptying can be inhibited if the small intestine is already full or if there is excess acidity, which is mediated by nerves and the hormone cholecystokinin, secreted by epithelial cells into the bloodstream to causes pancreatic bicarbonate (high pH) and water secretion to adjust pH
The small intestine is divided into 3 segments:
Duodenum: receives chyme from the stomach. Most of the digestion occurs here
Jejunum: most absorption happens here
Ileum: absorbs important things like vitamins
Duodenum is very with with four key processes:
receives chyme and HCl from the stomach
liver and gallbladder send bile to the duodenum
pancreas also delivers some important enzymes
the duodenum itself has brush border enzymes, which are important for absorption and for enzyme activity
brush border are in-foldings on the wall of the duodenum called villi
each villus is even more in-foldings, microscopic projections called microvilli
all these increase surface area for absorption and digestions, because the projections have enzymes
Digestion in the Duodenum
Protein is broken down by several enzymes in the small intestine into constituent amino acids
peptidase is found on the brush border
the pancreas sends trypsinogen and chymotrypsinogen, which an enzyme called enteropeptidase turn into their active forms of trypsin and chymotrypsin
Carbohydrates are broken down by amylase and lactidase (can only break apart lactose, found on brush border)
when you have a stomach bug it can inflame the duodenum and actually knock off some of the lactidase enzymes, thus you become temporarily lactose intolerant
eventually left with monosaccharides
Nucleotides are broken down by nucleosidases on the brush boarder which cleave the base-pentose bond
Fat is broken down by lipase, released by the pancreas and cleaves the triglycerides into glycerol and 3 fatty acids
bile released by the liver/gallbladder to organize the fatty acids
Absorption (Mostly in Jejunum)
After digestion, monomers are present (A.A’s, monosaccharides, nucleobases, fatty acids, etc.)
Amino acids are funneled into intestinal cells with primary active transport (uses ATP) and eventually enters a blood capillary
Sugar monosaccharides are funneled into and eventually out of the intestinal cells with secondary active transport (uses ion like sodium to flow down the concentration gradient to enter or exit to allow the monosaccharide to go the opposite direction)
P-pentose and nitrogenous base also enter/exit the cell with primary active transport and end up in the blood capillary
Fatty acids can just diffuse across the membrane into the enterocyte (intestinal cell) where they are organized into chylomicrons which are absorbed into the lymphatic capillary (lacteal) where they are further digested into smaller bits and then get into the veins and blood capillaries
Liver
Responsible for 4 main things:
metabolism- involves catabolism and anabolism
storage
carbs are stored a glycogen and cats can be stored as lipoprotein and triglycerides
protein aren’t stored but are turn into molecules like albumin which can be sent into the blood stream until they’re needed and retrieved back to the liver
detoxification- achieved mainly by cytochrome P450
can take many different kinds of substrates and react with them
causes a problem when we take medications because it decreases drug efficacy
bile production- needed for fat absorption
The liver has two separate blood supplies going to it, and one that leaves it. These vessels make up the portal triad
the portal vein supplies the liver with nutrient rich blood (nutrients absorbed in the intestinal tract which go through circulation and end up in the portal vein (turns excess nitrogen from proteins into urea)
proper hepatic artery supplies liver with arteriole, oxygen rich blood
hepatic vein carries away nutrient and oxygen poor blood
this blood then travels to the heart to be oxygenated, goes past the intestines to gain nutrients, then re-enters liver through portal vein
The other output from the liver is bile, which leaves through the common hepatic duct
Hepatic lobule
The portal triad is important to identify in surgery, and easy to identify when we look at pieces of the liver called hepatic lobules
in the hepatic lobule, there are many liver cells or hepatocytes, and around them are three distinct branches that make up the portal triad. There are actually bunches of portal triads surrounding hepatocytes- this leads to 6 distinct sides of the hepatic lobule
the portal vein is how we get nutrient rich blood to enter the hepatic lobule (portal vein branches are call sinusoids) where hepatocytes then break those nutrients down for storage or whatever is needed. The proper hepatic artery beings in oxygen to the hepatic lobule.
once those have been extracted, the blood collects in the center of the hepatic lobule into the central vein which then becomes the hepatic vein, which sends the blood back to the heart and intestines
Biliary tree
Bile is composed of bile pigments and bile salts (helpts emulsify fat into micelles, which can be absorbed in the ilium)
Bile thats made in the live travels through the common hepatic duct into the cystic duct which leads to temporary storage in the gallbladder
gallbladder is used to store bile, its the organ’s only focus
Cholecystokinin (CCK) is a hormone that causes bile to be released from the gallbladder though the organ contracting and squeezing the bile into the cystic duct to go to the common bile duct
the common bile duct then goes to the duodenum where the bile is released and fats are emulsified
bile salts are then absorbed by the ileum to circulate back to the liver to repeat the process
Exocrine Pancreas
The pancreas sits below and behind the stomach, and sort of hugs the duodenum of the small intestine
some say its in a different part of the body, the retroperitoneum (along with some big blood vessels) and not in the peritoneum (where the abdominal cavity rests)
The pancreas releases powerful enzymes that digest lots of macromolecules. Its also unique cause it’s un-encapsulated. (its just a slurry of cells, which is difficult especially for surgeons operating nearby)
Many consider the pancreas to the the ‘lion’ of the abdomen because of its importance and power
There are two main components to the pancreas:
the exocrine pancreas: takes salts an enzymes and releases them in the duodenum
the endocrine pancreas: releases hormones
The exocrine pancreas releases four main things:
Bicarbonate: neutralizes gastric acid (HCl with chyme from the stomach)
Amylase: breaks down starch into monosaccharides
Lipase: breaks down triglycerides into free FAs, monoglycerides, diglycerides, and glycerol
Proteolytic enzymes: includes trypsinogen and chymotrypsinogen
Trypsinogen is turn into its active form typsin by anteropeptidase enzyme in the duodenum and then chymotryspinogen is turned into its active form chymotrypsin by trypsin
if trypsinogen ends up turning into trypsin while in the pancreas… it would travel around and digest all sorts of proteins (in membranes, food, organs, not good)
The endocrine pancreas is more famous: it releases hormones rather than enzymes and salts. Those enzymes enter the bloodstream and move all over the body
The endocrine pancreas is composed of many islet cells that sit in “islands”
3 main types of islet cells:
alpha islet cells: release glucagon (breaks molecules, turns glycogen into glucose)
beta islet cells: release insulin (stores molecules, turns glucose into glycogen)
Also the hormone responsible for diabetes “eye, nerve, and kidney disease” , which is caused by too much glucose in the body because insulin isn’t working
Type 1: no insulin
Type 2: insulin receptors are broken
delta islet cells: release somatostatin (stops the effect of other hormones in GI tract)
Colon, Rectum, and Anus
After foot is absorbed in the small intestine, it travels to the large intestine (larger in diameter but shorter in length)
At the end of the small intestine/beginning of the large intestine is the ileocecal valve
The first main part of the large intestine is the cecum (with the appendix tail hanging off), then the ascending colon, transverse colon, and the descending colon. The last part of the large intestine is the sigmoid colon (has an S shape to it)
The large intestine is most responsible for absorbing:
Water
absorb too much water=constipation
absorb too little water= diarrhea
The disease cholera attacks certain proteins/receptors in the intestinal lining that cause tremendous fluid loss and eventually leads to death by dehydration
keeping a person very hydrated through the whole disease manifestation will lead them to eventually passing the bacteria and being okay
Inorganic Ions- potassium and sodium
absorbed through transport mechanisms like the kidney
inorganic ion absorption is more important in the kidneys, so you’ll be okay with you have a colonectomy in terms of ion absorption
The large intestine is also home to lots of micro-organisms that assist in digestion of things like carbs, making byproducts of methane, and dihydrogen sulfide
Rectum is after the sigmoid colon and it’s main function is storage- it holds onto stool until it is excreted
The anus is composed of 2 sphincters:
internal anal sphincter: smooth muscle, involuntary
external anal sphincter: skeletal muscle, voluntary
The internal anal sphincter releases to allow stool to move to allow us to know it is time for defecation. Defecation occurs once external sphincter opens
Hormonal Control of Appetite
When the stomach is empty, gastric cells produce the hormone ghrelin to stimulate appetite.
When the colon is full, the jejunum produces peptide YY to reduce appetite
The hormone leptin, produced by white adipose tissue is an appetite suppressant that acts as an ‘adipostat’ (maintains stable lipid content in the adipose tissue)
Leptin is secreted in response to increased triglyceride levels and works to suppress appetite until appropriate levels are store
Leptin is a focus on obesity research, in humans obesity is often associated with high levels of leptin but a lack of appetite suppression, which suggests the hypothalamus has become resistant to leptin due to down-regulation of receptors