Gas Exchange
Introduction to Gas Exchange
Importance of gas exchange in the respiratory system.
Overview of learning objectives:
Components of respiratory membrane.
Mechanisms of gas exchange and transport in the body.
Structure of Alveoli
Alveoli as the final air-holding structures in the lungs.
There are approximately 300-500 million alveoli in human lungs, shaped like cups.
Diagram Recap: Shows journey from terminal bronchioles to respiratory bronchioles to alveolar ducts, leading to alveolar sacs filled with alveoli.
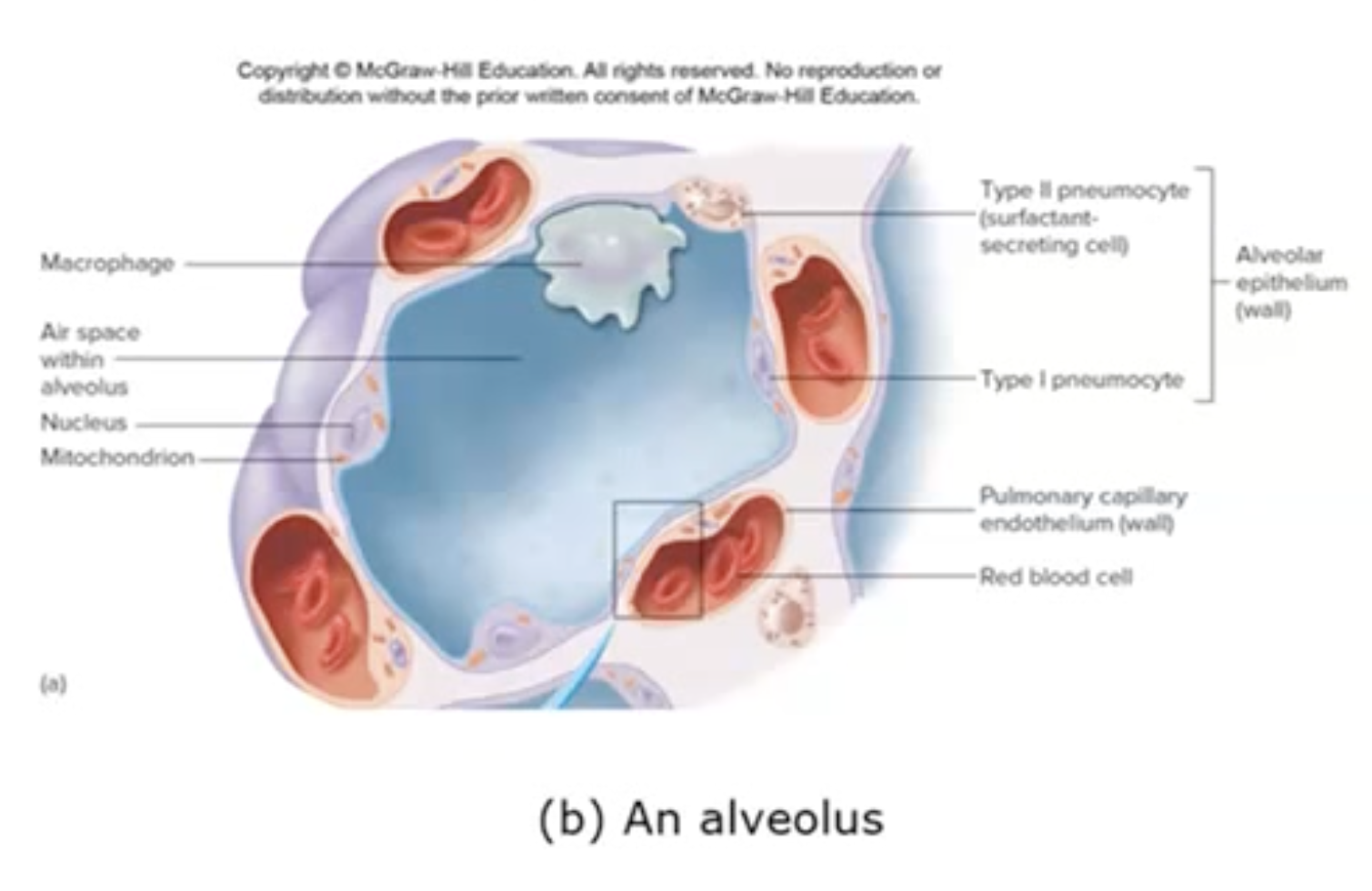
Alveolar Structure
Alveoli are surrounded by a dense capillary network.
Cell Types in Alveoli:
Type I Pneumocytes: Simple squamous epithelium that primarily facilitate gas exchange.
Type II Pneumocytes: Simple cuboidal cells that secrete alveolar fluid and surfactant.
Function of Surfactant: Reduces surface tension in alveolar fluid, preventing alveolar collapse.
Macrophages (Dust Cells): Patrol alveoli to remove dust and debris, as cilia are absent here.
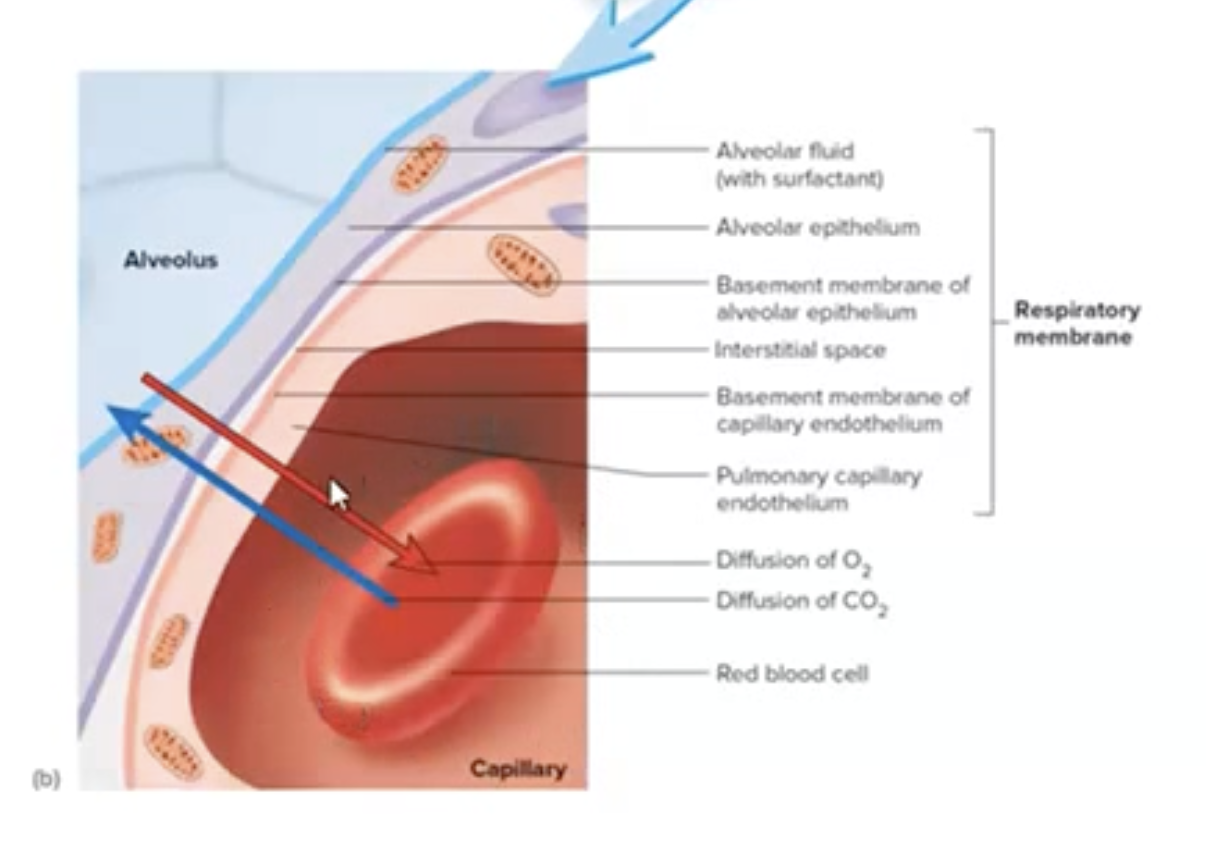
Respiratory Membrane
Characteristics:
Extremely thin (approximately 0.5 micrometers), allowing efficient gas exchange.
Components of the Respiratory Membrane:
Alveolar epithelium (simple squamous).
Capillary endothelium (also simple squamous).
Common basement membrane between these two.
Importance of Thickness:
Thicker membranes lead to poorer gas exchange; thickness in healthy humans is about 0.5-1 micrometre. This minimal thickness facilitates the rapid diffusion of oxygen and carbon dioxide, ensuring efficient gas exchange in the alveoli. s.
Factors Affecting Gas Exchange
**Surface Area:
Greater surface area increases gas exchange efficiency. **
Diffusion Coefficient: how easily a gas can diffuse in and out
Different gases have varying ease of diffusion:
Oxygen: Diffusion coefficient of 4 (in lungs).
Carbon dioxide: Diffusion coefficient of 20 (in lungs), indicating faster diffusion compared to oxygen.
Partial Pressure Gradient: pressure exerted by each gas in a mixture of gases
Gases move from areas of higher partial pressure to lower partial pressure.
Example:
Oxygen moves from high in the alveoli to low in deoxygenated blood.
Moist Membranes:
Gases must dissolve in a liquid to diffuse; alveolar fluid and blood plasma provide this fluid environment.
Gas Transport in the Body
Oxygen transport:
98.5% bound to hemoglobin; 1.5% dissolved in plasma due to low solubility.
Carbon dioxide transport:
70% as bicarbonate ions in plasma; 23% bound to hemoglobin; 7% dissolved in plasma.
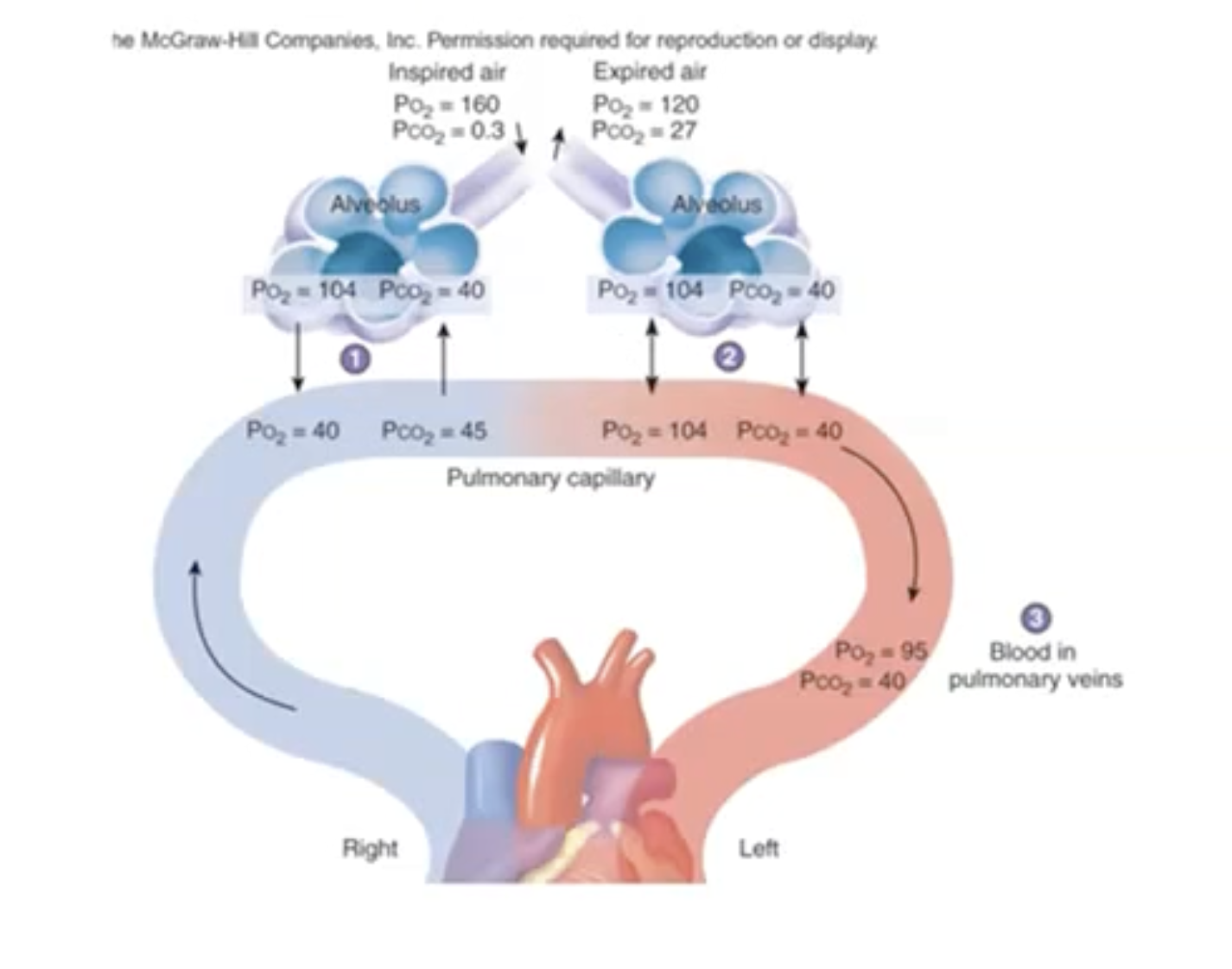
External vs Internal Respiration
External Respiration: Gas exchange between alveoli and blood.
Oxygen moves from alveoli (high PO2) to blood (low PO2).
Carbon dioxide moves from blood (high PCO2) to alveoli (low PCO2).
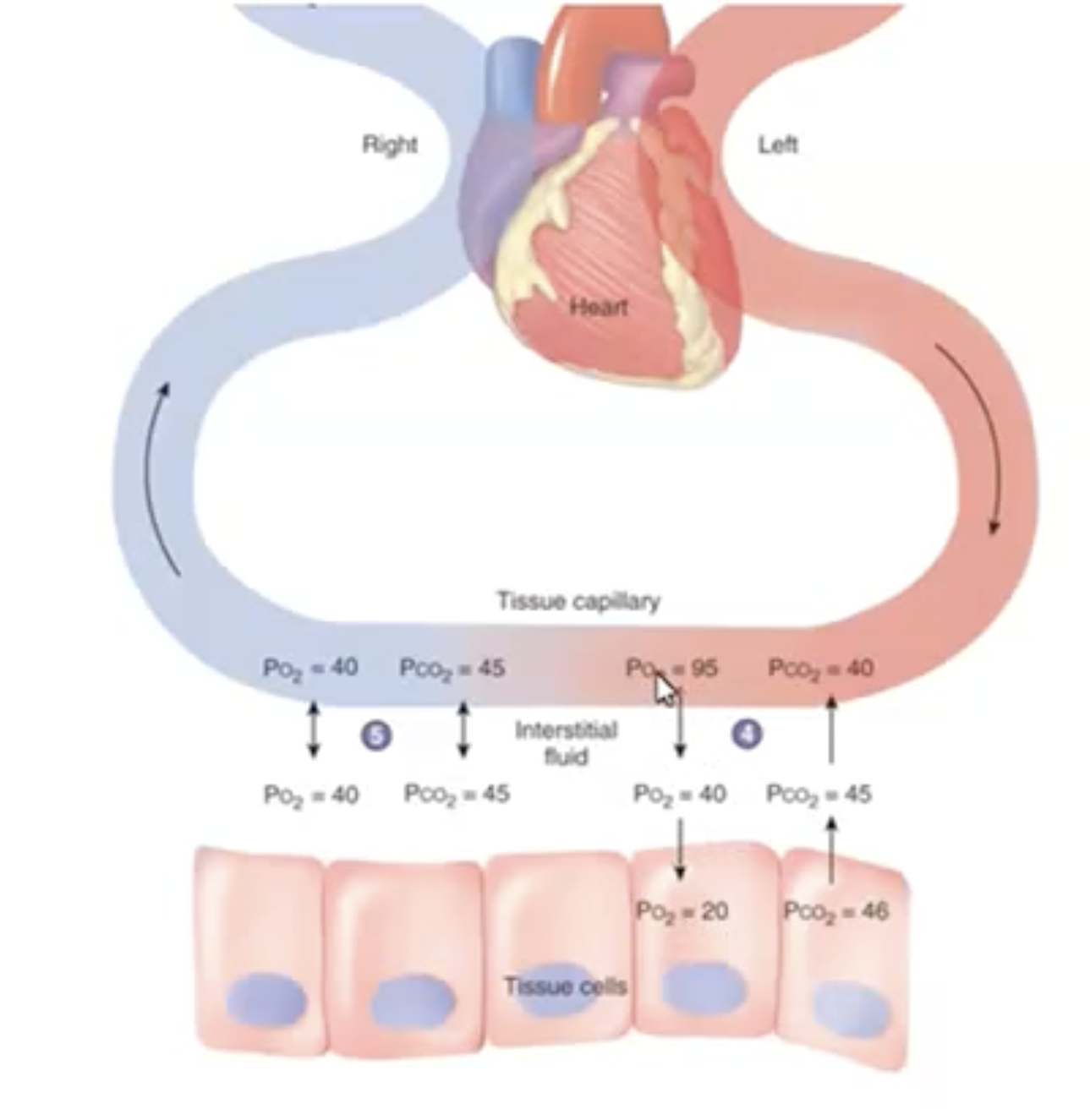
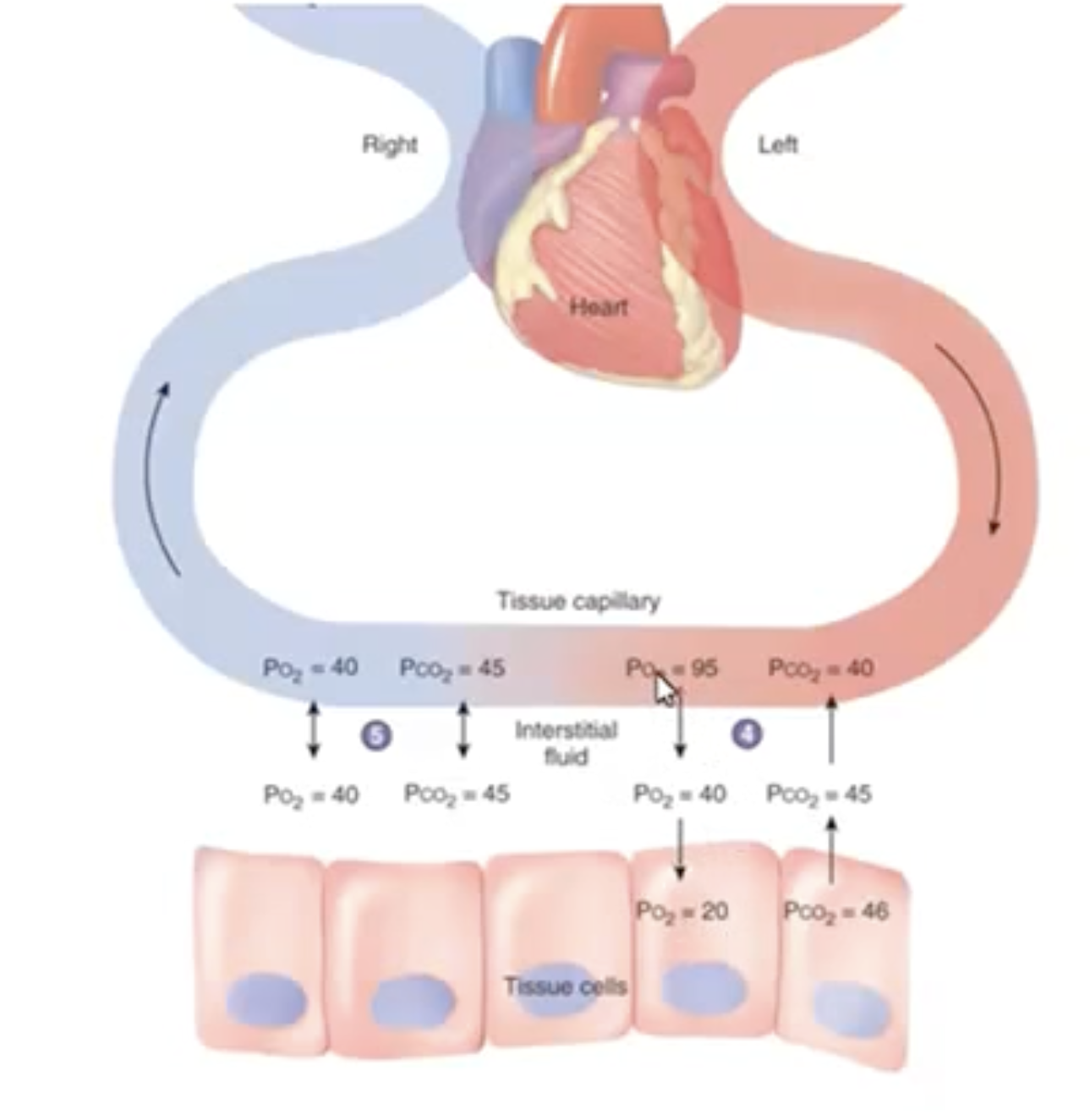
Internal Respiration: Gas exchange between blood and tissues.
Oxygen moves from blood (high PO2) to tissues (low PO2).
Carbon dioxide moves from tissues (high PCO2) to blood (low PCO2).
Pulmonary Ventilation
Overview of partial pressure changes during various stages of respiration.
Humidification of Air: Alters partial pressures when air enters the lungs.
Example of Partial Pressures:
Inhalation: Oxygen from 60 mmHg to 104 mmHg; CO2 from 0.3 mmHg to 40 mmHg.
Summary of Gas Exchange
**Process Overview: **
Inhaling air —>> external respiration (between alveoli and pulmonary capillaries) —>> gas transport via blood —>> internal respiration (between blood and tissues).
CO2 returns to lungs for oxygenation:
ensures continual oxygen delivery to tissues and removal of carbon dioxide.
Conclusion
Recap on how efficient gas exchange relies on:
Thin respiratory membrane, ample surface area, presence of fluid, strong diffusion gradients, and thickness control.
Questions addressed include how oxygen and carbon dioxide are exchanged in alveoli and between capillaries and tissues.
Importance of understanding respiratory mechanics for overall health and well-being.