Urinary System (15 & 16)
LO1: Explain the function of the Urinary System
LO2: Describe the macroanatomy of the Urinary System
LO3: Describe the microanatomy of the Urinary System
LO4: Identify diseases of the Urinary System
LO5: Explain glomerular filtration
LO6: Describe tubular reabsorption
LO7: Describe tubular secretion
LO8: Explain the process of excretion from the kidney
Function of the Urinary System
Renal System
Regulation of plasma ionic composition: By increasing or decreasing the excretion of specific ions in the urine (Na+, K+, Ca2+, Mg2+, Cl-, HCO3 2-and H2PO4 -, H+, and HPO4)
Regulation of plasma volume and blood pressure by controlling the rate at which water is excreted in the urine affecting total blood volume and pressure
Regulation of plasma osmolarity
Regulation of plasma hydrogen ion concentration (pH)
Removal of metabolic waste products and foreign substances from the plasma
Kidney’s
Function as endocrine hormones and secrete
Erythropoietin (which stimulates erythrocyte production by the bone marrow)
Renin (which is necessary for the production of angiotensin II, to regulate salt and water balance for long-term control of blood pressure)
The activation of vitamin D3 to regulate blood calcium and phosphate levels
Gluconeogenesis
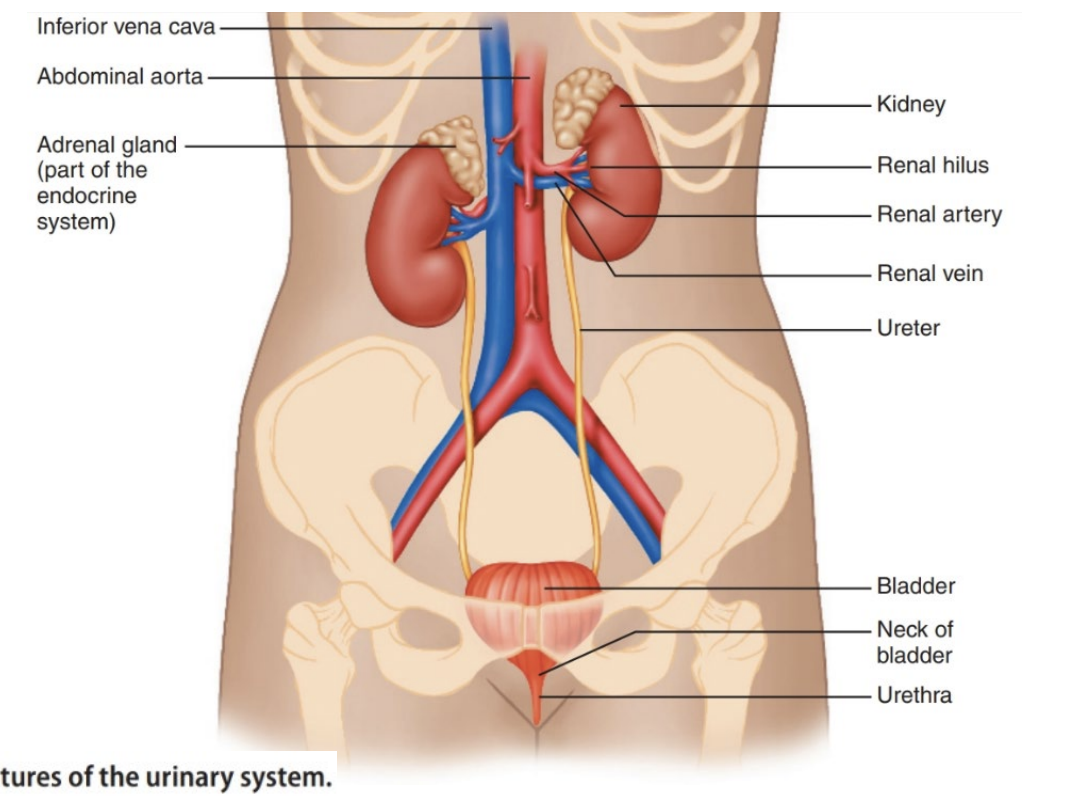
Describe the macroanatomy of the Urinary System
The Kidney’s
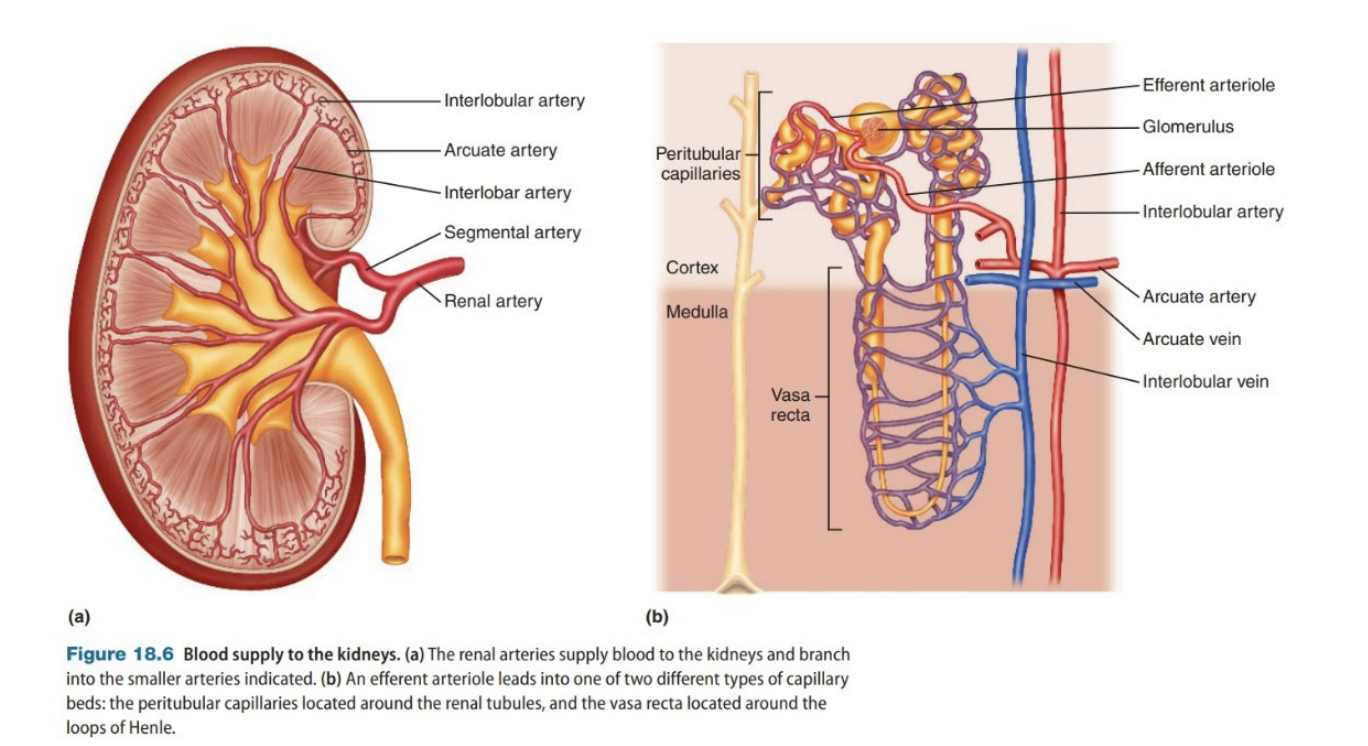
Blood Supply of the Kidney’s
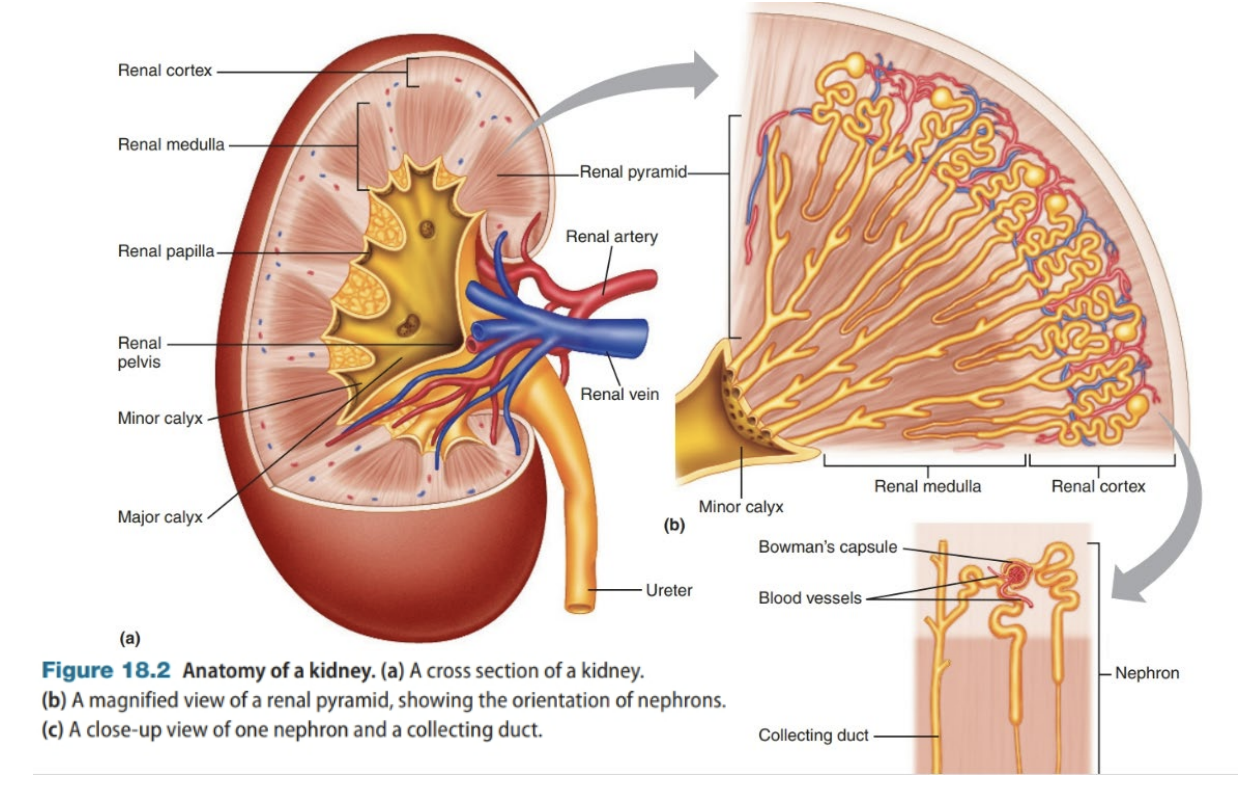
Describe the microanatomy of the Urinary System
Structure of a Nephron
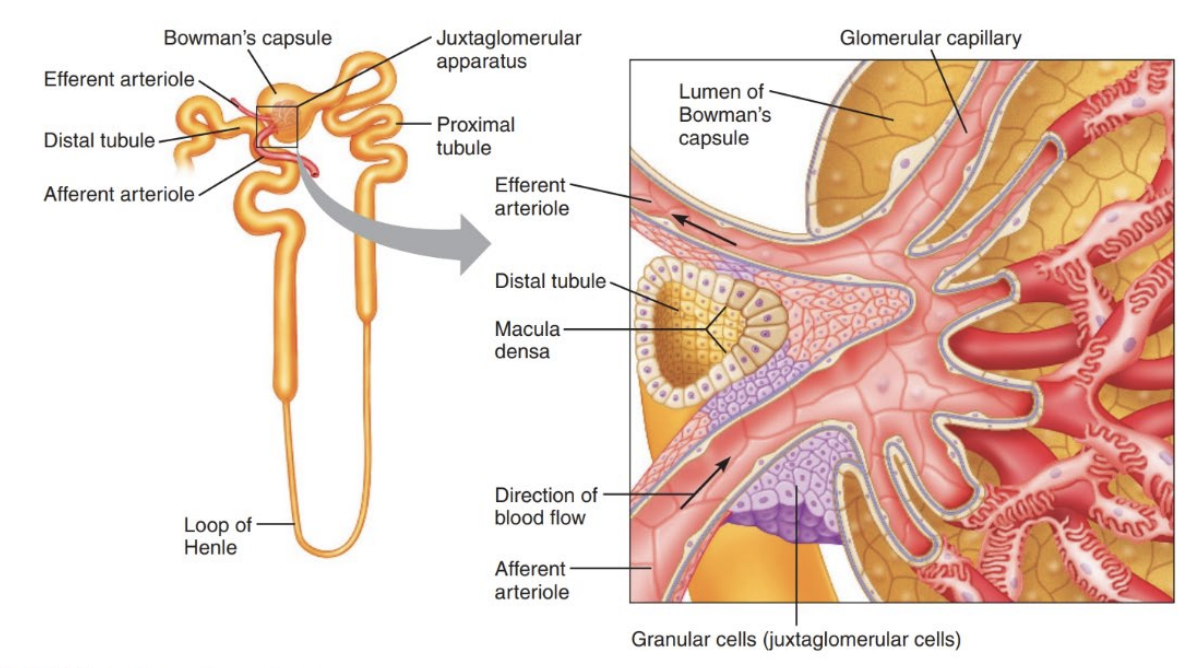
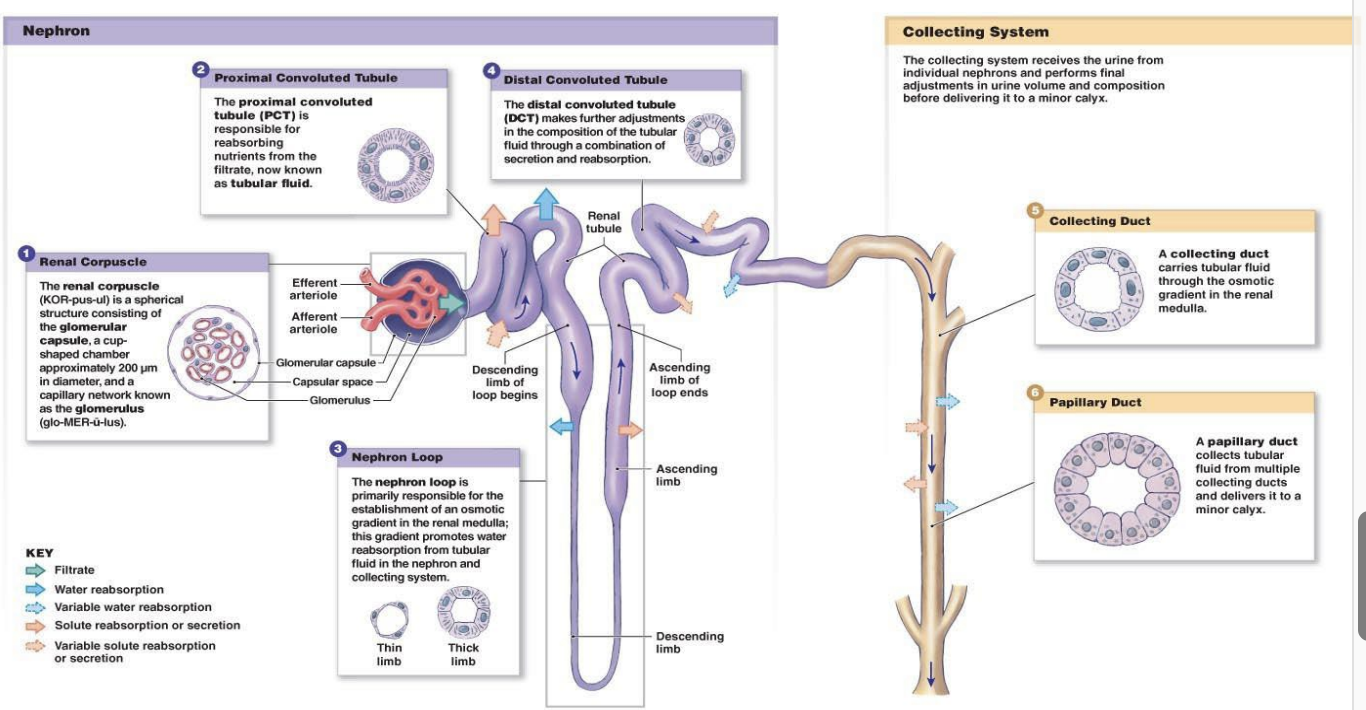
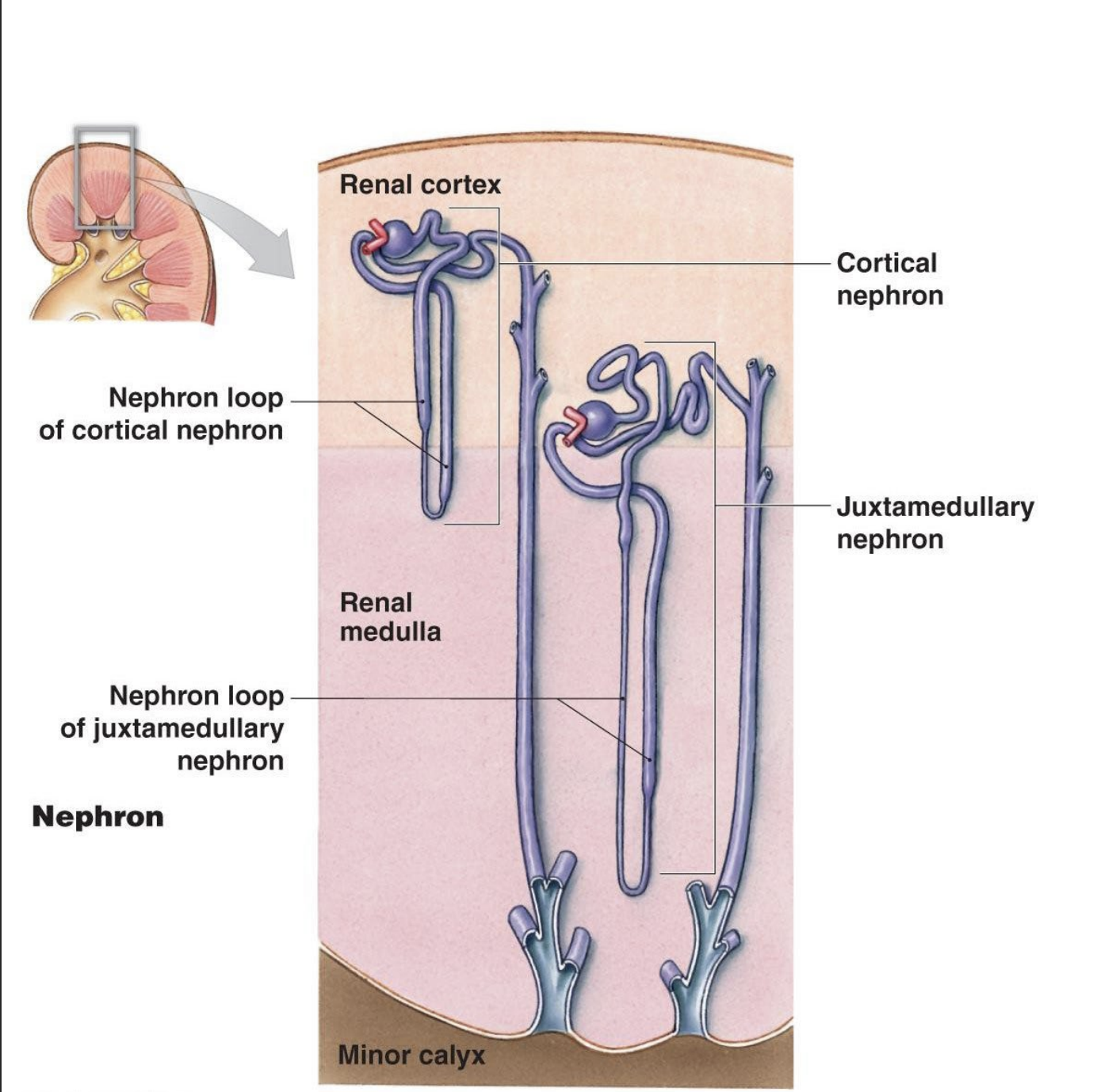
Types of Nephrons
Cortical nephrons
85%
Renal corpuscles in the outer part of the cortex.
Short loop of Henle extending into outer medulla.
Juxtamedullary nephrons
15%
Renal corpuscle in the proximity of the base of the renal pyramid.
Long loops of Henle, extending deep into the inner region of the pyramids (important for urine concentration mechanism).
Identify diseases of the Urinary System
Chronic Kidney Disease
Gradual loss of kidney function over months or years
Caused by diabetes mellitus, hypertension, glomerulonephritis or polycystic kidney disease
Leads to: decreased glomerular filtration rate, impaired electrolyte and acid-base balance, overactive RAA, hypertension
Diuretics
Medications that increase urine output by altering renal tubular reabsorption
Different types
Loop diuretics inhibit Na+ reabsorption
Thiazides act on distal convoluted tubule ―
Potassium-sparing diuretics affect collecting ducts
Reduce blood volume
Can affect electrolyte balance
Glomerular Filtration
Golmerular Filtration
The bulk flow of protein-free plasma from the glomerular capillaries into Bowman’s capsule.
The glomerular filtrate must cross three barriers to enter Bowman’s capsule
the capillary endothelial cell layer,
the surrounding epithelial cell layer
the basement membrane that is sandwiched between them
Water and small solutes cross the filter freely while cells and proteins do not
Filtration at the renal corpuscle is driven by Starling forces (hydrostatic and osmotic pressure gradients) existing across the walls of glomerular capillaries.
The filtrate resembles plasma in composition, except that it lacks most of the proteins found in plasma.
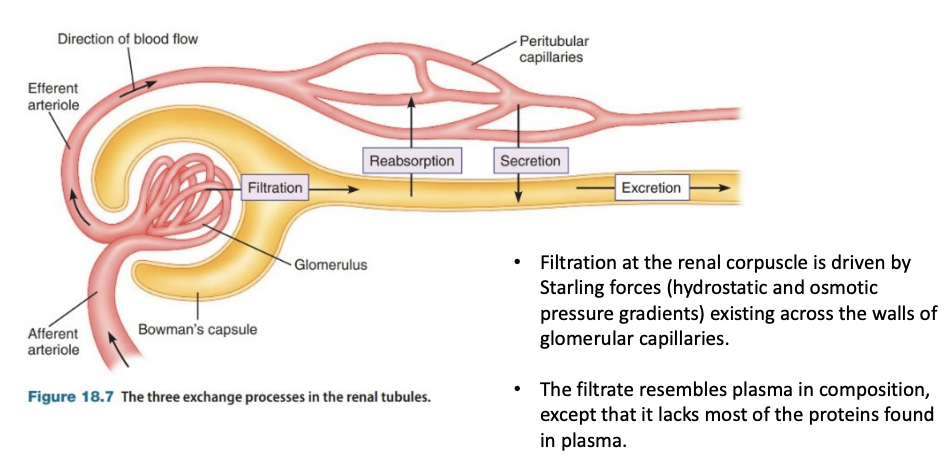
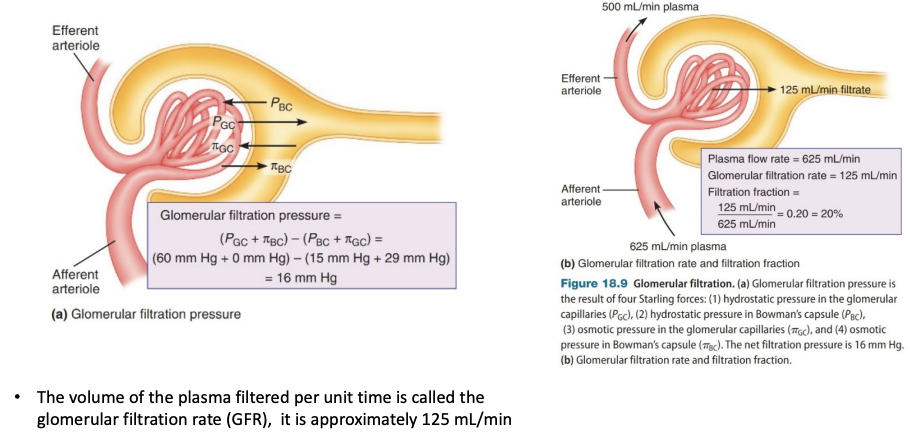
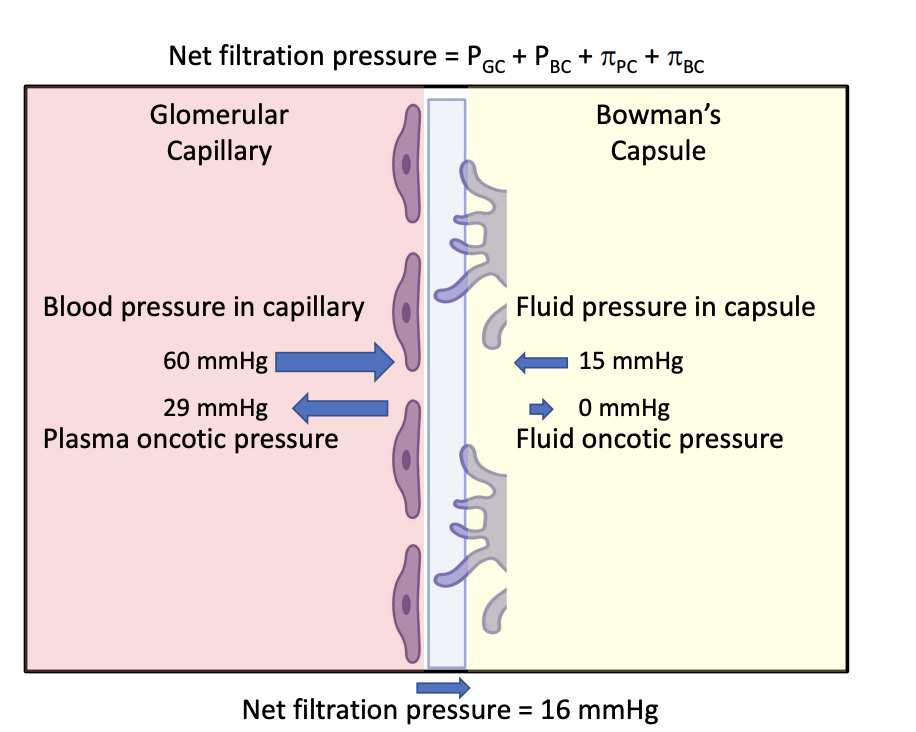
Pressure
Glomerular capillary hydrostatic pressure (PGC) favours filtration and is equal to the blood pressure in the glomerular capillaries (60 mm Hg)
Bowman’s capsule hydrostatic pressure (PBC) opposes filtration and is typically about 15 mm Hg.
Glomerular osmotic pressure (πPC)
Created by the presence of non-permeating solutes.
Opposes filtration because proteins in the plasma draw filtrate back into the glomerulus.
Bowman’s capsule osmotic pressure (πBC) is where the osmotic pressure in Bowman’s capsule favours filtration.
Fluid Pressure is a measurement of the force per unit area on an object in the fluid or on the wall of the vessel
Oncotic Pressure is a form of osmotic pressure induced by the proteins, notably albumin, in a blood vessel's plasma (blood/liquid) that causes a pull on fluid back into the capillary.
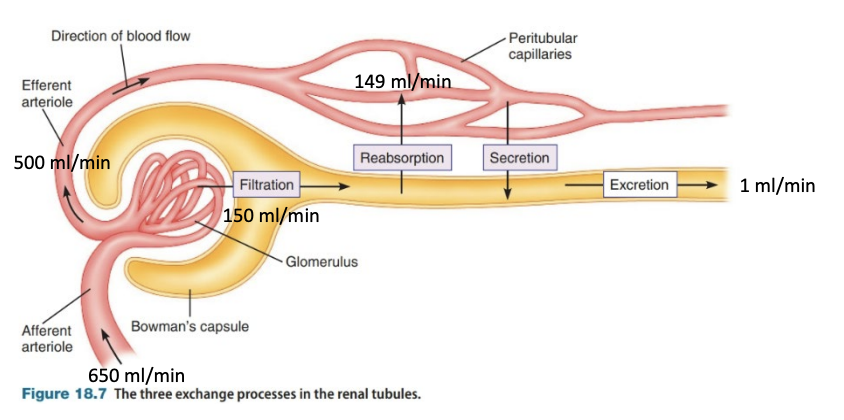
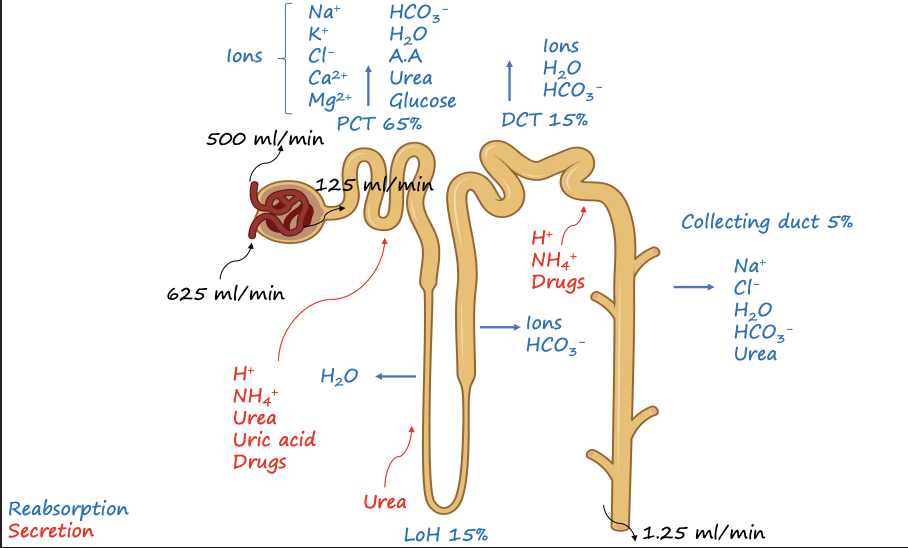
Tubular Reabsorption & Secretion
Excretion from the Kidneys
Excretion by the kidneys entails the elimination of solute and water from the body in the form of urine.
The rate at which a substance is excreted in the urine has a direct bearing on the volume and composition of the plasma.
Simple rule: material that enters the lumen of the renal tubules is excreted unless it is reabsorbed
Amount Excreted = amount filtered – amount reabsorbed + amount secreted
The rate at which a solute is excreted in the urine (expressed in moles/min) depends on:
The amount filtered
The rate at which the solute is secreted
The rate at which solute is reabsorbed.
If the amount of solute excreted per minute is less than the amount filtered, then the solute was reabsorbed in the renal tubules.
If the amount of solute excreted per minute is greater than the amount filtered, then the solute was secreted in the renal tubules.