Infection Control
Infection Prevention and Control Study Notes
Presenter Information
Name: Florence Schaefer, PhD, RN, ACNS-BC
Affiliation: UTHealth Cizik, The University of Texas School of Nursing, Health Science Center at Houston
Objectives
Identify the normal defenses of the body against infection.
Identify patients most at risk for infection.
Explain conditions that promote the transmission of healthcare-acquired infections.
Explain the rationale for standard precautions.
Explain procedures for each isolation category.
Describe the purpose of Personal Protective Equipment (PPE).
Understand the process of donning and doffing PPE.
Nature of Infection
Definition: Infection is the invasion of a susceptible host by pathogens or microorganisms, resulting in disease.
Colonization: Occurs when a microorganism invades the host but does not cause infection.
Communicable Disease: Infectious process transmitted from one individual to another.
Symptomatic Infection: Infection with clinical signs and symptoms present.
Asymptomatic Infection: Infection without clinical signs and symptoms.
Note: Colonization – harbor but don’t cause infection. MSRA is an example in everyone’s nose.
Additional Terminology
Virulence: The ability of a microorganism to produce disease.
Immunocompromised: Refers to having an impaired immune system.
Aerobic Bacteria: Require oxygen for growth and multiplication.
Anaerobic Bacteria: Thrive in environments with little or no free oxygen.
Bacteriostasis: Prevention of growth and replication of bacteria.
Bactericidal: Destructive to bacteria.
Virulence – abilithy to cause disease, flu and covid -19.
Bacteriostatis – cleaning bathrooms only
Chain of Infection
Components:
Infectious Agent: Pathogen (bacteria, viruses, fungi, protozoa).
Reservoir: Where pathogens live (human hosts, animals, food, water).
Portal of Exit: Route by which the pathogen leaves the reservoir.
Mode of Transmission: How the pathogen is transmitted (contact, droplet, airborne, vehicles, vector).
Portal of Entry: Entry route into a susceptible host (same route for exiting).
Susceptible Host: Individual with risk factors (nutritional status, chronic diseases, trauma, smoking).
Mode of Transmission
Contact Transmission: Direct (person-to-person) and indirect (inanimate objects).
Droplet Transmission: Large droplets (> 5 microns) from coughing/sneezing.
Airborne Transmission: Small particles (e.g., Tuberculosis).
Vehicles: Contaminated items, water, blood.
Vector: Animals or insects that transmit diseases.
Footnote: Direct: person to person
Indirect: contact with inanimate object (needles, dressings, etc)
Droplet: sneeze, cough, travels up to 6 feet
Airborne: suspended in air after sneezing or coughing
Vehicles: contaminated items, water, drugs, blood, food
Droplet – larger molecules, coughs and sneezes, flue
Airborne – TB , chicken pox , smaller
Vector – tick, mosquito, etc.
Risk Factors for Susceptible Hosts
Poor nutritional status.
Presence of chronic diseases (e.g., diabetes, cancer).
Traumatic injuries and stress.
Conditions for Thriving
Environment: Warm, dark, moist conditions enhance infection.
Food: Nutrients support growth.
Oxygen: Required by aerobic bacteria.
Water: Essential for all life.
Temperature: Optimal range for growth.
pH: Certain bacteria thrive at specific pH levels.
Light: Limited light can facilitate microbial growth.
Port of Exit and Port of Entry
Skin & Mucous Membranes: Infection can be released through drainage.
Respiratory Tract: Through sneezing or coughing.
Urinary Tract: Through urine (e.g., UTIs).
GI Tract: Through saliva, bowel elimination, bile.
Reproductive Tract: Through urethra or vagina.
Blood: Reservoir for infections like HBV, HCV, HIV.
The Infectious Process
Stages:
Incubation Period: Time between exposure and the onset of symptoms.
Prodromal Stage: Initial vague symptoms.
Illness Stage: Symptoms are evident.
Convalescence: Recovery period.
Types of Infections
Localized Infection: Confined to a specific area.
Systemic Infection: Affects the entire body.
Note: Incubation period: interval between exposure and appearance of symptoms
Prodromal stage: Interval between vague symptoms and more specific
Illness stage: interval where specific symptoms of infection are present
Convalescence: acute symptoms start to disappear
Defenses Against Infection
Normal Floras
Microorganisms that do not cause illness and maintain balance with other microorganisms.
Found on skin, saliva, oral mucosa, GI and GU tracts.
Broad-spectrum antibiotics can reduce body defenses.
Body System Defenses
Skin, eyes, mouth, respiratory tract, urinary tract, GI tract, vagina.
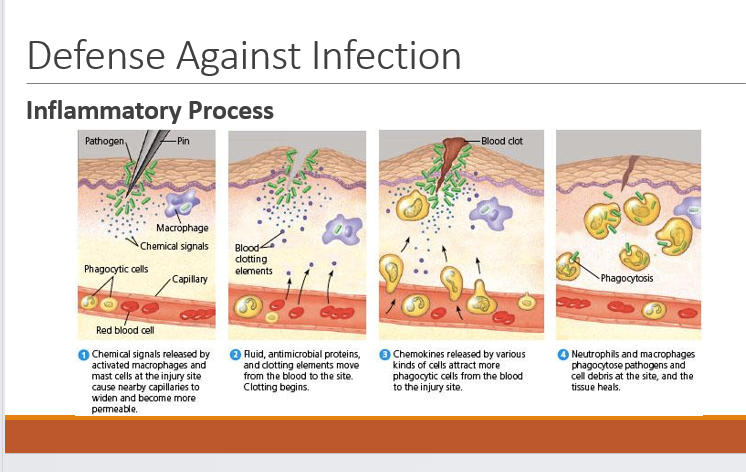
Inflammatory Process
Definition: Cellular response to injury, infection, or irritation.
Chemical Signals: Release from activated macrophages, causing capillary dilation and increased permeability.
Phagocytosis: Neutrophils and macrophages engulf pathogens at the injury site.
Types of Exudates in Inflammation
Serous, serosanguineous, sanguineous, seropurulent, and purulent.
Common Laboratory Tests to Confirm Infection
Laboratory Values and Indications
White Blood Cell (WBC) Count: Normal range 5,000-10,000/mm³; elevated in acute infection.
Erythrocyte Sedimentation Rate (ESR): Normal up to 15 mm/hr for men, 20 mm/hr for women.
Iron Level: Normal 60-90 g/100mL; a decrease suggests chronic infection.
Cultures: Indicates presence of infectious microorganisms.
Differential Blood Count
Neutrophils: 55%-70% - Elevated in acute infections.
Lymphocytes: 20%-40% - Increased in chronic bacterial infections.
Monocytes: 5%-10% - Increased during certain infections.
Eosinophils: 1%-4% - Increased in parasitic infections.
Basophils: 0.5%-1.5% - Normal during infection.
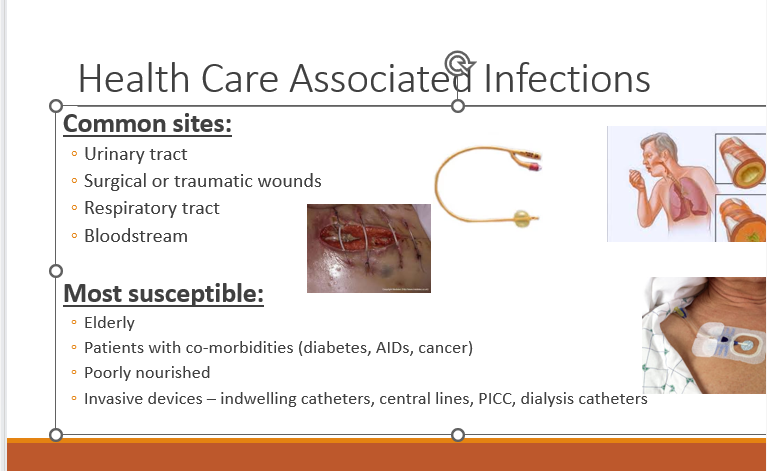
Healthcare-Associated Infections (HAIs)
Definition: Result from germs entering the body during medical care.
Common types:
Catheter-associated urinary tract infections (CAUTIs): Infections from contaminated urinary catheters.
Surgical site infections (SSIs): Infections occurring post-surgery.
Bloodstream infections: Pathogens entering the bloodstream via catheters.
Pneumonia: Infection of the lungs.
Footnote:You get in the hospital. Pneumonia is the most common.
Catheter is invasisve and can set you up for an infection. Twice a day and after a bowel movement. E. Coli.
High-Risk Patients
Elderly individuals, those with co-morbidities (e.g., diabetes, AIDS, cancer), poorly nourished persons, and those with invasive devices.
Implications
Increased healthcare costs, longer hospitalizations, and potential patient disability.
Factors Influencing Infection Prevention and Control
Age: Vulnerability varies with age; vaccinations help prevent diseases.
Nutritional Status: Proper nutrition supports immune function.
Stress: Increases susceptibility to infections due to hormonal effects on the body.
Disease Processes: Conditions like leukemia, AIDS, burns, and chronic diseases weaken immunity.
Hand Hygiene
Proper Handwashing Steps
Wet hands.
Apply liquid soap.
Lather and scrub for at least 20 seconds, ensuring not to forget areas between fingers, under nails, and tops of hands.
Rinse thoroughly for 10 seconds.
Dry hands thoroughly.
Turn off tap using elbow or paper towel.
Five Moments for Hand Hygiene
Before patient contact.
Before performing aseptic tasks.
After exposure to body fluids.
After patient contact.
After contact with patient surroundings.
Footnote:Before you go into a patients room, if you don’t wash before you leave.
C.Diff, must do soap and water.
If you play with the remotes, beds, etc. – have to wash again. Everytime.
Can’t share lotions.
Case Study: Nursing Process Application
Patient Profile
Ms. Thomas: 65 years old, medical history includes well-controlled diabetes and hypertension, post-op Day 4 right knee replacement.
Assessment Findings
Susceptibility & Defense Mechanisms: Factors include age, nutritional status, stress, disease processes.
Clinical Appearance: Assess wound and symptoms of infection via laboratory data (CBC, wound culture).
Nursing Diagnoses
Risk for infection.
Acute pain.
Impaired skin integrity.
Impaired tissue integrity.
Impaired physical mobility.
Risk for falls.
Knowledge deficits.
Planning and Implementation
Set priorities based on ABCs and Maslow’s hierarchy; include team collaboration; monitor signs of infection.
Goals: Prevent exposure to infections, control infection spread, maintain resistance, ensure patient understanding of infection prevention.
Evaluation of Goals
Measure if goals are met; assess patient understanding of hand hygiene.
Infection Prevention & Control Practices
Medical vs. Surgical Asepsis
Medical Asepsis: Clean technique, includes hand hygiene and barrier techniques.
Surgical Asepsis: Sterile technique, essential for procedures requiring skin perforation.
Footnote:Teach back washing hands to control infection
Medical Asepsis which is clean technique, gloves, clean gauze
Surgical Technique, wash hands, sterile gloves, sterile packages. Open up a surgical towel on table. Keep fingers outside of the container. Pull gauze package upside down on the sterile field. Cough, sneeze, laugh, don’t want to reach over the sterile field, don’t leave it unattended.

Disinfection and Sterilization
Disinfection: Eliminates most microorganisms except spores, except bacterial spores.
-low level disinfection - surfaces
-high level disenfection - endoscopes
Sterilization: Completely eliminates all microorganisms including spores (e.g., autoclave).
Reducing Infection Risk
Protective Measures
Separate personal care items (clean stethoscopes beteween patients), regular hygiene, adequate nutrition, and patient education on infection control measures (e.g., vaccines), adequate fluid intake and well balanced diet.
Footnote:Make sure to clean your stethoscopes between patients.
Daily oral hygiene's, more susceptible to pneumonia with bad mouth hygiene.
Dry skin is need to not break infection.
Dressing dry and intact.
Cough contained, cough in a tissue, throw away and wash hands
Proper Disposal Practices
Follow protocols for disposal of contaminated items, maintain cleanliness in patient care areas.

Sharps Container Guidelines
Dispose of needles immediately; avoid recapping to reduce risk of needle-stick injuries.

Isolation Precautions
Types of Isolation
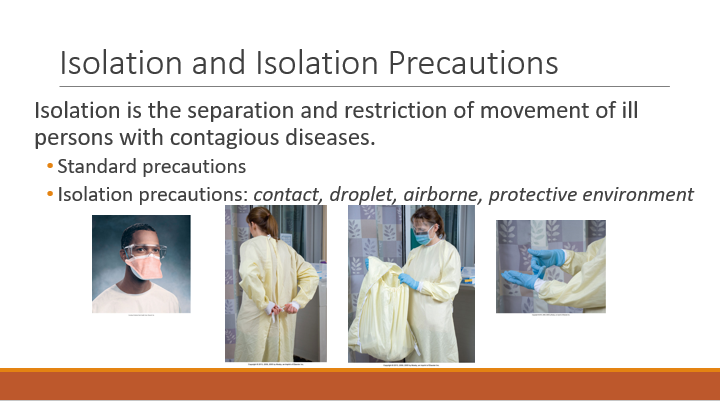
Standard Precautions: Apply to all patients; includes hand hygiene and PPE as needed.•Apply to contact with blood, bodily fluid, non-intact skin, wounds, mucous membranes
•Hand hygiene – before, after, and between direct contact with patient
•instant alcohol hand antiseptic (i.e. Purell)
•handwashing hands (C. diff)
•surgical scrub
•PPE: gloves
•Room Type: Private room is NOT necessary
Contact Precautions: For infections spread by touching (e.g., MRSA).
•Infections that are spread by touching a patient or items in the room
•Examples:
•Methicillin Resistant Staphylococcus aureus (MRSA)
•Respiratory syncytial virus (RSV)
•Wound drainage: abscesses
Room Type: Private or cohort patients
•PPE: gown, gloves
•Remove gowns and gloves
BEFORE leaving the room
•Patient Considerations:
•MUST wear clean gown
when leaving room
•Dedicated supplies:
thermometers, stethoscopes
Footnote: Gloves and a gown. If patient has infection they could share a room with someone with the same infection.
The rooms should be equipped with all PPE. Do not share testing items with infected people.
•Hand hygiene
Droplet Precautions: For pathogens spread by droplets (e.g., influenza).
•Infections that are spread in large droplets (> 5 microns) caused by coughing or sneezing
•Examples:
•Pneumonia
•Influenza
•Pertusis
•Room type: Private or cohort patient rooms (3 feet distance)
•PPE: surgical masks (within 3 feet of patient), gowns, and gloves
•Remove all PPE before leaving the room
•Patient Considerations:
•MUST wear surgical mask
when leaving room
•Dedicated supplies:
thermometers, stethoscope
•Hand hygiene
Airborne Precautions: For pathogens spread through the air (e.g., tuberculosis).

Protective Environment: For immunocompromised patients (e.g., stem cell transplants).
For Stem Cell Transplants
Room Type:
Private room
Positive air flow
HEPA filtration for incoming air
PPE:
Mask, gloves and gowns
Note:eserved for patients highly susceptible to infection due to an underlying condition
Personal Protective Equipment (PPE)

Determine what barriers you will need before entering a patient’s room:
◦Gloves
◦Gowns
◦Masks
◦Protective eyewear
◦Other materials:
◦Sharps container
◦Lab specimen collection
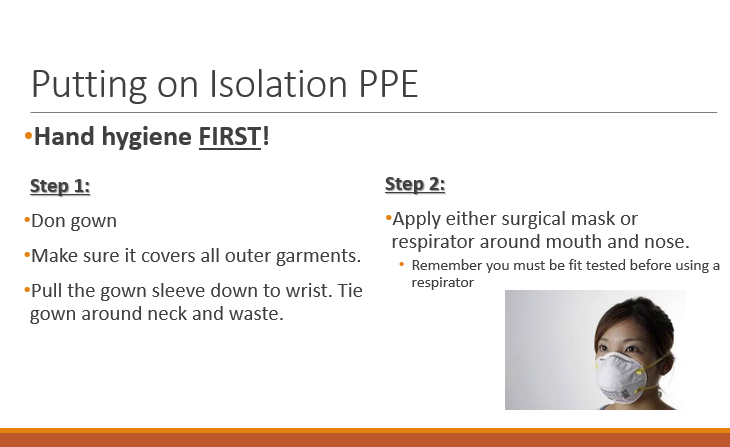
Donning Procedures:
Perform hand hygiene.
Don gown to cover clothing.
Apply mask or respirator and goggles if needed.
Don gloves last.

Doffing Procedures:
Remove gloves first, dispose properly.
Remove eyewear if present.
Untie gown and dispose.
Remove mask without touching the exterior surface and perform hand hygiene.

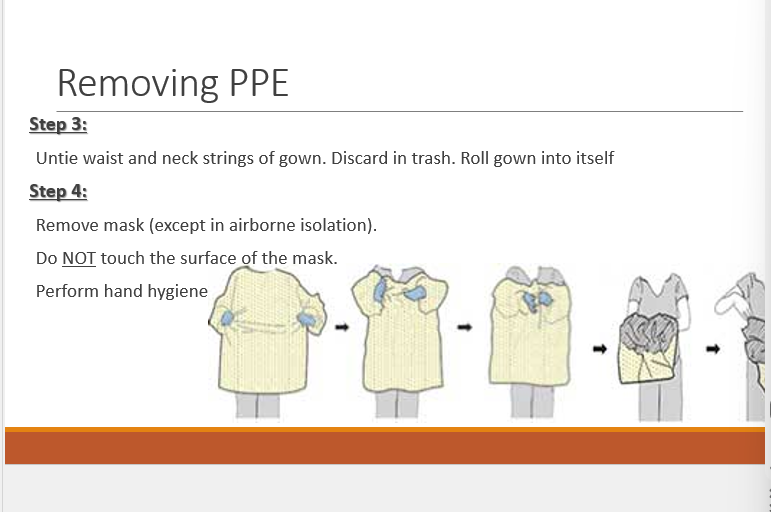
Remove gloves
Remove eyewear/face shield and goggles
Untie gown, allow gown to fall from shoulders, and do not touch outside of gown; dispose of properly.
Remove mask by strings; do not touch outside of mask.
Perform hand hygiene
Leave room and close the door
Psychological Implications for Patients
Patients may perceive feelings of loneliness, increased anxiety, and altered body image due to isolation protocols.
Nurses should provide compassionate care and address patient concerns.
Review Questions
Identify the patient most at risk for infection following a hip arthroplasty.
Appropriate nursing questions while admitting a patient with an infectious disease.
Correct order to remove PPE after patient care under droplet isolation.