L3: What happens to drugs in the body
Learning Outcomes
By the end of this lecture, you should be able to:
Define pharmacology and distinguish between pharmacokinetics (what the body does to a drug) and pharmacodynamics (what a drug does to the body).
Understand drug classifications and the three types of drug names.
Describe the four pharmacokinetic processes: absorption, distribution, metabolism, and excretion.
Explain factors influencing drug absorption, distribution, metabolism, and excretion.
Understand bioavailability and first-pass metabolism.
Interpret a plasma concentration-time curve.
Pharmacology Overview
Pharmacology: Study of how medicines work and affect the body.
Derived from Greek: pharmakon (drug) + logia (knowledge).
Two branches:
Pharmacokinetics: What the body does to the drug.
Pharmacodynamics: What the drug does to the body.
What is a Drug?
A substance that, when introduced to the body produces a biological effect for an intended purpose.
Often treats symptoms (not causes), e.g., antimicrobial drugs.
Types:
Small molecules
Biologics (proteins, antibodies)
Types of Drug Names
Type | Audience | Characteristics |
|---|---|---|
Chemical Name | Chemists | Describes the complex chemical structure (need to know the functional grp before changing the struc |
Generic Name | Pharmacologists | Indicates use, action, or structure |
Brand Name | Public | Marketing name, varies by manufacturer/country, made to be memorable |
Example: Lipid-lowering drugs (-vastatin): atorvastatin, fluvastatin, pravastatin
Pharmacokinetics: What the Body Does to a Drug
Absorption – Will it get in?
Distribution – Where will it go?
Metabolism – Will it remain intact?
Excretion – Will it stay in?
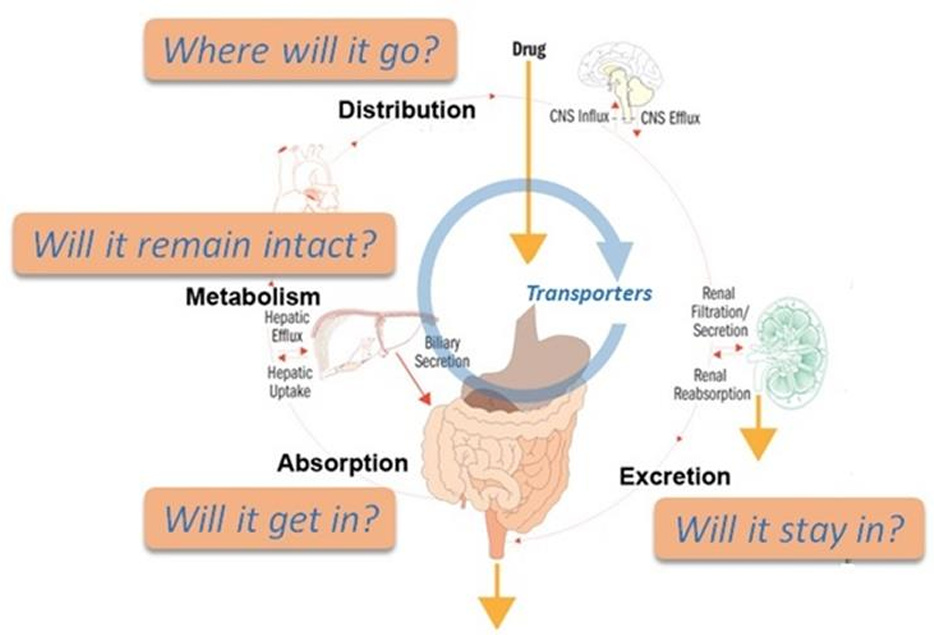
1. Drug Absorption
Movement of a drug from administration site to systemic circulation.
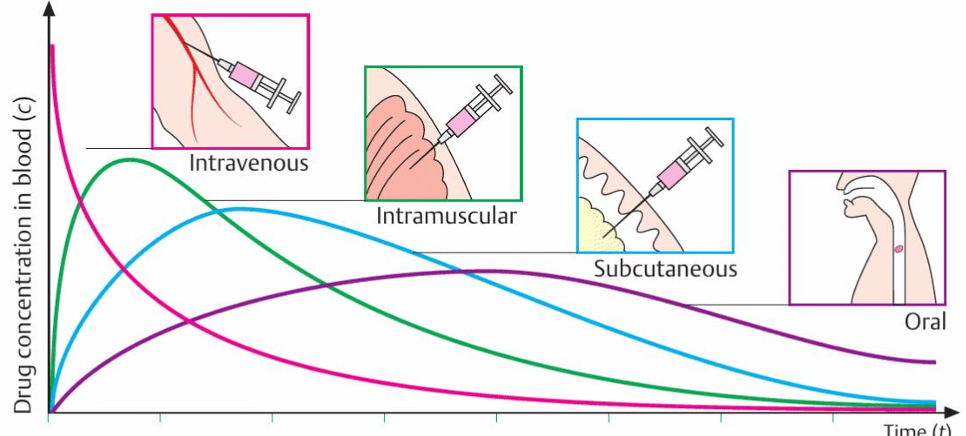
Routes: oral (most common), IV, nasal spray, subcutaneous.
Absorption influenced by:
Physicochemical properties:
Molecular size: larger = poorer absorption
Lipophilicity vs. hydrophilicity: some lipophilicity needed to cross epithelial cell membranes
Ionisation: only neutral (not ionised) molecules cross membranes passively as lipids are not good conductors
Biological factors:
Local pH, determines whether the drug is ionised to what extent
GI motility, eat before drinking so that slow down the movement of the gut to slow down absorption of alcohol
Enzymatic breakdown in gut wall
Transporters (can return drugs to gut lumen)
2. Drug Distribution
Reversible passage of drug between tissues, organs and compartments.
low plasma conc indicates widely distributed drug
Influenced by:
Lipophilicity/hydrophilicity:
Hydrophilic = stays in bloodstream
Lipophilic = accumulates in fat
Plasma protein binding: only free drug distributes
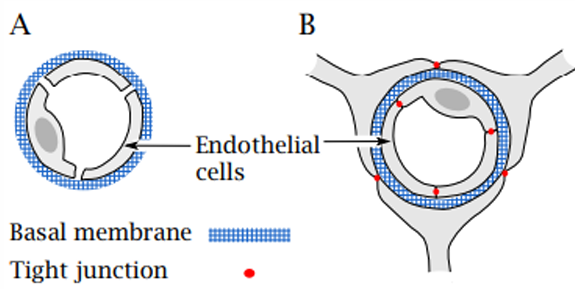
Blood-brain barrier: tight junctions, transporters
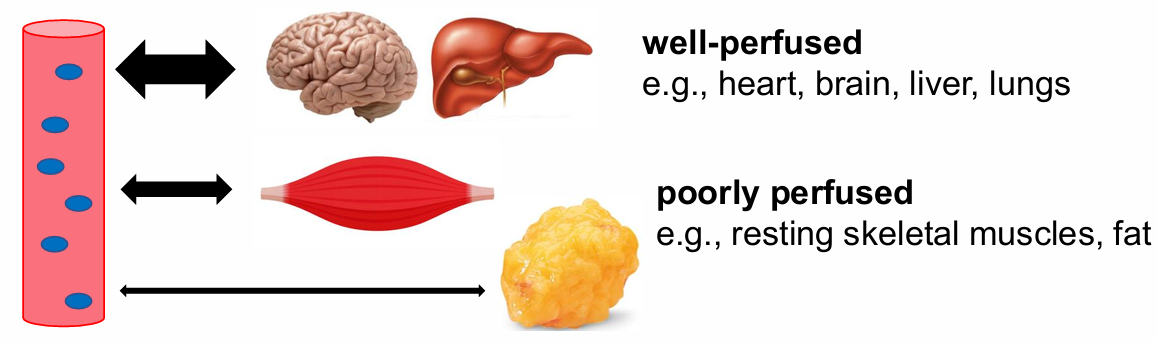
Blood flow:
Well-perfused: heart, brain, liver, lungs
Poorly perfused: resting muscles, fat
3. Drug Metabolism
Chemical transformation of a drug into metabolites.
Not all drugs undergo metabolism.
what goes in also comes out e.g. penicillin
Can be mediated by enzymes (act as catalysts).
Alters drug activity:
Active → inactive (most common)
Active → active
Active → toxic ft
Prodrug (inactive) → active
increases hydrophilicity of metabolites: ↓ lipophilic drug accumulation in tissues
Influencing factors:
Genetics: alters the expression and/or activity of enzymes
Disease (e.g., liver disease)
Ageing: ↓ liver function
Other medications: competition on which drug is metabolised
4. Drug Bioavailability
Fraction of administered does of the parent drug reaching systemic circulation.
IV drugs: 100% bioavailability.
Oral drugs: affected by absorption and first-pass metabolism (what is left after gut wall and liver).
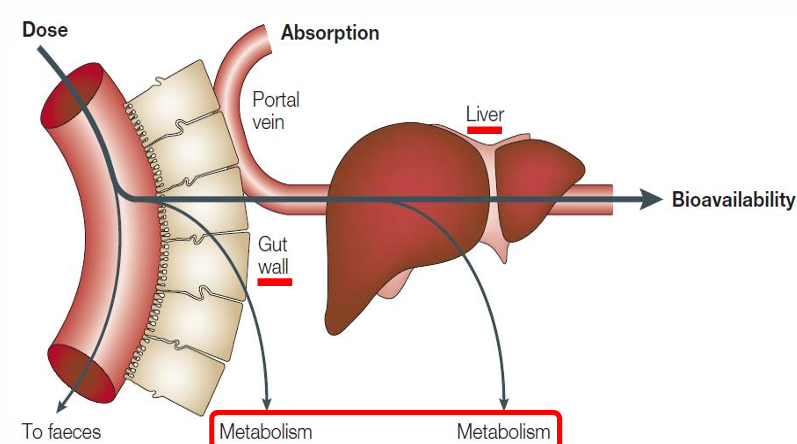
Influenced by same factors as absorption.
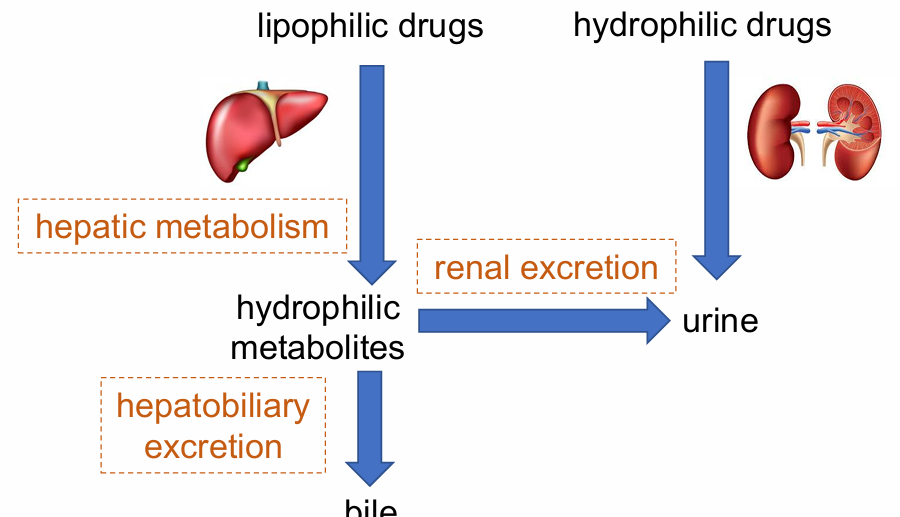
5. Drug Excretion
Refers solely to the physical processes that lead to the irreversible its metabolites from the body
~25% excreted unchanged.
Routes:
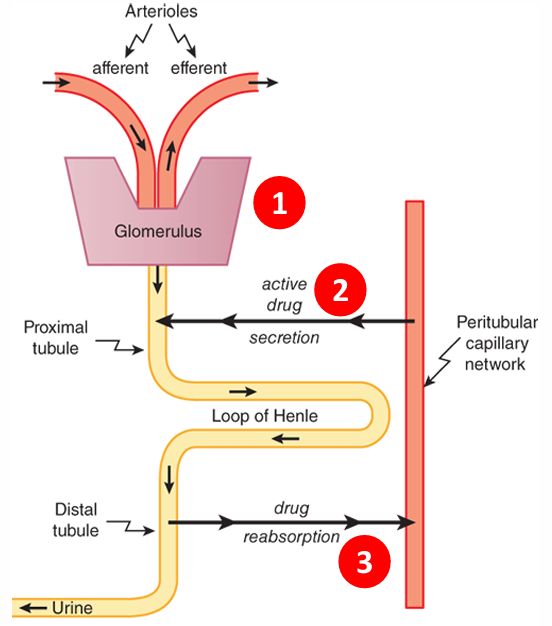
Urine (most important): filtration, secretion, reabsorption
Faeces (via bile)
Breast milk
newborns may be exposed to drugs through milk intake
Expired air (e.g., anaesthetics)
Hair, skin/sweat
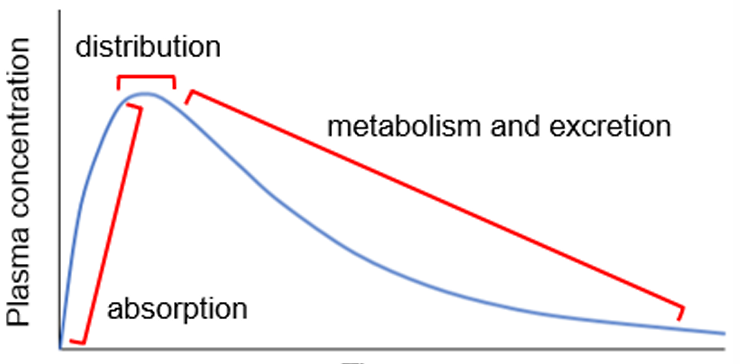
Plasma Concentration-Time Curve
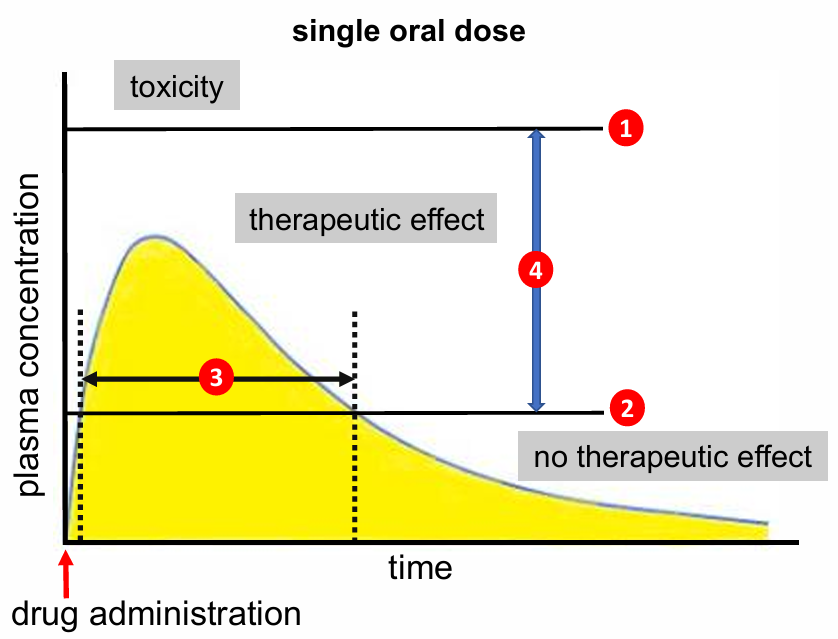
Key parameters:
Minimum toxic concentration
Minimum effective concentration
Duration of action
Therapeutic window
Revision Questions
Define drug absorption and describe one physicochemical property affecting it.
Drug A is found in the brain 30 mins after IV administration. Which process explains this?
Correct answer: B. Distribution
How does blood flow influence drug distribution?
Name the two plasma concentrations that define the therapeutic window.