8.2 - Pancreas (Part 1)
LECTURE NOTES
PANCREATIC EMBRYOLOGY
Abdominal accessory organ arise as foregut outgrowths
Proximal duodenum rotates
Ventral and dorsal ducts of the pancreas join together as the proximal duodenum rotates clockwise
Bile and pancreatic duts join to drain together at major papilla
PANCREATIC ANATOMY
Found otuside the abdomen
Four parts of the pancreas: head, neck, body and tail
Spleen is at the tip of the tail of the pancreas
PANCREATIC IMAGIN
CT scans are the best way to image the scans
MRCP - magnetic resonance cholangiopanreatography
Helps to see the finer structures within the pancreas more clearly
ENDOCRINE VS EXOCRINE SECRETION
Endocrine is only 2% of gland
Islets of langerhans
Secretes hormones into blood - insulin & glucagon (also somatostain and pancreatic polypeptide)
Regulation of blood glucose, metabolism and growth effects
Exocrine secretion is the remaining 98%
Secretes pancreatic juice to duodenum via MPD/sphincter of Oddi/ampulla
Digestive function (covered in this lecture)
PANCREATIC CELL DIFFERENTIATION
Acini
Produce pancreatic juice
Connected to ducts
Grape-like shape
Secrete pro-enzymes (inactive enzymes)
Islets
Derived from the branching duct system
Lose contact with ducts - become islets
Differentiate into alpha and beta cells
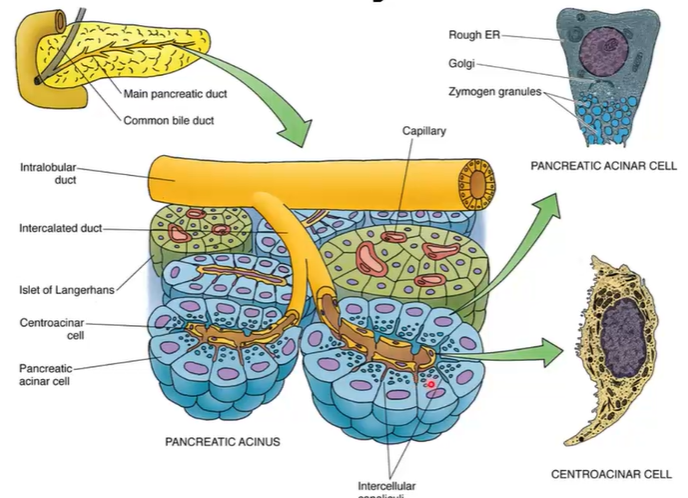
Pancreatic acinus - with many pancreatic acinar cells
Between them is intercellular canaliculi
Pancreatic juice secrete gradually join bigger and bigger ducts
COMPOSITION OF ISLETS
alpha: form about 15-20% of tissue and secrete glucagon
beta - form about 60-70% of islet tissue and secrete insulin
delta - form about 5-10% of islet tissue and secrete somatostatin
COMPOSITION OF ACINI
Secretory acinar cells - large with apical secretion granules
Produce thick, viscous, pure pancreatic jelly
Large with secretions around the duct (ducts are small and pale)
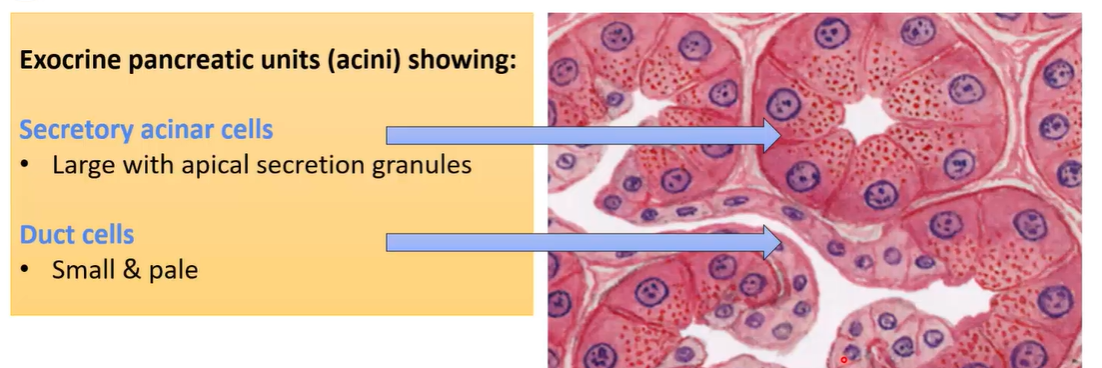
Acinar cells produce enzyme rich viscous mucinous low volume pure enzymes
Altered by high volume watery bicarbonate rich juice which is added to increase the pH and that is done by the duct and centroacinar cells
BICARBONATE SECRETION
Bicarbonate produced by duct and centroacinar cells
There to neutralise acid chyme from the stomach
Prevents damage to duodenal mmucosa
Raises pH to optimum range for pancreatic enzymes to work
Washes low volume enzyme secretion out of the pancreas into the duodenum
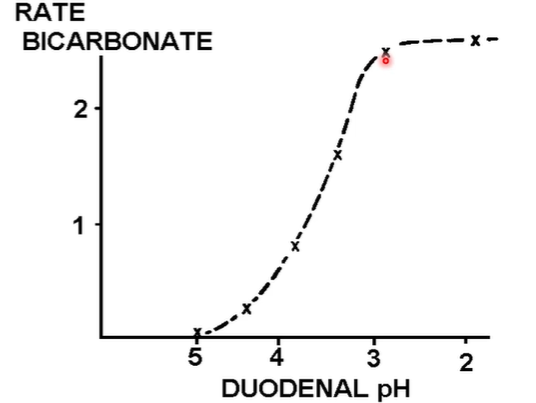
Bicarbonate secretion stops when pH is still acidic → main reason is because there are other things that can also help e.g bile and brunners glands secrete alkaline fluds
Pancreatic Cabronate Secretion
Catalysed by carbonic anhydrase
Separation of H+ and HCO3-
Sodium moves down gradient by tight junctoin and water follows
Chloride and bicarbonate exchange at llumen (Anion exchanger)
Na+ and proton exchange at basolateral membrane into bloodstream
Exchanges are driven by electrochemical gradient
High sodium concentration hgih outside compared to inside
High chloride in lumen compared to intracellular
Sodium gradient maintained by sodium potassium pump
Potassium returns to blood via potassium channel
Chloride returns to lumen via chloride channel (cystic fibrosis transmembrane conductance regulator - CFTR)
Gastric venous blood is very alkaline
Pancreatic venous blood is acidic
ACINAR CELL ENZYME SECRETION
Enymes for digestion of fat, protein and carbohydrates
Syntehsised and stored in zymogen granules
Proteases released as inactive pro-enzymes
Protects acini and ducts from auo-digestion
Pancreas also contains a trypsin inhibitor to prevent trypsin activation
Enzymes only activated in duodenum
Blockage of MPD may overload protection (auto digesiton which leads to pancreatitis)
Enzyme secretion
Duodenal mucosa secretes an enzyme - enterokinase, which converts trypsinogen into trypsin
Trypsin then converts all other proteolytic and some lipolytic enzymes
Lipase secrted in active form but requires colipase, and it also requires the presence of bile salts for effective action
ALTERED PANCREATIC ENZYME FUNCTION
Enzyme production depends on our diet
Orlistat increases faecal dat
occurs when pancreatic lipase secretion decreased
e.g. cystic fibrosis, chronic pancreatitis
PANCREATIC JUICE SECRETION
Cephalic phase - reflex resposne to sight/smell/taste of food
Gastric phase - stimulation of pancreatic secretion originating from food arriving in the stomach, and same mechanisms involved as for cephalic phase
Intestinal phase - hormonally mediated when gastric chyme enters duodenum with both components of pancreatic juice stimulated
CONTROL OF SECRETION
viscous components and bicarbonate components are separately controlled
controlled in acini by vagus nerve and cholecystokinin
Bicarbonate secretion controlled in duct and centroacinar cells by secretin (cAMP)
Vagus nerve - acetylcholine as NT - stimulates
Mechanisms responsible for controlling cholecystokinin afrom duodenal I cellsL]
GRP - gastric releasing peptide that stimulates pancres
Produce a monitor peptide which can then stimulate the cell to produce cholecystokinin
Taking in fatty acid will stimulate cholecystokinin releasing peptide (CCK-RP)
Tryspin has a negative effect on all these mechanisms
Acinar fluid is isotonic
Secretion of acinar fluids and proteins it contains is stimulated by cholecystokinin
Secretin stimulates secretions of water and bicarbonate from cells lining extralobular ducts and secretin-stimulated secretion is richer in bicarbonate cf acinar secretion because of chloride/bicarbonate exchange
CCK alone no effect on bicarbonate secretion
CCK and secretin increases rate of bicarbonate of secretion significantly
SUMMARY OF A MEAL
Food mixed, digested in stomach - acidic ph 2
Chyme squirted into the duodenum
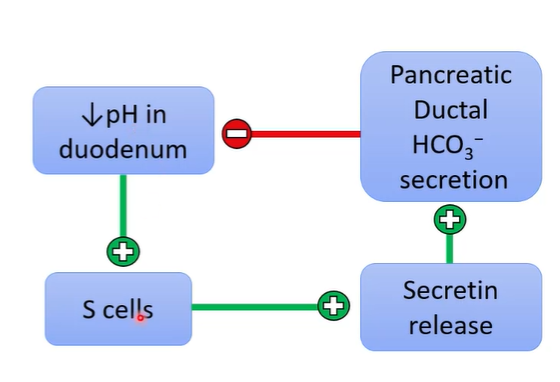
protons in duodenum increases secretin secretion and increases pancreatic juice secretion
this inc combination with bile and Brunner’s gland secretion increases pH to neutral and alkaline
Peptides and fat in duodenum cause sharp in cholecystokinin and vagal nerve stimulation which stimulates pancreatic enzyme release
Peaks by 30 mins continues until stomach empties
CCK potentiates effects of secrtin on aqueous component
Necessary as most of duodenum not at low pH