HUMAN REPRODUCTION AND REPRODUCTIVE HEALTH
Human reproduction
Sexually reproducing
Viviparous
Reproductive events
Gametogenesis
Insemination
Fertilisation
Implantation
Gestation
Parturition
REPRODUCTIVE SYSTEMS
Male Reproductive System
Location: Pelvis region
Includes:
Pair of Testes
Accessory Ducts
Accessory Glands
External Genitalia
1) PAIR OF TESTES
Location: Outside abdominal cavity within a pouch called scrotum
Scrotum helps in maintaining the low temperature of the testes which is 2-2.5°C lower than the normal internal body temperature which is necessary for spermatogenesis
Each testicle is oval in shape
Length: 4-5 cm
Width: 2-3 cm
The testis is covered by a dense covering
Each testis had about 250 compartments called testicular lobules
contains 1/3 highly coiled seminiferous tubule in which sperms are produced
Seminiferous tubule:- lined on its inside by 2 type of cells
Male germ cells
Setolli cells
Male germ cells
- undergo meoitic divisions leading to sperm formation
Sertolli cells
- Provide nutrition and shape to the germ cells
Interstitial Spaces: The regions located outside and between the highly coiled seminiferous tubules (regions surrounding the seminiferous tubules).
It contains:
Small Blood Vessels
Interstitial cells/Leydig cells
Immunologically Competent cells
LEYDIG CELLS
- synthesise and secrete androgens (testicular hormones)
2) ACCESSORY DUCTS
Includes:
Rete testis
Vasa Efferentia
Epididymis
Vas deferens / ductus deferens
Rete testis
- Seminiferous tubules open into the vasa efferentia through rete testis
Vasa Efferentia
- leave the testis and open into epididymis
Epididymis
- location: along the posterior surface of testis.
- 20 feet long, coiled tube
- within epididymis the sperm complete their maturation and their flagella become functional, if sperms are not ejaculated thn they are phagocytized after one month of storage
- smooth muscle in the wall of epididymis propel the sperm into the vas deferens
- stores the sperms (site of storage)
Vas deferens
- vas deferens extends from epididymis (in the scrotum) into the abdominal cavity through the inguinal canal
- INGUINAL CANAL ; an opening in the abdominal wall for the spermatic cord (A connective tissue sheath that contains the vas deferens, testicular blood vessels and nerves)
Ejaculatory Duct (2): It acts as a tube (formed by the vas deferens and seminal vesicle duct) that transports sperm to the urethra. Each one receives sperm from its respective vas deferens along with secretions from the seminal vesicle on the same side. Both ducts empty into the single urethra. It also stores sperm
Urethra: Urethra passes through the corpus spongiosum (the column of spongy erectile tissue in the penis that surrounds the urethra) and its opening is known as urethral meatus, which lies on the tip of the glans penis
3) ACCESSORY GLANDS
Seminal Vesicles (Paired)
Prostrate Gland (Single)
Bulbourethral glands (paired) [Cowper's gland]
Their collective secretion is called seminal plasma. It is rich in fructose, Ca
and enzymes.
Seminal Vesicles (Paired)
|
Prostrate Gland (Single)
|
Bulbourethral Glands/Cowper’s Glands (Paired)
|
SEMEN = 60% seminal fluid + 30% prostatic fluid + 10% sperm + small amount of secretion from Cowper’s glands. SEMEN = SEMINAL PLASMA + SPERM Seminal plasma is rich in fructose, calcium, and certain enzymes |
4) EXTERNAL GENITALIA
Penis —> Cylindrical, muscular erectile organ formed with certain specialized erectile tissues to facilitate insemination.
Penis —> Consists of a root, a body and the glans penis
Root: Attached portion (Bulb of penis, Crus of Penis)
Body of Penis
- Composed of three cylindrical masses of spongy tissue (erectile tissue):
1. CORPORA CAVERNOSA : 2 dorsolateral fibrous ligamentous tissue
2. CORPUS SPONGIOSUM : 1 ventral vascular spongy tissue
All three masses of tissue are enclosed by fascia and skin
Glans Penis—> distal enlarged end of penis [elongation of corpus spongiosum] and is covered with a fold of skin called the PREPUCE/FORESKIN.
IMPOTENCE —> Failure of erection of penis
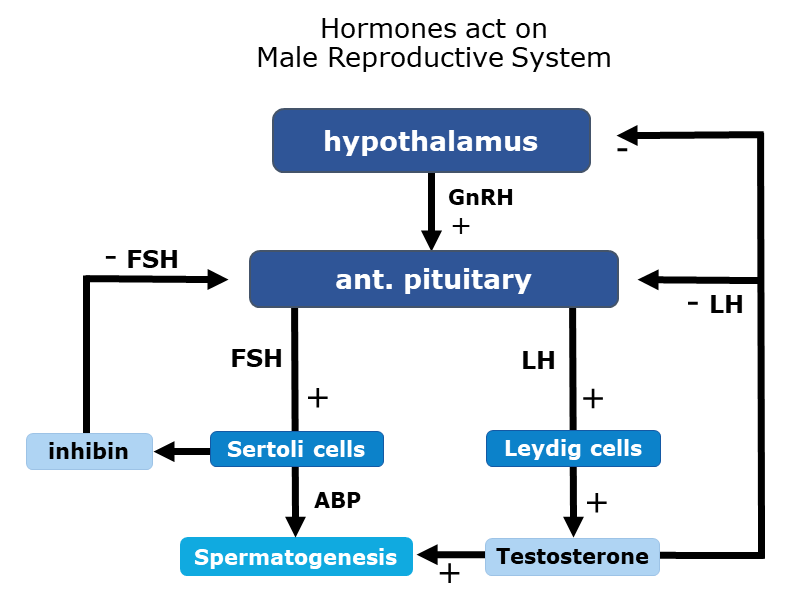
HORMONAL CONTROL OF MALE REPRODUCTIVE SYSTEM
When puberty starts —> neurosecretory cells [in hypothalamus] increase their secretion of gonadotrophin-releasing hormone (GnRH).
GnRH —> stimulate the Anterior pituitary to increase its secretion of Luteinizing hormone (LH) & follicle-stimulating hormone (FSH)
LH —> Stimulates Leydig cells to secrete testosterone, synthesized from cholesterol.
Testosterone —> acts in a -ve feedback to suppress secretion of LH by anterior pituitary & GnRH by hypothalamic neurosecretory cells
Androgens —> stimulate process of spermatogenesis
FSH —> acts on Sertoli cells and stimulate secretion of some factors which help in the process of spermiogenesis
Once spermatogenesis is sufficient for male reproductive functions, Sertoli cells release inhibin, which reduces FSH secretion from the anterior pituitary.
Other effects produced by androgens
(i) Prenatal Development: Before the birth of a son, testosterone stimulates the male pattern development of reproductive system ducts and descent of testes. DHT—> stimulates development of external genitals (ii) Development of male sexual characteristics: At puberty, testosterone and DHT cause the growth and enlargement of male sex organs and the development of masculine secondary sexual characteristics. (iii) Development of sexual functions: Androgens —> contribute to male sexual behaviour and sex drive (libido) in males (iv) Stimulation of anabolism: Androgenic-anabolic hormones [stimulate protein synthesis.] This is obvious—in heavier muscle and bone mass of most men compared to women |
Female Reproductive System
Location: Lower Pelvic region
The female reproductive system includes:
Pair Of Ovaries
Accessory Ducts
(i) Oviduct
(ii) Uterus
(iii) Cervix
(iv) Vagina
External Genitalia
Accessory Sex Glands
(i) Bartholin / Greater Vestibular glands / Bulbovestibular glands
(ii) Skene’s/Paraurethral/Lesser Vestibular Glands
(iii) Mammary Gland
1) OVARIES
Paired organs
Primary sex organs
Produce secondary oocytes and hormones like progesterone, estrogen, inhibin & relaxin.
They arise from the same embryonic tissue as the testes and are the size & shape of almonds [greyish-pinkish structures].
Length of Ovary: 2-4 cm
Location: Either side of lower abdomen on either side of uterus
—> Connected to dorsal abdominal wall by MESOVARIUM ligaments
—> Connected to uterus by OVARIAN ligaments
Blood vessels and nerves enter by mesovarium
Each ovary is covered by,
—> Surface covering: Germinal epithelium (simple cuboidal mesothelium; modified peritoneum)
—> Just beneath epithelium: Tunica albuginea (dense connective tissue layer)
—> Ovarian stroma (internal):
Cortex (outer/peripheral, dense): Contains ovarian follicles, corpus luteum, corpus albicans
Medulla (inner, loose): Contains blood vessels, lymphatics, nerves, and loose connective tissue (no follicles)
Surgical removal of ovaries—OOPHORECTOMY
Oophorectomized female—Menstruation & ovulation absent
2) ACCESSORY DUCTS
(i)Oviduct:
Known as the fallopian tube/Uterine tube
Extends laterally from the uterus (extends from the periphery of ovary to uterus)
Size: 10-12 cm long
Lined internally by ciliated columnar epithelia.
Removal of oviduct —> TUBECTOMY
Divided into 3 Parts;
Infundibulum
Ampulla
Isthmus
Infundibulum
- Funnel-shaped end, which lies close to ovary, broad-wide. It is open to the pelvic cavity.
- Ends in a fringe/finger like projection called Fimbriae.
- Helps for collection of ovum
Ampulla
- Infundibulum leads to ampulla - actual site of fertilisation
Isthmus
- Has a narrow lumen and joins the uterus
After ovulation, fimbriae sweep the secondary oocyte into uterine tube
The ovum is taken to the uterus through peristaltic movement in the fallopian tube.
(ii) Uterus:
Also called the womb/hystera/metra
Location: B/w the urinary bladder and rectum
Shape: Inverted pear
Site for implantation & fetal growth & helps for placentation & expelling the baby during parturition.
Surgical removal of the uterus - HYSTERECTOMY
The uterine wall is divided into 3 layers
—> Perimetrium (visceral peritoneum) - Thin, Membranous —> Myometrium: Middle thick muscular layers - consist of smooth muscle [strongest, thickest, and longest smooth muscle] - form bulk of uterine wall.
—> Endometrium: (glandular)
|
(Uterus) Divided into 3 parts
Fundus
Body/Corpus [The uterine wall (especially of the body/corpus) is composed of three layers: perimetrium, myometrium, and endometrium.]
(iii) Cervix
Fundus: upper-dome-shaped above uterine tube Body - central portion Cervix:
|
(iv) Vagina
Length: 8 - cm long
Fibromuscular tubular canal that extends from the exterior (of the body, vulva) to the cervix (uterine).
Tube - internally lined by non-keratinized stratified squamous epithelium
The vaginal opening —> vaginal orifice.
Receptacle for the penis during coitus (receives)
Outlet for menstrual Flow
Passage for childbirth (made of smooth muscles)
The vagina is highly vascular.
Contains mucosa (mucous membrane) —> contains large amounts of glycogen —> decomposition of glycogen by lactobacillus bacteria produces organic acid —> thus causing acidic environment [which retards microbial growth & is harmful to sperm]
3) EXTERNAL GENITALIA
Vulva/Pudenum
Divided into 6 categories
MONS PUBIS
LABIA MAJORA
LABIA MINORA
CLITORIS
VESTIBULE
HYMEN
1) MONS PUBIS Cushion of fatty tissue (elevation of adipose tissue) covered with skin and pubic hairs 2) LABIA MAJORA Outer, larger, fleshy fold of tissue which extends down from mons pubis and surrounding vaginal opening 3) LABIA MINORA Paired folds of tissue under the labia majora 4) CLITORIS
5) VESTIBULE
6) HYMEN A thin (mucous) membrane partially covering the vaginal opening (introitus). |
4) ACCESSORY GLANDS
(i) Bartholin / Greater Vestibular glands / Bulbovestibular glands⭐
One pair of small alveolar glands present just b4 labia minora on each side of vaginal orifice
Secretes mucus for lubricating the vagina during sexual stimulation, mating, parturition
(ii) Skene’s/Paraurethral/Lesser Vestibular Glands
Pair of small glands near the external urethral opening
Secrete fluid for urethral lubrication during arousal
Homologous to the prostate gland
(iii) Mammary Gland
Located in breasts
Modified Sweat glands that produce milk
Each breast has a pigmented projection - the nipple, which is surronded by a circular pigmented skin → areola
Attached to thoracic wall through Pectoralis Major Muscle
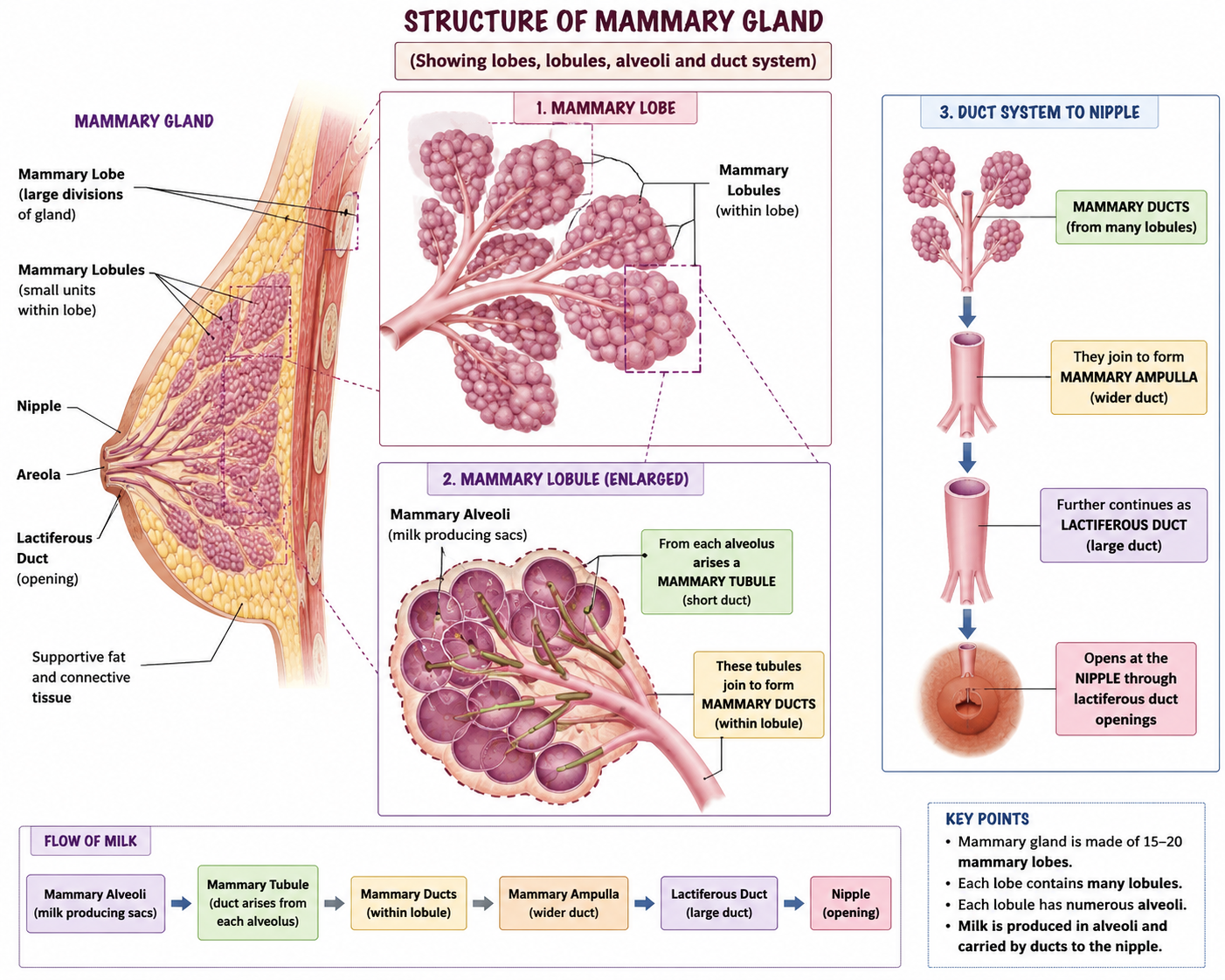
Each mammary gland consists of 15-20 lobes
Each lobe is divided into smaller lobules(many) inside which milk producing alveoli are found
The alveoli cells secrete milk which is stored in the lumen of alveoli
Mammary tubules arise from each individual lobule and carry milk from alveoli to larger ducts.[The alveoli open into mammary tubule]
The tubule of each lobe/lobule join to form Mammary duct
Several mammary ducts join to form many mammary ampulla located just below nipple
Ampulla is connected to 15-20 number of lactiferous ducts that opens to exterior through nipple through which milk is sucked out.
LACTATION: Sythesis, secretion and ejection of milk [ Process of milk production, secretion, and release from the mammary glands.]
GYNAECOMASTIA: Development of breast in males
MASTECTOMY(Female): Surgical removal of breasts
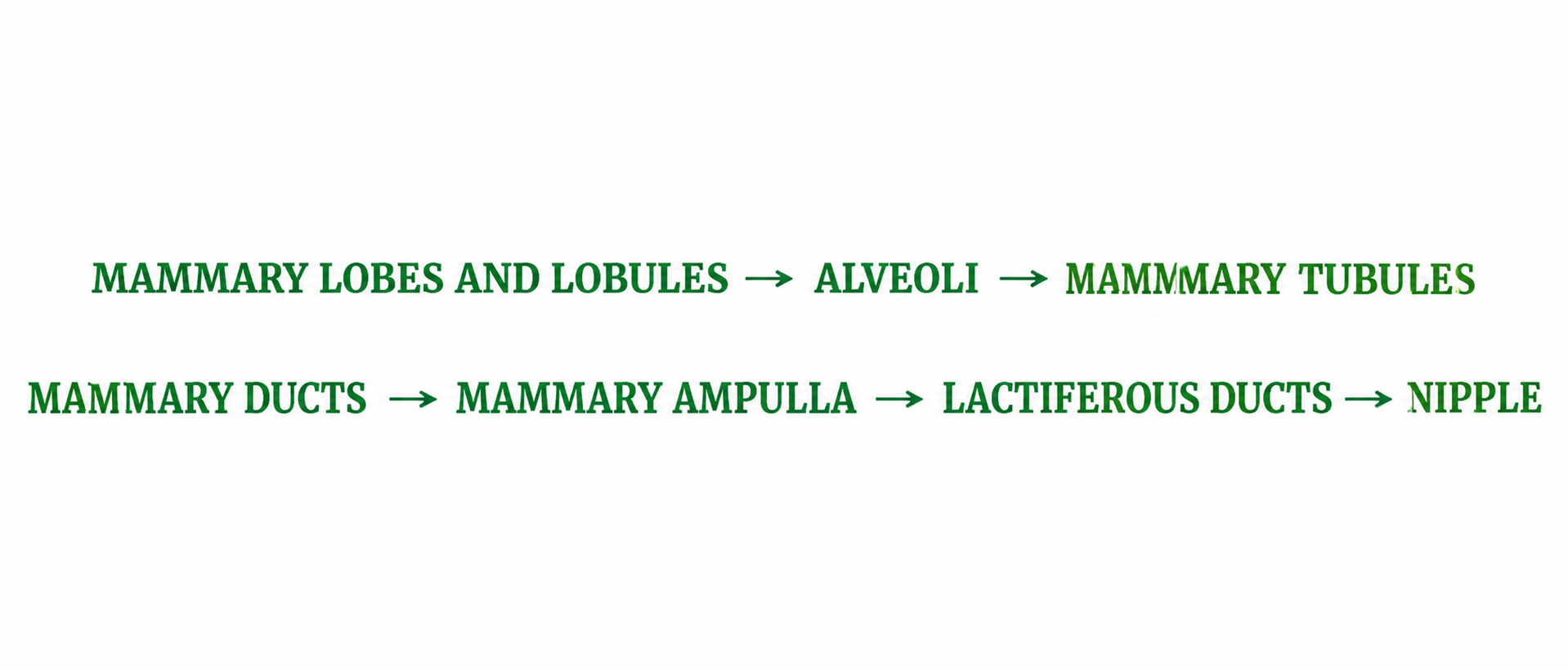
HORMONAL CONTROL OF FEMALE REPRODUCTIVE SYSTEM
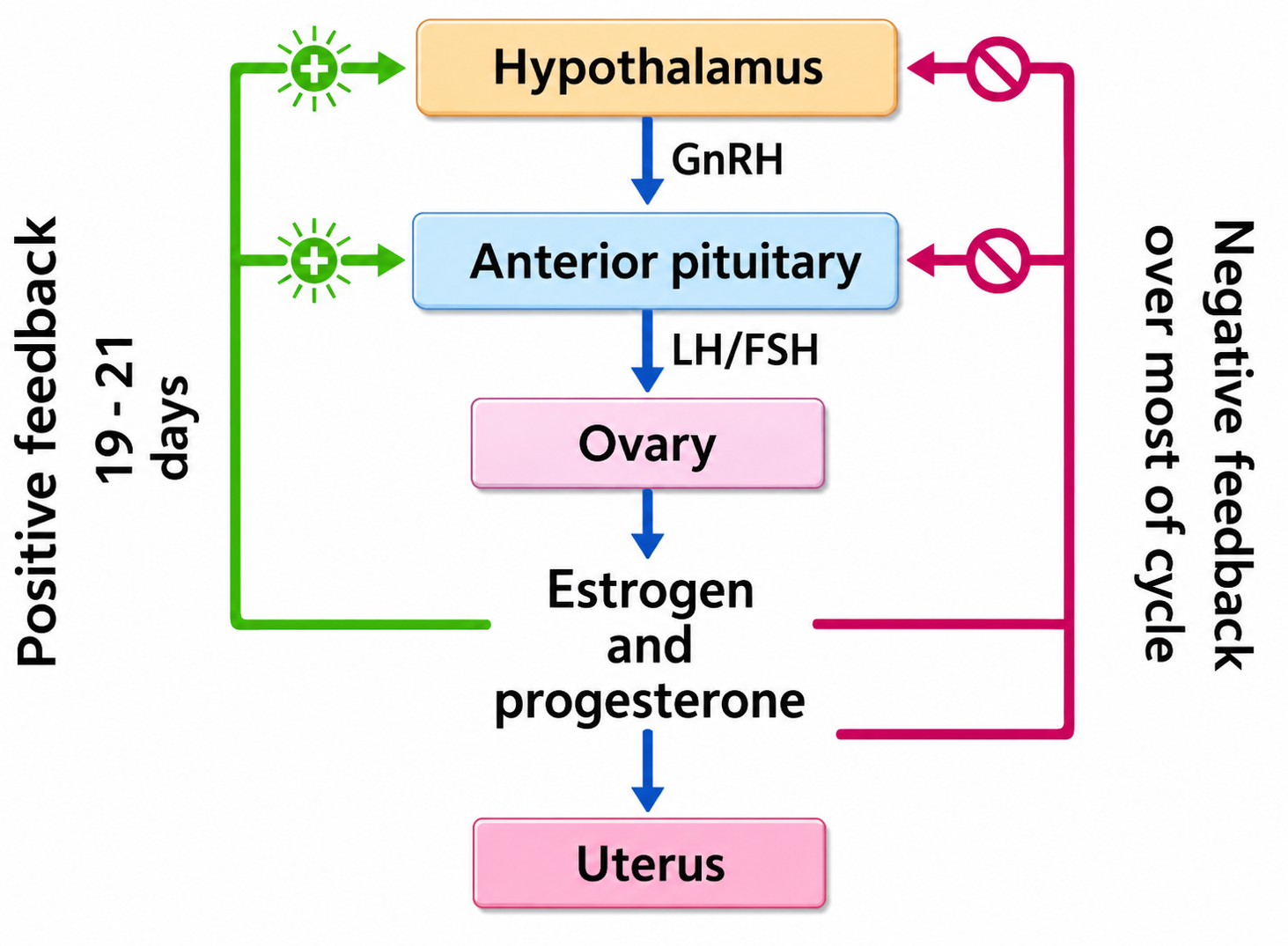
GnRH is secreted by the hypothalamus which stimulates the anterior pituitary to secrete LH and FSH
FSH —> stimulate growth of ovarian follicle , also increases the development of egg/oocyte within the follicle to complete the meosis 1 to form secondary oocyte
FSH also stimulates follicular cells in formation of estrogen
LH —→ stimulates the Corpus Leuteum to secrete progestrone and inhibin
Rising levels of progestrone & estrogen inhibit oversecretion of FSH , LH and GnRH(-ve feedback)
REPRODUCTIVE EVENTS
1) GAMETOGENESIS
Spermatogenesis
Begins at puberty
It occurs in 2 Different Stages
A) Formation of Spermatids
Multiplication Phase
Spermatogonia multiply by more and more mitotic division and increase in number(Type A and Type B)
Diploid spermatogonia undergo repeated mitosis to produce Type A cells that remain as stem cells and Type B cells that move on to become sperm.
Growth Phase
Type B spermatogonia significantly increase in size (by accumulating nourishing materials) and prepare for meiosis by transforming into primary spermatocytes.
Maturation Phase
a) Meiosis - 1
Primary spermatocyte undergoes Meiosis 1 —> formation of two haploid cells called Secondary Spermatocytes
b) Meiosis - 2
Secondary spermatocytes undergo second meiotic division to form four haploid spermatids
B) Spermiogenesis
Differentiation of spermatids to spermatozoa by the process of metamorphosis called spermiogenesis( during spermiogenesis sperm heads embed to Sertoli cells - allows the Sertoli cells to provide vital nutrients, structural support, and maturation signals)
Spermiation is the subsequent release of these mature spermatozoa from Sertoli cells into the lumen.
Spermatid → (attached to Sertoli cells during spermiogenesis) → differentiates into spermatozoa (gain nutrients from sertoli cells) and become mature spermatozoa → spermiation (release into lumen)
Oogenesis