Homeostasis
Homeostasis is the tendency for an organism or cell to maintain a constant internal environment within tolerance limits
Homeostatic mechanisms operate via feedback loops that may involve either the nervous or endocrine systems (or both)
If a physiological condition moves outside of a narrow set of tolerance limits, disease will occur as a consequence
A disease is a condition that disrupts the body's homeostatic processes, leading to a deterioration in the state of health (illness)
Internal equilibrium is maintained by adjusting a variety of physiological processes, including:
Body temperature (normally between 36 – 38ºC)
Blood pH (normally between 7.35 – 7.45)
Blood glucose levels (normally 75 – 95 mg/dL)
Blood osmotic concentrations (varies depending on individual body size)
Homeostasis
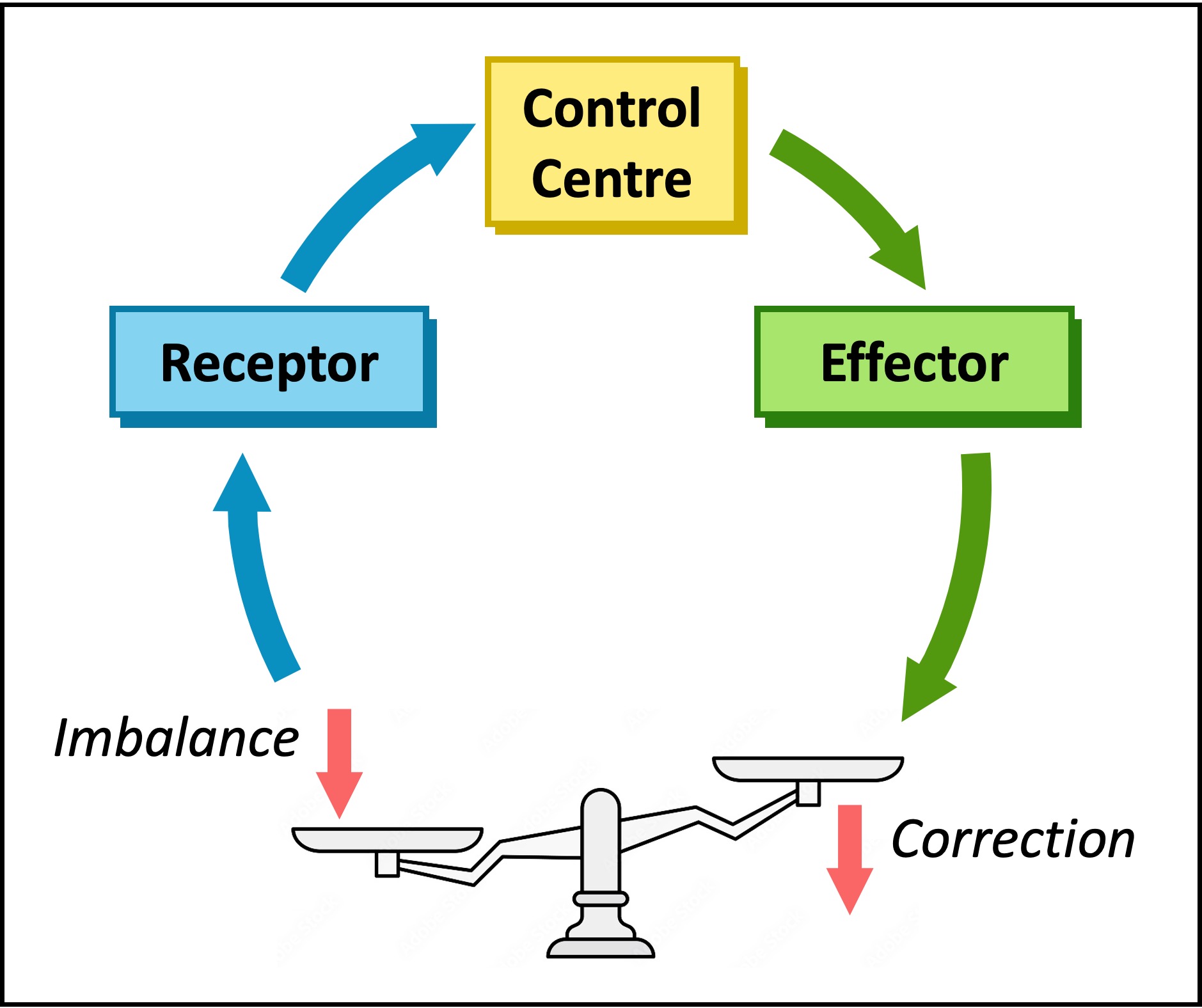
Feedback Loop
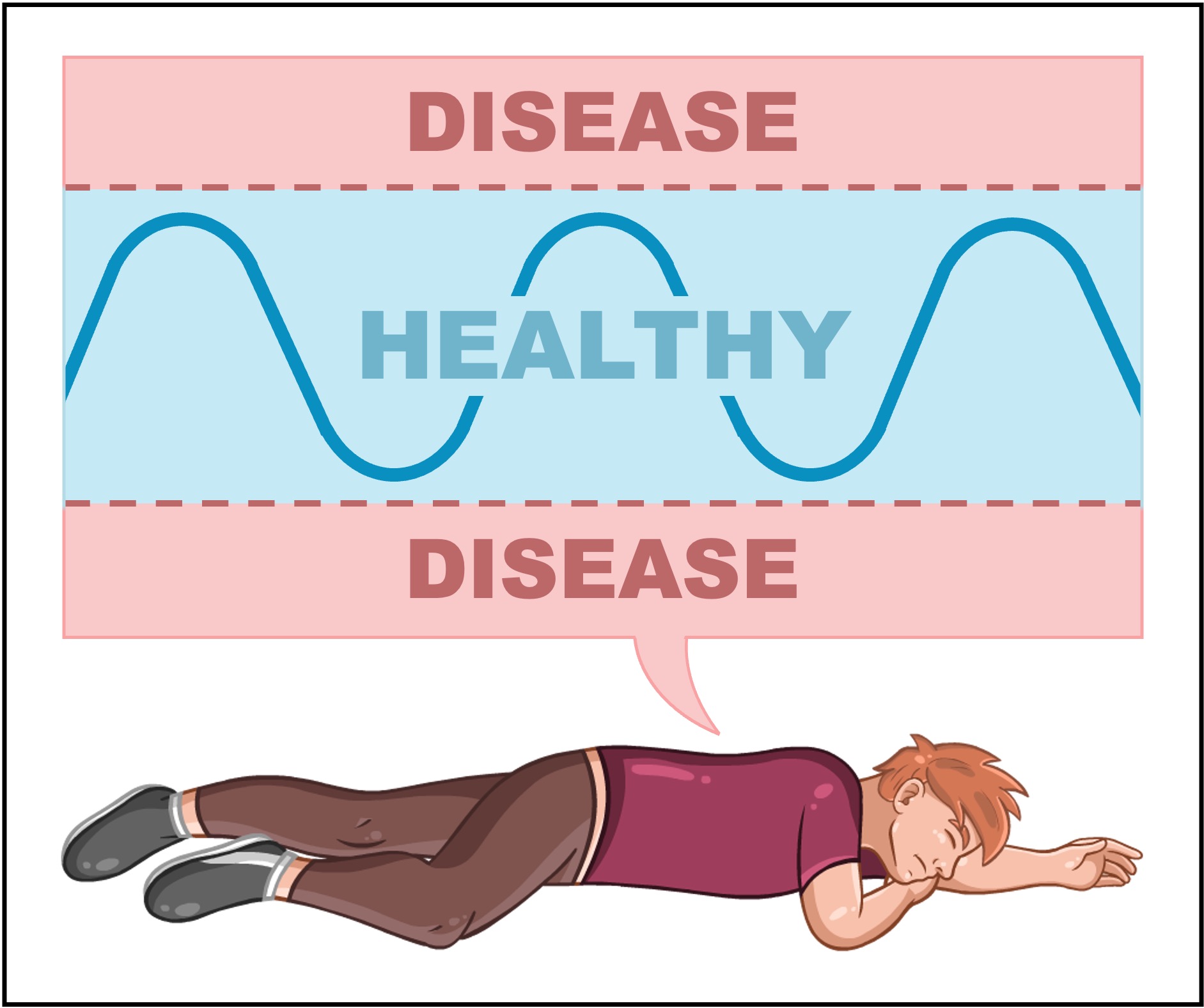
Healthy vs Diseased

D3.3.2
Negative feedback loops in homeostasis
Physiological processes are commonly moderated via two distinct feedback mechanisms – positive and negative feedback
Homeostatic processes are controlled by negative feedback and hence these systems occur more commonly within the body
Negative Feedback
Negative feedback involves a response that is the reverse of the change detected (it functions to reduce the change)
A change is detected by a receptor and an effector is activated to induce an antagonistic (opposite) effect – this promotes equilibrium
Examples of processes that utilise negative feedback loops include homeostatic systems, such as:
Thermoregulation (if body temperature changes, mechanisms are induced to restore normal levels)
Blood sugar regulation (insulin lowers blood glucose when levels are high ; glucagon raises blood glucose when levels are low)
Osmoregulation (ADH is secreted to retain water when dehydrated and its release is inhibited when the body is hydrated)
Positive Feedback
Positive feedback involves a response that reinforces the change detected (it functions to amplify the change)
Positive feedback loops will continue to amplify the initial change until the stimulus is removed – they do not promote homeostasis
Examples of processes that utilise positive feedback loops include:
Childbirth – stretching of uterine walls cause contractions that further stretch the walls (this continues until birthing occurs)
Ovulation – the dominant follicle releases oestrogen which stimulates LH and FSH release to promote further follicular growth
Lactation – the child feeding stimulates milk production which causes further feeding (continues until baby stops feeding)
The body needs glucose to make ATP (via cell respiration), however the amount required will fluctuate according to demand
High levels of glucose in the blood can damage cells (creates hypertonicity) and hence glucose levels must be regulated
Two antagonistic hormones are responsible for regulating blood glucose concentrations – insulin and glucagon
These hormones are released from pancreatic pits (called the islets of Langerhans) and act principally on the liver
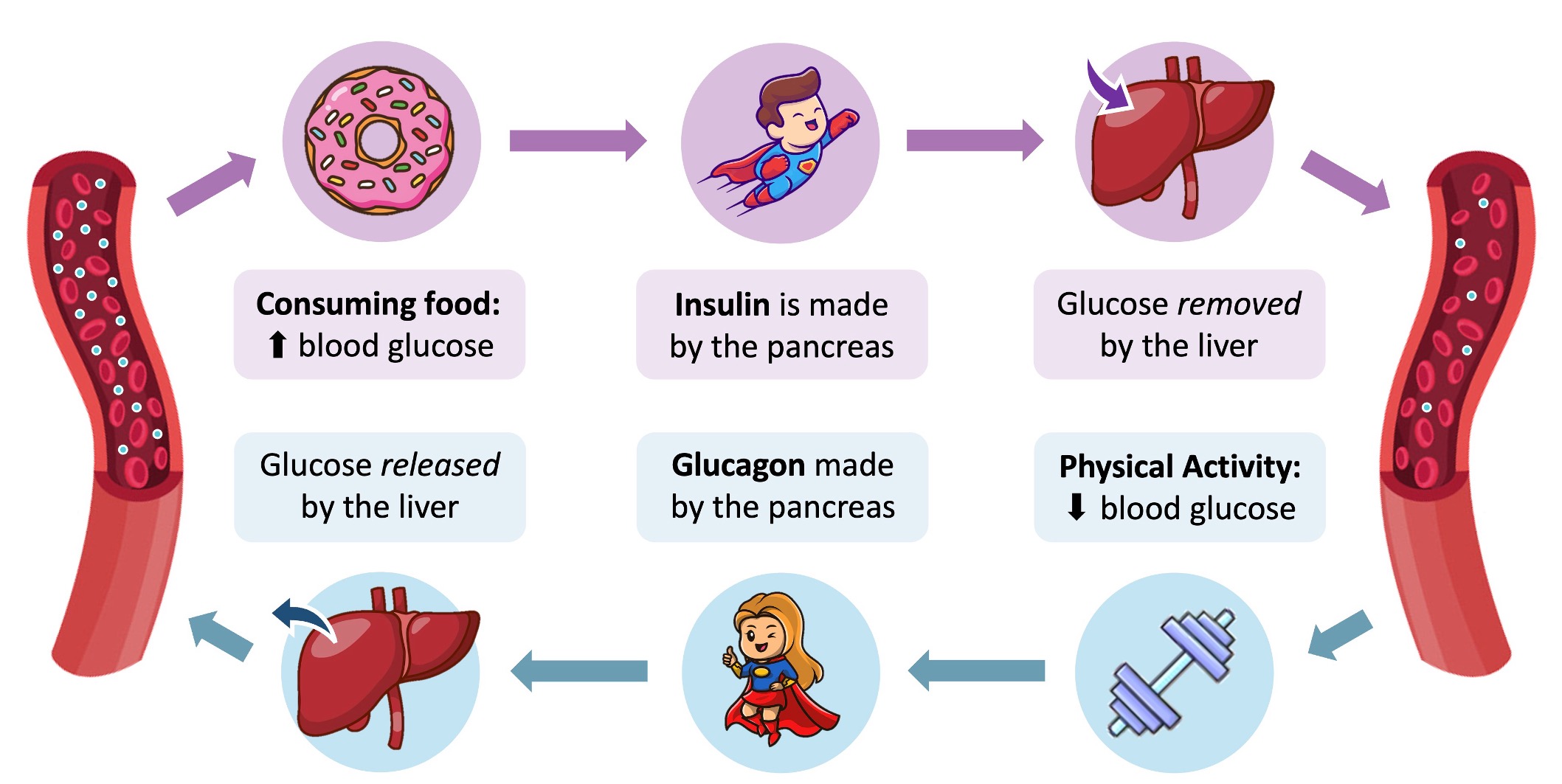
When blood glucose levels are high (e.g. after feeding):
Insulin is released from beta (β) cells of the pancreas and cause a decrease in blood glucose concentration by:
Stimulating the conversion of glucose into glycogen within the liver (glycogenesis)
Promoting glucose uptake by the liver and adipose tissue (fat)
Increasing the rate of glucose breakdown by cells (by increasing respiration rates)
When blood glucose levels are low (e.g. after exercise):
Glucagon is released from alpha (α) cells of the pancreas and cause an increase in blood glucose concentration by:
Stimulating the breakdown of glycogen into glucose within the liver (glycogenolysis)
Promoting glucose release by the liver and adipose tissue (fat)
Decreasing the rate of glucose breakdown by cells (by reducing respiration rates)
Regulating Blood Sugar Levels

D3.3.4
Physiological changes that form the basis of type 1 and type 2 diabetes
Diabetes mellitus is a metabolic disorder in which the body fails to either produce or respond to insulin – leading to high blood glucose concentrations (hyperglycaemia)
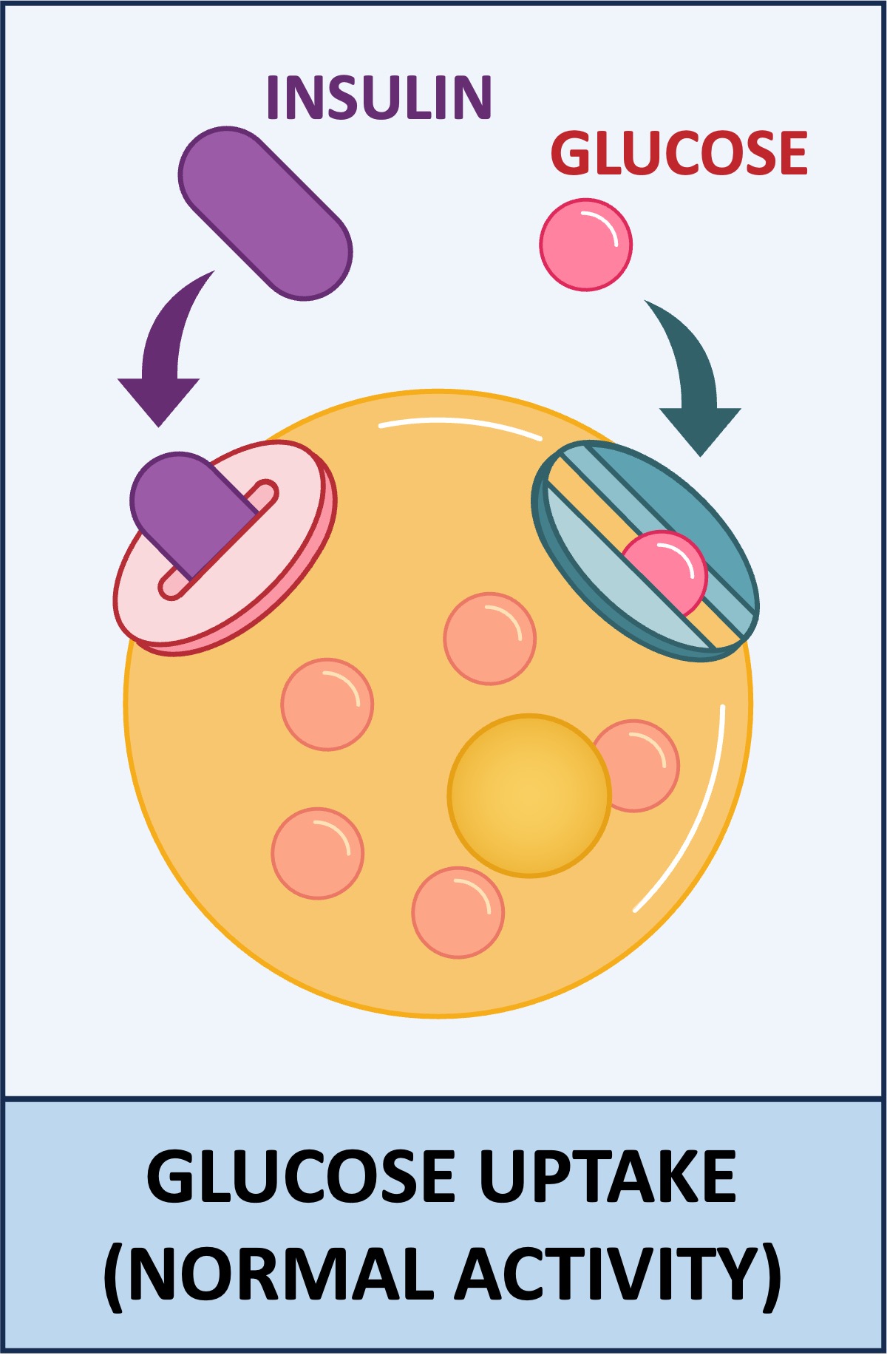
Normally, insulin binds to specific receptors on target cells and triggers the opening of glucose channels
A failure to detect or respond to insulin will prevent the opening of glucose channels, leading to the accumulation of glucose within the blood
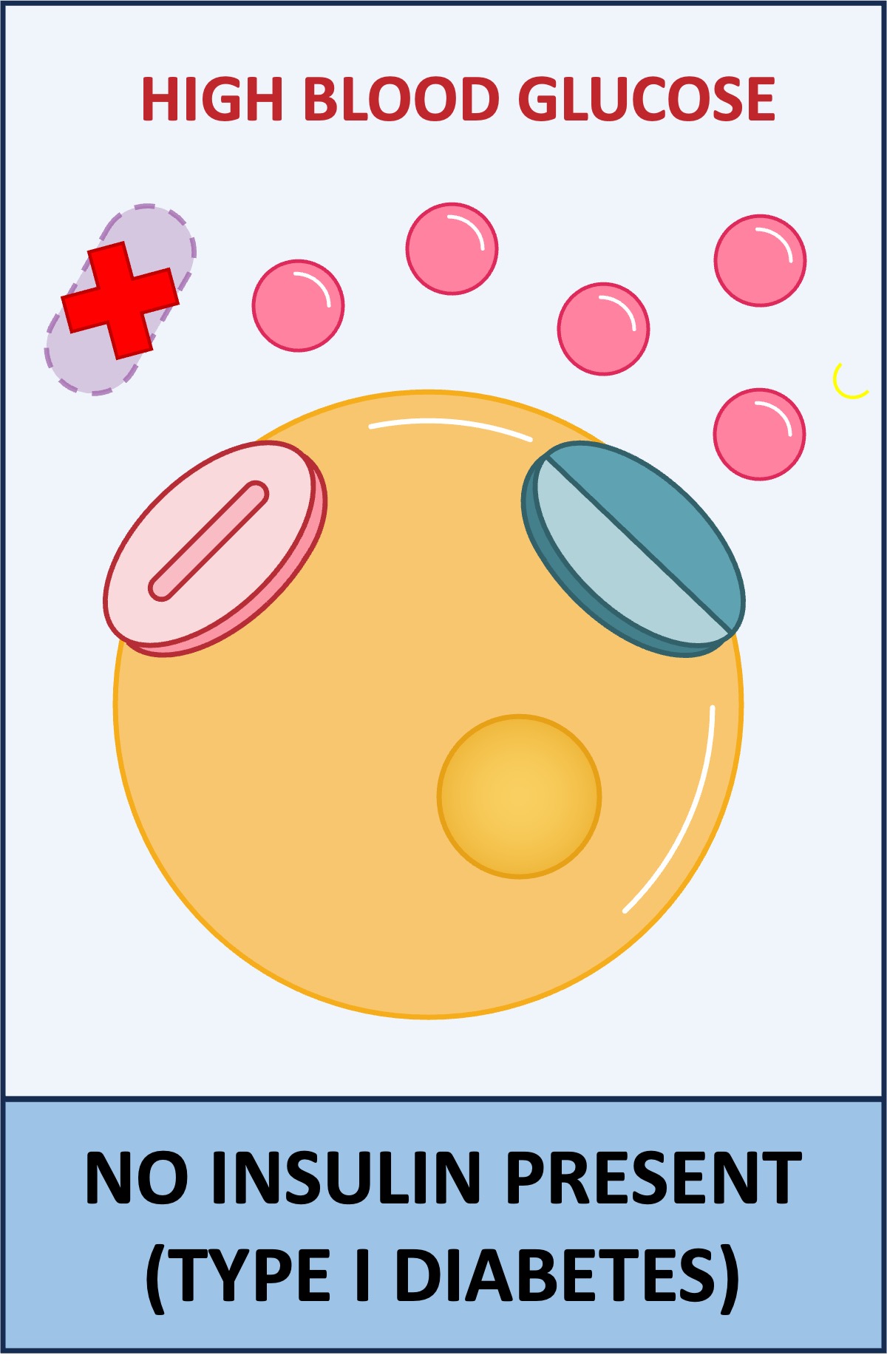
Type I Diabetes
The body does not produce sufficient levels of insulin
May be caused by the destruction of the pancreatic β-cells (via autoimmunity) and usually has an early onset (occurs during childhood)
It is treated via regular insulin injections to lower blood sugar levels (mismanagement can lead to hypoglycaemia)
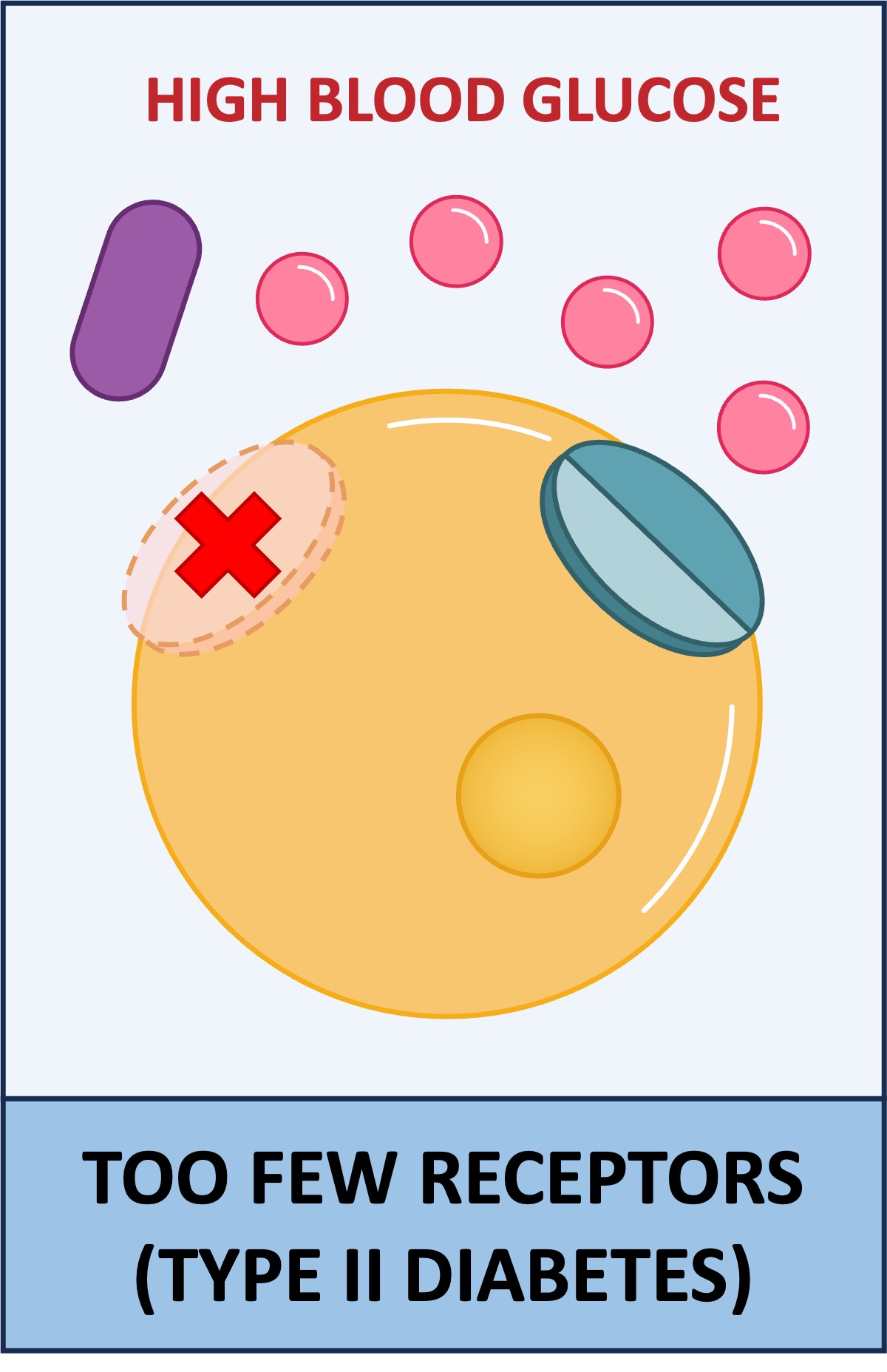
Type II Diabetes
The body does not respond to the insulin produced by the body
May be caused by the down-regulation of insulin receptors and usually has a later onset (occurs during adulthood)
It is controlled by managing an individual’s diet and lifestyle to maintain stable blood glucose levels
Type I vs Type II Diabetes
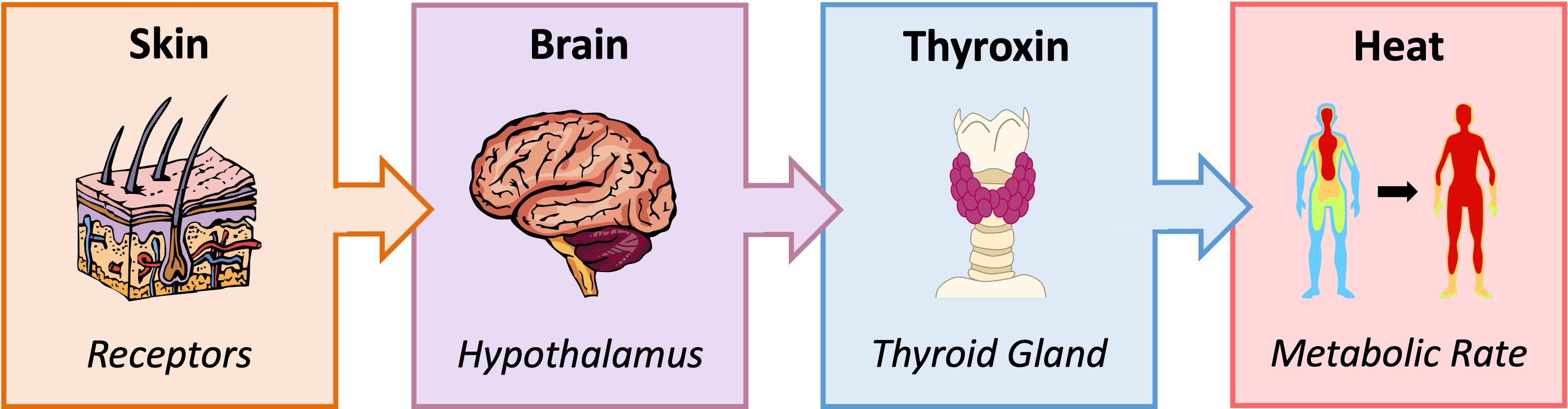
Thermoregulation describes the physiological processes by which warm-blooded animals (homeotherms) maintain a stable core body temperature
Peripheral thermoreceptors in the skin detect external temperature fluctuations and relay this information to the hypothalamus
The hypothalamus stimulates the pituitary gland to release TSH (thyroid stimulating hormone), which triggers the release of thyroxin from the thyroid gland
The primary role of thyroxin is to increase the basal metabolic rate (by stimulating carbohydrate and lipid metabolism)
A consequence of increasing metabolic activity is the production of heat – hence thyroxin helps to control body temperature
When body temperature drops, metabolic activity is increased via thyroxin to create heat and raise the core body temperature
When body temperature rises, thyroxin production is reduced to decrease metabolic activity and lower the core body temperature
Thermoregulation

D3.3.6
Thermoregulation mechanisms in humans
In addition to regulating metabolic activity, animals possess a range of other physiological and behavioural responses to maintain body temperatures
Physiological responses refer to the biological processes that regulate heat production, while behavioural responses refer to the conscious actions taken by the organism to control temperature fluctuations
Mechanisms by which homeotherms may function to heat the body if internal temperatures drop include:
Vasoconstriction – Skin arterioles constrict to move blood away from the body surface and retain the heat carried within the blood
Shivering – Muscles begin to shake in small movements, expending energy through metabolic activity (which produces heat)
Piloerection – Animals with furry coats can make their hair stand on end, trapping pockets of warm air close to the body surface
Mechanisms by which homeotherms may function to cool the body if internal temperatures rise include:
Vasodilation – Skin arterioles dilate to move blood closer to the body surface and allow for heat transfer (i.e. convective cooling)
Sweating – Sweat is released from exocrine glands, which evaporates at the cost of latent heat in the air (i.e. evaporative cooling)
Behavioural responses – Animals may physically remove themselves from warm environments in order to cool (e.g. burrowing)
Heating versus Cooling


Brown Adipose Tissue
Animals with brown adipose tissue are further capable of generating body heat via uncoupled respiration
Mitochondria possess an enzyme that synthesises ATP by using the energy released from the aerobic breakdown of organic compounds (such as carbohydrates and fats)
In brown adipose tissue an uncoupling protein is present, which prevents the released energy from being used to produce ATP
Instead, the energy is converted to heat (thermogenesis), resulting in an associated increase in body temperature
Brown fat cells have certain properties to maximise the production of heat via uncoupled respiration:
Many lipid droplets – They have multiple small lipid droplets to store large quantities of triglycerides
Many mitochondria – They have a comparatively large number of mitochondria (each with the uncoupling protein)
Circadian rhythms describe the body’s normal physiological responses to the 24 hour day-night cycle
Circadian rhythms are driven by an internal (endogenous) circadian clock, although they can be modulated by external factors
Melatonin is a hormone produced by the pineal gland within the brain and is responsible for synchronising circadian rhythms and regulating the body's sleep schedule
Melatonin is secreted in response to periods of darkness, resulting in higher concentrations at night
Light exposure to the retina is relayed to the hypothalamus, which then inhibits melatonin secretion
The hypothalamus contains a small region called the suprachiasmatic nucleus (SCN) which acts as a circadian pacemaker
Exposure to blue wavelengths of light (higher during the day) will trigger the suppression of melatonin secretion
Over a prolonged period, melatonin secretion becomes entrained to anticipate the onset of darkness and the approach of day
Melatonin functions to promote activity in nocturnal animals and conversely promotes sleep in diurnal animals (like humans)
During sleep, necessary physiological changes occur in body temperature, brain wave activity and hormonal production
Melatonin levels naturally decrease with age, leading to changes in sleeping patterns in the elderly
Modulation of Sleep Patterns
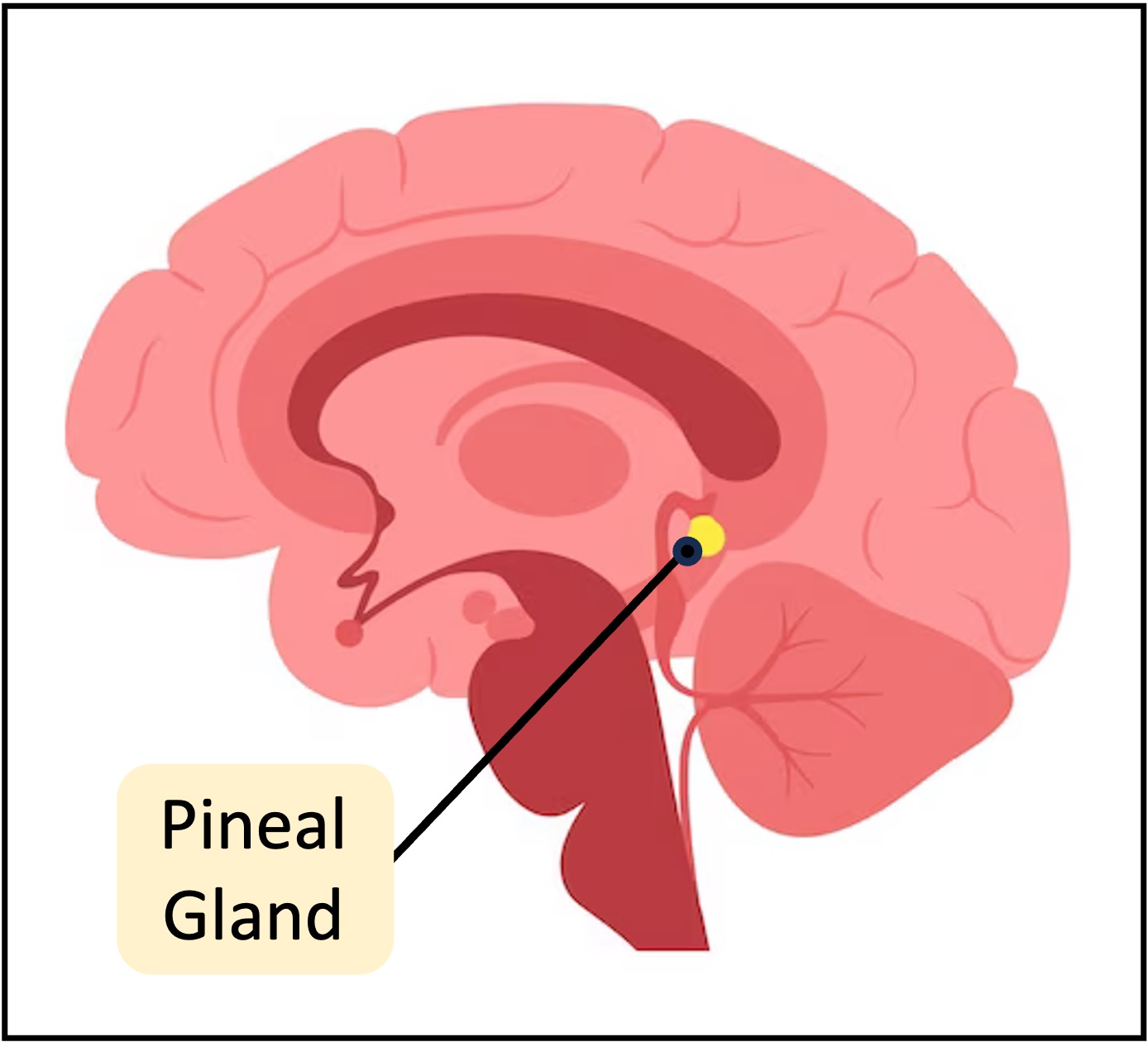
Pineal Gland
Melatonin Secretionis regulated by light exposure, with higher levels produced in darkness, which helps to signal to the body that it is time to sleep.
Exercise
The human body undergoes a number of physiological changes in order to prepare for vigorous physical activity
When exercising, the amygdala (an area of the brain involved in emotional processing) sends stress signals to the hypothalamus to initiate a ‘fight or flight’ response
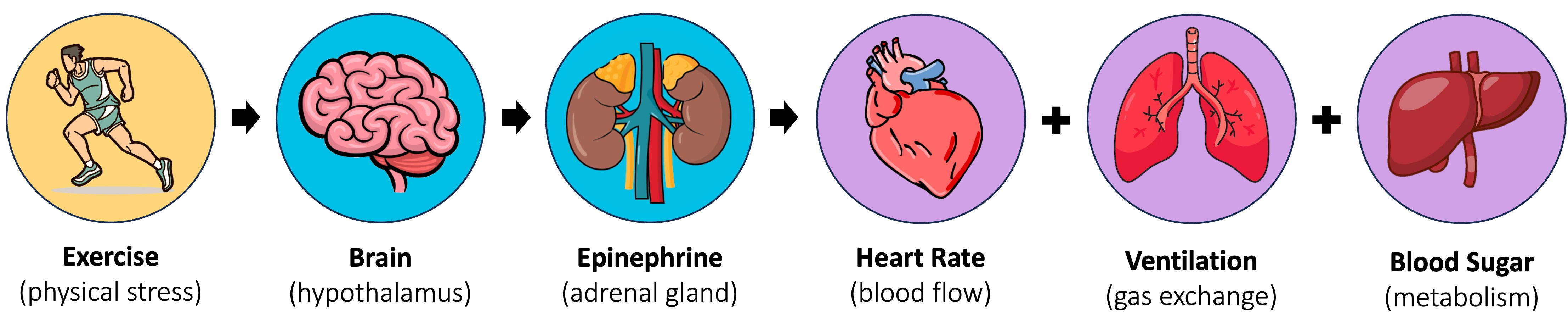
The hypothalamus will in turn stimulate the release of epinephrine (adrenaline) from the adrenal glands above the kidneys (‘epi’ = above ; ‘nephron’ = kidneys)
Epinephrine will circulate within the bloodstream and trigger a variety of physiological responses:
Heart rate will become elevated and the strength of cardiac contractions will increase – resulting in greater blood flow from the heart
Arterioles carrying blood to the skeletal muscles will dilate, while arterioles carrying blood to the kidneys and gut will constrict – redirecting blood to vital organs
Ventilation rate will also increase and the bronchioles will widen to improve the uptake of oxygen and the removal of carbon dioxide
Glucose and fats are released from storage organs (like the liver and adipose tissues) into the bloodstream, supplying energy to respiring tissues
Epinephrine Secretion

C3.1.14
Feedback control of heart rate following sensory input from baroreceptors and chemoreceptors
Blood Flow
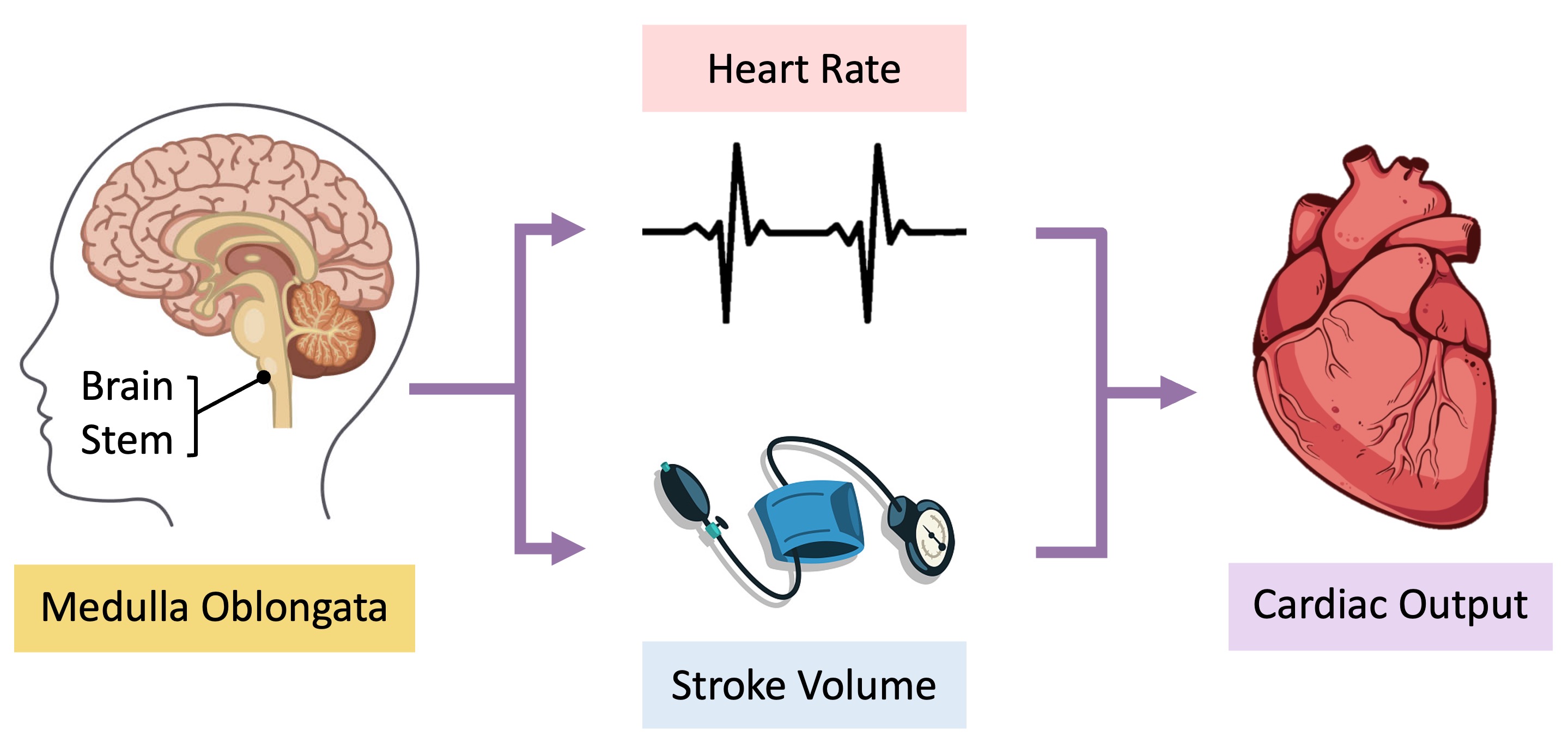
Cardiac output describes the amount of blood the heart pumps through the circulatory system in one minute
It is determined by both the heart rate (number of beats per minute) and stroke volume (amount of blood pumped per beat)
Cardiac output is autonomically controlled by the medulla oblongata (brainstem) and varies according to physiological requirements
Baroreceptors in the aortic arch and carotid sinuses detect changes in blood pressure and may trigger adjustments to either heart rate or vessel diameter
Peripheral chemoreceptors in the aorta and carotid arteries, along with central chemoreceptors in the medulla, may regulate heart rate according to changes in blood pH levels
Blood pH is affected by the composition of gases (such as oxygen and carbon dioxide) within the bloodstream
Cardiac Control Mechanisms

C3.1.15
Feedback control of ventilation rate following sensory input from chemoreceptors
Ventilation
Ventilation in humans changes in response to levels of physical activity, as the body’s energy demands are increased
ATP production (via cellular respiration) produces carbon dioxide as a waste product (and may consume oxygen aerobically)
Carbon dioxide lowers the pH of the blood (by forming carbonic acid) and this changes in pH is detected by chemosensors in the brainstem
As exercise intensity increases, so does the need for gas exchange, leading to an increase in levels of ventilation
The brainstem signals to the diaphragm and intercostal muscles within the thoracic cavity to influence ventilation in two main ways:
Increase ventilation rate (a greater frequency of breaths allows for a more continuous exchange of gases)
Increase ventilation volume (a greater volume of air taken in and out per breath allows for more gas exchange)
Respiratory Control
Ventilation Components
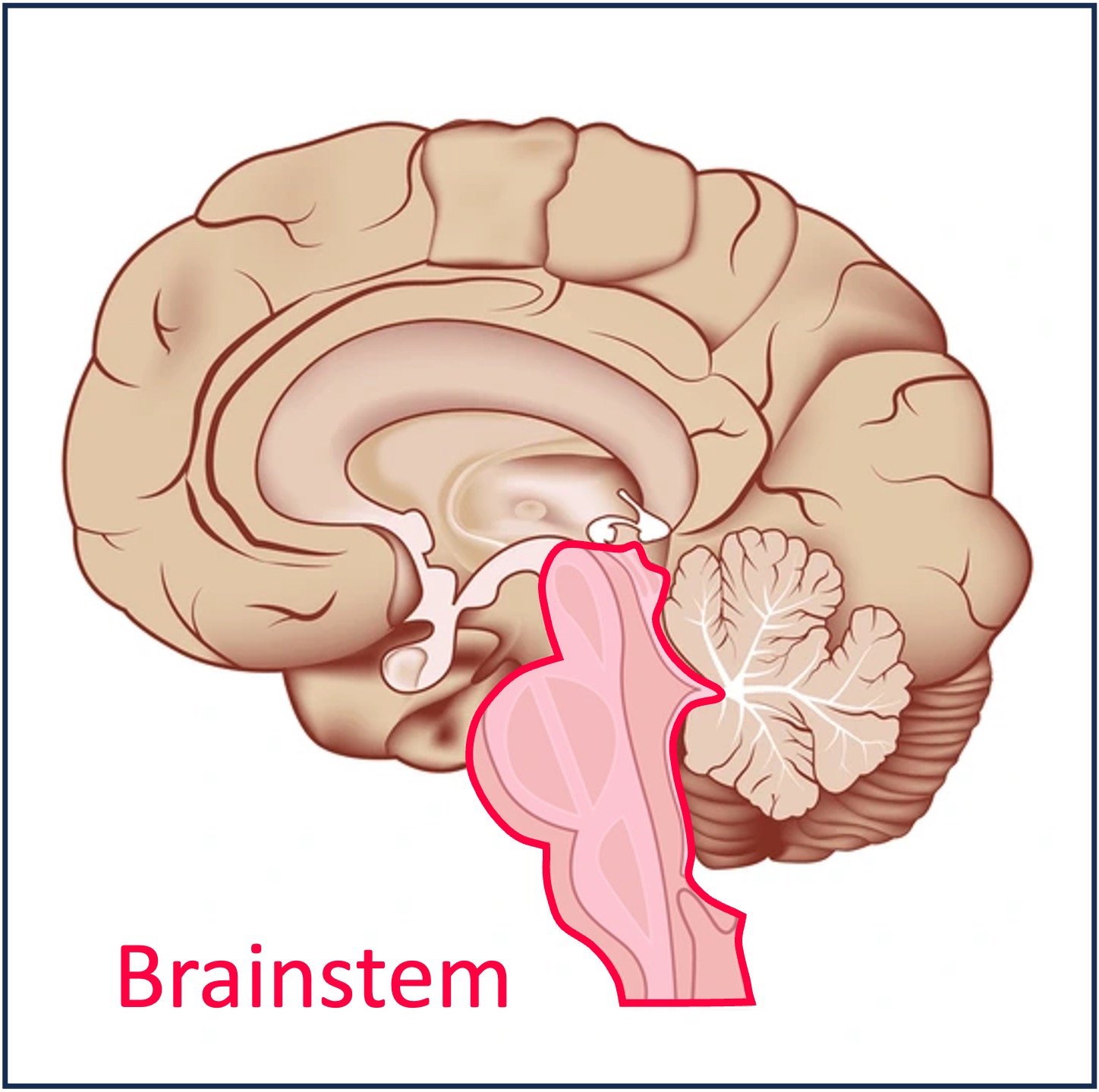
Medulla Oblongata
The medulla oblongata regulates the rhythm of breathing by sending signals to the diaphragm and intercostal muscles, ensuring that ventilation is maintained at optimal levels.
The neural pathways that coordinate digestion collectively form the enteric nervous system (enteric = ‘of the intestines’)
The enteric nervous system (ENS) involves both autonomic (involuntary) and somatic (voluntary) motor pathways
The initiation of swallowing and the egestion of faeces are under voluntary control by the CNS, however the passage of food between these points is involuntary
Peristalsis is the principal mechanism of food movement within the alimentary canal and involves the sequential contraction of longitudinal smooth muscles
This movement is autonomically controlled by the enteric nervous system to ensure the continuous movement of digested material