Chapter 18: Gas Exchange and Transport
Introduction to Gas Exchange
the body needs oxygen and removes CO2
hypoxia = too little oxygen
hypercapnia = increased concentration of CO2
to avoid these conditions, body responds to 3 regulated variables
oxygen
CO2
pH
classification of hypoxias
hypoxic, hypoxia - low arterial oxygen
caused by high altitude; alveolar hypoventilation
18.1 Gas exchange in the Lungs and Tissue
individual gases diffuse along partial pressure gradients until equilibrium
gas exchange between alveoli and blood:
PO2 alveolar air > PO2 blood
alveoli have more oxygen than blood
PO2 blood > alveolar air
venous blood has more blood than alveolar air
gas exchange between blood and tissues
PO2 blood > PO2 tissue
higher amounts of blood than tissue
PCO2 tissue > PCO2 blood
cells have more tissue than blood
Lower alveolar PO2 Decreases Oxygen Uptake
composition of inspired air
lower alveolar PO2 if inspired air = abnormally low oxygen content
higher altitudes decrease PO2
alveolar ventilation
low alveolar PO2 if ventilation is inadequate (hypoventilation)
decreased lung compliance
increased airway resistance
CNS depression:
alcohol poisoning
drug overdose
Diffusion Problems Cause Hypoxia
diffusion rate = surface area x concentration gradient x barrier permeability/distance
concentration gradient = primary factor affecting gas exchange
pathological changes that adversely affect gas exchange:
surface area
decrease in amount of alveolar surface area
diffusion (barrier permeability)
increase in thickness of alveolar membrane
diffusion distance
increase in diffusion distance between alveoli and blood
airway resistance
increase in resistance decreases ventilation
18.2 Gas Transport in the Blood
Fick equation = estimates oxygen consumption
(QO2) = CO x (Arterial [O2] - Venous[O2])
oxygen binding obeys the law of mass
increase PO2 shifts reaction to R (Hb + O2 —> HbO2)
decrease PO2 shifts reaction to L (Hb + O2 ←-HbO2)
Several Factors Affect O2-Hb binding
physiological changes alter O2-binding affinity
change in Hb O2 saturation curve reflects O2-binding affinity
shift to the right:
decreased affinity = more O2 released
represents an increase in metabolic activity (decrease PH, increase temp, increase PCO
shift to left
increased affinity = less O2 released
represents a decrease in metabolic activity (increase pH, decrease temp, decrease PCO2)
18.3 regulation of ventilation
dorsal respiratory group (DRG)
to muscles of inspiration- phrenic nerve to diaphragm
sensory input from chemoreceptors and mechanoreceptors to pons
glossopharyngeal nerve
vagus nerve
Neurons in the Medulla Control Breathing
pontine respiratory groups (PRG)
pneumotaxic center = “off” switch
controls rate and depth
apneustic = “stimulator” for inspiration
fine-tune medullary activity to produce normal, smooth respiratory patterns
ventral respiratory group (VRG)
pre-botzinger complex = basic pacemaker activity
areas for active expiration and less and normal inspiration
innervate muscles of: larynx, pharynx, tongue
VRG and DRG are both located in the medulla
18.15 neural activity during quiet breathing
cascade event
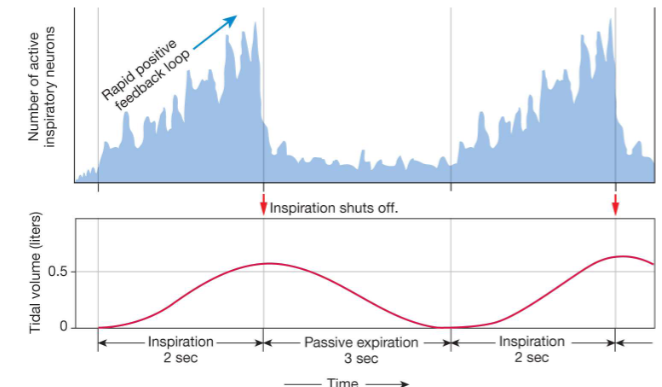
CO2, Oxygen, and pH Influence Ventilation
peripheral chemoreceptors
located in carotid bodies
senses changes
initiate increase in ventilation
- PO2 - low
- pH - low
- PCO2 - high
O2 must be <60 mm Hg to trigger reflex at a certain level
central chemoreceptors
located in medulla
responds to changes in PCO2
arterial increase PCO2, CO crosses into the brain ECF
CO2 is converted bicarbonate and H+
H+ is actually detected
Protective Reflexes Guard the Lungs
response to physical injury, irritation, and over inflation
bronchoconstriction- irritant receptors in airway mucosa send signals through sensory neurons
Hering Breur inflation reflex
prevents over-inflation of lungs
activated by pulmonary stretch receptors
travels via vagus nerve to brainstem
Higher Brain Centers Affect Patterns of Ventilation
we can control how we breath
cerebrum and hypothalamus can change brainstem breath rate and depth
higher brain center control is not a requirement for ventilation
Limbic system (emotion)- bypasses brain stem
cannot override chemoreceptor reflexes