BIO122 WK1 Pharmacokinetics
Pharmacokinetics: the effect of the body of a drug of choice
Absorption/ Distribution
Absorption is the passage of a drug from its site of administration into the bloodstream.
BIO121 Wk1 and 2, Molecular Transfusion
The route of administration affects the speed of absorption: site can be chosen for efficiency
- IV administration puts the drug directly into the bloodstream for the fastest absorption.
- Oral and transdermal routes require the drug to cross more cell membranes, resulting in slower absorption.
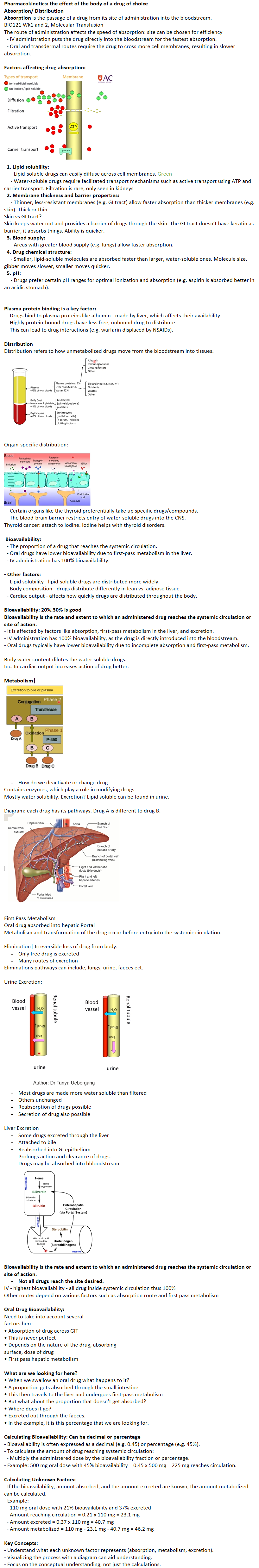
Factors affecting drug absorption:
1. Lipid solubility:
- Lipid-soluble drugs can easily diffuse across cell membranes. Green
- Water-soluble drugs require facilitated transport mechanisms such as active transport using ATP and carrier transport. Filtration is rare, only seen in kidneys
2. Membrane thickness and barrier properties:
- Thinner, less-resistant membranes (e.g. GI tract) allow faster absorption than thicker membranes (e.g. skin). Thick or thin.
Skin vs GI tract?
Skin keeps water out and provides a barrier of drugs through the skin. The GI tract doesn’t have keratin as barrier, it absorbs things. Ability is quicker.
3. Blood supply:
- Areas with greater blood supply (e.g. lungs) allow faster absorption.
4. Drug chemical structure:
- Smaller, lipid-soluble molecules are absorbed faster than larger, water-soluble ones. Molecule size, gibber moves slower, smaller moves quicker.
5. pH:
- Drugs prefer certain pH ranges for optimal ionization and absorption (e.g. aspirin is absorbed better in an acidic stomach).
Plasma protein binding is a key factor:
- Drugs bind to plasma proteins like albumin - made by liver, which affects their availability.
- Highly protein-bound drugs have less free, unbound drug to distribute.
- This can lead to drug interactions (e.g. warfarin displaced by NSAIDs).
Distribution
Distribution refers to how unmetabolized drugs move from the bloodstream into tissues.
Organ-specific distribution:
- Certain organs like the thyroid preferentially take up specific drugs/compounds.
- The blood-brain barrier restricts entry of water-soluble drugs into the CNS.
Thyroid cancer: attach to iodine. Iodine helps with thyroid disorders.
Bioavailability:
- The proportion of a drug that reaches the systemic circulation.
- Oral drugs have lower bioavailability due to first-pass metabolism in the liver.
- IV administration has 100% bioavailability.
- Other factors:
- Lipid solubility - lipid-soluble drugs are distributed more widely.
- Body composition - drugs distribute differently in lean vs. adipose tissue.
- Cardiac output - affects how quickly drugs are distributed throughout the body.
Bioavailability: 20%,30% is good
Bioavailability is the rate and extent to which an administered drug reaches the systemic circulation or site of action.
- It is affected by factors like absorption, first-pass metabolism in the liver, and excretion.
- IV administration has 100% bioavailability, as the drug is directly introduced into the bloodstream.
- Oral drugs typically have lower bioavailability due to incomplete absorption and first-pass metabolism.
Body water content dilutes the water soluble drugs.
Inc. In cardiac output increases action of drug better.
Metabolism|
How do we deactivate or change drug
Contains enzymes, which play a role in modifying drugs.
Mostly water solubility. Excretion? Lipid soluble can be found in urine.
Diagram: each drug has its pathways. Drug A is different to drug B.
First Pass Metabolism
Oral drug absorbed into hepatic Portal
Metabolism and transformation of the drug occur before entry into the systemic circulation.
Elimination| Irreversible loss of drug from body.
Only free drug is excreted
Many routes of excretion
Eliminations pathways can include, lungs, urine, faeces ect.
Urine Excretion:
Most drugs are made more water soluble than filtered
Others unchanged
Reabsorption of drugs possible
Secretion of drug also possible
Liver Excretion
Some drugs excreted through the liver
Attached to bile
Reabsorbed into GI epithelium
Prolongs action and clearance of drugs.
Drugs may be absorbed into bbloodstream
Bioavailability is the rate and extent to which an administered drug reaches the systemic circulation or site of action.
Not all drugs reach the site desired.
IV - highest bioavailability - all drug inside systemic circulation thus 100%
Other routes depend on various factors such as absorption route and first pass metabolism
Oral Drug Bioavailability:
Need to take into account several
factors here
• Absorption of drug across GIT
• This is never perfect
• Depends on the nature of the drug, absorbing
surface, dose of drug
• First pass hepatic metabolism
What are we looking for here?
• When we swallow an oral drug what happens to it?
• A proportion gets absorbed through the small intestine
• This then travels to the liver and undergoes first-pass metabolism
• But what about the proportion that doesn’t get absorbed?
• Where does it go?
• Excreted out through the faeces.
• In the example, it is this percentage that we are looking for.
Calculating Bioavailability: Can be decimal or percentage
- Bioavailability is often expressed as a decimal (e.g. 0.45) or percentage (e.g. 45%).
- To calculate the amount of drug reaching systemic circulation:
- Multiply the administered dose by the bioavailability fraction or percentage.
- Example: 500 mg oral dose with 45% bioavailability = 0.45 x 500 mg = 225 mg reaches circulation.
Calculating Unknown Factors:
- If the bioavailability, amount absorbed, and the amount excreted are known, the amount metabolized can be calculated.
- Example:
- 110 mg oral dose with 21% bioavailability and 37% excreted
- Amount reaching circulation = 0.21 x 110 mg = 23.1 mg
- Amount excreted = 0.37 x 110 mg = 40.7 mg
- Amount metabolized = 110 mg - 23.1 mg - 40.7 mg = 46.2 mg
Key Concepts:
- Understand what each unknown factor represents (absorption, metabolism, excretion).
- Visualizing the process with a diagram can aid understanding.
- Focus on the conceptual understanding, not just the calculations.