Chapter 14: The Somatic Nervous System Study Guide
Ch 14.1 Sensory Perception
Sensory receptors play a major role in helping organisms learn about the surrounding environment and the state of the internal environment.
Stimuli from varying sources and of different types are received and changed into the electrochemical signals of the nervous system.
The Process of Sensation
This transformation occurs when a stimulus changes the cell membrane potential of a sensory neuron.
The stimulus causes the sensory cell to produce an action potential that is relayed into the central nervous system (CNS).
Integration in the CNS combines sensory information with other data or higher cognitive functions to create a conscious perception of that stimulus.
Central integration may eventually lead to a motor response.
Sensation vs. Perception
Sensation: The activation of sensory receptor cells at the level of the stimulus.
Perception: The central processing of sensory stimuli into a meaningful pattern.
Perception depends on sensation, but not all sensations are perceived.
Receptor Mechanisms
Receptor Cells: The cells or structures that detect sensations. A receptor cell is changed directly by a stimulus.
Transmembrane Protein Receptor: A protein in the cell membrane mediating physiological changes in a neuron,
most often through the opening of ion channels or changes in cell signaling processes.
These receptors are often activated by chemicals called ligands (e.g., molecules in food for taste).
Physical Sensitivity: Other transmembrane proteins (not strictly called receptors) respond to mechanical or thermal changes.
Physical alterations in these proteins increase ion flow across the membrane, generating an action potential or a graded potential in the sensory neurons.
Sensory Receptors
Stimuli in the environment activate specialized cells in the PNS, and different types of stimuli are sensed by different types of receptor cells.
Classification of Sensory Receptors
Sensory receptors can be classified based on 3 different criteria:
cell type,
position,
and function
They are classified functionally on the basis of the transduction of stimuli, or how the mechanical stimulus, light, or chemical changes the cell membrane potential.
Structural Receptor Cell Type
The cells that interpret information about the environment can be classified into 3 structural types:
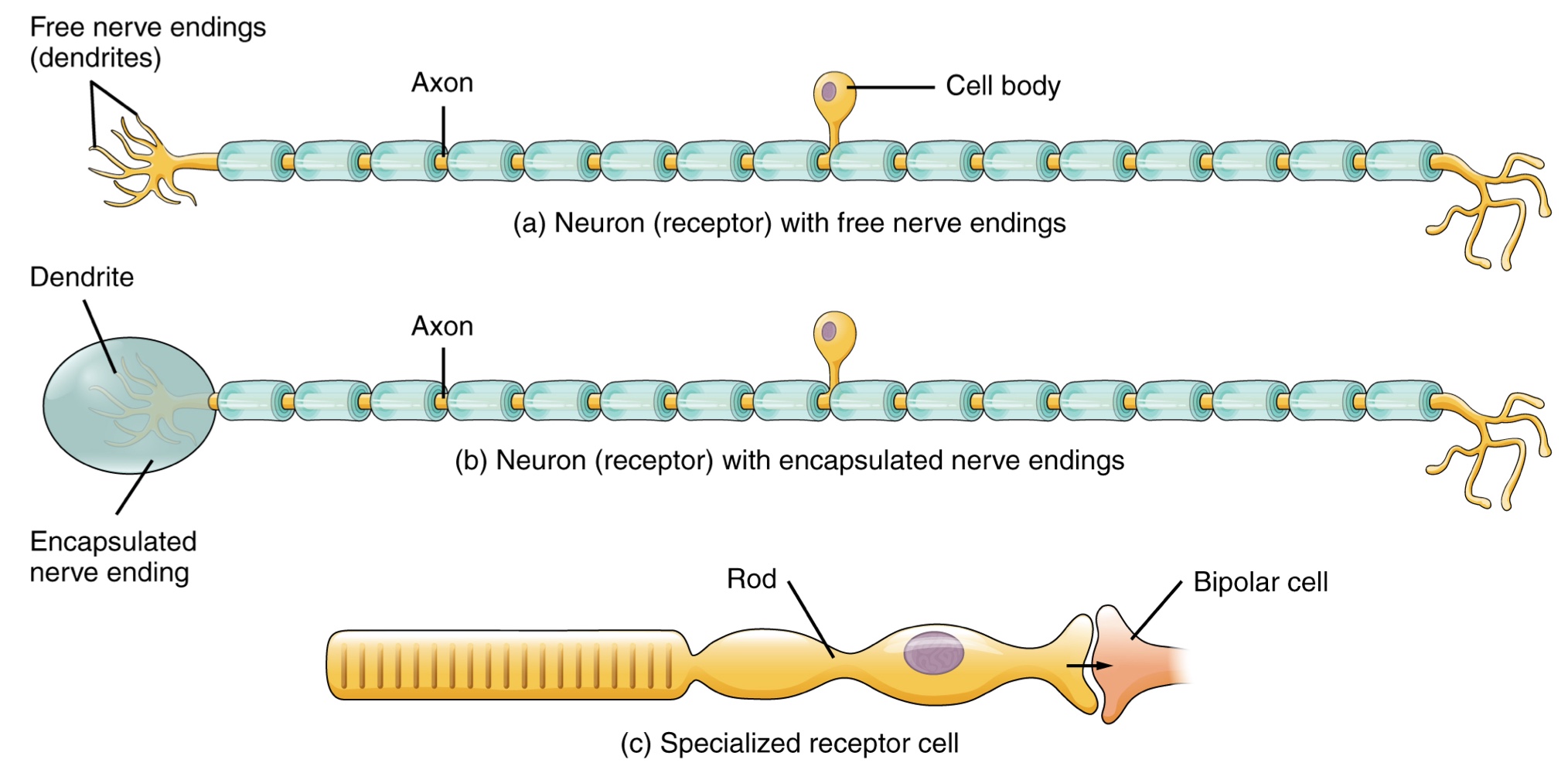
Free Nerve Ending
A neuron with dendrites embedded in tissue that would receive a sensation.
Examples include the pain and temperature receptors in the dermis of the skin.
Encapsulated Ending
A neuron where the sensory nerve endings are encapsulated in connective tissue that enhances their sensitivity.
Examples include lamellated corpuscles in the dermis that respond to pressure and touch.
Specialized Receptor Cell
Possesses distinct structural components that interpret a specific type of stimulus.
An example is a photoreceptor in the retina that responds to light stimuli.
Position (location) Classification of Sensory Receptors
Sensory receptors can also be classified based on 3 different criteria: cell type, position (location), and function.
Classification Based on Location
Exteroceptor: A receptor located near a stimulus in the external environment,
such as the somatosensory receptors found in the skin.
Interoceptor: A receptor that interprets stimuli from internal organs and tissues,
such as the receptors that sense an increase in blood pressure in the aorta or carotid sinus.
Proprioceptor: A receptor located near a moving part of the body,
such as a muscle, that interprets the positions of the tissues as they move.
Functional Classification Receptor Type
The third classification of receptors is by how the receptor transduces stimuli into membrane potential changes.
Stimuli are of 3 general types:
Chemical Stimuli: Ions and macromolecules that affect transmembrane receptor proteins when these chemicals diffuse across the cell membrane.
Physical Variations: Environmental changes (mechanical or thermal) that affect receptor cell membrane potentials.
Electromagnetic Radiation: Radiation such as visible light. While humans only perceive visible light, other organisms may have receptors for heat (snakes), ultraviolet light (bees), or magnetic fields (migratory birds).
Categories by Stimulus Type
Receptor cells can be further categorized on the basis of the type of stimuli they transduce.
Chemoreceptor: Interprets chemical stimuli, such as an object’s taste or smell.
Osmoreceptor: Responds to solute concentrations of body fluids.
Nociceptor: Interprets pain, primarily through the presence of chemicals from tissue damage or similar intense stimuli.
Mechanoreceptor: Responds to physical stimuli such as pressure and vibration, as well as the sensation of sound and body position (balance).
Thermoreceptor: Sensitive to temperatures above (heat) or below (cold) normal body temperature.
Sensory Modalities
The way that information is encoded is referred to as a sensory modality.
Modality refers to the way information is encoded, which is similar to the idea of transduction.
While the five major senses—taste, smell, touch, hearing, and sight—are well known, they are not exhaustive.
Other senses include balance and subdivisions of touch like pressure, vibration, stretch, and hair-follicle position
These are on the basis of the type of mechanoreceptors that perceive these touch sensations
Other overlooked senses include temperature perception by thermoreceptors and pain perception by nociceptors.
General vs. Special Senses
Senses can be categorized as either general or specific
General Sense: One that is distributed throughout the body and has receptor cells within the structures of other organs.
Examples include mechanoreceptors in the skin, muscles, or blood vessel walls.
General senses often contribute to sense of touch, proprioception (body movement), kinesthesia (body movement), or visceral sense (autonomic functions).
Special Sense: One that has a specific organ devoted to it, namely the eye, inner ear, tongue, or nose.
The main sensory modalities can be described on basis of how each is transduced.
(Refer to categories by stimuli type.)
Submodalities
Listing all different sensory modalities, which can be as many as 17, involves separating the five major senses into more specific categories, or submodalities, of the larger sense.Each individual sensory modality represents the sensation of a specific type of stimuli.
For example, somatosensation (the general sense of touch) can be separated into:
Light pressure
Deep pressure
Vibration
Gustation (Taste)
Only a few recognized submodalities exist within the special sense of taste, or gustation. Associated with the tongue.
Anatomical Structures of the Tongue:
The surface of the tongue and the oral cavity are lined with a stratified squamous epithelium.
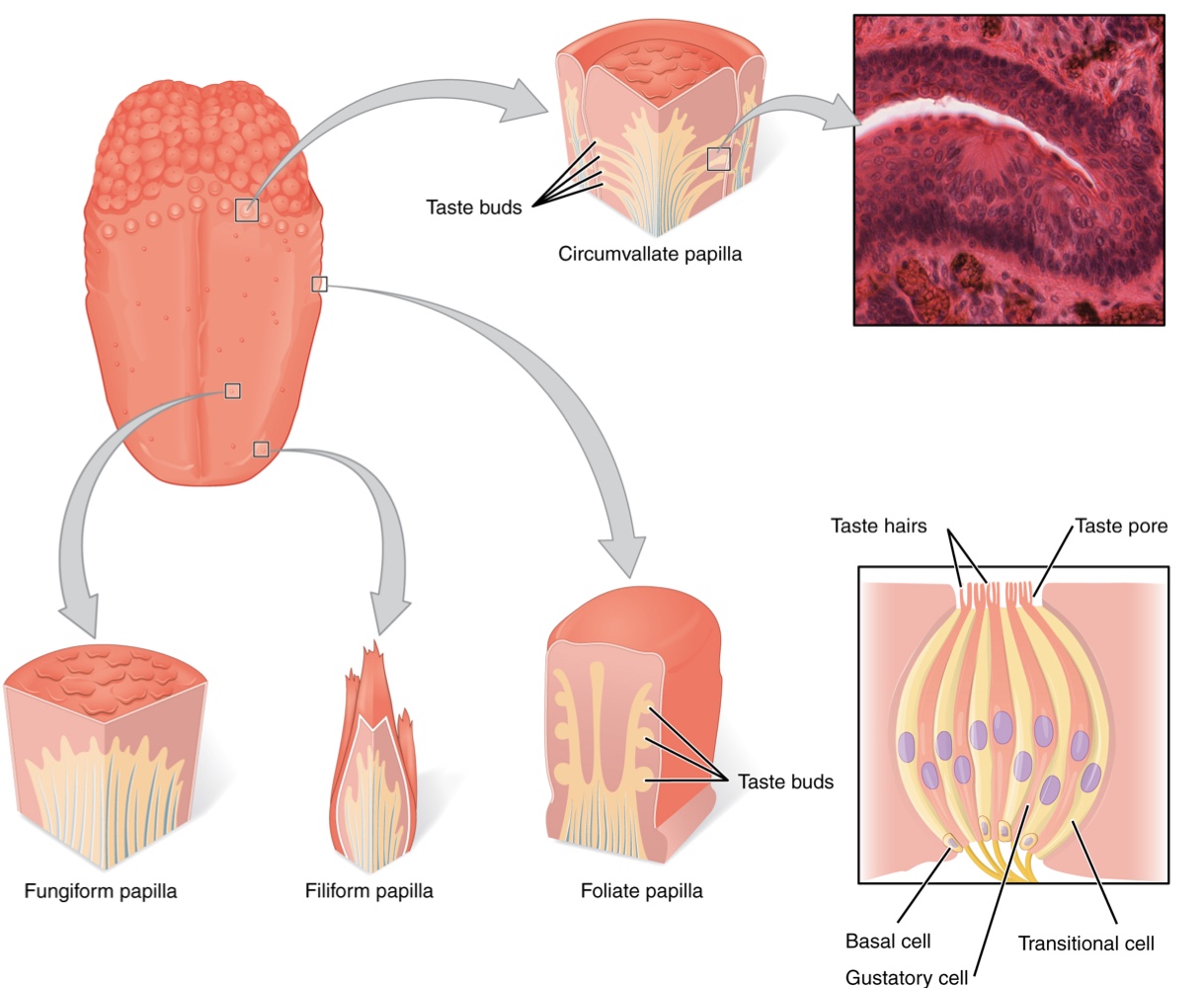
Papillae: These are raised bumps on the tongue that contain the structures for gustatory transduction.
There are 4 types based on appearance: circumvallate, foliate, filiform, and fungiform.
Taste Buds: Found within the structure of the papillae, taste buds contains specialized gustatory receptor cells responsible for transducing taste stimuli.
These receptor cells are sensitive to the chemicals contained within foods that are ingested, and they release neurotransmitters based on the amount of the chemical in the food.
Neurotransmitters from the gustatory cells can activate sensory neurons in the facial, glossopharyngeal, and vagus cranial nerves.
Primary Tastes:
Historically, only 4 tastes were recognized: sweet, salty, sour, and bitter.
Umami: Research at the turn of the 20th century led to the recognition of this fifth taste during the mid-1980s.
It is a Japanese word meaning "delicious taste," often translated as savory.
Recent research suggests a possible 6th taste for fats (lipids).
Transduction of Primary Tastes
Salty: The perception of sodium ions (Na+) in the saliva.
Salt crystals dissociate into Na+ and Cl−, which dissolve into the saliva in your mouth.
The Na+ concentration becomes high outside the gustatory cells, creating a high concentration gradient that drives the diffusion of Na+ into gustatory cells.
This leads to the depolarization of the cell membrane and the generation of a receptor potential.
Sour: The perception of hydrogen ion (H+) concentration, representing the acidity of food.
H+ ions enter the cell and trigger depolarization.
Higher H+ concentrations (lower saliva pH) result in progressively stronger graded potentials.
Sweet: Triggered by food molecules (e.g., glucose or artificial sweeteners like aspartame, saccharine, or sucralose) binding to a G protein-coupled receptor.
A G protein signal transduction system ultimately leads to a depolarizes the gustatory cell.
The affinity for each of these molecules varies and some will taste sweeter than glucose because they bind to the G-protein-coupled receptor differently.
Bitter: Also involves molecules binding to G protein-coupled receptors,
but with a high diversity of response mechanisms due to the wide range of bitter molecules.
Some molecules depolarize gustatory cells, while others hyperpolarize them.
Alkaloids: Nitrogen-containing molecules (e.g., coffee, hops, tea, aspirin) that are common in bitter plant products.
By containing toxic alkaloids, plants are less attractive to herbivores.
Likewise some bitter molecules increase G protein activation within the gustatory cells, whereas others decrease activation.
Protective Role: Bitter taste is primarily associated with stimulating the gag reflex to avoid ingesting poisons.
The highest concentration of bitter receptors is located in the posterior tongue. Where a gag reflex could still spit out poisonous food.
Umami: Known as the savory taste, it is based on the activation of G protein-coupled receptors by the amino acid L-glutamate.
It is frequently associated with protein-rich foods and meat.
Anatomical Structures of the Tongue
The surface of the tongue and the oral cavity are lined with a stratified squamous epithelium.
Papillae: Raised bumps containing the structures for gustatory transduction.
There are 4types: circumvallate, foliate, filiform, and fungiform.
Taste Buds: Found within the papillae, these contain specialized gustatory receptor cells responsible for transducing taste stimuli.
Signal Transmission
Activated gustatory receptor cells release neurotransmitters onto the dendrites of sensory neurons.
These neurons belong to specific cranial nerves categorized by their location on the tongue:
Facial Nerve (CN VII): Connects to taste buds in the anterior third of the tongue.
Glossopharyngeal Nerve (CN IX): Connects to taste buds in the posterior two-thirds of the tongue.
Vagus Nerve (CN X): Connects to taste buds in the extreme posterior tongue and pharynx. This nerve is highly sensitive to noxious stimuli (bitterness) and is dedicated to the gag reflex.
Olfaction (Smell)
Like taste, the sense of smell, or olfaction, is also responsive to chemical stimuli.
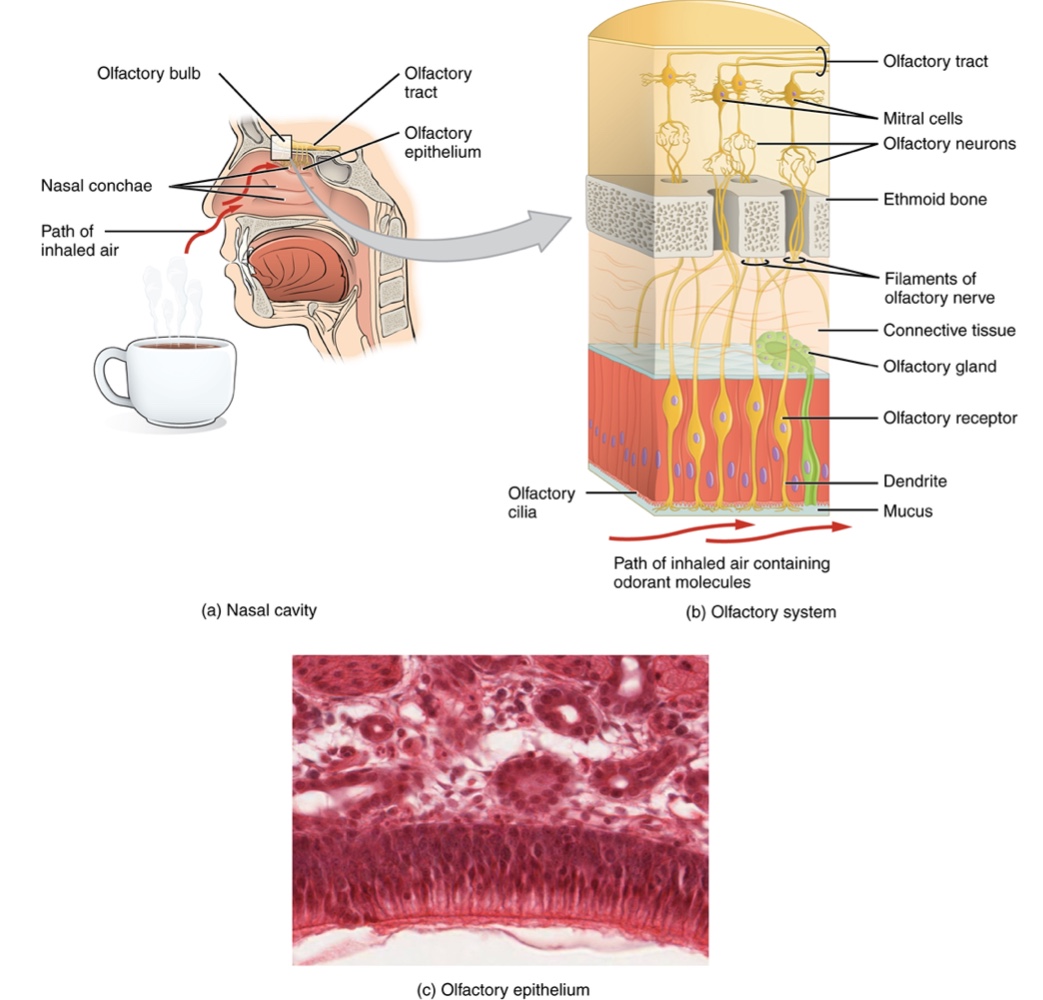
Olfactory Epithelium: Olfactory receptor neurons located in a small region within the superior nasal cavity that contains bipolar sensory neurons.
Olfactory Sensory Neurons:
Each neuron has dendrites that extend from the apical surface of the epithelium into the mucus lining the cavity.
Odorant Molecules: As these airborne molecules are inhaled through the nose, they pass over the olfactory epithelial region and dissolve into the mucus
they then bind to proteins that keep them dissolved in the mucus and help transport them to the olfactory dendrites.
The odorant-protein complex binds to a G protein-coupled receptor protein within the cell membrane of the dendrite.
This activation produces a graded membrane potential in the olfactory neurons.
Pathway to the Brain:
Axons extend from the basal surface of the epithelium, through the olfactory foramen in the cribriform plate of the ethmoid bone and into the brain.
Olfactory Tract: A group of axons that connect to the olfactory bulb located on the ventral surface of the frontal lobe.
From the bulb, axons split to travel to different regions:
Primary Olfactory Cortex: Located in the inferior and medial areas of the temporal lobe in the cerebrum.
Limbic System and Hypothalamus: Where smells associate with long-term memory and emotional responses.
Unique Characteristic: Olfaction is the only sensory modality that does not synapse in the thalamus before connecting to the cerebral cortex.
This intimate connection between the olfactory system and the cerebral cortex is one reason why smell can be a potent trigger of memories and emotion.
Neuronal Regeneration:
Olfactory neurons are regularly replaced because they are susceptible to damage from airborne toxic chemicals.
New axons grow along the path of existing axons in the cranial nerve to reconnect correctly with the olfactory bulb.
Audition, or hearing, is the transduction of sound waves into a neural signal made possible by the various structures of the ear.
The Ear Structure
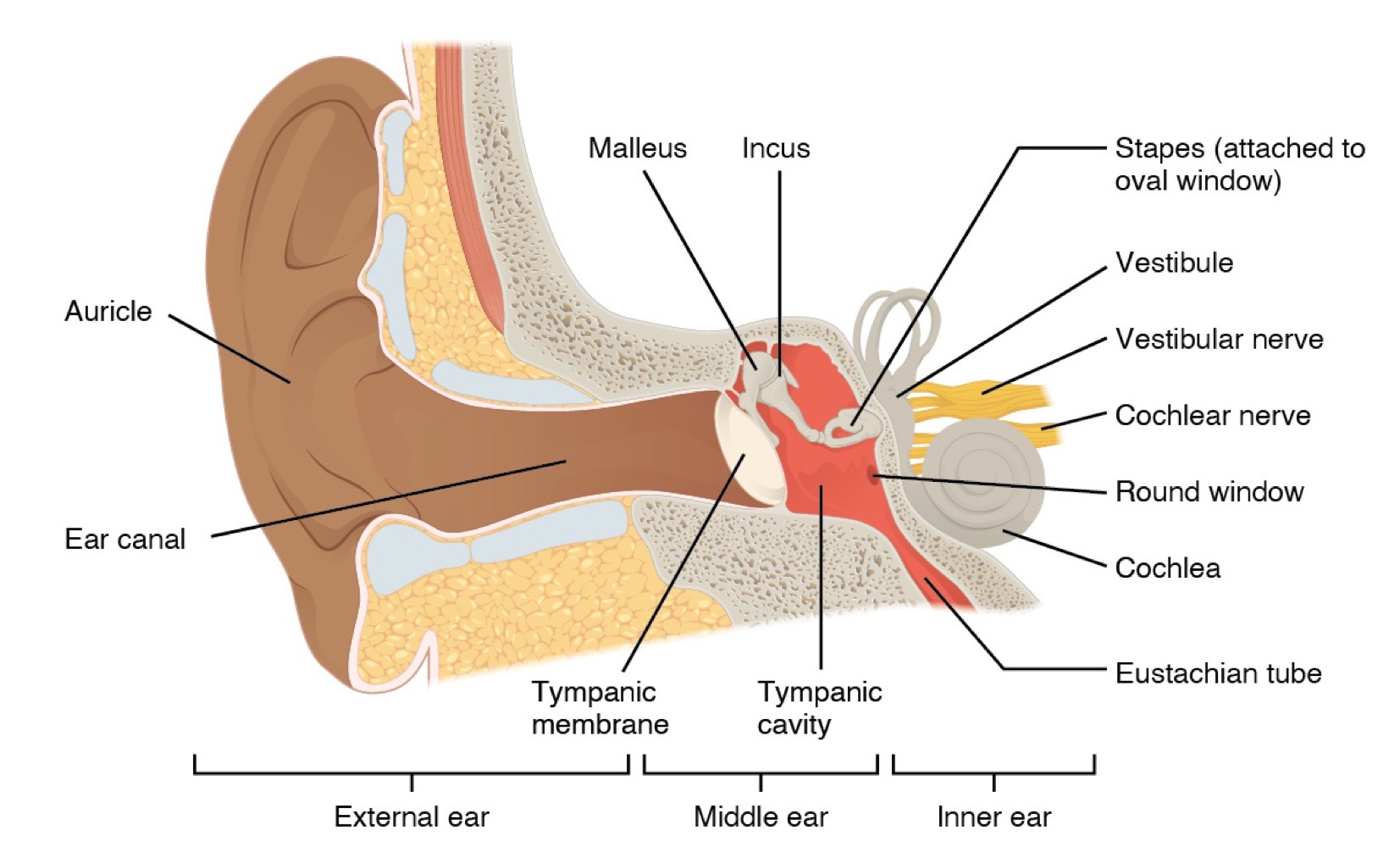
The ear is divided into three main regions: the external, middle, and inner ear.
External Ear
Auricle: Also known as the pinna, this is the large, fleshy structure on the lateral aspect of the head. Its C-shaped curves direct sound waves toward the auditory canal.
Auditory Canal: The canal that enters the skull through the external auditory meatus of the temporal bone.
Tympanic Membrane:Located at the end of the auditory canal, Commonly referred to as the eardrum, it vibrates when struck by sound waves.
Middle Ear
Consists of a space containing three small bones called the ossicles: the malleus, incus, and stapes.
Malleus: Attached to the tympanic membrane. articulates with the incus
Incus: Articulates between the malleus and the stapes.
Stapes: Attached to the inner ear where the sound waves will be transduced into a neural signal
Eustachian Tube: Connects the middle ear to the pharynx; it helps equilibrate air pressure across the tympanic membrane by opening during swallowing or yawning.
Inner Ear
Described as a bony labyrinth as it is composed of a series of canals embedded within the temporal bone, composed of canals with two primary regions:
Cochlea: Responsible for hearing.
Sound is transduced into neural signals within the cochlea region, which contains the sensory neurons of the spiral ganglia.
located within the spiral-shaped cochlea of the inner ear.
The cochlea is attached to the stapes through the oval window
Vestibule: Responsible for balance.
Neural signals from these regions are relayed to the brain stem via separate fiber bundles.
But these two distinct bundles travel together from the inner ear to the brain stem as the vestibulocochlear nerve.
The Process of Auditory Transduction
Oval Window: The stapes is attached to the cochlea through this membrane. It marks the beginning of a fluid-filled tube called the scala vestibuli.
The scala vestibuli extends from the oval window, traveling above the cochlear duct.
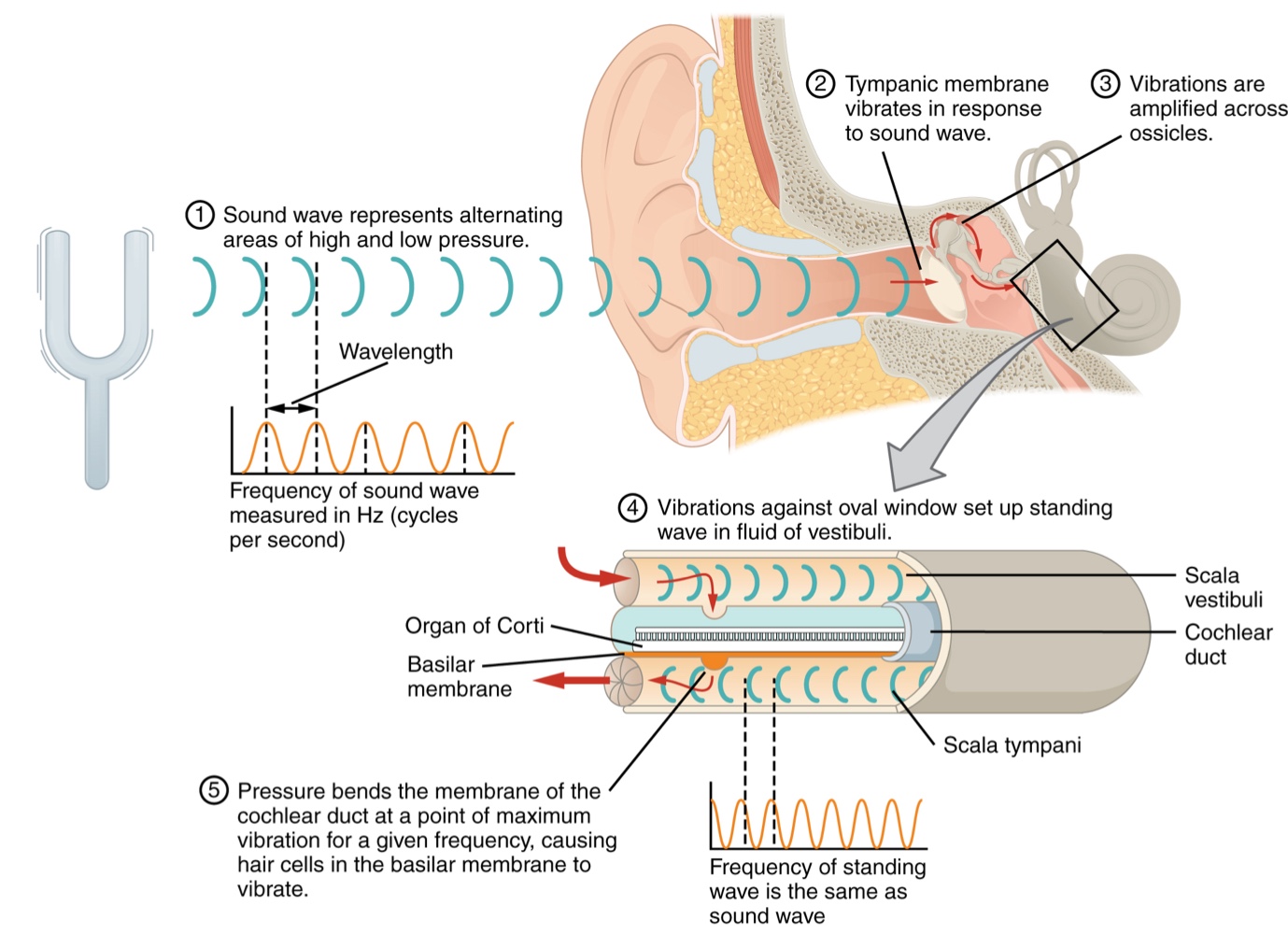
Cochlear Duct: The central cavity of the cochlea that contains the sound-transducing neurons. organs of Corti, which transduce the wave motion of the 2 scala into neural signals.
Scala Vestibuli and Scala Tympani:
At the uppermost tip of the cochlea, The scala vestibuli travels above the cochlear duct to the tip of the cochlea.
It then curves over the top and becomes the scala tympani, which travels under the cochlear duct back to the base.
The Scala tympani returns to the base of the cochlea, this time traveling under the cochlear duct.
The scala tympani, ends at the round window, which is covered by a membrane that contains the fluid within the scala.
As vibrations of the ossicles travel through the oval window, the fluid of the scala vestibuli and scala tympani moves in a wave-like motion.
The frequency of the fluid waves match the frequencies of the sound waves.
The membrane covering the round window will buldge out or pucker in with the movement of the fluid within the scala tympani.
Organs of Corti and the Basilar Membrane:
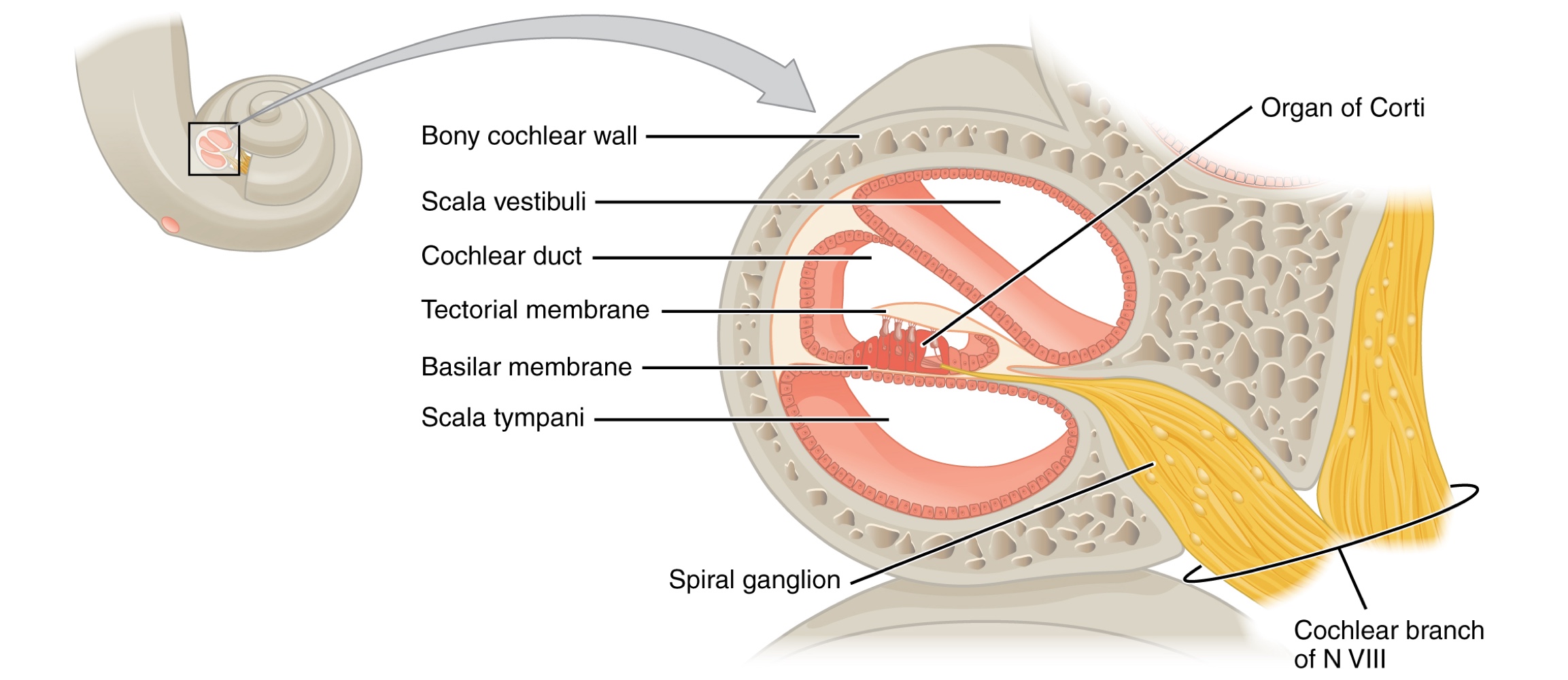
The cross-sectional view of the cochlea shows that the scala vestibuli and the tympani run along both sides of the cochlear duct.
The cochlear duct contains several organs of Corti which transduce the wave motion of the two scala into neural signals.
The organs of Corti lie on top of the basilar membrane, which is the side of the cochlear duct located between the organs of Corti and the scala tympani.
As fluid waves move through the scalae, the basilar membrane moves at a specific spot depending on the frequency of the waves.
Higher frequency waves move the region of the basilar membrane that is close to the base of the cochlea.
Lower frequency waves move the region of the basilar membrane that is near the tip of the cochlea.
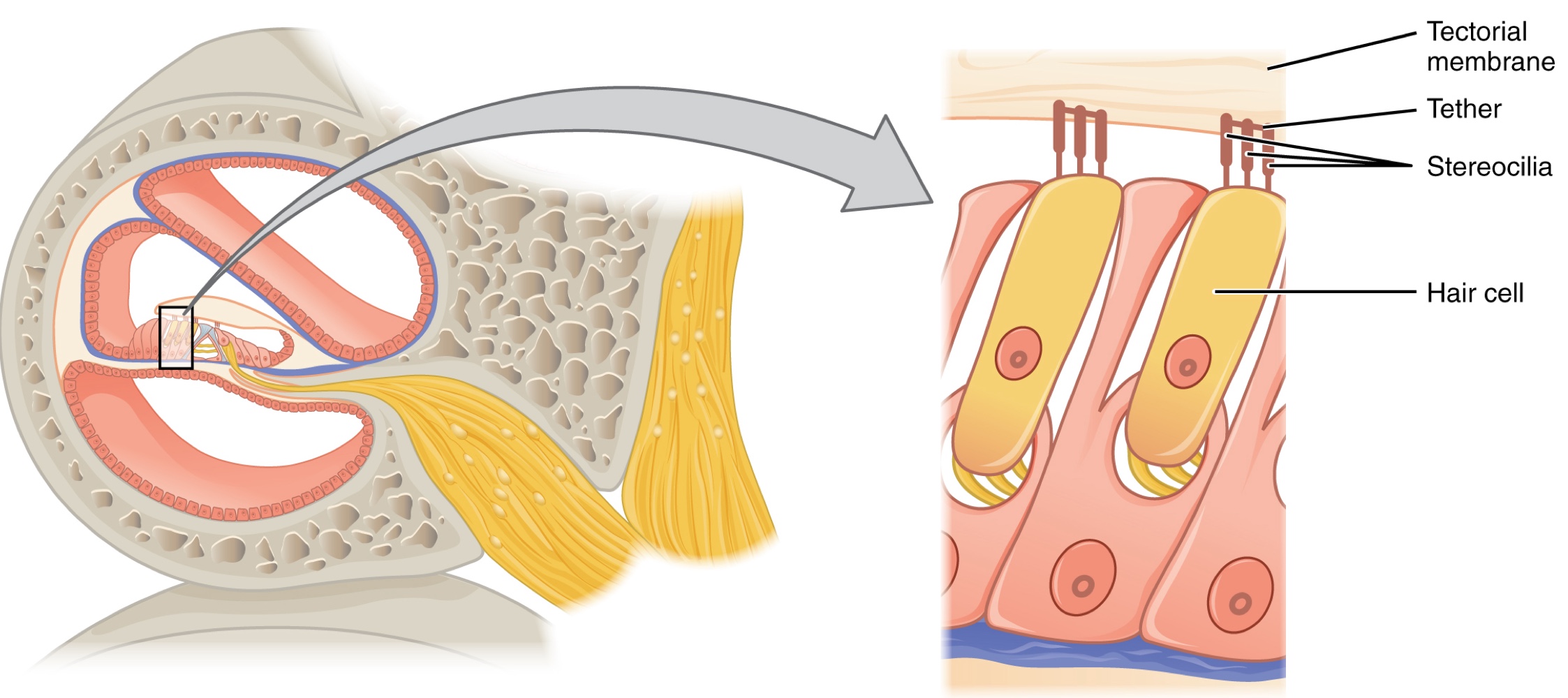
Hair Cells and Transduction:
The organs of Corti contain mechanoreceptor hair cells, named for the hair-like stereocilia extending from the cell’s apical surfaces.
The stereocilia are arranged from tallest to shortest and are tethered together by protein fibers so that the array will bend in response to movements of the basilar membrane.
Above the hair cells lies the tectorial membrane, which is attached medially to the organ of Corti.
Signal Generation Mechanism:
When pressure waves from the scala move the basilar membrane, the tectorial membrane slides across the stereocilia, bending them either toward or away from the tallest member of each array.
Bending toward the tallest member opens ion channels in the hair cell membrane (via tension in the tethers), triggering nerve impulses in the afferent nerve fibers.
Bending toward the shortest member slackens the tension on the tethers, closing the ion channels.
When no sound is present, stereocilia stand straight, and a small amount of tension maintains a slightly depolarized membrane potential.
Spiral Ganglia: These contain the sensory neurons located within the spiral-shaped cochlea.
Encoding Sound Frequency-
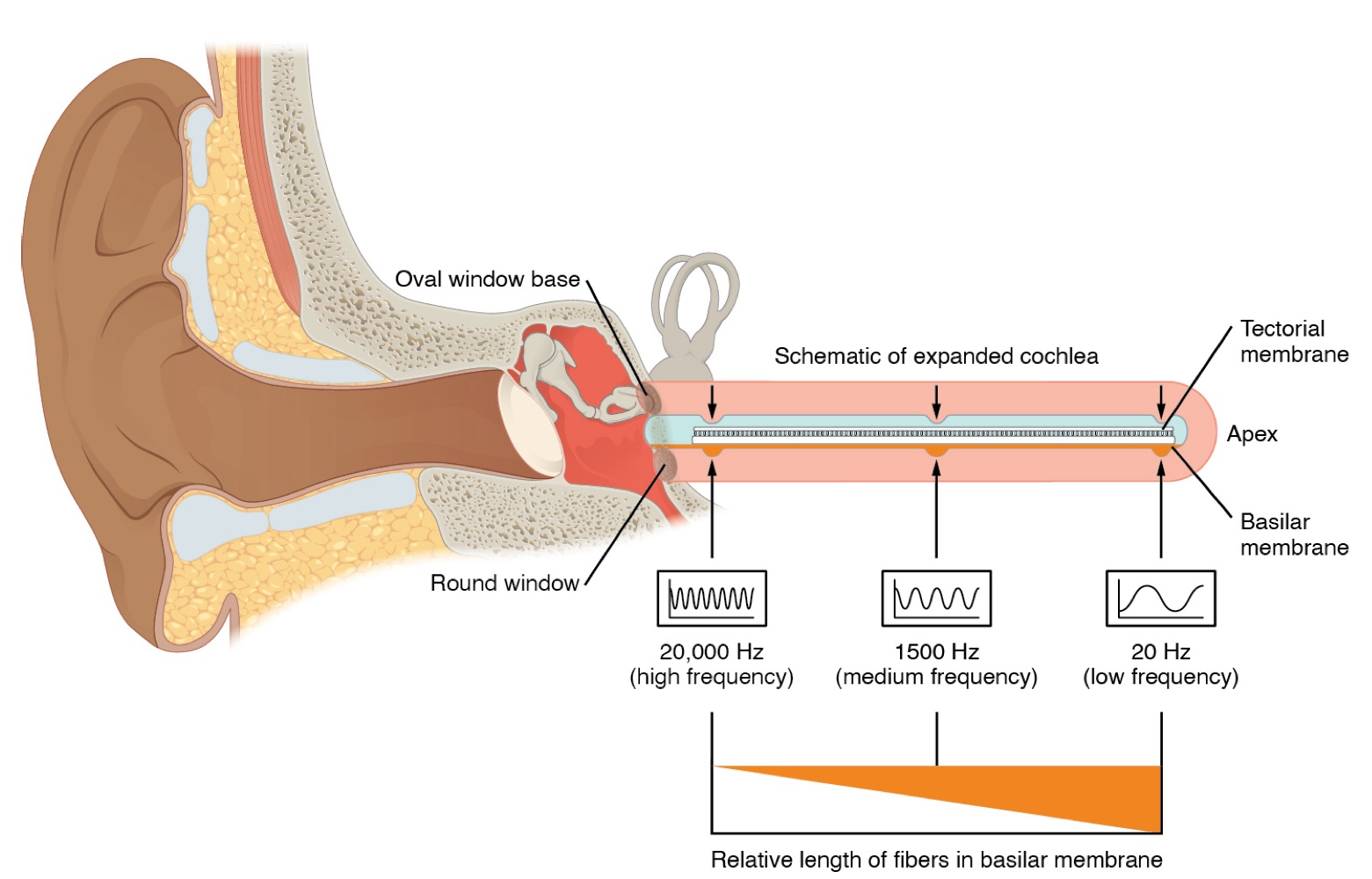
The movement of a specific region of the basilar membrane is dictated by the incoming sound wave's frequency.
Hair cells respond exclusively to the sounds of this specific frequency because the tectorial membrane only moves where the basilar membrane moves.-
The cochlea is responsible for encoding auditory stimuli for frequencies ranging from 20 to 20,000 Hz, which constitutes the range of human hearing.-
Hertz (Hz): The unit that measures sound wave frequency (cycles produced per second).-
Frequency Mapping:-
Low frequencies (e.g., 20 Hz) are sensed by hair cells located at the apex (tip) of the cochlea.
High frequencies (e.g., 20 KHz) are sensed by hair cells located at the base of the cochlea, near the round and oval windows.
Auditory stimuli often consist of complex mixtures of frequencies and intensities (amplitudes).
The specialized hair cells along the cochlear duct process these mixtures, allowing the cochlea to separate auditory stimuli by frequency, much like a prism separating visible light into colors.
Equilibrium (Balance)
Along with audition, the inner ear is responsible for encoding information about equilibrium, the sense of balance.
Sensory Mechanism
Utilizes mechanoreceptor hair cells with stereocilia to sense head position, movement, and bodily motion.
These cells are located within the vestibule of the inner ear.
Signals generated in the vestibular ganglion are transmitted through the vestibulocochlear nerve to the brain stem and cerebellum.
Positional vs. Rotational Sensing
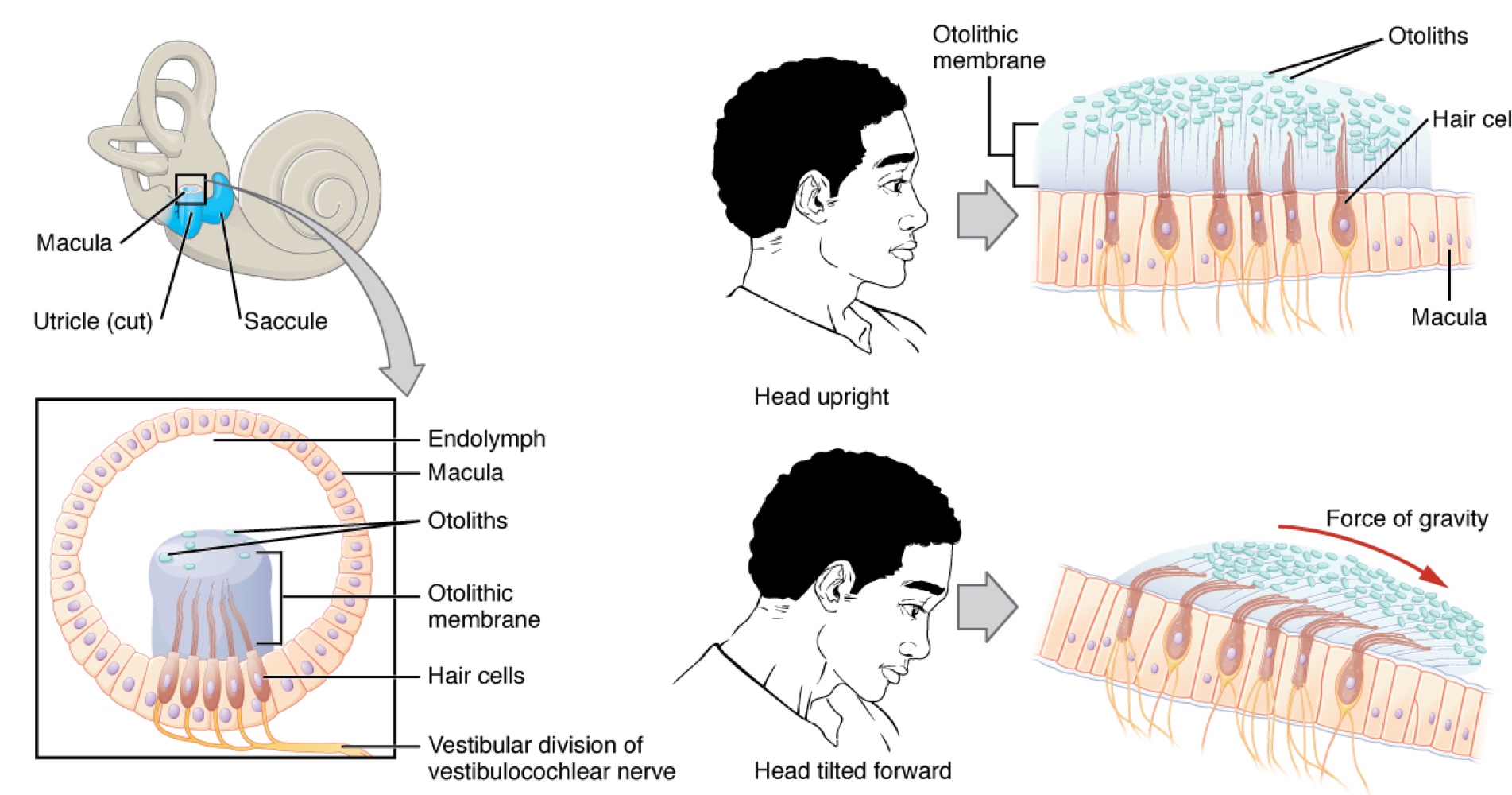
Utricle and Saccule: Sense head position.
The utricle and saccule are largely composed of macula (plural = maculae) tissue.
Macula is composed of hair cells surrounded by support cells
Otolithic Membrane: A viscous gel into which the stereocilia of the hair cells extend.
On top of the otolithic membrane is a layer of calcium carbonate crystals called otoliths.
Otoliths make the otolithic membrane top-heavy.
The otolithic membrane moves separately from the macula in response to head movements.
Tilting the head causes it to slide over the macula in the direction of gravity. — moving the otolithic membrane, in turn, bends the sterocila, causing some hair cells to depolarize as others hyper-polarize.
The exact position of the head is interpreted by the brain based on the pattern of hair-cell depolarization.
Semicircular Canals: Sense head movement (rotational). — These are three ring-like extensions of the vestibule.
One is oriented in the horizontal plane, while the other two are in the vertical plane.
The anterior and posterior ventral canals are oriented at approx. 45 degrees relative to the sagittal plane.
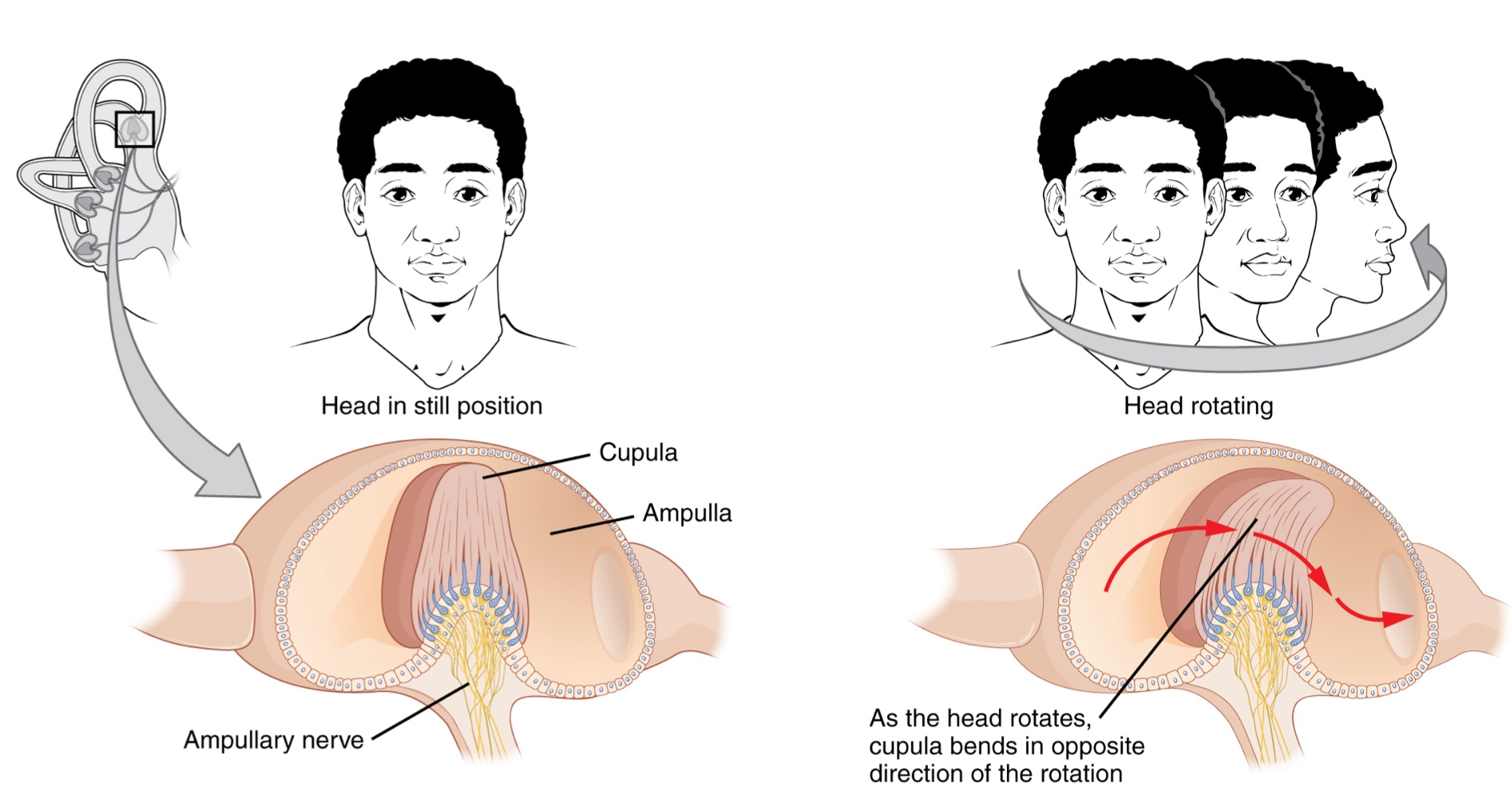
Ampulla: An enlarged region at the base of each semicircular canal where it meets the vestibule.
The ampulla contains hair cells that respond to rotational movement, such as turning the head while saying "no."
The stereocilla of these hair cells extend into the cupula
Cupula: A membrane that attaches to the top of the ampulla
As the head rotates in a plane parallel to the semicircular canal, the internal fluid lags, deflecting the cupula in the direction opposite to the head movement.
The semicircular canals contain several ampullae, with some oriented horizontally and some vertically.
By comparing the relative movements of these ampullae, the vestibular system detects the direction of head movements within three-dimensional (3-D) space.
Somatosensation (Touch)
Somatosensation is considered a general sense, as opposed to the special senses.
It consists of the group of sensory modalities associated with touch, proprioception, and interoception.
Modalities: These include pressure, vibration, light touch, tickle, itch, temperature, pain, proprioception, and kinesthesia.
Distribution: Receptors for this sense are not associated with a specialized organ but are instead spread throughout the body in various organs
Many of the somatosensory receptors are located in the skin, but receptors are also found in muscles, tendons, joint capsules, ligaments, and the walls of visceral organs.
Two major types of somatosensory signals transduced by free nerve endings are pain and temperature.
Thermoreceptors: These transduce temperature stimuli and are stimulated when local temperatures differ from body temperature.
Specific thermoreceptors may be sensitive to either cold or heat.
Nociceptors (Nociception): The sensation of potentially damaging stimuli
mechanical, chemical, or thermal stimuli beyond a set threshold will elicit painful sensations..
Stressed or damaged tissues release chemicals that activate receptor proteins in the.
For example consider the sensation of heat associated with spicy food involves capsaicin, the active molecule in hot peppers.
Capsaicin binds to a transmembrane ion channel in nociceptors that is sensitive to temperatures above 37^{\circ}C.
The dynamics of capsaicin binding with this ion channel is unusual, in that molecule remains bound to the receptor for a long period,
Because of this it decreases the ability of other stimuli to elicit pain sensations through that activated nociceptor.
Consequently, capsaicin functions as a topical analgesic, as seen in products like Icy Hot™.
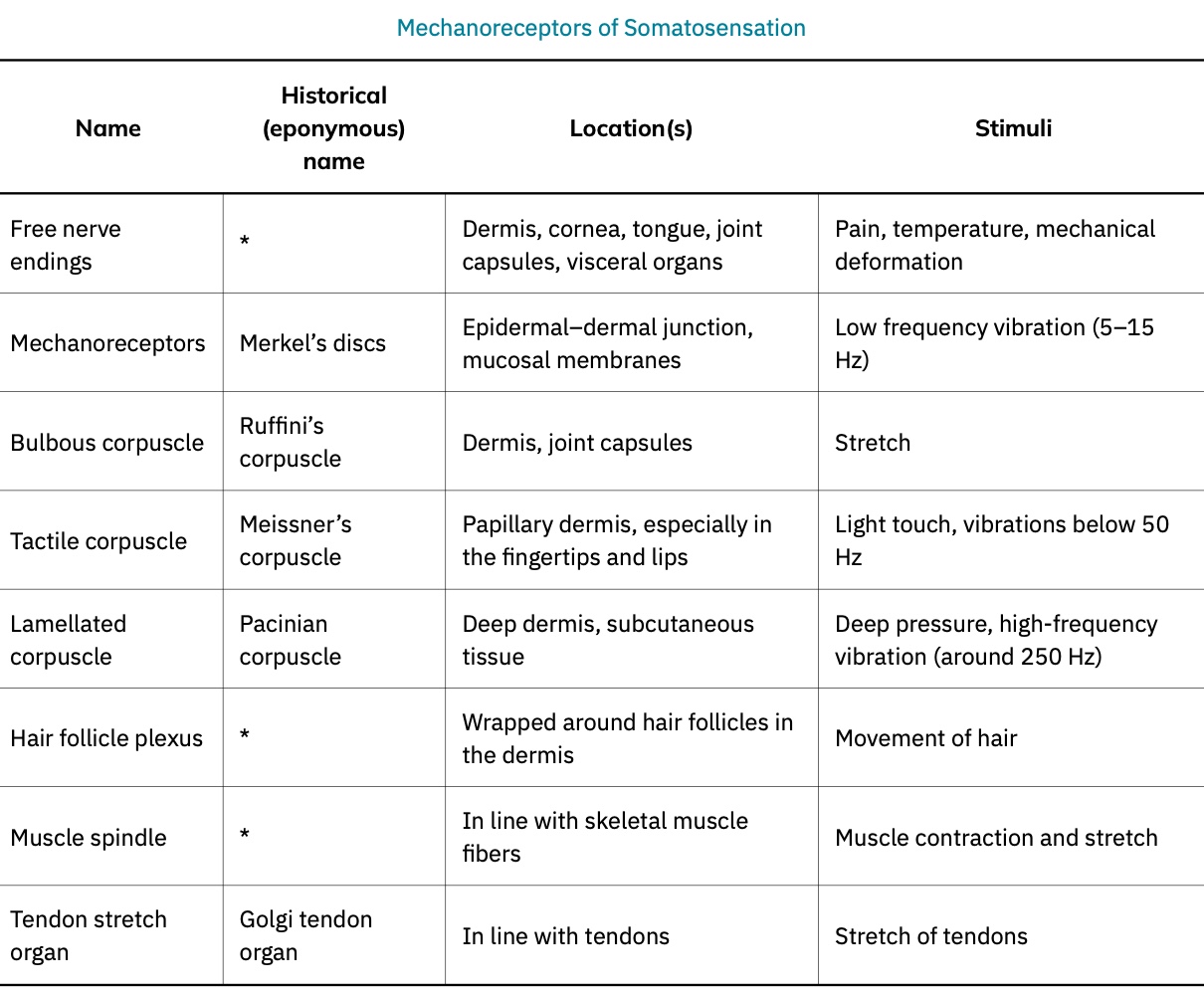
Specific Mechanoreceptors in the Skin
Merkel Cells (Type I Cutaneous Mechanoreceptors): Located in the stratum basale of the epidermis, these receptors sense low-frequency vibrations,
such as those produced when dragging a finger across a textured surface.
Tactile (Meissner) Corpuscles: Encapsulated endings that transduce the sensation of light touch.
Lamellated (Pacinian) Corpuscles: Encapsulated endings found deep in the dermis or subcutaneous tissue that transduce deep pressure and vibration.
Hair Follicle Plexus: A plexus of nerve endings wrapped around hair follicles that detect movement at the skin's surface, such as an insect walking along the skin.
Bulbous (Ruffini) Corpuscles (Type II Cutaneous Mechanoreceptors): Transduce skin stretch and are also found in joint capsules, where they measure stretch in the skeletal system components within the joint.
Proprioceptive Receptors in Muscles and Joints
These receptors monitor the stretching of tendons, muscles, and joint components to prevent over-contraction and tissue damage.
Muscle Spindles: Stretch receptors found in skeletal muscle tissue. When a muscle is stretched too far, these receptors initiate a reflex spasm to pull the muscle back into a less stretched state, preventing tearing.
Golgi Tendon Organs: Receptors that transduce the stretch levels of tendons.
Vision
the special sense of sight that is based on the transduction of light stimuli received through the eyes.
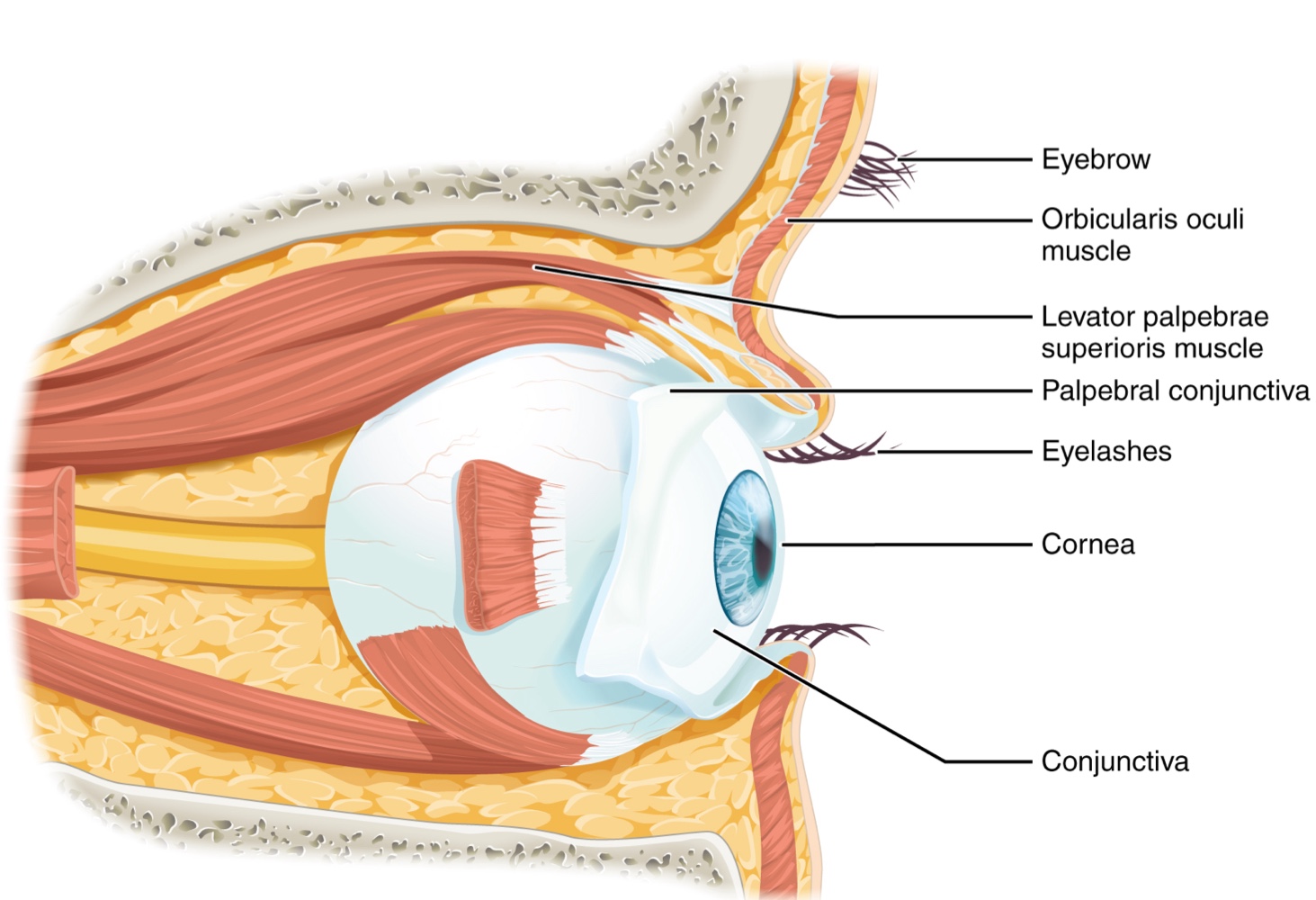
Eyes are situated within the bony orbits of the skull, which provide physical protection and anchor soft tissues
Eyelids and eyelashes protect the eye from abrasions by blocking foreign particles.
The palpebral conjunctiva is a thin membrane located on the inner surface of each eyelid.
The conjunctiva extends over the sclera (the white of the eye), connecting the eyelids to the eyeball.
The Lacrimal Apparatus
The lacrimal gland is located just inside the orbit, superior and lateral to the eyeball, and is responsible for producing tears.
Tears flow through the lacrimal duct to the medial corner of the eye.
As tears flow over the conjunctiva, they serve the function of washing away foreign particles.
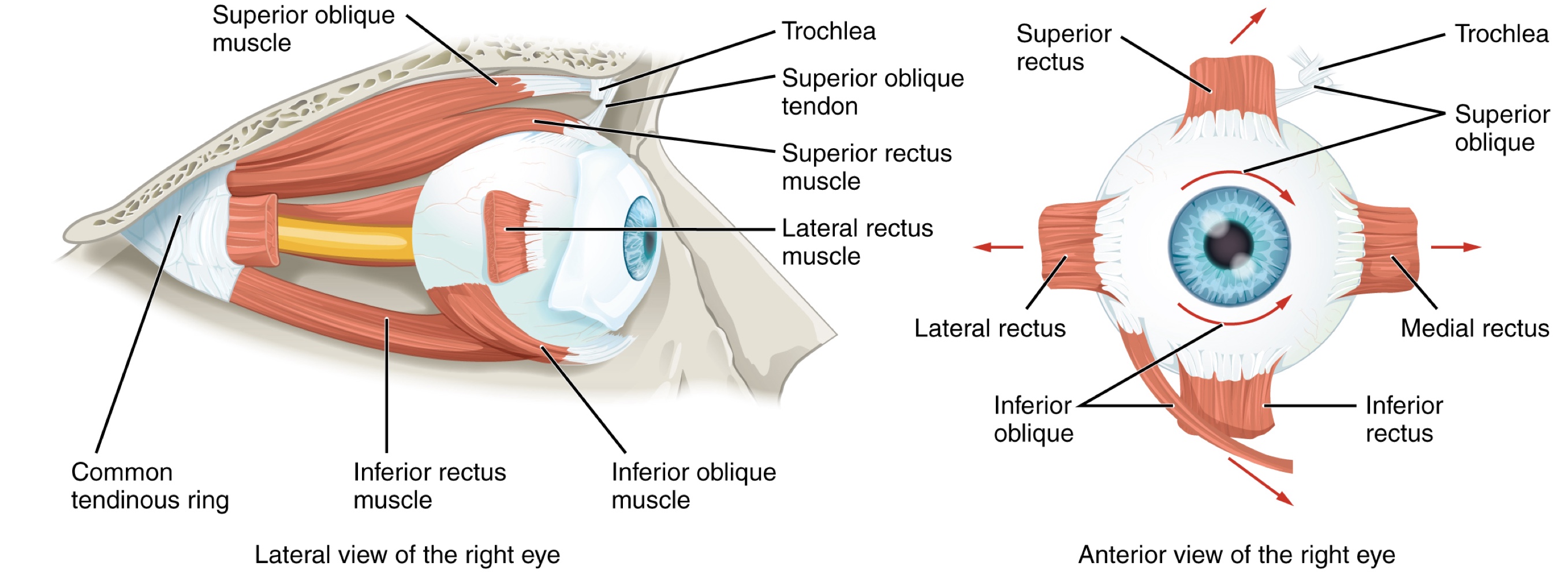
Extraocular Muscles
Movement of the eye within the orbit is accomplished by the contraction of six extraocular muscles originating from the orbit bones and inserting into the surface of the eyeball.
Rectus Muscles: Four muscles are arranged at the cardinal points around the eye:
Superior rectus: Rotates the eye to look up.
Medial rectus: Moves the eye medially.
Inferior rectus: Moves the eye downward.
Lateral rectus: Moves the eye laterally.
When each of the muscles contract, the eye moves toward the contracting muscle
Oblique Muscles: These are necessary because the eye is not perfectly aligned on the sagittal plane; they compensate for muscles like the superior rectus pulling at a 20 degree angle.
Superior oblique: Originates at the posterior orbit; near the origin of the 4 rectus muscles.
its tendon threads through a pulley-like piece of cartilage known as the trochlea.
The angle of the tendon through the trochlea means the contraction of the superior oblique rotates the eye laterally.
The tendon inserts obliquely into the superior surface of the eye.
Inferior oblique: Originates from the floor of the orbit and inserts into the infrerolateral surface of the eye
When it contracts, it rotates the eye laterally, in opposition to the superior oblique.
Levator palpebrae superioris: A seventh muscle in the orbit responsible for elevating and retracting the upper eyelid, usually moving in concert with the superior rectus.
The extraocular muscles are innervated by three cranial nerves whose nuclei connect to the brain stem to coordinate movements:
Abducens nerve: Innervates the lateral rectus (causing abduction of the eye).
Trochlear nerve: Innervates the superior oblique.
Oculomotor nerve: Innervates the levator palpebrae superioris and all remaining extraocular muscles.
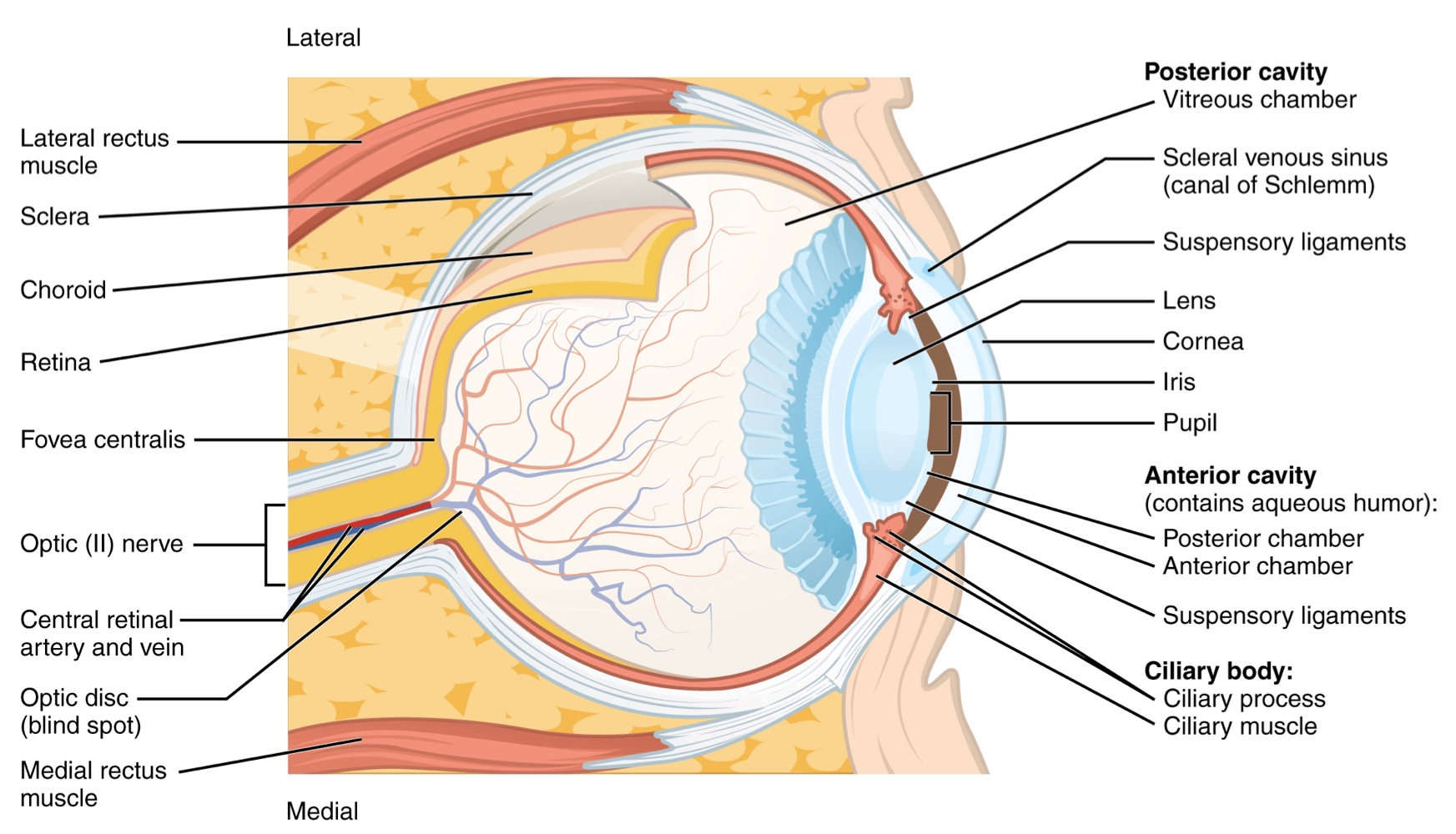
Structure of the Eyeball (Layers)
The eye is a hollow sphere composed of three layers of tissue:
Fibrous Tunic (Outermost): Includes the white sclera and the transparent cornea, which allows light to enter the eye.
The sclera accounts for five sixths of the surface of the eye, most of which is not visible
The transparent cornea covers the anterior tip of the eye and allows light to enter the eye
Vascular Tunic (Middle): mostly composed of the choroid, ciliary body, and the iris
Choroid: A layer of highly vascularized connective tissue providing blood supply to the eyeball.
The choroid is posterior to the ciliary body.
Ciliary Body: A muscular structure attached to the lens by zonule fibers (suspensory ligaments); these structures bend the lens allowing it to focus light to the back of the eye.
Iris: The colored part of the eye; a smooth muscle that regulates the size of the pupil to control light entry.
It overlays the ciliary body and is visible in the anterior eye.
The pupil is the hole at the center of the eye that allows light to enter.
The iris constricts the pupil in response to bright light and dilates the pupil in response to dim light.
Neural Tunic or Retina (Innermost): Contains the nervous tissue responsible for photoreception.
The eye is divided into two cavities:
Anterior Cavity: The space between the cornea and lens, including the iris and ciliary body. It is filled with a watery fluid called the aqueous humor.
Posterior Cavity: The space behind the lens that extends to the posterier side of the interior eyeball, where the retina is located. The posterior cavity is filled with a more viscous fluid called the vitreous humor.
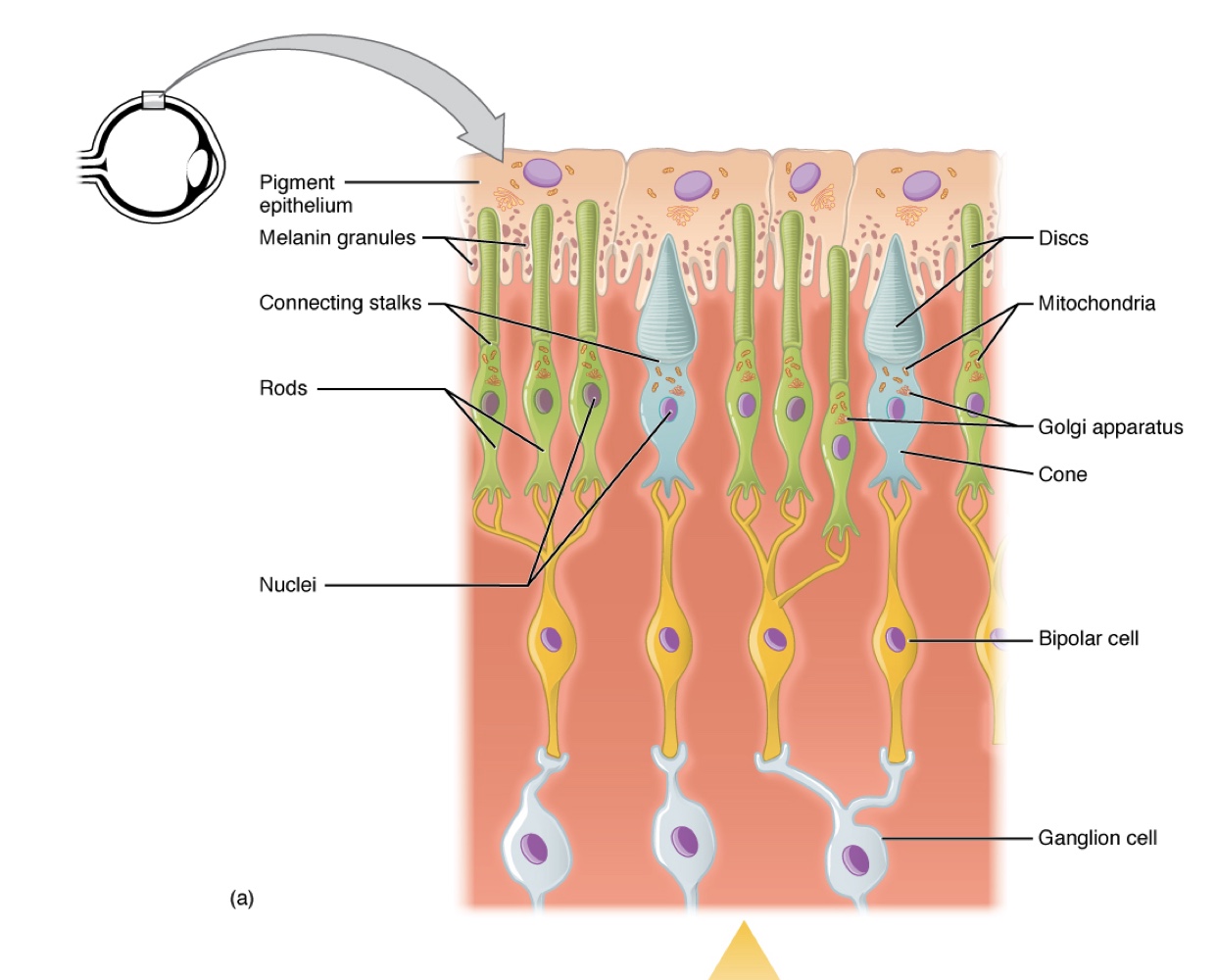
The retina is composed of several layers and contains specialized cells for the initial processing of visual stimuli.
Photoreceptors (rods and cones) Change their membrane potential when stimulated by light energy.
The change in membrane potential alters the amount of neurotransmitters that the photoreceptor cells release onto bipolar cells in the outer synaptic layer
Bipolar Cells: Located in the outer synaptic layer; they connect photoreceptors to retinal ganglion cells
Retinal Ganglion Cells (RGC): Are located in the inner synaptic layer; their axons form the optic nerve.
Amacrine Cells additionally contribute to retinal processing before an action potential is produced by the RGC.
The axons of the RGCs collect at the Optic disc and leave the eye as the optic nerve.
Because these axons pass through the retina, there are no photoreceptors at the very back of the eye, where the optic nerve begins.
This creates a “blind spot” in the retina, and a corresponding blind spot in our visual field
Optic Disc: The point where RGC axons leave the eye; because it lacks photoreceptors, it creates a blind spot in the visual field.
Photoreceptors in the retina are located behind axons, RGCs, bipolar cells, and retinal blood vessels.
A significant amount of light is absorbed by these structures before light reaches the photoreceptor cells.
There is a small area in the exact center of the retina known as the Fovea.
At the fovea, the retina lacks the supporting cells and blood vessels, and only contains photoreceptors. — This causes visual acuity (sharpness of vision), is greatest at the fovea.
This is because the fovea is where the least amount of incoming light is absorbed by other retinal structures.
As one moves in either direction from this central point of the retina, visual acuity drops significantly.
Each photoreceptor cell of the fovea is connected to a single RGC. — Therefore this RGC does not have to integrate inputs from multiple photoreceptors, which reduces the accuracy of visual transduction.
Towards the edge of the retina, several photoreceptors converge on RGCs (through the bipolar cells) up to a ratio of 50 to 1. Resulting in
A large part of the neural function of the eyes is concerned with moving the eyes and head so that important visual stimuli are centered on the fovea.
Photoreceptor Anatomy:
Light causes chemical changes in pigment molecules, leading to changes in RGC activity.
Photoreceptor cells have two parts:
Inner Segment: Contains the nucleus and common organelles of a cell.
Outer Segment: Specialized region where photoreception occurs
Types of Photoreceptors: They have 2 types of photoreceptors which differ in the shape of their outer segment.
Rod Photoreceptor: Has rod-shaped outer segments containing stacks of membrane-bound discs that contain the photosensitive pigment rhodopsin.
Cone Photoreceptor: Has cone-shaped outer segments that contain their photosensitive pigments in infoldings of the cell membrane.
There are three cone photopigments called opsins, which are each sensitive to a particular wavelength of light.
The wavelength of visible light determines its color.
The pigments in human eyes are specialized in perceiving three different primary colors: red, green, and blue.
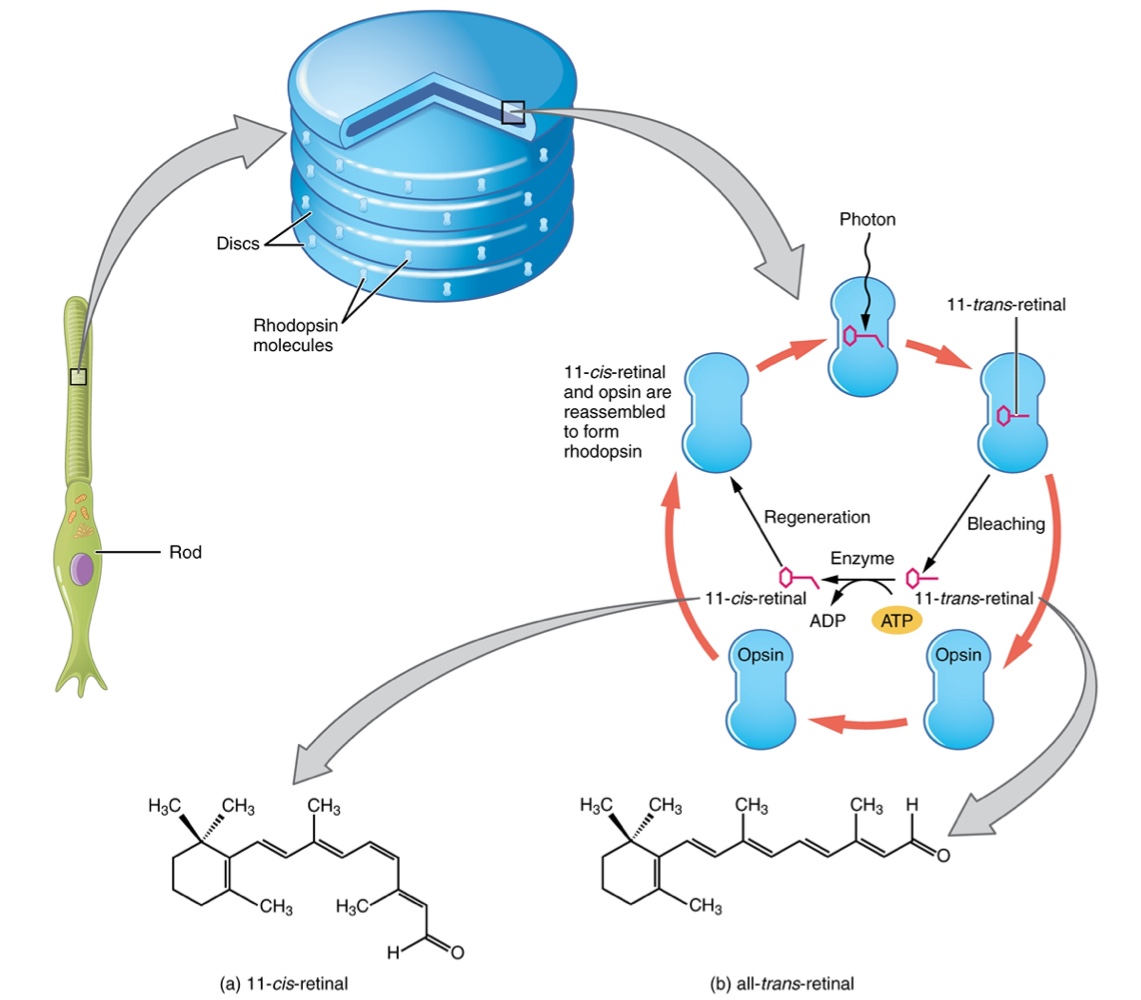
Molecular Level of Vision
At the molecular level, visual stimuli cause changes in the photopigment molecule that lead to changes in membrane potential of the photoreceptor cell.
Photons: Single units of light; discrete packets of energy with both particle and wave properties.
Wavelength (λ): Represents the energy of a photon
visible light is electromagnetic radiation with a wavelenght that ranges from 380 nm (blue) to 720 nm(dark red).
All other colors fall between red and blue at various points along the wavelength scale.
Ultraviolet: Wavelengths shorter than 380 nm
Infrared: Wavelengths longer than 720 nm
Photopigment Components:
Opsin Pigments are actually transmembrane proteins that contains cofactor retinal.
Retinal: A cofactor hydrocarbon molecule related to Vitamin A.
When a photon hits retinal, the long hydrocarbon chain of the molecule is biochemically altered.
Specifically, photons cause some double-bonded carbons within the chain to switch from a cis to a trans conformation, or Photoisomerization
Photoisomerization Process:
Before interacting with a photon, retinal’s flexible double-bonded carbons are in the cis conformation also referred to as:
11-cis-retinal: The flexible, bent shape of retinal before light interaction.
A photon interacting with this molecule causes the flexible double bonded carbons to change to the trans-conformation, forming:
all-trans-retinal: A straight hydrocarbon chain formed when a photon causes double-bonded carbons to switch conformation.
The Transduction Process: The shape change of retinal in the photoreceptors initiates visual transduction in the retina.
Activation of retinal and the opsin proteins result in activation of a G protein.
The G protein changes the membrane potential of the photoreceptor cell, which then releases less neurotransmitter into the outer synaptic layer of the retina.
Until the retinal molecule is changed back to the 11-cis-retinal shape, the opsin cannot respond to light energy this is called bleaching.
When a large group of photopigments is bleached, the retina will send information as if opposing visual information is being perceived.
Negative Afterimages: Perceived after bright exposure because overstimulated/bleached areas cannot send information until retinal is enzymatically reset to the cis form.
Photoreceptor Classes
Opsins are sensitive to limited wavelengths of light.
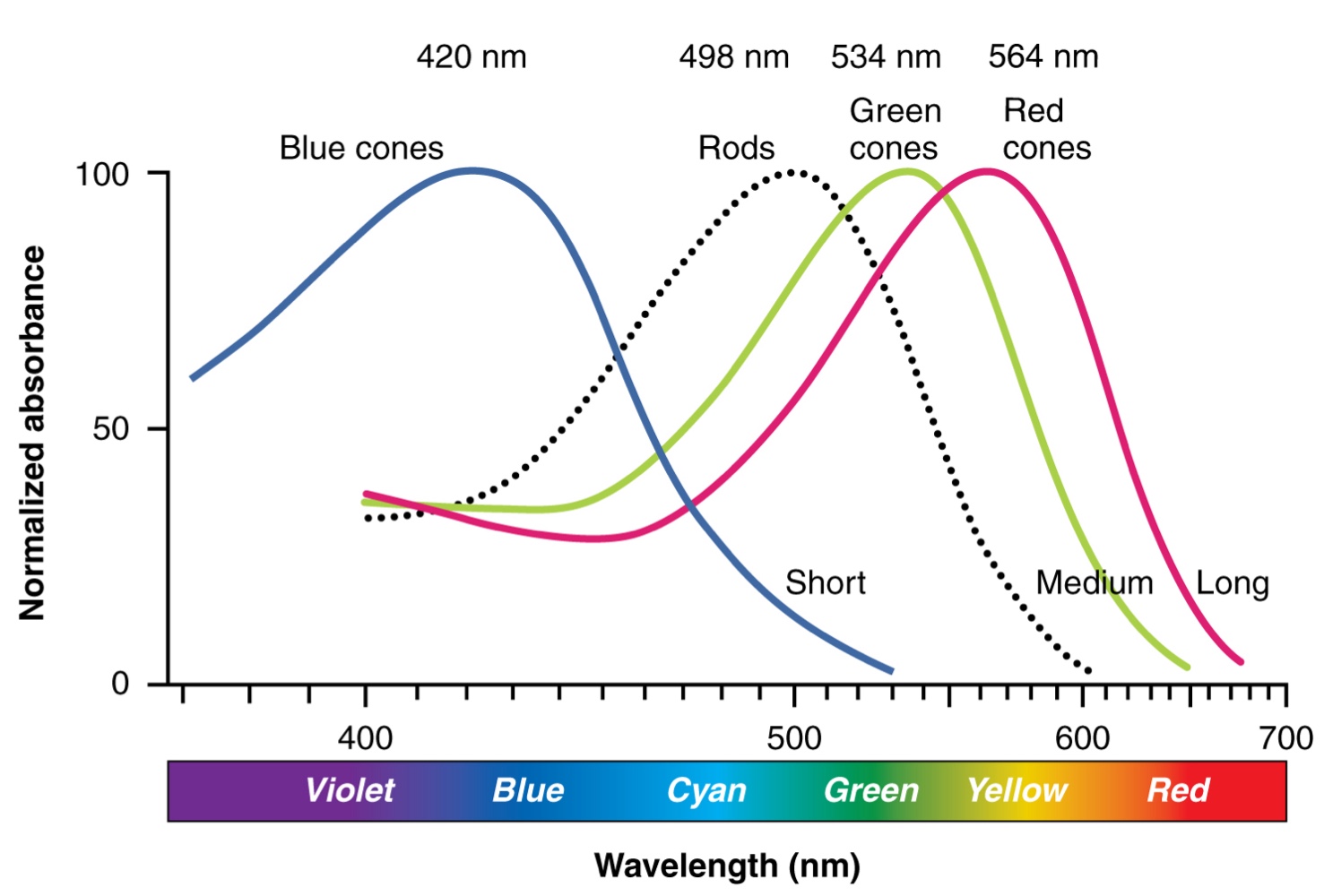
The three color opsins have peak sensitivities of:
Red (L): 564 nm.
Green (M): 534 nm.
Blue (S): 420 nm.
Rhodopsin, the photopigment in rods, is most sensitive to light at a 498 nm.
The absorbance of rhodopsin in the rods is much more sensitive than in the cone opsins.
Specifically, rods are sensitive to vision in low light conditions, while cones are sensitive to brighter conditions.
In normal sunlight, rhodopsin will be constantly bleached while the cones are active. In a darkened room, there is not enough light to active cone opsins, and vision is entirely dependent on rods.
Rods are so sensitive to light that a single photon can result in an action potential from a rods corresponding RGC.
The three types of cone opsins, being sensitive to different wavelength of light, provides us with color vision.
By comparing the activity of the three different cones, the brain can extract color information from visual stimuli.
For example, a bright blue light that has an approx. wavelength of 450 nm.
This would minimally activate the “red” cones, marginally activate the “green” cones, and the “blue” cones predominantly.
The relative activation of the three different cones is calculated by the brain, which perceives color as blue.
Cones cannot react to low-intensity light, and rods do not sense the color of light.
Therefore, our low-light vision is — in essence — in grayscale.
In other words, in a dark room everything appears as a shade of gray
if you think you can see colors in the dark, it is most likely because your brain knows what color something is and is relying on that memory.
Sensory Nerves
Once any sensory cell transduces a stimulus into a nerve impulse, that impulse travels along axons to reach the CNS.
In many special senses, the axons leaving the sensory receptors have a topographical arrangement.
This means the location of the sensory receptor relates to the specific location of the axon within the nerve.
Example: In the retina, axons from RGCs in the fovea are located in the center of the optic nerve, surrounded by axons from the more peripheral RGCs.
Spinal Nerves
These nerves generally contain afferent axons from sensory receptors in the periphery (such as from the skin) mixed with efferent axons traveling to muscles or other effector organs.
As the spinal nerve nears the spinal cord, it splits into two roots:
Dorsal Root: Contains only the axons of sensory neurons.
Ventral Root: Contains only the axons of motor neurons.
Pathways and Synapses:
Some branches will synapse with local neurons in the dorsal root ganglion, posterior (dorsal) horn, or anterior (ventral) horn at the level of the spinal cord where they enter.
Other branches travel short distances up or down the spine to interact with neurons at other levels of the spinal cord.
A branch may turn into the posterior (dorsal) column of the white matter to connect with the brain.
Contralateral Organization: Spinal nerve systems are typically contralateral;
the right side of the body connects to the left side of the brain,
and the left side of the body connects to the right side of the brain.
Cranial Nerves
They convey specific sensory information from the head and neck directly to the brain. Where as spinal information is contralateral, cranial nerve systems, with some exceptions are mostly ipsilateral.
Ipsilateral Organization: Unlike spinal nerves, these systems are mostly ipsilateral, meaning a nerve on the right side of the head connects to the right side of the brain.
Functional Composition:
Some cranial nerves contain only sensory axons
This includes the olfactory, optic, and vestibulocochlear nerves.
Some contain both sensory and motor axons
This includes the trigeminal, facial, glossopharyngeal, and vagus nerves (however, the vagus nerve is not associated with the somatic nervous system.
General senses of somatosensation for the face travel specifically through the trigeminal system.
Ch. 14.2 Central Processing
Sensory Pathway
Specific regions of the CNS coordinate different somatic processes using sensory inputs and motor outputs of peripheral nerves.
A simple case would be a reflex caused by synapse between a dorsal sensory neuron axon and a motor neuron in the ventral horn.
More complex arrangements are possible to integrate peripheral sensory information with higher processes.
The important regions of the CNS that play a role in somatic processes can be separated into the spinal cord brain stem, diencephalon, cerebral cortex, and subcortical structures.
Spinal Cord and Brain Stem
Ascending Pathways
A sensory pathway that carries peripheral sensations to the brain is referred to as an ascending pathway or ascending tract.
The various sensory modalities each follow specific pathways through the CNS.
Tactile and other somatosensory stimuli activate receptors in the skin, muscles, tendons, and joints throughout the entire body.
However, the somatosensory pathways are divided into 2 separate systems based on the location of the receptor neurons:
Below the Neck: Stimuli pass along the sensory pathways of the spinal cord.
Head and Neck: Stimuli travel through the cranial nerves (specifically the trigeminal system).
Major Somatosensory Tracts
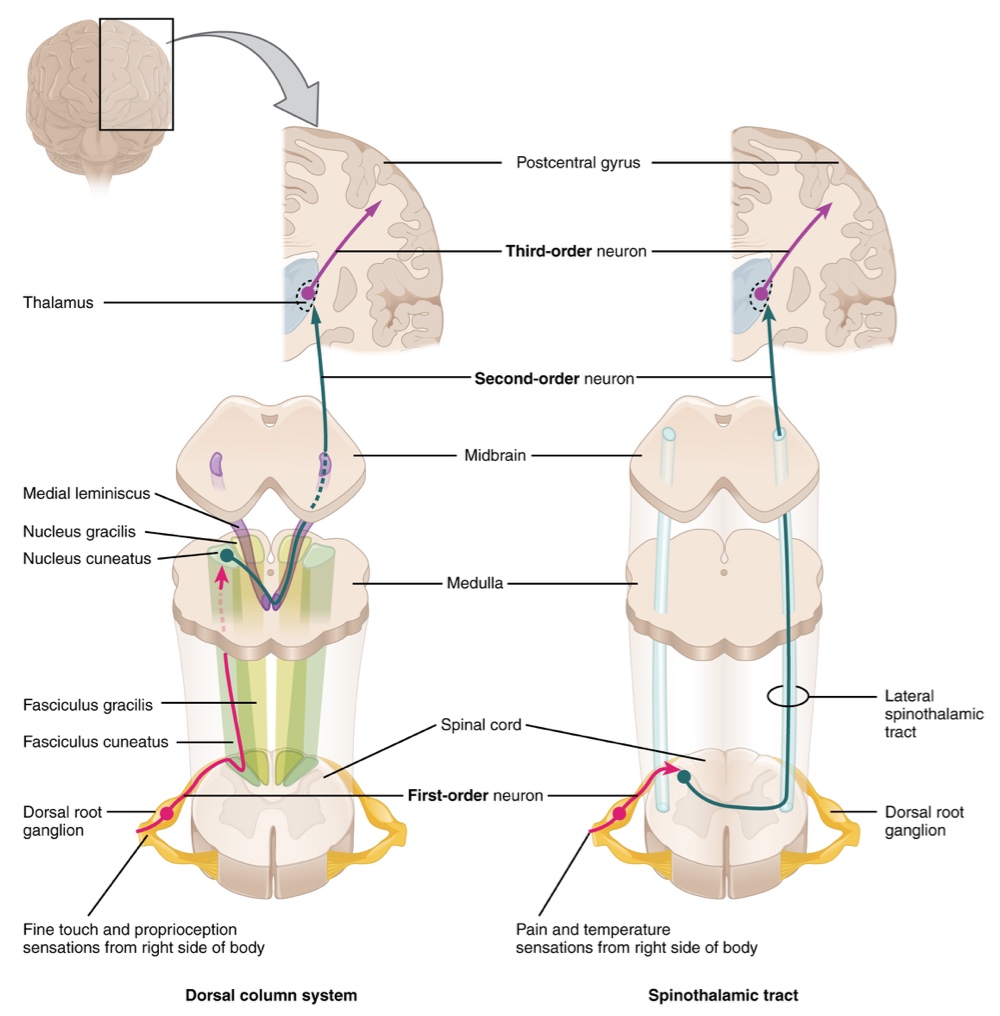
The two major pathways conveying sensory information to the brain are the dorsal column system (sometimes referred to as the dorsal column-medial lemniscus) and the spinothalamic tract.
Each of these systems is composed of 3 successive neurons.
These pathways are contralateral; the second neuron in both systems decussates to project to the opposite side of the brain or spinal cord.
In both the second neuron also synapse in the thalamus and the thalamic neurons project to the somatosensory cortex.
The Dorsal Column System (Medial Lemniscus)
Primarily responsible for touch sensations and proprioception.
This system begins with the axons of a dorsal root ganglion neuron entering the dorsal root and joining the dorsal column white matter in the spinal cord.
As axons of this pathway enter the dorsal column, they take on a positional arrangement so that axons from lower levels of the body position themselves medially,
whereas axons from the upper levels of the body position themselves laterally.
The dorsal column is separated into two component tract:
Fasciculus Gracilis: Contains axons from the legs and lower body.
Fasciculus Cuneatus: Contains axons from the upper body and arms.
The axons in the dorsal column terminate in the nuclei of the medulla, where each synapse with the second neuron in their respective pathway
Nucleus Gracilis: The target for fibers in the fasciculus gracilis.
Nucleus Cuneatus: The target for fibers in the fasciculus cuneatus.
These second-order neurons decussate (or crosses the midline of the medulla) and ascend the brain stem as a bundle called the medial lemniscus.
These axons terminate in the thalamus, where each synapses with the third neurons in their respective pathways.
Third Neuron: Axons project from the thalamus to the post-central gyrus of the cerebral cortex, where somatosensory stimuli are initially processed and the conscious perception of that stimuli occurs
The Spinothalamic Tract
Primarily responsible for pain and temperature sensations.
First Neuron: Neurons begin in the dorsal root ganglion and extend axons to the dorsal horn of the spinal cord, where they synapse with the second neuron in their respective pathways
The name “spinothalamic” comes from this second neuron which has its cell body in the spinal cord gray matter and connects to the thalamus.
These neurons decussate within the spinal cord at the same level at which information entered.
Axons then ascend to the brain and enter the thalamus to synapse with the third neuron in its respective pathway.
Third Neuron: Projects from the thalamus then project their axons to the spinothalamic tract, which synapses in the postcentral gyrus of the cerebral cortex.
The Trigeminal Pathway
Carries somatosensory information from the face, head, mouth, and nasal cavity.
First Neuron: Axons from the trigeminal ganglion enter the brain stem at the pons and project to three locations:
Spinal Trigeminal Nucleus of the Medulla: Receives pain and temperature (similar to spinothalamic).
Chief Sensory Nucleus in the Pons/Mesencephalic Nuclei in the Midbrain: Receives touch, pressure, vibration, and proprioception (similar to dorsal column).
Second Neuron: Axons decussate and ascend via the trigeminothalamic tract to the thalamus.
Third Neuron: Axons project from the thalamus to the primary somatosensory cortex.
Special Sense Central Processing
The Gustatory Pathway
Travels along the facial and glossopharyngeal cranial nerves. — which synapse with neurons in the solitary nucleus of the brain stem.
Neurons from the solitary nucleus then project to the ventral posterior nucleus of the thalamus.
Final projection is to the gustatory cortex of the cerebral cortex for conscious perception.
Auditory Central Processing
Sensory signals travel via the vestibulocochlear nerve to the cochlear nuclei in the superior medulla.
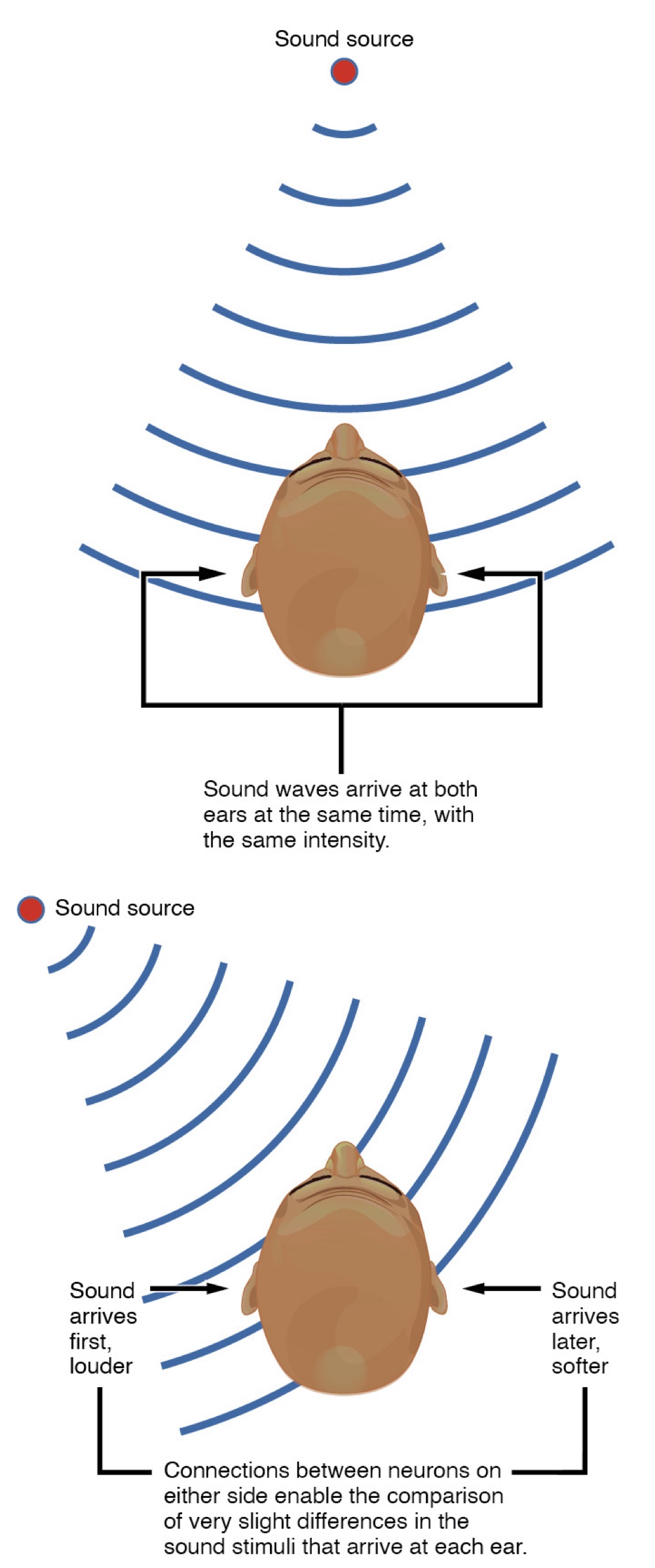
Within the brain stem, input from either ear is combined to extract location info from the auditory stimuli.
Initial auditory stimuli received at the cochlea strictly represent the frequency— or pitch— of the stimuli, the locations of sound can be determined by comparing information arriving at both ears
Sound Localization: Brain calculates location by comparing input from both ears.
Interaural Time Difference: Measures the microseconds difference in arrival time between ears.
Interaural Intensity Difference: Measures the difference in loudness caused by the head blocking sound waves.
Processing continues to the inferior colliculus in the midbrain, which projects to:
Medial Geniculate Nucleus: Located in the thalamus, it relays information to the auditory cortex in the temporal lobe.
Superior Colliculus: Integrates auditory, visual, and somatosensory input to initiate stimulation of the muscles that coordinate head and neck movement toward stimuli.
Equilibrium Central Processing
Balance is coordinated through the vestibular system.
Nerves from the vestibular ganglion carry information from the utricle, saccule, and semicircular canals to the vestibular nuclei of the medulla or directly to the cerebellum (with no intervening synapse from the vestibular nuclei).
This system contributes to controlling head and neck movements in response to vestibular system.
Cerebellum: Primarily responsible for initiating movements based on equilibrium info.
Neurons in the Vestibular Nuclei Project axons to targets in the brain stem:
Reticular Formation: Influences respiratory and cardiovascular adjustments during movement.
Spinal Cord: Initiates spinal reflexes to maintain posture and balance.
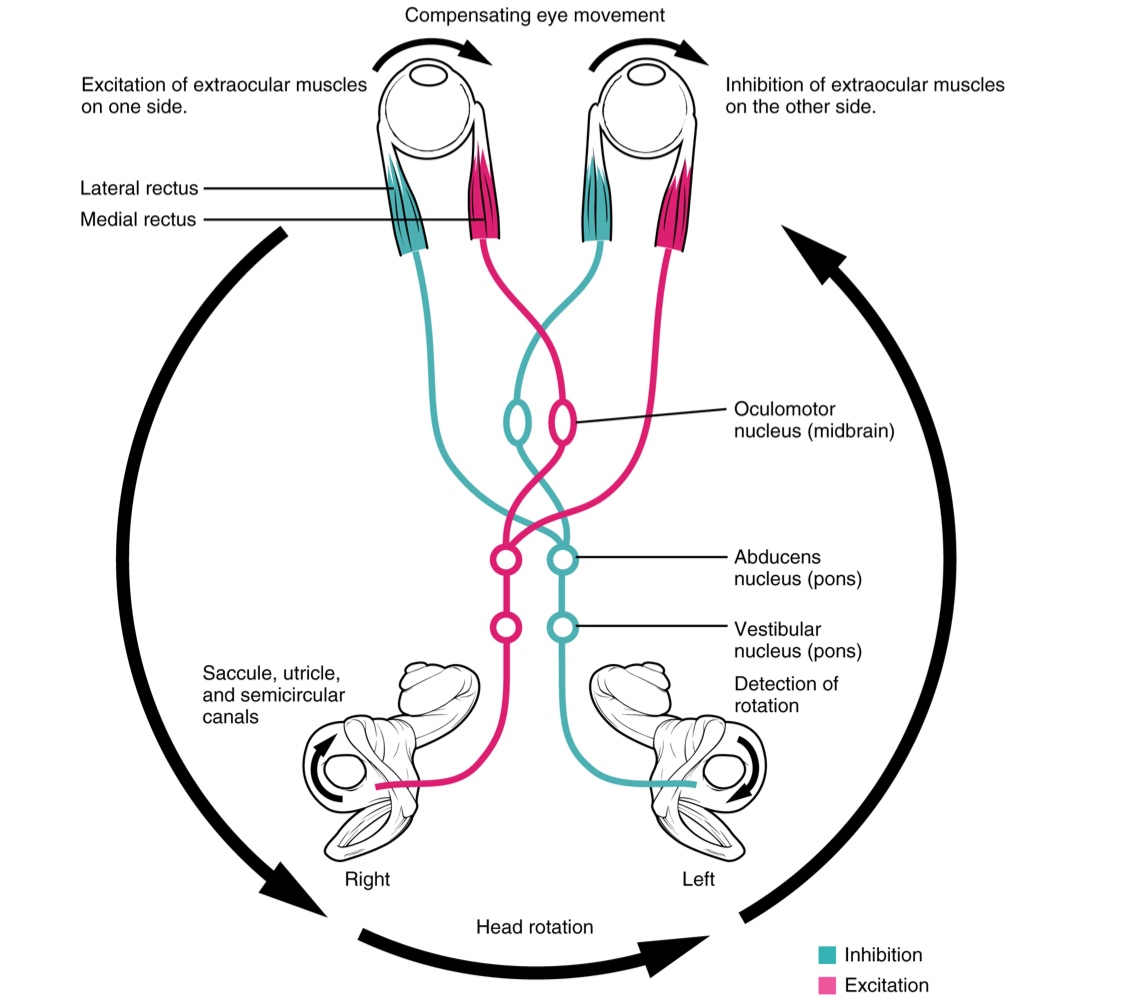
Cranial Nerve Nuclei (III, IV, VI): Mediates the vestibulo-ocular reflex (VOR) which compensates for head and body movement by stabilizing retinal images during movement.
This assist the visual systems.
Thalamus: Joins the proprioceptive pathway of the dorsal column system for conscious perception of balance.
Visual Central Processing
Instead of connections being between each eye and the brain, visual information is segregated between the left and right sides of the visual field.
Some of the information from one side of the visual field projects to the opposite side of the brain.
Within each eye, the axons projecting from the medial side of the retina decussate at the optic chiasm.
For example. Axons from the medial retina of the left eye cross over to the right side of the brain at the optic chiasm
The axons projecting from the lateral side of the retina do not decussate.
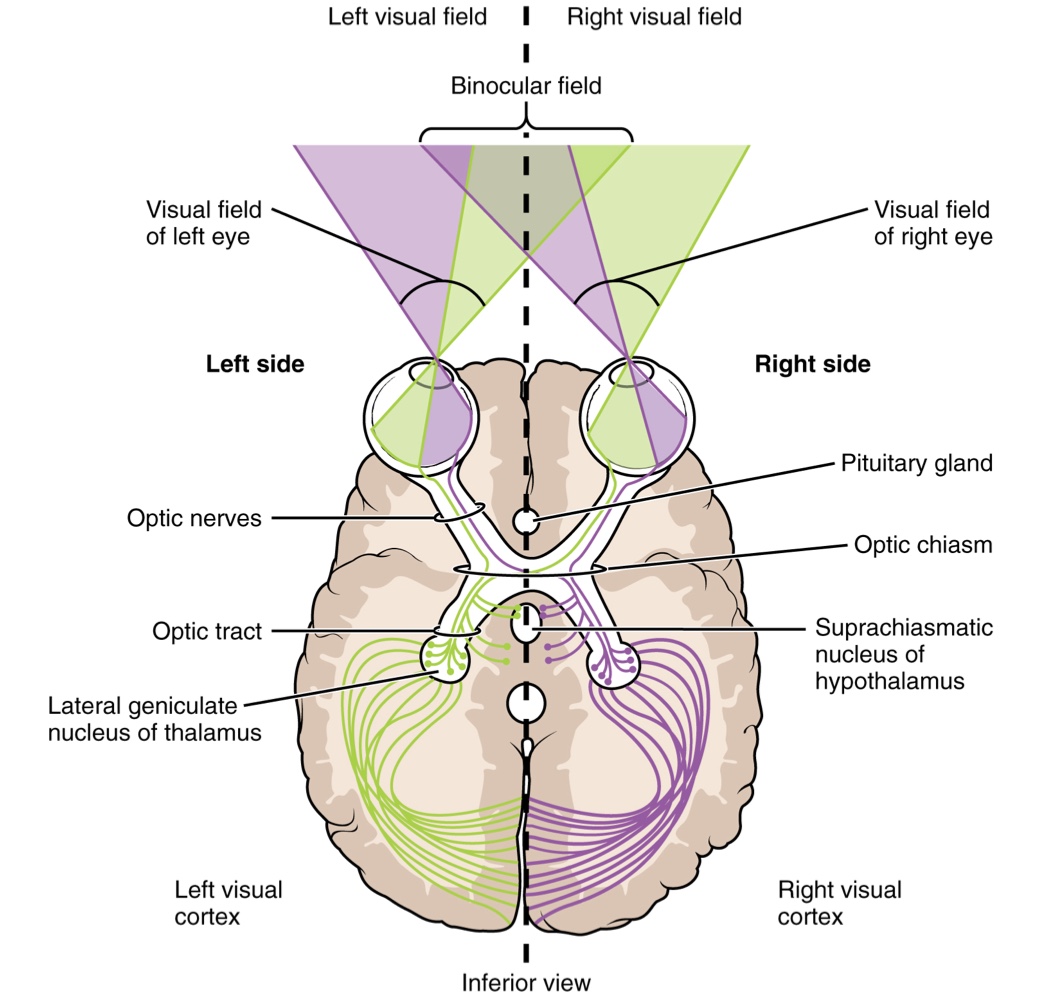
Clinical Presentation: Bilateral Hemianopia
Loss of lateral peripheral vision (outermost areas of the visual field).
Caused by a growth (e.g., pituitary gland) pressing against the optic chiasm, interfering with decussating signals.
Optic Tract Targets
Extending from the optic chiasm, the axons are referred to as the optic tract, which connects to 3 major targets (2 in the diencephalon and 1 in the midbrain):
Lateral Geniculate Nucleus (Thalamus): The primary target, projecting visual information to the visual cortex in the occipital lobe.
Superior Colliculus (Midbrain): An additional target for visual processing.
Suprachiasmatic Nucleus (Hypothalamus): Receives input from a small number of photosensitive RGCs. These cells respond to the presence or absence of light (without image perception) to establish the circadian rhythm by detecting day length.
Diencephalon
Located beneath the cerebrum, consisting primarily of the thalamus and hypothalamus.
Hypothalamus
Manages both somatic and autonomic functions.
Maintains communication with the limbic system, influencing memory functions and emotions.
Thalamus
Acting as a critical relay station, it facilitates communication between the cerebrum and the rest of the nervous system.
It is a required transfer point for most sensory tracts intended for the cerebral cortex, where conscious sensory perception begins.
The Olfactory Exception: Unlike other senses, the olfactory system projects axons from the olfactory bulb directly to the cerebral cortex, limbic system, and hypothalamus, bypassing the thalamic relay.
Functional Nuclei Groups: The thalamus is organized into 3 anatomical regions by internal white matter:
Anterior Nucleus: Serves as a relay between the hypothalamus and the emotion-producing limbic system.
Medial Nuclei: Relays cues from the limbic system and basal ganglia to the cerebral cortex; essential for alertness, learning, and memory creation.
Lateral Group of Nuclei: The primary connection site for somatic and special senses, which are then relayed to the specific sensory cortex of the cerebrum.
Cortical Processing
Sensory axons are positioned similarly to their corresponding receptor cells, a principle known as sensory topography. This arrangement allows the cerebral cortex to identify a stimulus's location based on which specific receptor cells are transmitting signals.
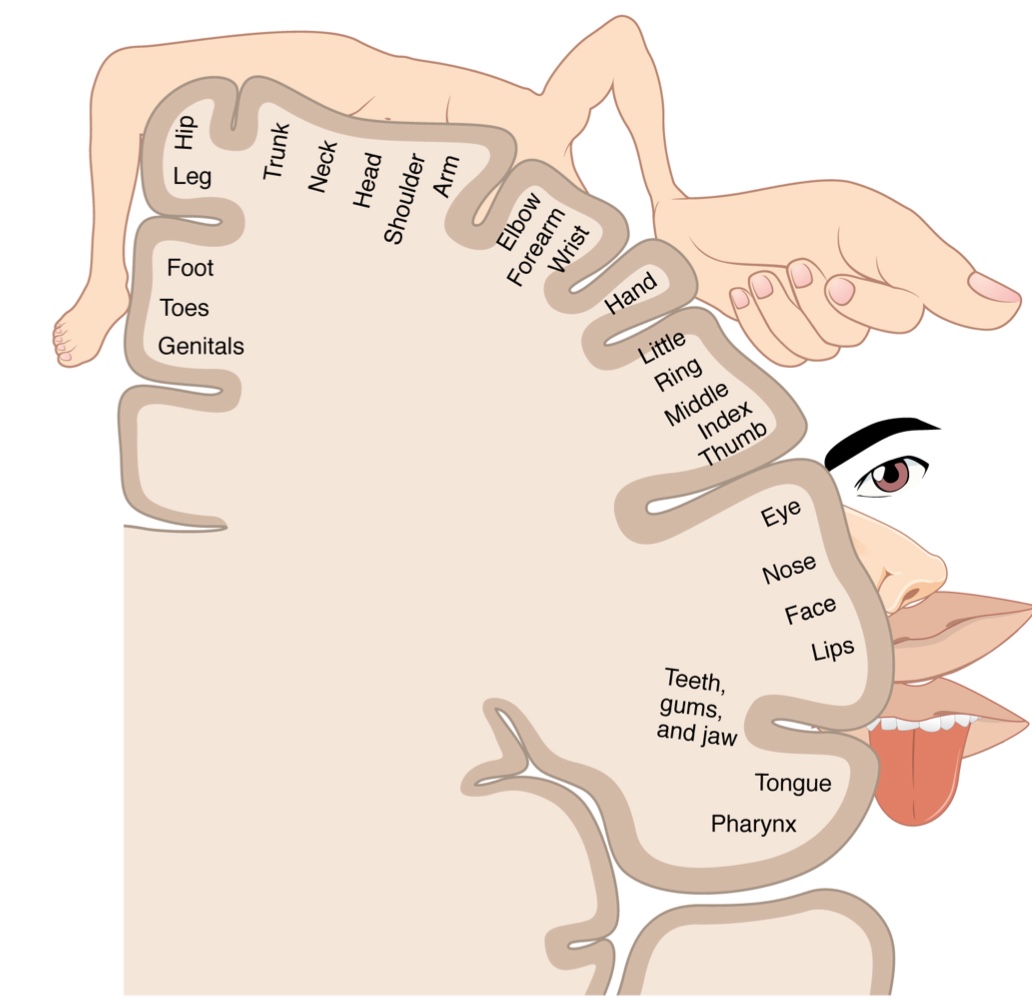
The Sensory Homunculus
Definition: Meaning "little man" in Latin, the homunculus is a topographical map of the human body laid across the somatosensory cortex.
Body Mapping Arrangement:
Medial Face: Represents the external genitals, feet, and lower legs within the longitudinal fissure.
Parietal Lobe Surface: The map proceeds laterally for the thighs, hips, trunk, shoulders, arms, and hands.
Lateral Sulcus: The head and face are mapped lateral to the fingers as the gyrus approaches this sulcus.
Structural Continuity: This organization continues the mapping seen in both the dorsal column system (fasciculus gracilis for lower body; fasciculus cuneatus for upper body) and the trigeminal system. Topography is strictly maintained through thalamic relays.
Cortical Representation: The map is not a scale model but is based on sensitivity. Exaggerated areas are allocated to highly sensitive regions (e.g., fingers and lower face), while less sensitive regions (e.g., shoulders and back) occupy much smaller areas of the cortex.
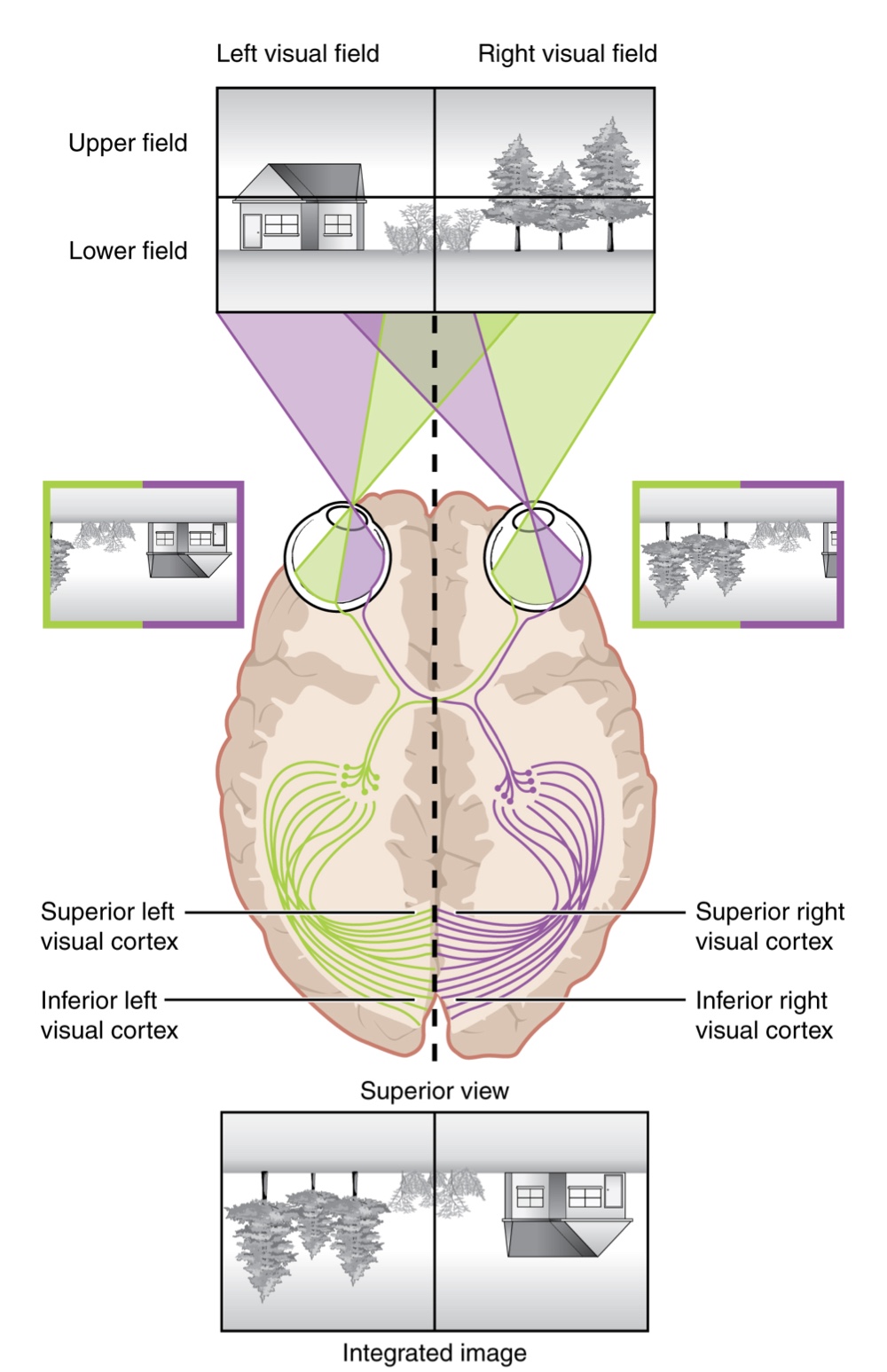
Visual Cortical Topography
The topographic relationship between the retina and the visual cortex is maintained throughout the visual pathway.
Lateral Sorting: The visual field is projected onto the two retinae with sorting at the optic chiasm; the right visual field is processed in the left visual cortex, and the left visual field is processed in the right visual cortex.
Superior/Inferior Inversion: Light from the superior visual field falls on the inferior retina, and vice versa. This topography is maintained such that the superior region of the visual cortex processes the inferior visual field.
Image Processing: As it enters the visual cortex, visual information is inverted (up is down) and reversed (left is right). The cortex then processes this information so that the final conscious perception is correct.
Magnification of the Fovea: Information from the foveal region of the retina is processed in the center of the primary visual cortex, while peripheral regions are processed toward the edges. Similar to the sensory homunculus, the area of the visual cortex dedicated to the fovea is disproportionately larger than those for peripheral vision.
Cortical Flexibility: An experiment in the 1960s demonstrated cortical adaptability. Subjects wearing prism glasses that inverted their visual field were able to acclimate after a few days, eventually behaving as if the world were represented correctly.
Hierarchy of Sensory Processing
Although the cortex contains specialized regions for processing distinct information (such as the visual, somatosensory, and gustatory cortices), the brain integrates these separate modalities into a seamless percept, allowing us to experience the world as a continuous whole.
In the cerebral cortex, sensory processing follows a specific hierarchical sequence:
Primary Sensory Cortex: The initial stage where sensory processing begins.
Association Area: The intermediate stage where information is further refined.
Multimodal Integration Area: The final stage where information from various sensory modalities is combined.
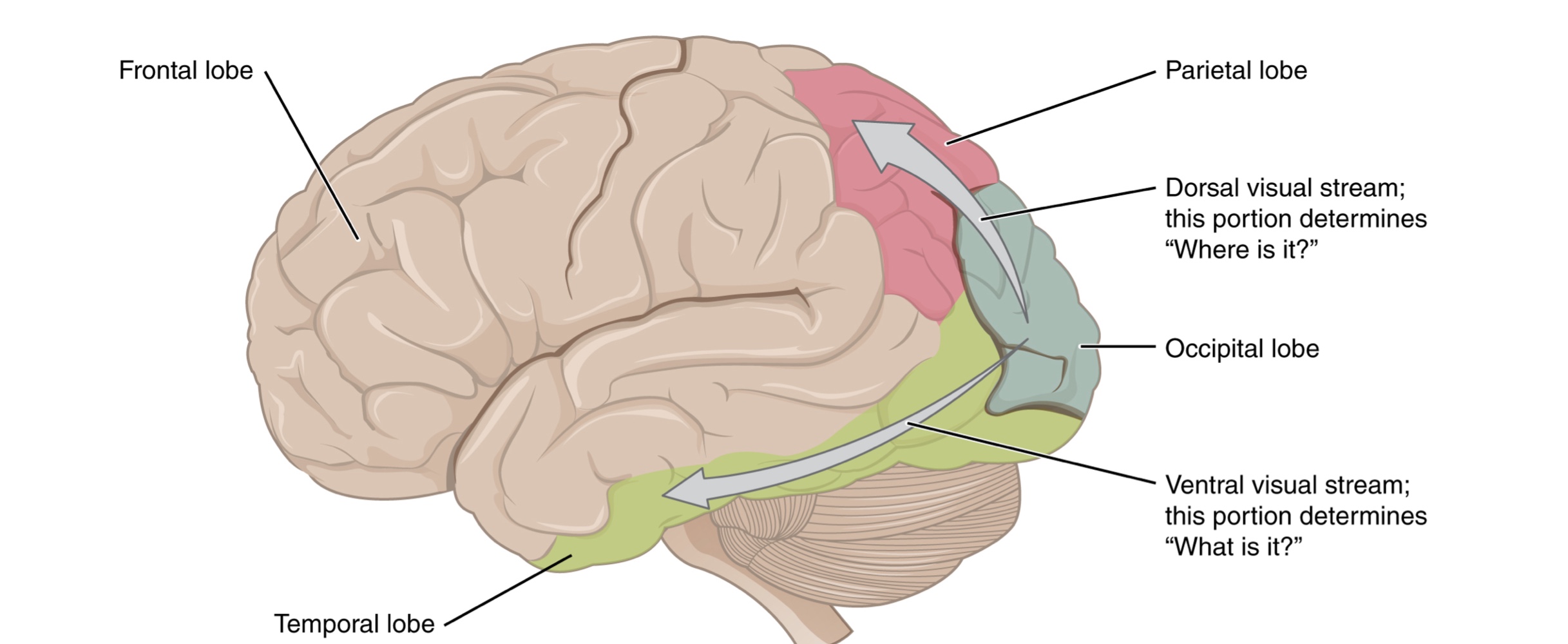
Visual Processing Streams: Information processed in the association areas is sent to either the temporal or parietal lobes via two separate streams:
Ventral Stream: Projects into the temporal lobe; it identifies visual stimuli and their significance. It interacts with non-visual cortex and contributes to visual memories.
Dorsal Stream: Projects into the parietal lobe; it locates objects in space and assists in guiding body movements. It interacts with somatosensory areas and influences motor functions in the frontal lobe.
Ch. 14.3 Motor Response
Cortical Responses
Sensory stimuli registered through receptors are relayed along ascending pathways to the cerebral cortex for processing.
The progression of sensory perception moves from the primary sensory areas to associative processing and finally to integration in multimodal areas of the cortex.
This integration allows sensory perceptions to be incorporated into memory and initiates motor processing in distinct cortical areas.
The Frontal Lobe and Executive Functions
While sensory processing occurs in the occipital, temporal, and parietal lobes, motor functions are primarily controlled by the frontal lobe.
Prefrontal Cortex (PFC): The most anterior regions of the frontal lobe responsible for executive functions, which are higher cognitive processes leading to goal-directed behaviors.
Working Memory: Known as a "mental scratch pad," it helps an individual organize and represent information that is not in the immediate environment.
Attention: The prefrontal lobe manages focus by inhibiting distracting thoughts and actions to achieve specific goals.
Personality and Cognitive Health
The prefrontal cortex is integral to personality, governing an individual's intentions and how they accomplish plans.
Phineas Gage (1848): A famous clinical case of prefrontal cortex damage where a metal spike impaled the region.
Though he survived, his personality changed from hardworking and amiable to irritable, temperamental, and lazy.
Modern evidence of his later life as a stagecoach driver suggests the brain possesses a significant ability to recover even from major trauma.
Secondary Motor Cortices
In generating motor responses, the executive functions of the prefrontal cortex initiate actual movements.
Defining the Prefrontal Area: Any region of the frontal lobe that does not elicit movement when electrically stimulated. These are primarily located in the anterior part of the frontal lobe.
Projections: The prefrontal areas project into the secondary motor cortices, which include the premotor cortex and the supplemental motor area.
Planning and Coordination:
These areas are most active leading up to the initiation of movement. For example, they prepare the body for necessary movements in anticipation of a stimulus, such as a traffic light changing.
Premotor Cortex: Located more laterally; it aids in controlling core muscles to maintain posture during movement.
Supplemental Motor Area: Located more medially and superiorly; it is hypothesized to be responsible for planning and coordinating movement. It also manages sequential movements based on prior experience (learned movements).
Specialized Motor Planning Centers:
Frontal Eye Fields: Positioned adjacent to the secondary motor regions, they are responsible for moving the eyes in response to visual stimuli and have direct connections to the superior colliculus.
Broca’s Area: Located anterior to the premotor cortex and primary motor cortex; it is responsible for controlling the movements of the structures involved in speech production.
The area is named after the French surgeon who studied patients who could understand speech but not produce speech sounds, suggesting a damaged or underdeveloped Broca's area.
Primary Motor Cortex
The primary motor cortex is located in the precentral gyrus of the frontal lobe and serves as the principal point for outputting motor signals.
Historical Discovery
Neurosurgeon Walter Penfield described much of the basic understanding of this region through electrical stimulation of the cerebrum surface while patients were under local anesthesia.
This research led to the observation that stimulating the precentral gyrus directly results in muscle movement.
Function and Pathways
The primary motor cortex receives input from several brain areas that assist in planning movement.
Its principal output stimulates spinal cord neurons, which in turn stimulate skeletal muscle contraction.
Organization: The Motor Homunculus
The motor cortex is arranged as a topographical map of the body, creating a motor homunculus.
Mapping Arrangement:
Medial Wall: Neurons responsible for the feet and lower legs.
Crest of the Longitudinal Fissure: Represents the thighs, trunk, and shoulders.
Lateral Face of the Gyrus: Represents the hands and face.
Cortical Allocation and Innervation
Like the sensory homunculus, space is not proportional to physical size but is based on the complexity of movement.
Fine Movements: The greatest amount of cortical space is given to muscles performing agile movements, such as the fingers and lower face.
Power Muscles: Regions that perform coarser movements, such as the back and buttock muscles, occupy much less space on the motor cortex.
Descending Pathways
The motor output from the cortex descends into the brain stem and to the spinal cord to control the musculature through motor neurons.
Betz Cells: These are large cortical neurons located in the primary motor cortex that synapse with lower motor neurons in the brain stem or in the spinal cord.
Major Descending Pathways: The axons of Betz cells travel along 2 main tracts named for their origin in the cortex and their targets:
Corticobulbar Tract: Targets the brain stem (the term "bulbar" refers to the brain stem as the bulb or enlargement at the top of the spinal cord).
Corticospinal Tract: Targets the spinal cord.
Both tracts are responsible for the conscious or voluntary movements of skeletal muscles.
Functional Directionality:
Corticobulbar Tract: These axons are ipsilateral, meaning they project from the cortex to the motor nucleus on the same side of the nervous system.
Corticospinal Tract: These axons are largely contralateral, crossing the midline of the brain stem or spinal cord so that the right motor cortex controls muscles on the left side of the body, and vice versa.
Anatomical Course of the Corticospinal Tract:
Internal Capsule: A bundle through which the tract passes in the deep white matter of the cerebrum, located between the caudate nucleus and the putamen.
Cerebral Peduncles: The location where the tract passes through the midbrain before burrowing through the pons.
Pyramids: Upon entering the medulla, the tracts form these large white matter structures
Pyramidal Decussation: The defining landmark at the medullary-spinal border where most fibers in the corticospinal tract cross over to the opposite side of the brain. At this point, the tract separates into 2 parts with control over different domains of the musculature.
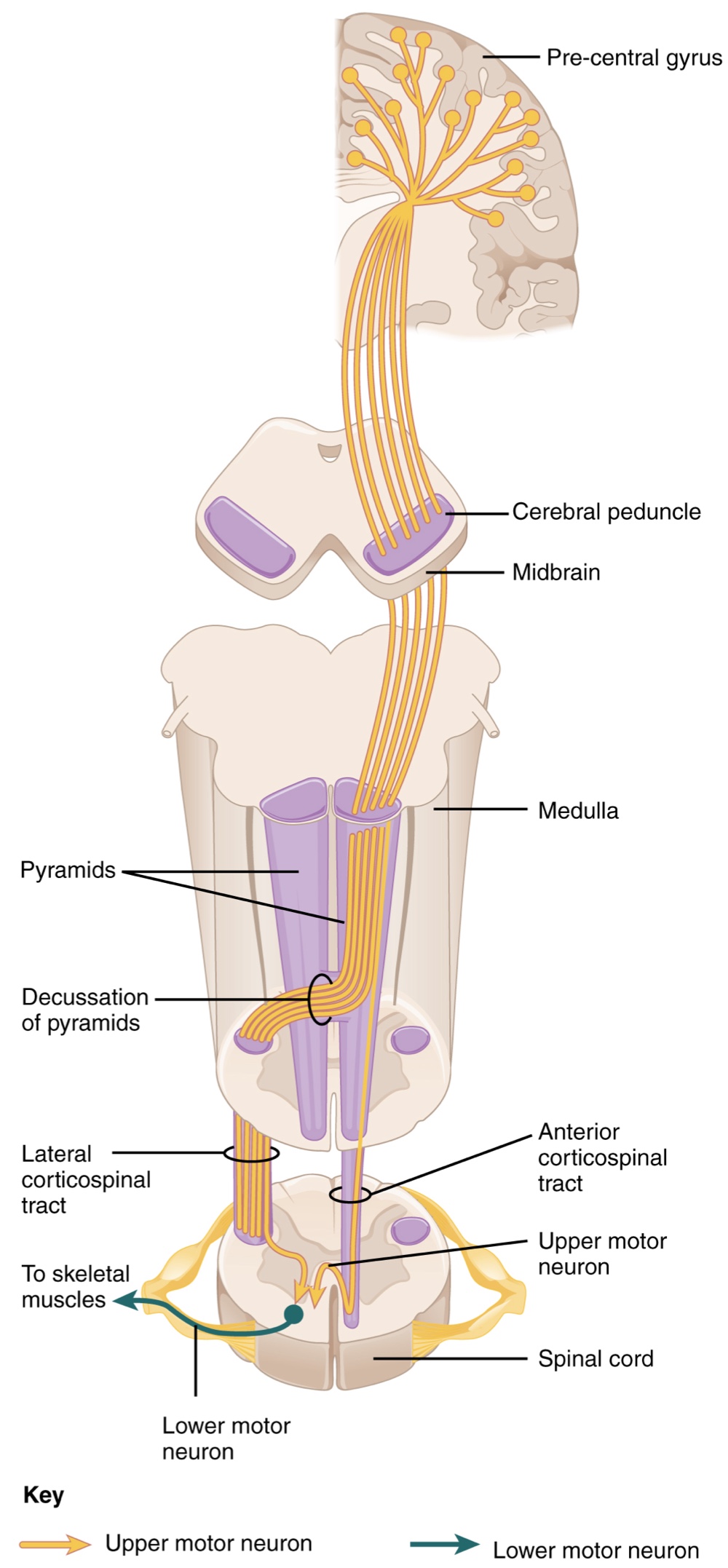
Appendicular Control
The lateral corticospinal tract is composed of the fibers that cross the midline at the pyramidal decussation
The axons cross over from the anterior position of the pyramids in the medulla to the lateral column of the spinal cord.
These axons are responsible for controlling appendicular muscles.
Muscle Regulation and Anatomy:
This influence over the appendicular muscles means that the lateral corticospinal tract is responsible for moving the muscles of the arms and legs.
The ventral horn in both the lower cervical spinal cord and the lumbar spinal cord both have wider ventral horns, representing the greater number of muscles controlled by these motor neurons.
Cervical Enlargement: Particularly large because there is greater control over the fine musculature of the upper limbs, particularly the fingers.
Lumbar Enlargement: Not as significant in appearance because there is less fine motor control of the lower limbs.
Axial Control
The anterior corticospinal tract is responsible for controlling the muscles of the body trunk.
Pathway and Decussation
These axons do not decussate in the medulla. Instead, they remain in an anterior position as they descend the brain stem and enter the spinal cord.
These axons travel to the specific spinal cord level where they will synapse with a lower motor neuron.
Upon reaching the appropriate level, the axons decussate, entering the ventral horn on the opposite side of the spinal cord from which they entered.
In the ventral horn, these axons synapse with their corresponding lower motor neurons.
The lower motor neurons are located in the medial regions of the ventral horn because they control the axial muscles of the trunk.
Bilateral Coordination
Because movements of the body trunk involve both sides of the body, the anterior corticospinal tract is not entirely contralateral.
Some collateral branches of the tract project into the ipsilateral ventral horn to:
Control synergistic muscles on that side of the body.
Inhibit antagonistic muscles through interneurons within the ventral horn.
Through the influence of both sides of the body, the anterior corticospinal tract coordinates postural muscles in broad movements of the body.
These coordinating axons are often considered bilateral, as they are both ipsilateral and contralateral.
Extrapyramidal Controls
Other descending connections between the brain and the spinal cord are referred to as the extrapyramidal system.
The name originates from the fact that this system is outside the corticospinal pathway, which includes the pyramids in the medulla.
Brain Stem Pathways
Tectospinal Tract: Projects from the midbrain to the spinal cord.
It is essential for postural movements driven by the superior colliculus (the tectum).
Reticulospinal Tract: Connects the reticular system (a diffuse region of gray matter in the brain stem) with the spinal cord.
It influences trunk and proximal limb muscles related to posture and locomotion, contributes to muscle tone, and influences autonomic functions.
Vestibulospinal Tract: Connects the brain stem nuclei of the vestibular system with the spinal cord.
Allows posture, movement, and balance to be modulated on the basis of equilibrium information provided by the vestibular system.
Subcortical and Basal Nuclei Influence
The pathways of the extrapyramidal system are influenced by subcortical structures.
Connections between the secondary motor cortices and the extrapyramidal system modulate spine and cranium movements.
The basal nuclei, which regulate movement initiated by the CNS, influence the extrapyramidal system as well as its thalamic feedback to the motor cortex.
Cerebellar Integration and Feedback
The conscious movement of muscles is complex; during movement, muscles relay information back to the brain, which then sends "revised" instructions.
The cerebellum is vital for this process, as it compares cerebral motor commands with proprioceptive feedback.
Information Streams:
Branches of corticospinal fibers synapse in the pons and project to the cerebellum.
Proprioceptive sensations of the dorsal column system have a collateral projection to the medulla that also projects to the cerebellum.
Red Nucleus and Rubrospinal Tract:
Conflicts detected in the cerebellar cortex between motor commands and body position cause the cerebellum to stimulate the red nucleus of the midbrain.
The red nucleus then sends corrective commands along the rubrospinal tract (named after the word for red, like "ruby").
Coordination and External Factors
Walking in Water: An original command to walk is adjusted by the cerebellum via the rubrospinal tract to overcome water resistance (e.g., by taking larger steps).
Alcohol Inhibition: Alcohol inhibits the cerebellum's ability to interpret proprioceptive feedback.
This leads to severely affected coordination and balance, making tasks like walking a straight line or touching the tip of the nose difficult.
Ventral Horn Output
The somatic nervous system provides output strictly to skeletal muscles.
Lower Motor Neurons: Responsible for the contraction of these muscles.
Location: Found in the ventral horn of the spinal cord.
Structure: These are large, multipolar neurons with a corona of dendrites surrounding the cell body and an axon that extends out of the ventral horn.
Path: Axons travel through the ventral nerve root to join the emerging spinal nerve.
Because they need to reach muscles in the periphery of the body, these axons are relatively long.
For example, lumbar motor neurons innervating the feet can have axons up to a meter in length.
To support these long axons, cell body diameters may be on the order of hundreds of micrometers.
Motor Units
Motor neuron axons branch to innervate multiple muscle fibers.
A motor unit is the combination of a single motor neuron and all the muscle fibers it controls.
Size and Precision: Motor units vary in size; the number of muscle fibers in a unit corresponds to the precision of control for that muscle.
Large Units: In muscles like the quadriceps, a unit may contain up to 1000 muscle fibers.
Small Units: In extraocular muscles, a unit may have only 10 fibers for higher precision.
Muscles with finer motor control have more motor units connecting to them, which requires a larger topographical field in the primary motor cortex.
The Neuromuscular Junction (NMJ)
The neuromuscular junction is a specialized synaptic structure where multiple axon terminals synapse with the muscle fiber sarcolemma.
Mechanism: The synaptic end bulbs of the motor neurons secrete acetylcholine, which binds to receptors on the sarcolemma.
Depolarization: This binding opens ligand-gated ion channels, allowing cations to move across the sarcolemma. This depolarizes the membrane and initiates muscle contraction.
Reliability: Unlike other synapses where graded potentials must reach a threshold, activity at the NMJ reliably leads to muscle fiber contraction with every nerve impulse received.
Variable Strength: The strength of contraction and the total number of fibers that contract can be influenced by the frequency of the motor neuron impulses.
Reflexes
Reflexes are basic elements of the somatic nervous system that provide rapid, involuntary responses to stimuli.
Simple somatic reflexes do not involve the higher brain centers associated with conscious or voluntary movement.
They are classified as either spinal or cranial, depending on the nerves and central components involved.
The Withdrawal Reflex
A primary example of a somatic reflex involves withdrawing the hand from a hot stove.
Since the neuromuscular junction is strictly excitatory, the biceps brachii contracts when its motor nerve is active.
To allow for movement, the antagonist muscle, the triceps brachii, must relax.
Process of Inhibition: Skeletal muscles do not actively relax; instead, the motor neuron must be inhibited.
An interneuron in the dorsal horn of the spinal cord receives a synapse from the sensory neuron and inhibits the motor neuron for the triceps.
This occurs by releasing neurotransmitters that hyperpolarize the motor neuron, making it less likely to initiate an action potential.
This allows the triceps to relax, facilitating faster withdrawal and minimizing tissue damage.
Stepping on a Stimulus: Nociceptors trigger the motor neurons for the tibialis anterior, causing dorsiflexion of the foot.
At the same time, an inhibitory interneuron (activated by a collateral branch of the nociceptor fiber) inhibits the gastrocnemius and soleus muscles to cancel plantar flexion, preventing the foot from pressing further into the stimulus.
The Stretch Reflex
This reflex is triggered when a skeletal muscle is stretched, activating a muscle spindle receptor.
The sensory axon from this receptor causes direct contraction of the muscle and utilizes a collateral branch to inhibit the motor neurons of the antagonist muscles.
Function: Helps maintain muscle length at a constant level.
Clinical Example: The knee-jerk reflex, which is elicited by striking the patellar ligament with a rubber hammer during a physical exam.
The Corneal Reflex (Eye Blink Reflex)
A specialized reflex focused on protecting the surface of the eye from tactile stimuli or even bright light.
Pathways:
Sensory Component: Tactile stimuli travel through the trigeminal nerve, while information regarding bright light travels through the optic nerve.
Motor Response: The signal travels via the facial nerve and innervates the orbicularis oculi muscle on the same side to initiate blinking.
Evaluation: This reflex is commonly tested in clinical settings using a gentle puff of air or a cotton-tipped applicator.