Urinary System
Functions of urinary system
Storage and excretion of urine
Filtration of blood
release of hormones (erythropoietin)
regulation of erythrocyte production
Regulation of ions and acid/base levels
Clinical progression of kidney disease
Kidneys are unable to filter imbalances, resulting in accumulation of uremic toxins
Kidney is no longer able to excrete erythropoietin, and therefore bones aren’t able to produce RBCs
Anemia leads to heart failure
Embryology
Urogenital system derives from embryonic tissue called intermediate mesoderm, which runs down the posterior abdominal wall
Urogenital ridge is formed from condensed intermediate mesoderm
3 sets of embryonic organs
Pronephros/pronephric duct
Used to start development of the kidneys; exist only to degenerate. Degeneration triggers formation of mesonephros
Pronephric duct remains
Mesonephros
Develop as sacs that functions in urine production
Pronephric duct becomes mesonephric duct
Remain until around week 10
Metanephros
Begin developing at week 5, are fully functional by week 10
Develop from ureteric buds and metanephric blastema
Ureteric buds will develop into structures that COLLECT urine
Ureter
Renal calyces
Renal pelvis
Collecting ducts
Metanephric blastema will develop into structures that PRODUCE urine
Glomerular capsule
Proximal convoluted tubule
Nephron looop
Distal convoluted tubule
Urorectal septum divides the cloaca into urogenital sinus and anorectal canal at week 7
Urogenital sinus will develop into urinary bladder and urethra
Weeks 6-9, kidneys migrate to more superior position in natal abdominal cavity
During ascent, kidneys receive bloodflow from temporary vessels
Week 9, kidneys are in final location and receive permanent renal arteries from abdominal aorta
Indifferent duct system
Developed by all embryos, genetics will determine which duct system is retained
Retention of mesonephric duct results in penis and associated structures
Retention of paramesonephric duct results in uterus and associated structures
Organs of urinary system
Paired kidneys
Filter waste from bloodstream
convert filtrate into urine
Location/description of kidney
Superior border is just below T12
Inferior border is around L3
Retroperitoneal (covered, not wrapped with peritoneum)
Suprarenal/adrenal gland sits on top each kidney
Kidney is reddish brown
R is slightly inferior to L
Surrounded by two layers of fat to absorb trauma
Ureters, urinary bladder, urethra
referred to as urinary tract, transport urine out of body
Structure of kidney
Renal capsule
Dense, irregular connective tissue
maintains shape of kidney and protects from damage/infection
Concave medial border referred to as HILUM
Divided into cortex (outer) and medulla (inner) and renal pelvis
Medullary pyramids act to increase surface area of medulla
Renal papilla connect medullary pyramids to renal pelvis
Urine is produced:
in nephrons
Flows to renal papilla → minor calyx → major calyx → renal pelvis → ureter → urinary bladder
Primary function of kidney is blood filtration
Renal veins bring deoxygenated blood back to IVC
Renal veins lie ANTERIOR to renal arteries
Asymmetrical due to location of IVC on R side of body
L Gonadal vein drains into L renal vein
L Renal vein is longer than R renal vein
Nutcracker syndrome
Entrapment of renal vein between sup mesenteric artery and abdominal aorta, blocking gonad drainage
5 segmental arteries branch from renal artery
Order of blood supply to kidney WILL BE TESTED
Renal artery
Segmental arteries
Interlobar arteries (between pyramids)
Arcuate arteries (across tops of pyramids)
Cortical arteries (penetrate cortex and give afferent atrioles)
Blood supply to Glomerulus
Cortical arteries branch off arcuate arteries and penetrate cortex
AFFERENT arterioles are the smallest branches
Created capillary balls called glomeruli
Efferent arterioles exit glomerulus
Nephron: functional unit of kidney
Corpuscle
Proximal convoluted tubule
Nephron loop of henle
Distal convoluted tubule
Collecting ducts
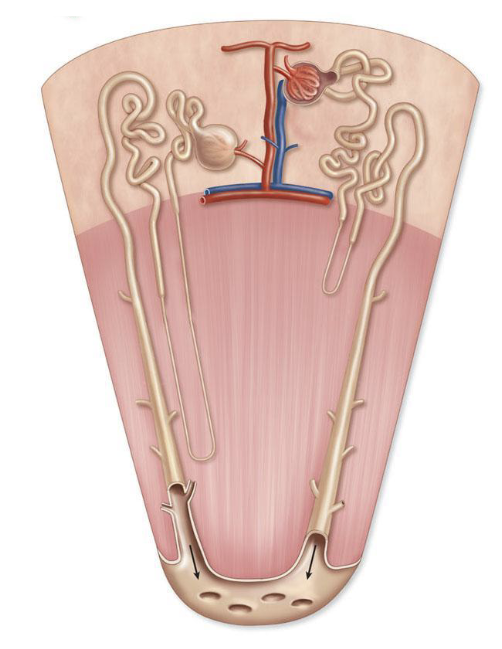
Nephron MODIFIES blood filtrate to form urine from 3 processes
Filtration
Movement of substances from blood to capsular space
Reabsorption
Movement of substances from tubular fluid back to blood
Secretion
Movement of substances from blood to tubular fluid
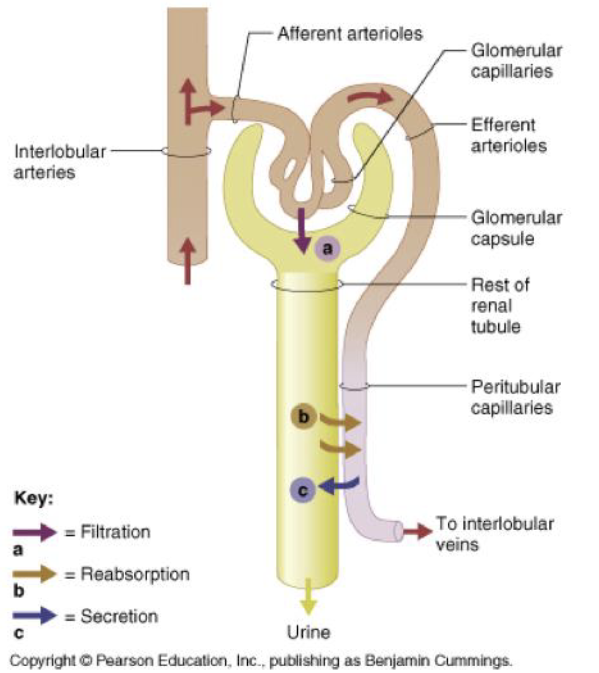
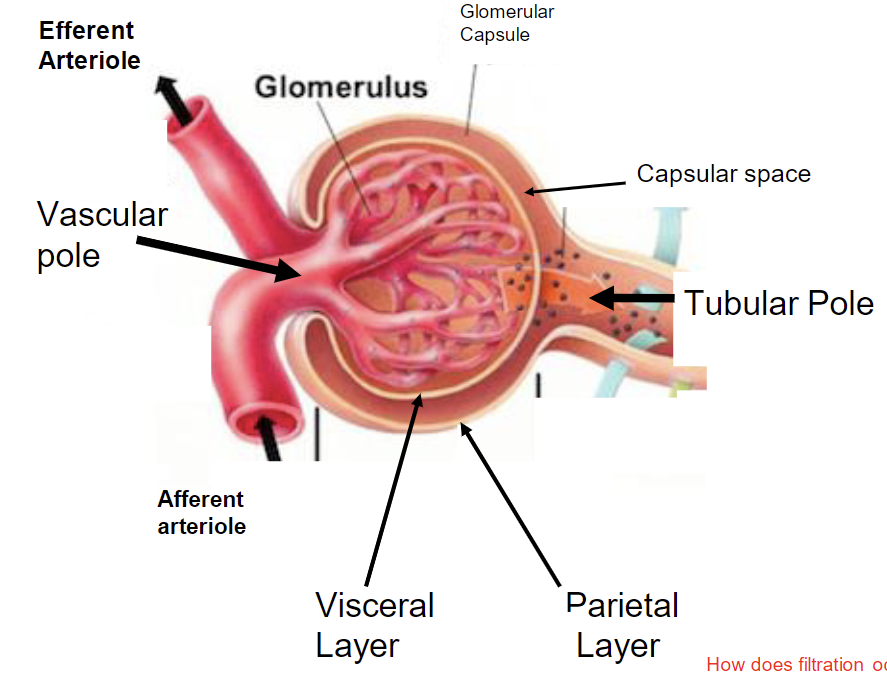
Structure of renal corpuscle
Renal corpuscle is made of
Glomerulus
glomerular capsule
2 poles
vascular
tubular
2 layers
Visceral
adhered to glomerulus and made of podocytes
parietal
simple squamous epithelium
capsular space lies between 2 layers and collects filtrate
filtration occurs because of increased pressure in glomerulus
Afferent arteriole is larger than efferent
glomerulus is tangle of capillaries that extend from afferent arteriole
glomerular capsule surrounds glomerulus
Filtration membrane is made of
Fenestrated endothelium (glomerulus)
Visceral layer of glomerular capsule
made of podocytes with filtration slits
allows only smallest solutes to exit glomerulus
pressed out due to high pressure in glomerulus
not selective filtration
Proximal convoluted tubule
Simple cuboidal epithelium w/ microvilli
increase reabsorption capacity
Actively reabsorbs and secretes substances to modify filtrate
Lumen looks “fuzzy” bcuz of microvilli
Nephron loop
has 2 limbs
Loop down into medulla and back into cortex
primary function is reabsorption of water back to blood
2 types of nephrons
Cortical nephrons
active during normal conditions
juxtamedullary nephrons
active during periods of high activity, produce concentrated urine
Distal convoluted tubule
Simple cuboidal epithelium with SPARSE microvilli
primary function is secretion and absorption
Lumen is clear and crisp
Blood flow around nephron
Peritubular capillaries
surround proximal and distal convoluted tubules
vasa recta
surrounds nephron loop
Collecting tubules
act under influence of anti diuretic hormone and aldosterone
Limits loss of water and Na ions from blood
Increase absorption of water back to blood
Urine exits kidney through ureter
fibromuscular tubes that carry urine from pelvic cavity to empty into urinary bladder
insert into posterolateral wall of bladder
3 layers of ureter
mucosa (transitional epithelium)
muscularis (smooth muscle)
produce peristaltic contractions to produce unidirectional movement (like esophagus/intestines)
adventitia (collagen/elastic fibers)
Ureter enters bladder at acute angle to allow ureter wall to form 1 way valve
Bladder is posterior and “tipped over” pubic symphysis
allows bladder to stand up and expand
bladder is retroperitenial
4 tunics of urinary bladder
mucosa
transitional epithelium
allows epithelium to stretch
mucosal folds called rugae allow for increased storage
submucosa
dense irregular CT
Muscularis
detrusor muscle
adventitia
outer loose ct, collagen and elastic fibers
Trigone is triangular area formed by entrance of ureters and formation of internal urethral sphincter
Urethra is made of smooth muscle from bladder
Internal urethral sphincter
made of smooth muscle
under autonomic control
external urethral sphincter
at distal end of urethra
made of skeletal muscle
voluntary control
Nervous control of bladder
Parasympathetic = pee
stimulate micturition
sympathetic = storage
inhibit micturition
Stretch receptors in bladder trigger micturition reflex center
impulses travel to detrusor muscle and internal sphincter
smooth muscle in internal sphincter relaxes
smooth muscle in detrusor contracts
person must consciously relax external sphincter