DANB RHS Ultimate Review
Radiology is the study of radiation as it’s used in medicine
History Of Radiology
Discovered by Wilhelm Conrad Roentgen (German physicist) on November 8, 1895
X-rays were referred to as roentgen rays
Radiology was referred to as roentgenology
Radiographs were referred to as roentgenographs
Roentgen was awarded the first Nobel prize in Physics in 1901
Otto Walkhoff made the first DENTAL radiograph
Dr. C. Edmund Kells is credited with the first practical use of radiographs in dentistry in 1896
Suffered from radiation exposure
Dental radiology has evolved overtime and new technology continues to improve dental images
Radiation Physics and Biology
Everything is composed of energy and matter
Atoms are the basic form of matter and they contain energy
Energy is the ability to do work
Matter is anything that takes space and has form or shape, made of molecules
The nucleus is made up of protons and neutrons
Protons have positive electrical charges
Neutrons has negative or no electrical charges
Electrons are small negatively charged particles that have little mass, they orbit the nucleus of the atom
Ionization:
Ionization is the process by which an atom or molecule acquires a negative or positive charge by gaining or losing electrons to form ions.
Producing an ion (an atom that gains or loses an electron and becomes electrically unbalanced) is a process called ionization
In the context of dental radiology, ionization occurs when X-rays or other forms of ionizing radiation interact with tissue. This can lead to disruptions in atomic and molecular structures, potentially resulting in biological effects
Properties of X-Rays:
X-rays are a form of energy that can penetrate matter
The Shorter the wavelength, the greater the energy and vice versa
Short wavelengths with high frequency = more energy
Long wavelengths with low frequency = less energy
Dental radiographs need short wavelengths or hard radiation — they have high frequency, high energy, and high penetrating power
Types of Radiation
Primary radiation →made of x-rays that come from the target of x-ray tubes
Secondary radiation →x-radiation that is created when the primary beam interacts with matter
Scatter radiation →form of secondary radiation that happens when an x-ray beam is deflected from its path when it comes into contact with matter
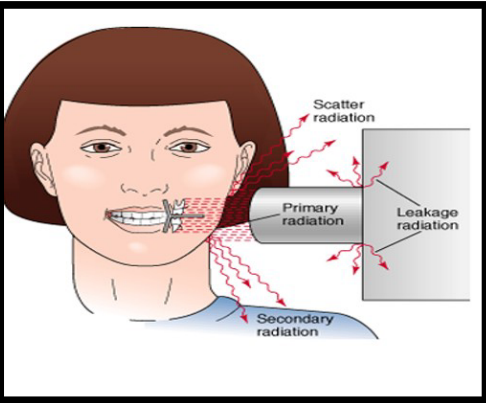
Primary radiation:
comes from the central beam of x-ray tube
has high energy, short wavelength, and travels in a straight line
Secondary Radiation
Primary x-rays come into contact with matter or strike the patient
Waves are longer
long = less energy
less energy = less diagnostic x-ray
Scatter Radiation
Defected from its path when it strikes matter
Scatters in all directions (hint hint) → DANGEROUS to everyone
Reason why operator must stand 6 feet away from the patient or behind a barrier that is thick
Leakage Radiation
Escapes in all directions from tubehead
X-rays must be checked for leakage and can’t be used until problem is addressed
Not useful
Long wavelengths cause harm only
X-ray anatomy
Plugged into wall outlet and when turned on the electrical currents enter the control panel
The current travels from the control panel to the tubehead through the electrical wires in the extension arm
Current travels through the step-down transformer to the filament to the cathode
The Filament circuit uses 3 to 5 V to heat the tungsten filament in the cathode portion of the x-ray tube
By heating the filament, the thermionic emission electrons are released
When the exposure button is pushed the high voltage circuit is activated
The electrons are accelerated across the x-ray tube to the anode
When the electrons strike the tungsten target, the kinetic energy is converted to x-ray energy and heat
Less than 1% of the energy is converted to x-rays and the remaining is lost as heat
Heat is carried away from the copper stem and absorbed by the oil in the tubehead
X-rays travel through the uleaded glass window, tubehead seal, and aluminum filter
Aluminum filter removes the long wavelengths
X-ray beam travels though the collimator
The beam then travels down the lead-lined PID and exits at the end of the PID
Dental X-Ray Machine
Tubehead:
Contains the x-ray tube that produces dental x-rays
Made of leaded glass or aluminum to keep the oil in the tubehead and acts as a filter for the x-ray beam
The metal body of tubehead is called metal housing filled with insulating oil
the x-ray tube is where x-rays are produced
Made of glass
About 6 inches long and 1 inch in diameter
PID
Lead lined to aim the x-ray bean to mouth
Placed against patients face
Cylinder or rectangle
Extension Arm
Moves
important in positioning the tubehead
Control panel
Contains master switch, indicator light, selector button, and exposure button
Interactions of X-Rays with matter
When x-rays come in to contact with matter:
No interaction
Photoelectric effect →when light shines on a metal, electrons are ejected from the surface of the metal
Compton scatter →x-rays are scattered on a material with an x-increase in wavelength
Scatters off
Radiolucent and Radiopaque Characteristics
Radiolucent structures allow x-rays to pass through them
Is dark or black on the radiograph
Radiopaque don’t allow x-rays to pass through them
appears white or light grey
Characteristics of the X-ray
Quality describes the energy or penetrating ability of x-ray beam
Quantity refers to the number of x-rays produced
Intensity combines quality and quantity →# of photons and energy of each photon
The sharpness and detail of the x-ray is determined by the movement, film speed, PID placement, and subject matter
Contrast
Contrast of image clearly shows radiopaque white of metal restoration, radiolucent black of air, and many shades of grey between
Contrast = difference between shades of grey
high kilovoltage produces more penetrating x-rays and lower radiographic contrast
90 kVp (maximum voltage applied) setting requires less exposure time and produced a radiograph that has low contrast
70 kVp requires slightly longer exposure time and produces a radiograph with high contrast
Higher kVp penetrates through areas BETTER and radiation does is LOWER
BUT a higher kVp will decrease the image contrast
Density
Density = overall blackness or darkness of an image
The correct density allows the dentist to see black areas (air spaces), white areas (enamel, dentin, and bone)
the degree of density is determined by the milliampere seconds (mA) —the amount of electrical current flowing through the x-ray tube
mA controls the temperature of the cathode filament →controlling how many electrons are produced
the MORE electrons the MORE x-rays emitted →better quality image
Intensity →combo of # of photons (mA) and the energy of photons (kV)
Geometric Characteristics
Sharpness →detail, resolution, or definition
Distortion →disproportion change in size caused by excessive or insufficient vertical angulation
Magnification →proportionate enlargement of dental image
Radiation Effects
all ionizing radiation is harmful and produced biological changes
entire x-ray area is considered to be a hazard area
Ionization is the process by which electrons are removed from electrically stable atoms
Atoms that lose electrons become positive ions, they are unstable and capable of interacting/damaging other atoms, tissues, or chemicals
Critical organs include: skin, thyroid gland, LENSES OF THE EYE (according to danb), and bone marrow
The effects of radiation may not become evident for many years after x-ray absorbed →called latent period
Radiation exposure has a cumulative effect over lifetime
Acute radiation is when a large dose of radiation is absorbed in a short time
Chronic radiation is when small amounts of radiation is absorbed repeatedly over a long time
Genetic and Somatic Effects
Genetic effects can’t be repaired and can be passed to generations
Reproductive cells are harmed and include sperm and ova
Somatic effects are not passed to the next generation and the consequence of radiation exposure remains with the person effected
Effects cells all over the body
USE LEAD APRON AND THYROID COLLAR FOR PROTECTION
Maximum Permissible Dose
The MPD is 5000 mrem (5.0) per year
Strive for 0
Radiation Safety
The effects of exposure increase every time the individual is exposed →called the long-term effect
Latent period = the period between direct exposure and the development of biological effects
ALARA = As Low As Reasonably Achievable
Using the least amount of radiation possible
Using x-rays during pregnancy is safe and doesn’t need to be altered
Radiation is monitored by a film badge, a pocket dosimeter, or a thermoluminiscent (TLD)
Fast-Speed Film
The film speed refers to the amount of radiation required to create the image
The size of the silver bromide crystals is the main factor in determining the film speed →the larger the crystals, the faster the film
Fast film requires less exposure to produce quality radiographs
Fast-speed film is the most effective method of reducing a patient’s exposure to x-rays
Fast-speed film is available for both intra and extraoral radiography
Digital Radiography
conventional x-ray machine is needed to expose an x-ray
digital radiography:
quick, less radiation, no chemicals, no processing errors, enhance images, etc.
Film is made with an emulsion of silver bromide, silver halide, and silver iodide that is sensitive to radiation
Latent Image: the image which is not visible before processing
Film Sizes:
0 for child
1 for narrow anterior
2 is adult size
3 is preformed bitewing
4 is occlusal size
Film Packet
One corner of the film packet is a small raised bump known as the identification dot
the black film wrapper protects the film from light
the lead foil sheet protects from back-scattered (secondary) radiation
the outer layer seals the film packet
The white side of the film must face the teeth and tubehead and the raised dot toward incisal/occlusal surface
Steps in Film Processing
Development
Rinsing
Fixation
Washing
Drying
Processing Solutions
3 forms: powder, ready-to-use liquid, and liquid concentrate
Intraoral Imaging
FMX
Contains periapical images and bitewing images
has 18-20 images
Periapical
Entire tooth from occlusal surface or incisal edge to a little over the apex →shows the periapical bone
Bitewing
Upper and lower teeth in occlusion
only crown and small portion of root exposed
Extraoral Imaging
Taken when large areas of the skull or jaw must be examined or when patients can’t open their mouths
Includes
Panoramic (360)
Cephalometric projection
Computed tomography (CT)
TMJ projection
Cone beam CT (CBCT)
Frankfort Plane: imaginary line from the middle of the ear to just below the eye socket →must be parallel with the floor
Midsaggital Plane: Imaginary line the evenly divides the face into right and left halves →must be perpendicular to the floor so that the head is not titled (image distortion)
Errors:
Ghost images (metal objects that aren’t removed)
Lead apron artifact (lead apron too high up and shown on x-ray)