advanced techs
pt 1
Tissue Harmonic Imaging (e.g CEUS)
Coded Excitation = B-flow Imaging, Speckle reduction
improves = penetration, speckle reduction, b-flow, improved contrast res & SNR without increasing pulse amplitude
high frequency US allows for good spatial res but poor depth
Coded excitation in ultrasound imaging resolves this issue by increasing the bandwidth of transmitted pulses. This means clinicians can achieve high-resolution images even at deeper tissue levels.
pulses which are much longer than convetional 3-4 cycle imaging transmit pulse = poor axial resolution
thus with coded excitation this is improved by embedding a digital code into the long transmit pulse (SNR also improves by identifying the transmitted code within the received echoes)

“Modulation is the process of encoding information in a transmitted signal, while demodulation is the process of extracting information from the transmitted signal.”
coded excitation methods
Amplitude modulation
Phase modulation = binary encoding
an ensemble of driving voltage pulses are applied to generate a single scan line. basically like having a higher intensity driving pulse
improves penetration depth without loss of AR,
Transmits ultrasound pulses have embedded within them a short code of zeroes and ones (binary code) When the echoes are received, they are passed through a digital/matching filter which is programmed to search for the code.
The longer the coded pulse = the higher will be the SNR
Range side lobes can be cancelled out using a pair of complementary codes known as a Golay pair.
weak echoes from blood are imaged and flow can be seen in gray scale along with the much stronger tissue echoes
Frequency modulation = requires only single pulse per line
varying the frequency of pulses over time, used to encode the transmit signal which can then be decoded upon reception to improve image quality & res
Upon reception, the frequency encoding is removed to timecompress the waveform
results in a shortened pulse which restores AR
b-flow
B-Flow displays the blood flow signals in gray scale imaging throughout the entire field of view. B-Flow is created using digitally coded technology. (phase modulation)
advantages = Detection of true vessel diameter – no tissue overwrite (Blooming) No doppler angle dependency Higher FR and spatial resolution than color flow doppler True flow hemodynamics from large to small vessels Visualization of both high and low velocity flows, simultaneously
applications - vascular, stenosis, thrombus, organ perfusion, plaque
Echoes scattered from tissue are suppressed using a technique called tissue equalization.
Tissue equalization is achieved by applying a line-toline high-pass filter. This suppresses echoes that do not change from line to line, such as those arising from stationary tissue.
PRI = pulse repetition interval = larger value is recommended for slow flow as slow flow detection requires more time separation between pulses so the system can detect the difference in flow profile.
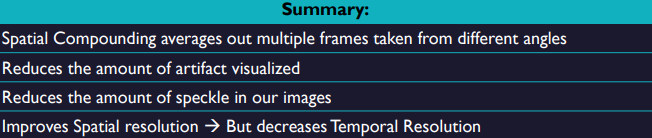
Spatial Compounding
linear convex transducers
have multiple frames with the beam being steered in various directions all taken simultaneously, a lot of info for machine
Once the machine gathers all the needed data, it will average everything together (superimposes several such angled views) in a single ‘compound’ scan
improves smoothness, angle dependent reflectors will be much more apparent (increased # of angles), artifacts less obvious and improved SNR
Shadowing from strong reflectors and enhancement from weak reflectors are less pronounced. SC can be used to improve visualization of structures posterior to a highly attenuating structure
reduces speckle, When the images are compounded, the different speckle patterns at each point in the image are averaged.
reduces frame rate

Extended Field of View Ultrasound (Panoramic Imaging)
creation of one really long image, stitching together a panoramic view, used mostly for vessels and muscles.
As the transducer is sliding, the machine is going to acquire information from the scan lines. The job of the machine is to look for scan lines that ”match up” with each other. Once the machine finds a few t hat ”match up” , it is going to recognize that those are areas that overlap with each other and its going to start displaying the overlap images beside each other, along the line that you are traveling in.
old echo information from previous frames is retained while the new echoes (scan lines) are added to the image in the direction in which the scan plane is moving.
Fusion Imaging
Real-Time Adaptive Filters
High Intensity Focused Ultrasound
pt 2
RTAF= real-time adaptive filters
made to be combined with spatial compounding
almost all adaptive filters are digital filters
can work in real time while preserving a decent FR
post-processing technique
uses a multiscale mathematical greyscale algorithm
a form of AI, new computer processing advancements allow it to work live and perform 350mil calculations per frame.
Improves…
contrast resolution and image quality
decreased noise
increase SNR
pre-processing | post-processing |
affects beam former, alters how sound enters body. manipulates echoes prior to being stored in memory and displayed. (ex: SC, THI, write zoom, persistence). | manipulation of echoes after they have been stored in image matrix, advanced processing on a pixel to pixel level, enhances final output display. (ex: measurements, grey maps, read zoom, RTAF) |
RTAF has 2 phases = analysis and enhancement
they simultaneously enhance structural edges and smooth tissue textures while suppressing artifacts to provide better contrast resolution.
→ these phases are a way for the computer to interpret the image and perform appropriate adjustments to improve image quality.
the algorithm scans the data in the image matrix pixel by pixel to determine relative amplitudes of signals.
then correlates them to a repeatable true tissue signal or a random noise signal artifact.
Analysis phase…
tissues are examined for two characteristics = anisotropic vs isotropic reflection
Anisotropic reflectors | Isotropic reflectors | |
what it is: | true signals from specular reflectors (diaphragm, vessel walls, bone) which are direction dependent. | associated with noise and scatter reflectors (tissue parenchyma) which are direction independent. |
if detected: | directs enhancement phase to smooth selectively along the structural edge to define its boundary. | smooth in all directions to increase homogeneity of parenchyma, suppress speckle artifact. |
Fusion Imaging
The combination of two or more imaging modalities in which two types of images are either put side by side or superimposed.
HIFU = high intensity focused ultrasound
used to interact with tissue via thermal and mechanical mechanisms.
Mechanical effect → cavitation
can generate very high pressures and temps, high shear stress and create microstreaming jets of liquid which can cause pitting of the cell wall.
Thermal effect…
can be used as a non-invasive thermal ablation technique for tumor treatment. (pancreas, liver, kidney, bone, prostate, breast, uterine fibroids, soft-tissue sarcomas).
spatial peak = location where intensity is greatest (most power in smallest area) this represent the focal point in US beams
note: a variety of different energies have been used for thermal ablation of tissues.
HIFU= Produces a focused beam which passes through skin and tissues to necrose a localized region.
this leads to lesion coagulative necrosis → cell death which occurs when blood flow to cells stops of slows (ischemia)
when tumor is ablated a very sharp boundary between dead disrupted cells and live normal cells is created. (no more than 50hm)
HIFU consists of two main components
firstly, a piezoelectric US transducer which is used to deliver the therapeutic US beam, most popular is a concave focusing transducer with a fixed aperture and focal length.
other types → phased array, flat transducer phased array
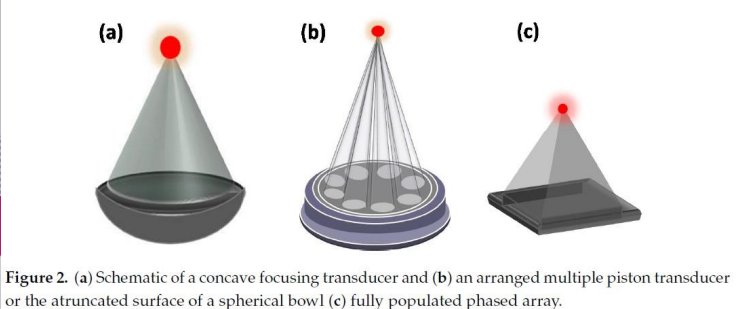
note: The mechanical movement of the transducer determines the position of the focal point, with electronic steering of the ultrasound beam allowing fine control of the focal spot location.
secondly, is the imaging modality used for guidance = US MRI
3 ways to apply HIFU to the body
readily accessible HIFU is applied through an acoustic window on skin by external transducers (kidney)
transrectally (prostate)
interstitial probes in development for treatment of biliary ductal and esophageal tumors, would be inserted orally and in close contact to tumor.
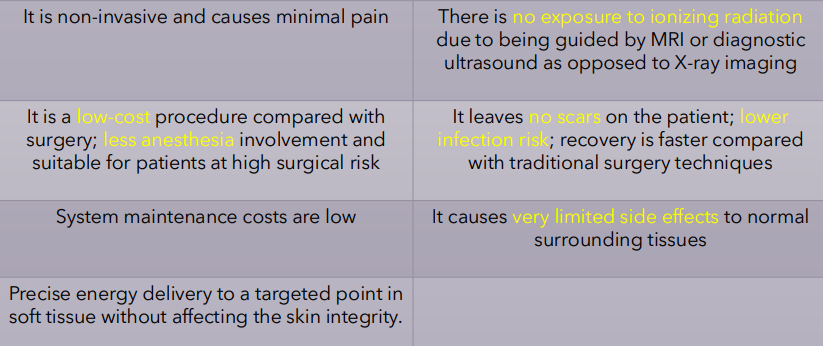
Benefits?
deeper tissue treatment
improved focus on target through its small wavelengths
precise control over shape and location of energy deposition
results in reduced toxicity compared to other ablation techniques
Downsides?
sensitive to movement
near-field heating
long (hours)
Severe full skin burns following extracorporeal shock wave lithotripsy (ESWL) for renal calculi or second-degree burns after shock wave lithotripsy have been reported.
Some patients face post-procedure side effects, such as pain, vomiting, and wounds on their skin.
fistula formation and rib necrosis with delayed rib fracture are also considered to be serious complications that can occur following hepatic and pancreatic cancer treatment
Risks
The heat generated by HIFU can result in a rapid rise in temperature in the exposed tissue to more than 60 °C, which leads to immediate and irreversible cell death in most tissues when it lasts longer than 1 s
thus focus US beam has very high intensity at focal point within a small volume of 1mm diameter and 10mm length, which minimizes potential damage to tissues outside the focus.
