Unit 10 - Cardiovascular Drugs (1)
Unit #10 - Cardiovascular Drugs
Objectives:
- List the 4 compensatory mechanisms of the cardiovascular system.
- List the 5 basic objectives in the treatment of cardiovascular disease.
- Understand the mechanisms the cardiovascular drugs work through (sympathetic vs. parasympathetic).
- Know the different types of cardiovascular drugs to explain what their indications are.
Compensatory Mechanisms of the Cardiovascular System:
- The cardiovascular system has a built-in reserve capacity which allows it to increase its output during times of need and to compensate for cardiac disease.
- The four basic compensatory mechanisms include:
- Increasing the heart rate
- Increasing the stroke volume. (amount of blood pumped out of the ventricles in 1 contraction)
- Increasing the efficiency of the heart muscle.
- Cardiac remodeling.
Objectives in the Treatment of Cardiovascular Disease:
Valvular disease: valves aren’t closing properly
Cardiac arrythmias: irregular heart rate
Myocardial disease: myocardial thickens, DCM (diet related), hypertrophic cardiomyopathy in cats.
Congenital defects: born with them- nerve issues, hypotension/ hypertension, heartworm (depending on location)
- Basic objectives in the treatment of cardiovascular disease include:
- Control rythm disturbances
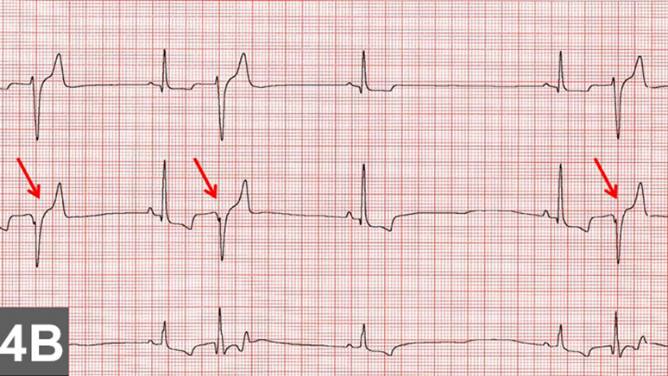 Maintain or increase cardiac output.
Maintain or increase cardiac output.- Increase the strength of contraction.
- Decrease afterload-resistance in the arteries
- Increase the oxygenation of the blood.
- Bronchodilation
- Ancillary Treatment
- Narcotics/sedatives
- Oxygen
Autonomic Nervous System Review:
- The autonomic nervous system is a network of nerves throughout the body that control unconscious processes.
- These are things that happen automatically.
- Connects the brain to most of the internal organs.
- The autonomic nervous system breaks down into three divisions, each with its own job:
- Sympathetic nervous system. (Fight or flight response, transmitters are epinephrine and norepinephrine)
- Parasympathetic nervous system. (Rest and digest, neurotransmitter is acetycholine)
- Enteric nervous system.
![]()
Receptors in the Body for the Autonomic Nervous System:
- α1
- Smooth muscle of blood vessels in skin, gut, kidney
- Epinephrine → vasoconstriction
- Acetylcholine → vasodilate GIT, little effect on skin.
- Smooth muscle of blood vessels in skin, gut, kidney
- α2
- For nerve cells located mostly in CNS
- Norepinephrine, Epinephrine → mentally alert
- Acetylcholine → little effect
- For nerve cells located mostly in CNS
- ß1
- Heart
- Epinephrine → increases force of contraction and heart rate
- Acetylcholine → decreases heart rate
- Heart
- ß2
- Smooth muscle of bronchioles, uterus, gut
- Smooth muscle of blood vessels of heart and skeletal muscle
- Mast cells
- Epinephrine → relax smooth muscle, prevent mast cell release of histamine.
- Acetylcholine → contract smooth muscle of bronchioles, uterus, gut.
Pre-sympathetic terminals
CNS, inhibit parasympathetic response
All SM, glands, organs
Heart- Increase HR, increase contracton
Juxtaglomerular cells (kidneys)- increase BP, Increase blood volume.
All SM, glands, organs
ANS Actions on the Cardiovascular System:
- Epinephrine release:
- α1
- ↑BP
- ↓ blood flow to skin, kidney, gut
- α1
- α2
- Little effect on the cardiovascular system
- β1
- ↑HR and force of contraction
- β2
- Bronchodilation
- Vasodilation
- ↑ blood supply to heart and brain
- α2
- Acetylcholine release:
- α1:
- ↓ BP
- Vasodilation- gut and kidney
- No effect on skin vessels
- β1
- ↓ HR
- β2
- Bronchoconstriction
- α1:
Drug Types:
- There are several drugs with selective stimulation of the receptors.
- Drugs with same action → mimetics
- Parasympathomimetic
- Activate the parasympathetic system & mimic or modify the effects of acetylcholine.
- E.g. – Organophosphates
- Drugs with opposite action → lytics
- Parasympatholytic
- reduces the activity of the parasympathetic nervous system.
- E.g., Atropine
Cardiovascular Drugs:
- Drugs which affect the ANS will have a variety of effects in the body.
 We choose drugs which target the specific organ or body part we need to influence.
We choose drugs which target the specific organ or body part we need to influence. - 5 categories:
- Anti - arrhythmic - Negative inotropes- weakens hearts contractions and slows HR
- Positive inotropes- pump more blood with fewer heartbeats
- Anticholinergics
- Vasodilators
- Diuretics- used to eliminate excess fluid
** Urinary Incontinence Drugs are in their own category.
 Anti-arrhythmic = Negative Inotropes
Anti-arrhythmic = Negative Inotropes
Negative inotrope- slows the heart
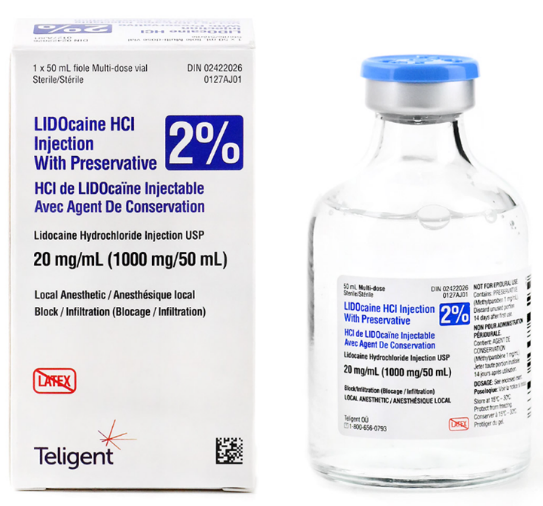
- Lidocaine
- Without epinephrine
- Sodium channel blockers so nerves cannot depolarize quickly.
- Used as IV bolus or infusion.
- Used for control of pre-ventricular contractions (PVC)
- Lidocaine HCl
![]() Adverse Side Effects:
Adverse Side Effects:
- Cats much more sensitive to lidocaine than dogs
- Can cause a 3rd or complete A-V block.
- Toxic side effects in CNS
- Toxic dose 10 mg/kg
- Small overdose = sedation
- Larger overdose = seizures
- Procainamide and Quinidine
- Human drug
- Same family of drugs as lidocaine
- Can be given orally
- Used for atrial fibrillation (A-fib), PVCs, and ventricular tachycardia.
![]()
![]()
- β1 blockers = β1 antagonists
- Block β1 receptors so blocks the SNS.
- Drugs in this group end in “olol”.
 Slow depolarization of heart
Slow depolarization of heart- slows heart rate.
Examples:
- Propanolol (Human)
- Carvedilol & Atenolol (Human)
- Newer β1 blockers = more specific to heart
- Less bronchoconstriction
- Newer β1 blockers = more specific to heart
Adverse Side Effects:
- Up-regulation of β receptors on heart
- Increases number of β receptors so will need more drug over time as there are more receptors to block.
- If withdraw β blocker quickly the heart becomes very sensitive to epinephrine
- Due to more receptors on heart
- Must slowly decrease dose to zero.
 Also blocks some β2 bronchioles → bronchoconstriction.
Also blocks some β2 bronchioles → bronchoconstriction.- Less so with newer drugs
- Diltiazem
- Calcium channel blocker
- Human drug
- Used for cats with hypertrophic cardiomyopathy.
**Caution with all negative inotropes – Do not use in CHF animals
- Positive Inotropes
 Increase strength of contraction of heart by increasing availability of calcium.
Increase strength of contraction of heart by increasing availability of calcium.
Examples:
- Epinephrine
- Stimulates most α and β receptors.
- Used for cardiac standstill
- Very short half-life
- Dopamine
- Human drug
- More selective than epinephrine
- Stimulates myocardial contractions.
- Some CNS stimulation
Adverse Side Effects:
- Short half live
- Downregulation
 Heart decreases number of β receptors and is less responsive over time.
Heart decreases number of β receptors and is less responsive over time.
- Pimobendan
- Acts as both a vasodilator and a positive inotrope.
- Treats CHF due to dilated cardiomyopathy (DCM) in dogs
- Vetmedin®
- Anticholinergic
- Atropine
- Works against acetylcholine
- Parasympatholytic
- Used to treat bradycardia, reduce salivation and bronchial secretions before surgery or as an antidote for overdose of cholinergic.
- Vasodilators
- Counteract arterial vasoconstriction caused by the SNS.
- Responding to decreased blood pressure due to Congestive Heart Failure
- Reverse vasoconstriction
- Start off slowly or can cause hypotension
- Seen as lethargy, ataxia, syncope.
RAAS- Renin-angiotensin-aldosterone system
-Markers all over the body that can detect when blood pressure drops, kidneys release renin combines with angiotensin. Compensatory system that kicks in when blood pressure drops
Examples:
- Arterial Vasodilators
- Amlodipine
 Antihypertensive/Antianginal
Antihypertensive/Antianginal
- Classified as a calcium channel blocker.
- Relaxation of smooth muscle lining the arterioles
- Used to treat secondary hypertension in cats with hyperthyroid, chronic renal disease, or diabetes mellitus.
- Hydralazine
- Causes arteriolar smooth muscle to relax.
- Used to treat Congestive Heart Failure (CHF)
- Venous Vasodilators
- Nitroglycerin
- Human drug
- Used to treat pulmonary edema from CHF and improve cardiac output.
- Dilates coronary arterioles so improves blood flow to the myocardium.
- Significant first pass effect = not given PO
- Applied as a topical cream (use gloves!)
![]()
 Mixed Vasodilators
Mixed Vasodilators- Used to treat Congestive Heart Failure
- Drugs often end in “pril
- Enalapril
- Benzaprol (Fortekor®)
Adverse Side Effects:
- ↓ K excretion in the kidneys so can see hyperkalemia
 Diuretics
Diuretics
- Remove excess fluid by increasing water loss in urine.
- Used to treat pulmonary edema from CHF or cerebral edema.
- All diuretics have their action by either:
- Preventing reabsorption of either Na or K from renal tubules.
- Increasing secretion of either Na or K from renal tubules.
- The Na or K takes water with it by osmosis to be secreted in the urine.
![]()
![]() Examples:
Examples:
- Furosemide
- Loop diuretic (Loop of Henle)
- Prevents reabsorption of Na from urine which osmotically retains water in the urine.
- Salix®
- Lasix®
 Since Na is so important to the body, the DCT then reabsorbs the sodium in exchange for potassium.
Since Na is so important to the body, the DCT then reabsorbs the sodium in exchange for potassium.- Hyponatremia- low sodium
Adverse Side Effects:
- Cause K+ loss which effects heart function
- Ototoxicity
 Trichlormethiazide
Trichlormethiazide- Inhibit reabsorption of Na and Cl
- Naquasone®
- Inhibit reabsorption of Na and Cl
- Naquasone® also has dexamethasone for inflammation.
- Injection for cattle and horses
Adverse Side Effects:
 Na will be reabsorbed in exchange for K so can also get hypokalemia.
Na will be reabsorbed in exchange for K so can also get hypokalemia.
- Mannitol
- Carbohydrate (sugar)
- Osmotic diuretic
- Used for cerebral edema
- Alleviates pressure in the eyes
Miscellaneous Cardiovascular Drugs:
- Acetylsalicylic Acid = Aspirin®
- Interferes with platelet clumping.
- Spontaneous formation of platelet plugs (thrombi) occurs in cardiomyopathies.
- Aspirin will prevent formation of thrombi which prevents emboli breaking off and going to the brain (stroke) or to the heart muscle (myocardial infarcts).
![]()
![]()
![]() Urinary Incontinence:
Urinary Incontinence:
- Sympathomimetic Agents =
aadrenergic- Phenylpropanolamine
- Propalin®
- Stimulates the urethral sphincter muscle.
- Used in spayed female dogs.
- Do not use with CV drugs such as β blockers or Atropine.
Adverse Side Effects:
- Behavioral – aggression, restless
- Cardiovascular – tachycardia
- Vomiting/diarrhea
- Seizures
Review Questions
- What are the neurotransmitters for the ANS?
- What effect does epinephrine and acetylcholine have on the α1, α2, β1 and β2 receptors in the cardiovascular system?
- What effect would a sympathomimetic drug have on the heart? bronchi?
- What effect would a parasympatholytic drug have on the heart? bronchi?
- What effect does a negative inotrope have on the heart? A positive inotrope?
- Which type of lidocaine is used for heart arrhythmias? Why?
- Review Questions
- What does upregulation or downregulation of receptors mean?
- How does vasodilation help an animal with CHF?
- Why should you use gloves when applying nitroglycerin ointment?
- What effect does a diuretic have? How does Furosemide work? What are the possible side effects?
- What type of drug is used to treat urinary incontinence? How does it work and what are the side effects?