Interaction of pathogens (with a host)
Interaction of pathogens (with a host)
Intended learning outcomes
- Describe how pathogens cause disease and how they overcome the innate host defence
- Demonstrate an understanding of basic concepts of epidemiology: how infections are propagated.
Commensal bacteria:
- Commensal bacteria act on the host's immune system to induce protective responses that prevent colonization and invasion by pathogens.
- Aid immune development
- Colonisation resistance
- Metabolic organ
- But can cause opportunistic infection in immunocompromised host - known as opportunistic pathogens
What is a immunocompromised host?
- Damage to epithelial such as skin infections (bacteria can't get through skin if its is intact)
- Disruption of commensal bacteria
- Impairment of the immune system caused by infection, chemotherapy or age
- Introduction of bacteria into new sites such as device associated infection
Obligate human pathogens:
- Disseminate solely through causing disease in humans
- Not part of the commensal flora, they have a poor survival rate outside the host
How do bacteria spread:
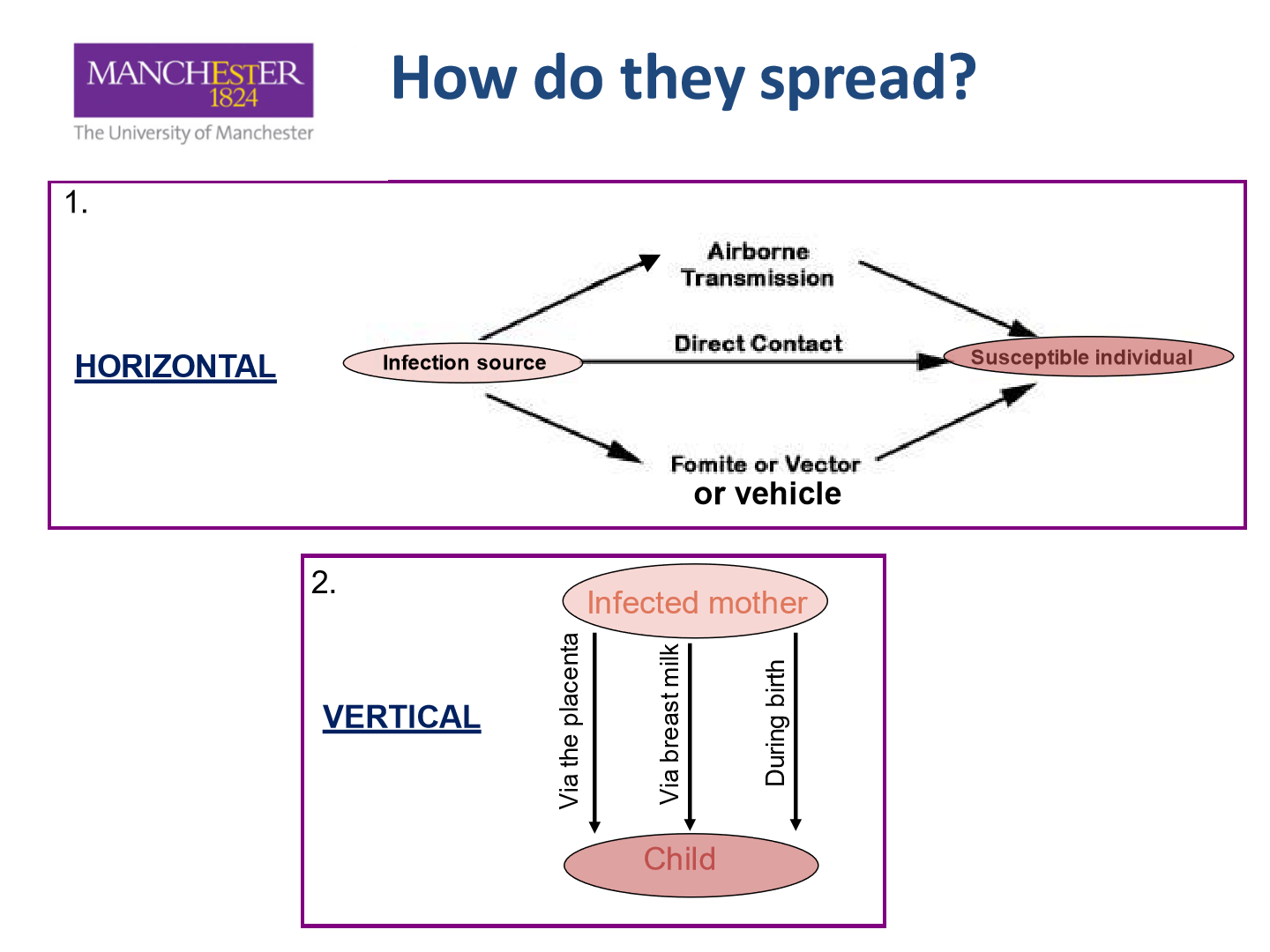
- Formite - inanimate object (e.g phone)
- Vector - blood feeding ( e.g mosquitos)
- Vehicle - food or water
How do bacteria cause infections:
- Bacteria have virulence factors which can cause infection
- Virulence factors are bacterial products or strategy that contributes to virulence or pathogenicity.
- Main categories of virulence factors:
- Promote colonisation and invasion
- Damage host
Colonisation and invasion:
- Fimbria/pilli
- Proteinaceous, non-flagella surface appendages
- Anchored to outer membrane enable the bacteria to adhere to host
- Different pilli have different targets
- Flagella
- Thin hollow, appendages which allow the bacteria to move via rotation
- Capsules
- A polysaccharide layer which surround the cell , provides attachment and prevents being stuck in mucus
- Capsule also helps the bacteria avoid immune invasion to cause a systemic infection.
- Bacteria avoid immune response by mimicking the host cell and preventing phagocytosis
- N.meningitidis
- Capsule has such a massive negatively charge that anything else that has a negative charge will be pushed away (phagocyte will be pushed away due to repulsion due to negative charge allowing to avoid phagocytosis)
- Prevents immunogenic response as it mimic host, so doesn't trigger immune response
- uncontrolled growth in the blood leads to meningococcal septicaemia
Endotoxins:
- Part of gram negative bacteria
- Part of lipopolysaccharide layer of the cell wall
- When bacteria die it cause endotoxins to be released which will enter surrounding area which trigger cytokine release
Exotoxins:
- Bacterial metabolites are actively excreted from the focus of the infection to specific parts of the body
Pneumolysin and CAP
- Pneumolysin is an pore forming exotoxin which is produced by S.pneumoniae, it is critical in the development of community acquired pneumonia
- pneumolysin causes cell apoptosis to macrophages
- For an immune response the body produces a proinflammatory reaction which is:
- Characterised by influx of neutrophils
- Complement activation of reactive oxygen species
- Virulence factors can allow the bacteria to avoid this reaction which can cause inflammatory mediated damage
- Very young and the elderly are more susceptible to CAP
Signs and symptoms of CAP:
- Fever
- Shortness of breath
- Productive cough
- Focal chest signs