White Blood Cells, Red Blood Cells, Plasma
Functions of Blood
Three main functions:
Transport: Blood delivers nutrients, gases, hormones, etc.
Regulation: Helps maintain temperature, pH, and fluid volume.
Protection: Prevents blood loss through clotting and infection via immune components.
Composition of Blood
Blood as Fluid Tissue:
The only fluid tissue in the body, classified as connective tissue.
Components:
Plasma: nonliving fluid matrix (~55% of blood).
Formed Elements: living blood cells suspended in plasma, which includes:
Erythrocytes (RBCs)
Leukocytes (WBCs)
Platelets
Blood Composition:
Erythrocytes on bottom (~45% of whole blood):
Hematocrit: percentage of blood volume that is RBCs.
Normal hematocrit values:
Males: 47% ± 5%
Females: 42% ± 5%
WBCs and platelets in Buffy coat (<1%): thin layer between RBCs and plasma.
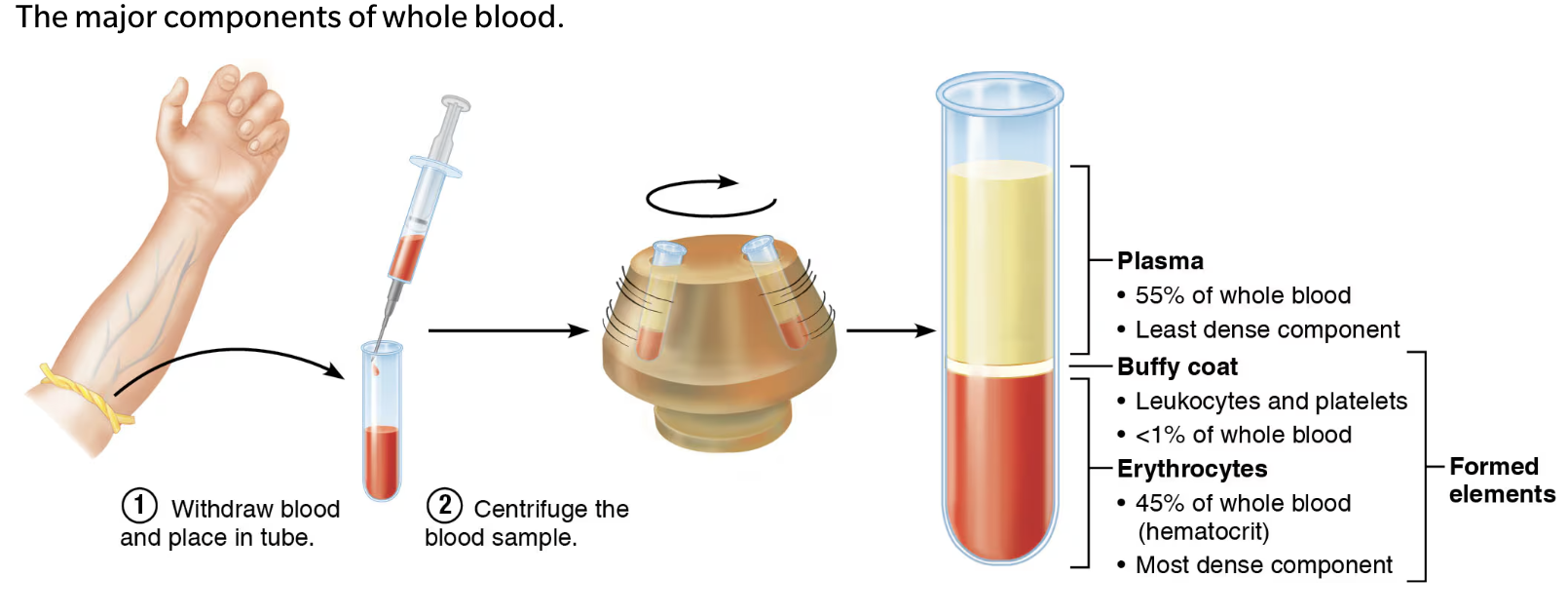
Physical Characteristics of Blood
Physical Characteristics:
Sticky, opaque fluid with metallic taste.
Color varies with oxygen content:
High O2 levels: scarlet red
Low O2 levels: dark red
pH: 7.35–7.45.
Blood makes up ~8% of body weight.
Average volume:
Males: 5–6 L
Females: 4–5 L
Blood Plasma
Plasma Characteristics:
Straw-colored, sticky fluid (~90% water).
Contains over 100 dissolved solutes: nutrients, hormones, waste, proteins, inorganic ions.
Most abundant solutes are plasma proteins:
Albumin: makes up 60% of plasma proteins; functions as a carrier, blood buffer, and contributor to osmotic pressure.
Globulins: constitute 36% of plasma proteins; they are involved in immune responses, functioning as antibodies and transport proteins for various substances.
Alpha: produced by liver and transport proteins for lipids and fat-soluble vitamins, playing a crucial role in lipid metabolism.
Beta: produced primarily in the liver, these globulins play a significant role in transporting iron and maintaining proper osmotic balance within the bloodstream.
Gamma (antibodies): produced by plasma cells, these globulins act as antibodies in the immune response, helping to protect the body against infections and foreign pathogens.
Fibrinogen: 4% of plasma proteins, synthesized by the liver, is essential for blood clotting as it is converted into fibrin during the coagulation process, forming a stable mesh that helps in sealing wounds and preventing excessive bleeding.
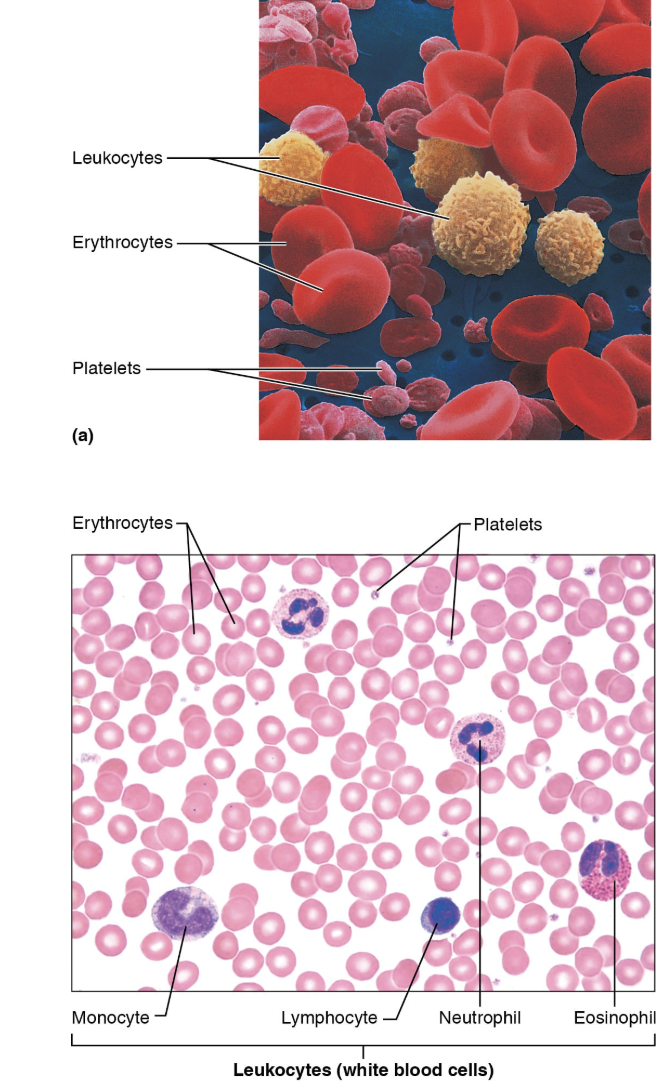
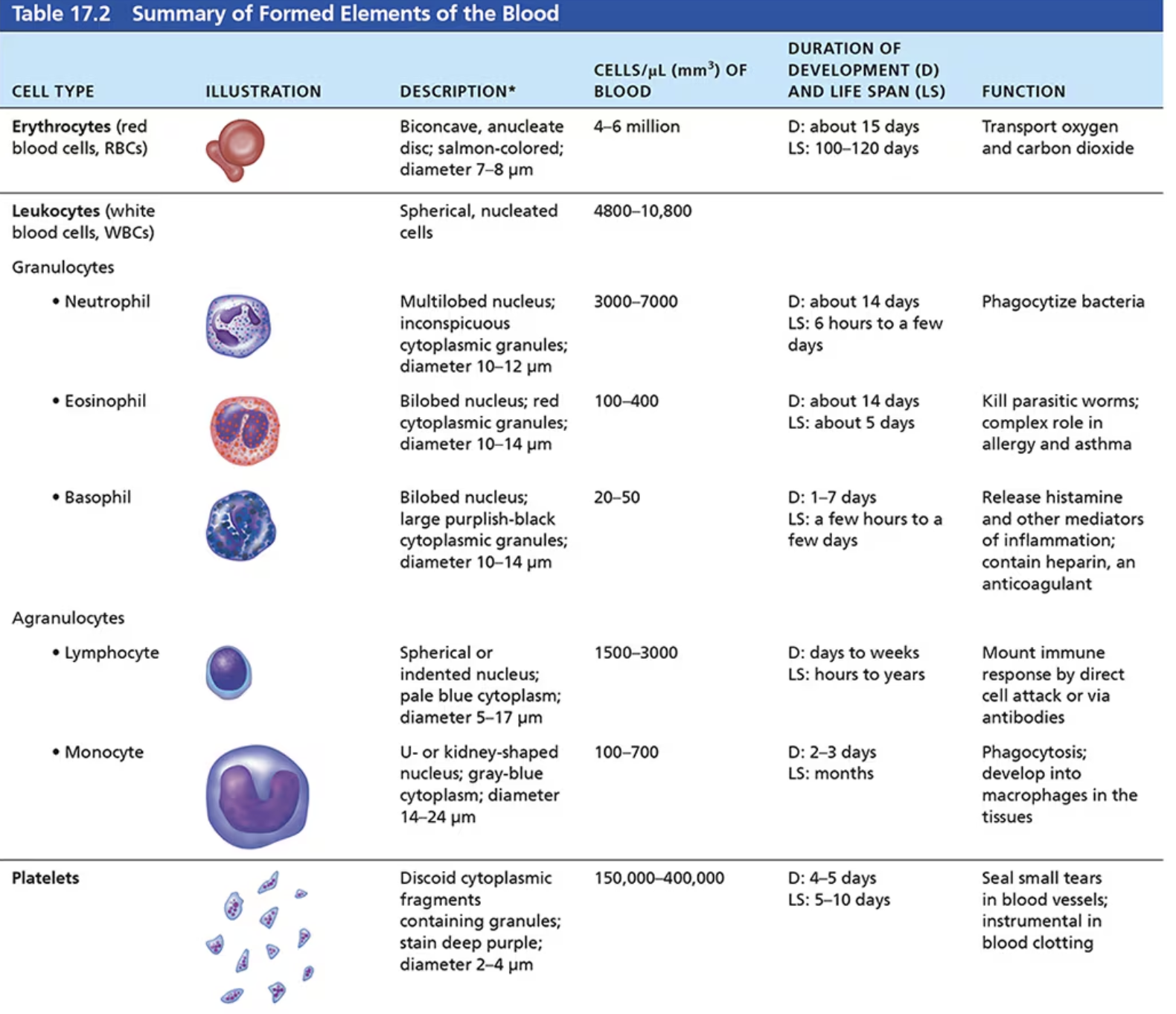
Formed Elements
Elements: erythrocytes (RBCs), leukocytes (WBCs), and platelets.
Only WBCs are complete cells with nuclei and organelles.
RBCs lack nuclei and organelles, survive in bloodstream only a few days, originate in bone marrow.
Erythrocytes (Red Blood Cells)
Structure:
Small diameters (7.5 μm), biconcave disc shape, anucleate, filled with hemoglobin (Hb).
Contain proteins such as spectrin for flexibility.
Function:
Dedicated to respiratory gas transport; Hb binds with O2.
Normal values for Hb:
Males: 13–18 g/100 ml
Females: 12–16 g/100 ml.
Hemoglobin Structure:
Comprised of heme pigments and globin protein (four polypeptide chains).
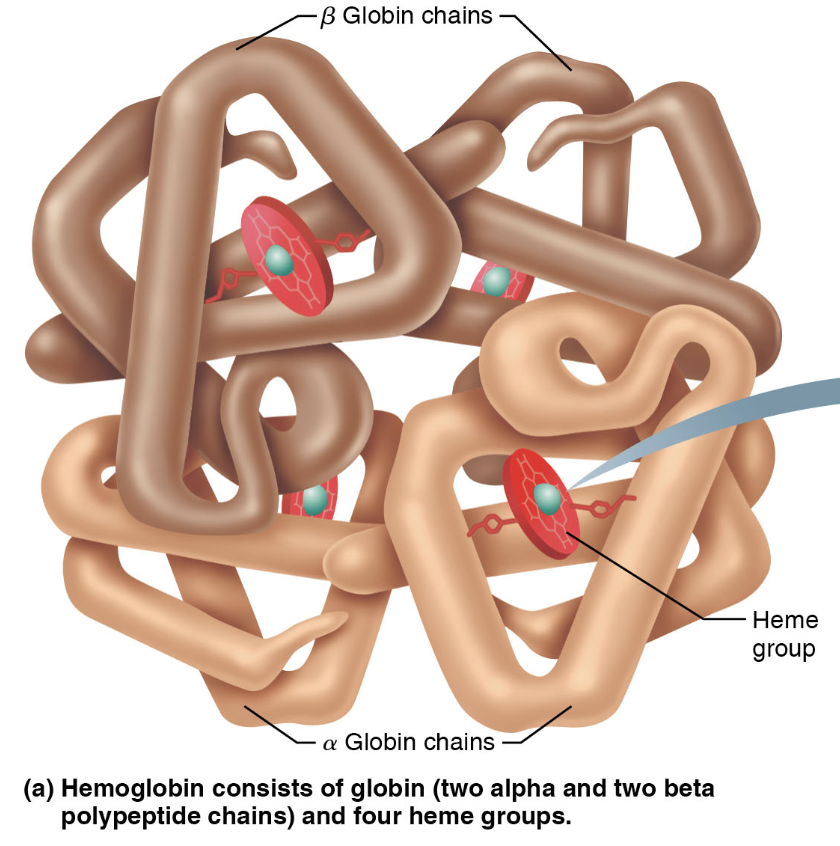
Gas Transport:
Each Hb molecule can transport four O2.
Also facilitates CO2 transport as carbaminohemoglobin.
Production of Erythrocytes
Hematopoiesis: Formation of all blood cells primarily in red bone marrow.
Stages of Erythropoiesis:
Process takes about 15 days, begins with hematopoietic stem cells.
Transformation stages from hemocytoblast to reticulocyte, indicating rate of RBC formation.
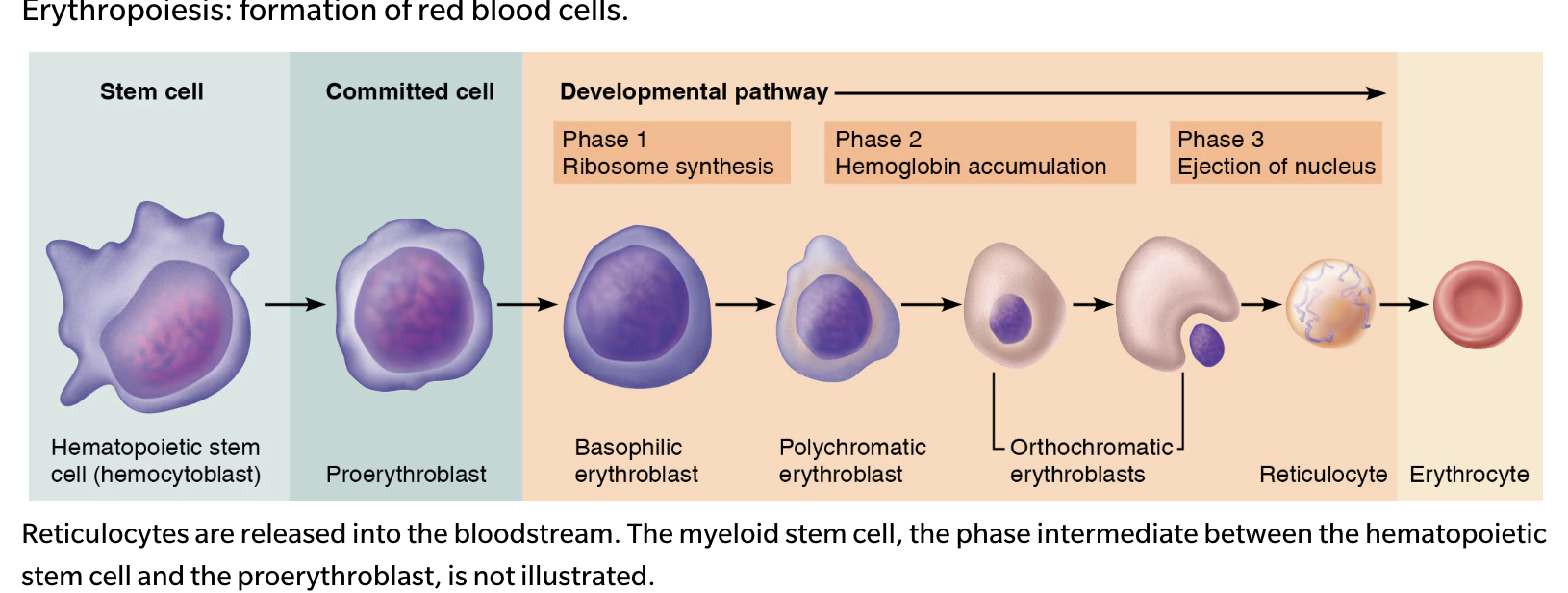
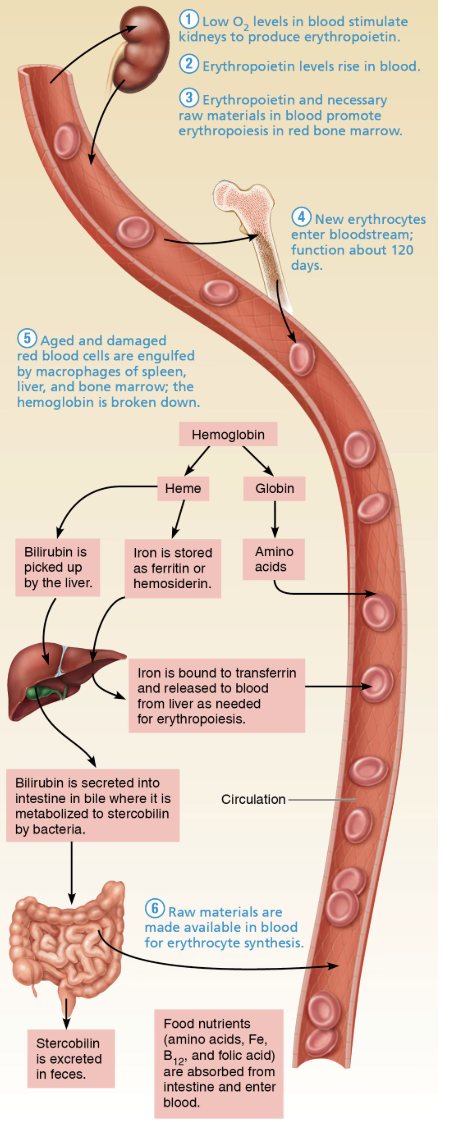
Regulation and Requirements of Erythropoiesis
Red Blood Cell Lifespan: 100–120 days.
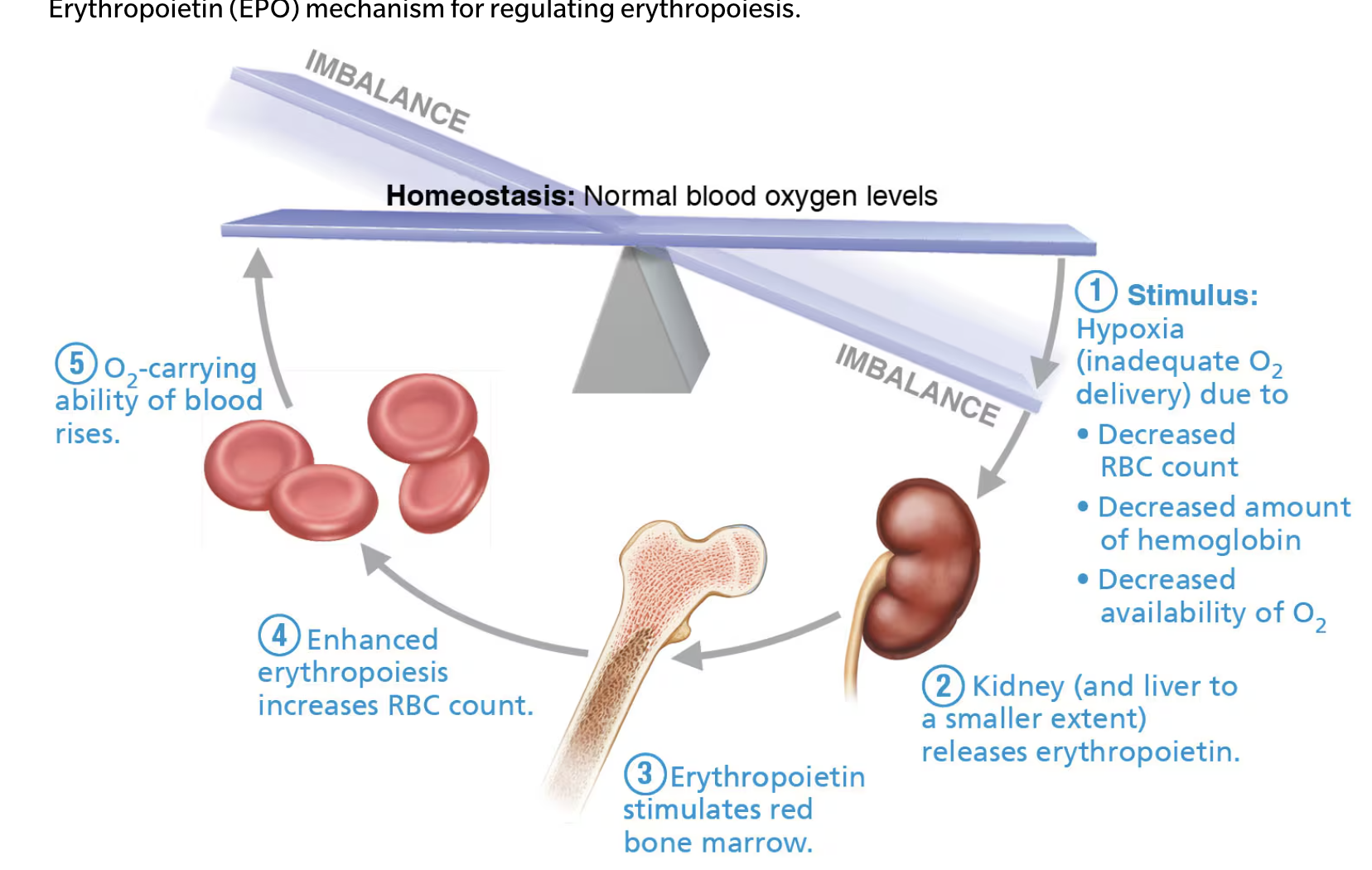
Hormonal Control: Erythropoietin (EPO) stimulates RBC production.
Released in response to hypoxia (low oxygen levels).
Dietary Requirements:
Amino acids, lipids, carbohydrates.
Iron and vitamins B12 and folic acid critical for RBC production.
Fate and Destruction of Erythrocytes
Breakdown: Old RBCs get trapped in the spleen, where macrophages engulf and break them down.
Products of Breakdown:
Iron is stored or reused, heme is converted to bilirubin and eventually excreted.
Globin is broken down into amino acids.
Erythrocyte Disorders
Anemia: Low O2-carrying capacity; caused by blood loss, insufficient RBC production, or excessive destruction.
Types of Anemia:
Hemorrhagic Anemia: Rapid loss due to severe wounds.
Iron-Deficiency Anemia: Caused by insufficient iron; results in microcytes.
Pernicious Anemia: Autoimmune condition affecting B12 absorption.
Thalassemias: Genetic disease affecting hemoglobin.
Sickle-Cell Anemia: Genetic mutation causing RBC deformation.
Polycythemia: Excess RBC; can result from primary bone marrow disease or secondary to hypoxia.
Leukocytes (White Blood Cells)
General Structure:
Complete cells with nuclei, <1% of blood volume (4,800–10,800 WBCs per µl blood).
Functions: Defense against disease; can exit capillaries (diapedesis) and move via amoeboid motion.
WBC Types: Granulocytes (neutrophils, eosinophils, basophils) and agranulocytes (lymphocytes (T cells and B cells), monocytes).
Mnemonic for abundance: "Never let monkeys eat bananas."
Production and Life Span of Leukocytes
Leukopoiesis: Production of WBCs stimulated by chemical signals.
All originate from hemocytoblasts, with pathways diverging to lymphocytes and myeloid cells.
Granulocyte and Agranulocyte Production: Involves multiple immature forms culminating in mature leukocytes.
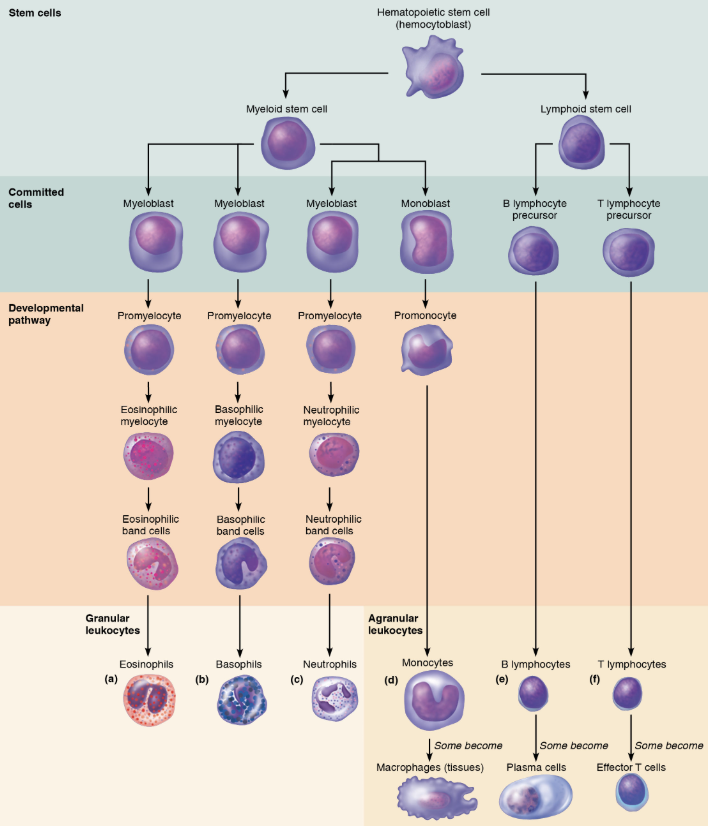
Leukocyte Disorders
Leukemias: Result from abnormal WBC proliferation.
Named by the type of WBC involved; treatment includes irradiation and antileukemic drugs.
Infectious Mononucleosis: Caused by Epstein-Barr virus; characterized by increased atypical agranulocytes.