APHY 102- ch 22-23
.
Meiosis
22.1 Meiosis
Gonads: Produce hormones and gametes (sex cells).
Male: Testes (male gonads) produce sperm.
A sperm cell has 23 chromosomes
Female: Ovaries (female gonads) produce ova (eggs/oocytes).
An egg cells have 23 chromosomes
Genetic Composition:
Gametes have one set of 23 chromosomes (haploid).
Body cells have two sets (diploid).
Normal body cells have 23 types of chromosomes, of those there are 2 copies, making 46 chromosomes total, 1 paternal copy, 1 maternal copy- diploid
Fertilization: Unites sperm and egg, restoring 46 chromosomes.
Meiosis: Produces gametes through two successive divisions.
Homologous Chromosome: the same type of chromosome but have a paternal and maternal one, same genes but different genetic code
Sister Chromatids: copy one of the chromosomes, and have two of them together, exact same pair/copy of chromosomes in a set of two
Meiosis Stages
Before Meiosis:
Sperm (23) + Egg (23) = 46 chromosomes
DNA replication = 46 chromosomes
why? - counting centromeres not chromatids
each chromosome replicates and contains 2 DNA strands, called chromatids, connected by the centromere

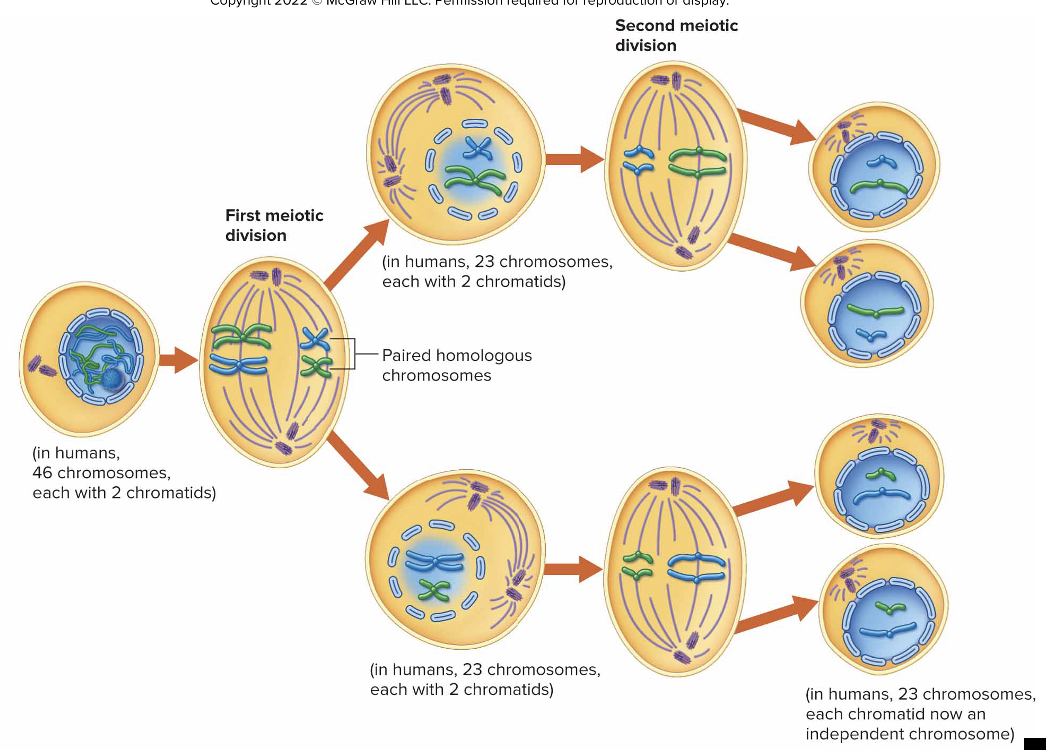
Meiosis I
separates homologous pairs of chromosomes
results in haploid cells - contain 1 set of chromosomes: 23 chromosomes total, one from each homologous pair
Four Phases in Meiosis 1- PMAT
Result: 2 haploid daughter cells, each one containing 23 chromosomes w/ 2 chromatids
Meiosis II
cells are still haploid, but chromosomes now have 1 chromatid
Four Phases in Meiosis 2- PMAT
Result: 2 daughter cells, each one w/with 23 chromosomes and 1 chromatid
END RESULT OF MEIOSIS 1 AND 2 IS HAPLOID
WHEN EGG AND SPERM ARE INTRODUCED THEY BECOME DIPLOID CELLS AND CHROMOSOMES ARE NOW PAIRED
Male Reproductive System
Gonads: Testes produce testosterone and spermatozoa.
Accessory Organs: Transport sperm, including seminal vesicles, prostate gland, and bulbourethral glands.
Epididymis: store/mature sperm
Ductus Defrens: tube to epididymis to Ejactulatory duct
Seminal Vesicle: produce alkaline fluid, fructose, prostaglandin
Prostate: release alkaline and prostaglandin
Bulbourethral gland: neutralizes urethra and secretes alkaline substance, provides lubrication.
Semen: combo of sperm, seminal vesicles, prostate gland, and bulbourethal glands. alkaline. avg. 120 million sperm cells/mL of semen.
Dartos Muscle: contracts/relaxes scrotum/testis in response to temp.
Penis: shaft contains 3 erectile tissues: 2 corpora cavernosa and 1 corpus spongiosum
Erection: parasympathetic event, nerve impulses release nitric oxide which dilates arteries in penis, penis swells and elogates
Orgasm: physiological and psychological release, dependent on sympathetic nerve impulses
Emission: movement of semen into the urethra
Ejaculation: movement of semen out of the urethra
Testes
In fetal development, testes descend into the scrotum due to testosterone influence.
Gubernaculum: Aids in descent through inguinal canal.
The tunica albuginea encloses each testis
Seminiferous tubules: sperm is developed here
Interstitial cells (Leydig cells): Produce testosterone.
Seminal Vesicles: Secrete alkaline fluid rich in fructose.
Prostate Gland: Produces thin, milky fluid that enhances sperm motility.
Sperm Cell
Head: contains nucleus, acrosome (enzymes that penetrate layers around oocyte)
Midpiece: contains mitochondria
Tail: contains microtubules
Hormones:
Hypothalamic Hormone
GnRH: regulates secretion of gonadotropins of anterior pituitary gland
Anterior Pituitary Hormones:
Interstitial Cell Stimulating Hormone (LH): development of interstitial cells in testes, secretes male sex hormones
Follicle stimulating hormone: stimulates cells of testes to mature, proliferate, and respond to testosterone
Androgens- male sex hormones- testosterone - produce some as baby then stop until puberty
Secondary sex characteristics:
increased growth of body hair, decreased growth of scalp hair
enlargement of larynx
thickening of skin
increased muscular growth
thickening/strengthening of bones
Female Reproductive System
Female Reproductive System
Primary Gonads: Ovaries produce oocytes and hormones (estrogen and progesterone).
Accessory Organs: Include uterine tubes, uterus, and vagina, facilitating fertilization and gestation activities.
Ovaries
Ovarian Medulla: inner layer
Ovarian Cortex: outer layer: granular appearance, tiny masses of cells called ovarian follicles (oocytes develop inside these follicles).
Fallopian/Uterine Tubes: connect ovaries to the uterus
Layers: inner mucosa, middle muscularis, outer peritoneum
Vagina: passage way for penis, menstuation, and childbirth.
Mammary Glands: feed offspring, develop in puberty due to estrogen being released, accessory organ.
External Accessory Organs: - all together are called Vulva
Labia Majora: skin like layers, outer layer
Labia Minora: skin like layer, inner layer
Clitoris: 2 erectile columns, sensory structures that aid in sexual stimulation
Vestibule: everything inside labia minora, encloses vaginal and urethal opening
vestibular glands: secrete mucus during sexual stimulation
Erection: in clitoris and around vaginal entrance
Lubrication: vestibular glands
Orgasm: clitoris responds to sexual stimulation, a physiological and psychological release
Uterus:
Body: upper 2/3rds
Cervix: lower 1/3rd
Layers: Endometrium, Myometrium, Perimetrium
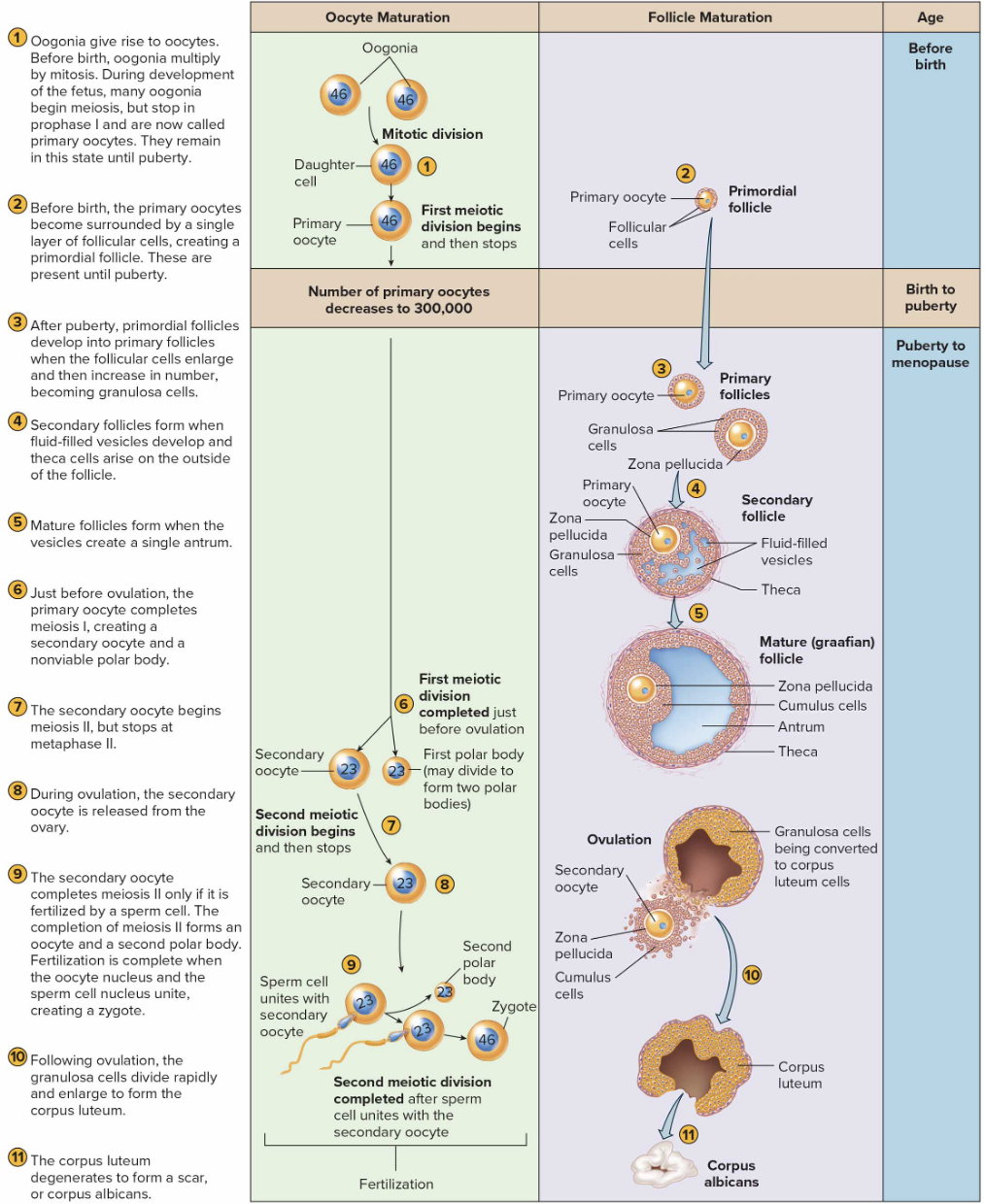
Primary Follicles:
primordial germ cells give rise to oogonia
Oogonia develop into primary oocytes
flat epithelial cells called follicular cells form primordial follicles
primary oocytes begin (in fetal development) but don’t finish meiosis until puberty
Primordial follicles are never produced again
Oogenesis
primary oocytes- haploid
unequal division, primary oocyte and secondary oocyte- outcome is secondary oocyte and polar body
polar body function- to contain DNA
secondary oocyte gets to keep all cytoplasm and organelles
Hormones
Gonadotropin-Releasing Hormone (GnRH): Triggers FSH and LH from the anterior pituitary, regulating ovarian function.
Estrogens and Progesterone: Control reproductive cycle, secondary sex characteristics, and pregnancy preparation.
breast and mammary gland duct development
increased adipose tissue in breasts, thighs, butt
increased vascularization of skin
Menstrual Cycle Phases
Follicular Phase: Dominant follicle matures.
Ovulation: Triggered by LH surge.
Luteal Phase: Corpus luteum forms and degenerates if no fertilization occurs.
corpus albicans: oocyte degenerates, scar tissue
corpus luteum: prepares uterus for implantation - follicular cells left after ovulation
FSH, LH, and Estrogen peak BEFORE ovulation
Progesterone peaks AFTER ovulation
Birth Control:
Coitus Intrruptus: withdrawing penis before ejactulation- not very effective
Rhythm Method: paying attention to cycle- not very effective
Mechanical Barriers: condoms, can work well if used properly
Chemical Barriers: creams, foams, etc,- most effective
Hormonal contraceptive: estrogen or progesterone based
IUD: causes inflammation by releasing copper
Emergency Contraceptive: stops ovulation
Sterilization: vasectomy and/or tubal ligation
Chlamydia, Gonorrhea: bacterial infection, can result in infertility, pelvic disease.
Chapter 23- Growth and Development
Growth: increase in size, or number of cells
Development: growth and aging, continuous process
prenatal: fertilzation-birth
postnatal: birth-death
Fertilization occurs in the fallopian tubes
corona radiata: sperm invades here first, layer of follicular cells that surround oocyte
zona pellucida: next sperm digest this glycoprotein layer that closely surrounds the oocyte
only 1 sperm shall win the heart of the oocyte and penetrate its membrane
Once sperm enters, secondary oocyte completes meiosis 2, producing tiny polar body and a large cell that contains nucleus w/female’s chromosomes
pronuclei: nuclei of sex cells until united
pronuclei now unite, completing fertilization> fertilized egg is now a zygote= 46 chromosomes
Pregnancy:
developing offspring in uterus, lasts about 38wks
three stages: pre-embryonic, embryonic, and fetal
Pre-Embryonic Stage: fertilzation-2/3wks
Cleavage: rapid cell division
blastomeres are the cells produced
Morula: when 16 cells have been developed, moved into uterus
Blastocyst: hollow ball of cells, attached to endometrium of uterus
inner mass cells: gives rise to embryo
trophoblast: produces hCG- maintains corpus luteum and prevents immune system from attacking, develops into structures that assist embryo
Chorion: will develop into embryonic portion of placenta
Amnion: membrane that develops around embryo, provides suitable environment for embryo to develop in
Yolk Sac: provides nutrients to embryo while placenta is forming
Embryonic Stage: 3rd wks-8th wk
Gastrulation: movement of cells within the embryonic disc to form multiple layers
primary germ layers:
Ectoderm: nervous system
Mesoderm: muscle, bone, blood, and reproductive system
Endoderm: resp. tract and digestive system
Gastrula: an embryo that has gone through gastrulation and contains all 3 germ layers
Fetal Stage: 8wks-birth
rapid growth stage
Fetal Hemoglobin is more efficient at carrying oxygen than adult hemoglobin