Lecture 1 – Reproductive Tract of Males
Testicular Development and Descent
the testes originate from the gonadal ridges, located in the upper lumbar region of the embryo
the gubernaculum is a key structure in descent
cord of tissue that attaches the testis to the posterior abdominal wall
doesn’t elongate as the fetus grows; relative shortening is thought to pull the testes downwards
the testes migrate from the abdomen
through the inguinal canal → into the scrotum
this process is primarily driven by androgens (male sex hormones)
cryptorchidism is the medical term for failure of one or both testes to descend into the scrotum
most common congenital defect in male newborns
consequence: endocrine function remains intact, but spermatogenesis is arrested
this is because the temperature in the abdomen is too high
scrotal temperature is important because:
the scrotum maintains a temperature 4–7°C lower than core body temperature
scrotal skin: high density of sweat glands for evaporative cooling
counter-current heat exchange: the spermatic artery is coiled around the pampiniform plexus
allows heat to be transferred from the artery to the vein, cooling the arterial blood before it reaches the testis
cremaster muscle: this muscle contracts in cold conditions to pull the testes closer to the body for warmth, and relaxes in warmth to allow them to hang lower and cool
Structure of the Testis
the testis is encased in a tough, fibrous capsule called the tunica albuginea
in the seminiferous tubules, each lobule contains 1–4 highly coiled seminiferous tubules which is the site of sperm production
there’s ~800 seminiferous tubules per testis
each tubule is ~80cm long, a single testis contains ~640m of tubules
large SA is needed for the continuous production of millions of sperm daily
The Spermatogenic Wave
spermatogenesis takes a fixed amount of time, with a new cycle starting every 16 days
mechanism: to maintain a continuous supply of sperm, the process isn’t synchronised across the entire testis. instead, different segments along the length of a single seminiferous tubule are at different stages of development. this is called the spermatogenic wave, ensuring that mature sperm are constantly being produced and released
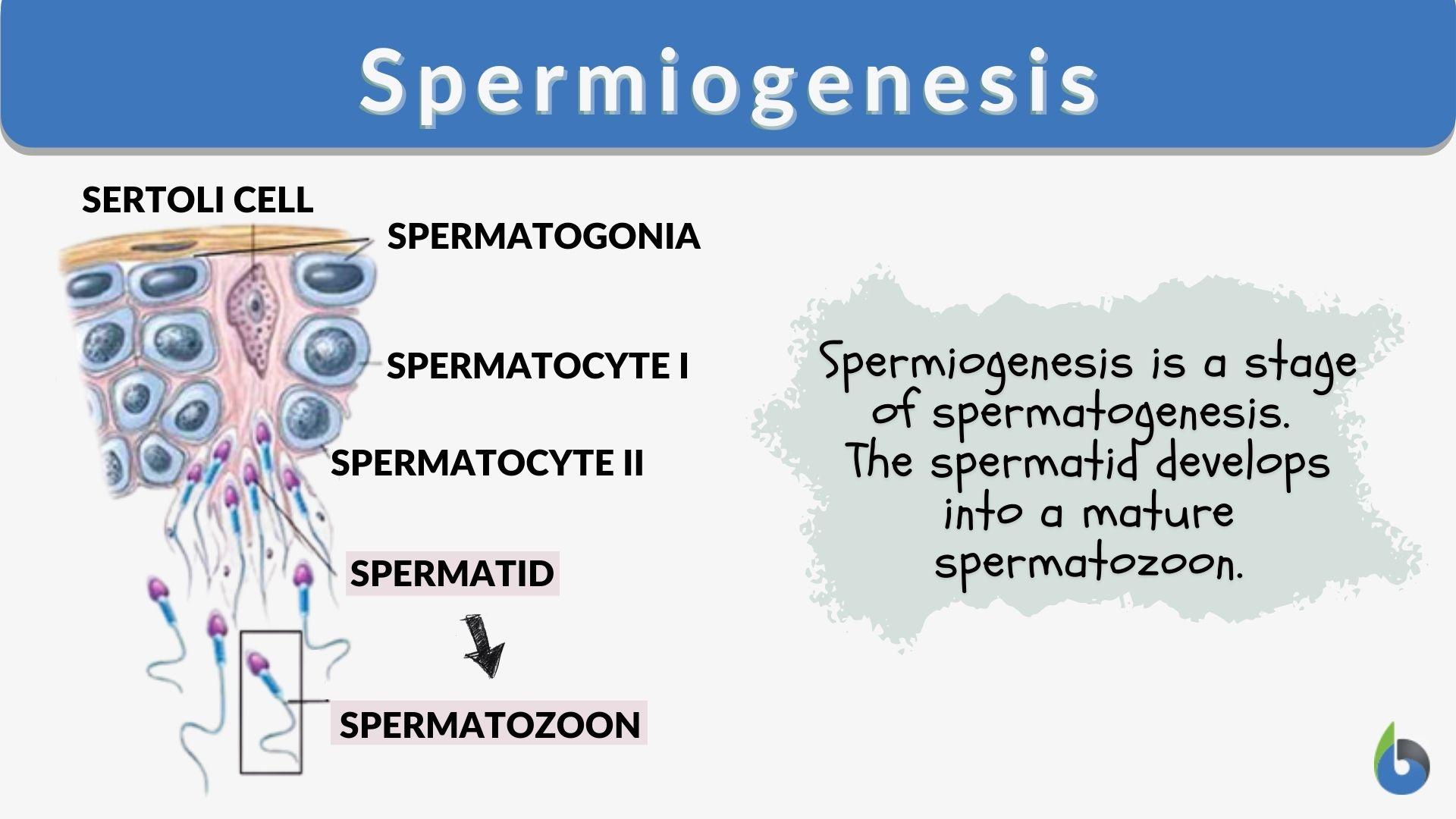
The Epididymis: Site of Maturation
the primary function is sperm maturation, not long-term storage. sperm spends ~12 days transversing the epididymis
a comma-shaped organ with three regions that lies along the posterior border of the testis:
head (caput)
receives sperm from the rete testis
it’s lined with stereocilia that absorbs fluid from the testis which concentrates the sperm 100-fold
sperm in this region are immotile and incapable of fertilisation
body (corpus)
the tubule becomes less convoluted, and the fluid content continues to decrease
tail (cauda)
the final region
muscular wall thickens to three layers:
inner longitudinal
middle circular
outer longitudinal
stereocilia are reduced
sperm in cauda have acquired the ability to move and fertilise, but they’re kept in a quiescent state until ejaculation
movement through the epididymis is driven by a combination of fluid flow and peristaltic contractions

The Vas Deferens: Site of Storage & Transport
this is the major site of sperm storage in men
structure
a muscular tube about 45 cm long
it has three distinct muscular layers:
inner longitudinal
middle circular
outer longitudinal
allows powerful peristalic contractions during ejaculation
the lumen is simple near the epididymis but becomes folded and enlarged near the prostate to form the ampulla, which provides additional storage capacity
congenital absence of the vas deferens
a condition affecting ~1 to 1000 men, accounting for 1–2% of male infertility
most commonly found in men with CF due to genetic mutations, though it can occur in men w/o CF
usually bilateral (both vas deferens are missing)
sperm that isn’t ejaculated are eventually broken down and reabsorbed or are lost in the urine