L1 Role of the kidneys in homeostasis and clinical cases
Pre-note
Post lecture note
Learning Outcomes
Understand the role of kidneys in homeostasis
Control of blood volume by kidneys
Maintenance of body pH by kidneys
Patient Case Overview
Patient: Mr. MD, 72 years old, retired chef
Medical History: Hypertension, atrial fibrillation, osteoarthritis, depression
Symptoms: Fever, nausea, weight loss, vomiting, itching, shortness of breath
Diagnosis possibilities: Kidney-related conditions
Functions of the Urinary System
Excretion: Removal of organic waste products
Elimination: Discharge of waste into the environment
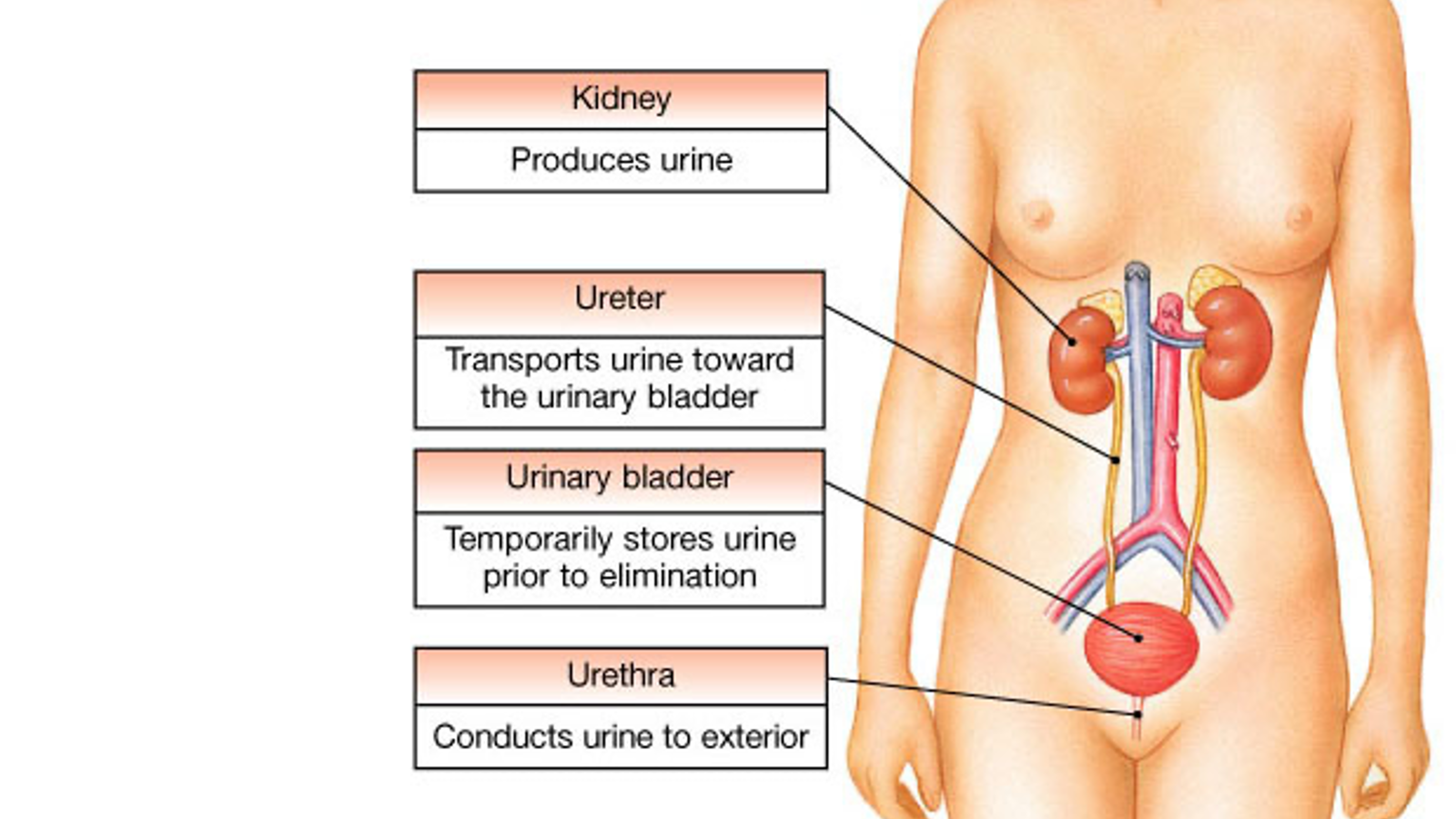
Essential Renal Functions
Kidney produces urine
Ureter transports urine towards urinary bladder
Urinary bladder temporarily stores urine prior to elimination
Urethra conducts urine to exterior
Excretion of endogenous waste products and drugs with their metabolites
Homeostasis of water, electrolytes, and acid-base balance
Regulation of hormone production (e.g., erythropoietin, renin)
Renal Function & Dysfunction
Renal failure can be acute (AKI) or chronic (CKD)
90% of renal failure is CKD, 10% is AKI
Severe renal failure can be fatal if untreated
Treatment: Dialysis or kidney transplantation
How Renal Dysfunction (Failure) shows in Relation to Each Essential Function
Renal Dysfunction or Failure is when the opposite of each essential function occurs
Excretion of endogenous waste products and drugs with their metabolites
Consequence: uraemia, azotaemia
Reason: Reduced renal excretory function
Excretion of drugs and their metabolites
Consequence: drug toxicity
Reason: reduced renal excretory function
Homeostasis of water, electrolytes, and acid-base balance
Consequence: metabolic
Reason: inability to maintain salt water and acid-base balance
Regulation of hormone production e.g. erythropoietin, renin
Consequence: anaemia, hypertension
Reason: compromised hormone function
Kidney's Role in Volume Homeostasis
Fluid Balance
the amount of water gained by the body each day equals the amount lost
Electrolyte Balance
the ion gain each day equals ion loss
Kidney's Role in Acid-Base Control
Acid-Base Balance
H+ gain is offset by H+ loss
Urine Formation Process
Glomerulus: Blood filtration
Proximal Tubule: Reabsorption/secretion
Loop of Henle: Urine concentration
Distal Tubule: Urine modification
Collecting Duct: Final urine modification
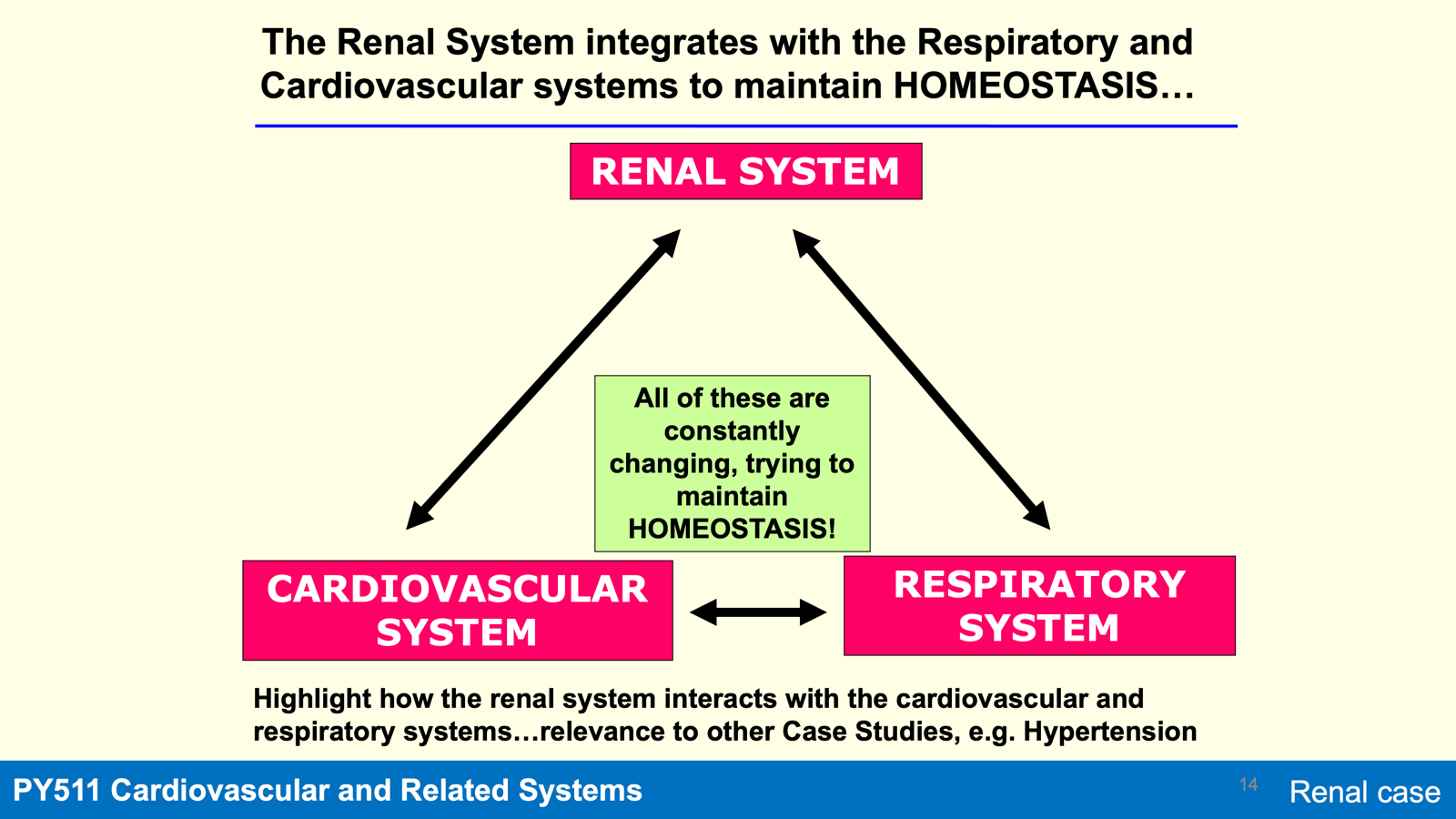
Renal, Cardiovascular and Respiratory Link
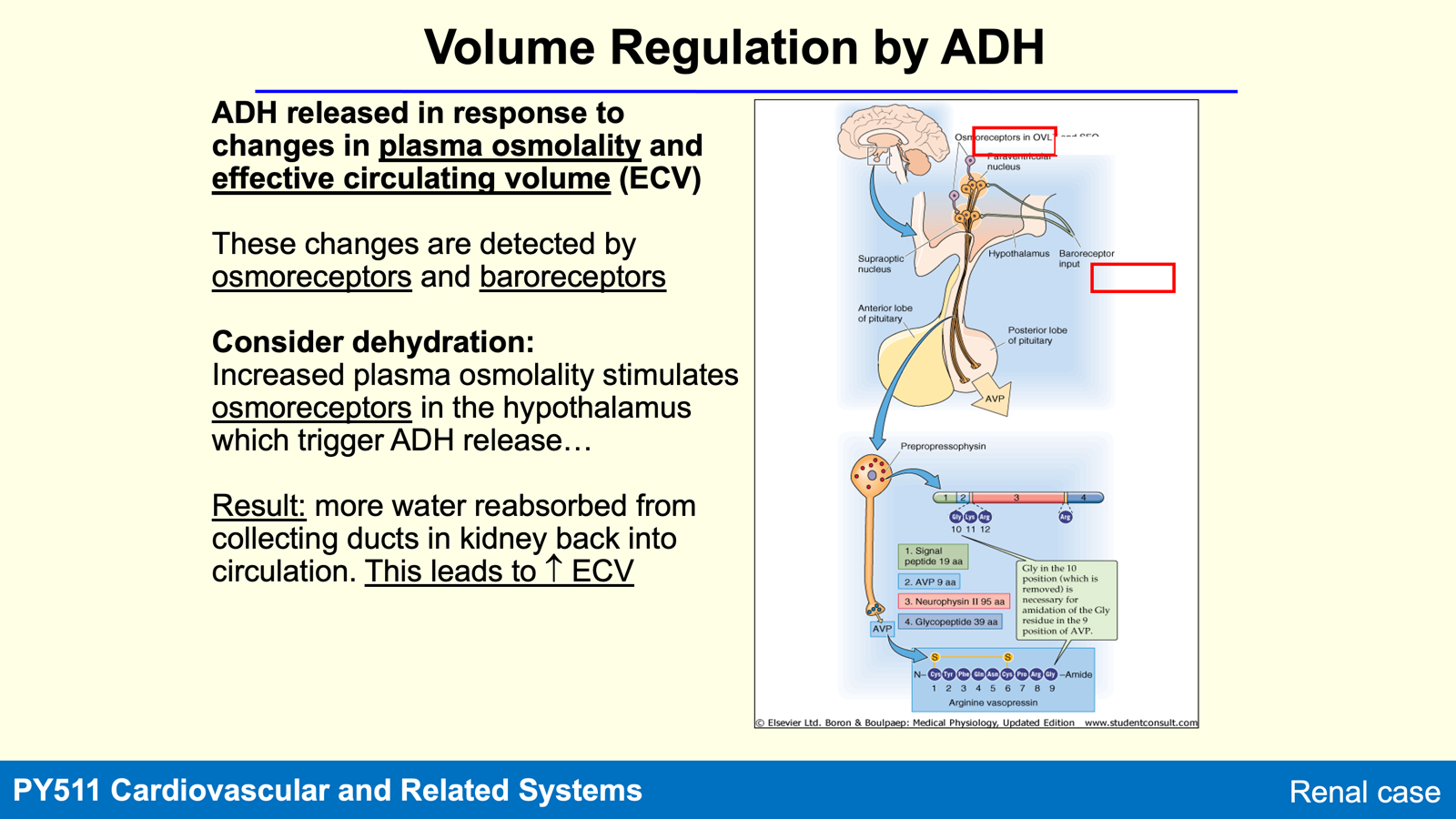
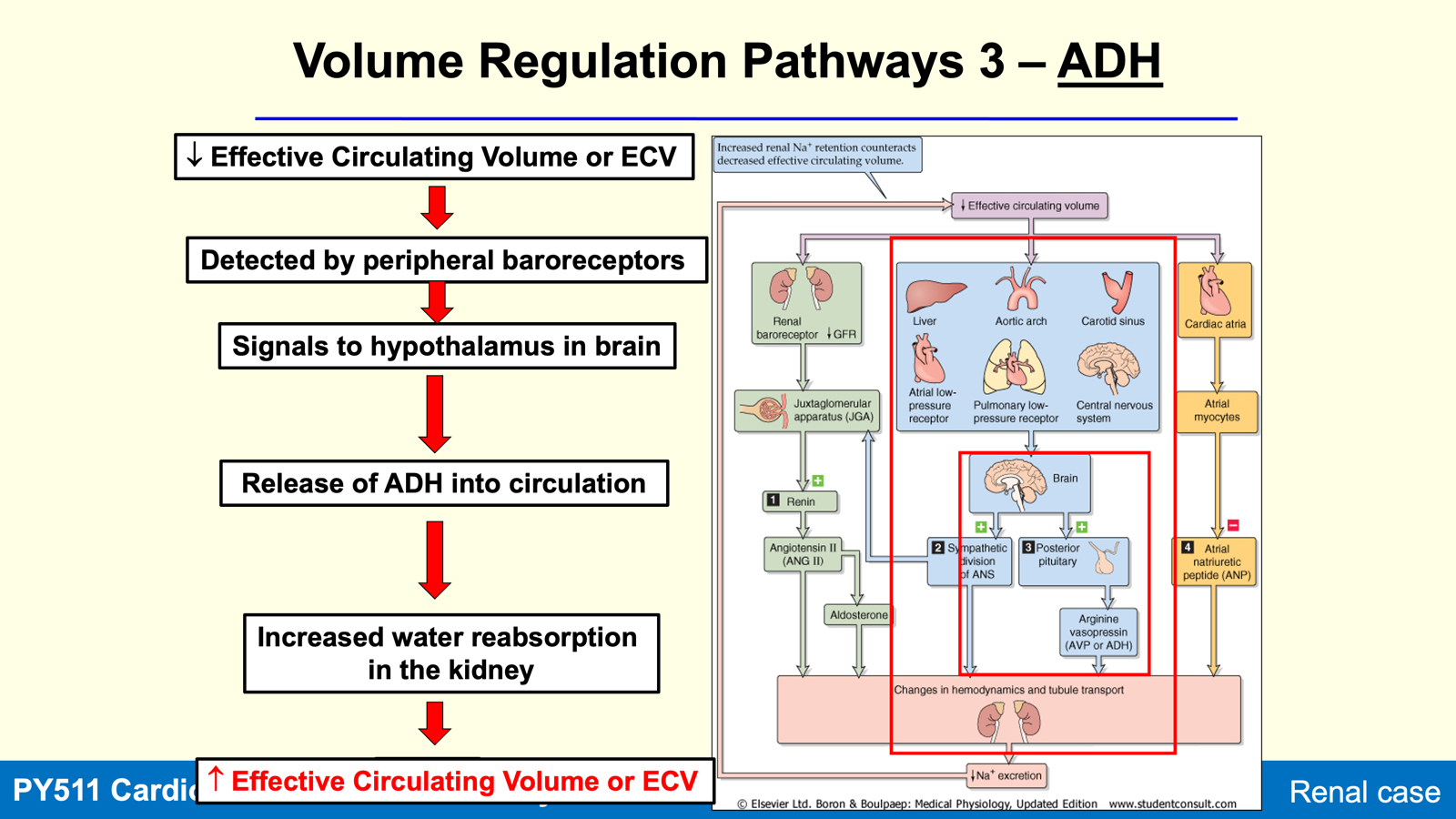
Hormonal Regulation of Water (ADH)
Alternative names: vasopressin or 8-arginine-vasopressin or AVP
ADH: Regulates water reabsorption
Plasma half-life: 10-15 min
Influenced by plasma osmolality and effective circulating volume (ECV)
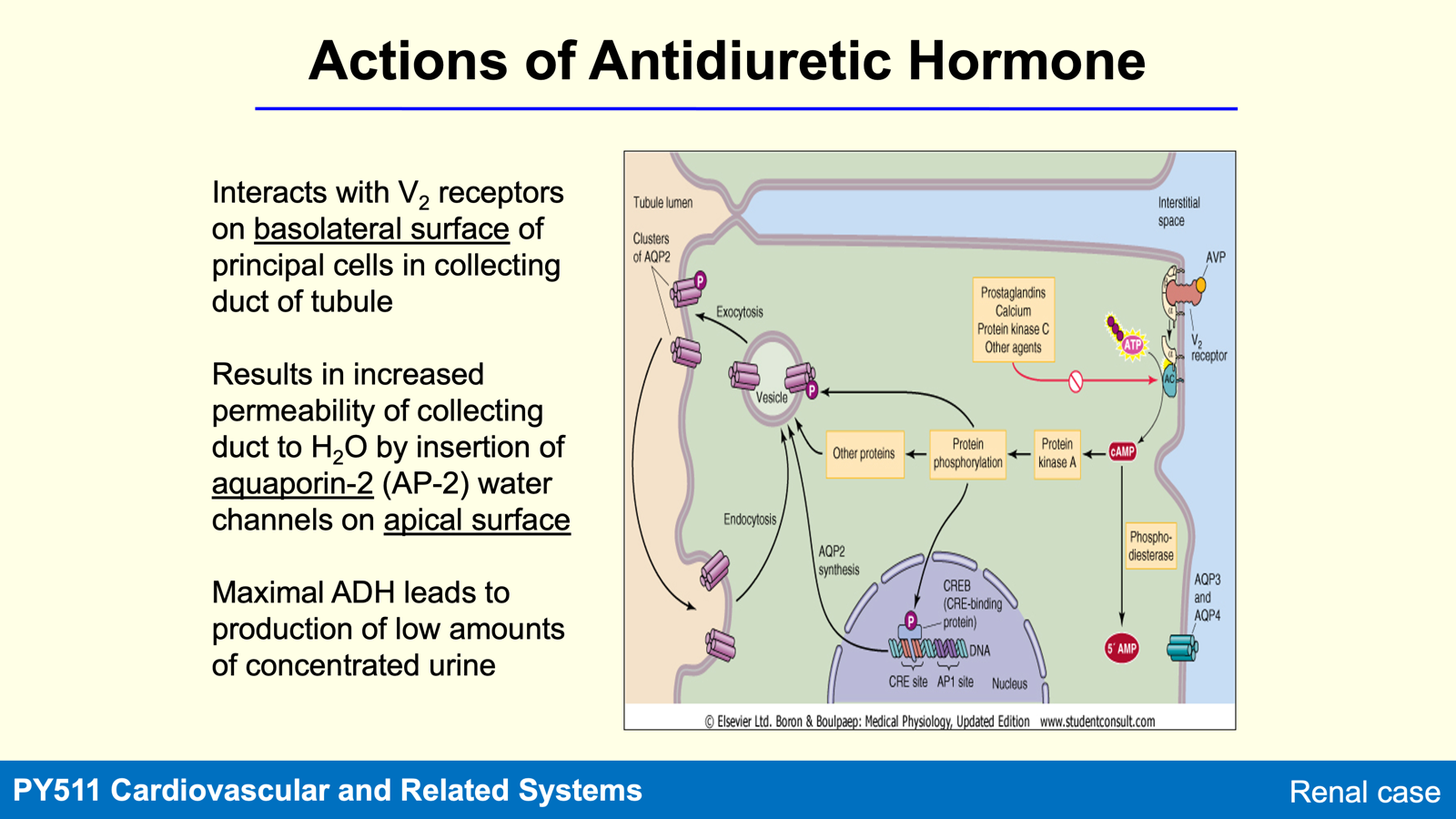
ADH acts on V2 receptors on basal membrane of principle cells collecting duct causing an insertion of aquaporin-2 (AP-2) into apical surface
Most important hormone for water balance
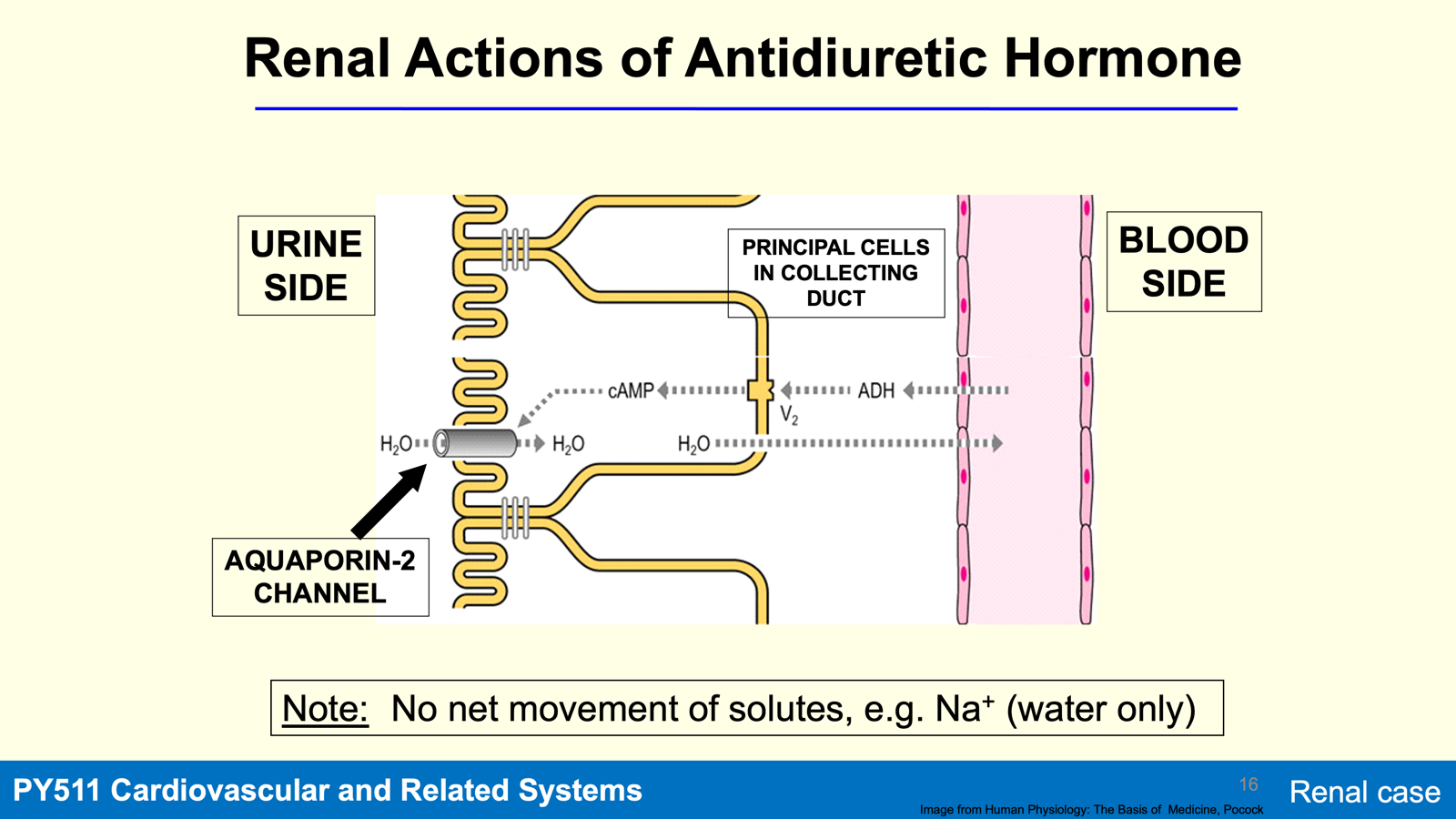
Actions of ADH
Increases water reabsorption from the collecting ducts back into circulation, resulting in concentrated urine production.
Released in response to increased plasma osmolality and decreased effective circulating volume (ECV).
Triggers thirst to promote water intake, further increasing ECV.

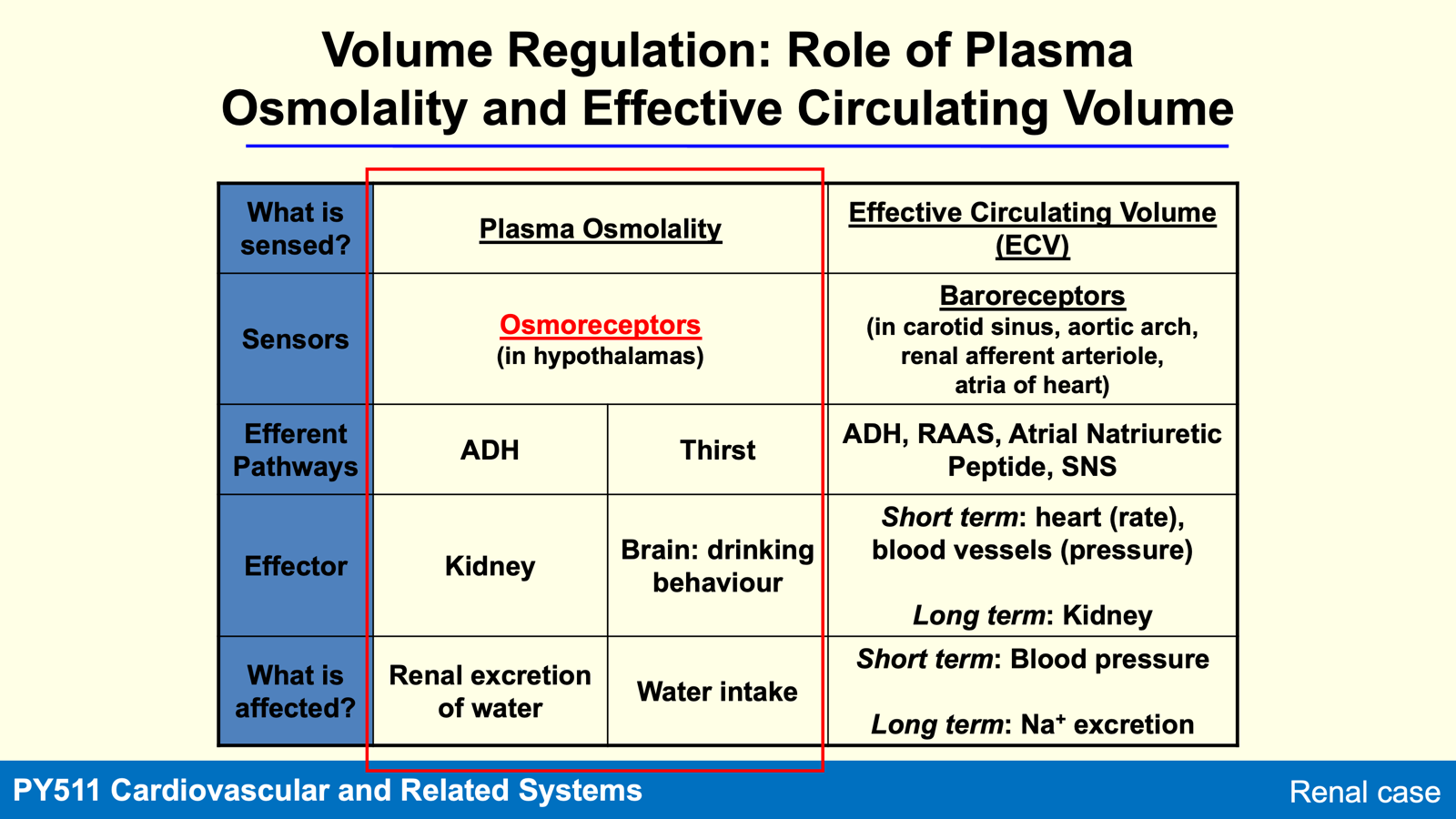
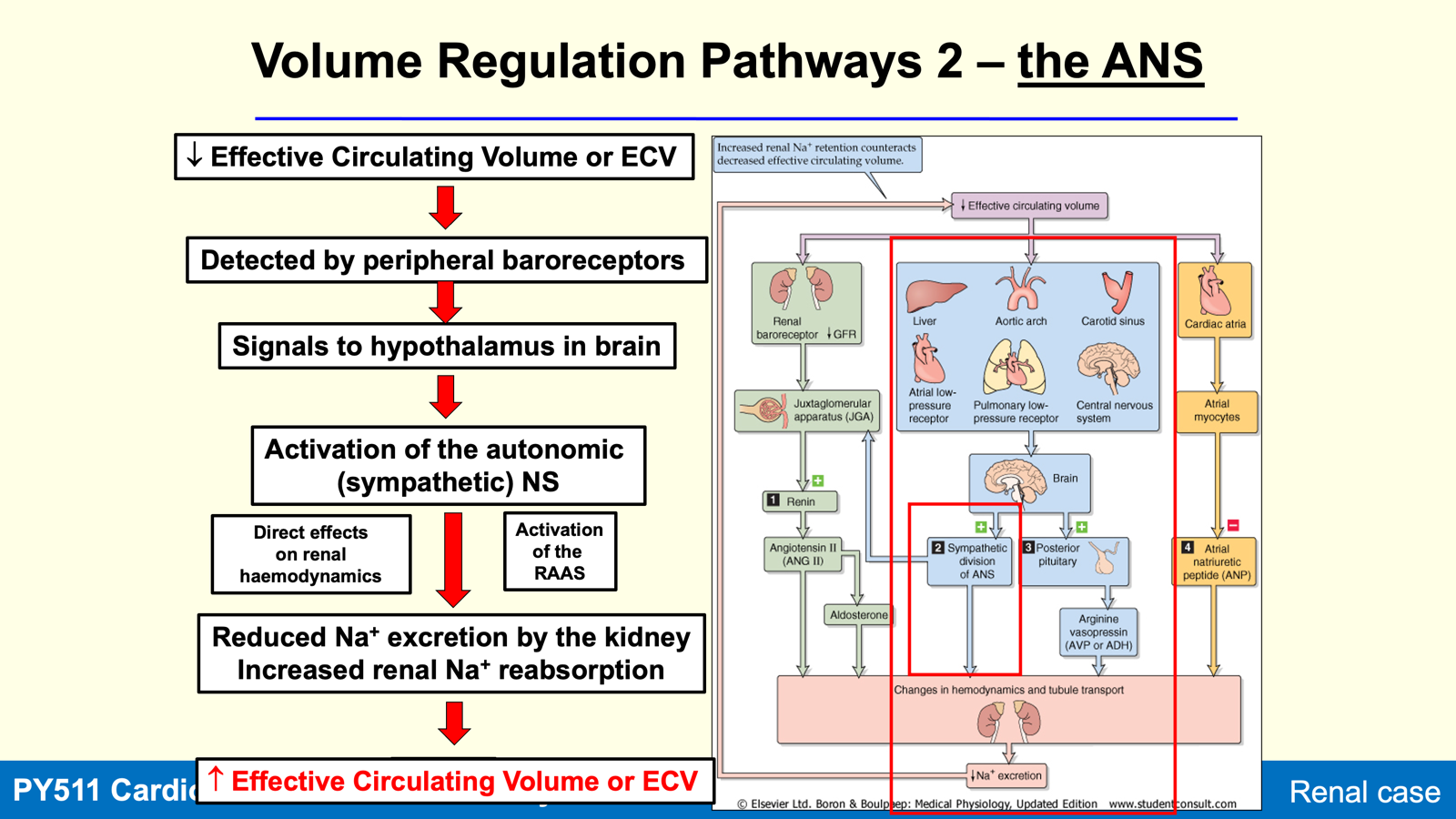
Sensors and Pathways in Volume Regulation
Key Sensors
Plasma Osmolality and ECV: Detected by osmoreceptors and baroreceptors.
Efferent Pathways: Include ADH, thirst response, RAAS, Atrial Natriuretic Peptide (ANP), and SNS.
Effects on Renal Function
Short-term effects on heart rate and blood vessel pressure.
Long-term effects involve kidney function and Na+ excretion.
Control of Effective Circulating Volume (ECV)
Baroreceptors
Function: Detect changes in ECV; involved in regulating blood pressure and volume.
Types:
Low-pressure receptors located in large systemic veins, cardiac atria, and pulmonary vasculature.
High-pressure receptors in carotid sinus, aortic arch and renal afferent arteriole (renal baroreceptor).
CNS and liver sensors aren’t as important
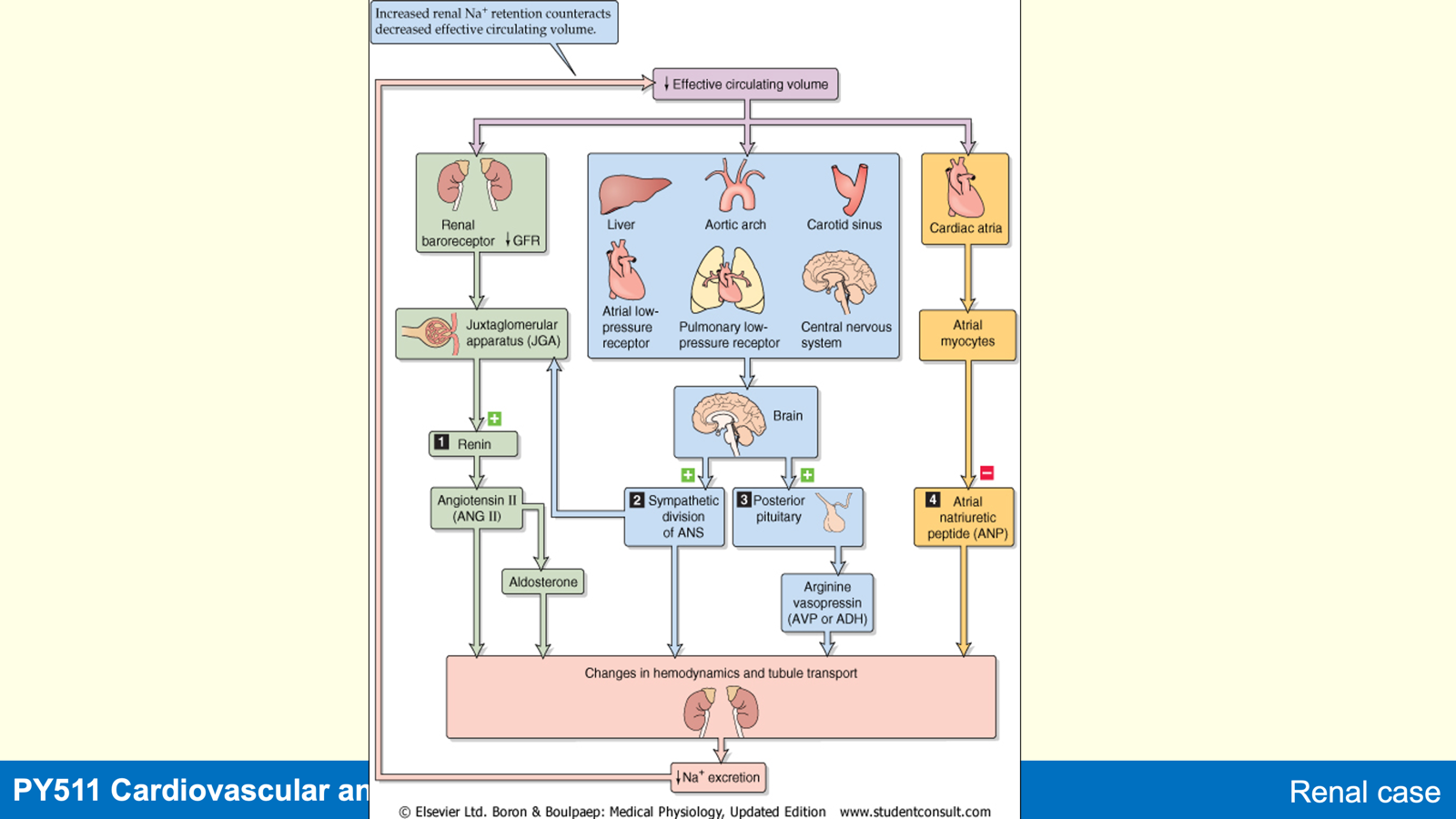
Control of ECV
Mediated by feedback control via baroreceptor stimulation.
Triggers four effector pathways affecting renal function:
RAAS.
Sympathetic nervous system.
ADH release.
ANP release.
Key Point: Pathway 4 is unique in reducing blood pressure/volume.
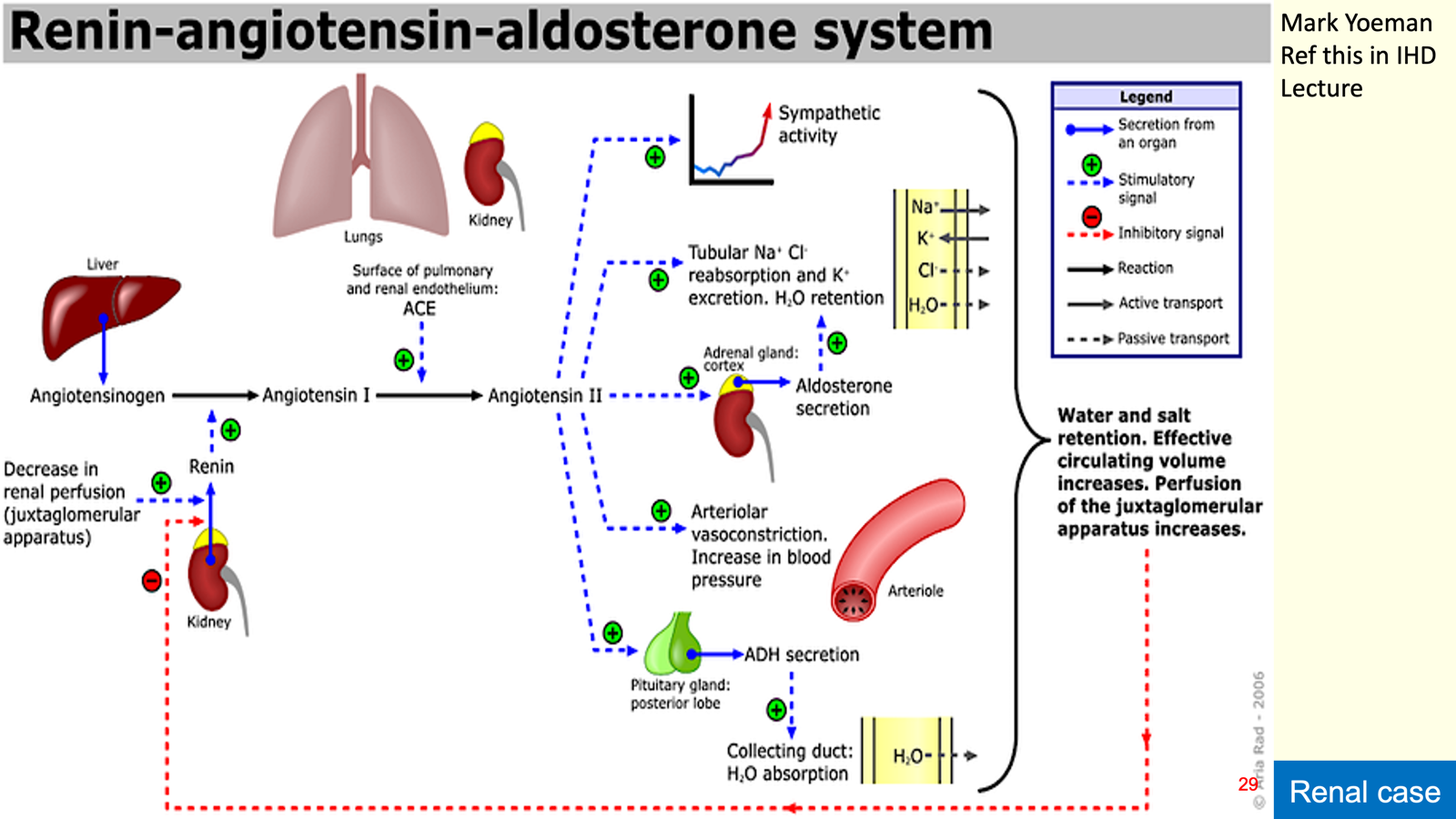
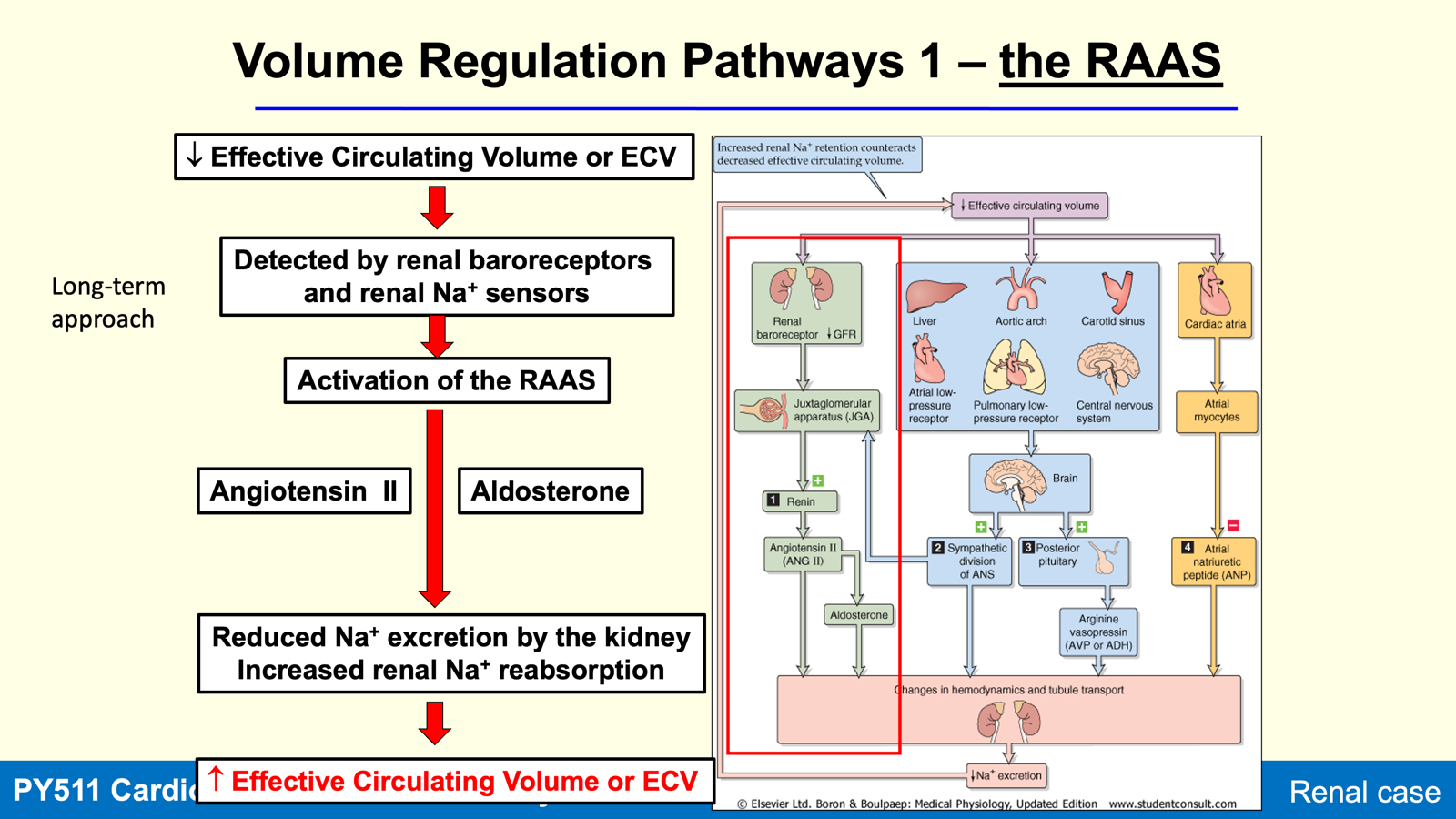
Renin-Angiotensin-Aldosterone System (RAAS)
Primary Control: Renin release from the juxtaglomerular apparatus (JGA) regulates plasma Ang II levels.
Stimulated by:
Decreased ECV (detected by renal baroreceptors).
Decreased Na+ concentration (detected by macula densa cells).
Decreased systemic blood pressure affecting SNS to JGA.
Actions of Angiotensin II
Enhances tubular Na+ transport, promoting Na+ and water reabsorption.
Stimulates aldosterone release from adrenal cortex, leading to increased Na+ reabsorption from distal tubule.
Acts on hypothalamus to stimulate thirst and ADH release into circulation.
Causes vasoconstriction of renal and systemic vessels, increasing systemic BP.
Longterm Effect: AngII causes renal cell hypertrophy for more protein synthesis of sodium transporters and channels
Aldosterone
Function: Collaborates with Ang II to increase ECV.
Stimulates Na+ reabsorption and K+ excretion in distal tubule and collecting duct.
Exerts indirect negative feedback on RAAS by increasing ECV and lowering plasma K+.
Conservers sodium and water
Excretes K+ from kidney which prevents large variations of K+ in plasma
Volume Regulation Pathways
Atrial Natriuretic Peptide (ANP)
Secreted in response to increased ECV
Actions lower ECV
Mechanism: Atrial stretches when ECV increases.
ANP is released in ersponse to stretch.
ANP promotes natriuresis (Na+ excretion from kidney) and renal vasodilation for increased blood flow, increased GFR and more Na+ excretion)
Na+ reaches macula densa at bottom of kidney and detects an increase in sodium.
JGA inhibits renin release in response to Na+ increase and AngII effects are reduced.
Overall: ANP inhibits actions of renin and opposes effects of AngII
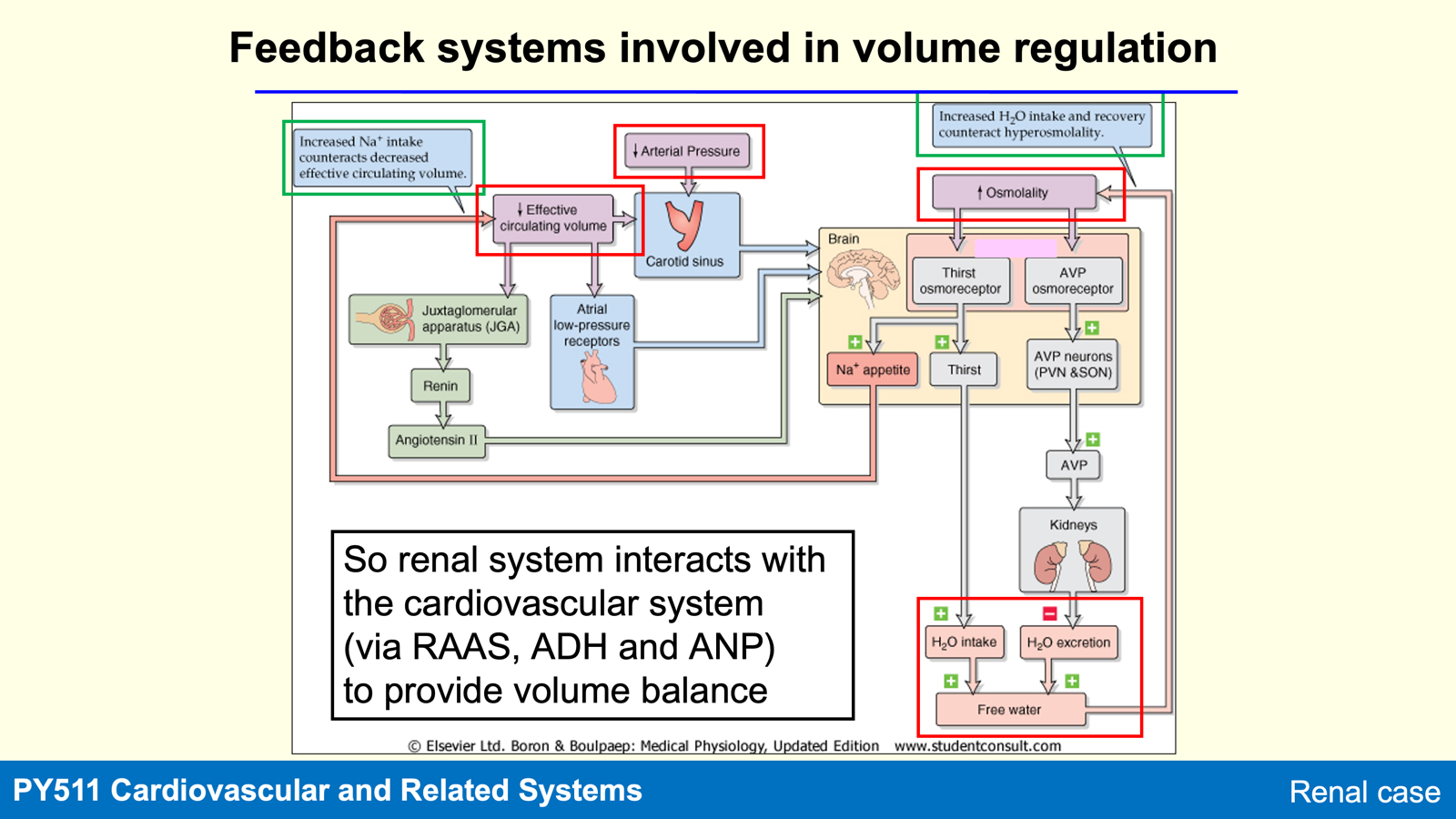
The renal system interacts with the cardiovascular system (via RAAS, ADH, ANP) to maintain volume balance effectively.
Lecture 2: Role of the kidneys in homeostasis and clinical cases
Acid-Base Balance
pH must be maintained between 7.35 - 7.45
Kidneys manage HCO3- reabsorption and H+ secretion
Lungs excrete CO2 as part of acid-base regulation
Responses to Acid-Base Disturbances
Acidosis: Increased H+; kidneys excrete H+ and generate more HCO3-
Alkalosis: Decreased H+; kidneys retain H+ and excrete HCO3-
Important Concepts
Inverse relationship between pH and CO2 levels
Role of kidneys and lungs in maintaining acid-base equilibrium
Body's compensatory mechanisms in acid-base regulation
Key Points
Understanding of kidney functions in blood volume and acid-base balance
Knowledge of regulatory mechanisms involving hormones
Recognition of clinical implications through patient cases
Example Questions
MCQ: Enzyme regulating CO2/H+ balance? (Answer: b) Carbonic anhydrase)
SAQ: Effects of vomiting on acid-base balance and kidney responses?