Homeostasis

Definitions:
Homeostasis – The process by which the body keeps its internal environment stable, even when external conditions change. It controls factors such as temperature, water levels, and blood glucose to keep the body working properly.
Glycogen – A large, branched carbohydrate made of glucose molecules. It is stored mainly in the liver and muscles and can be broken down to release glucose when blood sugar levels fall.
Diabetes – A medical condition where the body cannot properly regulate blood glucose levels. This happens either because the pancreas does not make enough insulin or because the body’s cells do not respond to it.
Excretion – The process of removing waste substances made by the body’s cells, such as carbon dioxide from respiration and urea from the breakdown of proteins. It helps prevent harmful waste buildup in the body.
Osmoregulation – The control of water and salt balance in the body to maintain the correct concentration of blood and body fluids. It mainly involves the kidneys, which adjust how much water is reabsorbed or lost in urine.
Nephron – The tiny functional unit inside the kidney that filters the blood, removes waste, and regulates water and salt levels. Each kidney contains about a million nephrons working together to produce urine.
Homeostasis
Homeostasis is the process that keeps the body’s internal environment constant.
It involves control systems that maintain stable conditions, like temperature and blood glucose.
Example: insulin controlling blood glucose levels.
Factors that need to be controlled:
Internal body temperature
Blood glucose levels
Waste product concentration (CO₂ and urea)
Blood water levels
Controlling body temperature
Enzymes work best at an optimum temperature.
If too cold, reactions slow down (reversible); if too hot, enzymes denature (irreversible).
Warm-blooded animals (endotherms):
Maintain a constant body temperature.
Adaptations include:
A fat layer under the skin for insulation
Fur, feathers, or hair trapping air to reduce heat loss
Hair erector muscles contract in cold, raising hairs to trap more air
Cold-blooded animals (ectotherms):
Body temperature changes with surroundings.
Control temperature by behaviour — basking in sun to warm up, seeking shade to cool down.
Often inactive in cold weather and rarer in cold regions.
Skin
Functions of the skin:
Protects internal organs from damage
Prevents pathogens from entering
Controls water loss
Detects temperature, pressure, and pain
Helps regulate body temperature
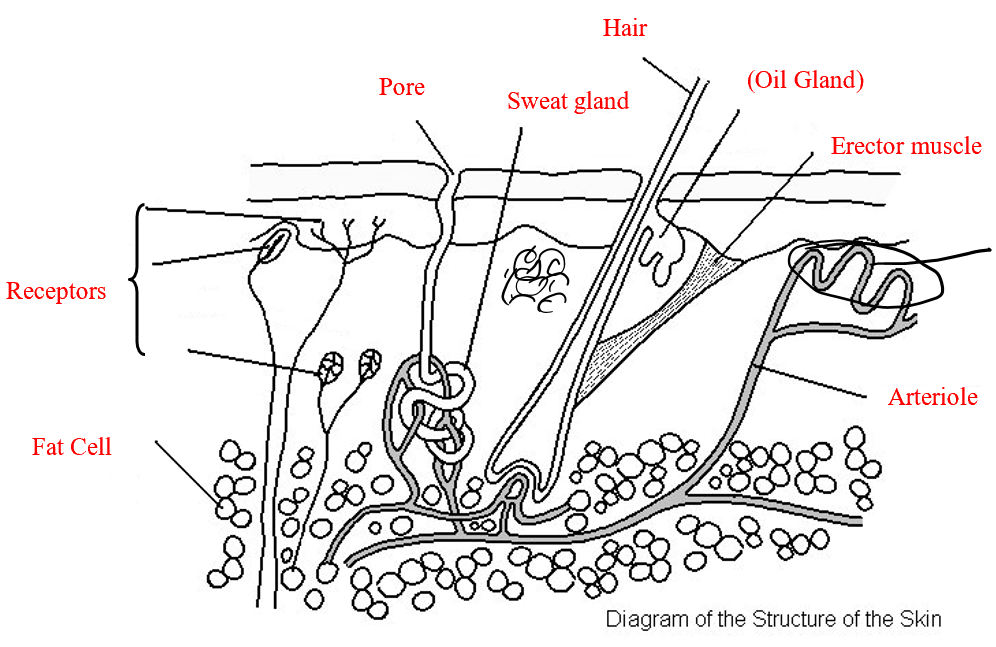
Controlling body temperature
Normal body temperature is about 37°C.
The hypothalamus in the brain monitors blood temperature and receives nerve signals from the skin about external temperature.
When it’s hot:
Arterioles widen (vasodilation), increasing blood flow to skin capillaries and heat loss by radiation.
Sweat glands release more sweat; as it evaporates, it cools the skin.
When it’s cold:
Arterioles narrow (vasoconstriction), reducing blood flow and heat loss.
Sweat production stops to prevent cooling.
Erector muscles contract, raising hairs to trap warm air.
Shivering occurs as muscles rapidly contract, producing heat.
Metabolism speeds up slightly, releasing extra heat.
Vasoconstriction and vasodilation:
The capillaries themselves do not dilate (they have no muscles)
Its the arterioles leading to the capillaries to dilate
Capillaries DO NOT move closer to the skin
Controlling blood glucose
Glucose is stored in the liver and muscles as glycogen, an insoluble carbohydrate similar to starch.
When glucose levels are low, glycogen is broken down to release glucose into the blood.
After a carbohydrate-rich meal, blood glucose rises as glucose is absorbed from the small intestine.
The hepatic portal vein carries this glucose-rich blood to the liver.
The pancreas releases insulin when blood glucose is high. Insulin makes liver and muscle cells absorb glucose and store it as glycogen, lowering blood glucose levels.
When blood glucose drops, insulin production stops, and glycogen breakdown increases.
This is an example of negative feedback — once balance is restored, the response stops.
How would high blood sugar levels affect the amount of water in cells?
The blood would have a lower water potential than the cells. Therefore, water would move by osmosis out of the cells and into the blood down the concentration gradient. Cells shrink/shrivel.
Diabetes:

Excretion
Excretion is the removal of metabolic waste produced by chemical reactions in the body, such as carbon dioxide and urea.
The two main waste products are:
Carbon dioxide – made during respiration, removed by the lungs.
Urea – made in the liver when excess amino acids are broken down (deamination); removed by the kidneys in urine.
Small amounts of waste, such as salts and water, are also excreted through the skin.
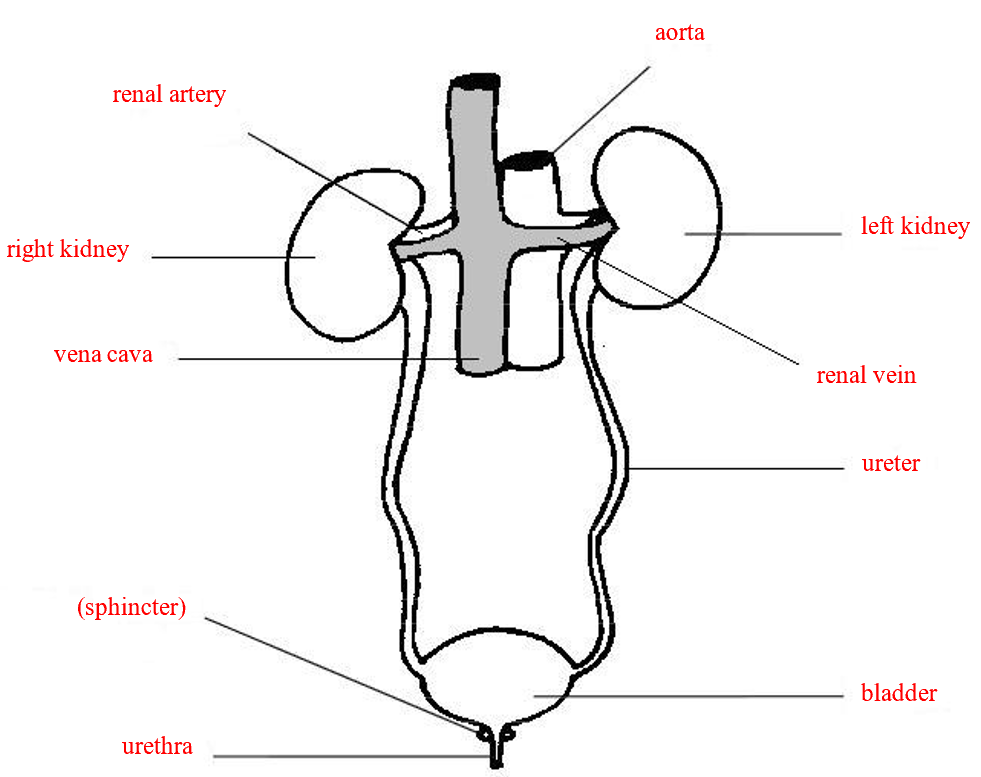
The urinary system
The kidneys filter the blood, removing waste and controlling water and salt levels.
Humans have two kidneys at the back of the abdomen.
Blood enters each kidney via the renal artery (from the aorta) under high pressure.
Filtered blood leaves through the renal vein, which joins the vena cava.
Urine from the kidneys travels through the ureters to the bladder, where it is stored.
It leaves the body through the urethra.
The urethra has two sphincter muscles:
The upper one is involuntary and relaxes automatically when the bladder is full.
The lower one is voluntary and allows conscious control of urination (babies learn this over time).
Extension:
The wall of the urethra contains two ring-like muscles called sphincters that can contract to close the urethra and hold back urine. The lower sphincter is consciously controlled, while the upper one is involuntary it automatically relaxes when the bladder is full. Babies have to learn to control the lower sphincter and this is why they can’t control their bladders
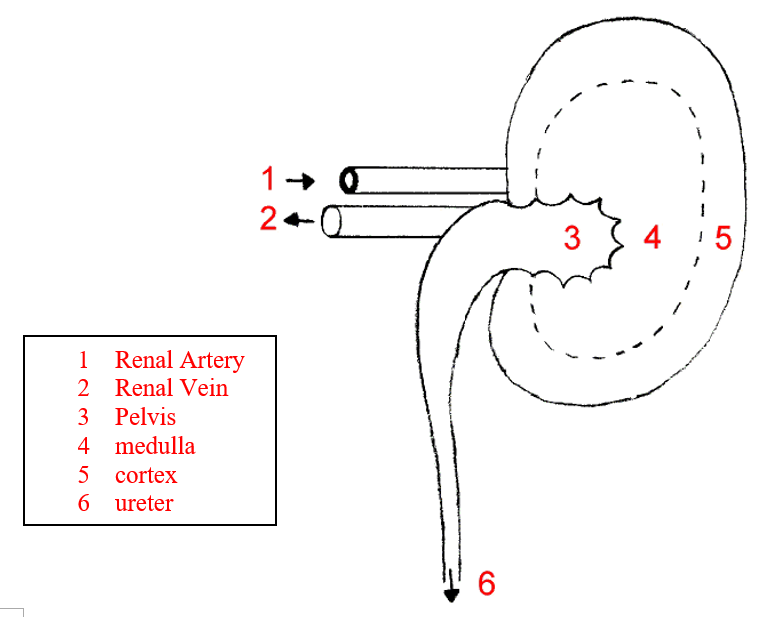
Functions of the structures of the kidney:
Details of kidney structure
The dark outer region is called the cortex, containing many small blood vessels branching from the renal artery.
The cortex also holds microscopic filtering tubes called nephrons (kidney tubules).
These tubules extend into the middle layer, the medulla, which contains inward-pointing pyramids.
The tubules join together at the tips of the pyramids and drain into the pelvis.
The pelvis connects to the ureter, which carries urine to the bladder for storage.
The nephron
The nephron is the tiny filtering unit of the kidney.
It removes waste products like urea and excess salts while keeping useful substances such as glucose, amino acids, and water in the blood.
The remaining waste forms urine, which is passed to the bladder.
The nephron has three functions; ultrafiltration, selective reabsorption and water regulation
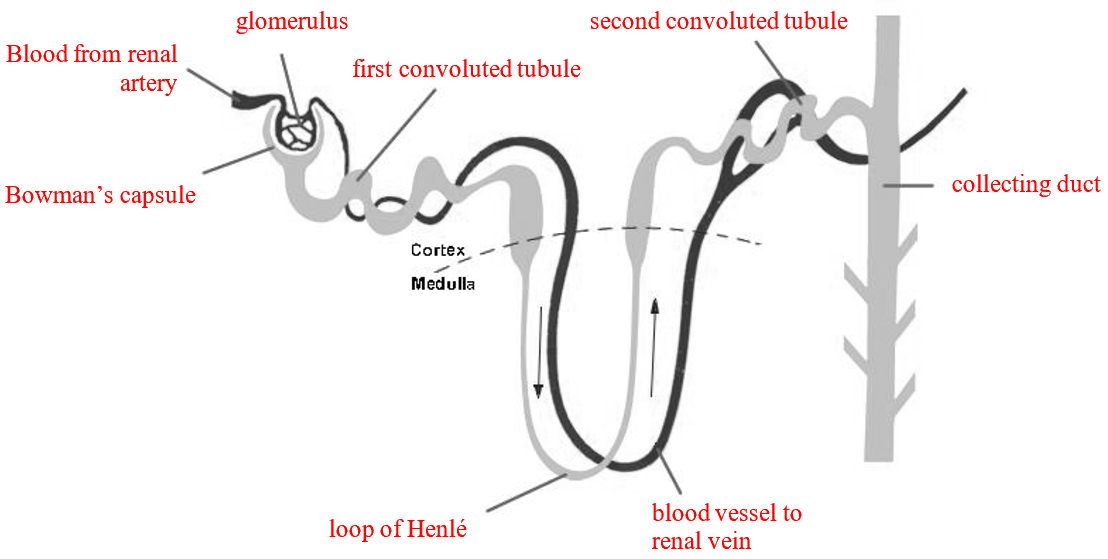
Ultrafiltration
At the start of the nephron is the Bowman’s capsule, surrounding a knot of capillaries called the glomerulus.
Blood enters the glomerulus under high pressure from the renal artery; the outlet vessel is narrower, increasing pressure.
This pressure forces water, ions, glucose, and other small molecules out of the blood into the Bowman’s capsule, forming the glomerular filtrate.
Large molecules like proteins and blood cells are too big to pass through and remain in the blood.
The filtrate then moves into the proximal convoluted tubule.
Selective reabsorption
In the proximal convoluted tubule, useful substances such as glucose, amino acids, and some water and salts are reabsorbed into nearby capillaries.
Reabsorption happens by diffusion and active transport, which uses energy.
Around 99% of the filtrate is reabsorbed; only about 1% leaves the body as urine.
Water regulation
The Loop of Henlé in the medulla creates conditions that allow water to be reabsorbed, concentrating the filtrate.
The distal convoluted tubule and collecting duct reabsorb more water to maintain balance.
This stage is controlled by the hormone ADH (anti-diuretic hormone).
The collecting duct carries the final urine to the kidney pelvis.
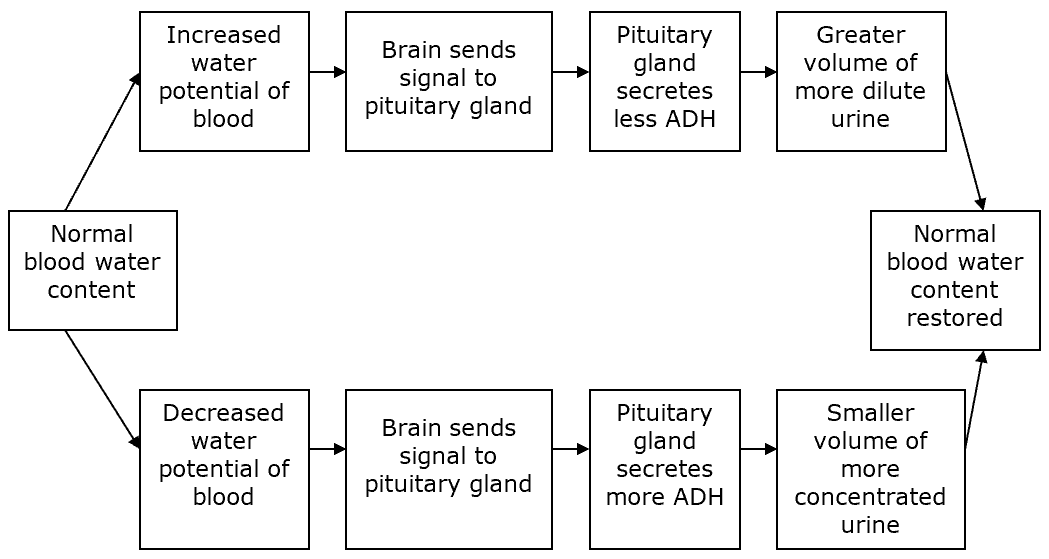
Osmoregulation and ADH
The kidneys regulate water and salt balance to keep the blood concentration stable — a process called osmoregulation.
Drinking lots of water produces a large volume of dilute urine.
When the blood is concentrated, the kidneys produce small amounts of concentrated urine.
These adjustments are controlled by ADH, made by the pituitary gland.
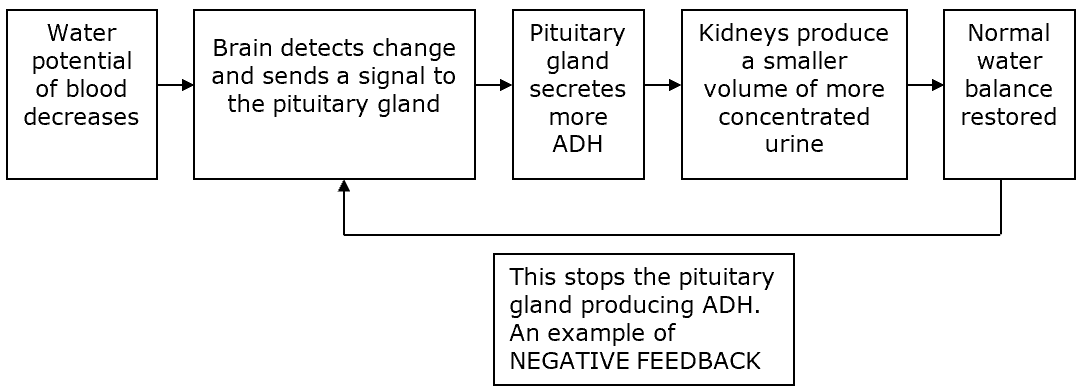
Too little water in the blood
Low water levels make blood more concentrated.
The hypothalamus detects this and signals the pituitary gland to release more ADH.
ADH makes the collecting ducts more permeable, so more water is reabsorbed into the blood.
Urine becomes concentrated, and blood returns to normal.
When balance is restored, ADH production stops — an example of negative feedback.
Too much water in the blood
When blood is too dilute, the hypothalamus tells the pituitary to release less ADH.
The collecting ducts become less permeable, so less water is reabsorbed.
This produces large volumes of dilute urine, restoring balance.
Explain which part of the nephron will the cells making up the wall contain the most mitochondria?
The part of the nephron where cells contain an abundance of mitochondria is the proximal convoluted tubule (PCT). It is the site of maximum tubule reabsorption and is where the most active transport occurs where particles such as glucose and amino acids are reabsorbed.
ADH summary
After exercise/hot day/dehydrated | No exercise/cold day/well hydrated | |
ADH levels | High | Low |
Permeability of collecting duct | High | Low |
Concentration of urine | High | Low |
Volume of urine | Small | Large |
Summary of osmoregulation: