Newborn 2-28 days
Biological behavior
physical development factors: gestational age, maternal health, nutrition during pregnancy, birth order, genetics, and multiple births
→ early/ mulitple = low weight
→ later age/ maternal DM = higher weight
VS
temp: 36.5-37.5C → fever >38C and always by HCP if found of <3m
axillary w/ 5 mins
HR: 110-160 = auscultated for full minute
irregular if ill
RR: 30-60 ← full minute + periods of tachy and apnea ok (not if >10sec)
BP: not routinely measured but average = 64-41
→ factors that change BP = maternal H, health prenatal, heart/ lung/ vessel/ kidney; exposure to certain meds/ illicit , genetic, congenital thyroid
O2 = >95%
height/weight:
post natal malnutrition from inadequate intake
weight loss of 10% in 2-3days after birth is ok→ regained by 2nd week
fastest weight in 3 months → inc 30 g/day
inc of 25cm in 1st yr
male: 50.8cm birth → 54.6cm
female: 50.17cm birth → 53.34cm
male>female in 1st month
head/ skull: bones not fused to be able to pass through canal → skull grows and fuses = head circumference and fontanels
circumference: mishappen resolve by 2nd week = more round
~ 35cm → 1m 38.1 cm → 1yr = 12cm inc
fontanels (soft stops) : 6
anterior = diamonds and largest between frontal and parietal over superior sagittal sinus
asculate
posterior= triangle between parietal and occipital lobes
should be flat and firmed when palpeted
sunken = dehydration → bulging = infection
SUTURE
PLAGIOCEPHALY = laying back bby flat back head
cranio stenatosis= premature or brain not growing
hair: some w/ hair but falls out ~ 1m and replaced
cardiac: ductus arteriosus and foramen ovale close = 12-24hrs → full 2-3w = inc flow to lungs → inc pressure + blood volume to all organs
resp: transition to breathing occur immediatly after birth but days to weeks to complete
central apnea can last 3-6 sec
newborn sneeze to clean airway → sound congested or noisy when breathing due to narrow nasal passage and small amount of nasal fluid
musculoskeletal: spine straighten w/ ocassional back arch
leg/ feet inward = bowlegged look
legs and arms stretch out
skin:
present w/ acrocyanosis = blue in extremities due to low O2 in peripheral + vasocontrict
—-all normal
mottling: skin patten of pale and red skin
milia: bby acne on nose and chin
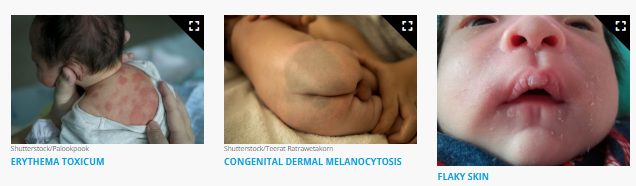
erythema toxicum: flesh-colored papules on erythematous base on face and trunk → newborn within 1 week after birth
congenital dermal melanocytotic = darker, bluish colored patches of skin ~ African, Indigenous, Asian
Salmon patches: disappear within a year
2 weeks after birth → newborn skin flake off (especially if born after 40 gestation weeks)
Abdomen:
full and rounded w/ protrusion of muscle tissue when crying or straining = resolve few w
umbilical hernia: opening of ab muscles around cord that allows intestines to protrude when bby is crying → close own but can require surgery
umbilical cord is clamped/tied then disconnected from placenta = 10d → 3w = dry off, fall, belly button
24hr need their 1st BM
Hirschsprung= missing nerves of large intestine
→ if soiled = stump washed w/ water to clean
→ report redness, discharge, foul smell
motor skill:
1sr month = adapt to surroundings but to motor to major muscles, hands, wrists → playtime
gross= uncontrolled, erratic, no neck stregth to hold neck → parents hold neck
innate reflexes: rooting, Moro, Babinski, grasp, tonic neck, suck, and stepping,
fine motor: bring hands to eyes and mouth, keep hands in tight fist in 1st month
→ swing arms at toys or people
psychosocial:
→ sleep, eat, cry (communication for attention)
→ bonds w/ parent: if they can expect their needs to be met
→ beginning to recognize voices of fidd parents = settling and calming when upset or crying
→ cuddling = binding, affection, safety sense
cognitive: thinking and learning
hearing → respond to familiar voices but cannot understand + startle at new sounds they do not recognize
vision → uncoordinated and crossed eye → fixate in face or light → infant begin to follow moving object
see clearly 8-12 in
use toys and mobile w/ strong colors
smell: best developed = perfer sweet → encourages rooting and sucking
touch: sense security in parent arms and swaddling improve newborn feeling and prevent from being startled
language development
primarly crying → end of 1st month coo + babbling
body language of parents (hold, feed, facial expression)
crying peaks 6-12w after birth
play: develop bond = smiling, singing, reading, rocking, toys (bold colors/ but soft texture)
therapeutic communication w/ parents
28days of development = physcial changes of wrols and ability to communicate needs
talk about appropriate weight gain, ways to help growth and development
encorage skin-skin contact, swaddle, speak and make eye contact, face-face and close (build motor control of neck and head)
change tone of voice or expression w/ talking, reading book, sing
mindful of needs
Newborn behavior
bind w/ parent, communication through crying comfort, sleep, and food, explore environment through sense
parent education on meeting newborns needs
cry
seek attention of needs or need to feel secure and loved
2-3hr or more (mostly on evenings) of crying daily for 1st 6w. infants cry more
as bond grow, needs are more distincted and easier to meet needs
reflex
from brainstem
root reflex: cheek or mouth gently stroked → turn head, open mouth and start sucking → aids on finding nipple
after time → becomes voluntary
suck reflex: 32-36 gestation
when nipple or bottle touch roof of bby mouth → suck
breathing and swallow while sucking is complicated so not efficient at first
→ suck fingers/ hand-to-mouth reflex
comfort measures such as pacifier/ thumb or finger sucking
moro/ startle reflex: when startled by a loud sound or sudden movement
→ pull on bby arms while laying on back ad let go of arms → sensation of falling and reacts = extends arms, legs, cries, and pulls arms/legs to core of body
no need to raise infant head off (more about sudden of stimulus)
25w of gestation and 30w gestation
tonic neck reflex:
lying on back and head is turned to one side → arm od side wll extend out w/ hand slighly open and the arm on the other will bend and flex fist clenched (fencing)
check if bilateral
grasp: 16w → 25w = palm stroked → fingers close
→ bby placed supine when awake and palm is stroked since pressure produces tendons and clings
only fingers not thumb
Babiski:
corticospinal tract and can see CNS (stroke or spinal injury) = expected since tract is not fully myelinated at birth→ reflex = dull, blunt object moved up to lateral plantar side of foot from heel to toe then up to metatarsal pads
→ dorsiflexion (fan out)
no movement os neutral response
step: 1st 2 months after birth
hold new born in flat surface → place one foot in front of other = cannot support themselves w/ reflex (not ready to walk)
helps make way from mother stomach to breast
bonding
can start from birth, or a little longer → can also happen w/ non-pregnant partner, siblings
hold newborn close to body, making eye contact; talking, singing, or reading to the baby; feeding the baby; and rocking them to comfort them within minutes to hours after birth.
new born : crying, smiling, rooting, and making eye contact
parent spending 16hrs or more w/ physcial contact is reluctant to leave bby w/ other person, try to calm down infant, engage in eye contact and caressing
inc physical contact = enjoy longer/ calmer sleep, better temp control, physcial muscoskeletal health
lack = inappropriate weight gain, withdrawn, indifferent, depressed
other parent or sibling = spent quiet time holding, comforting bby, eye contact, singing, reading, talking to newborn
sibling = help w/ new bby as much as possible, spend time together, newborn give gift to other sibling
communication w/ parent
calm, slow breaths while interacting w/ newborn + take breaks
reasure stess and overwhelmed is part of adapting to dynamics
parent should ensure infant does not show signs of illness, feed them, change their diaper, rock them or walk around holding them close, sing or talk to them, and play music.
go for a drive or for a walk with the newborn in the stroller, try a warm bath, give the infant a massage, and use different types of movement.
Disease and Prevention
car seat safety:
high risk of death from MVA due to developing spines and large heads
→ semi-reclined car seat (for airway open) + harness straps should be securely and flatly fastened over newborn shoulders with chest buckle at level of newborn armpit
no bulky cloth over newborn before buckling + empty spaces filled w/ rolled blankets on side of shoulder and head
rolled washcloth between diaper gap and buckle
falls
pay attention to footwear, having one hand to hold onto stair rails and having soft surfaces
head injuries: from fall or drop
Shaken baby syndrome (SBS) → abusive head trauma (AHT) = shaking newborn when caregiver becomes frustrated
place bby in room, leave room, call someone for support
→ give parents resources = counseling or local crisis center
smoke: → exposed to carcinogens and can get stuck in cloth and hair
→ increase sudden unexpected infant death (SUID), resp infections, ear infections, asthma since lungs are developing and affect brain
disease prevent/ health promotion
adults/ sibling get Tdap since infants dont receive vaccines until 2months
under 1m = breastmilk/ formula
in 6m = eats, sleep, grows ← pt learns cues
40-50% of energy should be provided by fats in breastmil and formula
Vit D 400IU/ day who soly breastfeeds
Rooting, sucking, and hand movements = hunger cues
+ if newborn continues to cry = diff to feed
slow pace of feeding, turning away, falling asleep = feeding complete
burped frequent = avoid overfeeding/ trapping air in stomach/ intestine
recommend breast feed 6 months = supports gastrointestinal function, immunological defenses, neurodevelopment, and psychological growth
but sometimes does not work = inadequate milk supply, difficult transition to home, and return to work for the breastfeeding parent.
Keeping the newborn in the room after birth, increased physical interaction and contact, and avoidance of infant formula increase the length of time babies are breastfed
fed ad lib ~ 2-3hr (8-12 times/ 24hrs) for 15 mins on each breast + 6-8 wet diapers/ day
latching diff = but good w/ time
formulas have iron
hypoallergic/ soy protein if cannot tolerate milk protein
2oz of formula 2-3hr in 1st week
+at least 6 diapers and 3 or more BM/day
→16-24oz/day
Meconium (tarry blac, sticky, 1st stool) passed ~ 24-48hr after birth
Sleep: sleep ~ 8-9hrs day and 9 hrs at night = begin not to sleep through night until later
place on back on firm surface
tight fitted sheet — no toys stuffed animals, blanket, bumper pads
don’t sleep w/ parent or others since suffocation by rolling onto bby or blocking airway= infant fatality
if falls asleep on car seat or bouncy seat, → relocate to crib and placed on back to sleep
don’t fall asleep while holding/ feeding newborn
activity:
Smiling, eye contact, and the sound of voices
sleeps alot in 1st month
→ when quiet, awake, alert = more likely to respond to interactions w/ others
if fussy or crying = will not be receptive to play or learning
Crying, hiccupping, sneezing, yawning, spitting up, burping, and gurgling
→ tummy time x4/ day for 15 min = builds neck muscle and allows exploration of space, motor skill + helps bby see in diff angles
→ pt should be sitting or lying next to newborn
infant responding w/ smile or babbling = communication
bright colors, mirrors, mobiles, and books, encourages the newborn’s eyesight to develop
therapeutic communication w/ parents:
avoid those who are sick or unvaccinated
get Tdap and good handwashing
listen to pt culture
education of vit D and appropriate feeding and dehydration
health concerns
altered nutritiom
growth restriction = undernutrition = growth failure/ failure to thrive inc risk of premature
→ problem w/ growth, thermoregulation, basal met rate
premature = inc risk of childhood and adult obesity, insulin resistance, and DMT2
100kcal/kg/day
neonate = 110-135 cal/ kg
check growth charts → <30g of gain/ day = check for metab, cardiac, CF
food sensitivity
check w/ Stool testing, blood testing, and skin testing
allergic reaction by cow milk protein
→ resp = wheezing, trouble breathing, coughing, hoarseness, throat tightness
→ GI = vomiting, diarrhea, indigestion
→ other s/s = itchy and watery eyes, hives, swelling, hypotension
if not use soy protein or extensively hydrolyzed formula or amino acid based formula
can also get milk protein by mom ingesting milk protein = can still breatfeed just be careful
monitor food eaten and how much dairy consumed
colic
when bay cries in extended period w/o known cause (3hrs/day more than 3 days/ week, for 3 weeks)
louder, higher pitched, more emergent than regular crying
bright red flushed face, a tight abdomen, pulling up of the legs toward the abdomen, and clenching of their fists
→ check CXR, blood test, health hx
common in 6w → no intervention require (3-4 months)
sooth bby, eliminate s/s
curved bottle in upright position to decrease gas or help burping often
theory = sensitivity to the transition to the external world, an inability to calm themselves, sensitivity to gas, or a possible milk allergy or intolerance
inc in evening and into night
parent communication
encourage breastfeed but monitor diet
if formula given = burping w/ every oz + curved bottle should be used, placed upright 30 mins after feed
if allergy sus → hypoallergic/ soy formular for trial
colic parents
→ take breaks, time to decompress, rejuvenate, reassure colic resolves on its own
nursing process
star w/ ascultation first since calm = anterior fontanel, heart, lungs, and abdomen
do head to toe
VS, capillary refill
head = fontanels, head shape
visualizing the eyes, ears, and nose for any discharge
PEERLA
hard and soft palates are intact and the tongue is freely movable.
neck mass, Palpate the clavicles.
chest symmetry/ shape
abd = soft to the touch, BS present.
umbilical cord should be clean, dry, and intact with no discharge, redness, or foul odor.
genitalia = abnormalities and rash.
Palpation of the testes in the scrotum is an expected finding in male newborns who are term.
Female newborns may have a prominent labia majora. Some vaginal bleeding due to withdrawal of the maternal estrogen
extremities for passive ROM, symmetry, the number of digits, and the presence of fused or webbed fingers.
Femoral and brachial pulses palpable and equal bilaterally.
birth marks or rashes.
spine for symmetry and make note of any tufts of hair at the sacrum, sinus tracts, masses, or a sacral dimple that is larger than 0.5 cm (0.2 in),
Reflexes, including Moro, Babinski, grasp, root, suck, tonic neck, and step reflexes.
assess feeding, voiding, stooling, and bonding., attachment style
prioritize: ABC, feeding, sleep (in safe enviroment)
nutrition= discuss proper nutrition and guide resorces
colic → stress + altered sleep pattens
→ ways to improve sleep, such as music therapy, infant massage, and skin-to-skin contact.
Down syndorme = hypotonic